Abstract
Background:
Little is known about the preferences for antiretroviral therapy (ART) administration methods, such as oral daily pills or long-acting injectable (LAI) options, as well as preferences for pre-exposure prophylaxis (PrEP) administration methods among people without HIV in Latin America.
Objectives:
This study aimed to assess the preferences for ART administration methods among people with HIV and PrEP methods among those without HIV, as well as to examine the correlations and reasons for these preferences.
Design:
We conducted a cross-sectional web-based questionnaire between April and July 2021, using social media accounts of a HIV non-governmental organization. The questionnaire was open to all adults living in Argentina, irrespective of their sexual orientation or gender identity.
Methods:
The questionnaire included questions on substance use, depression, chronic treatment, previous experiences with injectable medication, and HIV status. Those with HIV answered questions about ART adherence and their preferences for ART methods, while those without HIV were asked about condom use, awareness of PrEP, and their preferences for PrEP methods.
Results:
Out of 1676 respondents, 804 had HIV, and 872 did not. Among those with HIV, 91.5% expressed a high preference for LAI-ART, with significantly higher preferences among participants with higher educational levels, cisgender gay, bisexual, and queer men, younger individuals, and those with prior injectable medication experience. Among those without HIV, 68% preferred LAI-PrEP, and this preference was positively associated with previous positive experiences with injectable medication.
Conclusion:
The strong preference for LAI-ART suggests the potential for improved adherence and well-being among people with HIV. Additionally, the preference for LAI-PrEP among those without HIV emphasizes the importance of considering this option for HIV prevention strategies. This study highlights the need to offer diverse methods for ART and prevention to accommodate different preferences and improve health care outcomes in Latin America.
Keywords
Introduction
HIV has had a significant impact on Latin America, where it is estimated that more than 2 million people have contracted the virus. 1 In this region, the HIV epidemic disproportionately affects cisgender men who have sex with men (MSM), transgender women, and sex workers. Yet, despite extensive efforts to combat the epidemic, challenges persist due to a confluence of factors, including poverty, stigma and discrimination, lack of quality health care, inequities in access to antiretroviral therapy (ART), and the added strain of the COVID-19 pandemic. 2 In Argentina, where an estimated 140,000 people are living with HIV, the prevalence among transgender women is approximately 34%, among MSM it ranges from 12% to 15%, and among sex workers it ranges from 2% to 5%. As new cases continue to be identified, a broad spectrum of cisgender women and transgender people is affected. The distribution of new HIV diagnoses by gender between 2019 and 2021 was as follows: 60.4% for cisgender men, 29.3% for cisgender women, and 1.2% among transgender people. 3
Long-acting medications, such as contraceptives, have been delivered effectively and widely by injectable methods for over 50 years. Long-acting injectable (LAI) are well-known for their ability to promote adherence, maintain consistent medication levels in the bloodstream, and reduce the dosing frequency. 4 Moreover, in the last decade, there have been significant advances in the HIV field, with studies involving LAI options for antiretroviral administration, proving their safety and effectiveness in HIV management, both for therapy and prevention.5–7
LAI-based ART (LAI-ART) is viewed mainly positively by communities, donors, and policymakers as a means of tackling stigma and poor adherence.8–10 Among people living with HIV, LAI-ART has garnered acceptance, offering a possible liberation from concerns about missed doses, pill fatigue, and disclosure. Notably, people with higher education, younger age, and who identify as MSM, have shown a greater inclination toward LAI-ART.8,9,11,12 This newfound enthusiasm is echoed in Argentina. In a recent questionnaire, 83.5% of patients at a healthcare center in Buenos Aires have expressed willingness to transition from oral ART to monthly LAI-ART if provided the option. Feedback from participants in clinical trials conducted in the country underscores the convenience and discretion offered by LAI-ART. These aspects alleviate the daily reminder of one’s HIV status and the risk of unintended disclosure, emerging as key factors influencing the choice of this method.6,13
