Abstract
Introduction:
Despite the widespread use of the mouse transverse aortic constriction heart failure model, there are no reports on the characterization of the standard-of-care agent carvedilol in this model.
Methods:
Left ventricular pressure overload was produced in mice by transverse aortic constriction between the innominate and left common carotid arteries. Carvedilol was administered at multiple dose levels (3, 10 and 30 mg/kg/day per os; yielding end-study mean plasma concentrations of 0.002, 0.015 and 0.044 µM, respectively) in a therapeutic design protocol with treatment initiated after the manifestation of left ventricular remodeling at 3 weeks post transverse aortic constriction and continued for 10 weeks.
Results:
Carvedilol treatment in transverse aortic constriction mice significantly decreased heart rate and left ventricular dP/dt (max) at all dose levels consistent with β-adrenoceptor blockade. The middle dose of carvedilol significantly decreased left ventricular weight, whereas the higher dose decreased total heart, left and right ventricular weight and wet lung weight compared to untreated transverse aortic constriction mice. The higher dose of carvedilol significantly increased cardiac performance as measured by ejection fraction and fractional shortening and decreased left ventricular end systolic volume consistent with the beneficial effect on cardiac function. End-study plasma sST-2 and Gal-3 levels did not differ among sham, transverse aortic constriction control and transverse aortic constriction carvedilol groups. Plasma brain natriuretic peptide concentrations were elevated significantly in transverse aortic constriction control animals (~150%) compared to shams in association with changes in ejection fraction and heart weight and tended to decrease (~30%, p = 0.10–0.12) with the mid- and high-dose carvedilol treatment.
Conclusion:
A comparison of carvedilol hemodynamic and structural effects in the mouse transverse aortic constriction model versus clinical use indicates a strong agreement in effect profiles preclinical versus clinical, providing important translational validation for this widely used animal model. The present plasma brain natriuretic peptide biomarker findings support the measurement of plasma natriuretic peptides in the mouse transverse aortic constriction model to extend the translational utility of the model.
Introduction
Clinical guidelines recommend the use of β-adrenoceptor blocking agents for patients with heart failure (HF) with reduced ejection fraction (HFrEF) to reduce morbidity and mortality.1,2 Three β-adrenoceptor blockers, carvedilol, bisoprolol and sustained release metoprolol succinate, specifically have been shown to reduce death and hospitalization in patients with chronic HFrEF.3–6 Carvedilol blocks β1 and β2 adrenoceptors with equal affinity. Additionally, it blocks α1-adrenoceptors and possesses antioxidant and free radical scavenging activities.7–9 Carvedilol also functions as a β-arrestin-biased β1 adrenoceptor ligand to activate alternate cellular pathways and regulate microRNA processing independent of G-protein-mediated signaling.10,11 In a direct comparator study in chronic HFrEF patients, carvedilol displayed higher survival benefit than the selective β1 adrenoceptor antagonist, metoprolol. 12 A meta-analysis of randomized, controlled direct-comparator trials in acute myocardial infarction and HFrEF settings reported that carvedilol significantly reduced all-cause mortality compared to selective β1 antagonists in HFrEF patients. 13
The preclinical study of pharmacologic treatments for HF requires the use of appropriate animal models. These animal models should display phenotypic features and allow for the measurement of endpoints relevant to clinical HF.14,15 The mouse transverse aortic constriction (TAC) model is a widely used model of pressure overload-induced HF. The surgical banding or constriction of the aortic arch between the innominate and left common carotid arteries in the mouse TAC model produces an increase in left ventricular (LV) afterload which simulates clinical conditions such as aortic constriction and hypertension. This increase in LV afterload leads to the development of LV hypertrophy, followed by LV chamber dilation, decreased systolic function, increased LV filling pressure and at least in a subset of animals increased lung weight indicative of congestion.14–18
The proper use of an animal disease model inherently and critically requires the characterization of clinically efficacious standard-of-care agents in the model in order to define concordance (or lack thereof) in the pharmacodynamic/efficacy profiles of the standard agents in the animal model versus clinical setting. Such assessments of standard-of-care agents in the animal model, particularly in experimental designs which incorporate therapeutic treatment initiation after the manifestation of the disease state, are necessary to establish model validity and translational value and in doing so facilitate the interpretation of findings in subsequent assessments of novel HF treatments in the model.
Despite the widespread use of the mouse TAC HF model in preclinical research, to date there are no reports of the characterization of the standard-of-care agent carvedilol in this model. Furthermore, there are no published assessments of β-adrenoceptor blocking agents in general when administered in a therapeutic protocol design in the mouse TAC model. Accordingly, the objective of this study was to conduct the first detailed assessment of the HF standard-of-care agent carvedilol in the mouse TAC model in order to allow translational comparisons of the profiles for cardiac hemodynamic and structural effects in the model versus the established clinical effects in HF patients. To that end, multiple dose levels of carvedilol were assessed in a 13-week study utilizing a therapeutic protocol design, that is, with treatment initiated 3 weeks after TAC at a time point when LV hypertrophy was manifest. This study assessed carvedilol effects on heart and lung mass, and LV function and structure were measured serially by echocardiography and at end-study by invasive hemodynamic assessment. Additionally, given the current high clinical interest in the use of plasma biomarkers to diagnose and potentially guide HF therapy, the effects of TAC and carvedilol treatment on the plasma biomarkers brain natriuretic peptide (BNP), sST-2 and Gal-3 were characterized in the model.
Methods
Experimental animals
Male C57/BL6J mice were purchased from The Jackson Laboratory (Bar Harbor, ME, USA) at 9 weeks of age. All protocols for animal experiments were approved by the research laboratories of Merck & Co., Inc. (Kenilworth, NJ, USA) Institutional Animal Care and Use Committee and were carried out in accordance with the Guide for the Care and Use of Laboratory Animals as adopted and promulgated by the US National Institutes of Health.
TAC surgical preparation
At 11 weeks of age, mice were anesthetized with 1%–3% isoflurane (Henry Schein, Melville, NY, USA) and animal body temperature was maintained between 36°C and 37°C throughout the procedure using the MouseMonitorS (Indus Instruments, Webster, TX, USA). The animals were intubated and placed on a rodent ventilator (Harvard Apparatus, Holliston, MA, USA). To create pressure overload, the transverse aortic arch was constricted in the middle of the arch between the innominate and left common carotid arteries. The aortic arch was isolated by blunt dissection, and a custom blunt needle (26.5 g) was positioned parallel to the aorta. A non-absorbable 7.0 nylon suture (Ethilon; Ethicon, Somerville, NJ, USA) was tied around the vessel and the needle, and then the needle was quickly withdrawn. Sham control mice were subjected to an identical procedure without the placement of a ligature. The incision was then closed. The intubation was removed after self-breathing was re-established. The animal was maintained on a heating pad (T-Pump; Stryker, Kalamazoo, MI, USA) until fully recovered.
