Abstract
Hydatid cyst is a zoonotic parasitic disease with a global prevalence, especially in the Mediterranean region. We encountered a 37-year-old woman referred to the emergency department complaining of severe abdominal pain and spotting. After the emergency ultrasound, she underwent laparotomy with the diagnosis of missed ovarian torsion and was diagnosed as a hydatid cyst. We were prompted to report this case regarding the rarity of this cyst and its presentation.
Keywords
Introduction
Hydatid cyst is most frequently caused by Echinococcus granulosus. 1 This zoonotic parasitic disease has spread globally, especially in the Mediterranean region, including Iran. 1 The World Health Organization (WHO) has described this cyst as a neglected disease. 2 Hydatid cysts are rarely seen in the female reproductive system. 3 In 80% of involved genital tracts, the ovary and uterus are the most commonly affected organs. 4 In this regard, pelvic hydatid cysts are usually caused by the rupture of cysts in other areas of the abdomen, primarily the liver. 5 Most patients are asymptomatic, but as the cyst grows in the pelvic cavity, various symptoms occur due to the compressive effect of the cyst on nearby organs. 6 This article reports a rare pelvic hydatid cyst mimicking an ovarian torsion. This report aims to add to the literature a unique description of a rare pelvic hydatid cyst, which could be mistakenly diagnosed and treated.
Case report
Our case report is a 37-year-old woman referred to the emergency department complaining of severe abdominal pain and spotting from 2 months ago in Parsaabad, Ardabil. She reported generalized pain in the entire abdomen without obvious tenderness or rebound tenderness with no nausea, organomegaly, or a history of gynecological problems. The vital signs of the patient were stable. In a transvaginal ultrasound, the right ovary with dimensions of 78 × 45 × 33 mm and a volume of 125 cc (larger than normal) was reported with heterogeneous echo. However, the left ovary was normal. Doppler showed no arterial or venous vascularity in the right ovary. Ultrasound images suggested the probability of ovarian torsion. Abdominal and pelvic ultrasonography reported a spherical hypoechoic lesion with calcification of 30 × 30 mm in segment VII, right lobe of the liver, suggesting a silent hydatid cyst. Several calcified granulomas with a maximum diameter of 5 mm were evident in the right lobe of the liver.
The patient had a history of spotting from 2 months ago and a history of hydatid cyst surgery 6 years ago. Due to these characteristics and severe abdominal pain, she was sent to the center of the province (Alavi Hospital in Ardabil). After the emergency ultrasound, she underwent laparotomy with the diagnosis of missed ovarian torsion. Laparotomy revealed a 9 × 8 cm2 mass in the posterior cul-de-sac area behind the uterus, which had a soft consistency on examination (Figure 1). Therefore, oncology and emergency surgery consultation was performed. The vesicles appeared by cutting on the mass, and the hydatid cyst was considered according to the appearance of the mass during surgery and the patient’s history. The cyst was drained, its wall was completely removed, and the sample was sent to the pathology.
