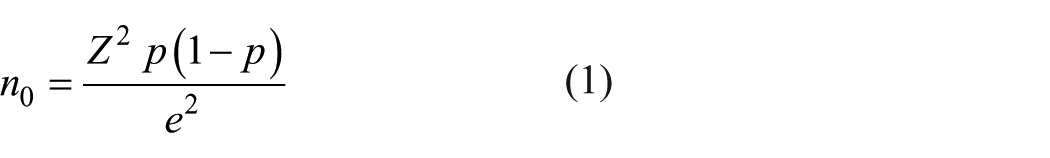Abstract
Objectives:
The primary objective of this study was to assess the outcomes and complication rates associated with different arteriovenous shunt cannulation methods among patients with end-stage chronic kidney disease.
Methods:
The study was carried out at two major hemodialysis centers in a resource-limited healthcare system. A total of 309 patients were included. Vascular access was achieved using the area puncture technique in 171 patients (55.3%) and the rope-ladder technique in 138 patients (44.7%).
Results:
Of the patients, 62 (20.1%) suffered vascular access complications (0.63 events/1000 access days). Hematoma was the most common complication, occurring in 43 patients. Hematoma was significantly associated with female sex (p = 0.024), shorter hemodialysis vintage (p = 0.026), and longer duration of hemodialysis sessions (p = 0.048). High venous access pressure was significantly associated with the rope-ladder technique (p = 0.022), jugular implanted shunts (p < 0.001), and with longer duration of hemodialysis sessions (p = 0.002). Bleeding was associated with a shorter hemodialysis vintage (p = 0.047). Infection was significantly associated with the area puncture technique (p = 0.043) and with cannulation during the noon dialysis shift (p = 0.007). Moreover, thrombosis was significantly associated with female sex (p = 0.014), residing in rural areas (p = 0.018), and absence of comorbidities (p = 0.008).
Conclusion:
Our findings underscore the critical need to implement evidence-based protocols, enhance staff training, and address systemic obstacles in vascular access management.
Keywords
Introduction
Arteriovenous fistulae and arteriovenous grafts are important vascular access types for hemodialysis in patients with end-stage kidney disease (ESKD).1–3 These fistulae are created by the surgical anastomosis of an artery and a vein. 4 Arteriovenous fistulae are widely regarded as the gold standard for vascular access in hemodialysis patients due to their superior long-term patency and lower rates of complications compared to alternatives such as arteriovenous grafts and central venous catheters.1,2
In clinical practice, clinicians often decide on using arteriovenous fistulae or grafts by weighing the need for durable, dependable access against individual patient factors and long-term outcomes. Comparative studies from diverse healthcare settings consistently demonstrated that arteriovenous fistulae are linked with reduced infection rates, fewer thrombosis events, and improved patient survival, thereby enhancing overall clinical outcomes and quality of life.1,2 Recent studies have further emphasized these benefits. For instance, a comprehensive review detailed how advancements in arteriovenous fistulae creation and maintenance, notably through improved surgical techniques and enhanced postoperative surveillance, contribute to access patency and reduced complication rates. 1 Furthermore, research comparing cannulation techniques, specifically the rope-ladder versus the area puncture approaches, suggested that the appropriate selection and execution of cannulation types may further decrease mechanical trauma and prolong the lifespan of the vascular access.1,2,4–12 The suitability of using arteriovenous fistulae depends on certain patient characteristics, including the presence of comorbidities and the architecture of the blood vessels.1,4 Conversely, arteriovenous grafts employ a synthetic conduit to connect an artery and a vein and present a viable option for patients who are ineligible for arteriovenous fistulae. Although arteriovenous grafts offer prompt usability, they are often associated with higher risks of thrombosis and infections.5,11 Despite this robust body of evidence, much of the literature originated from resource-rich settings, highlighting a gap in the evidence regarding their applicability in resource-limited settings.
In Palestine, hemodialysis faces distinct challenges influenced by the region’s socio-political and economic circumstances. 13 The inadequate healthcare infrastructure, together with restricted access to new medical technology, often adversely affects the quality and availability of dialysis treatments. Many hemodialysis centers operate under resource constraints, including shortages of essential supplies, which negatively influence treatment outcomes. Furthermore, geographic obstacles and mobility limitations may impede patients’ access to hemodialysis facilities, resulting in postponed or neglected treatments.14,15 Notwithstanding these limitations, initiatives are in progress to enhance hemodialysis treatment, including investments in infrastructure, personnel training, and collaborations with international organizations. Tackling these systemic obstacles is essential for guaranteeing fair and sustainable access to life-saving dialysis treatments for patients with ESKD in Palestine.
It has been argued that assessing the cannulation type for vascular access, techniques, and timing might help minimize complications, such as infections, aneurysms, hematomas, air embolism, and thromboembolic events.2,9,12,16 In addition, reducing cannulation-related complications can improve the overall quality of life and outcomes for patients with ESKD who are undergoing hemodialysis. Although vascular access is a critical component of successful hemodialysis, the outcomes of arteriovenous shunt cannulation types have not been thoroughly investigated in Palestine. This gap in the literature is particularly significant given the unique socioeconomic and healthcare challenges in resource-limited settings, which may influence both the implementation of cannulation techniques and the resulting complication profiles. The primary objective of this study was to assess the outcomes and complication rates associated with different arteriovenous shunt cannulation types, specifically the area puncture versus rope-ladder technique, in Palestinian patients with ESKD. The findings of this study might not only fill a critical gap by providing locally relevant and context-specific data but also offer insight that could inform improvements in vascular access management and patient care in environments facing similar resource constraints.
