Abstract
Powassan virus (POWV), a tick-borne flavivirus transmitted primarily by Ixodes ticks, poses a significant threat as it can lead to severe neuroinvasive illness. This review delves into the nuanced clinical presentation of Powassan infection, a challenge in diagnosis exacerbated by the absence of an available vaccine. Over the past decade, the prevalence of POWV has surged in North America, necessitating a thorough examination of its neurological manifestations alongside tick-borne encephalitis virus (TBEV). A comprehensive literature search conducted up to January 2024 revealed 135 cases of neurological symptoms associated with either Powassan or TBEV infection. Notably, severe occipital headache emerged as the most prevalent symptom (22.75%), followed by meningoencephalitis (10.34%), seizures (8.27%), and flaccid paresis (6.8%). Additional manifestations included poor balance, wide gait, dysarthria, facial nerve palsy, seizure, slurred speech, and absent deep tendon reflexes. Tragically, nine cases resulted in fatal outcomes attributed to POWV infection. This analysis highlights the intricate spectrum of neurological symptoms associated with Powassan infection and underscores the necessity for heightened awareness among medical practitioners, particularly in regions with a higher prevalence of the virus. The complexity of symptoms emphasizes the need for further research to unravel the factors contributing to this diversity. Additionally, exploring potential treatment avenues and vaccine development is crucial in addressing the rising threat posed by POWV, ultimately enhancing our ability to manage and prevent severe neurological outcomes.
Keywords
Introduction
Powassan virus (POWV), belonging to the Flavivirus genus, is closely akin to tick-borne encephalitis virus (TBEV), which has been extensively studied in both Europe and Asia, with more than 10,000 cases, posing an increasing threat to public health. In humans, TBEV induces central nervous system (CNS) infections, with the potential for severe consequences, including lasting neurological complications and, in some cases, fatality. 1 Like TBEV, POWV is transmitted by ticks and can inflict significant damage to the nervous system. Its recognition as a human pathogen dates back to 1958, originating from the isolation of the virus in the brain of a young child who succumbed to encephalitis in Powassan, Ontario.2,3 The virus is categorized into two distinct lineages: lineage 1 (POWV), found in North America and far Eastern Asia, and lineage 2 (DTV), exclusively present in North America. Despite representing two genotypes of the same virus, these lineages cannot be differentiated through serological methods.3,4 Ticks from the Ixodes genus, including species like Ixodes cookei (lineage 1), Ixodes marxi (lineage 1), and Ixodes scapularis, also known as the black-legged or deer tick (lineage 2), act as the primary carriers of the POWV. Graphical representation of the Powassan virus (POWV) Encephalitis is depicted in Figure 1. The virus is transmitted to humans through the bite of an infected tick, which has previously been fed to animals such as groundhogs, squirrels, mice, or other rodents carrying the virus in their bloodstream.5,6 In addition to the recognized transmission modes, there exist alternative pathways, including trans-stadial transmission, vertical transmission to offspring and transmission through infected milk, through which the POWV may propagate. Integrating these lesser-explored transmission routes into ongoing research and surveillance endeavors holds the promise of attaining a more holistic comprehension of POWV dynamics.7,8
Graphical representation of the POWV encephalitis.
Due to the POWV’s diverse clinical presentation and the absence of precise diagnostic techniques that match the intensity and complexity of the disease, this virus is regarded as a diagnostic challenge. The POWV currently lacks a vaccine, thus individuals who are afflicted only get supportive care and symptomatic therapy. 2 While the POWV has historically been infrequent, there has been a notable surge in cases over the past decade in both the United States and Canada. In the United States, the majority of POWV cases have been concentrated in the New England and Great Lakes regions. Specifically, the highest annual case counts are reported in Minnesota, Wisconsin, Massachusetts, and New York. 9 Typically associated with a 10% mortality rate post-infection, survivors often grapple with enduring neurological consequences, affecting at least 50% of those who recover. 4 Despite its relative rarity, POWV cases have been consistently documented each year since the confirmation of the first case in Minnesota in 2008. In 2021, Minnesota reported five instances of Powassan viral disease, all presenting severe neurological conditions – either meningitis or encephalitis – resulting in two fatalities. Individuals afflicted with such extreme cases commonly endure persistent medical issues, including recurrent headaches, loss of muscle strength and mental challenges.10,11 The prevalence of long-term outcomes is observed in approximately half of individuals with encephalitis or meningitis, with 10–15% of cases ultimately resulting in death. 10
An imperative demand for in-depth research and analysis on this flavivirus, particularly concerning its neurological manifestations, arises due to the existing gaps in our understanding of the POWV and its neurotropic properties. Conducting a comprehensive study could yield advancements in diagnostic methods, alternative treatments and potentially even the development of a vaccination. Our focus will extend beyond Powassan to include the tick-borne encephalitis (TBE) virus, given the limited availability of studies on Powassan, as we aim to scrutinize the neurological symptoms associated with these viruses.
