Abstract
Background:
Young people’s sexual health decision-making, including decisions to access and adhere to HIV prevention strategies such as Pre-Exposure Prophylaxis (PrEP), are influenced by a range of internal and external factors. Synthesizing these factors is essential to guide the development of youth-focused PrEP health promotion strategies to contribute to international goals of ending HIV transmission.
Objective:
To understand the individual, interpersonal, sociocultural and systemic barriers and facilitators to PrEP access, uptake and use experienced by young people 24 years and younger.
Design:
A systematic review that adhered to the Preferred Reporting Items of Systematic Review and Meta-Analysis Protocols.
Data Sources and Methods:
Eight databases (PubMed, Scopus, Cochrane, Medline, CINAHL, JBI, EMBASE, Web of Science) were systematically searched using terms related to young people, HIV and PrEP use. A narrative synthesis approach was used to delineate key barriers and facilitators to PrEP access, uptake and use.
Results:
Of 11,273 returned articles, 32 met the eligibility criteria for inclusion: 18 from the United States, 10 from African nations and two from Brazil. Barriers and facilitators to PrEP access, uptake and use experienced by young people were identified across intrapersonal, interpersonal, community and systems levels. These factors are described under four overarching themes that relate to knowledge, side effects and perceptions of risk; attitudes and perceptions of family and partners; community attitudes and stigma; and negative healthcare provider experiences and difficulties navigating complex costly healthcare systems.
Conclusion:
Findings suggest individual-level factors need consideration alongside the impacts of healthcare systems and broader systemic sociocultural structures within young people’s relationships when developing PrEP health promotion strategies and services. Without considering these wider external implications to access, uptake and use of PrEP, global targets towards the elimination of HIV transmission will likely remain out of reach.
Registration:
This review was registered with Prospero (CRD42022296550).
Plain language summary
Young people’s sexual behaviours and decision-making can be influenced by interpersonal factors including awareness, adherence, pill burden, and external factors such as parental attitudes/influence, peer/romantic/sexual relationships, community. This in turn can impact their HIV-related risks and prevention strategies they employ. This review aimed to understand the individual, sociocultural and systemic barriers and facilitators to HIV pre-exposure prophylaxis (PrEP) access, uptake and use experienced by young people ⩽24-years. Eight databases were systematically searched using terms related to young people, HIV, and PrEP use. Using a narrative synthesis approach data was delineated into key barriers and facilitators to PrEP access, uptake, and use. Of the 32 papers that met eligibility criteria for inclusion 18 were from the United States, 10 from African nations and two from Brazil. Barriers and facilitators to PrEP access, uptake and use experienced by young people were identified across the individual level, their relationships with family and partners, within the broader community and within healthcare systems. These factors are described under four overarching themes that relate to knowledge, side effects and perceptions of risk; attitudes and perceptions of family and partners; community attitudes and stigma; and negative healthcare provider experiences and difficulties navigating complex costly healthcare systems. Findings suggest individual-level factors need consideration alongside the impacts of health care systems and broader systemic sociocultural structures within young people’s relationships when developing PrEP health promotion strategies and services. Without considering these wider external implications to access, uptake and use of PrEP, global targets toward the elimination of HIV transmission will likely remain out of reach.
Introduction
The transition from adolescence to young adulthood is one that encompasses an array of physical, psychological and social developmental changes.1,2 These changes include internal changes such as increased levels of self-sufficiency, autonomy and personal agency and external changes, such as evolving family/peer relationships, development of romantic or sexual relationships and greater exposure to community and cultural influences. This myriad of factors influences the development of a young person’s sexuality, sexual health decision making and sexual behaviours (including HIV-related risk behaviours).1,3,4 They can also contribute to increased HIV risk by reducing a young person’s ability to seek HIV information and access prevention strategies, including HIV pre-exposure prophylaxis (PrEP). 4 This is of concern when evidence indicates younger people already have lower awareness and knowledge of, and uptake and adherence to, HIV prevention strategies.5–8
Despite global improvements in the scale-up of HIV testing, treatment and prevention, young people remain disproportionately affected by the HIV epidemic worldwide. Young people aged 15–24 years make up 22% of the global population and accounted for over 36% of all new HIV notifications in 2022.9–12 Despite this disproportionate burden, PrEP uptake within this group is lagging in many regions.13–18 Understanding factors that impact PrEP access, uptake and use in young people requires a holistic approach encompassing the nuanced understanding of individual, sociocultural and structural barriers that young people experience. This understanding can be garnered through the use of various frameworks such as the socioecological model (SEM) – which can be useful to explore the array of factors that can influence PrEP access and uptake and the interactions across the various levels of an individual’s life experiences. 19 In previous applications of the SEM within the HIV context these levels have been identified as synergistically influencing PrEP access in adults from priority populations. 19 Understanding these factors across an individual’s intrapersonal (individual), interpersonal (parents, partners, peers), community and structural (healthcare systems) experiences – particularly among priority subgroups (e.g. young MSM, young women) – is imperative in guiding successful interventions that improve access and uptake of HIV prevention methods.9,20
Provision of PrEP to young people has expanded in many regions (e.g. United States, Australia, Canada, France, Kenya, Eswatini),21–26 but to ensure young people have equitable access to PrEP, a nuanced understanding of their barriers and facilitators to PrEP access, uptake and use is essential. The purpose of this mixed-method systematic review was to conduct a narrative synthesis of the individual, interpersonal, systemic, and sociocultural barriers and facilitators to PrEP access, uptake and use experienced by young people ⩽24 years. 27 To our knowledge, this is the first article to review PrEP access and uptake experiences with young people globally. These findings will delineate strategies to ensure young people are not left behind in the race towards global fast-track targets to end the HIV epidemic by 2030. 28
Methods
Review registration
The review was registered with Prospero (PROSPERO 2022 CRD42022296550) to investigate two research questions: (1) What are the patterns of PrEP use among young people aged ⩽24 years? and (2) What are the factors influencing PrEP access, uptake and patterns of use among young people aged ⩽24 years? Upon reviewing the search yields, research question 1 was not explored given inadequate reporting of patterns of use among young people aged ⩽24 years globally.
