Abstract
Introduction:
The average age and survival of heart transplant recipients have improved significantly over the last 10 years. In these long-term survivors, coronary allograft vasculopathy is one of the most common causes of death. There is a paucity of large-data research highlighting the short-term outcomes of percutaneous coronary interventions in cardiac allograft recipients.
Methods:
We compared the in-hospital outcomes of heart transplant recipient and non-transplant recipients following percutaneous coronary intervention using data from the National inpatient sample (NIS). All adult patients (age ⩾ 18 years) who had percutaneous coronary intervention in the index admissions from January of 2005 to December of 2014 were included in the analysis. They were then divided into two groups based on their heart transplant status. The primary outcome was in-hospital mortality. Secondary outcomes were stroke, cardiac arrest, duration of hospitalization, and total hospital charges. Logistic regression models were used to compare in-hospital outcomes between the two groups.
Results:
Of 1,316,528 patients who had percutaneous coronary intervention, 618 (0.05%) were heart transplant recipients and 1,315,910 (99.95%) were not. The heart transplant recipient group was significantly younger with lower rates of obesity and peripheral vascular disease but higher rate of chronic kidney disease, iron deficiency anemia, and chronic liver disease. There was significantly higher in-hospital mortality in transplant recipients below 65 years of age (adjusted odds ration = 2.3,
Conclusion:
Heart transplant recipients younger than 65 years had higher in-hospital mortality. Subjects in the heart transplant recipient group were also younger and had longer duration of hospitalization than the non-transplant cohorts.
Keywords
Introduction
The average age and survival of heart transplant recipients (HTR) have improved significantly over the last 10 years. 1 The median survival in adult recipients of heart transplant is currently around 11 years. 2 In these long-term survivors, coronary allograft vasculopathy (CAV) is an important cause of death. 2 Varying severity of CAV has been found in more than 40% of HTRs after 5 years of heart transplantation. 3 Five-year survival in patients with CAV has been found to be less than 20% in some studies. 4 According to a 2014 report of the International Society for Heart and Lung Transplantation (ISHLT), CAV and allograft failure caused one-third of all deaths by 5 years after cardiac transplantation. 2
Multiple mechanisms and processes have been suggested to explain the pathogenesis of CAV. Prominent among these is the influence of acquired immune system as well as responses to infectious agents like the cytomegalovirus (CMV). 5
Percutaneous coronary interventional procedures are often used in the treatment of select patients with CAV. There is a paucity of large-data research highlighting the short-term outcomes of percutaneous coronary interventions (PCIs) in cardiac allograft recipients. The presence of multiple medical and psychiatric comorbidities have been suspected to play key roles in long-term outcomes in these patients. 2 It is not clear how these factors impact short-term outcomes following PCI.
We studied the National Inpatient Sample (NIS) to determine the in-hospital outcomes of patients with CAV treated with PCI.
Methods
Approval for the study was sought from the Institutional Review Board (IRB) at McLaren Regional Medical Center, Flint Michigan. The study was determined to be a non-human study and exempted from IRB review as the authors had no access to the patients, and the de-identified data are publicly available.
The authors performed secondary analysis of the NIS (the largest publicly available all-payer in-patient healthcare database in the United States of America) to determine the impact of heart transplant status on in-hospital outcomes following PCI.
The main objective was to determine in-hospital mortality in patients with CAV following treatment with PCI. This was then compared with in-hospital mortality in patients with native hearts who also had PCI. Other outcomes determined and compared included in-hospital stroke, cardiac arrest, duration, and charges of hospitalization.
Inclusion and exclusion criteria
All adult patients (aged 18 and above) who had PCI in the index admissions from January 2005 to December 2014 were included in the analysis irrespective of their heart transplant status. The authors excluded patients who were younger than 18 years and those who did not have PCI during the index admissions. The subjects were then classified into HTR and non-transplant recipient (NTP). We extracted the baseline characteristics using the ICD-9 codes as well as comorbid and demographic variables already made available in the database. 6 Burden of comorbid conditions was assessed in both groups using the Elixhauser score. 7
Statistical analysis
All statistical analyses were performed with statistical analysis system (SAS) software version 9.4, SAS institute, Cary, North Carolina, USA, using survey procedures accounting for weighting and nesting of variables in a clustered, probability sampling design. 8
Continuous variables were presented as mean and standard deviations when the distribution was normal. Otherwise, median and interquartile range were used. Categorical variables were presented as percentages.
Multivariate logistic regression models were utilized to compare outcomes between the two groups. Subgroup analysis was also done to determine the effect of age on in-hospital mortality. We used variance inflation factor to remove redundant variables as a result of collinearity, otherwise, variables that are shown to have statistical significance were included in the multivariate model. Analyses were done putting into consideration the sampling methods. All reported analyses were two tailed, and statistical significance was set at
Results
There were 1,316,528 patients in the study, 618 (0.05%) of them were HTR and 1,315,910 (99.95%) were NTP. Table 1 shows the baseline characteristics. Patients in the transplant group were significantly younger with mean age of 54.9 years compared to 64.5 years (
Baseline characteristics of patients after PCI by transplant status.

HTR: heart transplant recipients; NTP: non-transplant recipients; SE: mean Elixhauser score.
