Abstract
Background:
Nasogastric tube (NGT) insertion is one of the most commonly performed procedures for critically ill patients through the nostril or mouth into the stomach, which is indicated for multiple reasons.
Objective:
This study is, therefore, aimed to enhance the NGT insertion skill performance of third-year nursing students using the updated checklist, 2021.
Method:
A facility-based pre-post intervention study was conducted among third-year nursing students of the School of Nursing, Jimma University. An updated checklist and intervention package were used among 26 randomly selected nursing students. The collected data was entered into EpiData version 3.1, EpiData Association, Denmark and exported to SPSS version 23, IBM Corp, Armonk, NewYork for analysis. Descriptive statistics were made for each item and Paired T-test analysis was conducted to summarize the findings.
Result:
The highest NGT skill insertion performance score from 40% before the intervention was 35; however, after the intervention, the score increased to 40.3. Their mean score in NGT skill performance was increased by 11 after the intervention of implementing the intervention package using the updated checklist from 26.5 ±5 0.3 the pre-intervention to 37.8 ±5 1.7 post-intervention. The finding indicated that the improvement was statistically significant at p < 0.001.
Conclusion:
Implementing an intervention package and employing an updated NGT insertion checklist improved the performance of third-year nursing students’ NGT insertion skills by an average of 11 points compared to their pre-test scores. A large-scale control randomized trial study was recommended to control for the effects of confounding factors on the implementation of intervention packages.
Introduction
Nasogastric tube (NGT) insertion is one of the most commonly performed procedures for critically ill patients through the nostril or mouth into the stomach, which is indicated for multiple reasons like abdominal operation, feeding, medication administration, comatose, and gastric decompression.1–5 Most of the time anatomic landmarks are commonly used to facilitate NGT insertion. 6 SORT is a mnemonic term that represents four main steps of the maneuver, namely: Sniffing position, NGT Orientation, contralateral Rotation, and Twisting movement. 3
Technically, NGT insertion starts by measuring from the nose to the ear lobe to the xiphoid process of the sternum or from the forehead to the xiphoid process that students are frequently taught in nursing schools.7–9 The routine way for NGT insertion is the blind technique that means the nurse cannot see where the tube is going as it passes out of sight through the patient’s nose and throat. 10 Thus, the placement and patency of NGTs should be checked before administration of medication, commencement of feeding, or decompression.11,12
Although the vast majority of blind NGT insertions result in successful placement in the intended location—the stomach—each tube can potentially be misplaced, even when the procedure is performed by an experienced professional that compromises patient safety, increasing the risk for severe and even fatal complications.13–16 So, confirmation is mandatory to minimize the risks related to misplacements before the administration of dietary tube feedings, medications, and decompressions.17,18 The position of the NGT is verified through different techniques such as auscultation of an air bolus, observation of abdominal content by aspiration, and pH measurement of aspirated fluids.1,10 Most of the bedside verification methods do not allow the detection of improper positioning of NGTs within the gastrointestinal tract, thus increasing aspiration risk. 19 So, the “gold standard” method, radiation (x-ray, Computed tomography) is the best indication to confirm its final position.16,20
Insertion of an NGT in an anesthetized, comatose, and intubated patient is not always as easy as in a conscious, cooperative patient as they cannot follow the swallowing instructions, and thus has a high failure in the first attempt of insertion.10,21 Therefore, nurses must adhere to standard nursing protocols on NGT insertion to maintain patients’ physiological and nutritional status of patients. 22
NGT insertion is one of the common clinical procedures carried out by nurses in health institutions in all groups of patients, from neonates to older people.3,23
Though the clinical implications of misplaced NGTs are well addressed, the nonclinical implications are significant and often occur indirectly. These nonclinical implications may include a compromised hospital reputation and cause economic losses. 24
The Actionable Patient Safety Solutions from the Patient Safety Movement Foundation lays out best standard practices for the implementation of NGT placement protocols in health institutions to ensure consistency across the organization and preserve patient safety at the forefront of all clinical endeavors. 24
Despite the reality that nursing education is a practice-based profession and it is program had a demonstration and practice session to provide an opportunity for students to over and over practice required competencies in a conducive working environment without fear of hurting patients, some gaps may occur during the class demonstration, and professional practicing period.25,26 The demonstration and clinical attachment play a critical role in the integration of the theory or knowledge, skills, and clinical judgment.27–29
Nursing performance is evaluated by the needs of patients and reflects an integration of knowledge, skills, and experience. 30 Understanding the basic concept in nursing practice with a specific standard checklist is used to enhance students’ performance. 31 Students should know about NGT size selection, assessment of tube position, and ways of inserting a tube and confirmation. 32 Therefore, giving the correct patient’s position, checking the patency of the tube, checking the food content, and auscultation of the bowel sounds are critical components to play down the dangers of NGT-related complications and to provide optimal patient safety and comfort.
