Abstract
Arthrogryposis multiplex congenita (AMC) is an uncommon condition present from birth that is marked by a combination of weakened muscles and multiple joint contractures. We present a case of a 2-year-old boy with AMC, who was born to consanguineous parents in Saudi Arabia. He presented with musculoskeletal abnormalities of all four limbs, including symmetric contractures in multiple joints of the body, bilateral developmental dysplasia of the hip, and vertical talus. Dysmorphic features included low-set ears, chin recession, triangular face, and nevus flammeus on the face. The child also had lactose intolerance, gastritis, inguinal hernia, and right-sided undescended testis. Surgical interventions were planned after a multidisciplinary team discussion. This case report highlights the good prognosis of AMC with all four-limb involvement and the importance of a thorough physical examination and a multidisciplinary approach to the diagnosis and management of AMC.
Keywords
Introduction
Arthrogryposis multiplex congenita (AMC) is a rare congenital disorder characterized by joint contractures and muscle weakness. The condition can manifest in various ways, and the severity and number of affected joints can vary widely. The etiology of AMC is not fully understood, but several factors, including genetic and environmental factors, have been implicated in its development. 1 The severity of AMC can vary greatly, and treatment options are often limited. 2 In this case report, we describe a 2-year-old patient with AMC who presented with vomiting after breastfeeding, musculoskeletal abnormalities of all four limbs, and dysmorphic features, including low-set ears, chin recession, and triangular face with nevus flammeus. The patient was born to a consanguineous family who did not have any family history of AMC. At birth, he had a history of noisy breathing and difficulty swallowing due to a high-arched palate, for which he received nutrition via an NG tube and IV fluids to hydrate. The patient’s physical examination revealed bilateral developmental dysplasia of the hip (DDH), symmetric contractures in multiple joints of the body, and other dysmorphic features. Laboratory investigations revealed some abnormalities, including decreased white blood cells and monocytes and increased red blood cells in the complete blood count. The patient received appropriate surgical interventions to manage their AMC. The multidisciplinary team provided ongoing care and support to optimize the patient’s physical abilities and overall health. This case report highlights the importance of early diagnosis, appropriate interventions, and multidisciplinary care in managing AMC and improving patients’ quality of life. 3
Case presentation
A 2-year-old son was presented by a 29-year-old P1 + 2 mother in a tertiary care hospital in Pakistan with complaints of vomiting after breastfeeding. On general physical examination, the patient had musculoskeletal abnormalities, including symmetric congenital, rigid contractures in multiple joints, particularly in the knee, elbow, and neck. He had dysmorphic features, including low-set ears, chin recession, and a triangular face. In addition, the patient had an internal rotation of the shoulder, fixed extension of the elbows, and pronation of the forearm, flexion of the wrist. There was severe equinovarus deformity of the foot and shortness of affected limbs (5%–10%), along with the marked decrease in limb muscle mass. Based on the findings, the patient was diagnosed with AMC, a rare congenital disorder characterized by joint contractures and muscle weakness.
The patient was born to a consanguineous family in 2018, with an APGAR score 4 of 8 at 1 min. The patient had noisy breathing and difficulty swallowing due to a high-arched palate and received nutrition via an NG tube and IV fluids to hydrate. Details revealed that the patient’s mother had a history of polycystic ovarian syndrome and hypothyroidism in the past, for which she received appropriate treatment. The patient’s mother also had a history of two previous miscarriages; however, there was no family history of a child with arthrogryposis. Proper testing is also required to check for the possibility of AMC manifesting as a heritage syndrome.
Prenatal ultrasound at 32nd week revealed the following: a fundal height of 28 cm, a normal biparietal diameter, and a head circumference. The abdominal circumference was 24.5 cm, which was at the 2.5th percentile. Estimated fetal weight was 1465 g (3 lb., 4 oz), which placed the infant in the 3rd percentile. The amniotic fluid index was 6.0 cm (less than the 2.5th percentile), confirming the diagnosis of IUGR. Whole-genome sequencing was advised but not carried out due to the unavailability of the test in the country and higher testing costs abroad (i.e., Canada).
The patient’s physical examination revealed bilateral DDH, which was clinically diagnosed immediately after birth. The patient had musculoskeletal abnormalities, including contractures in multiple joints, particularly in the knee, elbow, and neck (Figure 1).

Physical examination of the patient.
The patient was not able to flex his knees, and his hand could not open completely. The bilateral thumb was clenched and adducted, while other contractures were found in the elbow and neck. Dysmorphic features included low-set ears, chin recession, triangular face, multiple birthmarks on the face, a dark brown patch between hips and anus, and a red eye patch on the left eye (Figure 2).

