Abstract
Background:
Improper disposal of medications is a growing global concern, leading to environmental contamination and public health risks, including accidental poisoning and antimicrobial resistance. This study assessed public knowledge, attitudes, and practices regarding disposing of unused and expired medications among community pharmacy visitors in Kathmandu, Nepal.
Methods:
A cross-sectional study was conducted using the Return and Disposal of Unused Medication questionnaire among 395 randomly selected participants, and a 100% response rate was achieved. Descriptive and inferential statistics, including chi-square tests, were used to identify significant associations with the Statistical Package for Social Sciences version 23.
Results:
Over half of the respondents (n = 247, 62%) understood the proper disposal methods for unused and expired medication. Additionally, a majority of participants (n = 366, 92%) exhibited a positive attitude, while more than two-thirds (88.1%) were aware of the detrimental effects of incorrect medicine disposal on the environment. Approximately 43% (n = 171) of respondents reported having unused medicines stored at home, with analgesics (46%) and antibiotics (42%) being the most common types. Most participants disposed of expired medicines in household garbage bins and retained unused medications at home until their expiration. Furthermore, a significant association was identified between respondents’ knowledge levels and their actual practices in medicine disposal (p < 0.001).
Conclusion:
Despite positive attitudes, gaps in practice highlight the urgent need for awareness campaigns and structured disposal programs. The findings suggest actionable measures, including national guidelines and pharmacy-led take-back programs, to mitigate improper disposal of unused and expired medicines.
Introduction
The global production and consumption of pharmaceuticals have been rising rapidly, raising significant concerns about the proper disposal of pharmaceutical waste and its impact on the environment and human health. Pharmaceutical wastes include a range of substances such as expired medications, unused prescriptions, spilled or contaminated drugs, and outdated vaccines. 1 Among these, expired or unused medicines pose a particular risk due to their potential toxicity and challenges associated with their safe disposal. 2 Various pharmaceuticals have been detected in freshwater and marine ecosystems worldwide, 3 mainly due to improper disposal practices such as discarding medications in household garbage or flushing them down sinks or toilets. 4 In addition to improper disposal, other pathways contribute to pharmaceutical contamination of waterways, including human excretion of drugs in urine, and runoff from animal farms where antibiotics and hormones are extensively used. Proper medication disposal is a preventable source of contamination and, if addressed, would not add to the burden already imposed by these unavoidable mechanisms.
These practices and pathways lead to widespread contamination of water sources, affecting both human health and the ecosystems. For instance, exposure to endocrine-disrupting chemicals has been associated with adverse effects in wildlife, including reduced fertility and abnormal thyroid function in birds and fish. 5 Furthermore, antibiotics in sewage systems have raised alarms about the propagation of drug-resistant microorganisms. 6
Improper disposal practices also pose direct threats to public health. Medications discarded in household trash, particularly narcotics and sleeping pills, can be misused if accessed.2,7 Similarly, improperly stored or disposed medicines increase the risk of accidental poisonings, particularly among children. 7 In response to these risks, the U.S. Food and Drug Administration (USFDA) has established guidelines recommending structured disposal methods, including drug take-back programs and secure incineration systems.8,9 Additionally, the USFDA allows certain medicines that pose an immediate danger, such as some narcotics, to be flushed if no other disposal options are available. However, such programs are absent in Nepal, where improper medication disposal remains a significant concern. In this context, the concept of ecopharmacovigilance (EPV) has emerged, focusing on detecting, assessing, and preventing environmental risks caused by pharmaceuticals, particularly those arising from improper disposal of expired or unused medicines. 10 By encouraging safer disposal practices, EPV aims to reduce pharmaceutical pollution and protect both ecosystems and public health. 11 Incorporating EPV principles into waste management strategies is essential for minimizing expired drugs’ environmental impact, especially in countries like Nepal, where structured disposal systems are lacking.
In Nepal, households often accumulate unused or expired medications due to changes in treatment regimens, over-prescription, or poor adherence to medication therapies. 1 Unfortunately, Nepal’s healthcare waste management guidelines do not explicitly address the disposal of household pharmaceuticals. 12 Studies have shown that a lack of awareness, infrastructure, and proper guidelines leads many individuals to dispose of medication waste in municipal garbage dumps, thereby contributing to environmental pollution.13,14 While hospitals in Nepal generally use contracted services to manage pharmaceutical waste, there is no structured framework for community pharmacies or households to safely dispose of unused or expired medications. This gap is exacerbated by Nepal’s dual healthcare system, where public facilities primarily serve rural areas, and private providers dominate urban regions, creating disparities in waste management practices.
