Abstract
Objectives:
A lesion in the spinal accessory nerve is typically iatrogenic: related to lymph node biopsy or excision. This injury may cause paralysis of the trapezius muscle and thus result in a characteristic group of symptoms and signs, including depression and winging of the scapula, drooped shoulder, reduced shoulder abduction, and pain. The elements evaluated in this long-term follow-up study include range of shoulder motion, pain, patients’ satisfaction, delay of surgery, surgical procedure, occupational status, functional outcome, and other clinical findings.
Methods:
We reviewed the medical records of a consecutive 37 patients (11 men and 26 women) having surgery to correct spinal accessory nerve injury. Neurolysis was the procedure in 24 cases, direct nerve repair for 9 patients, and nerve grafting for 4. Time elapsed between the injury and the surgical operation ranged from 2 to 120 months. The patients were interviewed and clinically examined after an average of 10.2 years postoperatively.
Results:
The mean active range of movement of the shoulder improved at abduction 44° (43%) in neurolysis, 59° (71%) in direct nerve repair, and 30° (22%) in nerve-grafting patients. No or only slight atrophy of the trapezius muscle was observable in 75%, 44%, and 50%, and no or controllable pain was observable in 63%, 56%, and 50%. Restriction of shoulder abduction preceded deterioration of shoulder flexion. Patients’ overall dissatisfaction with the state of their upper extremity was associated with pain, lower strength in shoulder movements, and occupational problems.
Conclusion:
We recommend avoiding unnecessary delay in the exploration of the spinal accessory nerve, if a neural lesion is suspected.
Keywords
Introduction
Owing to the nature of its anatomy, the spinal accessory nerve (SAN) is susceptible to injury, 1 typically being an iatrogenic lesion related to a neck dissection. The minority of injuries are due to distension of the nerve or penetrating trauma. SAN provides motor innervation to the trapezius muscle, which acts to elevate, retract, and rotate the scapula. 2 Injury to the SAN can cause weakness or paralysis of the trapezius muscle, leading to loss of trapezius restraint, altered scapular kinematics, and limited shoulder elevation.2–4 In trapezius paralysis, physical examination typically shows weakness in movements of the affected arm above the horizontal plane, especially in shoulder abduction, winging of the scapula, drooping of the shoulder, stiffness of the shoulder girdle, and atrophy of the trapezius muscle. Usually, the patients suffer from shoulder pain, sometimes associated with arm pain and posterior neck discomfort.2,3,5–7
The mean delay from injury to surgical repair has been reported to be 5 months, 8 6 months, 9 7 months,6,10 8 months, 11 11 months, 12 or as long as 13 months.1,13 Controversy continues regarding prospects for good surgical results. Generally, an early procedure (direct nerve repair or nerve grafting) of the SAN, as with other nerves, is most likely to result in the best recovery. If surgery is carried out within a few days of a laceration of the nerve, direct suture is usually possible. Later, neuroma formation occurs, and the ends of the nerve may have retracted, meaning that a nerve graft will be necessary to achieve a tension-free repair.2,14 It is not uncommon that during exploration the nerve is found constrained by a thick scar, but the nerve responds to the electrical stimulus. The role of neurolysis in these cases is debatable.
The objective of this study was to review the long-term results of the surgical treatment of SAN injuries. Range of movement (ROM), pain, and the level of subjective patient satisfaction were assessed in relation to the operative delay, occupational status, functional outcome, and other clinical findings.
Methods
Patients and surgical intervention
We reviewed the medical records of a consecutive 37 patients (11 men and 26 women) undergoing surgery for a suspected lesion of the SAN between October 1978 and December 1994 in Orton Hospital, formerly the Orthopaedic Hospital of the Invalid Foundation, Helsinki, Finland. The SAN injury was confirmed with an electroneuromyography (ENMG) study. Traditionally, the criterion for the pathological finding is the presence of muscle fibrillation and the lack of voluntary motor unit activation. However, these can be blurred by aberrant innervation from cervical plexus.11,15–17 All the patients were preoperatively examined and operated on by M.V. The operation involved exploration of the SAN; if the nerve, when stimulated electrically, showed conduction to the muscle, neurolysis was performed under a microscope. Otherwise, direct repair was performed by a microsurgical technique or, in case of segmental loss, by use of a sural nerve graft. No immobilization was advised after neurolysis, whereas after direct nerve repair or nerve grafting, treatment was 2-week immobilization with an opposite-side neck-shoulder orthosis preventing harmful neck motion.