Methods
Study design and settings
This prospective cohort study assessed the outcomes and complications associated with arteriovenous shunt cannulation in patients with ESKD undergoing hemodialysis. The study was carried out at two major hemodialysis centers in the West Bank of Palestine. The study was conducted in the period between January 2024 and December 2024. The study was conducted and reported in accordance with the Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) guidelines. Adherence to the STROBE checklist is provided in Supplementary Table S1.
Study population, inclusion, and exclusion criteria
The study population consisted of patients with ESRD undergoing hemodialysis at the study hospitals. Patients were eligible if they met the following criteria: (1) age ⩾18 years, (2) a diagnosis of ESRD requiring hemodialysis, (3) the presence of an arteriovenous vascular access (fistula or graft), and (4) use of either the area puncture or rope-ladder cannulation technique during dialysis sessions.
Patients were excluded if they did not meet the eligibility requirements for the study. Specifically, patients were not considered if they were receiving renal replacement therapy through a central venous catheter or peritoneal dialysis, if they lacked complete medical records or regular follow‑up at the participating centers, or if they had a documented psychiatric or cognitive disorder that could compromise the reliability of data collection or informed consent. These exclusions were applied to ensure a homogeneous study population and to minimize potential sources of bias in the assessment of vascular access outcomes.
Sample size and sampling technique
According to the statistics from the Palestinian Ministry of Health, there were 1601 patients receiving hemodialysis for ESKD in the West Bank of Palestine in 2022. 17 The primary parameter for sample size estimation was the 12‑month proportion of patients experiencing at least one vascular access complication, regardless of the complication. In this study, we calculated the sample size to estimate the 12‑month proportion of patients with any vascular access complication with 95% confidence interval (95% CI) and 5% margin of error (e). Because robust local prevalence data were absent, we used the conservative assumption p = 0.50 to maximize sample size and ensure adequate precision across subgroups. The initial sample size was calculated based on the equation (1):
Where n0 is the initial sample size, Z at 95% CI = 1.96, and e = 0.05. This yielded a sample size of 384 patients. We then adjusted this sample size for the finite source population (N = 1601) using equation (2):
The final target sample size was 310 patients. Due to real‑world screening logistics, we could enroll 309 patients in this study. In case p = 0.20 had been assumed, the finite‑corrected sample size would be ~180. However, we retained the conservative assumption to ensure adequate precision for the primary proportion and subgroup/adjusted analyses. Our prospective cohort was primarily powered for estimating a single proportion; comparisons between cannulation techniques were exploratory. Given the observed complication rates, a post‑hoc detectable absolute difference between groups of about 8%–10% at 80% power (two‑sided α = 0.05) is plausible with the achieved group sizes (171 versus 138).
To thoroughly capture potential complications, patients were followed for 12 months (January–December 2024), with meticulous recording of vascular access-related variables including infection episodes, thrombosis events, bleeding complications, aneurysm or pseudoaneurysm formation, blood pump speed (Qb) recorded during each dialysis session, and interventional procedures (e.g. angioplasty, thrombectomy). A convenience sampling method was employed, whereby consecutive patients visiting the hemodialysis facilities during regular shifts were invited to participate, ensuring representation across age, sex, and clinical characteristics to minimize selection bias.
Study tool and variables
A standardized data collection form was used to systematically acquire the pertinent information. The form was initially developed by the research team after an extensive review of the relevant literature and discussions with vascular surgeons, nephrologists, and hemodialysis specialists.1–3,5–9,18–26 To ensure the authenticity and reliability of our data collection form, content and face validity were then established by an expert panel of independent vascular surgeons, nephrologists, and hemodialysis specialists who were external to this research. To further ensure reliability, the form was pilot‑tested on 30 patients prior to full implementation. The pilot confirmed clarity and feasibility, and minor modifications were incorporated before applying the instrument to the entire cohort. The final data collection instrument is provided in Supplementary Table S2.
The form collected data on patients’ age, sex, and place of residence. Additionally, information regarding comorbid health conditions and medications was obtained. The duration since the initiation of hemodialysis was also recorded. Furthermore, the form gathered details pertinent to the cannulation techniques, vascular access type, anatomic location of the arteriovenous anastomosis, timing of arteriovenous shunt cannulation, hemodialysis session duration, and blood flow rate. In this study, the measured blood pump speed referred to Qb, representing the rate of blood circulated through the dialysis circuit by the dialysis machine. Venous pressure was monitored during every dialysis session using 16‑gauge metal needles. Although international guidelines such as Kidney Disease Outcomes Quality Initiative (KDOQI), Buttonhole, Rope-ladder, Stepladder, and British Columbia Renal Agency recommend maintaining Qb within 300–350 mL/min when using 16‑gauge needles, in Palestinian practice, higher values are tolerated in real‑world monitoring, often up to 400 mL/min. This reflects the realities of resource‑limited settings, where maximizing dialysis efficiency is prioritized despite guideline thresholds. Venous pressure was displayed continuously on the dialysis machine. Arterial pressure was also routinely monitored and adjusted as needed; however, venous pressure was emphasized in this study because it is more sensitive to changes in outflow resistance and can serve as an early indicator of access dysfunction. Importantly, in local practice, a marked rise in venous pressure accompanied by a less negative arterial pressure is considered suggestive of underlying stenosis.