Search strategy
This review adhered to the Preferred Reporting Items of Systematic Review and Meta-Analysis Protocols (PRISMA). The initial search strategy was devised by three authors (SW, JD, JF) in consultation with university library staff experienced in systematic searching to refine search terms relating to young people, HIV and the use of PrEP (Supplemental Table 1). Eight databases were systematically searched (PubMed, Scopus, Cochrane, Medline, CINAHL, JBI, EMBASE, Web of Science) in January 2022 and were re-run in May 2024. To further identify potential studies, backwards and forwards reference search of the included studies was conducted.
Inclusion criteria and study selection
To align with international definitions of young people used by The Joint United Nations Programme on HIV/AIDS (UNAIDS) and the World Health Organization (WHO),29,30 articles that discuss PrEP access, uptake and use in young people aged 24 years and younger were included. To be eligible articles needed to specifically stratify results to young people 24 years and younger. Studies published in peer-reviewed journals, written in English, and encompassing all study methodologies were included.
Endnote 20 31 was used to combine database searches. Title and abstract reviews were completed by the first author (SW), with a random review of 10% by a second author (JF) to ensure reliability and consistency of paper inclusion. Discrepancies were resolved through group deliberation. Full-text review was completed by the first author (SW), with all excluded articles checked by the second reviewer (JF).
Data extraction, analysis and quality assessment
A narrative synthesis approach was used to systematically review and synthesise the qualitative and quantitative data using a textual approach in order to ‘tell the story’ from the findings of the included articles. 32 The analysis was guided by the methods described by Popay et al. 32 A data extraction table was used to extract descriptive details from each study and identify the key barriers and facilitators from each paper to help determine similarities across the studies. A preliminary analysis was then used to code the similarities across four components of the SEM – intrapersonal/individual (knowledge, attitudes and perceptions), interpersonal (parents and partners), community (stigma and social support) and structural (healthcare systems) 19 – and was reviewed by all authors with all discrepancies deliberated as a team. A narrative synthesis using a thematic analysis approach was then used to develop groupings of similar codes to form an understanding of how each component influenced PrEP access, uptake and use independently and simultaneously within young people.
The included studies were critically appraised using the Mixed Methods Appraisal Tool (MMAT) version 2018. 33 The MMAT tool provides a validated quality appraisal tool for reviews that include multiple study designs including qualitative, quantitative and mixed-methods. 33 The overall quality rates for each study are provided in Supplemental Table 2.
Results
Initial searches yielded 8837 articles, and the updated search identified an additional 2936 (total yield = 11,273), which were refined to 32 articles from 23 separate studies/programmes (Figure 1). Table 1 summarises the descriptive details of the included articles. Eighteen of the articles were from the United States and 12 in countries across the Africa region (including Kenya (8), South Africa (3), Uganda (2), Zimbabwe (1), Namibia (1) and Tanzania (1)) and two from Brazil. Eighteen articles reported findings that used qualitative methods (e.g. in-depth interviews, focus groups),34–51 eight used quantitative methods (e.g. cross-sectional surveys, randomised controlled trial)52–59 and six articles were multi-methods/mixed-methods designs.60–65

PRISMA flow diagram.
Characteristics of included articles.