Beyond the scope of treatment, antiretrovirals have also emerged as a potent tool for pre-exposure prophylaxis (PrEP) against HIV infection for the most affected groups. Long-acting PrEP (LAI-PrEP), administered via injection, has exhibited safety, efficacy, and superiority over oral daily PrEP in clinical trials.14–19 In studies conducted in Brazil and Peru, LAI-PrEP would be the most chosen option, while in Mexico, it ranked second compared to oral PrEP. 20 In another qualitative study in Brazil, high interest in LAI-PrEP was demonstrated, linked to the elimination of barriers such as pill burden and greater autonomy in the healthcare system. 18 Barriers were mentioned to a lesser extent compared to advantages and included issues related to fear of needles, lack of knowledge about effectiveness, and side effects. 18
As Argentina struggles with restricted access to oral PrEP and limited awareness of LAI-PrEP, a recent implementation study of oral PrEP revealed an initiation rate of 52% among eligible individuals from the key population. This rate aligns with the acceptability reported in other countries within the region. 13 In this context, gaining a comprehensive understanding of preferences becomes crucial. Preferences are influenced by the intricate interplay of various psychosocial factors, including but not limited to convenience, confidentiality, and health-related concerns. 13
Given these considerations, the goal of this study is threefold: first, to assess the preference of ART administration methods among people with HIV and PrEP methods among those without HIV; second, to examine the correlations with demographic and psychosocial factors; and third, to describe the motives driving method preferences.
Methods
Study design
A cross-sectional web-based questionnaire was conducted using Surveymonkey.com® (SurveyMonkey Inc., San Mateo, CA, USA) between April and July 2021.
Setting and sample
Participants were recruited through the social media platforms of a non-governmental organization (NGO) dedicated to HIV and sexual and reproductive health. The extensive reach and engagement of this NGO’s social media accounts facilitated the inclusion of a wide range of people from diverse backgrounds and regions across Argentina.
Participants were required to meet two primary criteria: (1) age of 18 years or older, and (2) current residency in Argentina. The participants that did not meet the criteria, were disqualified and not permitted to complete the remainder of the questionnaire. Regarding the missing values, incomplete questionnaires were discarded (respondents with >90% of unanswered questions).
Data collection
Instrument
The questionnaire items were developed drawing from the factors associated with ART and PrEP method preferences found in existing literature aiming to design a questionnaire that was both comprehensive and short for online administration. Additionally, a multidisciplinary research team, consisting of a pharmacist, a physician, a psychologist, and community members who worked as peer navigators within the NGO, contributed by proposing subjects and questions they considered pertinent to the topic. Moreover, the peer navigators tested the final web-based questionnaire to ensure its clarity and cultural appropriateness.
The final questionnaire included the following variables (Table 1): socio-demographic questions, sexual orientation and gender identity, substance use, depression symptoms, presence of chronic treatment, previous use of injectable medication, perception of experience with injectable medication, and HIV status.
Variables and questions.

ART, antiretroviral therapy; LAI, long acting injectable; PrEP, pre-exposure prophylaxis; STI, sexually transmitted infection.
In addition, following the inquiry regarding awareness of PrEP, the questionnaire incorporated a concise explanation about PrEP to provide participants with the necessary information to make informed responses about their preferences for methods of administration. The questionnaire included predefined options for preference reasons, along with an open-ended ‘other’ option for providing additional details or reasons.
Data analysis
The data was analyzed for two distinct groups: people with HIV and their preferences regarding LAI-ART or pills, and for people without HIV and their preferences for LAI-PrEP or pills. Sexual orientation and gender identity responses were grouped to simplify the analysis and to facilitate the interpretation of the results. The following groups were formed: cisgender gay, bisexual, and queer men; cisgender heterosexual men; cisgender lesbian, bisexual, and queer women; cisgender heterosexual women; and transgender and non-binary people. Frequencies and percentages were calculated for categorical variables, and medians and interquartile ranges (IQRs), for continuous variables.