Methods
Data sources and search strategy
This study followed the 2020 Preferred Reporting Items for Systematic Review and Meta-Analysis (PRISMA) guidelines 12 shown in Figure 2.

PRISMA flowchart.
We used MESH phrases and ‘AND’ and ‘OR’ to conduct an organized literature search in PubMed, Google Scholar, and Cochrane Library. We used the following search terms:
Powassan AND [‘encephalities’ (All Fields) OR ‘encephalitis’ (MeSH Terms) OR ‘encephalitis’ (All Fields)]. Our objective was to encompass studies exploring neurological manifestations akin to those associated with POWV or TBEV, even if not explicitly tied to POWV itself.
Study selection and eligibility criteria
Without regard to language, we accessed databases from their creation until January 2024. Studies that matched the following PICOs criteria were included in our analysis: (1) Individuals with a medical history featuring neurological manifestations similar to those linked with the POWV, even if not directly connected to Powassan, are included. This encompasses patients discussing symptoms or diseases comparable to those associated with TBEV. (2) Following infection, some individuals had incident encephalitis. (3) Case-reporting and case-series publications that describe the symptoms and (4) articles in English should be evaluated for inclusion. Following studies were excluded: Reports without a prior history of encephalitis or situations when encephalitis had already existed before the infection. (1) Articles in which the authors concluded that a different aetiology may account for encephalitis, (2) case-unspecific studies, and (3) abstracts or articles that were not available as full text.
Data extraction
Two investigators (SR and UZ) independently extracted the following information from each included study: study characteristics (first author, year of publication, country, sample size, and study type) and participant baseline characteristics. Any disparities among the reviewers were resolved through group discussions, continuing until a consensus was achieved.
Risk of bias and quality assessment
Two authors (SR and UZ) independently assessed the risk of bias in the included studies using the Murad scale. This evaluation considered six evidence-based criteria, examining aspects such as selection, representativeness of cases, ascertainment of outcomes and exposure, and comprehensive reporting. 13 The questions utilized for the assessment of each study can be found in Supplemental Table S1. The classification of study bias was determined based on the number of criteria met. A study was categorized as having a low risk of bias if all six criteria were met, a moderate risk of bias if five or four criteria were met, and a high risk of bias if three or fewer criteria were met. 14 The corresponding scores for each study can be found in Supplemental Table S1. Any discrepancy between data extractions was resolved by the discussion or consultation with the third author (AF).
Results
Literature search
The study selection process is illustrated in Figure 2, which presents a thorough PRISMA flowchart. 12 Following the preliminary literature search, a total of 5246 articles were identified. After removing 326 duplicates, 4920 articles underwent screening. Upon screening, 4765 were excluded based on title and abstract review. After the full-text screening of 155 studies, 101 studies15 –115 were deemed appropriate for inclusion in this Review. The main characteristics of the included studies such as demographic data (age and gender), study design, publication year, study location, time of infection, incubation period, and time from onset of symptoms to diagnosis are presented in Tables 1 and 2, respectively.
Study characteristics of the included studies.

POWV, Powassan virus; TBEV, tick-borne encephalitis virus.
Summary of symptoms, time from onset of symptoms to diagnosis and overall survival.
