Abstract
Unilateral proptosis is an abnormality in which one eye sticks out forward more than the other. Bulging of the eye is commonly seen in Graves’ ophthalmopathy, but it’s mostly bilateral. Thyroid eye disease presents as the most common extrathyroidal manifestation of Graves’ disease, and rarely leads to unilateral proptosis. A 25-year-old female with a history of weight loss, menstrual irregularities, and palpitations presented with progressive right eye bulging, which was further confirmed by magnetic resonance imaging and biochemical investigations. Magnetic resonance imaging of the orbit revealed unilateral extraocular muscle enlargement and enhancement with sparing of the tendons. Timely therapy is crucial for reversing the ocular manifestations of thyroid eye disease.
Introduction
The most common extrathyroidal manifestation of Graves’ disease (GD) is thyroid eye disease (TED) 1 observed in 25–50% of the Graves’ patients. A total of 75% of the patients with thyrotoxicosis develop Graves’ ophthalmopathy (GO) within a year of diagnosis. 2 TED is an autoimmune disorder that can cause a rise in retrobulbar pressure and proptosis due to inflammation, swelling, and fibrosis of the extraocular muscle (EOM). It is caused by thyroid-stimulating immunoglobulins targeting the thyroid stimulating hormone receptor (TSH-R), which can activate it and contribute to the development of TED. 3 In the majority of patients, both eyes are equally affected, although often in an asymmetric manner. 1 Unlike bilateral proptosis, which is mostly seen in thyroid disease, unilateral proptosis has a great variety of differential diagnoses, including orbital pseudotumor, orbital cellulitis, cavernous sinus thrombosis, or intra-orbital neoplasms. 4 Unilateral ophthalmopathy mostly progresses to bilateral disease, while only 5–11% of cases show no progression, making pure unilateral ophthalmopathy rare. 1 Here, we present the case of a young female with GD who developed unilateral proptosis without any visual disturbances.
Case presentation
A 25-year-old female presented to the outpatient department with a history of weight loss, menstrual irregularities, and occasional palpitations for 2 months. She had no history of night sweats, fever, chest pain, cough, or shortness of breath. She complained of bulging of her right eye, which was insidious in onset and gradually progressive without any difficulty in vision. There was no history of pain, discharge, redness, or trauma associated with her condition. She had no remarkable prior medical history nor any history of allergies to medication or other substances. She was a nonsmoker but consumed alcohol occasionally.
At the time of her presentation to the hospital, she had a blood pressure of 130/80 mmHg, oxygen saturation of 97% on room air, and a pulse rate of 125 beats/min. On ocular examination, her EOM movements were normal. The visual acuity was 6/6 in both eyes, with a clinical severity score of 3/7, Hertel’s exophthalmometry of 23 mm in the right eye and 21 mm in the left eye. Laboratory investigations revealed a hemoglobin level of 13.6 g/dL and a white blood cell count of 7400/mm3 with 57% neutrophils, 39% lymphocytes, and 3% monocytes. The free T3 level was 10.12 pmol/L (reference range: 3.10–6.80), free T4 level was 25.88 pmol/L (reference range: 12.0–22.0), TSH was 0.006 mIU/L (reference range: 0.27–4.20), and TSH receptor antibody (TRAb) was 3.56 IU/L (>1.75 (96% sensitivity and 99% specificity for GD)). The liver and renal function tests were within normal limits. Magnetic resonance imaging (MRI) of the orbit revealed unilateral EOM enlargement and enhancement with tendon sparing and relative right proptosis (Figure 1).

(a) Orbital axial and (b) orbital coronal; post-contrast MRI showing unilateral EOM enlargement and enhancement with tendon sparing and relative right proptosis.
She was diagnosed with GD with GO and started on methimazole 5 mg twice daily with intravenous methylprednisolone 500 mg once weekly for 6 weeks, followed by 250 mg once weekly for 6 weeks for a total duration of 12 weeks. On follow-up after 3 months, she responded well to the medication, leading to the resolution of her eye symptoms.
Discussion
Our patient presents with proptosis, weight loss, menstrual irregularities, and palpitations, which are commonly seen in GD. However, our patients present with unilateral proptosis without any visual disturbances, and this is rare.