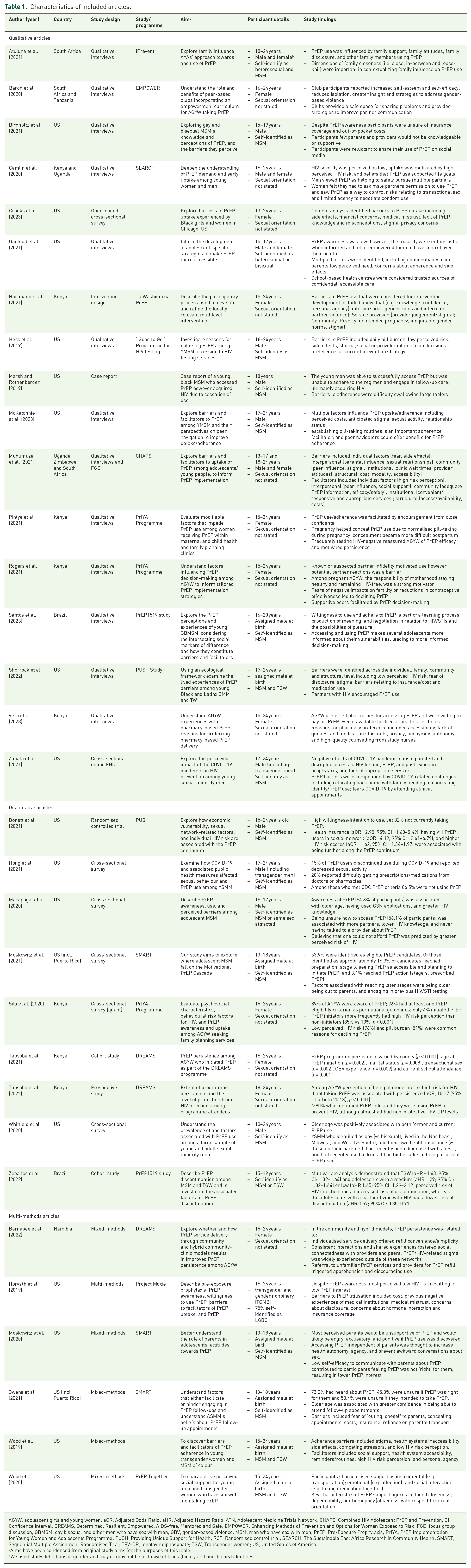
AGYW, adolescent girls and young women; aOR, Adjusted Odds Ratio; aHR, Adjusted Hazard Ratio; ATN, Adolescent Medicine Trials Network; CHAPS, Combined HIV Adolescent PrEP and Prevention; CI, Confidence Interval; DREAMS, Determined, Resilient, Empowered, AIDS-free, Mentored and Safe; EMPOWER, Enhancing Methods of Prevention and Options for Women Exposed to Risk; FGD, focus group discussion; GBMSM, gay bisexual and other men who have sex with men; GBV, gender-based violence; MSM, men who have sex with men; PrEP, Pre-Eposure Prophylaxis; PrIYA, PrEP Implementation for Young Women and Adolescents Programme; PUSH, Providing Unique Support for Health; RCT, Randomised control trial; SEARCH, The Sustainable East Africa Research in Community Health; SMART, Sequential Multiple Assignment Randomised Trial; TFV-DP, tenofovir diphosphate; TGW, Transgender women; US, United States of America.
aAims have been condensed from original study aims for the purposes of this table.
bWe used study definitions of gender and may or may not be inclusive of trans (binary and non-binary) identities.
Overall, five of the quantitative articles reported that young age was significantly associated with lower PrEP awareness, use and persistence. This was observed across all age groups when comparing young people to older adults (younger than 18/19 years compared to those ages 19/20 and older)52,57 and within groups of young people (14/15 year olds compared to 18 year olds).54,55,58 Thematic analysis of the 32 studies provides nuance to this finding that young people are significantly less likely to be aware of, and adhere to, PrEP for HIV prevention, and delineates the socioecological challenges and supports impacting young people. These themes and their identified subthemes are described in detail below and presented in Table 2. Quotes selected from the qualitative articles are used to provide context and voice to young people.
Summary of narrative synthesis on the barriers and facilitators to access, uptake and use of PrEP in young people.

HCP, healthcare providers; PrEP, pre-exposure prophylaxis.
Knowledge, perceptions and experiences influence PrEP use
Fifteen qualitative articles35–47,61,65 and five of the quantitative articles,53,54,56,59,63 discussed the intrapersonal factors that impact PrEP access, uptake and use in young people. These factors included knowledge and awareness of PrEP, inconvenience, pill burdens, and perceptions of risk.
Is PrEP for us and is it worth the hassle? – Knowledge perceptions, and experiences of young people influence PrEP use
A lack of awareness of PrEP and uncertainty around its efficacy was reported in four articles involving young people from the United States.38,39,41,61 and six articles from African nations.35,37,40,44–46 Two quantitative articles involving young people from the US found reluctance to take PrEP was associated with lower HIV knowledge,
54
and lower PrEP awareness.54,63 Young people reported uncertainty of PrEP efficacy and perceived condoms to be more effective.39,41,46 Young women from African nations raised concerns about PrEP reducing the efficacy of hormonal contraceptives, and misconceptions about the effects of the ‘chemicals’ in PrEP on pregnancy outcomes and breastfeeding.35,45,46 Young women in the US reported fears that PrEP may interfere with natural adolescent development or worsen pre-existing conditions.
38
A lack of representation of young people, and specific populations of young people in advertisements and endorsements, reinforced the idea that PrEP is not for them.36,44 For example, young women in the US described not being aware that PrEP was available to women.
38
Young people reported that PrEP use by peers seen through social media was a motivator for use.