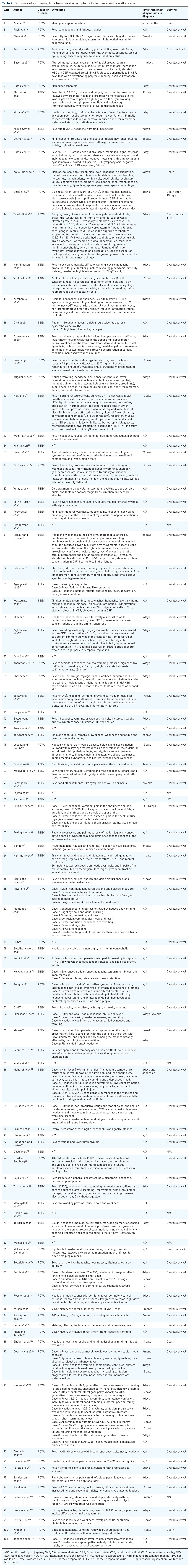
ADC, Antibody–drug conjugates; AMS, Altered mental status; CRP, C-reactive protein; CSF, cerebrospinal fluid; CT, Computed tomography; EEG, Electroencephalogram; FLAIR, fluid-attenuated inversion recovery; MRC, Medical research council; MRI, Magnetic Resonance Imaging; N/A, not available; POWV, Powassan virus; TBE, tick-borne encephalitis; TBEV, tick-borne encephalitis virus; URI, Upper respiratory infection; WBC, white blood cells.
Study characteristics
The review comprises an analysis of 101 studies that involve patients discussing symptoms or illnesses related to either the POWV or TBEV across a multitude of countries. These studies comprise a mix of case reports and case series, varying from individual instances to multiple cases within a series. The countries under investigation exhibit a wide-ranging diversity, spanning the USA, Sweden, Croatia, Russia, Germany, Poland, Switzerland, England, Denmark, Belgium, France, Austria, Italy, Netherlands, Finland, Saudi Arabia, Norway, Bulgaria, Turkey, Australia, Ireland and specific regions such as New York and Europe presented in Table 1.
Quality assessment
Murad scale was employed to evaluate the risk of bias in the included studies. 13 The majority of studies demonstrated either a low or moderate risk of bias represented in Supplemental Table 1.
Neurological manifestations
The dataset comprises a diverse array of research conducted in various countries, including the USA, Sweden, Croatia, Germany, Poland, and Japan, among others. This extensive geographical representation greatly enriches our potential for developing a thorough comprehension of how the infectious agent impacts distinct populations. The gender distribution observed across studies, wherein some investigations specifically focus on males, females, or both genders, adds a layer of complexity to our understanding. The age spectrum underscores the broad demographic diversity encapsulated in the data. Notably, specific cases within the studied populations provide in-depth age-related information.
It is imperative to acknowledge the variability in symptom reporting across studies, resulting in disparate patient counts for each symptom. Collectively, the data from these studies encompass 135 patients exhibiting neurological symptoms associated with either the Powassan or TBEV infection, as outlined in Table 3. The possible window for contracting the POWV spans from as soon as 1 week to as long as 1 month after exposure. Following infection, there is an incubation period lasting 2–4 weeks before observable symptoms manifest. In contrast, for TBEV, the incubation period ranges from 1 week to 3 weeks. However, the duration between the onset of these symptoms and the formal diagnosis exhibits variability, contingent upon factors such as diagnostic test availability, the strength of healthcare infrastructure, and the level of awareness among healthcare providers. Consequently, the time required to confirm a POWV infection may vary across diverse geographical locations and healthcare settings.
Prevalence of patients’ neurological complications.

Among the various symptoms observed, a severe occipital headache emerged as the most prevalent, affecting approximately 33(22.75%) (Table 3) of the patients. This particular finding holds critical importance as these intense headaches can substantially diminish patients’ quality of life and necessitate prompt medical intervention. Following closely, meningoencephalitis was identified in approximately 15(10.34%) of the patients. Meningoencephalitis characterized by inflammation of the brain and meninges was diagnosed. Meningoencephalitis is a severe condition that demands urgent medical treatment to prevent potential complications and mitigate the risk of long-term neurological deficits. Seizure was observed in 12(8.27%). Flaccid paresis refers to the weakening or loss of muscle tone, a condition that can lead to varying degrees of paralysis was observed in 10(6.8%) The implications of flaccid paresis can be particularly debilitating for patients, as it can severely hamper their ability to perform daily tasks and maintain their independence (Table 3).
Additionally, poor balance was reported in approximately 9(6.20%) of patients, potentially indicating impairment within the cerebellar or vestibular systems. These symptoms underscore the complexity of neurological involvement in the infection and highlight the need for multidisciplinary approaches to assessment and management. Wide gait was observed in approximately 3(2.06%) (Table 3) of the patients, suggesting difficulties in walking. Accurate diagnosis and targeted interventions are essential to address the underlying causes of these walking difficulties and to improve the patient’s overall mobility and functional independence.