Experimental protocol
Eight cohorts of mice ((25 mice/cohort) were entered into this study with staggered start dates and temporally overlapping study durations. All animals were housed in plastic boxes (1 per box) and received standard rodent diet 5053 (LabDiet, St Louis, MO, USA) and water ad libitum. Approximately 1 week prior to surgery, all mice underwent echocardiographic assessment to determine baseline cardiac function and structure, after which the mice were randomly allocated to sham or TAC surgery. Echocardiography was repeated at 3 weeks following surgical procedure. Immediately following the 3-week post-procedure echo, TAC mice were randomly allocated into TAC untreated or treatment groups (described below) such that after full enrollment, each TAC group had a total group size (recruited from all cohorts) of ~20–25 mice. Entry criteria for the enrollment of TAC mice were applied as described recently to enhance the desired phenotype, that is, only TAC animals that had greater than a 30% increase in LV mass (echo) over within-animal baseline at 3 weeks were enrolled into the study, and TAC mice meeting this criterion then were assigned to blinded treatment groups based on the 3-week ejection fraction (EF). 19 Two separate untreated TAC control groups maintained on standard rodent diet were enrolled and run separately within this study for the purpose of assessing between-group consistency. When analyzed at end-study, no significant differences in echocardiographic, invasive hemodynamic and organ weight changes in response to TAC were detected between these two groups, and therefore these groups were combined to serve as one TAC untreated control group after study completion. Three TAC groups were allocated to treatment with 3, 10 or 30 mg/kg/day per os (PO) carvedilol (LKT Laboratories, St. Paul, MN, USA) formulated in standard rodent diet 5053 by Research Diets (New Brunswick, NJ, USA). Sham control mice maintained on standard rodent diet were randomly allocated into the study targeting a full-enrollment total group size (recruited from all cohorts) of ~15 mice. In summary, study groups in this study were sham untreated controls (control diet), TAC untreated controls (control diet groups 1 and 2), TAC—3 mg/kg/day carvedilol, TAC—10 mg/kg/day carvedilol and TAC—30 mg/kg/day carvedilol. The numbers of mice entered into the present sham and TAC untreated control and treatment groups were justified based on treatment group sizes reported in published literature both for model characterization and the assessment of other mechanistically diverse standard-of-care agents in this model. Specifically, the group sizes used in this study were equivalent to or exceed those reported in directed characterizations of untreated sham versus untreated TAC mice (group n sizes ranging from 6 to 28 and 11 to 46 per group, respectively)16,18,19 and TAC treated groups (group n sizes ranging from 5 to 25 per group).21–34 All investigators conducting the serial echocardiographic and end-study invasive hemodynamic assessments, terminal tissue collections and plasma biomarker analyses were blinded to group assignments.
Echocardiography was repeated at 6, 9 and 13 weeks after surgical procedure (i.e. at 3, 6 and 10 weeks of treatment). Mice underwent invasive LV hemodynamic assessment 1–5 days after the 13-week echocardiography. After completion of the invasive hemodynamic study, blood samples were collected from the vena cava. Mouse blood samples were collected into ethylenediaminetetraacetic acid (EDTA) tubes containing 50 µM dipeptidyl peptidase IV (DPP-IV) inhibitor (EMD Millipore, Billerica, MA, USA) and a 1× concentration of Protease Inhibitor Cocktail (Roche Life Science, Indianapolis, IN). Whole blood was centrifuged and plasma was stored at −80°C until analysis. The heart was then removed and dissected to obtain the isolated right atria, left atria, right ventricle and left ventricle + septum tissue weights. The whole heart weights were determined by adding each section. The tibia was removed, cleaned of connective tissue and measured to determine tibia length. The lungs were removed and weighed. Dry lung weights were determined by drying the lungs for at least 48 h at room temperature.
Echocardiographic assessment
M-mode echocardiography was performed with a VisualSonics Vevo-2100 ultrasound system (Toronto, ON, Canada). Briefly, mice were anesthetized with 1.5%–2% isoflurane, and transthoracic echocardiography of the left ventricle was performed in order to measure LV wall thickness, LV chamber size, LV function and LV mass. Echocardiography was performed approximately 1 week prior to TAC surgery and again at 3, 6, 9 and 13 weeks post surgical procedure (sham or TAC).
Invasive hemodynamic assessment
Mice were anesthetized with 1%–2.5% isoflurane (Henry Schein, Melville, NY, USA), and animal body temperature was maintained between 36°C and 37°C throughout the procedure using the MouseMonitorS. The left jugular vein was isolated by blunt dissection, and a venous catheter was inserted for volume calibrations at the completion of the procedure. The right carotid artery was exposed and isolated and a conductance catheter (Millar Instruments, Houston, TX, USA) was advanced into the left ventricle via the ascending aorta. The animal was stabilized for approximately 15–30 min following the surgical preparation. Following the stabilization period, pressure–volume loops were recorded for 5 min using a data acquisition system (PowerLab; ADInstruments, Colorado Springs, CO, USA). These values were recorded with LabChart version 8.0 (ADInstruments). At the end of the data collection, a hypertonic saline solution (Teknova Inc., Hollister, CA, USA) was injected via the venous catheter for a parallel volume calibration. This parallel volume calibration was repeated three to four times, approximately 3–4 min apart.
Measurement of plasma biomarkers
Mouse BNP was measured using the BNP-45 Fluorescent Immunoassay Kit from Phoenix Pharmaceuticals (Burlingame, CA, USA). The assay was performed according to the manufacturer protocol. Briefly, frozen plasma was thawed on ice and 50 µL of plasma was placed into assay wells followed by an addition of 25 µL primary antibody per well. The mixture in the assay plate was incubated overnight at 4°C. Following the incubation period, biotinylated peptide was added to the mixture and incubated at room temperature for 1.5 h while shaking at 300 r/min. The assay plate was then washed and Streptavidin–horseradish peroxidase (HRP) was added for 1 h at room temperature. The plate was washed, and Substrate Solution was added and incubated at room temperature for 20 min. Stop Solution was added to the Substrate Solution to stop the reaction. The plate was immediately read on a SpectraMax M2 spectrophotometer (Molecular Devices, Sunnyvale, CA, USA) at 325 and 420 nm wavelengths. Data were analyzed using Softmax Pro version 5.4 (Molecular Devices).
