Abstract
Objectives:
Rheumatoid arthritis is a chronic inflammatory autoimmune disease. This study aimed to determine the association of interleukin-17A-197G/A polymorphism with rheumatoid arthritis in Sudanese patients.
Methods:
A case–control study was conducted between March and December 2018. Clinical and demographic data of the study participants were collected and analyzed. Polymerase chain reaction restriction fragment length polymorphism molecular technique was done to investigate interleukin-17A-197G/A polymorphisms. All statistical tests were considered statistically significant when p < 0.05.
Results:
The study population included 266 participants aged between 1 and 85 years, with an average of 40 years, classified into 85 (31.2%) cases (mean age 48.5 ± 11.3 years), and 181 (68.8%) controls (mean age 35.3 ± 15.9 years). The interleukin-17A homozygote AA genotype was more frequent among the control group compared to the case group; 95 (52.5%) and 7 (8.2%), respectively. The homozygote GG and the heterozygote AG genotypes were proportionally not different among the cases and control groups; 13 (54.2%) and 11 (45.8%), and 65 (46.4%) and 75 (53.6%), respectively. According to the distribution of interleukin-17A genotypes, a statistically significant difference was observed among cases with the interleukin-17A AA and AG genotypes, p values 0.001 and 0.004, respectively. For the association interleukin-17A genotypes and family history a negatively significant association was reported (95% confidence interval, –0.219, p value = 0.001). There was also a negatively significant association of interleukin-17A genotypes and anti-cyclic citrullinated peptide (95% confidence interval, −0.141, p value = 0.002).
Conclusion:
This study is the first study in Sudan established the association between interleukin-17A-197G/A (rs2275913) polymorphisms and susceptibly to rheumatoid arthritis. These findings appeal for further research in Sudan to investigate the exact role of IL-17A in immunopathology and disease severity among Sudanese rheumatoid arthritis
Introduction
Rheumatoid arthritis (RA) is the most prevalent chronic inflammatory disease characterized by an autoimmune response that affects mainly the joints and various parts of the human body. At late stages, RA leads to deformities of joints and bones and cause severe pain.1–5 Many factors were hypothesized to be involved in the induction and the progression of RA. The most accepted theory for the development of the disease is a multifactorial theory involving the interaction of environmental factors on genetically susceptible individual, making them more prone to RA. 6 The disease severity is varied from one population to another; Sudanese patients suffer from a severe form of the disease compared to other countries. 7
The microenvironment at the sites affected by active RA shows adherence to several types of inflammatory cells including polymorph nuclear cells and macrophages as well as T-cells. 8 A growing body of evidence indicates the central role of T-cells in the pathophysiology of RA as the patients carrying human leukocytes antigen (HLA)–DRB1 are more susceptible to disease development.9–12
Recently, a newly discovered subset of T Helper cells known as Th 17 reported playing a crucial role in the RA disease process.13,14 Th-17 cells produce a family of cytokines which consist of interleukin (
Methods
Study design and study population
This was a case–control study conducted from February 2017 to December 2018 in Khartoum State, Sudan at Zain Medical Center. A small volume (3 mL) of blood samples were collected into ethylenediaminetetraacetic acid (EDTA) blood containers from RA patients and healthy controls who voluntarily agreed to participate in the study after reading and signing informed consent. Parents and/or guardians signed informed consents on behalf of their children. Personal interviews were conducted to obtain these demographic and clinical data of participants: age, gender, locality, tribe, family history, and duration of RA. Patients who attended the hospital for follow-up of RA were given a similar chance to participate in the study, and healthy co-patients regardless of their age and gender were included as a healthy control group. Participants diagnosed with autoimmune diseases rather than RA were excluded from the study. During the study period, a total of 266 participants were successfully recruited. The number of excluded participants were 2 RA patients diagnosed with Systemic lupus erythrocytosis.
Ethics approval
The study ethical approval was obtained from the Ministry of Health Ethical Committee on February 2018 (No. 1.2.2018). A written, informed consent was obtained from all the study participants. Parents and/or guardians signed informed consents on behalf of their children.
DNA extraction and IL-17A genotyping
The total genomic DNA was extracted from the blood samples using the QIAamp DNA Blood Mini Kit (Qiagen, Germany). The extracted DNA checked for quality using nanophotometer (Implen, Germany). Then, DNA stored at −20°C until molecular genotyping.
Statistical analysis
Data analysis was conducted using the Statistical Package for the Social Sciences (SPSS v20). Fisher’s exact used to assess the association of IL-17A rs2275913 single-nucleotide polymorphism (SNP) with RA susceptibility. Kruskal–Wallis test was used to test the significant association of clinical parameters and participants status. One-way analysis of variance (ANOVA) test was used to assess the association between IL-17A rs2275913 SNP and RA duration. A p value < 0.05 was considered a statistically significant.