Several other notable neurological symptoms were observed among the patients. Facial nerve palsy and absent deep tendon reflexes each was reported in 6(4.13%) of the cases. Facial nerve palsy signifies disruptions in normal neurological functioning and can range from mild to severe manifestations. The absence of deep tendon reflexes also raises concerns about potential nerve or muscle involvement and requires thorough evaluation.
Dysarthria, characterized by difficulty in articulating speech was observed in 6(4.13%) of the cases. Similarly, slurred speech affected around 5 (3.44%) (Table 3) of the cases, providing further insight into the infection’s impact on regions associated with speech production and motor control.
Overall survival
Among 135 patients, 9 cases (6.66%) resulted in fatal outcomes attributed to POWV infection, as outlined in Table 2. Specifically, a 63-year-old immunocompromised male with follicular lymphoma undergoing maintenance rituximab therapy passed away on the 14th day, according to Solomon et al. Additionally, Birge et al. reported the death of a 67-year-old woman, who had a medical history notable for colon cancer, on the 13th day. Tavakoli et al. documented the demise of a 62-year-old man with a 4-year history of chronic lymphocytic leukaemia–small lymphocytic lymphoma (CLL–SLL) on the 17th day. McLean et al. recorded the tragic passing of a 5-year-old boy on the fourth day of hospitalization. Gholam et al. documented the demise of a previously healthy 64-year-old man who had reported a headache persisting for the last 3 days, accompanied by a fever (38.9°C). Additionally, he had been experiencing drowsiness and slurred speech in the preceding day. The cause of death, as established through autopsy, was identified as a substantial pulmonary embolism. Kroopnick et al., Yu et al., Kakoullis et al. and Cavanaugh et al. have independently documented cases resulting in mortality attributed to POWV. The overall survival rate remains at 94.81%. Nevertheless, several patients encountered complications, including paralysis, tremors, cognitive defects and other issues, detailed in Table 3.
Discussion
The POWV, a tick-borne flavivirus, is a significant public health concern due to its potential to cause severe neuroinvasive disease in humans. In our comprehensive review of 101 studies discussing symptoms or diseases similar to those associated with either POWV or TBEV with concurrent neurological manifestations, our findings indicate that individuals of any age group can acquire POWV infection, but elderly individuals exhibit a higher susceptibility to neuroinvasive illness, with a slight male predominance. Those showing symptoms undergo an incubation phase lasting 2–4 weeks, followed by a febrile prodrome characterized by manifestations such as sore throat, sleepiness, headaches, and confusion. Timely diagnosis and intervention are imperative to mitigate complications and avert long-term neurological deficits. The presence of various other neurological symptoms, such as dysarthria, facial nerve palsy, seizure, and absent deep tendon reflexes, further emphasizes the complexity of POWV infection and its diverse effects on the CNS. These symptoms can lead to significant disability and require comprehensive management by healthcare professionals. In serious cases, side effects of ataxia, quake, muscle shortcoming, oculomotor and pseudobulbar paralysis have been depicted. 15 In addition to neurological complications, eye involvement, though rare, can present with symptoms such as non-granulomatous anterior uveitis, vitreous inflammation, and retinal haemorrhages, along with bilateral multifocal chorioretinitis.30,88
According to a case report, a 58-year-old man visited the emergency department due to occipital headaches and balance problems, followed by vision loss in his right eye 6 weeks after reporting a tick bite. 30 His eye examination showed non-granulomatous anterior uveitis, vitreous inflammation and retinal haemorrhages without macular swelling or papillitis. 30 Another case, involved a 51-year-old man who had a history of chronic bilateral noninfectious anterior and sporadic uveitis. 88 He was receiving treatment involving mycophenolate mofetil and adalimumab. In May 2017, he underwent a sudden alteration in his mental state accompanied by a high fever of 104°. Subsequent lumbar puncture confirmed the presence of distinct antibodies (IgM and neutralizing IgG) specific to the POWV. 88 This finding indicated that the virus was responsible for inducing bilateral multifocal chorioretinitis characterized by linear clustering within his eyes, resembling the pattern observed in eyes affected by the West Nile Virus.