Mouse ST2 was measured using the Quantikine Mouse ST2 enzyme-linked immunosorbent assay (ELISA; R&D Systems, Minneapolis, MN, USA). The assay was performed according to the manufacturer protocol. Briefly, frozen plasma was thawed on ice before diluting 50-fold in Assay Diluent. The assay was performed at room temperature. The assay plate was pre-wetted with 50 µL Assay Diluent followed by an addition of 50 µL of diluted plasma. The mixture was incubated for 2 h while shaking at 300 r/min. The assay plate was then washed and the ST2-conjugated antibody was added for 2 h at room temperature. Plates were washed and Substrate Solution was added and incubated at room temperature for 30 min. Stop Solution was added to the Substrate Solution to stop the reaction. The plate was immediately read on a SpectraMax M2 spectrophotometer (Molecular Devices, Sunnyvale, CA) at 450 and 540 nm wavelengths. Data were analyzed using Softmax Pro version 5.4 (Molecular Devices, Sunnyvale, CA, USA).
Mouse Galectin-3 was measured using the Mouse Galectin-3 DuoSet ELISA (R&D Systems). The assay was performed according to the manufacturer protocol. Briefly, 2 µg/mL of Galectin-3 antibody was coated overnight at 4°C in an Immulon 4HBX plate (Thermo Fisher, Waltham, MA, USA). Subsequent incubations were performed at room temperature while shaking at 300 r/min. Frozen plasma was thawed on ice before diluting 50-fold in Diluent. The assay plate was washed, blocked with Diluent for 1 h and washed again. A volume of 100 µL of diluted plasma was added to the assay plate and incubated for 2 h. Following the incubation period, the plate was washed and incubated for an additional 2 h with 0.2 µg/mL biotinylated Galectin-3 antibody. After a plate wash, Streptavidin–Europium (PerkinElmer, Waltham, MA, USA) was added for 20 min followed by an additional plate wash. DELFIA Enhancement Solution (PerkinElmer) was added to the plate and incubated in the dark for 1 h. The plate was read on a PHERAstar spectrophotometer (BMG Labtech, Ortenberg, Germany) at 337 and 615 nm wavelengths. Data were analyzed using MARS version 2.41 (BMG Labtech).
Measurement of plasma carvedilol concentrations
Carvedilol plasma concentrations were quantified by liquid chromatography–tandem mass spectrometry (LC-MS/MS) after protein precipitation using acetonitrile. The LC-MS system consisted of a Transcend LX2 platform (Thermo Fisher, Pittsburgh, PA, USA) and an AB Sciex API 5000 Triple Quadrupole mass spectrometer (AB Sciex, Concord, ON, Canada) operating in the positive ion mode using the TurboIonSpray interface (AB Sciex, Concord, ON, Canada). Carvedilol was separated using a Waters UPLC HSS T3 column (1.8 µm particle size, 50 × 2.1 mm internal diameter (I.D.)) and selected reaction monitoring of transition m/z 407.6–283.3 was used for quantitation (Waters Corporation, Milford, MA, USA). A calibration curve (1–5000 ng/mL) together with three sets of quality controls (5, 20, 2000 and 5000 ng/mL) were prepared and analyzed in the same manner as the study samples. Sciex MultiQuant 3.0.1 was used to process results.
Statistical methods
All results are reported as mean ± standard error of the mean (SEM). Longitudinal echocardiographic data, body weight and food intake data were analyzed using a mixed linear effect model. 20 End point data (terminal weights, invasive hemodynamics and biomarkers) were analyzed using a one-way analysis of variance (ANOVA) followed by a Wald test to compare among treatment groups; p < 0.05 was considered significant. Relationships among end-study plasma BNP concentrations and LV EF, end diastolic pressure and heart weight were assessed by determination of Pearson correlation coefficients.
Results
Cardiac functional and structural changes after TAC
Mice were randomly allocated to TAC or sham surgery. At 3 weeks post procedure, survival was 82% and 100% in the TAC and sham groups, respectively. Using the enrollment criteria described in the “Methods” section, 81% of surviving TAC mice at 3 weeks post procedure were enrolled and randomized into treatment groups. At 13 weeks post procedure (end-study), the survival of mice that were enrolled into the TAC and sham untreated control groups at the 3-week treatment initiation time point was 84% and 100%, respectively. The following summaries of cardiac functional and structural changes with TAC are based on data obtained in surviving mice in the TAC and sham untreated control groups.
Changes in cardiac structure and function were evaluated non-invasively using echocardiography. Table 1 summarizes baseline (pre-procedure) and 13-week post-procedure (end-study) echocardiographic parameters in sham and TAC untreated control mice. At baseline, there were no significant differences in any echocardiographic measures between the sham control and TAC groups. At end-study, TAC mice displayed LV hypertrophy reflected in significant increases in LV mass (echo) and in anterior and posterior LV diastolic wall thicknesses compared to sham mice. LV chamber dilation was evident in TAC mice as reflected in increased LV end diastolic and systolic diameters and volumes. Cardiac functional performance measures of EF, fractional shortening, stroke volume and cardiac output were decreased in TAC versus sham untreated control mice at end-study.
Cardiac function and structure measured by echocardiography at baseline (pre-procedure) and at 13 weeks post procedure (end-study) in untreated sham-operated (Sham) and TAC control mice.
