Abstract
Non-ossifying fibromas usually occur in the metaphysis of the long bones in children, and are extremely rare in the mandible. Here, we present a case of non-ossifying fibromas which occurred in the mandible of a 4-year-old boy. The patient had no complaint of ache. Laboratory blood examination of serum calcium, phosphorus, and parathormone levels was normal. Computed tomography of the maxillofacial region showed a well-defined osteolytic lesion affecting the right mandible. Microscopically, the lesion showed whorled bundles of spindle-shaped fibroblasts, as well as foam cells, mingled with scant multinucleated giant cells, without any bone formation. It is necessary to distinguish non-ossifying fibromas from other giant cell-containing lesions because of the extremely infrequent occurrence of this lesion in the mandible. We reviewed the histologic features of 14 cases of non-ossifying fibromas involved in the jaw.
Introduction
Non-ossifying fibromas (NOFs), which are considered a phenomenon of metaphyseal remodeling during skeletal growth, 1 are nonneoplastic lesions that occur commonly in the metaphysis of the long bones in children and are extremely rare in other areas of the skeleton. 2 NOF was first described by Jaffe and Lichtenstein 3 in 1942. It has been estimated that approximately 30%–40% of children have one or more occult NOFs. Radiographic studies have shown that 54% of boys and 22% of girls have NOF at the age of 4 years. 4 The natural history is gradual reossification as the child enters the second and third decades of life. 1
The first use of the term ‘non-ossifying fibroma’ to describe a lesion of the mandible was made in 1980. 5 Here, we present a case of NOF that occurred in the mandible of a 4-year-old boy with a brief literature review.
Case report
A 4-year-old boy presented with non-tender mass near the right lower molars. This had been incidentally noted by the kid’s parents. The patient had no complaint of ache to the area. He was subsequently admitted to our hospital for further check. Laboratory blood examination of serum calcium, phosphorus, and parathormone levels was normal.
