Abstract
This case reports on a critically ill patient (Male, 74) with severe subcutaneous emphysema which progressed to causing respiratory distress. We document both the severity of the condition we observed and then present a novel intervention. In this case, we decompressed the patient at the intensive care unit-bedside and resolved the condition. While subcutaneous emphysema is relatively common, the severity of the condition we observed, and the lack of definitive treatment guidance have prompted us to present this case as a plausible treatment guide.
Introduction
Subcutaneous emphysema (SE) is a condition frequently seen in intensive care units. It is typically of moderate concern but rarely life-threatening. 1 This condition generally presents as sudden, painless, soft tissue swelling involving the trunk, face, eyes (periorbital), neck, upper extremities, and lower extremities. 2 At times, depending on the extent and acuity of SE, it has been shown to cause severe patient discomfort, airway compromise, cardiac tamponade or even tension pneumomediastium. 1 SE has also been shown that increased accumulation of air in deeper tissue spaces of the thoracic outlet can cause compression of the trachea and great vessels. This can cause compromise of the airway, venous return, and blood flow to the head and neck. 2 There are a multitude of mechanisms and risk factors that can potentially cause SE—namely blunt or penetrating trauma, pneumothorax, infection, malignancy, or more commonly, as a complication of surgical procedure. Resolution generally requires intervention as spontaneous resolution is not commonly seen. 2 The most common clinical sign of SE, besides the obvious swelling, is the palpable cutaneous tension and crepitation on palpation. Progression of SE leading to airway compromise requiring intubation is a very rare occurrence without clearly defined incidence. This leaves practitioners in a difficult clinical conundrum of increasing inspiratory pressures at the expense of worsening SE. Many approaches have been identified in literature to alleviate pressure and subcutaneous decompression which includes subcutaneous drains (SBDs; uni~ or bilateral) or performance of infraclavicular incisions (ICIs);1–3 however, there is no definitive guidance on the alleviation of SE.
Case report
We present here a case of serious SE progressing to airway obstruction and a novel technique to achieve rapid relief of this patient’s respiratory symptoms. A 74-year-old male presented to the emergency department due to noticeably progressing facial and trunk swelling. The patient has a significant history of severe chronic obstructive pulmonary disease (COPD) on 2 L continuous oxygen, with poorly differentiated squamous cell carcinoma characterized as T1 N0 M0, status post stereotactic radiation. Three weeks prior to presentation, the patient experienced a mechanical fall striking his left thorax. The patient first noticed subcutaneous swelling involving the left side of his face, with progressive extension over the entire upper half of his body. Chest X-ray showed extensive SE involving the mediastinum and the subcutaneous areas over the upper chest with evidence of small left-sided pneumothorax (Image 1(a)). Air outlines of individual fibers of the pectoralis muscle were observed in the X-Ray (Image 1(a)). The computed tomography (CT) of the chest (Image 2) suggested similar findings of severe SE diffusely involving both lungs and destructive changes of the left upper lobe, which were chronic due to patient’s past medical history. Patient was initially asymptomatic and hemodynamically stable while on room air, though he experienced acute vision loss because of obstruction due to extensive air infiltration of the lids (Image 3(a)). This proceeded to worsening shortness of breath beyond his typical baseline status. The patient eventually required increased oxygen demand of 15 L via facemask and stated his throat was feeling full. He was intubated via fiberoptic bronchoscopy due to patient’s significant swelling. The severity of SE- in this case was so extreme that we have not been able to find an analogous example in the literature. The patient was placed on ventilator with a positive end-expiratory pressure (PEEP) of 0 and provided 100% oxygen to help create a concentration gradient for the subcutaneous air to track back into circulation and be expelled from the body.
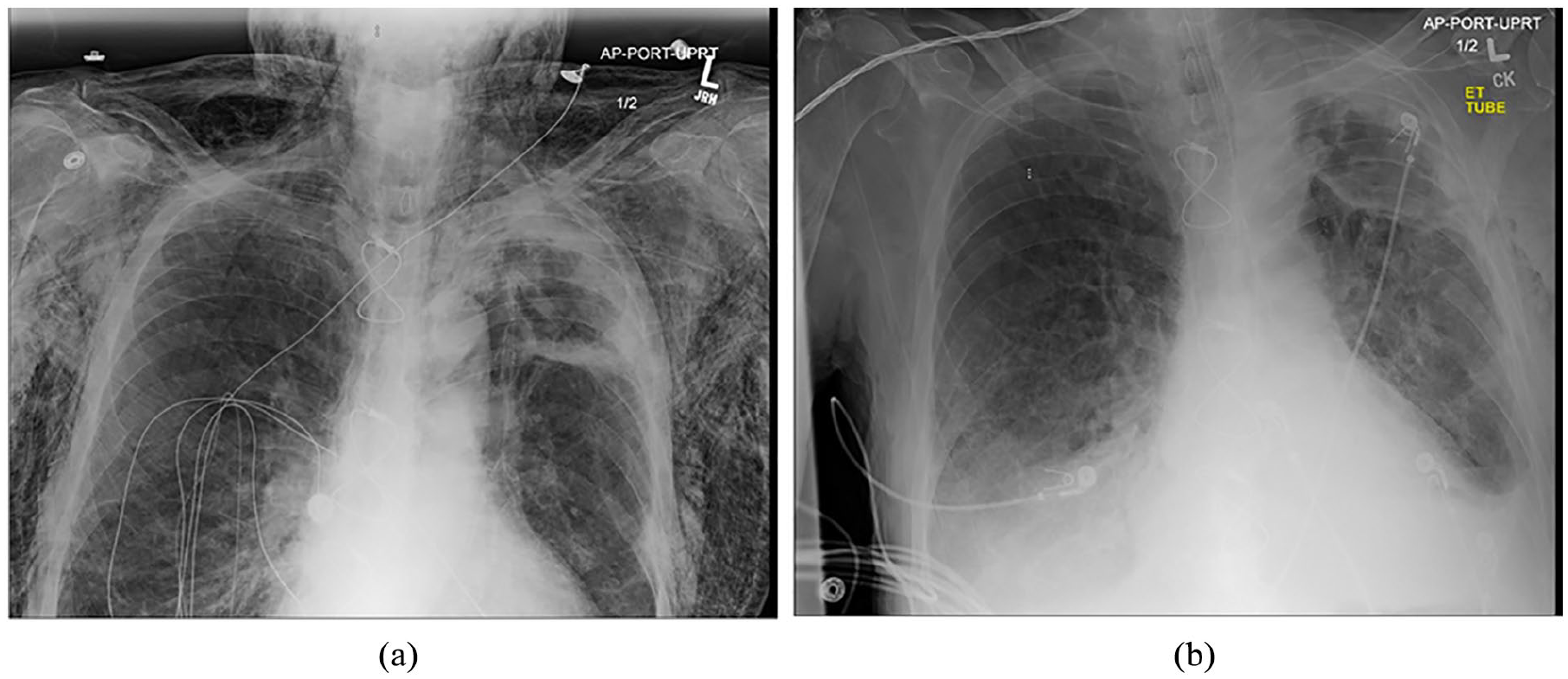
