Abstract
Scrub typhus is an acute febrile bacterial illness and has a high mortality if left untreated. It is caused by bacterium called Orientia tsutsugamushi which is transmitted to humans as zoonosis by bite of chigger mites that are infected by the bacterium. The diagnosis is based on clinical features and specific laboratory tests. Treatment of Scrub typhus is done with antibiotics and symptoms management. This report is a case of a 24-year-old female febrile patient who presented with complications of Scrub typhus due to missed diagnosis at Primary Health Centre and managed at district hospital. This case report highlights the challenges faced by health workers in management of acute febrile illness in a diagnosis-constrained setting.
Keywords
Introduction
Scrub typhus is an acute febrile bacterial disease with an estimated 1 million new infections each year in the Asia Pacific region alone. 1 There are also evidences of Scrub typhus patients documented in the Middle East and South America. 2 It is a leading cause of treatable non-malarial febrile illness and has a seroprevalence ranging from 9.3% to 27.9% with a median of 22.2% and a median mortality of 6.0% for untreated and 1.4% for treated Scrub typhus patients. 3
The cause of Scrub typhus is a bacterium called Orientia tsutsugamushi, which survives on a reservoir called the chigger mite, and these mites live in the Rattus genre of the rodent family. 4 The bacterium is transmitted to humans accidentally as zoonosis by the bite of the infected chigger mites.
In Bhutan, Chhukha district is endemic to Scrub typhus as per report of the Ministry of Health, Bhutan.5,6 There are no diagnostic facilities at Primary Health Centres (PHC) but Rapid Diagnostic Test (RDT) for Scrub typhus is available at the district hospitals in Bhutan. The reference test or Enzyme-Linked Immunosorbent Assay (ELISA) is available only at Royal Centre for Disease Control, Thimphu. There are reports of a delay in the recognition of Scrub typhus in August -October 2014 in a district in Bhutan, which resulted in two deaths due to complications of the disease. 7
We report a case of missed diagnosis of Scrub typhus, and the patient developed complications by the time she reached the district hospital but was diagnosed clinically and managed at the hospital despite a negative report of Scrub typhus on RDT. The purpose of reporting this case of Scrub typhus is to create awareness among health workers about this unattended or unnoticed disease. Its early recognition and prompt treatment prevented fatal complications. This case report highlights the challenges faced by health workers in resource-constrained facilities and the importance of clinical updates to the health workers on Scrub typhus.
What do we already know about this topic?
Scrub typhus is an acute febrile bacterial illness and a leading cause of treatable non-malarial fever with nonspecific presentation, which carries a median mortality of 6.0% for untreated and 1.4% for treated patients.
How does my research contribute to the field?
Health workers should suspect Scrub typhus as the cause for undiagnosed fever, body pain and headache in patients presenting during cardamom harvesting seasons in endemic area. They should search for eschar in the patient and manage as Scrub typhus if eschar is present when RDT is not available or the test report is negative for Scrub typhus.
What are my research implications towards theory, practice or policy?
The article highlights that health workers should be trained on clinical suspicion of Scrub typhus in patients who present with non-specific fever symptoms in the endemic area.
Case report
A 24-year-old female patient was referred from a local PHC to Gedu Hospital, Chhukha, Bhutan with 10 days duration history of fever, shortness of breath, cough and generalized body ache. The patient did not have any travel history outside her village. She had worked in her cardamom field 15 days ago. She was seen at the PHC on 14 October, 2022 for the same presentation. The prescription available with the patient showed the history taken and the treatment prescribed. There were no examination findings mentioned in the prescription. She was prescribed capsule Amoxicillin 500 mg 8 hourly for five days, tablet paracetamol 500 mg 8 hourly for 3 days, tablet vitamin C 250 mg 12 hourly for 5 days and injection diclofenac sodium 75 mg intramuscular one dose. The patient had visited the same PHC again on 18 October, 2022, was seen by the same health worker and then referred to Gedu Hospital. The patient then reached Gedu Hospital at 06.00 pm on 19 October, 2022.