43
. . . .I think it requires campaigns to be done in the population like you moving around encouraging young people to take PrEP and you people telling us why it’s good. (female 21 years; Zimbabwe)
44
Confidence in PrEP efficacy and normalisation of its use was gained by young people across Africa, through user experience, testing negative at follow-up appointments37,45,46 and awareness of use and testimonies from within the community.37,46 However, young people from across these settings described aversion to taking pills39,42,44,45 and difficulties swallowing large PrEP pills.39,42,44,45 Sila et al. (2020)
56
reported among their cohort of adolescent girls and young women in Keyna, that 51% declined PrEP due to pill burden. The need for periodic follow-up appointments resulted in PrEP being considered a ‘burden’ or a ‘hassle’ not worth the effort.36,39,41,44,45 For others, there were anticipated struggles with adherence due to forgetfulness39,45; lack of a daily routine or inconsistent schedules39,49; being away from home39,44,49; limited privacy to take pills
44
; and changes in circumstances.39,45 Incorporating PrEP into one’s routine (e.g. with other medications) or using phone reminders (although participants reported these could be easily ignored) were reported to facilitate adherence.43,45,47 Macapagal et al. (2020)
54
reported that a reluctance to use PrEP due to fear of side effects was significantly associated with lower HIV knowledge, and never having heard of PrEP before their study. Additionally, experiences of side effects (including dizziness, fatigue, nausea, diarrhoea) led to discontinuation.37,39–41,44–46,47,49,
54
,61,65
Even if you just bring tablets and put them there, I just vomit. Some may fear to take PrEP tablets and say that “I rather fall sick with the thing [HIV] than taking those tablets.” (female 13–17 years; Uganda)
44
Not ‘risky’ enough to take PrEP – Perceptions of HIV risk impacts PrEP uptake
Perceptions surrounding personal risk were discussed in fifteen of the articles across the three contexts (African,37,44,45,49,56 the United States36,41,43,53–55,61,65 and Brazil47,59). Barriers to use and discontinuation were significantly associated with low perceived HIV risk54,56,59 and reductions sexual behaviours – despite Hong et al.
53
reporting that 53.5% still meet national guideline criteria for PrEP. In qualitative findings PrEP use was associated with perceptions of being ‘promiscuous’ and only needed for those with multiple sex partners or engaging in risky sexual practices.36,41,44,45,47,6 Young people from Kenya and Uganda described not feeling scared of HIV and expressed greater fears of other things such as accidental pregnancy or cancer.
37
Some youth now days do not see HIV/AIDS as a serious disease, just because they know there is ARVs [antiretrovirals]. Some youths say, “even if I contract HIV I will go to [the] health center and start taking ARVs.”. . .For girls, they are mostly scared about pregnancy and the boys are only scared of being imprisoned for having impregnated a girl. (male; 15-24 years; Uganda)
37
A higher perception of risk, having higher numbers of sexual partners and engagement with STI/HIV testing lead to increased PrEP awareness and uptake.43,47,49,54–56,58,65 For young women in Kenya, Uganda, Zimbabwe and South Africa, partners having sex outside the primary relationship increased the perceived risk of HIV, motivating them to seek PrEP for their personal protection.35,37,44,49
Gatekeepers versus cheerleaders – The impact of interpersonal relationships on PrEP use
Fifteen qualitative34–37,39–41,44–48,51,62,63 and eight quantitative articles52,54,55,56,57,59,62,63 provided findings on the positive and negative impacts of interpersonal relationships (family/partners) on attitudes and perceptions towards PrEP that act as ‘cheerleaders’ and facilitators by promoting a sense of acceptance and support or ‘gatekeepers’ and barriers that fostered attitudes, perceptions and environments where young people felt pressure to conceal use due to fear of judgement and harm.
The ‘freedom’ to use PrEP – Family attitudes led to concealment or support for PrEP use
Young people from both the United States36,39,51,62,63,65 and African settings34,35,37,44–46 reported parental and family concerns of PrEP use, including efficacy and side effects, 34 having sex under 18-years or before marriage,44, 62 misperceptions that PrEP was used to ‘sleep around’,37,62,63 that PrEP was an illegal substance or believed that it was used for HIV treatment (not prevention).34,35,62 Fears about repercussions and punishment for sexual identity and behaviours,62,63 or physically being prevented from using PrEP (e.g. confiscating pills, throwing pills out)34,37,44 led to ‘sneaking around’ to conceal use34,35,39,44,51,62,63 or leaving PrEP at friends’ houses. 34 Being able to discreetly take PrEP (such as transferring the pills into another bottle), increased autonomy and agency while avoiding parental/family gatekeeping and judgement.45,47,62 In the United States, Moskowitz et al. 62 reported that among their samples 62.9% would use PrEP if their parents would not find out, and Owens et al. 63 found that parental support was significantly associated with greater confidence in PrEP adherence. Within these two studies over 80% of participants reported they would definitely or probably access PrEP if provided for free and able to use with discretion (e.g. parents not finding out).62,63
Young people in the United States described fears around parents being unsupportive of sexual identities or not being ‘out’ to parents as a barrier to access and uptake.36,48,51,62,63,65
You’re afraid to even ask your parents, it’s like basically saying, ‘Oh, I want to have gay sex’. And so it’s something that I try and find a way to discreetly do without my parents knowing if possible. And if it’s not possible, it’s probably something I’d just not do. (assigned male at birth; 15 years; U.S.)