To account for potential surgeon/provider fatigue, the dialysis shift (morning, noon, evening) during which cannulation occurred was collected; the timing of surgical shunt implantation was not recorded. In the hemodialysis centers, hemodialysis session duration was prescribed on an individualized basis by the treating nephrologist, with standard treatments set at 4 h thrice weekly. Prescription length was determined to achieve adequacy targets (
In this study, cannulation was performed using two established techniques: the rope-ladder and the area puncture approaches. The rope-ladder technique entails advancing needle insertion sites sequentially along the entire length of the arteriovenous fistula or graft, thereby dispersing mechanical trauma across the access and supporting long-term patency. By contrast, the area puncture technique confines all punctures to a limited, predefined segment of the access, often chosen for its ease of palpation or visualization, which can simplify cannulation but concentrates repetitive injury in one location. Both types were carried out by experienced dialysis staff under standardized aseptic conditions, using uniform needle types and insertion protocols to ensure consistency across sessions. Dialysis frequency was not included in the data collection form because all patients in this cohort uniformly received hemodialysis three times per week. Information on prior vascular access types (e.g. central venous catheters, fistulae, or grafts) and underlying kidney disease was also not collected, as the study was designed to focus specifically on outcomes related to the current arteriovenous access cannulation technique. Including these variables could have introduced confounding factors unrelated to the primary comparison of cannulation methods.
All cannulations were performed by experienced hemodialysis nurses, each with more than 5 years of clinical experience in vascular access management. The procedures were supervised by a vascular surgeon with over 15 years of expertise, who also ensured adherence to standardized cannulation protocols. This approach provided consistency in practice and minimized variation related to operator expertise or decision‑making regarding cannulation technique. A standardized definition of each technique was applied, and no patient switched from one method to the other during the study period; therefore, outcomes were not influenced by crossover between techniques. To ensure that the rope‑ladder technique did not inadvertently devolve into the area puncture approach, we implemented a structured system of zoning, training, supervision, and documentation. Each dialysis unit was divided into two zones, with one zone assigned exclusively to the rope‑ladder technique and the other to the area puncture technique for the entire study period. Nurses were formally educated in the technique designated for their zone through dedicated workshops, visual demonstrations, and competency assessments, and were instructed not to cross‑apply methods. A standardized cannulation schedule was maintained in the rope‑ladder zone, requiring nurses to advance puncture sites sequentially along the access and to document the exact location of each insertion in the patient’s record. In the area puncture zone, nurses were trained to consistently use the predefined segment and likewise document the puncture location. Documentation forms included schematic diagrams of the access, on which nurses marked each cannulation site, thereby providing a visual record that could be audited. These records were reviewed weekly by the research team and cross‑checked by the supervising vascular surgeon and the head nurse of each zone. Any deviation from the assigned technique triggered immediate retraining and corrective feedback. This layered system of education, strict documentation, and continuous monitoring ensured fidelity to the assigned cannulation method and minimized the risk of inadvertent crossover. Importantly, no patient switched between rope‑ladder and area puncture techniques during the study period, as confirmed by documentation audits. However, information on cannulation practices prior to enrollment was not systematically collected; therefore, our analyses reflect outcomes associated with the assigned technique during the prospective follow‑up rather than the entire lifespan of the vascular access.
Ultrasonography was not used to plan or guide cannulation. Duplex ultrasound was reserved for cases where elevated venous pressure raised suspicion of thrombosis, serving as the confirmatory diagnostic tool. Venous tourniquets were not applied. All cannulations were performed under a standardized hygiene protocol. Puncture sites were disinfected with 2% chlorhexidine in 70% isopropyl alcohol using sterile swabs, allowed to air‑dry for at least 30 s, and cannulation proceeded only after drying was complete. Nurses adhered to aseptic precautions, including surgical masks, disposable gloves, and single‑use aprons. After needle removal, direct manual pressure was applied with a 10 × 10 cm gauze pad until bleeding ceased; gauze was discarded immediately thereafter. No topical ointments or dressings were used unless clinically indicated. Compliance was monitored by the head nurse and supervising vascular surgeon to ensure strict adherence. Standard equipment included the AV‑set SRB‑R 4008, BiBag 5008 650Gm AF 80, and sodium chloride 0.9% (1000 mL). All sessions were conducted using the Fresenius 5008S Cordiax machine (Fresenius Medical Care, Germany).
Data on cannulation technique were collected prospectively at the dialysis centers. From January to December 2024, research staff systematically documented patient identifiers and all vascular access complications using the standardized data collection form that included predefined fields for hematoma, high venous pressure, infection episodes, thrombosis events, bleeding complications, along with an open‑ended section to capture any additional events. If the same type of complication occurred multiple times in a single patient, each episode was documented as a separate event to allow accurate assessment of complication frequency and recurrence. To ensure data integrity, entries were cross‑checked for completeness and accuracy, with discrepancies resolved in consultation with clinical professionals. All suspected complications were independently reviewed by two investigators, and any unresolved disagreements were adjudicated by an external vascular surgeon, thereby ensuring consistency, reliability, and validity of the collected data.