Statistical analyses were performed using Statistical Package for the Social Sciences v29.0 (IBM Corporation, Armonk, New York, USA). 21 Given that data was not normally distributed, the Mann–Whitney U test was used for comparisons between groups. To explore variables associated with preference of LAI versus pills, Chi-square tests were conducted, calculating the odds ratios (ORs) and their confidence intervals (CIs). Variables with expected frequency in each cell not less than 5, Fisher’s test was used. The influence of confounding factors on the analysis was corrected by evaluating the OR in the unadjusted and adjusted setups. The OR values in unadjusted and adjusted setups assessed the influence of multiple confounders or one specific confounder on the outcome of LAI preference. The significance level was set at 5%. Significant parameters in bivariate analyses were included in the multivariable analysis (logistic regression).
Results
Sociodemographic characteristics
Of a total of 1940 who opened the questionnaire’s link, 6 (0.3%) did not accept the informed consent, 34 (1.7%) reported being younger than 18 years of age, and 81 (4.2%) did not live in Argentina, resulting in 1819 eligible participants. In total, 1676 (92.1%) of those who started the questionnaire completed it and were included in this analysis as the final sample size.
Sociodemographic characteristics are presented in Table 2. Participants were young (median = 33 years, IQR = 28–41), 40.1% self-identified as cisgender heterosexual women, 6.8% as cisgender lesbian, bisexual, or queer women, 5.1% as cisgender heterosexual men, 42.8% as cisgender gay, bisexual, and queer men, and 5.2% as transgender or non-binary people. Almost all respondents (94.2%) completed secondary school, 94% were born in Argentina, 54.8% lived in AMBA (Area Metropolitana de Buenos Aires/Metropolitan Area of Buenos Aires) and 98.2% received injectable medication before. Nearly half of the sample (48%) were people with HIV and 52% were people without HIV or unknown status.
Characteristics of the total sample (n = 1676).

AMBA, Area Metropolitana de Buenos Aires-Metropolitan area of Buenos Aires; GBQ, gay, bisexual, and queer; IQR, interquartile range; LBQ, lesbian, bisexual, and queer.
Preference for LAI-ART among people with HIV
As is shown in Table 3, a total of 804 people with HIV completed the questionnaire with a median age of 35 years (IQR: 30–43). Most of them were cisgender gay, bisexual, or queer men (62.4%), 98% were receiving ART of which 58% reported taking an ART consisting of two or more pills per day. Regarding the preference for ART modality, almost all people with HIV (91.5%) preferred LAI-ART (13.4% of them injectable every 2 months and 78.1% every 6 months) and 4.1% to continue with pills. Preference of LAI-ART was high in all gender/sexual orientation groups: 94.8% cisgender gay, bisexual, or queer men, 87% cisgender heterosexual women, 85.1% transgender and non-binary people, 84.6% cisgender heterosexual men, and 84.2% cisgender lesbian, bisexual, and queer women.
Characteristics of the sample and correlates associated with the preference of LAI for ART in people with HIV (n = 804).

Fisher’s exact test.
AMBA, Área Metropolitana de Buenos Aires-Metropolitan area of Buenos Aires; ART, antiretroviral therapy; GBQ, gay, bisexual, and queer; IQR, interquartile range; LAI, long acting injectable; LBQ, lesbian, bisexual, and queer; OR, odds ratio.
Boldface indicates statistical significance.
Multivariable analysis of predictors and correlates of LAI-ART preference
Logistic regression analyses were conducted to identify predictors of LAI-ART preference. The model is shown in Table 4. Goodness-of-fit tests were used to evaluate the suitability of the logistic regression model. Score and omnibus test values were statistically significant (p < 0.05). The model showed adequate goodness of fit according to the Hosmer and Lemeshow statistical value (p > 0.001), meaning that the model conforms to the goodness-of-fit criteria. The Nagelkerke R2 value showed that 10% of the total variance of the model was explained.
Multivariable logistic regression analysis of factors associated with preference of LAI for ART in people with HIV (n = 804).

Cox and Snell R2 = 0.043, Nagelkerke R2 = 0.098, −2 Log likelihood = 430.096.