Red patch on the left eye.
The patient had an inguinal hernia and a right-sided undescended testis on ultrasound.
Laboratory investigations revealed decreased white blood cells and monocytes and increased red blood cells in the complete blood count. Blood chemistry showed increased neonatal and unconjugated bilirubin levels (13.51 mg/dl). A thyroid-stimulating hormone of 0.177 mIU/ml (normal = 0.35–4.50 mIU/mL) and a free T4 of 29.8 μg/dL (normal = 5.0–12.0 μg/dL) were observed. Blood, urine, and rectal swab culture, newborn biochemical screening for 17 OH progesterone, galactose 1 phosphate uridyltransferase activity, biotinidase activity, free carnitine, acylcarnitine, creatinine, and amino acids were unremarkable.
The patient received treatment for vomiting after breastfeeding, including the provision of lactose-free formula. The patient’s inguinal hernia and right-sided undescended testis were planned to be treated with appropriate surgeries. In addition to physiotherapy and occupational therapy, surgical interventions were also utilized to manage the patient’s AMC. The orthopedic surgeon on the multidisciplinary team performed surgery to release the joint contractures and improve the patient’s range of motion. The patient was closely followed up after the surgery to monitor their progress and ensure proper healing (Figure 3).
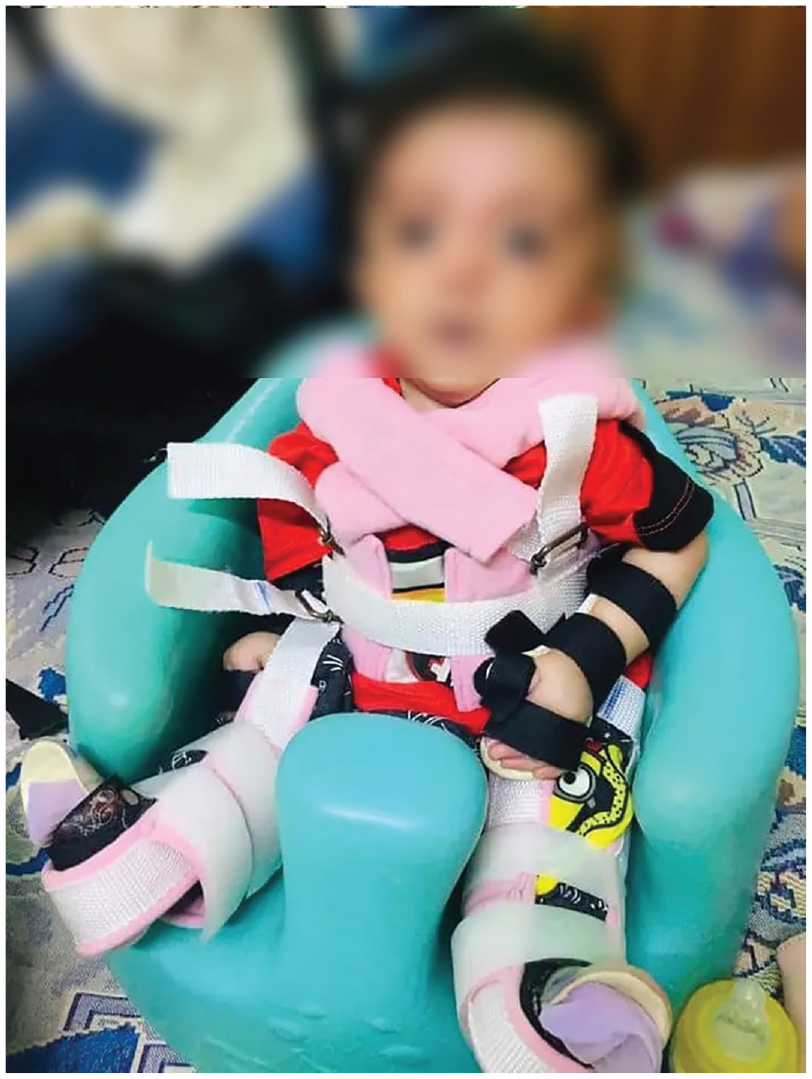
Postsurgical appearance of the patient.
The multidisciplinary team continued to provide ongoing care and support to the patient to optimize their physical abilities and overall health. Regular assessments and check-ins were conducted to monitor the patient’s growth and development, including their motor milestones and cognitive function. With the help of the multidisciplinary team and appropriate interventions, the patient was able to make significant progress in managing their condition and improving their quality of life.