Vascular access complications were diagnosed according to predefined clinical, laboratory, and, where available, imaging criteria. Hematoma was identified as a localized subcutaneous collection of blood presenting as swelling and discoloration at the cannulation site, confirmed by visual inspection and measured by the treating clinician.3,9,23,26 Venous pressure was continuously monitored during dialysis. In routine practice, high venous pressure was defined as either (a) a sustained reading above 200 mmHg during dialysis or (b) an acute rise of more than 50 mmHg over the patient’s baseline. This dual definition ensured consistency with local monitoring practices while providing a standardized threshold for complication reporting.27,28 Bleeding was defined as persistent bleeding from the puncture site lasting longer than 5 min despite application of direct pressure. This 5‑min cutoff was selected to standardize real‑time documentation by nursing staff during dialysis sessions and to capture only clinically significant bleeding events requiring additional attention. Hemostasis data were collected only during routine dialysis treatments, and inter‑dialytic bleeding episodes were not systematically recorded.28,29 The time from needle withdrawal to hemostasis was systematically monitored by the dialysis nursing staff during each treatment. Immediately after needle removal, nurses applied direct manual pressure to the puncture site and observed the site continuously until bleeding ceased. A standardized 5‑min cutoff was used: if bleeding persisted beyond 5 min despite uninterrupted pressure, the extended duration was recorded in the nursing record and on the complication reporting form, together with any additional measures taken (e.g. continued pressure, compressive dressing, or change of gauze). This approach ensured that the 5‑min threshold was consistently applied across all patients and that prolonged bleeding episodes were prospectively documented as clinically significant complications. Infection at the arteriovenous access site was diagnosed in patients presenting with local signs of inflammation, erythema, warmth, swelling, or purulent discharge. For every episode of suspected access-site infection, aseptic swab or aspirate cultures of the exit site were obtained as a standard diagnostic step, regardless of the severity of clinical signs or presence of systemic features. Positive cultures were defined as growth of ⩾105 colony-forming units per milliliter. In patients exhibiting systemic manifestations (e.g. fever or chills), additional blood cultures were also drawn. Importantly, any case with negative local cultures but clear clinical evidence of infection, prompting the initiation of systemic antibiotic therapy, was likewise classified as an access-site infection.18,22,30 Thrombosis was suspected when there was abrupt loss of a palpable thrill or auscultatory bruit over the access and reduced blood flow during dialysis; confirmation was obtained using duplex ultrasound, as per the study protocol to demonstrate an occlusive intraluminal thrombus or by intraoperative visualization of thrombus during surgical thrombectomy.1,24 Shuntoplasty was defined as open surgical venous outflow revision, performed by longitudinal venotomy followed by patch angioplasty or segmental interposition grafting, depending on lesion length and vessel quality. An aneurysm was defined as a localized, permanent dilation of the arteriovenous fistula segment exceeding 150% of the adjacent normal vessel diameter, with or without associated wall thinning. 26
All information regarding vascular access complications was obtained from patients’ hospital medical records, which included nursing notes, dialysis machine logs, and physician reports documenting access‑related events. To ensure that medical records were properly and consistently utilized, the research team developed a standardized complication reporting form that was integrated into routine dialysis practice. Nursing staff completed this form in real time during each dialysis session to record any suspected vascular access complication, including hematoma, bleeding, infection, thrombosis, or high venous pressure. Each entry was cross‑checked against the patient’s medical record to verify accuracy and completeness, and discrepancies were resolved in consultation with the treating nephrologist or vascular surgeon. All suspected complications were reviewed independently by two investigators, with adjudication by an external vascular surgeon when necessary. This dual‑source approach, systematic medical record review combined with prospective real‑time reporting, ensured that all complications were comprehensively captured and consistently documented in accordance with the study protocol.
Statistical analysis
Data analysis was conducted using IBM SPSS version 22.0 [International Business Machines (IBM) Corporation, Armonk, New York]. Descriptive analysis was employed to describe the variables. Quantitative variables with non-normal distributions were reported using their medians along with the lower (Q1) and upper (Q3) quartiles. Categorical variables were expressed as frequencies and percentages. To evaluate the outcomes and complications associated with arteriovenous shunt cannulation types, we used chi-square/Fisher’s exact tests or Mann–Whitney U tests. Furthermore, a multivariate logistic regression analysis was conducted to control for potential confounding variables, and the relevant demographic and clinical variables were retained in the regression models. Supplementary Table S3 presents the covariates retained in our multivariate logistic regression models alongside those omitted, with detailed justifications for each inclusion or exclusion. A p < 0.05 was considered statistically significant. Both hemodialysis vintage and duration of hemodialysis session were treated as continuous variables, reported as medians (Q1–Q3), and compared across groups using the Mann–Whitney U test. For descriptive clarity, we also refer to ‘shorter’ versus ‘longer’ durations relative to the cohort median values. No external or a priori cut-off points were imposed; ‘shorter’ indicates values below the median, and ‘longer’ indicate values at or above the median.
Ethical considerations
This study strictly adhered to the ethical guidelines outlined in the Declaration of Helsinki. Approvals were obtained from the Institutional Review Board (IRB) of An-Najah National University and from the two hemodialysis centers (approval # Med. Dec. 2023/49). The patients provided written informed consent prior to inclusion in the study. Throughout the study, the participants’ autonomy was upheld, and no attempts were made to unduly influence their participation. Data confidentiality was rigorously maintained by anonymizing patient information using assigned code numbers and securely storing all data in locked cabinets with access limited solely to the research team. The patients retained the right to withdraw from the study without any obligation to provide a reason.