36
Young people from Africa34,35,37,45 and the United States55,62,63 reported having supportive family members and listing them as clinic contacts
34
enabled the ‘freedom’ to maintain PrEP use by supporting appointments attendance34,63 and adherence reminders.34,35,45 Parents support of sexual orientation/behaviours enabled young people to feel more comfortable discussing their sexual health needs34,55,62 and encouraged them to seek PrEP.
34
Parental support helped young females in Kenya37,45 and Uganda
37
conceal PrEP use from male partners, helping mitigate the lack of support and HIV risk from partners.
I actually shared [my PrEP use] with my mum. . . .I had a lot of quarrels with my husband and I had to run back to my mum’s house . . . So my mum sat me down and told me that there is no need to keep running away all the time. That I should stay put because it is men’s nature to wander away [have outside partners] when they have cash. She advised me that I should look for a way to protect myself [against HIV] (female; 20 years; Kenya)
45
Do I need my partners permission to use PrEP?
Young women from regions of Africa35,37,40,44–46,52,56,57 reported that partners’ accusations of infidelity,37,
44
–46 scepticism/misperceptions about partner’s HIV status35,37,45,46,56 and traditional power imbalances or normative gender roles37,44 influenced perceptions of risk and autonomy to access PrEP. Partners engaging in practices such as concurrent sexual partners35,37,45 and polygamy
37
increased young women’s perception of their HIV risk. Engaging in transactional sex was also found to be associated with higher PrEP use across both quantitative52,54,56,57 and qualitative articles.
37
Difficulties in condom negotiation,37,44,45 experiences of physical violence35,40,46,57 and reports of partners hiding, confiscating or discarding PrEP pills35,45 made young women feel they needed to seek permission from male partners to take PrEP
37
and/or resort to concealment of use.35,37,40 Such experiences of gender-based violence were significantly associated with lower PrEP persistence.
57
On my side, when I tell my partner that I use PrEP and he does not agree, I will use it secretly. Because these drugs are in bottles and to them, they feel they are ARVs. And because of that, he keeps beating me all the time and because of that I am forced to use them secretly in hiding. (female; 23 years; Kenya)
40
PrEP use for some female participants was motivated by future plans such as finishing school, having a family, preventing vertical transmission and staying healthy and alive to look after their current children,37,45,46 particularly if they felt partners behaviours placed them at risk.45,46 Young people in Brazil described PrEP use as unnecessary while being in a monogamous relationship and ‘building trust’ with their partner.
47
Being able to maintain privacy/discretion when taking PrEP was also a facilitator for use, such as convincing partners it is medication for pregnancy.
45
Quantitative findings indicated that PrEP use was also significantly associated with having a sexual partner who uses PrEP
52
with qualitative findings reporting young people describing support from partners also taking PrEP or living with HIV.35,37,44–47,52,56
My husband is also taking his medicine [ARVs] at the same time with me, so I have not seen any difficulty [in remembering to take PrEP]. Sometimes if I forget, he reminds me. Sometimes my phone alarm might go off and he reminds that it is time [to take PrEP]. (female; 24 years; Kenya)
45
Communities can discourage use – Community stigma can be overcome by supportive peers
Seventeen qualitative articles from across the three contexts (African nations, 35,37,40,44,46,50,60 the United States38,39,41,43,48,51,61,62,65 and Brazil,
47
) described how community attitudes and stigma prevented PrEP use. Community attitudes and peer disapproval made young people feel discouraged and ‘embarrassed’ of PrEP use35,37,39,41,44,48,60 and fearful of people thinking ‘you have the disease [HIV]’39,65 or being labelled ‘dirty’, a ‘whore’ or as you ‘sleep around’35,37,38,41,43,60,62 along with fear of judgement, rumours regarding pill recognition,37,43,44 and being seen attending clinics.37,44,50 One paper from the US described how posting PrEP use on social networking and partner meeting sites was viewed as promoting condom non-use and risky behaviour and was met with negative reactions which led to discontinuation.
48
And when I say that I take PrEP, she [a friend] thinks that I have sex with everyone under the sun, and that’s why I take PrEP. There’s much prejudice to a person who takes PrEP (male; 17 years; Brazil).
47
Eight African-based articles35,37,42,44–46,56,60 and two from the United States42,64 reported on the positive benefits of community, social clubs/groups. Peers provided support through improving PrEP awareness, providing connection and shared experiences, and support for PrEP uptake and continuation.35,37,44,60,64 Such support was particularly helpful for participants who had to hide PrEP use from partners.35,37,56 Support in the form of a ‘treatment buddy’ (someone to take pills with) or partner provided motivation, encouraged the incorporation of PrEP into daily routine and helped young people to remember to take pills and maintain adherence.45,60,64 Having had a sexual partner who used PrEP was significantly associated with PrEP awareness, uptake and use.
52
Witnessing PrEP use among community peers aided in normalisation, encouraging and empowering young people to use PrEP and attend clinics.35,44,46
The best way for them [peers] to use it is when they see me using it. . .Yaahh, they want protection, they need to see me having used it and am alive. Then they will say let’s go boys and we get them [PrEP pills] together (male; 19-21 years; Zimbabwe).