Mendoza et al. conducted a retrospective study at Mayo Clinic, encompassing 16 cases of neuroinvasive POWV. The study revealed a slight predilection for older and male patients. The diverse clinical presentations included rhombencephalitis (6), isolated meningitis (4), meningoencephalitis (3), meningoencephalomyelitis (2), and opsoclonus myoclonus syndrome (1). The diagnosis was typically established around a median of 18 days after the onset of symptoms. The observed mortality rate was 18.8%, and a substantial 72.7% of survivors exhibited enduring neurologic deficits. 116 This study stands as a comprehensive exploration of neuroinvasive POWV cases, emphasizing the importance of recognizing varied presentations and potential long-term consequences.
Despite the increasing number of cases and the severity of neurological effects related to Powassan infection, substantial obstacles persist in both diagnosing and managing this virus. One key hurdle is the varied clinical presentation, which can imitate other neurological disorders or arboviral infections. Furthermore, currently available diagnostic techniques for POWV lack specificity that matches the intricacy and gravity of the disease. As a general principle, there are no distinctive clinical indicators to differentiate POWV disease from other arboviruses. 3 Notably, the brainstem, spinal cord, cerebellum, cerebral cortex and basal ganglia have all been noted as areas of specific damage, although previous reports did not incorporate a semi-quantitative evaluation of inflammation. Less commonly, instances of inflammation in the thalamus, hippocampus and white matter have been documented. 15 Interestingly, only one case reported an adverse outcome, tragically resulting in fatality. Our observations indicate that these symptoms often follow a self-limiting trajectory, which corresponds with existing research emphasizing the impact of factors such as the patient’s age, occupation, epidemiological context, and underlying health conditions on the outcome.
Medical professionals in areas where POWV is prevalent should possess knowledge about the virus and consider conducting serologic tests on blood or cerebrospinal fluid (CSF) specimens at state or other laboratories equipped to handle POWV testing. When POWV RNA is detected, the pathological and molecular findings imply a combination of direct viral-induced CNS neuronal damage along with broad-ranging lymphocytic inflammation and microgliosis involving the leptomeninges and brain tissue. 20 It is essential for medical practitioners to remain attentive in identifying these signs, particularly in regions like the USA with documented POWV prevalence. Recognizing exposure to ticks is pivotal in facilitating the diagnosis. Additionally, there is an apparent expansion in the geographic distribution of POWV infections. Timely identification and suitable treatment have the potential to notably enhance patient outcomes. By recognizing the pivotal elements that contribute to the diversity in symptoms, healthcare providers can customize their strategies to offer more individualized and efficient care for those affected.
This study has certain limitations that warrant acknowledgment. Firstly, the information included in each case relies on the reporting from individual studies, and in several instances, the data were incomplete. The literature search strategy was crafted to comprehensively address neurological manifestations, not strictly tied to the POWV. It’s important to note that the term ‘tick-borne flaviviruses’ is occasionally used as an umbrella term, encompassing both the POWV and those linked to TBEV. Moreover, despite the absence of reported POWV cases in the EU, European countries were included based on studies examining symptoms or diseases similar to those associated with TBEV.
Conclusion
In conclusion, POWV is an emerging tick-borne flavivirus that can cause severe neuroinvasive disease in humans. The neurological presentations associated with Powassan infection are diverse and can have debilitating effects on patients. Early recognition of symptoms, especially severe occipital headaches and flaccid paresis, is critical to prompt appropriate diagnostic testing and intervention. Therefore, further research is imperative to develop more accurate diagnostic tools, effective treatments and potentially a vaccine. Public health efforts to control tick populations and educate the public about the risks of POWV are essential to reduce the incidence of infection. Further, subsequent research endeavours could involve conducting more focused studies in European regions aimed at discerning the prevalence or absence of the POWV. By fostering collaboration among researchers, healthcare professionals, and public health authorities, we can advance our understanding of POWV and develop strategies to mitigate its impact on affected communities.
Supplemental Material
sj-docx-1-tai-10.1177_20499361241247470 – Supplemental material for A comprehensive neurological perspective on tick-borne flaviviruses, with emphasis on Powassan virus
Supplemental material, sj-docx-1-tai-10.1177_20499361241247470 for A comprehensive neurological perspective on tick-borne flaviviruses, with emphasis on Powassan virus by Areeba Fareed, Samia Rohail, Ushna Zameer, Abdul Wahid, Syed Muhammad Muneeb Akhtar and Waniyah Masood in Therapeutic Advances in Infectious Disease
Footnotes
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