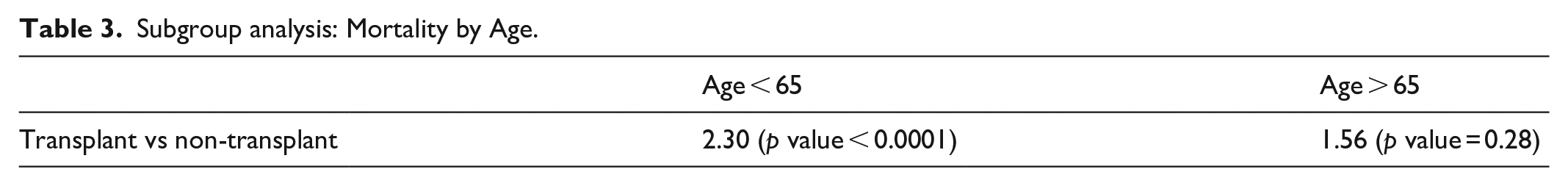
Tables 2 and 3 depict the clinical outcomes. The primary outcome of in-hospital mortality was higher in the HTR group, only reaching statistical significance in those younger than 65 years (adjusted odds ratio (aOR) = 2.3,
Multivariate adjusted model predicting different clinical outcomes by patients’ transplant status.

HTR: heart transplant recipients; NTP: non-transplant recipients.
aOR: adjusted odd ratio for categorical variables.
MD: adjusted mean difference for continuous variable.
Length of stay among those that survived till hospital discharge.
Subgroup analysis: Mortality by Age.
Discussion
In this study using a national database, there was significantly higher in-hospital mortality in HTR following PCI compared to NTP in those younger than 65 years. This was not statistically significant in cohorts above the age of 65 years. This contrasts with findings from previous studies. Dasari et al. found similar rates of in-hospital mortality in the NTP and HTR groups in an analysis of another database. 9 A study based on the National Readmissions Database by Enezate et al. also found similar mortality rates in the HTR and NTP groups following admissions for acute myocardial infarctions (AMIs). 10 The higher rate of all-cause in-hospital mortality in HTR found in this study likely resulted from an interplay of many factors.
IDA was more prevalent in the transplant group. An earlier study found IDA in about one-third of HTRs. 11 The high incidence of IDA in this category of patients may be related to chronic immunosuppression. Another possible explanation for anemia is higher prevalence of malignancies in transplant recipients. Results from studies evaluating the impact of anemia on outcomes of PCI have been mixed. Some have demonstrated worse mortality, while others found no mortality difference between anemic and non-anemic patients following PCI.12,13 Almost all the available studies are in agreement that anemic patients have more comorbid conditions compared to their non-anemic counterparts. 14 This may tilt the scale of survival away from the anemic patients.
HTRs had higher prevalence of chronic kidney disease (CKD). Previous studies also demonstrated this. 15 In addition, this study showed a significantly higher incidence of AKI in the transplant group. This may be related to the higher prevalence of CKD and maintenance dialysis in the transplant group. CKD, AKI, and maintenance dialysis have been independently shown to contribute to worse in-hospital and long-term outcomes following PCI.16,17
In this study, CLD was more prevalent in the transplant group compared to the NTPs. Previous studies have mixed results regarding the impact of CLD on the prognosis of patients with AMI and those who had PCI. The Kyoto model linked liver cirrhosis to adverse outcomes in patients who underwent PCI. 18
Another study found that chronic hepatitis B infection is associated with poorer outcomes following acute coronary syndrome (ACS) only in women. 19 Therefore, the higher prevalence of CLD in the HTR group may be one of the factors responsible for the higher mortality rate in that group.
Previous studies have suggested an association between CMV infection and development of CAV. 20 According to a study by Klimczak–Tomaniak et al., this is especially true in those who have breakthrough CMV infections after transplantation. 21 There are still uncertainties about the impact of CMV on mortality in those who already developed CAV. 5
On the other hand, comorbid conditions like dyslipidemia, hypothyroidism, PVD, and obesity were found more commonly in the non-transplant group. This is likely to have resulted from closer follow-up and risk modification in the transplant group. There is a paucity of data in the literature on the effects of dyslipidemia on in-hospital or short-term outcomes following PCI but use of lipid lowering medications especially the statins have been shown to improve long-term outcomes following ACS.22,23
PVD has been linked with worse in-hospital outcomes including in-hospital mortality following PCI. 24 This is true irrespective of the type of stent deployed during the procedure. The prevalence of PVD rises with age. This fact, together with other risk factors may be one of the reasons for the similarity in mortality rates above the of 65 years.
Conclusion
In the study, there was a higher incidence of in-hospital mortality in HTRs after undergoing PCI. This may be a result of an interplay between many factors as IDA, CKD, and CLD were more common in the transplant group while more traditional cardiovascular comorbidities like PVD, dyslipidemia, and obesity were more prevalent in the non-transplant group. More studies are needed to determine how each of the factors contributes to post-PCI outcomes and also to assess how modification of these factors would affect clinical outcomes.
Limitations
Limitations of this study include its non-randomized nature. The researchers did not have access to some baseline characteristics and data on severity of coronary artery disease (CAD) in the subjects. Sample size determination and power calculation were not done as survey data were utilized for this study. However, analyses were made to reflect nationwide distribution. The authors attempted to limit the effects of confounders with the use of logistic regression models as well as subgroup analysis.
Footnotes
Acknowledgements
The authors acknowledge the support of Dr. Parul Sud and Dr. Andrew Champine of Michigan State University and McLaren Regional Medical Center, Flint for their support toward the completion of this project.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical approval
Ethical approval for this study was waived by * Institutional Review Board at McLaren Regional Medical Center, Flint, Michigan* because the study was determined to be non-human as it involved no direct interaction with patients or their identifiers.
Informed consent
Informed consent was not sought for this study because the data used for the study are publicly available, and the authors had no access to the patients or their identifiers. This requirement was waived by the IRB.
