Abstract
Background:
Pre-exposure prophylaxis (PrEP) is an important intervention for reducing the risk of HIV transmission among high-risk populations such as female sex workers in Africa, where HIV prevalence remains high. We aimed to assess the use of PrEP among female sex workers in Gulu, Uganda.
Methods:
In this community-based cross-sectional study, we included HIV-negative female sex workers purposely selected from hotspots within Gulu city, Uganda between February and March 2023. A semi-structured questionnaire was administered to collect data on sociodemographic characteristics, reproductive data, sexual practices, and self-reported PrEP use in the past 3 months. Symptoms of depression were screened using Patient Health Questionnaire-2 tool. Predictors of PrEP use was determined using modified Poisson regression analysis model.
Results:
We enrolled 273 female sex workers with a median age of 27 (interquartile range: 24–32) years. Overall, 181 (66.3%) participants used PrEP. PrEP use was associated with; regular source of income beside sex work [adjusted prevalence ratio (aPR): 3.7, 95% confidence interval (CI): 2.11–6.35,
Conclusion:
Almost two in three of the female sex workers in Gulu city were currently using PrEP. Previous use of PEP was associated with lower use of PrEP. These findings suggest the need for targeted interventions to increase PrEP uptake and decrease HIV acquisition in this high-risk population among female sex workers, especially those with low income and limited access to healthcare.
Introduction
Despite significant efforts to reduce the incidence of HIV in Africa, the region continues to bear a disproportionate burden of the epidemic. 1 In Uganda, the prevalence of HIV is highest among key populations, including female sex workers.2,3 Female sex workers are at high risk of HIV acquisition due to the nature of their work, which often involves multiple sexual partners and inconsistent condom use. 3 Moreover, female sex workers are at a high risk of experiencing violence, criminalization, stigmatization, and discrimination, which further challenges their access to healthcare services. 4 Consequently, the prevalence of HIV among female sex workers is significantly higher than in the general population (31.3 compared to 5.2%). 3
In this context, pre-exposure prophylaxis (PrEP) has emerged as an important intervention for reducing the risk of HIV transmission among high-risk populations such as female sex workers.5,6 PrEP involves the use of antiretroviral medication by HIV-negative individuals prior to potential high-risk exposure to prevent HIV acquisition. 7 PrEP has been shown to be highly effective in reducing the risk of HIV transmission when used consistently and correctly.8–10
Despite the proven effectiveness of PrEP, uptake, and consistent use of these interventions among female sex workers in Africa remains low.11–13 Several factors contribute to this low uptake, including lack of awareness and knowledge of PrEP, stigma, discrimination, and limited access to healthcare services.4,11
Since 2017, the Uganda Ministry of Health adopted the use of PrEP for individuals most at risk of acquiring HIV, including female sex workers and people who inject drugs, as well as other priority populations – including pregnant and lactating women and adolescent girls and young women. 14 However, there is paucity of data on the use of PrEP among female sex workers. Understanding the prevalence and factors influencing the uptake and consistent use of PrEP among female sex workers in Uganda is crucial for informing targeted interventions to reduce HIV transmission in this population. Therefore, this study aimed to assess the use of PrEP among eligible female sex workers in Gulu city, Uganda.
Methods
Study design
This was a community-based, cross-sectional study conducted among female sex workers in Gulu city, Uganda between February and March 2023.
Study site
The study was conducted in several hotspots within Gulu city, which has an estimated 1300 female sex workers. A total of 15 hotspots across the city constituted the study sites.
Participants
Participants were recruited from different locations within Gulu city where female sex workers were known to congregate, including bars, nightclubs, brothels, and streets. To be eligible for the study, participants had to be 18 years or older, female, HIV negative, and currently working as a sex worker. HIV-negative status was verified from the most recent HIV testing results less than 3 months old. We excluded cisgender female living with HIV and transgender women with or without HIV infection from this study.