As a trusted and most accessible healthcare provider for the general public, community pharmacies can play a vital role in educating the public about safe medication disposal.15,16 This study examines the knowledge, attitudes, and practices of individuals visiting community pharmacies in Kathmandu, Nepal. The study aims to provide evidence to inform policy development, establish sustainable disposal practices, and reduce the environmental and health risks associated with improper pharmaceutical waste management by addressing this gap.
Methods
Study design and study site
A cross-sectional study was conducted at various community pharmacies in Kathmandu District, Nepal, between August 2020 and January 2021. The study duration was extended due to the national lockdown imposed by the government of Nepal to curb the spread of COVID-19. Kathmandu, the capital city of Nepal, is located in the northwestern part of Kathmandu Valley and spans ~50 km2. The district represents around one-twelfth of Nepal’s total population of ~30 million. It was selected for its accessibility to essential amenities, including healthcare and transportation, and its diverse representation of urban and semi-urban areas.
Study population
The study population comprised individuals aged 18 years or older who were visiting selected community pharmacies in the Kathmandu District. Participants were required to be able to read and speak Nepali or English. Individuals below 18 years of age and those with incomplete responses were excluded.
Sample size and sampling technique
The sample size was calculated using a single population formula:
Where n = sample size = confidence interval level (95% = 1.96), p = estimated population proportion 50%, w = margin of error (5%).
To account for potential non-responses, a total of 395 participants were recruited. Community pharmacies across different wards of Kathmandu Metropolitan City were selected using a convenient sampling method.
Study instrument
Data were collected using a structured questionnaire designed to assess knowledge, attitude, and practice regarding the disposal of unused and expired medications. The questionnaire was adapted from the Return and Disposal of Unused Medication questionnaire (Supplemental Material), a pre-validated tool developed in Malaysia. 17 The adaptation process involved thoroughly reviewing existing literature15,18 and incorporating region-specific factors to ensure its relevance to the Nepali context. This included modifying certain questions to reflect local practices and environmental conditions.
Face and content validity
The questionnaire to assess the disposal practices of unused and expired medicines was adapted from previous literature with modifications to suit the local context.8,18 It was initially developed in English, translated into Nepali by a bilingual expert, and then back-translated into English by a second bilingual expert to ensure linguistic consistency and conceptual equivalence. To establish content validity, the questionnaire was reviewed by a panel of experts in community pharmacy, clinical pharmacy research, and statistics, who provided feedback on its relevance, clarity, and appropriateness for the target population. Pretesting was conducted on 39 randomly selected participants (10% of the total sample size), and necessary adjustments were made to improve clarity and relevance based on the feedback.
Reliability test
The reliability of the questionnaire was evaluated using Cronbach’s alpha, calculated from the pretest responses of 39 participants. The alpha value was 0.71, indicating acceptable internal consistency. An alpha value of ⩾0.7 was deemed acceptable for the study instrument. 19
The final data collection questionnaire comprised five sections: socio-demographic characteristics, knowledge, attitude, practice, and actual practice of unused and expired medicines. The knowledge section comprised 10 questions with options for “True,” “False,” and “Do not know.” The attitude and practice sections included 10 questions each, using a Likert-type scale for responses. The disposal section consisted of eight questions that focused on participants’ disposal behaviors and suggestions for improvement. 17
Scoring system
To evaluate participants’ understanding of proper methods for disposing of unused and expired medicines, we assigned a score of 1 for correct responses and 0 for incorrect or “Do not know” answers. These scores were then added, and the average score was calculated. Participants scoring above this average were categorized as having “Good Knowledge,” while those scoring below were categorized as having “Poor Knowledge.” In addition to knowledge, we also assessed participants’ attitudes using a five-point Likert scale ranging from “Strongly Disagree” (1) to “Strongly Agree” (5). Similarly, participants scoring above the average were labeled as having a “Positive Attitude,” while those scoring below were categorized as having a “Negative Attitude.” Both the measurement methods for knowledge and attitude were adopted from prior studies.18,20 It’s important to note that the practice section questions were not scored but instead described descriptively.