44
Some young people39,43,46,47,62,65 rejected stigma as a barrier, opinions of others were insignificant in their decision-making process. PrEP was viewed as part of their general wellness with one participant describing ‘If you want to not become sick, you eat oranges. So PrEP is my oranges.’
65
Young people claimed personal agency and autonomy, identified as important factors in personal decision-making and use of PrEP.
I feel like you should just be happy that I’m trying to prevent getting HIV instead of worrying about what I’m doing. I feel like as long as I’m taking care of my health, there shouldn’t be a problem. (female; 16 years; United States)
39
The healthcare system paradox – The healthcare system itself limits healthcare access
Twenty articles that included nine qualitative articles36,38,39,41,51,61–63,65 and five quantitative articles53,54,58,63 from the United States, six of the qualitative articles from African nations35,37,40,44,46,50 and one qualitative article from Brazil 47 reported on the impacts healthcare systems and healthcare providers had on access and use of PrEP. These included difficulties navigating healthcare systems, negative experiences, healthcare provider stigma, confidentiality fears and costs associated with accessing medication.
Similar difficulties accessing healthcare were reported across regions of Africa and the United States including proximity to healthcare providers and pharmacies offering PrEP,37,39,41,44,46,49,50 clinic closures,50,51 long clinic wait times,44,50 health centres running out of medications,
44
a lack of access to affirming healthcare
51
and reliance on parent transportation.
63
I live in a conservative rural community and have to drive a long way to a supportive care facility, I just choose to not take PrEP at all right now because of the frequent required visits. (male; 17-24 years; United States)
51
The need for 3-monthly follow-up appointments was seen as inconvenient, unmanageable, and resulted in scheduling conflicts with school/going away for school, extracurricular activities, and unanticipated events.36,37,39,49,61,63,65 Confidentiality fears were shared by young people in African settings around healthcare provider disclosure of PrEP use to parents.37,44
Financial barriers were also described across the three settings,35,38,39,41,43,44,46,47,51,61–63,65 including medication costs, travel to clinics, healthcare costs, and unstable employment, and living costs. For young people in the United States, further hesitancy occurred through the inability to afford PrEP without the use of parental health insurance, creating fears of raising parental suspicions, and unwanted breaches of confidentiality, especially if young people are not ‘out’ to their parents about their sexual identity or behaviours.38,39,41,51,58,62,63,65 Unexpected financial strain associated with loss of employment, unstable income, moving and the need to prioritise other essential expenses (e.g. food) also affected PrEP use.35,38,44,51
If you know that you are not sick you will say let me go do something else with that money and you overlook your health. . . .if not for paying [for PrEP] then it will be very easy for me. (female 17 years; Uganda).
44
Providing PrEP at low/no cost, at local clinics/pharmacies and without the need for a prescription was described to make PrEP attainable for young people,38,44,50,62,63 while circumventing unwanted parental disclosure. 61 Having spoken with healthcare providers about PrEP, 54 and access to one’s own health insurance were significant predictors of greater awareness and access to PrEP.52,58 School/college-based health clinics that assured confidentiality and required no parental involvement,39, 51 proximity to affordable local clinics, school-based clinics, PrEP provided through pharmacies and affirming care also made it easier to adhere to PrEP and follow-up appointments.39,44,46,50,51
HCP practices and attitudes influence care – Negative experiences led to medical mistrust
Across both the United States36,51,61 and African settings37,40,44 young people described negative experiences with healthcare providers (HCP), including judgement or discrimination of ‘lifestyle’, sexual orientation, or sexual partners numbers36,40,44,51 and even positive health-seeking behaviours such as regular testing.
36
Provider-related barriers including lack of HCP knowledge,
36
unsupportive and non-affirming care,36,51 HCPs not providing PrEP to some key populations such as bisexual men
51
and HCP beliefs (e.g. strong religious beliefs) deterring sexual identity disclosure
36
were identified as factors that could impact access to PrEP.
36
There was one time that it wasn’t my primary care doctor. It was a different doctor. . . . and she spoke heavily religiously and was telling me, because she thought I had depression, she was saying going to church would help that. And I felt in my mind if she believes this as a doctor and is recommending this to me, I probably should not tell her about being gay (assigned male at birth; 17 years; United States).
36
These negative experiences meant that the commonly used words such as ‘speak to your doctor for more information’ were a deterrent for young people who did not feel comfortable speaking with their healthcare provider. 36 Support provided by healthcare providers, such as adherence focused support, PrEP adherence counsellors and regular reminders helped young people maintain adherence.60,65 Having trust in their provider and being offered practical advice about side effects, how to discontinue and re-initiate PrEP, and guidance on missed dosages was a facilitator to use. 60 Providing information enables young people to feel empowered to continue PrEP when faced with challenges such as side effects, stigma, and help educate family and partners to support use. 60
Discussion
This review found that factors affecting access, uptake and use of PrEP in young people occur across multiple levels including intrapersonal factors (e.g. knowledge, personal attitudes), interpersonal (parents, partners), community (stigma, community support) and structural (healthcare systems).13–16 The synthesis of findings highlights that young people experience commonalities in barriers and facilitators associated with access and uptake of PrEP across low- and high-income countries. While these commonalities are clear, the specific experiences of young people based on their sociocultural contexts should not be overlooked.