Follow-up examination
All the patients were contacted and agreed to be reexamined, with no patient dropouts. They completed a questionnaire and were interviewed for pain, with a peripheral nerve injury score: 18 none, controllable (daily activities possible and sleep undisturbed), severe (work interrupted, sleep difficult, and requiring medication), and ungovernable (sleep disturbed regularly and work impossible). Furthermore, numbness anywhere in the upper extremity and changes in occupation were documented. The patients were asked to rate their satisfaction with the state of the upper extremity as excellent, good, fair, or poor. One author (H.G.) examined the patients for trapezius muscle atrophy (no, slight, marked, and complete), winging of the scapula with arm elevated, depression of the shoulder in centimeters, and ROM of the active shoulder. Furthermore, the strength of abduction and flexion with the arm 90° elevated was measured with a spring balance. The study was approved as a clinical follow-up study by the Ethical Board of Orthopaedic Hospital of the Invalid Foundation, Helsinki, Finland.
Statistical analysis
All continuous variables were determined to be non-normally distributed according to the Kolmogorov–Smirnov test. For determining correlations between two continuous variables, Spearman’s rank correlation coefficient served to test statistical significance. For differences between groups, the Mann–Whitney U-test was employed for comparisons between two groups and the Kruskal–Wallis test for three or more groups. For two simple categorized variables, Fisher’s exact test served to test statistical significance. Kendall’s tau or Phi coefficient allowed for more complex cross-tabulations at the ordinal or nominal level, respectively. In all tests, p < 0.05 was considered significant. The analyses are performed for all patients if not otherwise stated.
Results
Description of the patients and surgical procedures