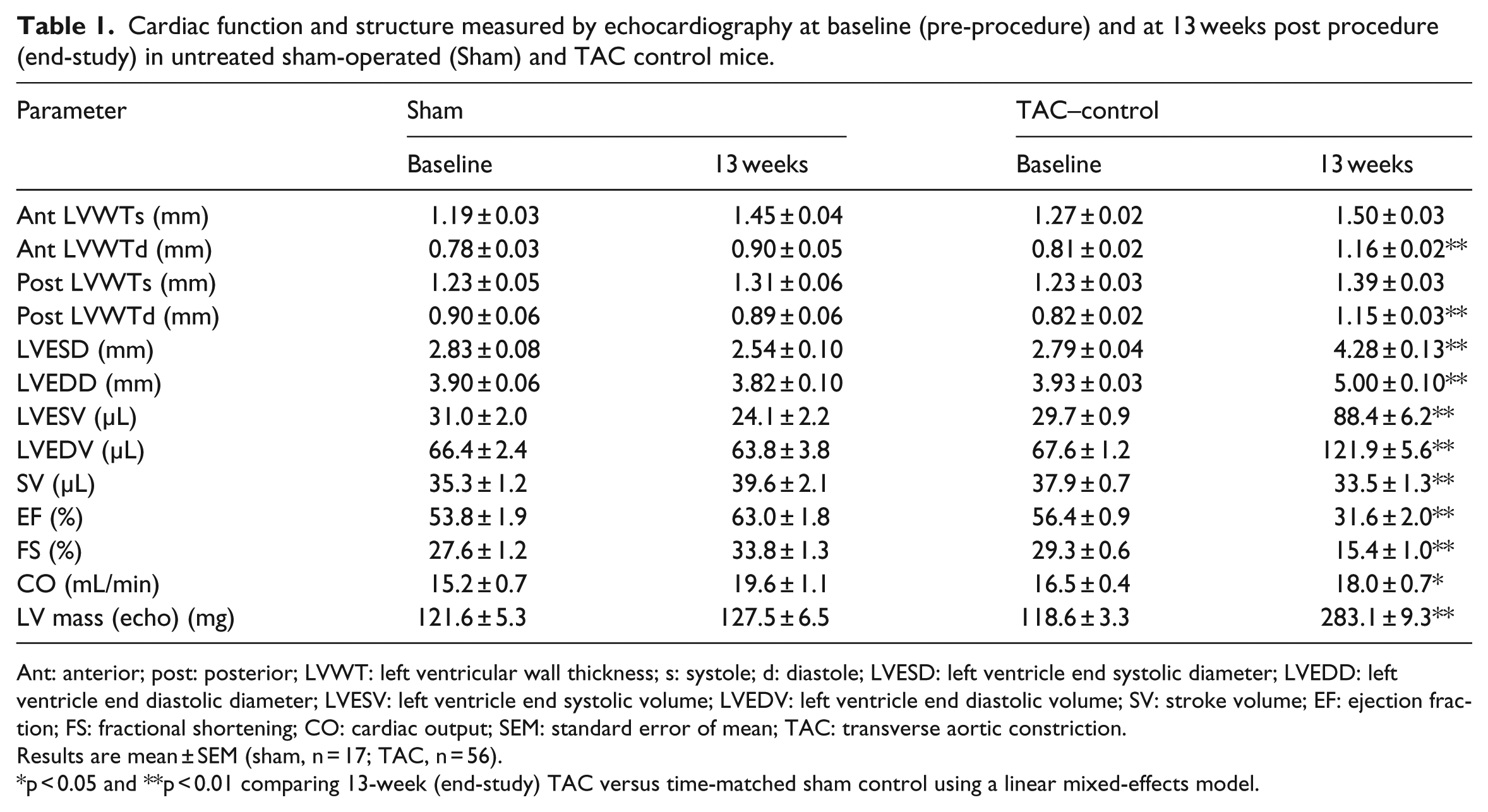
Ant: anterior; post: posterior; LVWT: left ventricular wall thickness; s: systole; d: diastole; LVESD: left ventricle end systolic diameter; LVEDD: left ventricle end diastolic diameter; LVESV: left ventricle end systolic volume; LVEDV: left ventricle end diastolic volume; SV: stroke volume; EF: ejection fraction; FS: fractional shortening; CO: cardiac output; SEM: standard error of mean; TAC: transverse aortic constriction.
Results are mean ± SEM (sham, n = 17; TAC, n = 56).
p < 0.05 and **p < 0.01 comparing 13-week (end-study) TAC versus time-matched sham control using a linear mixed-effects model.
Figure 1 displays the time course for changes of several key echocardiographic parameters in TAC versus sham untreated control mice. Significant hypertrophy measured as LV mass (echo) was manifested at 3 weeks post TAC and continued to increase with time (Figure 1(a)). During this early phase of hypertrophy, a thickening of LV wall in diastole was also manifested, followed by a partial regression of wall thickening at later time points as chamber diameter and volume increased (Figure 1(b) and (c) for LV anterior wall diastolic thickness and end diastolic diameter, respectively). Cardiac performance parameters exemplified by EF (Figure 1(d)) were reduced in a time-dependent manner throughout the 13-week post-TAC time frame.

Time-course changes in echo-derived parameters: (a) LV mass (echo), (b) anterior left ventricular end diastolic wall thickness (Ant LVWTd), (c) left ventricular end diastolic diameter (LVEDD) and (d) ejection fraction (EF) in sham-operated (Sham) and transverse aortic constriction (TAC) untreated control mice. Baseline is pre-procedure echocardiographic assessment. *p < 0.05 and **p < 0.01 comparing time-matched TAC versus sham controls using a linear mixed-effects model. Results are presented as mean ± SEM. (e) Example of whole hearts from sham-operated (Sham) and TAC untreated mice at end of the study.
Invasive hemodynamic assessments were performed in TAC and sham untreated control mice at end-study by generating pressure–volume loops using an LV conductance catheter. Following this hemodynamic assessment, terminal tissue weights were measured. Table 2 summarizes the terminal invasive hemodynamic results and tissue weights for all groups. As expected, compared to sham control, TAC untreated control mice displayed significantly higher LV developed and systolic pressures as well as elevated arterial elastance. Compared to sham control mice, LV end diastolic pressure (LVEDP) and the LV relaxation rate, tau, were increased in TAC control mice consistent with diastolic dysfunction. In this study, heart rate was increased, whereas LV dP/dt (max) and LV dP/dt (min) did not differ significantly between TAC and sham control mice. Assessment of terminal organ weights revealed cardiac hypertrophy in the TAC untreated control mice with significantly increased heart weight mainly derived from increases in left ventricle + septum and left atrial masses. Right ventricle and right atrial masses also were elevated in the TAC control mice. Wet and dry lung weights were increased in the TAC untreated control mice compared to the sham control.
Invasive hemodynamic parameters and terminal tissue weights at 13 weeks post procedure (end-study) in untreated sham-operated (Sham) and TAC mice–untreated control or treated with carvedilol at 3, 10 or 30 mg/kg/day.