At an interpersonal level, key themes identified included limited awareness and knowledge of PrEP uptake and use, 66 even in contexts where young people are known to be at higher HIV risk.3,9,13,14,29,67 As evidenced in studies included in this review and other literature, there are greater disparities in PrEP knowledge linked to younger age groups.3,66,67 HIV prevention and PrEP initiatives that include education and media (including television, internet and social media) campaigns aimed at young people have been shown to be effective at not only improving awareness, but also willingness and use of PrEP.68,69 There is need for concerted efforts to improve PrEP awareness and knowledge among young people and consider the implementation of such strategies with more targeted approaches to education and promotion of PrEP towards young people to increase awareness and uptake.
Our study highlighted how perceptions of risk vary among young people, but strongly influenced decisions to use PrEP, especially when there is absence of peer representation in PrEP promotion. Currently promotion of PrEP largely relies on people being able to accurately self-identify HIV risk.70,71 Accurate risk perception has been defined as a fundamental component in determining engagement with protective behavioural changes, thus inaccurate perceptions can impede engagement with HIV prevention.4,72–75 While inaccurate perceptions of risk are known to occur in populations of adults and young people, younger people have a greater likelihood of inaccurately identifying their personal risk.4,74 This combined with findings presented in this paper suggest that current promotion and framing PrEP around individual risk of HIV may not be adequately reaching young people. 76
Our synthesis of research found that some young people articulated PrEP use as empowering, rejecting negative reactions and stigma from others. Prevention strategies that places emphasis on individual behaviour change in young people without consideration of social, cultural and systemic factors (e.g. stigma, financial limitations or poverty, education, healthcare access) that can impact HIV transmission, access to care and create a sense of personal fault that coincides with infection.77–79 Representation of young people as stakeholders in the development and design of interventions and messaging is critical to ensure PrEP-related promotion is acceptable and sustainable.80,81 Framing of HIV prevention outside of individual behaviour changes is needed, with more focus on promoting community and systems change that support the ability and empowerment of young people to make positive sexual health decisions.82–84 The efficacy of PrEP access, uptake and use within some populations is based on targeted messaging (e.g. among MSM in Australia85,86), however for some groups this may perpetuate stigmas that PrEP is associated with particular identities or persons engaging in particular ‘behaviours’. 76 Thus, while targeted messaging is effective, universal health promotion messaging could be effective in reaching boarder populations of young people by removing the emphasis on risk associated only with particular identities or behaviours. 76
Young people face challenges with HIV-related medication adherence, and those accessing PrEP also have reduced rates of medication adherence, difficulty in adapting to a daily pill-taking regimen and higher rates of discontinuation of use compared to adults.4,8,87 This is reflected in our findings along with aversion to taking pills and challenges attending follow-up appointments. Across study settings of the included articles and in other literature,25,88–91 the use of support groups, peers/peer-led support and ‘treatment buddies’ were reported to be beneficial in improving medication adherence and improving adherence for follow-up appointments, increasing personal agency, mitigating stigma, reducing isolation, providing side-effect support and increasing open communication about HIV. Expanding adherence support through the use of mobile apps, modifiable or flexible PrEP refill schedules, and the integration of PrEP into other health services could help overcome challenges in clinic attendance and follow-up while also increasing access and convenience for young people regardless of where they live.92–96 Few studies described the patterns of PrEP use in young people, highlighting a direction for future research.
Our study highlights the pervasive effects of stigma that surrounds HIV and PrEP and the urgent need to acknowledge and address such stigma. Decision-making in young people is often influenced by their social acceptability, interactions with interpersonal relationships and the broader community.4,67,97 Stigma surrounding PrEP use largely overlaps stigma and perceptions around sexual behaviours.98–100 Including PrEP use as part of positive sexual health plans and risk-reduction packages targeted towards young people could be an important step towards reducing stigma, increasing education and supporting uptake and continuation of PrEP.98,101 The development of personal agency in young people through positive sexual health decision-making and encouraging protective behaviours can also result in lower rates of other sexually transmissible infections and increased HIV testing.102,103 Early development of these protective behaviours and ownership over one’s sexual health can promote longevity of these behaviours into adulthood and facilitate greater sexual health communication with partners and engagement with prevention strategies.103–105 Our study showed that perceiving PrEP as a positive choice in protecting oneself or family facilitated use and adherence. Therefore, it is important to reframe HIV prevention and PrEP as a positive and proactive sexual health choice.101–103
Our findings highlight that it is critical to include families, partners, peers and broader community members in PrEP awareness strategies. Support from family, partners and community, and open discussions surrounding sexual health and HIV have been associated with increased awareness and willingness to use PrEP among young people – as well as reductions in PrEP-related stigma.97,106–109 However, peers, partners, family and broader community members can also be gatekeepers or prevent PrEP uptake.82,110,111 Therefore, co-designing HIV prevention strategies with young people in collaboration with their broader intergenerational community networks may help facilitate culturally congruent uptake and effective use of PrEP and enhance related health literacy. 80