GD is an autoimmune disorder that is more frequent between 20 and 50 years of age and occurs in 2% of women.4,5 The annual incidence of GO is 16 per 100,000 women. 2 The symptoms of GO include a dry, gritty feeling in the eyes, photophobia, excessive tearing, double vision, and pressure feeling behind the eyes, as reported by nearly half of the patients of Graves’ hyperthyroidism. 6 The most typical symptoms of GO are proptosis, ophthalmoplegia, orbital congestion, eyelid edema, eyelid erythema, conjunctival chemosis, difficulty moving eyes, eyelid retraction, and less frequently, compression of the optic nerve. 5 Proptosis can cause corneal exposure and injury in severe cases, especially if the lids fail to shut during sleep, and in most cases, there is subclinical involvement of the eyes. 6
The most widely accepted cause of Graves’ orbitopathy is the formation of autoantibodies against thyrotropin receptors located in both the thyroid gland and the orbit. This activates T cells, resulting in the release of inflammatory mediators. 7 Inflammatory cells and hyaluronans infiltrate the muscle, causing enlargement of the EOMs, an increase in the orbital fat volume, and ultimately, collagen deposition leading to fibrosis. 8 The disease often progresses via two distinct phases: an active, inflammatory phase followed by a static, non-inflammatory phase with fibrosis. 3
The risk factors for TED as smoking, older age, extreme physical or psychological stress, prior treatment with radioactive iodine, and increased titers of antithyroid-stimulating hormone receptor antibodies are well described in published literature. 9 However, unilateral proptosis can be attributed to several factors, such as an asymmetrical distribution of antigens, anatomical variations in blood flow or lymphatic drainage, the elasticity of orbital septa, or other localized conditions. Infections or differences in the ability to generate adipose tissue can be a potential trigger for unilateral proptosis. 10
The onset of symptoms and unilateral proptosis involves a variety of alternate diagnoses including inflammatory, neoplastic, infectious, vascular, or neuromuscular conditions. 11 Orbital cellulitis is an acute condition that progresses rapidly. Orbital cellulitis mimics GO most frequently but may have a subacute onset over days or weeks, may be associated with pain, and involve any EOM, including the tendons, on MRI of the orbit. 11 The appearance of the extraocular eye muscles in MRI aids in differentiating TED from other conditions such as lymphoma and idiopathic orbital inflammation where the tendons are involved. 9 Neoplastic involvement was a consideration in our patient as it may present as a painless, restrictive eye involvement and occurs gradually over weeks or months, with or without a mass effect. 11 Lymphomas account for more than 50% of malignant orbital tumors in people 60 years and older, making them the most prevalent primary orbital tumors. 11
Computerized tomography (CT) of the orbit, MRI, and TRAb help diagnose GO. Orbital imaging is indicated in a patient with GO, particularly in a patient with unilateral proptosis. 5 In our patient, TRAb was positive with a rise in serum-free T3 and free T4 levels and a fall in TSH, suggesting GO and the high level of antithyroid peroxidase, which may indicate transient hyperthyroidism due to Hashitoxicosis. 12 The TRAb and insulin-like growth factor 1 receptor antibodies could have contributed to the pathogenesis of infiltrative ophthalmopathy. 2
Corticosteroids are usually used in the treatment of GO due to their anti-inflammatory and immunosuppressive properties. 13 Methimazole is an antithyroid medication for GD but does not directly affect extrathyroidal manifestations like GO. Our patient improved with combined therapy of corticosteroids and antithyroid medications.
Reported cases of unilateral proptosis in GO are shown in Table 1. Among the reported cases, four of them were euthyroid GD and two were hyperthyroid GD with subsequent eye symptoms. Our case reveals unilateral proptosis in hyperthyroid GD with no eye symptoms.
Reported cases of unilateral proptosis in GO.