The descriptive statistics are summarized in Table 1. Lymph node biopsy or excision was the most common reason for SAN injury. Of the 37 patients, exploration and neurolysis were carried out for 24. The nerve was repaired end-to-end in nine patients, and four cases required nerve grafting. The time between injury and surgery ranged from 2 to 120 months (mean: 14.4 months). The length of the follow-up period ranged from 2 to 17 years (mean: 10.2 years).
Descriptive statistics.
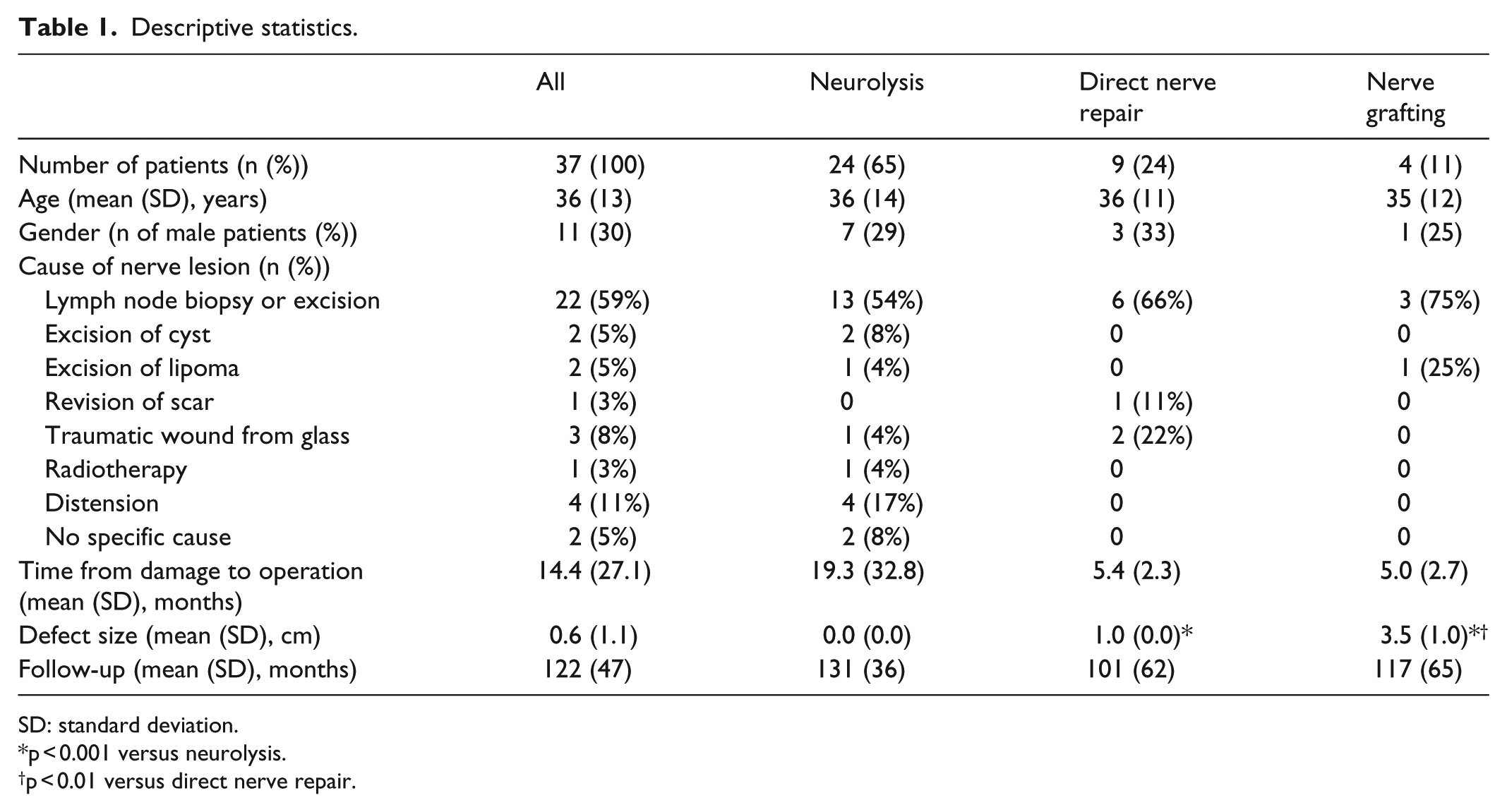
SD: standard deviation.
p < 0.001 versus neurolysis.
p < 0.01 versus direct nerve repair.
ROM and strength of the shoulder
Mean active pre- and postoperative ROM in abduction and flexion and postoperative strength measurements of the shoulder are summarized in Table 2. Figure 1 demonstrates the effect of the time interval between the injury and the operation to ROM recovery. When all patients (i.e. neurolysis patients not excluded) were included in the analysis, a shorter delay was associated with better preservation of flexion (R = −0.400, p = 0.043). Patients operated on within 8 months of the injury sustained flexion, whereas those with a longer delay failed to gain subsequent improvement or even lost their ROM (p = 0.016). Irrespective of surgical delay, abduction was significantly (p < 0.001) higher at the follow-up than preoperatively, also if patients having neurolysis were excluded (p = 0.025). The cutoff point was 8 months for shoulder abduction (p = 0.035). Greater strength in flexion at follow-up was correlated with shorter time elapsed between injury and surgery (R = −0.338, p = 0.041). If patients who went through only neurolysis were excluded from the analysis, the delay of surgery had no statistically significant effect on recovery.
Active range of movements and forces.

ROM: range of movement; SD: standard deviation.
No statistically significant differences between groups.
p = 0.002 between preoperative and follow-up measurements.
p = 0.025 between preoperative and follow-up measurements when direct nerve repair and nerve-grafting groups are pooled.