As a nursing school and Jimma University Medical Center (JUMC), there is a standard checklist to insert an NGT and it is expected that students will gain the knowledge and skills necessary to perform NGT insertion during their education. Upon graduation, they will gain competence under the guidance of a preceptor until they can complete the procedure independently. Thus, this study is aimed to enhance the students’ performance of NGT insertion using a standard checklist.
Materials and methods
Study design and setting
A facility-based pre-post intervention study was employed at Jimma University, Institute of Health, Facultyof Health Sciences, School of Nursing. Jimma University was founded in 1930 G.C., which is located in Jimma town, 355 km to the south-west of Addis Ababa. In the 2021 academic year, there were 60 third-year nursing students. The study was conducted from February 28, 2021, to March 03, 2021.
Participants
Randomly selected third-year nursing students who were available at the demonstration room per our call, able to respond to the skill performance checklists, and who were volunteers to take part in this study.
Inclusion and exclusion criteria
Study participants who completed the debriefing, demonstration, and re-demonstration sessions of the NGT placement and had both pre-test and post-test findings were included. Those who did not fulfill the stated criteria were excluded from the study.
Sample size determination and sampling technique
The sample size was computed using G*Power 3.1.9.4 with the following assumptions: 95% confidence interval, 80% power, the maximum percentage of outcome score using the prior checklist 35%, 5% effect size, and a final estimated sample size of 26. The calculated sample of students was randomly selected using their registration list as the sampling frame.
Data collection instrument
A structured NGT checklist developed after reviewing relevant literature was used for students’ NGT insertion performance skill assessment. The original checklist contained 19 items and was prepared in English. The newly developed NGT checklist was pretested on the 5% of the calculated sample size for reliability assurance
Data collection procedure and intervention strategies/packages
Initially, the procedure was debrief students on the contents and items of the newly developed NGT insertion checklist, then demonstrated the procedure for them, and gave a chance for some of the students to re-demonstrate the procedure for the rest of the students. Finally, students’ skill performance was assessed using the updated NGT checklists (Table 1).
Intervention packages used for enhancing NGT insertion skill performance of nursing students.

NGT: Nasogastric tube; PIs: Principal Investigators: NA: Not Applicable.
Data analysis and presentations
The collected data was entered into EpiData version 3.1 and exported to SPSS version 23, for analysis. Descriptive statistics were made for each item. For testing the score difference for the student’s skill performance from using the routine and updated NGT insertion checklists, total item score, minimum, maximum, mean, and standard deviations were computed for each item and comparisons were made for pre- and post-intervention skill performances of the students. A paired samples T-test was used to compare the pre-test and post-test mean score differences of the participants. The statistical significance was reported at p-value < 0.05. The findings of the data were presented using statements and figures.
Data quality assurance
Data was collected using the pre-tested and validated checklists. Before and after the pre-test data collection, and before the actual students’ skill assessment principal investigators discussed each checklist item, any unclear parts of items were made clear for them by the team leader, and reached to consensus on its clarity, on a similar assessment, and scoring procedures and then debriefed it for the students. Additionally, based on the pre-test findings, the items of the new checklist were re-checked and amended by the teams.
Result
Participants’ socio-demographic characteristics
The mean age of the study’s participants was 22.19, with a standard deviation of ±1.38. Other sociodemographic details were presented in Table 2.
Socio-demographic characteristics of study participants.