Results
Demographic, health, and hemodialysis characteristics of the patients
Between January and December 2024, a total of 340 patients receiving hemodialysis were screened for eligibility. Of these, 31 were excluded and 309 patients were enrolled, all of whom completed follow‑up and were included in the final analysis. A flow diagram of the patient section process is shown in Supplementary Figure S1. The median age of the patients was 61.7 years (range: 54.3–67.4). Of these patients, 185 (59.9%) were male and 153 (49.5%) resided in urban areas. The patients had been undergoing hemodialysis for a median duration of 54.2 months (range: 33.0–82.8). Vascular access was achieved using the area puncture technique in 171 patients (55.3%) and the rope-ladder technique in 138 patients (44.7%). The majority of patients (n = 291, 94.2%) had arteriovenous fistulae, whereas 18 (5.8%) had arteriovenous grafts. Regarding shunt location, most patients (n = 252, 81.6%) had a shunt in the brachial artery, while 54 patients (17.5%) had one in the radial artery. The median duration of hemodialysis session was 220.0 min (range: 209.5–228.5), and the median blood flow rate was 378.0 mL/min (range: 342.0–399.0). Additionally, 196 patients (63.4%) had other comorbidities. Detailed demographic, health, and hemodialysis characteristics of the patients are shown in Table 1, and further details regarding comorbidities and chronic medications are provided in Supplementary Table S4.
Demographic, health, and hemodialysis characteristics of the patients (n = 309).

Q1: lower quartile; Q3: upper quartile.
Thigh arteriovenous anastomoses utilized a transposed superficial femoral vein, mobilizing the superficial femoral (or popliteal) vein from below the knee and anastomosing it side-to-side with the superficial femoral artery in the mid-thigh or a loop of the great saphenous vein, employing a segment of the saphenous vein tunneled superficially on the anterior thigh and connected end-to-side with the common femoral artery.
Jugular arteriovenous anastomoses were located between the common carotid artery and the internal jugular vein, as created at the root of the neck deep to the sternocleidomastoid muscle, just above the clavicle.
Vascular access complications
Of the patients, 62 (20.1%) suffered vascular access complications. Among the 62 patients who experienced complications, 53 had a single complication and 9 had two complications. The median number of complications per patient was 1 (1.0–2.0). To address the primary objective, vascular access complications were stratified by cannulation technique and normalized to access days. Among patients receiving the rope‑ladder technique (n = 138), 31 experienced at least one complication, yielding a rate of 0.69 events/1000 access days. In the area puncture group (n = 171), 31 patients also experienced complications, corresponding to 0.58 events/1000 access days. Hematoma was the most frequent complication in both groups, occurring in 17 rope‑ladder patients (0.36/1000 access days) and 26 area puncture patients (0.38/1000 access days). The most frequent sites of hematoma were arteriovenous fistulae located in the left brachial region (n = 29, 67.4% of hematoma cases) and the right brachial region (n = 9, 20.9%). The median size of the hematoma was 4.0 (3.0–4.0) cm. Cold compression was used to manage more than half of the hematoma cases (n = 25, 58.1%), while the remainder were treated conservatively with limb elevation, compressive bandaging, and analgesic therapy. High venous pressure and bleeding were more common in the rope‑ladder group, with 8 and 6 cases, respectively (0.17 and 0.13/1000 access days), while infections and thrombosis occurred exclusively in the area puncture group, with 5 and 4 cases, respectively (0.089 and 0.071/1000 access days). High venous pressure was managed by shuntoplasty and bleeding by pinpoint pressure. Cultures revealed no growth and infections were treated with vancomycin. All thrombosis cases occurred within arteriovenous fistulae located in the left brachial region and were managed by thrombectomy. Using the definition, no cases of aneurysm or pseudoaneurysm were identified during the 12‑month follow‑up period. Details of the vascular access complications are shown in Table 2.
Complication counts and rates per 1000 access days stratified by cannulation technique (area puncture versus rope‑ladder).

Associations between cannulation techniques, vascular access type, and other variables of the patients
In this study, patients who received the rope-ladder cannulation technique were more likely to have significantly longer duration of hemodialysis session (p < 0.001) and were more likely to experience high venous pressure (p = 0.022). On the other hand, those who received the area puncture vascular access type were more likely to reside in urban areas (p = 0.001) and experience infections (p = 0.043). Significant associations between cannulation techniques and patient variables are shown in Table 3. Non-significant associations are provided in Supplementary Table S5.
Significant associations between cannulation techniques and patient variables.

Statistically significant p values are in boldface.
Q1: lower quartile; Q3: upper quartile.
Chi-square test.
Mann–Whitney U test.
In this study, patients who received an arteriovenous graft were more likely to be male (p = 0.036), to have comorbidities (p = 0.021), to have undergone hemodialysis for a longer period (p = 0.001), and to have had the shunt implanted via the radial artery (p = 0.001), and most cannulation procedures were performed during the morning shift (p = 0.032). Conversely, no significant associations were observed between the vascular access type and other patient variables. Significant associations between vascular access type and patient variables are shown in Table 4. Non-significant associations are provided in Supplementary Table S6.
Significant associations between vascular access type and the other variables of the patients.

Statistically significant p values are in boldface.
Q1: lower quartile; Q3: upper quartile.
Chi-square test.
Mann–Whitney U test.