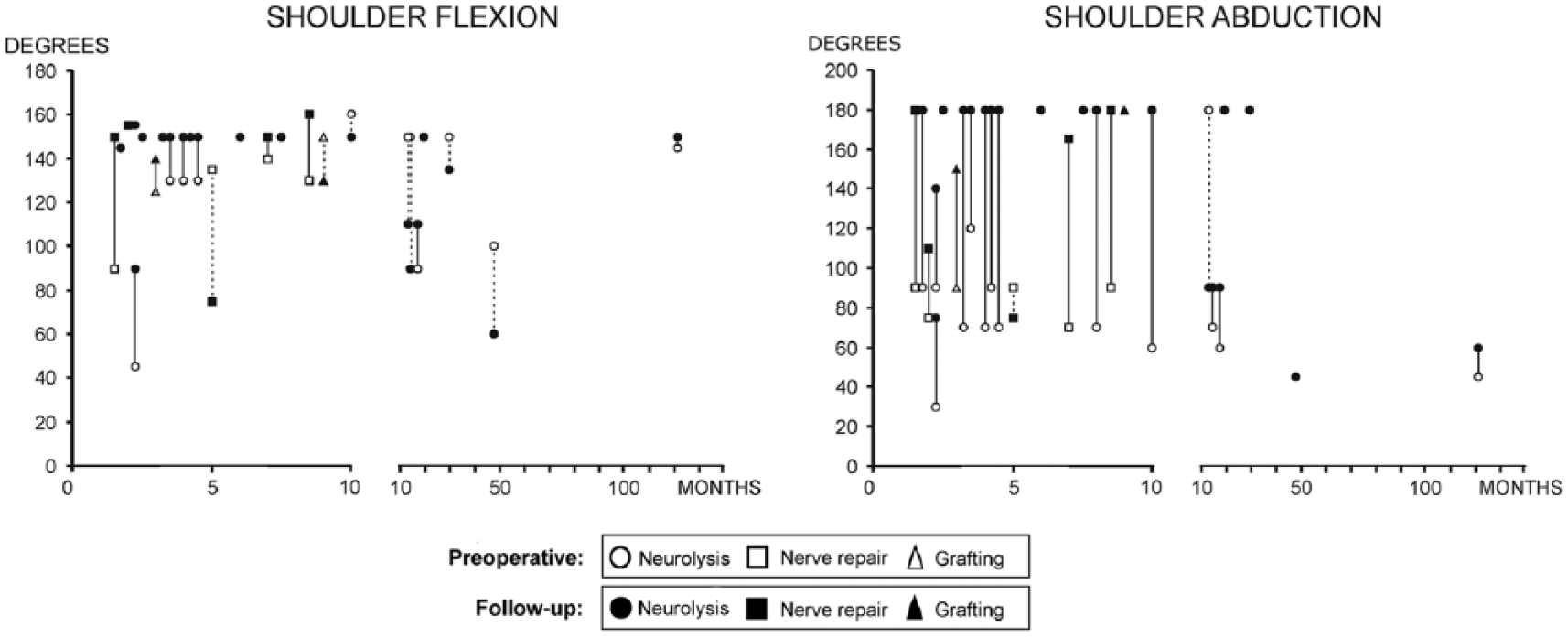
Effect of delay from injury to surgical operation to restoration of active range of movement (ROM) of the shoulder in flexion and abduction. Each symbol represents one patient’s ROM of the shoulder either preoperatively or at follow-up. The solid line stands for improvement and dashed line for the patient’s decline in ROM.
Pain
Patients’ estimation of their pain at the follow-up is demonstrated in Table 3. Severity of pain was associated with older age (p = 0.016), severity of pain preoperatively (p = 0.014), lower strength at follow-up in flexion (p = 0.009) and abduction (p = 0.006), higher rate of occupational problems: subjective working performance (p = 0.003), and change of occupation (p = 0.016).
Subjective pain of the patient at follow-up.