Sample size determination
The sample size of 300 participants was calculated using the modified Kish-Leslie formula 15 for a cross-sectional study in a single population, with an estimated uptake of PrEP use at 11% from a previous study conducted in Uganda, 16 a population size of 1300, and type 1 error of 5%, a standard deviation (SD) at 95% confidence interval (CI) (1.96), 10% non-response rate, and a design effect of 2.
Recruitment
Eligible participants were enrolled consecutively through purposive sampling. Recruitment was conducted by using a respondent-driven sampling approach, and by engaging peer leaders of a hotspot who knows most of the female sex workers who operate within his/her area.
Data collection
Data were collected through face-to-face interviews using a structured questionnaire in a private room within the hotspot by a trained research assistant who was a former sex worker. Each interview lasted between 20 and 30 min. The questionnaire was developed in English by the authors based on existing literature and translated into the local language,
Operational definition
PrEP use was assessed using a single question with a Yes/No answer; ‘
Similarly, previous PEP use was assessed by asking the question, ‘
Symptoms of depression over the past 2 weeks was assessed using the Patient Health Questionnaire-2 (PHQ-2) and a score, with a cut-off score of 3 used to define depressed mood. 18
Data analysis
Descriptive statistics were summarized using proportions for categorical variables, means with SDs for continuous variables with normal distributions, and medians with interquartile ranges (IQRs) for continuous variables with skewed distributions. Associations between PrEP use and categorical variables were assessed using Chi-square or Fischer’s exact tests, and associations between PrEP use and numerical variables were assessed using student
Ethical considerations
The study received ethical approval from the Gulu University Research Ethics Committee (approval number: GUREC-2022-414). This study followed the Strengthening the Reporting of Observational Studies in Epidemiology reporting guidelines for cross-sectional studies. 19
Results
Recruitment
Of the 350 female sex workers approached, 23 declined participations, 2 were transgender women, and 52 were living with HIV. A total of 273 female sex workers were included in the final analysis, Figure 1.

Study flow diagram.
Baseline characteristics
The median age of all the study participants was 27 (IQR: 24–32) years. Only six (2.2%) participants had not received formal education and most (
Baseline characteristics of female sex workers in Gulu city, Uganda.

IQR, interquartile range.
A total of 103 (37.7%) had a history of abortion, 238 (87.2%) used condoms in their last sexual encounter, and 181 (66.3%) reported use of dual contraception. Regarding source of income, 195 (71.4%) participants reported a regular source of income besides sex work. Most (