Results
Characteristics of the study population
The study population included 266 participants aged between 1 and 85 years, with an average of 40 years, classified into 85 (31.2%) cases with a mean age of 48.5 ± 11.3 years, and 181 (68.8%) controls with a mean age of 35.3 ± 15.9 years. For the cases, the mean age at diagnosis with RA was 42.4 ± 10.8 years. Among the case group, females were 79 (92.9%), and males were 6 (7.1%). The control group was consisted of 91 (50.3%) males and 90 (49.7%) females. Based on ethnicity, Arab ethnicity were the most frequent among the case group; 63 (74.1%), whereas, for the control group, the majority were Darforian; 56 (30.9%), followed by 48 (26.5%) Bbeja and 46 (25.4%) Arab. Concerning the duration of RA among the case group, RA durations were grouped into four categories. RA cases diagnosed with RA for <5 years were 42 (49.4%); constituting the majority of the cases, followed by those who had RA for 5–10 years; 29 (34.1%). For those who were diagnosed for 11–15 years and 16–20 years were 7 (8.2%); for each. Family history of RA was not reported among the control group. However, among the cases family history of RA was reported among 27 (31.8%) cases. Clinical parameters of RA diagnosis used in the study to investigate clinical outcomes included RF, CRP, anti-CCP, and ESR. The median of RF among the cases was 30.0, while in the control group was 6.4, whereas, the median of CRP was 6.0 and 3.7 among the cases and controls, respectively. The median of anti-CCP among the cases was also lower compared to the controls; 1.2 and 4.2, correspondingly. The median of ESR was measured higher in cases when compared to the controls; 37.0 and 19.1, respectively. Based on treatment, the majority of RA cases; 47 (55.3%), were admitted to methotrexate, while 12 (14.1%), 10 (11.8%), 10 (11.8%), and 6 (7.1%) were admitted to sulfasalazine, azathioprine, antimalarial, and leflunomide, respectively (Table 1).
Demographics and clinical features of the patients with rheumatoid arthritis and healthy controls.
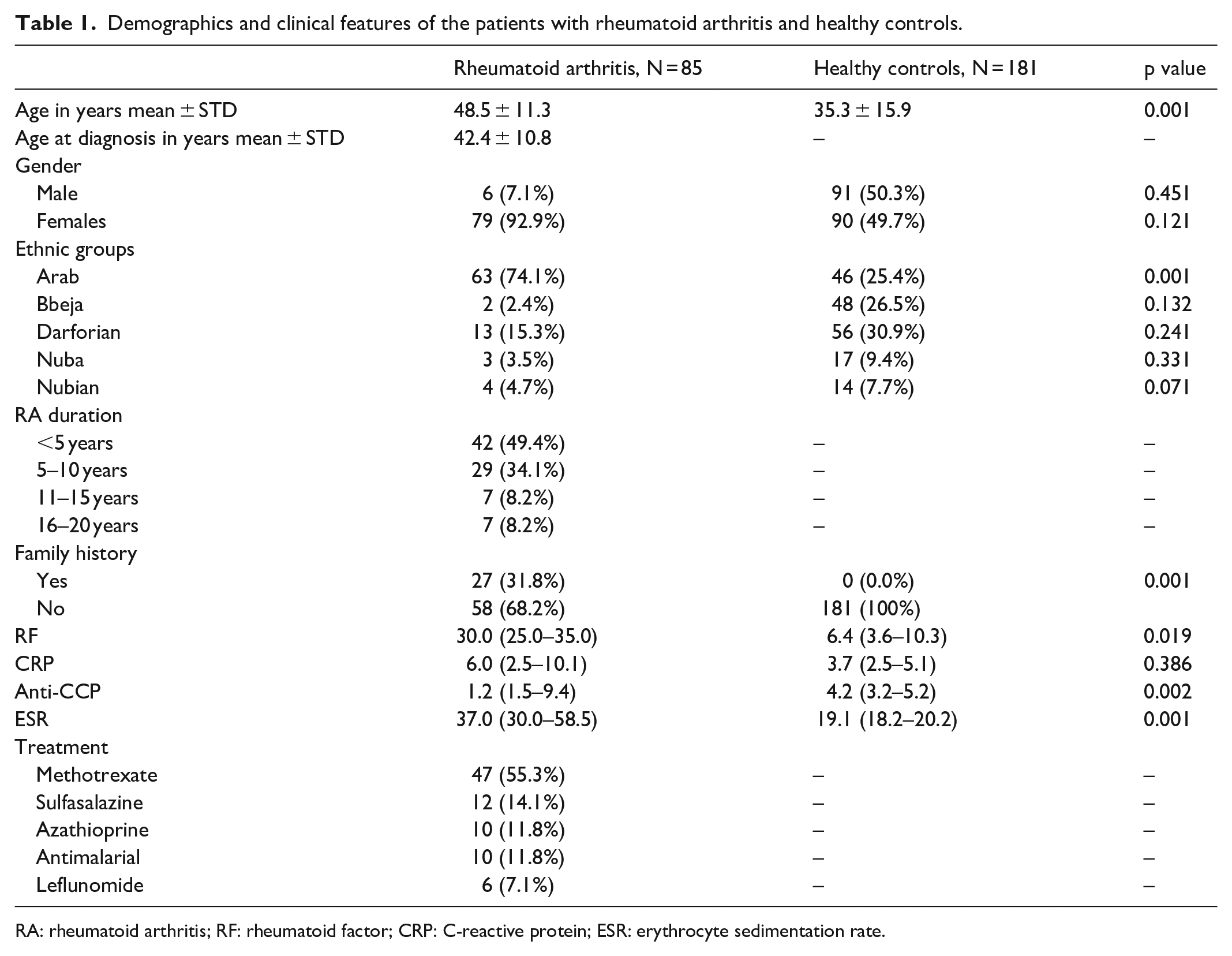
RA: rheumatoid arthritis; RF: rheumatoid factor; CRP: C-reactive protein; ESR: erythrocyte sedimentation rate.
Prevalence of IL-17A genotypes in the study population
The distribution of
Distribution of IL-17A genotypes among RA cases and controls.

IL-17A: interleukin 17A; OR: odds ratio; CI: confidence interval.
The distribution of
Distribution of IL-17A genotypes among RA cases and controls based on ethnic groups.

IL-17A: interleukin 17A.
Association of IL-17A genotypes with family history of RA
The association of
Association of IL-17A genotypes with RA duration among RA cases.

IL-17A: interleukin 17A.
Association of IL-17A genotypes with family history of RA and the clinical examination.

IL-17A: interleukin 17A; RF: rheumatoid factor; CRP: C-reactive protein; ESR: erythrocyte sedimentation rate; ND: not determined.
Discussion