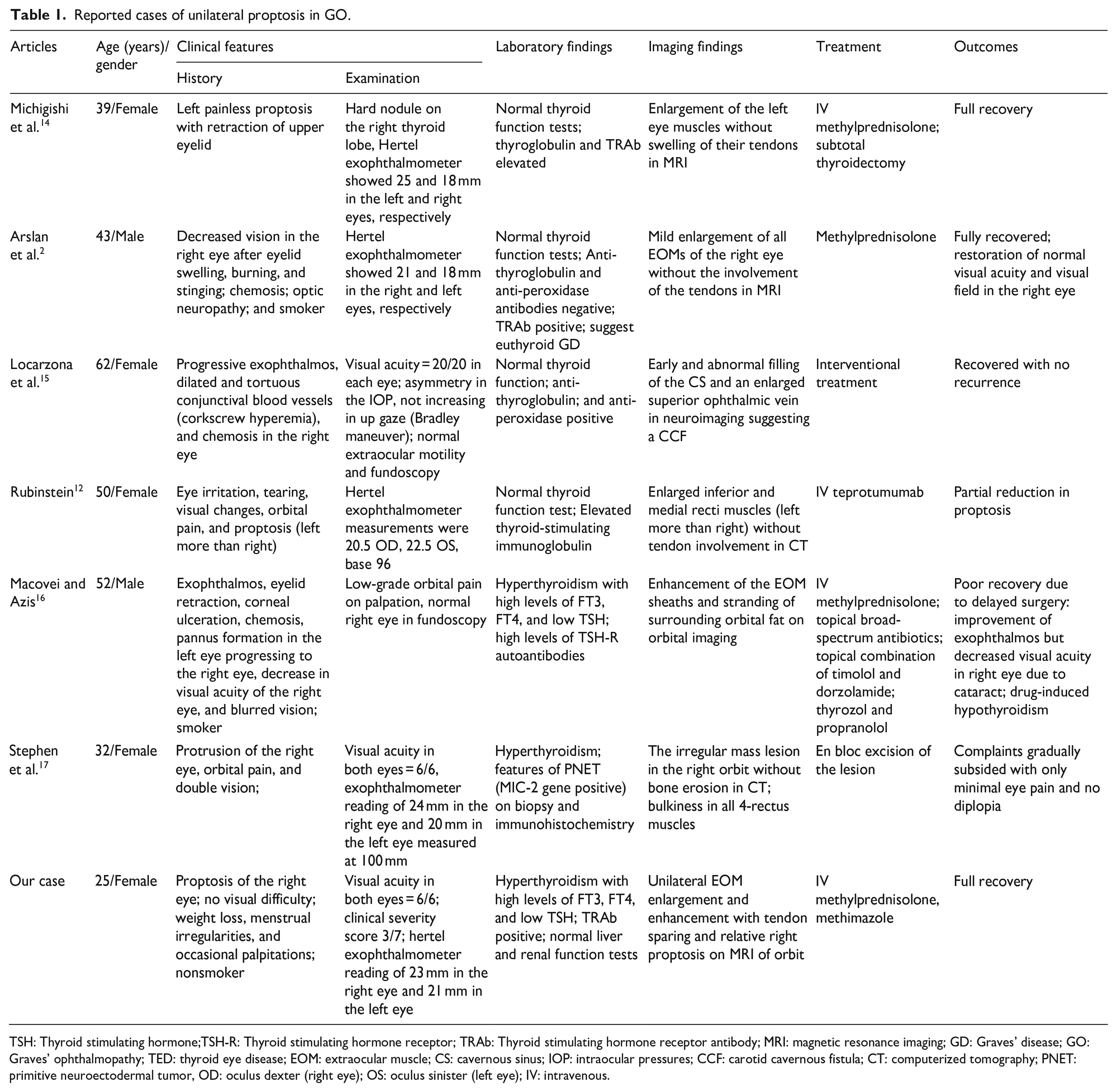
TSH: Thyroid stimulating hormone;TSH-R: Thyroid stimulating hormone receptor; TRAb: Thyroid stimulating hormone receptor antibody; MRI: magnetic resonance imaging; GD: Graves’ disease; GO: Graves’ ophthalmopathy; TED: thyroid eye disease; EOM: extraocular muscle; CS: cavernous sinus; IOP: intraocular pressures; CCF: carotid cavernous fistula; CT: computerized tomography; PNET: primitive neuroectodermal tumor, OD: oculus dexter (right eye); OS: oculus sinister (left eye); IV: intravenous.
Conclusion
This clinical case is a diagnostic challenge because the true unilateral disease is rare, and bilateral asymmetric eye involvement is seen in GO. Numerous differential diagnoses should be considered and studied before diagnosing this uncommon entity, even though noticeable unilateral proptosis supports the atypical presentation of GO in GD. The patient’s response to treatment medications suggests that timely therapy is crucial for reversing the ocular manifestation of TED.
Footnotes
Acknowledgements
The authors do not have any acknowledgment to report for this article.
Author contributions
H.B.B., I.T., and S.D. wrote, reviewed, and edited the original article. P.B.S., M.B., B.P., S.K., S.L., S.G., and B.B. reviewed and edited the original article.
Declaration of conflicting interests
The author(s) declare no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical approval
Our institution does not require ethical approval for reporting individual cases or case series.
Informed consent
Written informed consent was obtained from the patient for the anonymized information to be published in this article.