Associations between the complications and other variables of the patients
Hematoma occurred in 43 of 309 patients (13.9%) and was significantly more common in female (24/124; 19.4%) than male (19/185; 10.3%, p = 0.024) patients. Those who developed hematomas had a shorter hemodialysis vintage (median 43.1 months (interquartile range [IQR] 21.6–79.2) versus 55.6 months (35.2–82.9), p = 0.026) and underwent longer sessions (225.0 min (217.0–229.0) versus 217.0 min (209.0–228.0), p = 0.048). High venous access pressure was observed in 10 of 309 patients (3.2%) and was significantly associated with rope-ladder cannulation (8/138; 5.8%) compared with the area puncture technique (2/171; 1.2%, p = 0.022). Hemodialysis sessions with high venous access pressure also lasted longer (median 232.0 min (232.0–232.0) versus 218.0 min (209.0–228.0), p = 0.002). Bleeding complications were recorded in 12 patients (3.9%). Those affected had a markedly shorter dialysis vintage (21.3 months (19.8–78.0) versus 54.6 months (34.5–82.8), p = 0.047). Infection developed in five patients (1.6%) and was significantly linked to the area puncture technique (5/171; 2.9% versus 0/138; 0.0% with rope-ladder, p = 0.043) and was cannulated during the noon shift (5/126; 4.0% versus 0/183; 0.0% in morning sessions, p = 0.007). Thrombosis affected four patients (1.3%) and occurred exclusively in female patients (4/124; 3.2% versus 0/185; 0.0% males, p = 0.014) and those residing in rural areas (4/104; 3.8% versus 0% in urban/refugee settings, p = 0.018). No thrombosis was observed among patients with other comorbidities (0/196 versus 4/113 without comorbidity; p = 0.008). These details are shown in Supplementary Table S7.
We conducted multivariate logistic regression analysis to control for potential confounding variables. This analysis indicated that female patients were 2.1-fold (95% CI: 1.0–4.1) more likely to suffer hematoma compared to their male counterparts. Moreover, patients who received the rope-ladder technique were 10.4-fold (95% CI: 1.3–86.2) more likely to experience high venous access pressure, and those who received a jugular shunt were 4.3-fold (95% CI: 1.4–12.9) more likely to develop high venous access pressure compared to patients who underwent cannulation via other techniques. Similarly, patients who underwent longer hemodialysis sessions were 1.1-fold (95% CI: 1.0–1.1) more likely to experience high venous access pressure. These associations are presented in Table 5.
Factors predicting complications.

Statistically significant p values are in boldface.
CI: confidence interval, OR: odds ratio, SE: standard error.
Discussion
The present study explored the Palestinian experience with arteriovenous shunt vascular cannulation for hemodialysis in patients with ESKD. This study is the first to describe outcomes, arteriovenous shunt cannulation-related complications, and their associated factors in Palestinian clinical practice. The principal results revealed that, in Palestinian clinical practice, arteriovenous fistulae were the primary vascular access type, predominantly established using the area puncture approach. Furthermore, the results of this research indicated that the rope-ladder technique was associated with a reduced incidence of infections when compared to the area puncture method.
The findings of this study revealed an overall complication rate of 20.1%, with hematoma being the most common arteriovenous shunt cannulation‑related complication, occurring at a rate of 0.63 events/1000 arteriovenous fistula days and affecting 69.4% of patients who experienced complications. These findings are consistent with those reported in other healthcare systems.2,9,16 Hematoma is frequently cited as the most common early complication following arteriovenous fistula cannulation. For example, Allon reported hematoma rates ranging from 10% to 25% in incident fistula patients, with risk factors including female sex and shorter dialysis duration, findings echoed in our study. 2 However, compared with previous studies, the incidence of hematomas in our study was relatively higher.2,6,9,16 Possible contributing factors include resource constraints, variability in procedural techniques, and differences in patient populations. It should also be noted that the definition of hematomas may vary across studies, which could partly explain the higher frequency observed in our cohort compared with earlier reports.
Of the factors associated with hematoma formation, only prolonged hemodialysis session duration is directly modifiable in clinical practice. Although female sex and shorter hemodialysis vintage were also linked to higher hematoma risk, these represent non-modifiable patient characteristics and treatment history. Accordingly, targeted interventions should focus on optimizing session length and refining cannulation technique, through standardized protocols and enhanced staff training, to reduce hematoma rates. 9 Implementing standardized protocols, pre-cannulation risk assessment, ultrasound-guided site selection, strict aseptic technique with site rotation, and post-cannulation care minimizes vessel trauma and infection.1,2 Scheduling high-risk patients (e.g. women and those new to dialysis) with experienced staff during less busy shifts can further lower complication rates. Routine audit-and-feedback cycles are essential for monitoring adherence and early detection of issues.
Hematomas are generally managed with conservative measures such as cold compression and localized pressure, along with modifications of cannulation techniques to minimize repetitive trauma at the same site. 2 Conducting vascular access research and implementing optimal cannulation practices in resource‑limited settings presents unique challenges. Advanced methods such as ultrasound‑guided cannulation or the use of plastic cannulas can significantly reduce complications like hematoma and infiltration; however, their high cost and limited availability often make them impractical in low‑resource environments. In our study context, these tools were not routinely available. Instead, we focused on low‑cost, feasible strategies to minimize complications, including comprehensive nurse education, strict adherence to standardized cannulation techniques, and close supervision by a vascular surgeon and head nurse. Strengthening staff training, promoting consistent documentation, and ensuring early detection of access issues through regular clinical assessment may represent sustainable and effective alternatives for improving cannulation outcomes in such settings.
Infections, while less frequent with arteriovenous fistulae compared to grafts or catheters, remain a significant concern. For instance, arteriovenous fistula infection rates were reported at ~0.2–0.5 episodes/100 patient‑months, which corresponds to about 0.07–0.17 events/1000 arteriovenous fistula days. In our study, infections occurred at a rate of 0.089 events/1000 arteriovenous fistula days. Substantially lower rates were seen with grafts, but still clinically relevant, particularly in settings with limited resources or staff training. 1 In this study, infections were observed in 8.1% of patients with complications. Infections were associated with the area puncture technique and noon cannulation. Area puncture cannulation was associated with a higher risk of infection compared with the rope‑ladder technique in this study. This finding is biologically plausible, as repeated puncture of the same site in area puncture cannulation can cause localized tissue trauma, impaired healing, and increased susceptibility to bacterial entry.2,8,18,24,26 In contrast, the rope‑ladder method distributes punctures across multiple sites, allowing time for tissue recovery and thereby reducing infection risk.