Pre-intervention NGT insertion skill performance was conducted on third-year nursing students using the routine NGT skill performance checklist containing 19 items, and the highest students’ skill performance score of 40% was 35 while the lowest score was 18 (Figure 1).

Pre-intervention NGT insertion skill performance scores among nursing students.
After the intervention, the NGT insertion skill performance of third-year nursing students was enhanced to 40.3 with the lowest score of 33.6 (Figure 2).

Post-intervention NGT insertion skill performance scores among nursing students.
Enhancement in NGT insertion skill performance among third-year nursing students
The mean score in NGT skill performance of third-year nursing students was increased by 11 after the intervention from 26.5 ±5 5.3 the pre-intervention to 37.8 ±5 1.7 post-intervention (Figure 3).

Comparisons in NGT insertion skill performance score before and after intervention.
The improvement was statistically significant; (t (25) = 13, p < 0.001 at 95% CI (−14.27, −7.72). Similarly, students’ NGT insertion skill performance enhanced across all items of the checklists after the intervention compared to the pre-intervention items’ scores. They score more on the item preparing the tube, moderate on the item measuring the tube (both pre-test and post-test), and less on the item washing hands and explaining the procedure for the patients at post- and pre-test phases respectively (Figure 4).
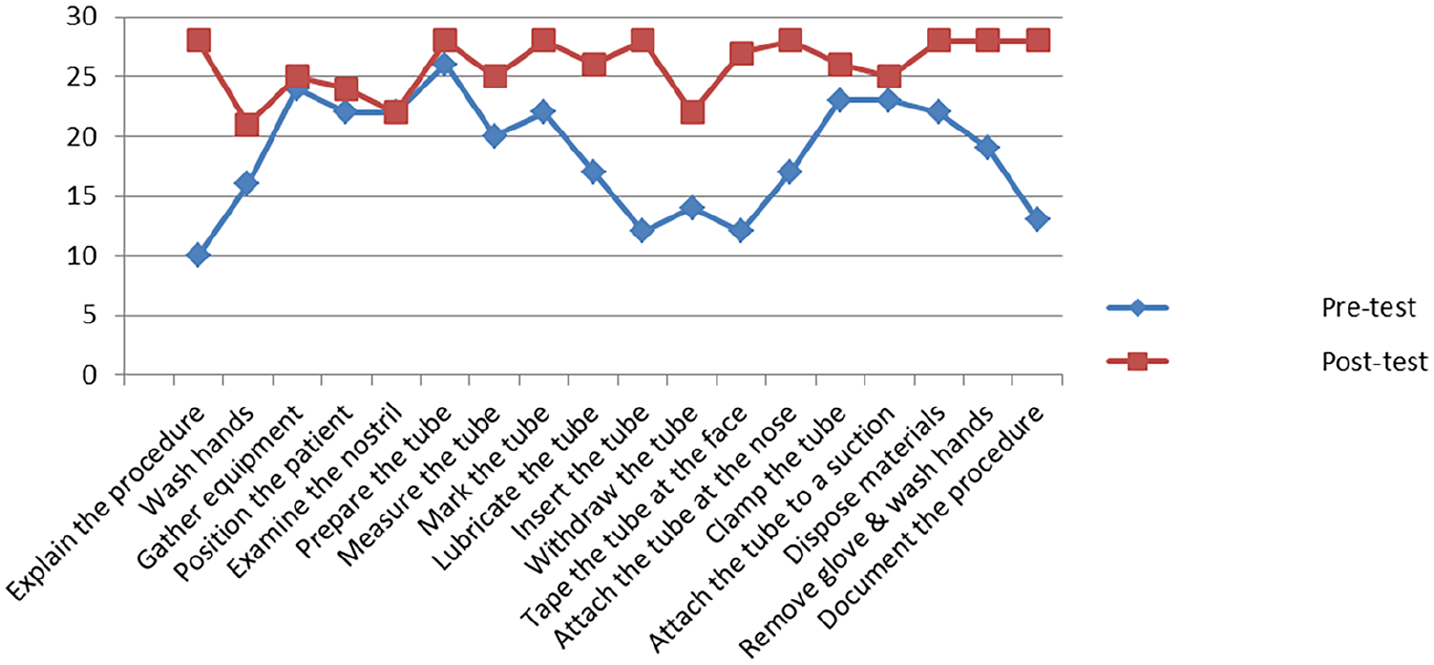
Students’ NGT insertion items score trends before and after the intervention.