ART, antiretroviral therapy; CI, confidence interval; GBQ, gay, bisexual, and queer; LAI, long acting injectable; LBQ, lesbian, bisexual, and queer; LGBQ, lesbian, gay, bisexual, and queer; OR, odds ratio; Ref, reference value.
Boldface indicates statistical significance.
The regression coefficient β and Wald statistics were evaluated in the logistic regression analysis. Accordingly, LAI-ART preference was found to be significantly high and more common among those who reported higher educational level (adjusted Odds Ratio [aOR] = 2.691, p = 0.006), those who identify as cisgender gay, bisexual, and queer men (aOR = 2.015, p = 0.025), younger individuals (aOR = 0.969, p = 0.015), and those who have received injectable medication (aOR = 0.261, p = 0.039).
The most common reasons to choose injectable (Figure 1) over pills were ‘The discomfort of having to take pills every day’ (52.8%) and ‘I think it would improve my quality of life’ (40.3%). Respondents mentioned in the open answer that they expect less digestive discomfort and more independence from the health system (no waiting for monthly refills, reduced engagement with health insurance bureaucracy, and increased freedom for travel). Conversely, the most common reasons to choose pills were convenience (60.3%) and safety and efficacy of pills (35.3%). Regarding the ‘convenience’ of pills, some participants stated in the open response that they have more control over pills and can manage if their health insurance is late for refill, while injectable PrEP could be limited by time and provider constraints. Considering the safety of pills, participants mentioned that they already know and are more comfortable with the pills’ side effects and think LAI could be ‘stronger’. Reasons did not differ across variables of interest.

Reasons to choose LAI or pills for ART in people with HIV (n = 804).
Regarding the setting where they could receive treatment, 36.2% preferred to receive LAI at the doctor’s office, and 30.9% had no preferences among a physician’s office, a nursing office, a pharmacy, or by themselves.
Preference for LAI-PrEP among people without HIV or unknown status