PrEP use
All study participants were aware of PrEP. Overall, 181 (66.3%) participants used PrEP in the past 3 months.
Factors associated with PrEP use
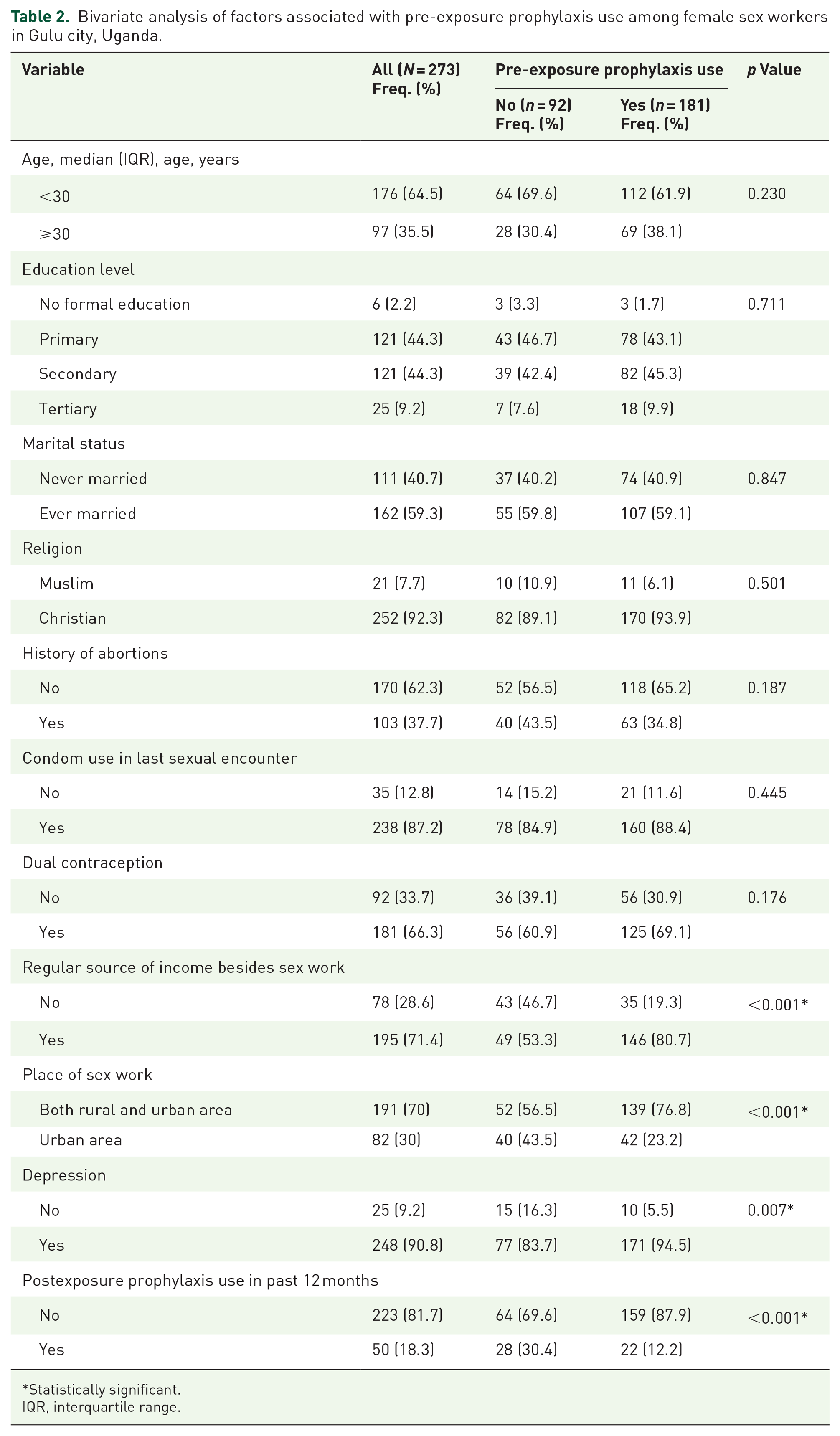
At bivariate analyses, regular source of income, place of sex work, having symptoms of depression, and PEP use in the past 12 months were statistically significantly associated with PrEP use, Table 2. A significantly higher proportion of female sex workers who used PrEP had regular sources of income besides sex workers compared to those who relied only on sex work as a source of income (19.3%
Bivariate analysis of factors associated with pre-exposure prophylaxis use among female sex workers in Gulu city, Uganda.
Statistically significant.
IQR, interquartile range.
In multivariable analyses, the prevalence of PrEP was almost fourfold higher among female sex workers who had a regular source of income besides sex work (aPR: 3.7, 95% CI: 2.11–6.35,
Multivariable analysis of factors associated with pre-exposure prophylaxis use among female sex workers in Gulu city, Uganda.

Statistically significant.
Discussion
In this study aimed at assessing the use of PrEP among HIV-negative female sex workers in Gulu city, Uganda, we found that about two-thirds of participants had used PrEP in the past 3 months. PrEP use was associated with having a regular source of income besides sex work, practicing sex work in both rural and urban areas, having symptoms of depression, and being in a polygamous marriage. Previous use of PEP was associated with lower use of PrEP. The findings of this study are in keeping with the existing literature and inform the development of targeted interventions to reduce HIV transmission among female sex workers in Uganda. The findings of this study have important implications for HIV prevention efforts among female sex workers in Africa.
Our findings are comparable to the results from a study conducted in Nigeria, where the prevalence of PrEP use among female sex workers was estimated at 88.6%, with good adherence observed among approximately 80%. 20 This high adherence was driven by factors such as education level, commencement of sex work at 18 years and above, and high monthly income. 20 Contrary to our findings, results from other studies done in Brazil, Tanzania, central Uganda, Kenya, Ghana, and China, reported significantly lower prevalence rates of PrEP use among female sex workers, ranging from 1.4 to 11%.16,21–25 The difference in prevalence rates could be attributed to various factors, including differences in sample size, geographical location, cultural norms, access to healthcare services, and the promotion of PrEP initiatives in the diverse settings.