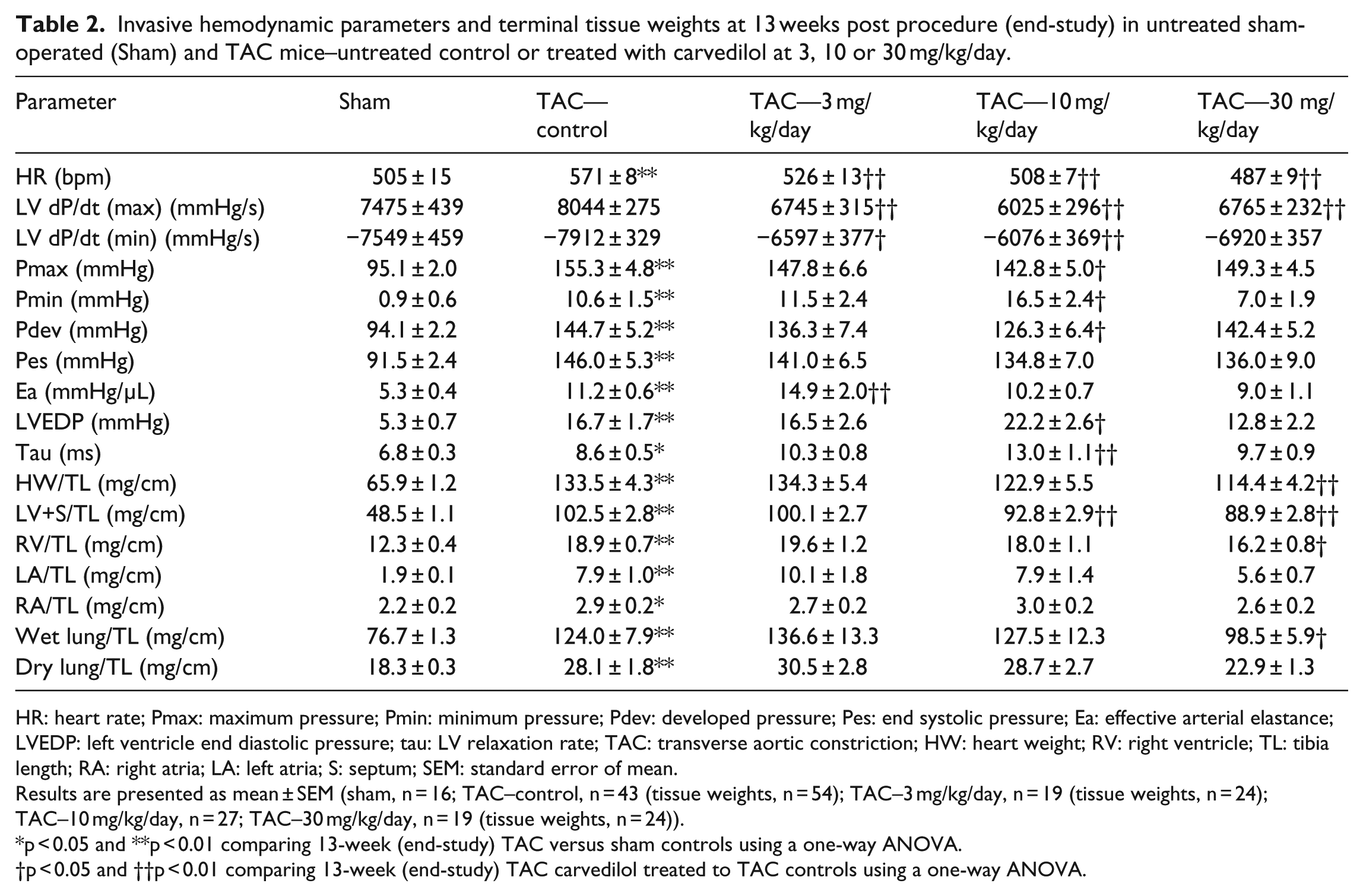
HR: heart rate; Pmax: maximum pressure; Pmin: minimum pressure; Pdev: developed pressure; Pes: end systolic pressure; Ea: effective arterial elastance; LVEDP: left ventricle end diastolic pressure; tau: LV relaxation rate; TAC: transverse aortic constriction; HW: heart weight; RV: right ventricle; TL: tibia length; RA: right atria; LA: left atria; S: septum; SEM: standard error of mean.
Results are presented as mean ± SEM (sham, n = 16; TAC–control, n = 43 (tissue weights, n = 54); TAC–3 mg/kg/day, n = 19 (tissue weights, n = 24); TAC–10 mg/kg/day, n = 27; TAC–30 mg/kg/day, n = 19 (tissue weights, n = 24)).
p < 0.05 and **p < 0.01 comparing 13-week (end-study) TAC versus sham controls using a one-way ANOVA.
p < 0.05 and ††p < 0.01 comparing 13-week (end-study) TAC carvedilol treated to TAC controls using a one-way ANOVA.
Effects of carvedilol treatment
For the purpose of identifying and validating carvedilol doses to be used in the present 13-week duration mouse TAC study, a 4-week duration pharmacokinetic/tolerability study with carvedilol first was conducted in normal male C57/BL6J mice. In this preliminary study, carvedilol was administered in feed at doses of 10, 30 and 100 mg/kg/day PO. Dose-dependent decreases in heart rate were observed at all doses tested, with no changes in food intake or body weight noted over the 4-week study duration. Plasma concentrations of carvedilol at end-study in the 30 mg/kg/day PO group approximated reported clinical concentrations for this agent. Based on these findings, carvedilol doses of 3, 10 and 30 mg/kg/day PO were chosen for the longer term TAC study.
In this study, TAC mice were randomized to no-treatment diet (untreated controls) or in-diet carvedilol treatment at doses of 3, 10 or 30 mg/kg/day at 3 weeks post TAC and then were monitored for 10 weeks of continuous treatment (i.e. end-study at 13 weeks post TAC). Survival at 13 weeks post TAC was 84%, 84%, 88% and 76% in the TAC untreated control and carvedilol 3, 10 and 30 mg/kg/day treatment groups, respectively (p = ns among groups). Plasma concentrations of carvedilol in the 3, 10 and 30 mg/kg/day treatment groups at end-study were 0.002 ± 0.0002, 0.015 ± 0.004 and 0.044 ± 0.008 µM, respectively. The following summaries of the effects of carvedilol treatment on cardiac functional and structural changes are based on data obtained in surviving mice in the TAC untreated and treated groups.