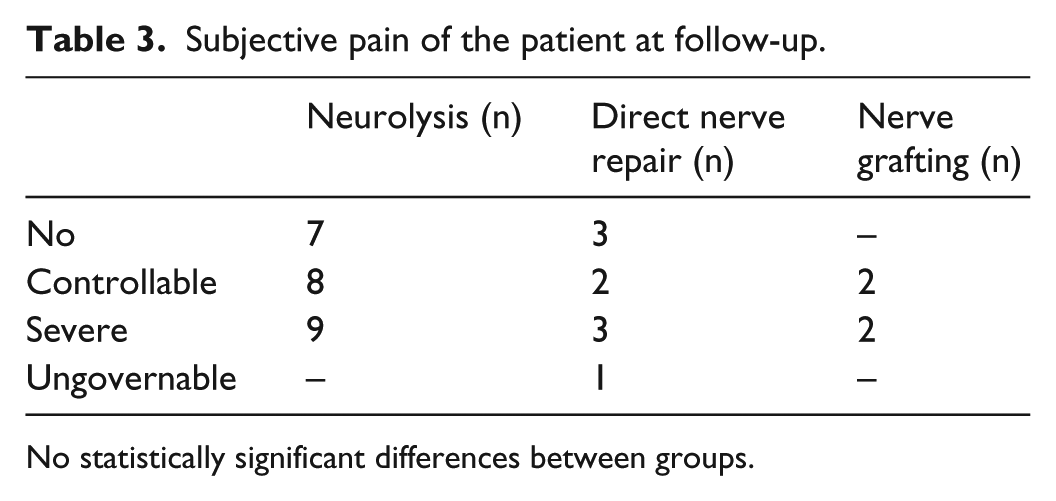
No statistically significant differences between groups.
Patient satisfaction
Subjective satisfaction of the patient with the overall status of the upper extremity is summarized in Table 4. High satisfaction was correlated with greater strength postoperatively (p = 0.028 for flexion, p = 0.010 for abduction) and the absence of winging of the scapula (p = 0.016 in flexion, p = 0.024 in abduction). Similarly, it was associated with less pain (p < 0.001) and better subjective working performance (p = 0.001). Patient satisfaction was not correlated with delay time from the injury to surgery.
Subjective satisfaction of each patient with overall status of the upper extremity at follow-up.

No statistically significant differences between groups.
Occupation
Of the 24 patients with neurolysis, 19 were working before the injury and 7 changed their occupation or retired because of the SAN injury during the follow-up period. The corresponding figures were two of six having direct nerve repair and none among four having nerve grafting. No statistically significant differences emerged between groups.
Atrophy and posture
Severity of the trapezius muscle atrophy at follow-up is summarized in Table 5. At follow-up, of the 24 patients with neurolysis, 3 had winging of the scapula when actively abducting the shoulder, whereas of the 13 patients having either direct nerve repair or nerve grafting, 6 had a winging scapula (p = 0.042). The winging scapula was associated with greater pain (p = 0.043) and numbness anywhere in the upper extremity (p = 0.050). The mean depression of the affected shoulder compared to the uninjured side was 1.8 cm in neurolysis (standard deviation (SD): 1.3 cm), 1.0 cm in direct nerve repair (SD: 1.0 cm), and 2.5 cm in nerve-grafting groups (SD: 1.0 cm). A significant difference (p = 0.043) existed between the direct nerve repair and nerve-grafting groups.
Severity of trapezius muscle atrophy at follow-up.

No statistically significant differences between groups.
Discussion
An iatrogenic injury to the SAN is not uncommon during neck surgery involving the posterior cervical triangle because its superficial course here makes it susceptible. This nerve is most frequently damaged as a complication of a cervical lymph node biopsy or excision. The problem is usually compounded by a failure to recognize the error immediately after surgery when surgical repair has the greatest chance of success.1,19
Clinical presentations of patients with identical lesions of the SAN differ. Differences in retention of some shoulder motor function are attributable to anatomic variations in trapezius innervation because the trapezius may receive contributions from the cervical plexus11,15–17 and compensation by the levator scapulae and rhomboid muscles.3,13 Differences in clinical presentation may create confusion and thus delay diagnosis. The same anatomic variations blur ENMG diagnostics.