On physical examination, a smooth and non-tender mass was palpated in the right lower molars. The oral cavity checkup was not exceptional.
Computed tomography of the maxillofacial region showed a well-defined 25 mm × 16 mm osteolytic lesion affecting the right mandible; erosion of the cortex was present (Figure 1). The lesion was delicately excised using a piezosurgery and sent for frozen section that showed spindle cell, chronic inflammation, and macrophages. The gross specimen of the lesion showed whorled bundles of spindle-shaped fibroblasts (Figure 2), as well as foam cells, mingled with scant multinucleated giant cells, without any bone formation in the lesion. The lesion showed strongly and diffusely positive staining for SATB2 (Special AT-rich sequence binding protein 2) (Figure 3), focal positive for SMA (Anti-smooth muscle antibody), KP1 (Anti-CD 68 antibody), and ER (Estrogen Receptor) (Figure 4), and negative for H3.3G34W by immunohistochemistry. With respect to USP6 (Ubiquitin-specific proteases) break-apart fluorescence in situ hybridization, the result was negative (Figure 5). Whole exon sequencing for this lesion tested KRAS codon 12, codon 13, codon 61, and codon 146, which were all negative. The postoperative course was uneventful, the patient was followed for 15 months and continues to be asymptomatic.

Computed tomography of the maxillofacial region showed a well-defined 25 mm × 16 mm osteolytic lesion involving the right mandible.
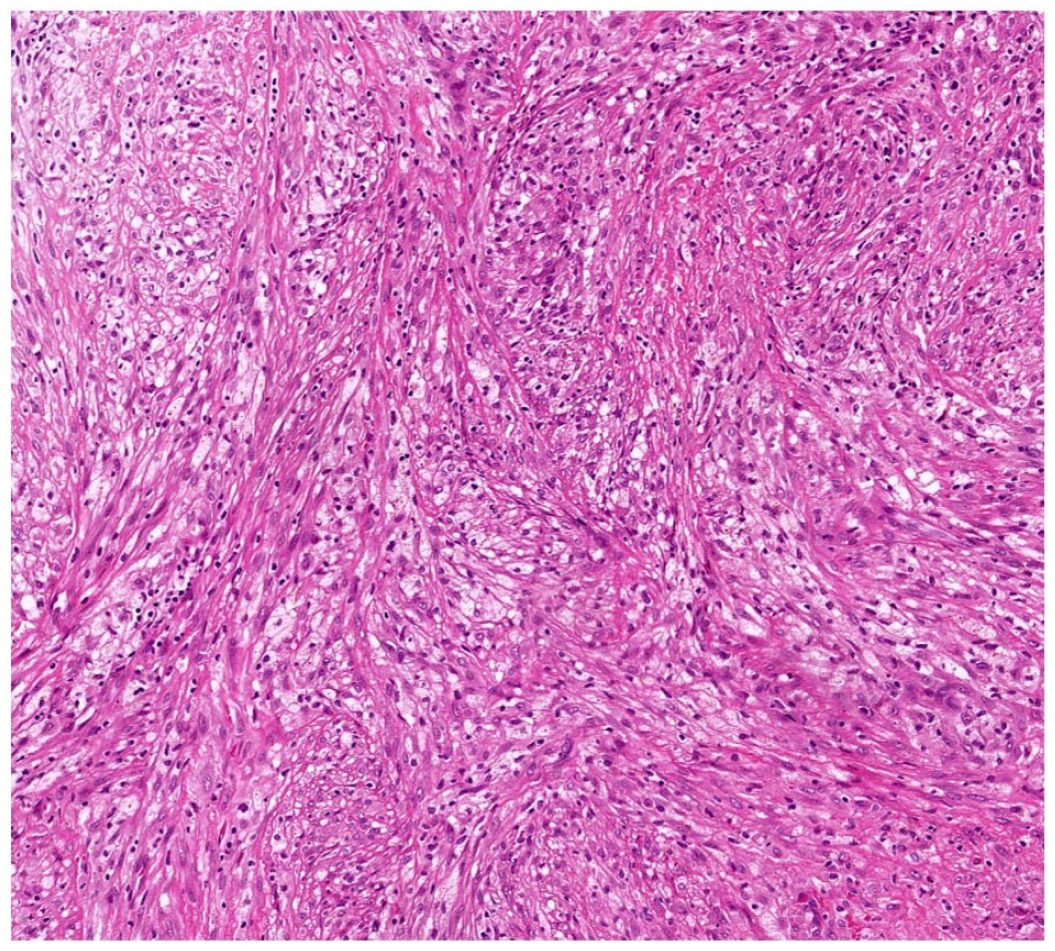
Gross specimen showed bundles of spindle-shaped fibroblasts as well as foam cells (hematoxylin and eosin, ×100).

Strongly and diffusely positive staining for SATB2 by immunohistochemistry (Envison, ×200).

ER expressed in the NOF (Envision, ×400).
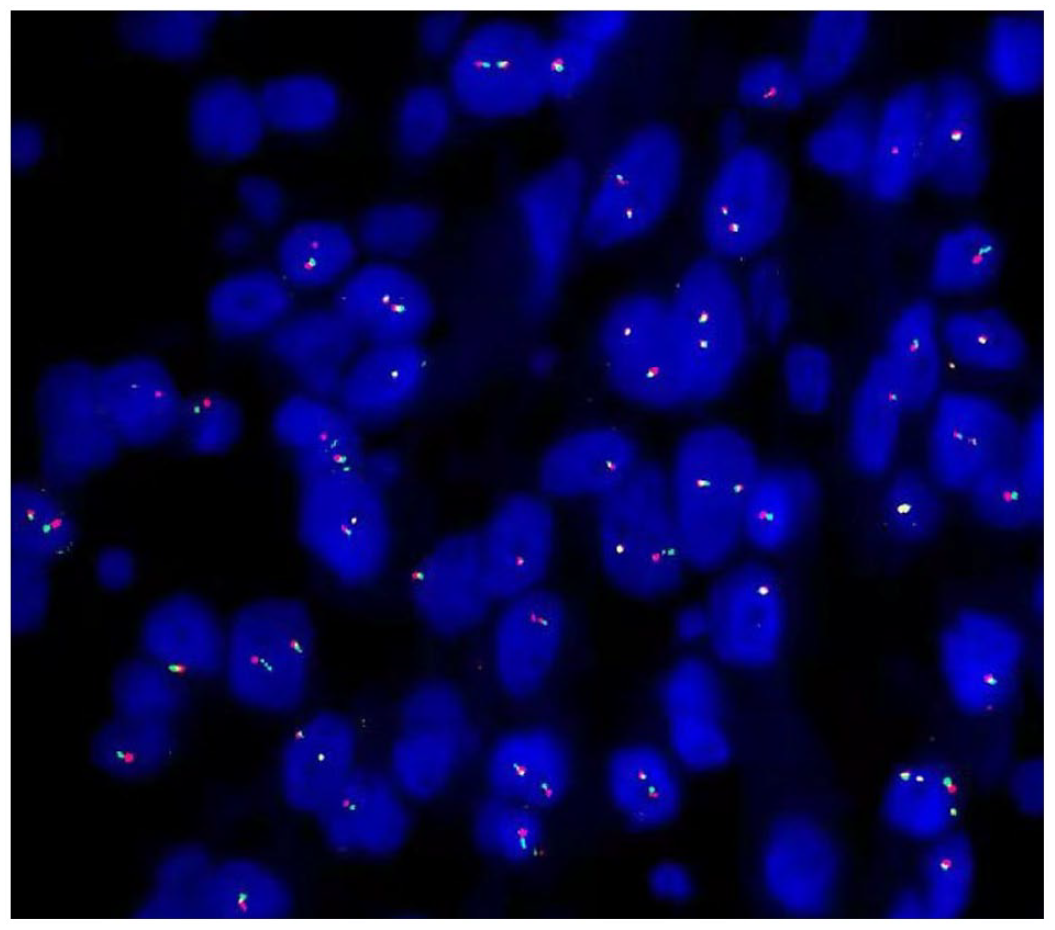
USP6 break-apart fluorescence in situ hybridization.