Ethical implications
Ethical approval was obtained from the ethical board of Nepal, that is, Nepal Health Research Council (Ref no. 2283). Informed written consent was obtained from each participant before collecting the data. Participants were sufficiently informed about the purpose of the study and their role in the study before obtaining permission. The confidentiality of each participant was highly maintained.
Data collection technique
Community pharmacies were approached, and permission was secured from pharmacy owners to conduct interviews. Participants (individuals visiting community pharmacies) were recruited using convenience sampling during business hours (11:00 am–05:00 pm). Trained researchers administered the questionnaire through face-to-face interviews after explaining the study’s objectives and obtaining informed consent.
Data management and analysis
Data were coded, entered, and analyzed using Statistical Package for Social Sciences (SPSS) version 23 (SPSS, Inc., Chicago, IL, USA). Descriptive (frequencies and percentages) were used to summarize socio-demographic characteristics, knowledge, attitudes, and practices. Inferential statistics, including the Pearson chi-square test, were applied to identify associations among categorical variables. A p < 0.05 was considered statistically significant.
Results
A total of 395 individuals took part in the study. As shown in Table 1, the majority of participants were aged 18–29 and predominantly male. The sample also highlighted a significant proportion of individuals with chronic conditions in their households (n = 214, 54.2%). Table 1 presents the socio-demographic information of participants visiting community pharmacies.
Socio-demographic characteristics of respondents.
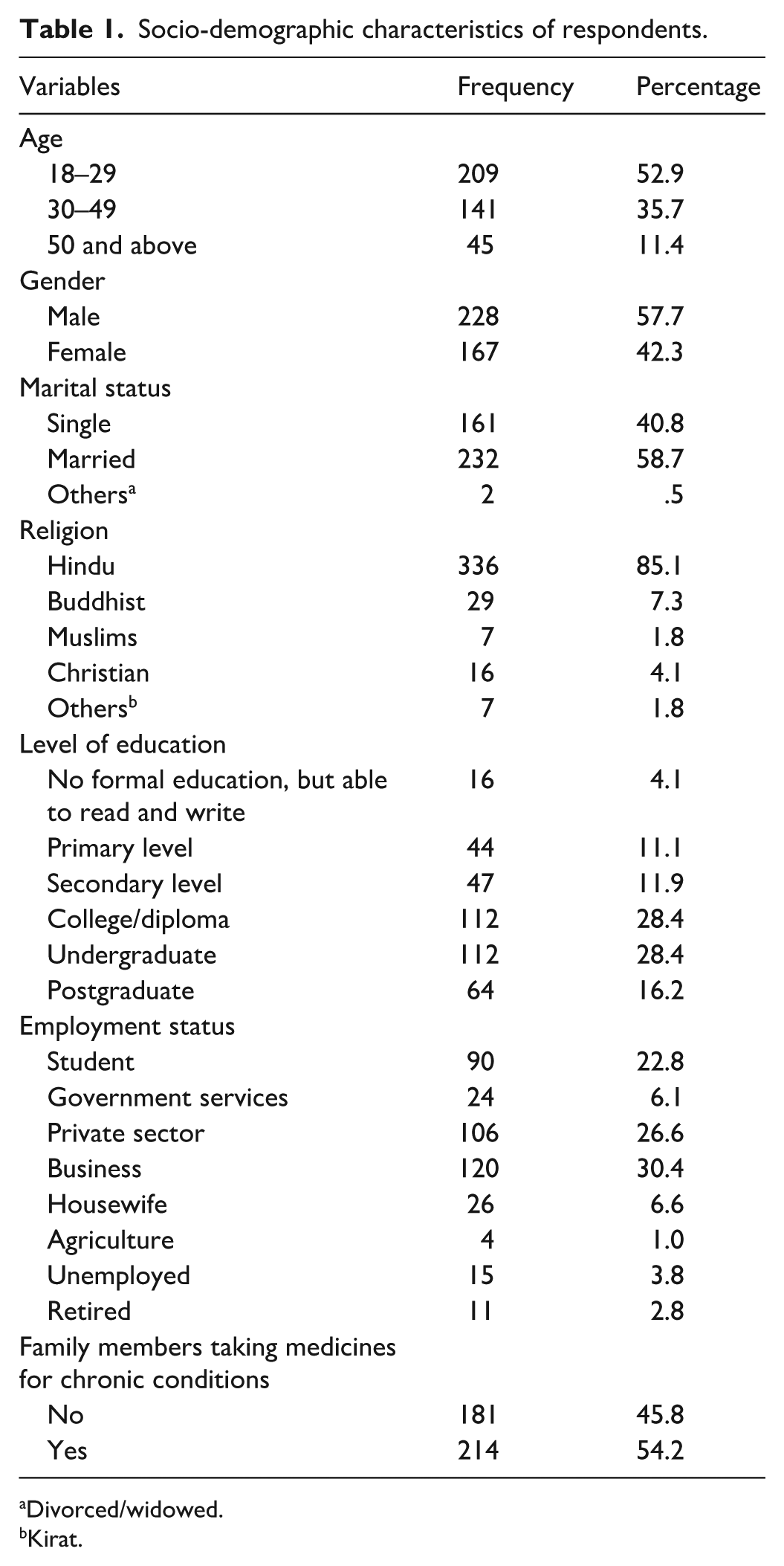
Divorced/widowed.