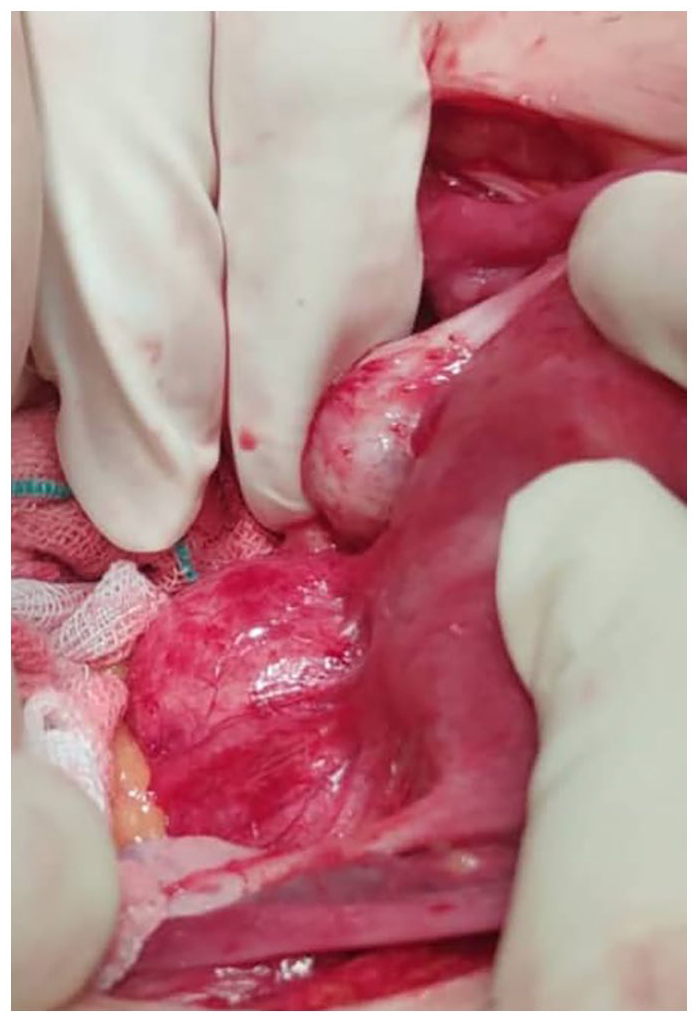
Pelvic hydatid cyst.
The pathology report indicated that:
(a) Sections showed cyst wall structures with a marked fibrotic layer in the inner parts and surrounded by smooth muscle fibers in the outer layer in some areas. Chronic inflammatory cells were infiltrated mostly in the inner parts of the cyst and were associated with foreign body type reactions.
(b) Microscopic examination showed a chitin-liked, acellular, laminated cyst wall associated with necrotic material. The lesion staging was stage IIb (Figure 2).

The pathology report figure.
Discussion
Hydatid disease is commonly caused by Echinococcus granulosus and is endemic in several countries, including Iran.1,7 The main host and most common source of this infection are dogs, which can incidentally transmit the parasite to humans. 8
The patient was a young woman with no underlying disease. The only known risk factor for this patient was living in rural areas, having contact with dogs, and having a history of hydatid cyst surgery 6 years ago. Symptoms are usually absent. Also, in many cases, the infection is accidentally detected on imaging for other reasons. Symptoms will develop in a confined space due to the compressive effect of the growing cyst.
Tarafdari et al. 9 reported a case of a hydatid cyst that underwent laparotomy with malignant ultrasound features but was diagnosed as a hydatid cyst. However, unlike our case, it was a primary cyst as no other lesions were detected at the time.
Mohammed et al. 10 reported an 18-year-old woman who had complained of abdominal pain and frequent urination in the past 3 months. Abdominal ultrasound showed left adnexal cystic lesions, while laparoscopy showed left ovarian hydatid cyst.
The literature review shows only a few cases of primary involvement of female pelvic organs. Such cases are commonly diagnosed as para-ovarian cysts and are most often diagnosed during surgery. 11
Limitations
The limitation of this study is that the imaging and laparoscopy facilities were not available in the Governmental hospital, so pathology findings were the gold standard to identify the staging of the lesion in this case (stage IIb).
Conclusion
Despite technical advances in the surgical and medical treatment of hydatid cysts, diagnosing and treating this disease still poses many challenges for physicians. Besides, there is no defined consensus for patient follow-up. In this regard, a high sensitivity is needed to diagnose, especially if there is a cystic lesion anywhere on the body.
Footnotes
Acknowledgements
The authors acknowledge the patient and Alavi Hospital personnel who collaborated on this study.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethics approval
The Ethics Committee of Ardabil University of Medical Sciences approved the study (IR.ARUMS.REC.1401.063).
Informed consent
Written informed consent was obtained from the patient(s) for their anonymized information to be published in this article.