As shown in Table 5, people without HIV or unknown status were younger than people with HIV, with a median age of 31 years (IQR: 26–38). Most of them were cisgender heterosexual women (56%). Half (53.3%) had heard of PrEP before. Only 39.4% reported that they always used condoms.
Characteristics of the sample and correlates associated with the preference of LAI for PrEP in people without HIV (n = 872).
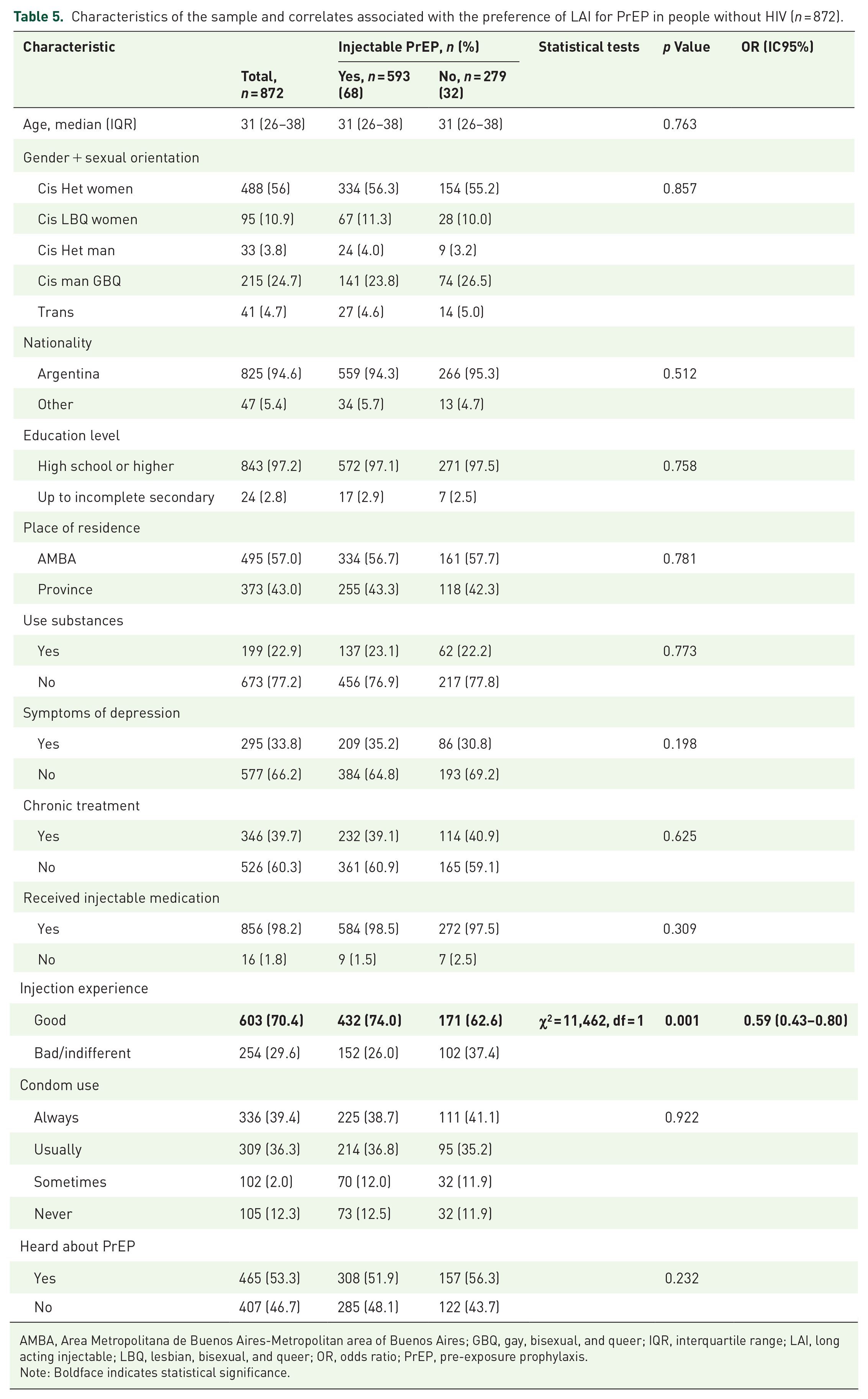
AMBA, Area Metropolitana de Buenos Aires-Metropolitan area of Buenos Aires; GBQ, gay, bisexual, and queer; IQR, interquartile range; LAI, long acting injectable; LBQ, lesbian, bisexual, and queer; OR, odds ratio; PrEP, pre-exposure prophylaxis.
Note: Boldface indicates statistical significance.
Regarding the modality of PrEP administration, 68% preferred injectable (15.8% of them every 2 months and 84.2% every 6 months), 23.3% one pill per week, and 8.7% one pill per day. Preference of injectable PrEP was similar in all gender/sexual orientation groups: 72.7% cisgender heterosexual men, 70.5% cisgender lesbian, bisexual, and queer women, 68.4% cisgender heterosexual women, 65.9% transgender and non-binary people, and 65.6% cisgender gay, bisexual, and queer men. Preference for LAI-PrEP was positively associated with prior good experiences using injectable medication (p < 0.05).
The most common reasons to choose (Figure 2) injectable PrEP over pills were ‘I’m afraid of forgetting a pill’ (57.9%) and convenience (55.5%). Respondents elaborate in the open response stating that injections every 2 or 6 months are practical and similar to vaccination, and it is easier to receive one injection than to get pills refill more often. Among those who choose pills, the most common reasons for their preference were convenience of the pills (76.2%) and dislike for the injectable option (29.9%). Participants mentioned in the open response that pills are ‘convenient’ because they would not have to inject themselves; going to a health clinic for the injectable seems inconvenient, whereas taking pills at home feels more comfortable and private than asking for an appointment. A 2 or 6 months period of time between injections is too long and they might forget; forgetting one injectable dose seems more problematic than forgetting one pill, and taking pills daily or weekly gives them more control and autonomy over medication. Reasons did not differ across variables of interest.