Kirat.
Respondent’s knowledge regarding unused and expired medication disposal
Overall, 62.53% of participants demonstrated good knowledge, while 37.46% (n = 148) had poor knowledge of proper disposal methods. The majority (88.1%, n = 348) were aware of the environmental harm caused by improper medicine disposal. Among the total respondents, 63.3% (n = 120), 69.1% (n = 131), and 72.4% (n = 137) were aware that disposing of solid medicines in the garbage, liquid medicines by pouring them down the sink, and flushing them down the toilet is unacceptable. Moreover, 79.2% (n = 313) stated that returning medicines to a pharmacy or healthcare facility was the proper disposal method, while only 29.9% (n = 118) knew about incineration as an environmentally sound disposal method. Table 2 shows the knowledge of respondents regarding disposing of unused and expired medicines.
Knowledge among respondents concerning the disposal of unused and expired medicines.

Association of demographic characteristics of the participants and their level of knowledge
There was no statistically significant association between demographic variables and knowledge levels. However, a significant association was observed between awareness of proper medicine disposal methods and knowledge level (p = 0.003). These results are presented in Table 3.
Association of demographic characteristics of the participants with their level of knowledge.

The boldfaced values indicate that the result is statistically significant.
Respondent’s attitude regarding unused and expired medicines disposal
The majority (n = 366, 92.6%) had a positive attitude towards returning and disposing of such medicines. Most respondents agreed that they were responsible for protecting the environment (n = 365, 92.4%), living species on earth (n = 356, 90.2%), and their family members (n = 356, 90.1%) from unintended exposure to unused/expired medicines. Additionally, 65.5% (n = 258) expressed willingness to donate unused medicines to reduce wastage, and 62% (n = 229) shared excess medicine with others. Media reports and campaigns were believed to influence 61.4% (n = 242) of respondents in returning unused medicines, while 66.6% (n = 263) agreed that monetary incentives could further encourage them to return unused medicines. Table 4 showcases respondents’ attitudes towards disposing of unused and expired medicines.
Respondents’ attitude towards unused and expired medicine disposal.

Association of demographic characteristics of the participants and their level of attitude
A significant association between demographic factors such as education level and participants’ attitudes toward proper medication disposal (p = 0.006) was found (Table 5). Participants with higher education levels and males tended to have a more positive attitude towards disposing of unused and expired household medicines.
Association of demographic characteristics of the participants and their level of attitude.

Divorced/separated.
Kirat.
The boldfaced values signifies that the result is statistically significant.
Respondent’s disposal practice of unused and expired medicines
Respondents acknowledged having unused medicines because they ceased taking them when they felt better (n = 249, 63%) or when the doctor altered the treatment (n = 202, 40.11%), or when they didn’t experience the expected improvement (n = 196, 44.8%). However, 42% (n = 164) of respondents reported having unused medicines due to unwanted side effects, followed by 52.1% (n = 121) citing non-adherence. Over half of the respondents (n = 198, 52.2%) agreed they should retain medicines they no longer need for future use. Concerning medicine disposal, respondents indicated that they dispose of medicines when they expire (n = 309, 78.2%), when they experience unwanted side effects (n = 171, 43.3%), when medicines deteriorate in smell, taste, or appearance (n = 180, 45.6%), and when medicines spoil due to improper storage (n = 242, 61.3%; Table 6).