Discussion
NOF are benign and generally self-limiting spindle cell tumor in the metaphysis of the long bones in children. Asymptomatic lesions do not require biopsy confirmation in cases with a typical radiographic appearance. In the mandible, because of the extremely infrequent occurrence of these lesions, this diagnosis generally is challenging. Most mandibular lesions are small and asymptomatic. 6
The differential diagnosis is difficult, since it must include most odontogenic and non-odontogenic lesions of the mandible. Radiological differential diagnosis of NOF includes cemento-ossifying fibroma, 7 odontogenic keratocyst, or ameloblastoma.
Histologically, It is necessary to distinguish NOF from other giant cell-containing lesions, including giant cell lesions of the jaws (GCLJ), the bone giant cell tumor, aneurysmal bone cysts, or the brown tumor of the jaws.
NOFs appear to be related to GCLJ in histological alteration. While Slootweg 8 noted that NOF is more common in immature individuals with whorled, storiform, spindle-shaped fibroblasts and foam cells, bone formation was nearly absent in NOF. It seems reasonable to consider GCLJ and NOF as different entities. KRAS mutations are the most frequently identified genetic alteration. Our whole exon sequencing for this lesion tested codon 12, codon 13, codon 61 and codon 146, which were all negative.
The bone giant cell tumor is a locally aggressive tumor, the immunohistochemistry of the H3.3G34W mutant is a highly sensitive and specific surrogate marker for differential diagnoses of histological mimics, 9 which in our case is negative.
Fluorescence in situ hybridization for USP6 break-apart is a useful technique in distinguishing primary aneurysmal bone cysts from giant cell-rich lesions and other morphologically similar lesions. 10 Our case does not share this rearrangement.
The brown tumor of the jaws is a manifestation of hyperparathyroidism. The diagnosis of brown tumor requires laboratory tests, histopathological features, and radiographic examination of other bones as well. 11 Laboratory blood tests for serum calcium, phosphorus, alkaline phosphatase, and parathormone levels in our case were normal.
According the recent research by Cleven et al., 12 positive ER expression finding could favor the diagnosis of NOF above other giant cell-containing bone lesions. Our case also showed the expression of ER which was consistent with the research. Increased endocrine regulation by estrogen signaling through the ER alpha receptor during puberty can involve spontaneous regression of NOFs.
A review of the literature from 1980 to the present revealed 14 NOFs of the jaws with detailed histologic features.2,5–6,13–21 Eight of the 10 patients were female. The average age at diagnosis was 14 years and 6 months. Our review of the reported cases demonstrated the histologic features in the following aspects: (1) whorled bundles of spindle-shaped fibroblasts; (2) variable presence of foam cells and multinucleated giant cells; and (3) lack of bone production within the lesion. The clinical behavior appears to be that of a benign lesion with no reports of recurrence, 19 All cases have been successfully treated by curettage or resection with no reports of recurrence (see Table 1).
Reported cases of mandible NOF: histologic features.

LTF: lost to follow-up; NOF: non-ossifying fibroma.
Duration of follow-up (months) after NOF diagnosis is given in parentheses.
Conclusion
NOF are nonneoplastic lesions that occur commonly in the metaphysis of the long bones in children. In the mandible, this diagnosis is challenging due to the rare occurrence. Histologically, NOF showed whorled bundles of spindle-shaped fibroblasts with variable presence of foam cells and multinucleated giant cells, but lack of bone production within the lesion. More studies are necessary to establish the role of the pathogenesis of the lesion.
Footnotes
Acknowledgements
The authors would like to thank the patient’s parents for permission to share the medical history for educational purposes and publication.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethics approval
Ethical approval to report this case was obtained from The Ethics Committee of Zhuhai People’s Hospital Review Board (No. LW-(2022)No. 8). We have identified the patient details. Our institution’s committee on human research gave approval for this study.
Informed consent
Written informed consent was obtained from a legally authorized representative for publication of this case report.
Patient consent statement
Our institution’s committee on human research gave approval for this study, and written informed consent was obtained from a legally authorized representative for publication of this case report.