Reasons to choose LAI or pills for PrEP in people without HIV (n = 872).
Regarding the place of administration, 36.9% had no preference, 22.9% chose the nurse office, and 18.9% doctor’s office.
Discussion
The present study assesses preferences for methods of ART among people with HIV and PrEP among people without HIV, as well as examines the correlations and reasons for these preferences in Argentina. Preference for LAI-ART, like previous studies (69–88%)13,22,23 was high among people with HIV (91.5%), while preference for LAI-PrEP (25–74%)3,12,15 was in the range (68%) among self-identified people without HIV or unknown status.
Moreover, LAI-ART preference was positively associated, as in previous studies, with cisgender gay, bisexual, and queer men, younger, and higher education and previous use of injectable medication.18,22,24 For young people, LAI-ART could be preferable because of their more hectic or unstable lifestyle that could lead to missing pills. Regarding education, it is possible that people with lower levels could believe that LAI would not be beneficial for them or fear its side effects. These findings underscore the need to tailor future LAI-ART intervention for those of older age and low level of education, and provide them with information about the beneficial aspects of new technology for HIV treatment, such as LAI.
Regarding frequency of LAI-ART, it was observed that those who choose one injection every 6 months were more likely to be using illicit substances. Although it was not clear why drug users preferred a longer spacing between injections, this result is consistent with other studies that showed that some groups of people with HIV (e.g. youth, women using long-acting contraceptives) indicate a stronger willingness to switch to LAI-ART if the dosing frequency were 3 months or every 6 months. While currently available LAI-ART options are monthly or bi-monthly dosing, developers should consider more frequency options for different groups of people with HIV.25,26
Regarding LAI-PrEP, consistent with previous studies,15,18,27 preference for LAI was positively associated with having prior good experience using injectable medication. Although fear of needles is one of the less reported concerns in the LAI-PrEP literature and our study shows that people with HIV are not conditioned by previous experiences with injectable medication, it should be pointed out that bad healthcare experiences could affect patients’ future treatments or their continuation. This seems to be particularly true regarding people without HIV and less exposure to good or bad experiences in the healthcare system. LAI should be provided by well-trained health care workers that could provide a good experience to increase the chance of retention. Preference of LAI-PrEP did not differ between sex orientations or gender identities. They reported that this method modality could prevent them from missing doses and that it is convenient mostly because they could visit health care facilities fewer times than they would need to for pill refills. On the other hand, those who would prefer pills perceive them to be more convenient because there is no need to find a provider to administer as in the case of injection.
As participants answered the questionnaire based on subjective appraisals, personal beliefs, and prior information rather than experience of use, the perception of pills expectedly differed significantly between people with and without HIV. Given that people without HIV mentioned that they most likely would not administer the injection by themselves, their need to visit a health clinic to receive injections would present an inconvenience. Thus, taking pills would give them more control and autonomy over medication. Conversely, people with HIV that have more experience with the healthcare system and living with a chronic condition emphasized that LAI-ART would offer more independence from the health system, freeing them of (the need for) monthly refills and health insurance bureaucracy. 9 Also, the decreased preoccupation about missed doses and pill fatigue was highly valued by participants and many stated that LAI-ART could improve their quality of life. This response most likely implied that LAI-ART would increase their well-being in many areas of their life (better adherence, relationship with health care, more confidentiality and less stigma, among others). These findings are in line with other studies demonstrating that people with HIV highlight the benefits of convenience, better adherence, reduced disclosure, and improved emotional well-being of decreased stigma. On the other hand, other participants preferred to keep taking daily pills to have agency over problems with dosage and refills shortage and adverse effects.