Heart rate was significantly and dose-dependently decreased, and LV dP/dt (max) was decreased significantly at end-study at all dose levels of carvedilol treatment compared to TAC untreated controls. LV dP/dt (min) was decreased significantly at 3 and 10 mg/kg/day, with a trend (p = 0.054) for decrease with 30 mg/kg/day carvedilol (Table 2). There were no consistent effects of carvedilol treatment on LV developed and systolic pressures, LVEDP, arterial elastance or the LV relaxation rate, tau, with a paradoxical but non-dose-dependent elevation of filling pressure and increase in tau seen in the middle carvedilol dose (Table 2). At the middle dose of carvedilol, a significant decrease in end-study LV weight was detected along with a trend (p = 0.08) for decreased heart weight. Significant decreases in heart weight, LV weight, right ventricular weight and wet lung weight were observed at the higher carvedilol dose (Table 2).
Table 3 summarizes the effects of carvedilol treatment on echocardiographic parameters at end-study in TAC mice. Significant increases in EF and fractional shortening were detected in TAC mice treated with the higher dose level of carvedilol compared to TAC controls. A significant decrease in LV end systolic volume was also observed with the higher carvedilol dose, consistent with improved cardiac functional performance. Similarly, a trend (p = 0.053) for decrease in LV end systolic diameter was observed with the higher carvedilol dose. No significant changes in LV end diastolic diameters and volumes or in LV anterior or posterior wall thicknesses were observed with carvedilol treatment at end-study. A significant decrease in LV mass (echo) was detected at end-study with the higher dose of carvedilol with a trend (p = 0.12) for decrease in LV mass (echo) seen at the middle dose of carvedilol, consistent with the observed decreases in terminal cardiac weights. Figure 2 graphically summarizes time-course changes in LV mass (echo), LV end systolic volume, EF and fractional shortening from the point of treatment initiation (i.e. 3 weeks post TAC) in the TAC control and treated groups. The higher 30 mg/kg/day carvedilol dose significantly reduced LV mass (echo) at weeks 9 and 13 of study (i.e. 6 and 10 weeks of treatment), with a trend (p = 0.063) for reduction at week 6 of study (i.e. 3 weeks of treatment; Figure 2(a)). A significant decrease in LV systolic volume and increase in EF and fractional shortening were detected only at week 13 of study (i.e. 10 weeks of treatment), although trends for increase in EF and fractional shortening (p = 0.052 and 0.051, respectively) were observed at week 9 of study (i.e. 6 weeks of treatment; Figure 2(b)–(d)).
Cardiac function and structure measured by echocardiography at 13 weeks post procedure (end-study) in TAC mice–untreated control or treated with carvedilol at 3, 10 or 30 mg/kg/day.

Ant: anterior; post: posterior; LVWT: left ventricular wall thickness; s: systole; d: diastole; LVESD: left ventricle end systolic diameter; LVEDD: left ventricle end diastolic diameter; LVESV: left ventricle end systolic volume; LVEDV: left ventricle end diastolic volume; SV: stroke volume; EF: ejection fraction; FS: fractional shortening; CO: cardiac output; SEM: standard error of mean; TAC: transverse aortic constriction.
Results are mean ± SEM (TAC–control, n = 56; TAC–3 mg/kg/day, n = 26; TAC–10 mg/kg/day, n = 29; TAC–30 mg/kg/day, n = 28).
p < 0.05 and ††p < 0.01 comparing 13-week (end-study) TAC carvedilol treated to TAC controls using a linear mixed-effects model.

Time-course changes in echo-derived parameters with treatment in TAC mice from the point of treatment initiation (Tx Initiation). Absolute changes in parameters were calculated and plotted from the time point of treatment initiation (i.e. 3 weeks post TAC). (a) LV mass (echo). (b) left ventricular end systolic volume (LVESV). (c) Ejection fraction. (d) Fractional shortening in untreated sham-operated control mice (Sham), untreated transverse aortic constriction (TAC) control (TAC–control) or TAC mice treated with carvedilol at 3, 10 or 30 mg/kg/day. *p < 0.05 and **p < 0.01 comparing time-matched TAC versus sham controls using a linear mixed-effects model. †p < 0.05 and ††p < 0.01 comparing time-matched TAC carvedilol treated to TAC controls using a linear mixed-effects model. Results are presented as mean ± SEM.
Plasma biomarker changes after TAC and carvedilol treatment
Plasma concentrations of sST-2, Gal-3 and BNP were measured at end-study in the sham untreated control, TAC untreated control and TAC carvedilol-treated mice. No differences among or changes with treatment were observed in any of the study groups for sST-2 and Gal-3. End-study plasma sST-2 concentrations in the sham and TAC control groups were 42.8 ± 4.4 and 40.2 ± 1.2 pg/mL, respectively, and ranged between 38.9 ± 1.4 and 48.0 ± 4.6 pg/mL in the TAC carvedilol treatment groups. End-study plasma Gal-3 concentrations in the sham and TAC control groups were 24.8 ± 1.7 and 27.0 ± 1.7 pg/mL, respectively, and ranged between 26.3 ± 1.3 and 27.7 ± 1.2 pg/mL in the TAC carvedilol treatment groups. Figure 3 summarizes the effects of TAC as well as carvedilol treatment in TAC mice on plasma BNP concentrations. Plasma BNP levels were elevated significantly by approximately 150% in TAC untreated control versus sham control mice at end-study (120.0 ± 16.4 vs 48.2 ± 10.9 pg/mL). While carvedilol treatment failed to significantly decrease plasma BNP levels at end-study, plasma BNP concentrations in the middle and higher carvedilol dose groups (86.7 ± 12.4 and 82.8 ± 11.3 pg/mL) were reduced 28% and 31% (p = 0.12 and 0.10, respectively) compared to TAC untreated controls. Figure 3(b)–(d) depicts plasma BNP concentrations determined at end-study in sham untreated control, TAC untreated control and TAC carvedilol-treated mice plotted as functions of end-study LV EF, end diastolic pressure and heart weight. Panels B and D demonstrate strong relationships between plasma BNP concentrations and EF (Figure 3(b)) and heart weight (Figure 3(d)), with Pearson correlation coefficient r values of 0.65 and 0.69, respectively. Treatment with carvedilol in this model resulted in a shift in the position of TAC animals toward higher EF and lower heart weight regions within these relationships. A more moderate relationship between plasma BNP concentration and LVEDP was evident, with an r value of 0.51 (Figure 3(c)).

End-study (13-week post procedure) plasma biomarker results. (a) Brain natriuretic peptide (BNP) in untreated sham-operated control mice (Sham), untreated transverse aortic constriction (TAC) control (TAC–control) or TAC mice treated with carvedilol at 3, 10 or 30 mg/kg/day. *p < 0.05 comparing 13-week (end-study) TAC versus sham controls using a one-way ANOVA. Results are presented as mean ± SEM. Correlations of BNP to 13-week parameters. (b) Correlation to ejection fraction (EF). (c) Correlation to left ventricular end diastolic pressure (LVEDP). (d) Correlation to heart weight (HW) in untreated sham-operated control mice (Sham), untreated transverse aortic constriction (TAC) control (TAC–control) or TAC mice treated with carvedilol at 3, 10 or 30 mg/kg/day.