Although the pathogenesis of RA is still unclear, the Th-17 cells produce several pro-inflammatory cytokines that participate in this pathogenicity such as IL-17A.
24
Previously, investigation of
The abnormal values of the clinical examinations including RF, CRP, anti-CCP, and ESR are the most features to determine RA. Both ESR and CRP provide suitable information about the acute phase response. 27 However, in this study, the lack of the disease activity score index (DAS28) may influence the association of CRP with RA patients. This is also contrary to a study in which the level of CRP was shown to be significantly correlated with the severity of RA. 28 Also, RF and anti-CCP are considered very helpful during the diagnosis of RA. However, anti-CCP shows a superior specificity than RF for the diagnosis of RA.29,30 In this study, all the investigated clinical examinations showed a higher mean in RA cases compared to controls.29,30
In this study, the
Conclusion
Although the study lacks the DAS28 index which constitutes a major index in assessing RA activity and severity, RA diagnosis was mainly dependent on RF, CRP, anti-CCP, and ESR examinations. Therefore, including the DAS28 index in future studies and associate it with the RA activity and severity can be useful in assessing RA patients’ prognosis and treatment follow-up. It is noteworthy that most of the RA cases were admitted for Methotrexate which may cause liver damage, particularly if taken for a long period of time. Therefore, a need to assess treatment outcome along with IL-17A genotypes to ease IL-17 targeted treatment can be useful for reducing RA severity. This study is considered the first study in Sudan that established the association between
Footnotes
Acknowledgements
The authors are grateful to the patients, controls, and their families and the staff at Zain Medical center for their continued collaboration and generous hospitality during the samples collection.
Authors’ contribution
R.M.O., A.A.M.A., N.S.M., and E.E.S. designed and led the study. M.N., A.E.A., H.A., R.A.O., M.M.A., A.M.E., and O.S. conduct the laboratory work. M.S.M., A.A., N.S.M., and E.E.S. analyzed and interpreted the data. R.M.O., A.A.M.A., R.H., E.S.A., L.A.H., O.E.H.B., and E.E.S. drafted the manuscript. All authors read, revised, and approved the final manuscript.
Availability of data and materials
The data sets used and/or analyzed during this study are available from the corresponding author on reasonable request.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical approval
The study ethical approval was obtained from the Ministry of Health Ethical Committee on February 2018 (grant no. 1.2.2018). A written, informed consent was obtained from all the study participants.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Informed consent
Written informed consent was obtained from all subjects before the study, in case of children, parents or guardians signed the informed consents on behalf of their children before the study.