As for convenience and preference of healthcare setting to receive LAI-ART, one-third chose the doctor’s office and another third had no preference. Our findings are in line with other studies, 28 which report that regardless of the setting, it is important to consider that providers should be free of stigma and discrimination and help patients to overcome the challenges of the healthcare system (medication authorizations, procurement and storage, appointment availability, and others). Moreover, contrary to other studies, people with HIV showed no difference in LAI-ART preference between those reporting a bad experience using an injectable treatment compared to those reporting good experiences. This could imply that they placed more value in other benefits of LAI-ART than in the modality of administration. Further studies will be needed to explore more on how preconceptions and previous experiences with injectable methods and relationship with the health system would play a role in the implementation phase of the use of LAI-ART.7,11
Limitations
Firstly, the participation of women was higher than expected, given that the NGO’s Facebook and Instagram audience was 78.7% cisgender women. Efforts were made by asking activists and health promoters of the community to post the questionnaire in their social media and send it to their WhatsApp contacts in order to reach a significant number of participants, particularly people with HIV, and to disseminate this questionnaire among gay, bisexual, and queer men and transgender and non-binary people. Nonetheless, this provides an opportunity to include cisgender women who, despite being affected, are an underrepresented group in HIV prevention and treatment research.29,30 Moreover, studies among cisgender women are scarce, and these results raise new study questions regarding preference of LAI-ART and how this is associated with previous experience with other medications, including injectable and implantable contraceptives.
Secondly, online recruitment resulted in participants with a higher educational level, most likely because that is the population with higher internet access and likelihood of being reached by online questionnaires. Future studies should encourage more community participation particularly in transgender and non-binary people, who are key to LAI-ART and PrEP implementation.
Thirdly, since there are only few studies on different methods for ART and PrEP in Latin America, it is necessary to further explore LAI-ART and PrEP preferences in other countries of the region, mainly among the most vulnerable populations who will benefit the most from LAI, such as transgender and non-binary people. Despite transgender and non-binary people being vulnerable to HIV and encountering more discrimination in social and healthcare settings because of HIV, there is no greater preference for the use of LAI-PrEP compared to the other groups. It is possible that the sample was too small, and it remains to be seen in future studies the factors that impact in their choice.
Fourthly, we did not ask about PrEP eligibility, participation in clinical studies, and current use of PrEP because it was not widely available in Argentina at the time of the study. Although PrEP has been recently approved by the regulatory agency, the number of people receiving PrEP was limited to clinical trials and pilot projects under the Ministry of Health, resulting in most participants answering the questionnaire based on subjective appraisals rather than experience of use.
Fifthly, although we did not have a specific set of questions to evaluate ART adherence, most of the participants with HIV responded they were currently taking ART (98%). Further studies should explore perceptions and preference of ART methods among people with HIV who do not adhere to treatment.
Finally, since we used a quantitative approach and an online questionnaire, participants had limitations to express their opinions and explain their choices. Further qualitative studies could bring in-depth understanding of the reasons why people would or would not use LAI.
Conclusion
Overall, acceptance of LAI was high for both ART users and potential PrEP users. Participants expect that the use of LAI-ART antiretrovirals would positively impact adherence and general well-being because of decreased chances of missing doses and increased convenience compared to pills. Additionally, the preference for LAI-PrEP among those without HIV emphasizes the importance of considering this option for HIV prevention strategies. This study highlights the need to offer diverse methods for ART and prevention to accommodate different preferences and improve health care outcomes in Latin America. More information is needed related to the perspective of decision makers and health care providers for its implementation.
Supplemental Material
sj-docx-1-tai-10.1177_20499361241228341 – Supplemental material for Preference for long-acting injectable for ART and PrEP among people with and without HIV: a cross-sectional study in Argentina
Supplemental material, sj-docx-1-tai-10.1177_20499361241228341 for Preference for long-acting injectable for ART and PrEP among people with and without HIV: a cross-sectional study in Argentina by Sergio Sciannameo, Virginia Zalazar, Luciana Spadaccini, Mariana Duarte, Pedro Cahn, Ines Aristegui and Omar Sued in Therapeutic Advances in Infectious Disease
Footnotes
Acknowledgements
We thank all study participants for their time and commitment to this research. The authors would like to acknowledge Ana Clara Zeltman for her assistance in the editing of the manuscript.
Declarations
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