We hypothesize that the midday shift’s higher infection rate reflects a convergence of peak procedural volume, transitional handovers around lunch, mild provider fatigue, and slightly warmer environmental conditions, each of which can subtly compromise strict aseptic technique. Prospective time-motion studies and environmental sampling are warranted to isolate and mitigate these factors.
Infections are addressed by adhering to strict aseptic protocols during cannulation, early detection of microbial colonization, and prompt initiation of appropriate antibiotic therapy. 5 These results underscore the importance of staff training and adherence to evidence‑based cannulation practices to minimize infection‑related complications.
Thrombosis is another major complication that can lead to access loss. For instance, a study reported thrombosis rates of 0.11–0.23 events/patient‑year for arteriovenous fistulae, equivalent to about 0.30–0.63 events/1000 arteriovenous fistula days. 5 In our study, thrombosis occurred at a rate of 0.09 events/1000 arteriovenous fistula days. Higher rates were observed in women and patients with suboptimal vessel anatomy.
In this study, thrombosis was observed in 6.5% of patients with complications. Thrombosis was more frequently observed among female patients, those residing in villages, and those without comorbidities. An additional consideration is that female patients residing in rural areas may have used their fistula-bearing arm more frequently for daily household or agricultural activities. Such repetitive or strenuous use could plausibly contribute to mechanical stress on the vascular access and increase the risk of thrombosis. Although our study did not specifically assess arm use outside the dialysis setting, this factor may partly explain the observed association. Future studies incorporating patient-reported activity levels and arm usage patterns could provide further insight into the impact of physical activity on vascular access outcomes.
Comparative studies of cannulation techniques have shown that the rope-ladder method is associated with a lower risk of both hematoma and thrombosis compared to the area puncture technique, although the difference in infection rates was not statistically significant.1,2,8,9,12,16,18,24,26,27,29,31
Thrombosis is typically managed through early diagnosis using imaging modalities, followed by timely interventions such as thrombectomy and anticoagulant therapy.
This research work revealed associations between several complications related to the cannulation of arteriovenous shunts, including high venous access pressure, hemorrhage, and aneurysm formation, and certain patient characteristics, including vascular access type and hemodialysis session duration.
High venous access pressure and prolonged bleeding episodes are clinically significant and require careful monitoring. Scheduling high-risk patients with experienced staff and implementing structured surveillance protocols can mitigate these risks. Shuntoplasty and aneurysm management remain important surgical interventions when complications arise.
In this investigation, significant associations were observed between the vascular access type and patient outcomes. Hematomas occurred at a rate of 0.63 events/1000 arteriovenous fistula days, infections at 0.089 events/1000 arteriovenous fistula days, and thrombosis at 0.09 events/1000 arteriovenous fistula days. Previous studies have suggested that the rope‑ladder technique may require slightly longer cannulation time because a new puncture site must be identified at each session.2,5,9,12 Our study did not measure or compare cannulation time between techniques; this observation is drawn from the literature. In our cohort, the rope‑ladder technique was associated with lower infection rates. However, these variations may also be attributed to differences in clinical practice and patient characteristics. Overall, the evidence supports expanding the use of the rope-ladder technique, which minimizes access complications and helps maintain long-term fistula function. We acknowledge that some variability in procedural technique among nursing staff is inevitable in routine clinical practice. However, in this study, we took several measures to minimize its potential impact on outcomes. All nurses received standardized training, were assigned exclusively to one cannulation technique, and were supervised regularly by the vascular surgeon and head nurse. Furthermore, all procedures were performed according to a unified protocol, and adherence was continuously monitored throughout the study period. These safeguards ensured consistency across groups, and while minor individual variations may have occurred, they are unlikely to have significantly influenced the overall results.
Furthermore, multiple international guidelines, including the KDOQI (2019) and the UK Kidney Association, explicitly advise against the use of the area puncture technique, as it is associated with serious complications such as aneurysm formation, infection, and vascular access failure.32,33
Our results resonate with the KDOQI Vascular Access guidelines, which endorse the rope-ladder cannulation technique and routine access surveillance (including dynamic venous pressure monitoring and duplex ultrasonography) to optimize patency and minimize infection.20,21,34 Large observational cohorts have further demonstrated that early complication rates predict long-term access survival and that center-level adherence to standardized cannulation protocols is associated with 12-month patency rates exceeding 80% and infection rates below 0.5 episodes/100 patient-months. 31
Strengths of the study
There are several strengths of this study. First, the research provided a thorough assessment of the complications associated with arteriovenous shunt cannulation in Palestinian medical practice. Second, it examined the various clinical and demographic variables linked to these complications, thereby enhancing our understanding of their determinants. Third, the study included a relatively large sample size of hemodialysis patients, which enhances its external validity and facilitates the generalizability of the results to the broader Palestinian context. Fourth, the use of a prospective design with a 12-month follow-up period ensured rigorous monitoring of outcomes over time, thereby strengthening the methodological rigor of the findings. Finally, the rigorous data collection and validation procedures employed throughout the study increased the reliability and accuracy of the results. Collectively, these strengths underscore the robustness of the research and its valuable contribution to vascular access management in resource-limited settings.