Respondent’s disposal practice of unused and expired medicines.

Actual disposal practice of unused and expired medicines disposal
The most favored method of disposing of expired medicines was throwing them in the household garbage or rubbish bin (Figure 1). The majority of respondents (51.02%) kept unused medicines at home until they expired, followed by disposal in the rubbish bin (36.22%) and returning them to the pharmacy (36.73%; Figure 2).

Method of disposal of unused medicines, N = 395.

Method of disposal of expired medicines, N = 395.
Of the 395 respondents, ~43% (n = 171) reported having unused medicines stored at home. The majority of respondents (n = 286, 72.4%) indicated that they were unaware of the correct method for medicine disposal, and 82% (n = 324) stated that their healthcare provider had never advised them on the proper disposal method for unused or expired medicines. The most common types of medicines kept in households were antipyretics (52.1%), followed by analgesics (46.7%), and antibiotics (42%). Reasons for having unused medicines at home included self-discontinuation (50.29%), excessive purchase of medicines for future use (39.18%), and medicines reaching their expiration date (31.58%; Table 7). Nearly all respondents (n = 383, 97%) believed awareness campaigns on properly managing unused or expired household medicines were necessary. When asked about the most effective medium for conducting such awareness programs, 42.3% (n = 162) of participants preferred community pharmacies as the primary channel for educating patients on proper medicine disposal methods.
Reasons for having unused medicines, N = 171.
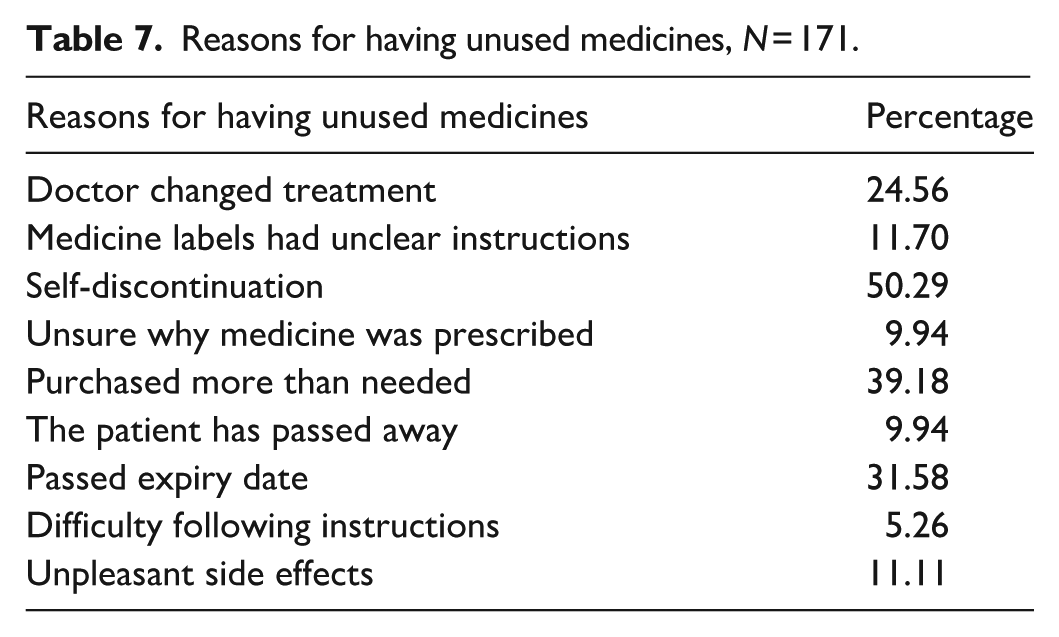

Association of knowledge and actual disposal practice of expired medicines
There is a significant correlation between respondents’ knowledge of medicine disposal methods and their actual practices (p < 0.001). Among those unaware that discarding unused or expired medicines in the rubbish bin was unacceptable, 93% (n = 44) disposed of them in their household bins, compared to 64.45% of those aware of the inappropriate method. While about 80% (n = 248) understood that returning medicines to a pharmacy or healthcare facility was acceptable, only 20.76% (n = 65) did so (Table 8).