Discussion
Prior literature reports have described assessments of HF standard-of-care agents of varying mechanism of action in the mouse TAC pressure overload model. Several studies reported that treatment with the angiotensin converting enzyme (ACE) inhibitors captopril and ramipril reduced cardiac hypertrophy in studies ranging from 1 to 9 weeks post TAC,21–24 with a 9-week study reporting beneficial effects of captopril on LV dimension and cardiac function. 23 Three studies assessed the effects of the mineralocorticoid receptor (MR) antagonists eplerenone and/or finerenone in 1–7 week duration mouse TAC studies and reported decreases in cardiac hypertrophy,25–27 with the 7-week TAC study reporting an increase in cardiac function. 27 Experience with ARBs in mouse TAC has been inconsistent. While several studies with losartan, telmisartan and additional ARBs reported reductions in cardiac hypertrophy at 1–5 weeks post TAC,21,24,28,29 three studies with losartan reported no attenuation of hypertrophy at 4–9 weeks post TAC.30–32 Two studies with losartan in a 4-week post-TAC assessment reported beneficial effects on cardiac function and/or filling pressure (LVEDP),29,30 whereas three studies with losartan, telmisartan and additional ARBs reported no beneficial effects on cardiac function, LV dimension and LVEDP.28,31,32 Regarding previous experience with β-adrenergic receptor blockers, the β1-selective blocker celiprolol and the non-selective β1 and β2 blocker propranolol have been assessed in 4- and 8-week duration mouse TAC studies, respectively. Both β-blockers decreased cardiac hypertrophy, improved cardiac function and decreased LV dimension.33,34 Of critical note, the great majority of these standard-of-care studies in the mouse TAC model, including both prior studies with β-blockers, utilized a prevention-type protocol design with test agent treatment initiated concurrent with or prior to TAC, that is, before the manifestation of LV remodeling. Also, most of the standard-of-care studies were conducted with only one dose level of test agent. Only two of the standard-of-care studies, both with losartan, reported effects on survival with a 4-week study reporting numerical survival benefit but with very low group sizes and a 9-week study reporting no survival benefit. Finally, only one standard-of-care mouse TAC study reported effects on plasma biomarkers, with the MR antagonist finerenone, but not eplerenone, decreasing plasma BNP approximately 20% relative to vehicle treatment at 4 weeks post TAC. 26
This study provides the first characterization of the HF standard-of-care agent carvedilol in the mouse TAC model and overall the first characterization of any β-adrenoceptor blocking agent with treatment initiated in therapeutic mode after the manifestation of LV remodeling in this model. In this study, carvedilol was administered at three dose levels for 10 weeks in a therapeutic protocol design, with treatment initiated at 3 weeks post TAC at a time when significant increases in LV mass and diastolic wall thickening already were evident on echocardiographic assessment. The determination of end-study plasma concentrations of carvedilol demonstrated that dose-dependent exposures of the test agent were achieved. Of note, the end-study mean plasma concentrations for the mid- (10 mg/kg/day) and high-dose (30 mg/kg/day) carvedilol regimens of 0.015 and 0.044 µM, corresponding to concentrations of 6 and 18 ng/mL, respectively, are numerically consistent with plasma levels observed in HF patients administered carvedilol for 7–28 days.35,36 More importantly, pharmacodynamic effects indicative of β-adrenoceptor blockade were observed with the present carvedilol dosing regimens in the mouse TAC model. All three dose levels of carvedilol significantly decreased heart rate and LV dP/dt (max) consistent with β-blockade. Clinical studies in HF patients have reported decreases in heart rate with carvedilol.37–41 In the present mouse TAC study, while the decreases in heart rate with carvedilol appeared dose-dependent, carvedilol effects on LV dP/dt (max) and dP/dt (min) were not apparently dose-dependent, suggesting that the carvedilol effects on the latter parameters may have been essentially maximal in all dosing regimens with some variation across groups leading to different levels of statistical significance or also reflecting multifactorial modulation of LV dP/dt (max) and dP/dt (min) by carvedilol, including, for example, direct β-adrenoceptor blockade as well as secondary effects such as heart rate changes. In the present mouse TAC study, significant reductions in cardiac hypertrophy were observed with carvedilol, with a decrease in LV weight observed at the middle dose level and reductions in total heart weight and left and right ventricular weights demonstrated with the higher carvedilol dose. Clinical studies in HF patients also have reported significant decreases in LV mass with carvedilol.42–44 No significant effect of carvedilol on LV wall thickness was detected in the present TAC model study. As noted in the “Results” section, the mouse TAC model run in this study duration displays some later regression in LV wall thickening due to progressive chamber dilation and wall stretch. It is likely that the time-dependent regression of wall thickness as the heart grows in size may confound the ability to detect a test agent–mediated effect on wall thickness in this model. The higher carvedilol dose reduced wet lung weight in the mouse TAC model, suggesting a beneficial effect on congestion. In the present TAC study, the higher dose regimen of carvedilol significantly increased LV EF relative to untreated controls by an approximate mean 6.6% points. Clinical studies mainly in New York Heart Association Class II–III (NYHA II–III) HF patients administered carvedilol for durations ranging from 4 to 12 months have reported increases in left ventricular ejection fraction (LVEF) of 3%–11% percentage points,37–43,45–47 with a meta-analysis of 13 carvedilol clinical HF studies reporting a mean 6.5% point increase in LVEF. 48 The higher dose regimen of carvedilol also significantly increased fractional shortening and decreased LV end systolic volume consistent with improved cardiac function in the mouse TAC model. Clinical studies in HF patients similarly have reported significant increases in fractional shortening40,43,49 and decreases in LV end systolic volume41,43,44,47 with carvedilol. No significant effects of carvedilol on stroke volume and cardiac output were detected in the present mouse TAC study. Clinical studies in HF patients have reported varying effects of carvedilol on stroke volume including some studies detecting no effect.37,38,40,41,47 Carvedilol has been reported to have no effect on cardiac output in clinical HF studies, with decreased heart rate suggested to blunt an effect on this calculated parameter.40,47 The present findings in the mouse TAC model demonstrate clear antihypertrophic activity with carvedilol resulting in improved cardiac function, with the latter requiring highly effective β-blocking exposures. Overall, the comparison of carvedilol hemodynamic and structural effects in the mouse TAC model versus clinical experience indicates a strong concordance in effect profiles preclinical versus clinical, providing novel and important translational validation for this widely used animal model.