On examination, the patient had a temperature of 100.6° Fahrenheit, blood pressure was 103/73 millimeters of mercury, pulse was 105 per min, respiratory rate was 28 per min and saturation of peripheral oxygen (SPO2) was 77% in room air. The patient was pale and jaundiced. Eschar was present on the left chest wall along the posterior axillary line at the level of seventh rib (Figure 1).
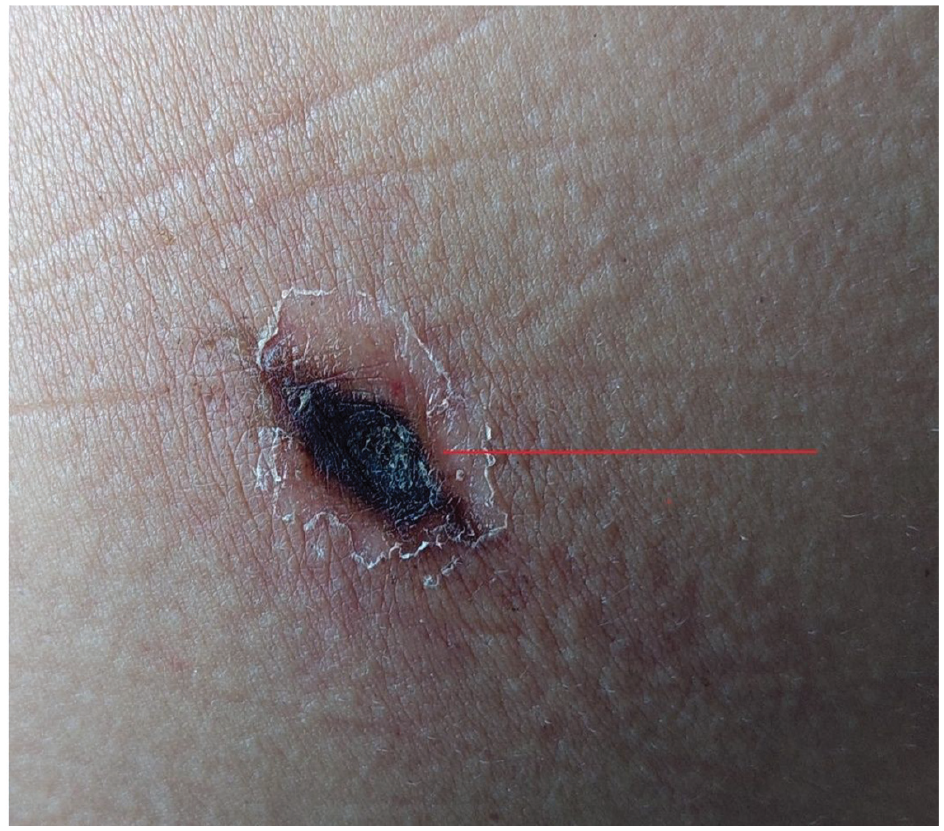
Presence of eschar on left chest wall along the left posterior axillary line at the level of seventh rib (red arrow) in a 24-year-old female patient who was managed as a complication of Scrub typhus.
The chest radiography showed bilateral basal pneumonitis (Figure 2).

Chest radiography of a 24-year-old female patient showing basal pneumonitis (red arrows) and managed as complication of Scrub typhus.
The initial blood investigation showed increased White Blood Cells (WBCs) count, low haemoglobin, low platelet counts and raised liver enzymes. The RDT report for Scrub typhus was negative. The patient was started on capsule doxycycline 200 mg first dose and then 100 mg12 hourly. Intravenous fluid resuscitation was given with Ringer’s lactate 1000 ml and Dextrose Normal Saline 500 ml. Tablet paracetamol 500 mg was given 6 hourly. Two follow up blood investigations were done (Table 1).
Blood investigation findings of a 24-year-old female patient who was managed as complication of Scrub typhus.

The patient had improved clinically from the second day of initiation of treatment and subsequent two blood investigations showed improved parameters.
The patient was managed with the same medicines and discharged on 26 October, 2022 without any complications.