Association of knowledge and actual disposal practice of expired medicines.

The boldfaced values signifies that the result is statistically significant.
Discussion
The improper disposal of unused and expired medications is a growing public health and environmental concern,21,22 particularly in low- and middle-income countries like Nepal, where formal medicine take-back systems are lacking. Although a significant portion of manufactured pharmaceuticals remains unused and ultimately expires, most households lack the knowledge or means to dispose of them safely. Without structured disposal mechanisms, such medicines are often discarded inappropriately, typically through household waste—raising serious risks of environmental contamination and accidental exposure. While the findings of this study indicate that participants generally possessed a reasonable level of knowledge and a positive attitude toward safe disposal, their actual practices were inconsistent with this awareness, reflecting a gap between knowledge and behavior. These results align with previous studies in Nepal and India, which similarly reported that household waste bins were the most common disposal route.23,24
Approximately 62% of respondents in our study demonstrated good knowledge of proper medication disposal methods, slightly higher than the findings from Northern Ethiopia. 20 A majority of participants recognized the environmental harm caused by improper disposal, consistent with studies conducted in Malaysia (89.2%), Iraq (84%), and Indonesia (82.75%).18,25,26 However, knowledge levels in our study were lower compared to Ethiopia (91.4%) and Kabul, Afghanistan (98%),15,27 possibly due to differences in awareness campaigns or public education initiatives across these regions.
Despite a good overall understanding, fewer respondents were aware of environmentally safe methods such as returning medications to pharmacies or healthcare facilities. This is consistent with findings from Kuwait, the USA, and Malaysia18,28,29 which highlight the need for stakeholder engagement and public education to promote proper pharmaceutical waste management.
The study revealed a predominantly positive attitude towards responsible disposal practices. Over 90% of participants acknowledged their responsibility to protect the environment, wildlife, and children from the adverse effects of pharmaceutical waste, aligning with findings from studies conducted in India 30 and Malaysia. 18
However, attitudes towards medication sharing and donation varied across cultural contexts. For instance, in some regions, sharing unused medications is seen as acceptable31,32 despite the associated risks of self-medication and drug misuse.
Many respondents (61%) indicated that media reports influenced their attitudes, and 67% believed monetary incentives could encourage proper disposal behaviors. These findings highlight the potential of targeted awareness campaigns and incentive-based programs to drive behavioral changes, as observed in Malaysia. 18
Despite high knowledge and positive attitudes, disposal practices among respondents were inadequate. Less than half reported storing unused medications at home, a lower prevalence than findings from Indonesia, India, and Afghanistan.15,25,33 Common reasons for retaining included self-discontinuation of treatments and purchasing excess supplies for future use, 34 emphasizing the need to educate patients on adherence to prescribed regimens and the risks of self-medication.
Studies conducted in Northern India, Indonesia, Ghana, and New Zealand reported similar reasons for having unused and leftover medicines at home.25,34–36 This result implies the lack of awareness among consumers of the importance of compliance with therapy and the dangers of self-medication without consultation with a healthcare provider. Furthermore, having unused and excess medicines promotes self-medication and increases the risk of accidental childhood ingestion and the issue of inappropriate disposal.36,37 Therefore, patient education, especially among pharmacists and prescribers, is recommended.
The majority of participants in our study (72%) were unaware of the proper methods for medicine disposal, higher than reported in Ahmedabad, India (61%). 23 This lack of awareness likely contributes to the widespread practice of discarding expired medications in household garbage, which was also observed in studies from 23 Bangladesh, Indonesia, Afghanistan, and Poland.15,25,38,39 Such practices pose significant risks to ecosystems, as medications can leach into soil and water systems, endangering public health. 40
In contrast, countries with established systems, such as Sweden, report higher compliance with safe disposal methods due to accessible medication take-back programs and robust public awareness campaigns. 9 Nepal’s lack of similar infrastructure and awareness initiatives highlights the need for structured interventions to promote proper disposal practices.