The high uptake of PrEP among female sex workers in this study suggests that these interventions are acceptable and feasible for this population.12,26,27 In addition, high uptake reflects the wide availability of PrEP services in health facilities in Uganda with an equitable access to the services among HIV-negative women. In fact, the joint efforts of The AIDS Support Organization – Uganda and Reproductive Health Uganda mobile clinics that target female sex workers in Gulu city have enhanced awareness, accessibility, and uptake of PrEP services among female sex workers; hence the universal awareness registered in this study. Similarly, a study in Zimbabwe showed that peer-led community-based provision of PrEP services increased the uptake of PrEP among female sex workers from about 33% to up to 51%.
28
Factors such as approachability, acceptability, affordability, and appropriateness of HIV prevention, testing, and counseling services are pivotal in the access of the services to female sex workers in sub-Saharan Africa.
29
Furthermore, interventions such as PrEP adherence support groups that meet physically or online
Another factor associated with PrEP use was practicing sex work in both rural and urban areas. This finding is consistent with previous studies that have shown that female sex workers who operate in multiple locations may have increased exposure to HIV and may be more likely to use HIV prevention services. 32 One of the factors associated with PrEP use in this study was having a regular source of income besides sex work. This suggests that financial stability may play a role in enabling female sex workers to access HIV prevention services. This finding is consistent with previous studies that have shown that poverty and economic insecurity can be a barrier to accessing HIV prevention and treatment services. 32 As such, the ministry of Health of Uganda has ensured availability of HIV preventive measures at no cost especially to key populations such as female sex workers. As is in other countries such as South Africa, use of PrEP among female sex workers significantly reduces the health costs on management of HIV infections with projections showing that each dollar spent on PrEP among female sex workers results into 1.42 dollars saved on anti-retroviral therapy (ART) costs. 33
We postulate that having symptoms of depression was significantly associated with use of PrEP among female sex workers due to fear of contracting HIV infection and its sequalae, which would worsen the depressive symptoms or result in severe depression. However, this is contrary to the findings from other studies which indicate that depression resulting from factors such as intimate partner violence, client-perpetrated violence, forced condomless sex, and PrEP-associated stigma are associated with decreased use of PrEP.34–37 Moreover, depression is associated with high HIV risk behaviors such as inconsistent condom use.38,39 Being in a polygamous marriage is associated with increased likelihood to use PrEP since polygamy increases self-perceived HIV risk among sexual partners.40,41 Female sex workers who had ever used PEP were less likely to use PrEP possibly because of fear of side effects of antiretroviral drugs experienced while using PEP. Furthermore, recent publications have showed concerns expressed by female sex workers toward the use of PrEP including fear of side effects of PrEP as described on the leaflets or health workers.42–44
Our study has some limitations. Firstly, the sample size was relatively small, which may limit the generalizability of the results to other populations of female sex workers in Uganda. Secondly, the study relied on self-reported data, which may be subject to social desirability bias. Lastly, the study did not assess the barriers to access and uptake of PrEP, which could provide important insights into the low uptake of these interventions among female sex workers in Gulu city. However, this study provides a baseline data for further interventional and implementation studies to optimize HIV prevention interventions such as use of PrEP among female sex workers in Northern Uganda and Uganda at large.
Conclusion
Almost two in three of HIV-negative female sex workers in Gulu city, Uganda used PrEP in the past 3 months. Having a regular source of income besides sex work and practicing sex work in both rural and urban areas were significant associated with higher PrEP use. These findings underscore the importance of addressing economic and social barriers to accessing HIV prevention services and highlight the need for targeted interventions that address the needs of this population. These efforts are crucial in reducing HIV transmission among female sex workers in Africa and achieving the goal of ending the HIV epidemic.