Discussions
The diagnosis of Scrub typhus is difficult in the absence of knowledge on disease epidemiology, clinical features or in a facility without standard reference investigation. The acute onset of fever, joint pain and headache during August to October in Bhutan, with a history of working in Scrub vegetation and the availability of eschar, gives clues to the diagnosis even in the absence of a definitive diagnostic test. Tandin Zangpo et al. have stated from their studies that harvesting cardamom was the highest risk factor for Scrub typhus, which had a conditional OR of 1519.00 (95% CI 26.23–88005.98). 8 Cardamom is a short bushy plant that is grown in Bhutan in preferably shaded condition in moist soil on hilly terrains. 9 Cardamom harvest season extends from August to September in low and middle altitudes and October to November in high altitudes and this period coincides with Scrub typhus risk season. 10 Major risk factors for Scrub typhus occurred in China and Japan at hilly terrains and autumn period of harvest.11,12 Our patient presented in October with a history of acute onset of the symptoms and had a history of working in the cardamom field about 2 weeks prior to the onset of symptoms. We found an eschar which provided clue to our diagnosis. Eschar is a painless sore with a central necrosis appearing like cigarette burn mark surrounded by erythema and located mostly over the covered areas such as the groin, chest, genitalia, infra-mammary area and axilla. 13 Patient did not complain of the eschar, but it was found out when we searched for it.
We conducted RDT for Scrub typhus, but the report was negative, and we conducted other supportive tests: complete blood count and liver function test. The RDT kit available at our hospital had a sensitivity of 95.95% and this could be the reason for false negative report. This demanded caution while interpreting the report because the reference gold standard test or ELISA facility was not available at the hospital. Depending solely on the presence of an eschar as a diagnostic clinical sign may not consistently lead to the conclusive diagnosis of Scrub typhus because eschar has other differential diagnosis as well. 14 However, the history of working in a cardamom field 15 days prior to onset of illness, improvement in the clinical and laboratory findings following the treatment for Scrub typhus contributed to the clinical diagnosis of the patient. Further, Weil–Felix tests are also performed in resource-limited settings, but they are not available in the hospitals. Other supportive blood investigations in later stages of the disease show increased WBC count and decreased platelets and anemia. 15 Liver is affected at complication stage resulting in elevated liver enzymes manifesting as jaundice, encephalopathy, coma and death. 16 The respiratory complications include respiratory distress and interstitial pneumonitis in the chest X-ray. 17 Our patient had Leucocytosis, thrombocytopenia, anaemia, elevated liver enzymes and jaundice. She also had increased respiratory rate and a radiography of chest showed bilateral infiltrative changes of pneumonitis.
The standard treatment for Scrub typhus is capsule doxycycline with other symptomatic treatments. 18 We continued the same treatment because the clinical features started improving from the second day of initiation of the treatment. The follow up blood investigation conducted on the third day showed improved parameters as compared to the report of the first day. There was further improvement in the blood parameters on the fifth day of the treatment and same treatment was continued till discharge. Follow up radiography of chest was not done as the patient was improving and there was no clinical indication to repeat it. The final diagnosis of Scrub typhus was made based on the improved clinical features and laboratory reports with the treatment because further standard confirmatory tests were not available in the hospital.
This patient could have been managed as Scrub typhus at PHC during initial presentation if the patient was examined and looked for eschar. Examination of the patient could have found out eschar which could have contributed to the probable diagnosis of Scrub typhus and treated based on the clinical findings. There were no other morbidities associated with this patient during discharge on day 7 of admission except for the low haemoglobin for which 1 month of iron therapy was prescribed.
The follow up information about this patient after discharge from hospital is not available and this is the limitation in our case report.
Conclusion
Health workers in a diagnosis-constrained facility should be updated on clinical suspicion of Scrub typhus in patients coming from endemic area and presenting with unexplained fever, headache and body pain. Health workers should examine the patient, search for eschar and manage as Scrub typhus if eschar is present when RDT is not available or negative for Scrub typhus.
Footnotes
Acknowledgements
The authors thank the patient for giving them the consent to publish clinical information and photos without any identification.
Author contributions
T.N. designed the case report and drafted the article. S.D. reviewed the report and finalized the article.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical approval
Our institution does not require ethical approval for reporting individual cases.
Informed consent
Written informed consent was obtained from the patient for her anonymized information to be published in this article. This informed consent is available with the principal author.