There is high interest and extensive ongoing clinical investigation on the use of circulating biomarkers as diagnostic and prognostic tools as well as their potential to guide therapy in HF. Such biomarkers prominently include natriuretic peptides which are released in response to myocyte stretch.50,51 Emerging biomarkers include sST-2, the soluble form of the interleukin-1 receptor member ST2 thought to reflect cellular response to stress and serve as a marker for cardiac remodeling and fibrosis,52,53 and Gal-3, the macrophage-secreted beta-galactoside–binding lectin linked to cardiac fibrosis and also thought to serve as a marker for renal fibrosis and function.54,55 Clinical guidelines recommend the use of plasma natriuretic peptide concentration, including BNP, as a diagnostic test to establish the presence and severity of HF and guide in the need for further cardiac investigation, whereas usefulness to guide therapy is not yet established and is the subject of ongoing investigation.1,2 Clinical guideline statements on plasma sST-2 and Gal-3 range from the acknowledgement that sST-2 and Gal-3 are predictive of outcome in patients with HF 1 to the caution that at this time, there is no definitive evidence to recommend their use in clinical HF practice. 2 As noted in the review of published mouse TAC studies above, there has been scant reporting on the effects of standard-of-care agents on plasma biomarkers including BNP, sST-2 and Gal-3 in this model. In the present mouse TAC study, no differences among or changes with treatment were observed in sham control, TAC control and TAC carvedilol-treated mice for end-study plasma concentrations of sST-2 and Gal-3. In contrast, end-study plasma concentrations of BNP were elevated significantly in TAC untreated controls relative to sham controls (120.0 ±16.4 vs 48.2 ± 10.9 pg/mL), with plasma BNP levels associated with cardiac hypertrophy and EF status. Plasma BNP concentrations tended to decrease in TAC mice treated with carvedilol 28%–31%, albeit non-significantly (p = 0.10–0.12). For clinical perspective on the use of BNP as a plasma biomarker in assessing the presence or severity of HF, a plasma BNP upper limit of normal value in the non-acute setting of 35 pg/mL, with a higher normal cut-off value of 100 pg/mL in the acute setting, has been cited. 2 Several clinical studies varying in objective, design and criteria for HF definition have reported elevated levels of plasma BNP in HF cohorts, including the following (mean or median values): 165 pg/mL in NYHA II and 409 pg/mL in NYHA III stable symptomatic HF patients (EF < 50); 56 142 pg/mL in stable symptomatic NYHA I/II and 244 pg/mL in NYHA III/IV HF patients (EF < 40); 57 917 pg/mL in NYHA III/IV HF patients (EF < 45); 58 approximately 400 pg/mL in NYHA I and II and 700 pg/ml in NYHA III and 1300 pg/mL in NYHA IV (mean EF 25%); 59 and 180 pg/mL in NYHA I, 227 pg/mL in NYHA II and 726 pg/mL in NYHA III–IV in dilated cardiomyopathy (DCM) patients with atrial and ventricular overload (EF < 45). 60
Caveats to this study include the acknowledgment that the scope of this preclinical mouse TAC study focused primarily on physiologic cardiac hemodynamic and organ-level structural changes (e.g. organ weight, chamber dimension, wall thickening) with carvedilol treatment in order to allow comparison to carvedilol clinical HF experience in order to assess translational value, but did not include histologic studies. It is acknowledged that while not part of the present scope of investigation, histologic studies would, in a follow-on study, provide additional information and a more complete characterization of carvedilol effects in this model particularly if compared concurrently to other more selective β-adrenoceptor antagonists. Regarding caveats to the findings with carvedilol and the plasma markers sST-2, Gal-3 and BNP, it is noted that plasma concentrations of these markers were measured only at end-study with comparisons conducted across treatment groups. Longitudinal with-in animal studies of changes in such plasma biomarkers would be required to more definitely assess the utility of these markers in informing on disease severity as well as treatment efficacy in this as well as other animal HF models. That said, the present findings with plasma BNP in mouse TAC with carvedilol treatment, in concert with the findings of Grune et al. 26 demonstrating a 20% decrease in plasma BNP with finerenone in the mouse TAC model, support the incorporation of the measure of plasma natriuretic peptides to extend the translational utility of this model, both for stratification of disease severity and association to treatment effects on hemodynamic and structural status within the model, as well as for correlation to clinical treatment efficacy.
Conclusion
The proper use of animal disease models inherently and critically requires the characterization of clinically efficacious standard-of-care agents in the model in order to define concordance (or lack thereof) in the pharmacodynamic/efficacy profiles of the standard agents in the animal model versus clinical setting, thereby informing on the translational value of the model. This study provides the first characterization of the HF standard-of-care agent carvedilol in the mouse TAC model and overall the first characterization of any β-adrenoceptor blocking agent administered in a therapeutic protocol design in this model. Carvedilol, administered to TAC mice at three dose levels for 10 weeks in a therapeutic protocol design treatment, significantly decreased heart rate and LV dP/dt (max) consistent with β-adrenoceptor blockade. The higher dose level of carvedilol significantly reduced cardiac hypertrophy, reduced wet lung weight indicative of a salutary effect on congestion, improved EF and fractional shortening and accordingly reduced LV end systolic volume. Terminal measures of plasma BNP increased significantly in TAC mice in association with decreases in EF and increased heart weight, with carvedilol treatment tending to decrease plasma BNP (p = 0.10–0.12). A comparison of carvedilol hemodynamic and structural effects in the mouse TAC model versus clinical use indicates a strong agreement in effect profiles preclinical versus clinical, providing novel and important translational validation for this widely used animal model. The plasma BNP biomarker findings support the incorporation of the measure of plasma natriuretic peptides in the mouse TAC model to extend the translational utility of the model.
Footnotes
Animal welfare
All animal experiments were carried out in accordance with the Guide for the Care and Use of Laboratory Animals as adopted and promulgated by the US National Institutes of Health.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Ethical approval
All protocols for animal experiments were approved by the research laboratories of Merck & Co., Inc., Kenilworth, NJ, USA, Institutional Animal Care and Use Committee.
Funding
The author(s) received no financial support for the research, authorship and/or publication of this article.