Our study identified a significant association between respondents’ knowledge and their disposal practices. While most participants were aware that disposing of medications in trash bins was improper, 64% still did so. This aligns with findings from Malaysia, where well-informed respondents exhibited a gap between knowledge and practice. 18 This may be due to a lack of convenient disposal options, insufficient or weak enforcement of proper disposal practices.
Similarly, although 80% of respondents believed returning medications to pharmacies was appropriate, only 18% reported doing so, reflecting barriers to action due to a lack of accessible disposal options. 41
Our study found no significant association between socio-demographic variables and participants’ knowledge levels. This contrasts with findings from Adigrat City, Ethiopia, where age and education significantly influenced knowledge. 20 However, awareness of proper disposal methods was strongly associated with higher education levels, emphasizing the importance of educational outreach in promoting better practices.
Limitations
This study has several limitations. First, it was conducted exclusively in selected community pharmacies in Kathmandu, potentially limiting the generalizability of findings to other regions of Nepal. As an urban district, Kathmandu may not reflect the behaviors and practices of rural populations. Second, reliance on self-reported data introduces the risk of recall and social desirability biases. Finally, the cross-sectional design limits our ability to establish causal relationships. Future studies should employ diverse sampling methods and objective measures of disposal practices to gain a more comprehensive understanding.
Recommendation
The findings underscore the need for comprehensive interventions to address gaps in knowledge and practice. Policymakers should prioritize the development of national guidelines and establish medication take-back programs to ensure safe disposal.42,43 Healthcare professionals, particularly pharmacists, can be pivotal in raising public awareness and guiding patients on appropriate disposal methods.14,18,44–47 Community-led initiatives, supported by media campaigns and government programs, can further foster sustainable disposal practices and promote environmental stewardship. 40
Conclusion
While many participants demonstrated good knowledge and a positive attitude toward the proper disposal of unused and expired medications, a significant gap persists between awareness and actual practices. This disconnect highlights the urgent need to establish effective drug take-back programs and the development of national guidelines for safe pharmaceutical waste disposal. Healthcare professionals should be central in leading public education and awareness initiatives. Additionally, further research with a larger sample size and a more diverse sample is essential to inform evidence-based policies and legislative efforts to improve medication disposal practices.
Supplemental Material
sj-docx-1-smo-10.1177_20503121251375355 – Supplemental material for Disposal of unused and expired medications: A study of knowledge, attitudes, and practices among community pharmacy visitors
Supplemental material, sj-docx-1-smo-10.1177_20503121251375355 for Disposal of unused and expired medications: A study of knowledge, attitudes, and practices among community pharmacy visitors by Januka Khatri, Rajani Shakya, Ranish Shrestha and Sunil Shrestha in SAGE Open Medicine
Supplemental Material
sj-docx-2-smo-10.1177_20503121251375355 – Supplemental material for Disposal of unused and expired medications: A study of knowledge, attitudes, and practices among community pharmacy visitors
Supplemental material, sj-docx-2-smo-10.1177_20503121251375355 for Disposal of unused and expired medications: A study of knowledge, attitudes, and practices among community pharmacy visitors by Januka Khatri, Rajani Shakya, Ranish Shrestha and Sunil Shrestha in SAGE Open Medicine
Footnotes
Acknowledgements
The authors thank Dr. Saval Khanal (King’s College London) and Dr. Sujata Sapkota (Manmohan Memorial) for their comments and insightful suggestions while finalizing the research questionnaire and final article.
Ethical considerations
Ethical approval was obtained from the Nepal Health Research Council (NHRC; Ref no. 2283). Informed written consent was obtained from each participant before collecting the data. Participants were sufficiently informed about the purpose of the study and their role in the study before obtaining permission. The confidentiality of each participant was highly maintained.
Consent to participate
Written informed consent was obtained from all subjects before the study.
Author contributions
Januka Khatri conceptualized the idea of this article, did a literature review, and wrote the initial draft. Rajani Shakya made substantial changes in the conception, provided intellectual feedback to the concept of the study, and supervised the study. Ranish Shrestha contributed to the critical review of the manuscript and made necessary changes to the final version of the article. Sunil Shrestha provided intellectual feedback during the conceptualization of the study, did a literature review and also provided a critical review of the manuscript.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data availability statement
The datasets used and/or analyzed during the current study are available from the corresponding author upon reasonable request.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.