Limitations of the study
Despite the strengths of our prospective design, relatively large cohort, and rigorous adjudication process, several limitations should be acknowledged. The study was conducted in two major hemodialysis centers using a convenience sample of consecutive patients. While this approach reflects real‑world practice and ensures proportional representation across shifts and demographic groups, the non‑random sampling may limit generalizability beyond the Palestinian context. The 12‑month follow‑up period allowed us to capture early and mid‑term complications, which represent the majority of clinically relevant events; however, longer‑term patency and durability outcomes were not assessed. Aneurysm formation, for example, often develops after several years of repeated cannulation, and extended follow‑up would therefore be required to evaluate its incidence in relation to rope‑ladder and area puncture techniques. Future studies with longer follow‑up are needed to link early complications with long‑term access survival. Although our data collection tool underwent expert review and pilot testing, it was not formally psychometrically validated. Some outcomes, such as cannulation difficulty, pain, and inter‑dialytic bleeding were not systematically recorded, which may have led to underestimation of the overall burden of cannulation‑related complications. Similarly, prior vascular access history and underlying kidney disease were not captured, which could have provided additional context for complication risk. Definitions of complications were based on internationally accepted criteria and adjudicated by independent reviewers; nonetheless, systematic imaging (e.g. duplex ultrasound for all patients) was not feasible in this resource‑limited setting, and some subclinical events may have been missed. The small number of infections (n = 5) and thrombosis events (n = 4) also limited the statistical power of multivariable models, resulting in wide CIs. For these outcomes, simplified or univariate analyses may provide more robust estimates.
Although all cannulations were performed by experienced nurses under vascular surgeon supervision and standardized protocols, operator‑level variables such as years of practice or workload during specific shifts were not recorded. These unmeasured factors may have contributed to the higher infection rates observed at midday. In addition, the small subgroup of patients with arteriovenous grafts reflects local practice patterns but limited our ability to draw firm conclusions about graft‑specific outcomes. Taken together, these limitations reflect the challenges of conducting high‑quality vascular access research in resource‑constrained environments. Nonetheless, they do not undermine the central finding that cannulation technique, session characteristics, and patient factors materially influence complication risk. Future studies should incorporate longer follow‑up, systematic imaging, patient‑reported outcomes, and operator‑level data, and ideally employ randomized designs to strengthen causal inference.
Finally, complications in arteriovenous fistulae and grafts are not solely determined by the cannulation technique but are also influenced by patient‑level biological and comorbidity factors. Individuals with polycystic kidney disease are predisposed to aneurysm formation, patients with diabetes often develop vascular stenosis due to endothelial dysfunction, and female patients may have smaller‑caliber vessels that affect fistula maturation and increase susceptibility to complications. Because these disease‑specific and anatomical determinants were not systematically captured in our dataset, our findings should be interpreted as reflecting procedural associations rather than the full spectrum of patient‑related risks. Future studies incorporating these variables could provide a more comprehensive understanding of complication risk.
Conclusion
In conclusion, this study described the Palestinian experience with arteriovenous shunt cannulation and its related complications, highlighting an overall complication rate of 20.1%, with hematoma emerging as the predominant issue, affecting 13.9% of the patients and accounting for 69.4% of all access-related events. Our findings underscore the critical need to implement evidence-based protocols, enhance staff training, particularly around techniques that minimize hematoma risk, and address systemic obstacles in vascular access management. Future studies should focus on long-term outcomes, the durability of interventions that reduce hematoma incidence, and the development of targeted strategies to improve the quality of care for hemodialysis patients in resource-constrained settings.
Supplemental Material
sj-docx-1-smo-10.1177_20503121251407165 – Supplemental material for Arteriovenous shunt cannulation in hemodialysis patients: A prospective cohort study of outcomes and complications in a resource-limited healthcare system
Supplemental material, sj-docx-1-smo-10.1177_20503121251407165 for Arteriovenous shunt cannulation in hemodialysis patients: A prospective cohort study of outcomes and complications in a resource-limited healthcare system by Ramzi Shawahna, Aseel Hafaitha, Lyan Saadi, Salwa Haj-Yahia, Tala Adawi, Sultan Saada and Hatim Hijaz in SAGE Open Medicine
Footnotes
Ethical considerations
This study strictly adhered to the ethical guidelines outlined in the Declaration of Helsinki. Approvals were obtained from the Institutional Review Board (IRB) of An-Najah National University and from the two hemodialysis centers (approval # Med. Dec. 2023/49).
Consent to participate
The patients provided written informed consent prior to inclusion in the study. Throughout the study, the participants’ autonomy was upheld, and no attempts were made to unduly influence their participation. Data confidentiality was rigorously maintained by anonymizing patient information using assigned code numbers and securely storing all data in locked cabinets with access limited solely to the research team. The patients retained the right to withdraw from the study without any obligation to provide a reason.
Author contributions
Ramzi Shawahna, Sultan Saada, and Hatim Hijaz were involved in the conception and design of the work, analysis and interpretation of data, and drafting and final approval of the article. Aseel Hafaitha, Lyan Saadi, Salwa Haj-Yahia, and Tala Adawi were involved in the data acquisition, analysis, drafting of the work, and final approval of the version to be published. All authors approved the final article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data availability statement
All data analyzed in this study were included in the article. The datasets used in the analysis or entered into statistical software can be obtained from the corresponding author upon making a reasonable request.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.