Discussion
In this study, the pre-post interventional study was conducted to enhance third-year nursing students’ NGT insertion skill performance. Post-intervention scores of students’ NGT skill performance, mean scores, and scores on each item were dramatically enhanced. In our recent study, the mean NGT skill performance of students after the intervention was 37.8 ±5 1.7, indicating a drastically enhanced NGT skill performance among students compared to their pre-intervention mean scores. This enhancement in NGT skill performance among nursing students is contributed by the intervention packages we implemented. However, the study conducted in North America on NGT insertion performance assessment of NGT feeding in ICU on an unconscious intubated patient showed, that the mean score performance of nurses in NGT feeding was 57.49 ±5 9.58. 33 This discrepancy in mean score might be attributed to the differences in study areas, types of patients on which the NGT skill was performed, by whom the skill was performed, and the purpose of the NGT skill performance between the recent and the previous studies.
In this study, students performed moderately on the “measure the tube” item of the NGT insertion skill performance both before and after the intervention. This is because, in both performances, students used the similar landmark of nose–ear–xiphoid for NGT length measurement before its insertion. This was consistent with the previous studies indicating that 36.2% of nurses used nose–ear–xiphoid measurement to define the internal length of the NGT, while, according to the multicenter cross-sectional survey in China, nearly all (98.5%) nurses used nose–ear–xiphoid or for head-xiphoid measurement alone or in combination. 34
Limitations of the study
One of the limitations of this study was the lack of a control group. Another limitation is a small sample size of previous students’ NGT insertion skill performance for pre-test data, and the effects of other confounding factors on the outcome variable. Moreover, the comparison to a previous study on NGT insertion performance assessment done in North America may not be directly comparable due to differences in study areas, demographics, and settings. A large-scale control randomized trial study was recommended to control for the effects of confounding factors on the implementation of intervention packages.
Conclusion
In this study, the third-year nursing students’ NGT insertion skill performance was enhanced by 11 from the pre-test scores by implementing an intervention package and using an updated NGT insertion checklist.
Supplemental Material
sj-docx-1-smo-10.1177_20503121241255265 – Supplemental material for Enhancing nasogastric tube insertion skill performance by using updated checklist among nursing students
Supplemental material, sj-docx-1-smo-10.1177_20503121241255265 for Enhancing nasogastric tube insertion skill performance by using updated checklist among nursing students by Ebissa Bayana Kebede, Yonas Biratu Terfa, Abebaw Tiruneh, Enatfanta Sehumehone and Bekana Fekecha in SAGE Open Medicine
Footnotes
Acknowledgements
We would like to thank Jimma University, School of Nursing and the participants of the study for their outstanding efforts and support in the implementation of our study.
Author contributions
EBK contributed starting from its conception, study design, execution, data acquisition, analysis, and interpretation and took part in drafting and critically reviewing the article. YBT contributed starting from its conception, study design, execution, data acquisition, interpretation, and critically reviewing the article. AT contributed starting from its conception, execution, study design, and critically reviewing the article. EF contributed starting from its conception, study design, execution, and critically reviewing the article. BF contributed starting from its conception, study design, execution, analysis, interpretation, and critical reviewing the article. Finally, all authors gave final approval to the article and agreed to be published.
Data availability
Data used for this manuscript is included in the manuscript.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethics approval and consent to participate
The study was submitted to the committee of the higher diploma program at Jimma University for ethical approval. Participants were informed clearly about the objective of the study, anonymity and confidentiality of their information, privacy, their volunteer participation, and benefits of the study. Participants’ right to refuse to participate in the study was assured. Finally, participants’ verbal informed consent was secured before they participated in the study because the higher diploma program committee approved the study to be conducted in such a way.
Informed consent
Verbal informed consent was obtained from all subjects before the study.
Trial registration
Not applicable.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