(a) Chest X-ray of patient on admission showing significant SE. (b) Resolution of SE 48 h after insertion of subcutaneous chest tube and simple percutaneous angiocatheter.

CT Chest showing extensive subcutaneous emphysema.

(a) Image of patient on admission with significant periorbital SE. (b) Image of patient on post intervention with resolution of his SE.
Simultaneously, a chest tube was intentionally placed subcutaneously with fenestrations created with scissors prior to placement, inserted in along the left anterolateral aspect of the chest, and turned to suction. Along the right chest and shoulder, two 14G-angiocatheters were placed and secured with a tegaderm patch. Subcutaneous decompression was achieved within 24 h with a noticeable decrease in swelling along the face and upper body. The subcutaneous chest tube and angiocatheters were removed 48 h after insertion (Images 1(b) and 3(b)). Repeat chest X-ray was performed after removal that also showed resolution of SE. The patient was subsequently extubated 48 h after the initial intervention.
Discussion
SE is a common phenomenon which was first described by Louise Bourgeois, midwife to the queen of France, in 1617 and later characterized by Laennec in 1819. 4 It has been described in patients having direct injury, surgery, mechanical ventilation, and infection. Causes and interventions have been analyzed and reviewed thoroughly in literature; 3 however, no definitive treatment has been established for cases of SE. Other techniques cited are submandibular incision, wide angiocatheters, central venous catheters, ICIs, and liposuction. 3 While a number of techniques have been documented as effective in decompressing and relieving tension in underlying tissue, we believe the technique implemented here is simple, minimally invasive, and effective under direction of qualified and experienced practitioners. As mentioned in Theodoros et al., these interventions were provided as a bi- or unilateral approach depending on presentation with the most common interventions being SBD and ICI. 3 Of note, the SBD that were place all measured > 24 French (Fr). In our case, we elected to use a 14 Fr SBD to reduce risk of injury at time of insertion, thoracic pain, and initial size of incision, while also getting the desired effect of the larger SBD. 5 When compared to ICI our approach also reduces the risk of infection, scar formation and regular dressing changes. 6
Explanations as to why respiratory compromise may occur in patients with SE are likely attributable to restriction of thoracic expansion due to the underlying air in the tissue. 7 Another explanation, operative in this case, is that of direct airway compression: Attributable to the subcutaneous air in the surrounding tissue, originating from the lungs. This air may track from the lungs, potentially due to a small tear in the pleura; or track from the alveoli within the bronchoalveolar sheath toward the hilum of the lungs thus escaping into the endothoracic fascia creating SE. 8 Whether air in this tissue space can cause airway compromise remains debatable; however, this case supports this hypothesis due to direct visualization of the airway with fiberoptic bronchoscopy noting swelling and occlusion of the airway.
Conclusion
Regardless of the exact mechanism of airway compromise in this specific case, the patient benefited from early subcutaneous decompression via subcutaneous chest tube and percutaneous angiocatheter placement. This case highlights the importance of continued assessment of patients presenting with initially asymptomatic SE. In patients with massive SE, a patient’s airway can, rarely, become obstructed leading to respiratory failure. While there are many different interventions which could potentially achieve subcutaneous decompression, the intervention described here can be quickly and effectively implemented in patients who develop acute respiratory failure due to SE.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethics approval
Our institution does not require ethical approval for reporting individual cases or case series.
Informed consent
Written informed consent was obtained from the patient for their anonymized information to be published in this article in the form of Hospital consent form in which the patient signed. Consent was obtained from the deceased subject, this was in the form of written informed consent from the legally authorized representative of the patient.