According to the literature, good recovery of the trapezius muscle is achievable when the SAN is repaired within 32,9,20,21 or 62,10,22,23 months. However, good results have been reported after surgical delays from 5 to 12 months.6,11,24,25 Furthermore, Teboul et al. 13 reported satisfactory outcomes within a 20-month period after the injury. In a sample of 111 SAN injury patients, no correlation emerged between delay of surgery and outcome, and the maximum delay was over 40 months for a patient who still had a good outcome. 1 Our own patients operated on within 8 months of the injury had improvement in flexion, whereas those with any longer delay gained no subsequent improvement. However, it has to be kept in mind that neurolysis was performed for majority of our patients. Since it is possible that spontaneous recovery plays a major role in recovery of these patients, we cannot know the impact of surgery itself on the final outcome of these patients. Recovery of shoulder abduction was diminished in patients having greater delay than 8 months, and restrictions of shoulder movement in flexion became permanent. Interestingly, as evident in Figure 1, those patients undergoing surgery after a long delay gained no benefit in abduction and seemed, in fact, to lose ROM in flexion during follow-up. This suggests that the changes in active flexion movement are compensatory rather than directly linked to the SAN injury. Patients who have SAN injury can learn to use compensating muscles. Therefore, it cannot be confirmed that the improvement in ROMs is purely due to operation—especially, since the improvement is the most evident among patients who have had a more recent injury.
The differences in the recovery from SAN injury between different types of operation (neurolysis, direct repair, or nerve grafting) were found marginal and only affecting scapular winging. However, it has to be noted that the group sizes were limited, and the statistical power is, therefore, limited. This is particularly true concerning nerve grafting, which could be supposed to yield poorer results than direct repair or neurolysis. The role of neurolysis on recovery is debatable, but since there are no reliable tools to evaluate integrity of small nerves such as SAN without surgery, exploration and subsequent neurolysis are justifiable procedures.
Pain is generally considered one of the main symptoms of SAN injury.1,26 According to Camp and Birch, 1 pain is swift in onset and often severe. They reported 13% of the patients as being painless and 15% as having very strong ungovernable pain before the operative procedure. Postoperatively, 93% of the patients had no or controllable pain, and 3% had very strong pain. We used the same peripheral nerve injury pain score as did Camp and Birch. 1 This score has been shown to have strong concordance with scores of the visual analog scale. 18 However, our results remained inferior to Camp and Birch’s. 1 Of our patients, 59% were painless or had controllable pain. However, similar to their findings, only 3% (one patient) had ungovernable pain after the procedure. Not surprisingly, the dissatisfaction of the patients in the status of their upper extremity was strongly associated with pain, loss of strength, and occupational problems.
This study is burdened by some limitations. Since this is a retrospective study about a condition, where there is a strong consensus favoring operative treatment as soon as the dysfunction and a positive ENMG finding have been noted, a control cohort is an impossibility. Furthermore, although the preoperative examination was meticulous, medical records did not contain data on pain or preoperative ROM of the shoulder for every patient. When patients were seen initially or at follow-up, we obtained no validated functional scores like a Constant–Murley score because these were not in common use 20 or more years ago. We consider that in evaluation of accessory nerve injury, in addition to ROM and strength measurements, atrophy of the trapezius muscle, scapular winging in abduction, and pain are decisive. Furthermore, the long follow-up time may distort the findings since during the 10 years after surgery, additional trauma or degeneration may impair shoulder function irrespective of SAN injury.
We conclude that although after SAN injury partial recovery will take place irrespective of operative delay, it is advisable to avoid unnecessary delay in the exploration of the SAN. Also, patients who had poor recovery of shoulder abduction had marked worsening of shoulder flexion in the long run. This was evident not until the long follow-up period, highlighting the secondary role of trapezius muscle in shoulder flexion.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethics approval
Ethical approval for this study was obtained from the Ethical Board of Orthopaedic Hospital of the Invalid Foundation, Helsinki, Finland (#R19912).
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The institution of the authors has received, during the study period, funding from EVO, HUS (Government grant from Helsinki University Hospital District).
Informed consent
Written informed consent was obtained from all subjects before the study.
Research ethics
The study was approved as a clinical follow-up study by the Ethical Board of Orthopaedic Hospital of the Invalid Foundation, Helsinki, Finland. Each author certifies that his or her institution approved the human protocol for the investigation that all investigations were concluded in conformity with ethical principles of research and that informed consent was obtained for participation in the study.