Discussion
AMC is a developmental condition characterized by multiple joint contractures that result in substantial functional limitations in many areas of routine life activities. 3 There are two categories of AMC: the initial one involves arthrogryposis as an accompanying indicator in various illnesses, predominantly neuromuscular diseases; in contrast, the second group has arthrogryposis as the primary and unchanging feature. 5 Subdivision of AMC includes amyoplasia, distal arthrogryposis, and pterygium syndrome. One article mentions the genetic involvement of TNNI2 and TPM2 in type 1 distal arthrogryposis transmission. 6
Amyoplasia is the most common subtype of AMC. The most comprehensive symptoms of AMC include constrained movement around multiple joints leading to contractures, hypoplastic muscles, soft doughy tube-like limbs, and muscle mass discrepancy around joints.3,7 Type amyoplasia is also associated with stork marks on the face, and 10% of individuals have gastroschisis. 3 The affected patient in our case report met the general diagnostic criteria of type Amyoplasia. 8 Most of the cases reported for Amyoplasia have a sporadic origin that lacks genetic linkage and recurrence 8 but consangious relationship of the parent in our case highlights that amyoplasia should be considered a heritage syndrome and should be investigated for genetic method.
Approximately 25% of patients with AMC may have intellectual difficulty and central nervous system (CNS) involvement according to previous research, and it is thought to be lethal in the neonatal period.9,10 In our case, the CNS was intact, and any deficit in intelligence was unremarkable.
The diagnosis of AMC can be challenging, as 75% of cases remain undiagnosed prenatally, 11 and a few modalities have been described by Niles et al. in their exceedingly detailed work. Prenatal diagnostic modalities include high-quality ultrasound, fetal MRI, whole-exome/genome sequencing, trimester-wise ultrasound surveillance, biophysical profile, and 2D or 3D ultrasound for fetal lung volume estimation autopsy partial autopsy, and molecular autopsy may be performed in cases of Intra Uterine Death or if parents decide to cease the pregnancy. 12
While prenatal ultrasound findings such as nuchal translucency and cystic hygroma in the first trimester and prominent joint contracture in the 2nd trimester are diagnostic clues, 13 this is not always the case. Clinical findings in an AMC infant may include characteristic facial features, such as whistling face syndrome and visible limb contractures. Vascular birthmarks along the midface are frequently observed; however, the intelligence in these individuals is normal. 14 Electromyography is performed to demonstrate reduced motor units without fasciculations, and muscle biopsy shows fibrosis or replacement with fatty tissue. 14
The management of AMC involves a multidisciplinary team and may include both surgical and nonsurgical interventions. Early aggressive management and consistent treatment can lead to positive outcomes for patients with AMC. A symptomatic and systematic approach mixed with physiotherapy, occupational therapy, and multiple surgeries guarantees a better outcome. 3
Aggressive physical therapy, joint manipulation, stretching exercises, removable splints, and serial casting are all helpful in treating AMC. 3 Early aggressive management can result in the ability to walk and perform daily activities, and a high success ratio in the ability to walk and perform daily activities after rehabilitation and orthopedic intervention has been reported.6,15
Upper limb management aims to enable the child to perform daily activities independently, such as feeding, toileting, and being able to mobilize using crutches and a wheelchair. 15 Specific interventions for shoulder, elbow, and wrist contractures are necessary. 16
The general health of a child with AMC is also important since physical aspects of AMC portray a greater risk of weakening immune function, thus acquiring infections, weight gain, and failure to grow. Feeding problems, reported in a few infants with structural abnormalities in the tongue and jaw, were addressed with initial tube feeding and speech and physiotherapist appointments later. 2
Conclusion
In conclusion, AMC is a complex developmental condition that affects multiple joints, resulting in functional limitations in various areas of daily life. It is important to recognize the different subtypes of AMC and their associated symptoms to ensure appropriate diagnosis and management. While the prenatal diagnosis of AMC can be challenging, a multidisciplinary approach involving a team of medical professionals can help manage and improve outcomes for affected individuals. Early intervention with physical therapy and surgical and nonsurgical interventions can lead to significant improvement in functional abilities and independence. Regular monitoring and management of associated medical conditions, such as feeding difficulties and immune system weakness, are also important to ensure the overall health of individuals with AMC. Further research and understanding of the genetic and molecular mechanisms underlying AMC may lead to more targeted and effective treatments in the future.
Footnotes
Acknowledgements
Not applicable.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethics approval
Our institution does not require ethical approval for reporting individual cases or case series.
Informed consent
Written informed consent was obtained from a legally authorized representative (parent) for anonymized patient information to be published in this article.