This review highlights the importance of considering power discrepancies and gender roles associated with traditional sociocultural normative beliefs and attitudes, particularly among young women. Social support services were reported to help young women navigate these cultural and societal factors, parental and partner influence, gender roles, gender-based violence and inabilities to negotiate condom use – factors known to impact HIV risk and PrEP use in this population.25,112,113 Social/peer support, both formal and informal outside of the family and partner network has been found to effectively increase personal agency of young people in relation to their sexual health and communication, increasing protective behaviours, HIV prevention and willingness to access PrEP.3,99,103–105,114,115 In contexts where PrEP use is often linked to sexual identity (being MSM), PrEP use can lead to unwanted exposure or being ‘outed’, 116 such models of peer and social support can provide safe spaces for young people to feel engaged, validated, share experiences and navigate difficulties in maintaining PrEP use.94,115,117,118
Healthcare systems can create multiple and cumulative barriers for young people accessing PrEP and HIV services both in high- and low-income contexts accessing PrEP and HIV services.90,119,120 Actual or perceived HCP stigma can adversely impact access to HIV prevention/treatment services. Access is further barred by costs associated with clinic attendance and PrEP medications.99, 120 –122 Financial barriers can be exacerbated for young people who commonly fall into the lowest income bracket. 123 Financial dependence on parents or guardians can create barriers through concerns around confidentiality.3, 124 –126 The provision of PrEP at no or subsidised costs for young people has been linked to an increased willingness to use PrEP, 69 and is effective in national uptake of PrEP.69,127–129 Young people in our included studies cited perceived costs as barriers to uptake, it is important that young people are made aware of programmes that can offer PrEP for free to support access and uptake. For example, young people in the United States can access Ready, Set, PrEP 130 a programme offering free PrEP to people without health insurance in the United States. Support is needed for HCP to overcome barriers to the provision of PrEP to young people such as lack of awareness, reduced sense of need in young people and lack comfortability in initiating sexual health and HIV conversations.3,131–134 However, reducing medication and health service cost alone is not sufficient. Our review emphasises the need to consider travel costs and other related cost barriers such as living expenses and unstable or loss of employment. HCP need to be aware of the risk and stigma facing young people trying to access PrEP and their duty of care to provide equitable access to supportive non-judgemental healthcare that ensures confidentiality.99,122 Additionally, expanding PrEP delivery through non-traditional models of care (e.g. through nurse-led and pharmacy-led PrEP) can be effective in overcoming some of these challenges for young people by improving accessibility, anonymity and autonomy.135,136
The findings highlight how young people experience intersecting barriers and facilitators to PrEP uptake, use and adherence. Clearly, future research and practice need to be collaborative with young people to design strategies to overcome barriers and facilitate access. Research and practice must also engage with the broader holistic sociocultural context of young people to create meaningful change. Summarised in Table 3 are key recommendations for practice, research, and policy based on our findings to guide collaborative and holistic health promotion strategies and interventions with young people.
Key recommendations for practice, research and policy to support PrEP access, uptake and use in young people.

PrEP, pre-exposure prophylaxis.
Strengths and limitations
This study provides insight into the differing impacts that young people face in access and use of HIV prevention, however the inclusion of articles from only African nations, the United States and Brazil, limits the generalisability of our findings within other geographical and sociocultural contexts. The articles included in this review did not report other factors around the age of consent or laws pertaining to healthcare or medications, which could further impact access to services and PrEP.2,126
Conclusion
There is a need to move beyond prevention efforts that address only individual-level barriers to PrEP for young people. PrEP health promotion strategies and services need to consider the impacts of social, cultural and systemic structures on HIV transmission and prevention in young people. There is a need for a multiprong approach, supported by appropriate legislation, policy, and systems, designed to increase PrEP awareness across all ages, develop supportive social networks within interpersonal networks and the wider community, and improve PrEP service delivery and access. Improved access to affordable age appropriate culturally congruent, affirming PrEP services is imperative to support the needs of young people. Without considerations for these wider implications to access, uptake and use of HIV prevention and PrEP, global targets towards the elimination of HIV transmission by 2030 will remain out of reach.
Supplemental Material
sj-docx-1-tai-10.1177_20499361241303415 – Supplemental material for Pre-exposure prophylaxis access, uptake and usage by young people: a systematic review of barriers and facilitators
Supplemental material, sj-docx-1-tai-10.1177_20499361241303415 for Pre-exposure prophylaxis access, uptake and usage by young people: a systematic review of barriers and facilitators by Sarah Warzywoda, James A. Fowler, Amalie Dyda, Lisa Fitzgerald, Amy B. Mullens and Judith A. Dean in Therapeutic Advances in Infectious Disease
Supplemental Material
sj-docx-2-tai-10.1177_20499361241303415 – Supplemental material for Pre-exposure prophylaxis access, uptake and usage by young people: a systematic review of barriers and facilitators
Supplemental material, sj-docx-2-tai-10.1177_20499361241303415 for Pre-exposure prophylaxis access, uptake and usage by young people: a systematic review of barriers and facilitators by Sarah Warzywoda, James A. Fowler, Amalie Dyda, Lisa Fitzgerald, Amy B. Mullens and Judith A. Dean in Therapeutic Advances in Infectious Disease
Footnotes
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
