Abstract
A 46-year-old man who had undergone hematopoietic stem cell transplant twice because of acute lymphoblastic leukemia with recurrence presented with dyspnea, leading to a diagnosis of pulmonary arterial hypertension which was quickly and effectively treated with the phosphodiesterase type 5 inhibitor tadalafil. To our knowledge, pulmonary arterial hypertension related to hematologic malignancies requiring hematopoietic stem cell transplant is rarely reported. Importantly, the present case suggests that early diagnosis and treatment with a pulmonary vasodilator, such as tadalafil, can greatly decrease pulmonary vascular resistance in patients with severe pulmonary arterial hypertension after hematopoietic stem cell transplant and can then improve other symptoms. Accordingly, pulmonary vascular disease should be considered if respiratory symptoms develop following hematopoietic stem cell transplant, because treatment with pulmonary vasodilator may lead to significant improvement in pulmonary arterial hypertension.
Keywords
Case description
A 46-year-old Japanese man diagnosed with T-lymphoblastic leukemia with complex karyotype (without Philadelphia chromosome) underwent hematopoietic stem cell transplant (HSCT) using a total body irradiation (TBI) containing conditioning regimen in January 2015, but the disease relapsed in October 2018. Fortunately, a second complete remission was achieved with salvage chemotherapy of clofarabine, etoposide, and cyclophosphamide. To prevent leukemia recurrence, a second HSCT was planned. Prior to that, a baseline transthoracic echocardiogram demonstrated normal heart size with normal estimated pulmonary artery systolic pressure (PASP), right atrial (RA) size, right ventricular (RV) size, and RV function. We performed a second allogeneic cord blood transplantation using non-TBI regimen, which consisted of fludarabine, melphalan, and busulfan in December 2018. To prevent graft-versus-host disease, tacrolimus was administered. After a few months, he recovered and was discharged to home in late March 2019.
In April 2019, the patient developed dyspnea with WHO functional Class III limitations and was evaluated at the department of hematology. A chest CT showed significant cardiomegaly and pericardial effusion, and the patient was referred to the Department of Cardiology. When seen, he complained of weakness and shortness of breath. His blood pressure was 122/80 mm Hg, heart rate was 109 beats per minute, and oxygen saturation was 95% on room air. On physical examination, he had a loud P2 heart sound, jugular venous distension, and peripheral edema. An ECG demonstrated a sinus rhythm with late R/S transition but was otherwise unremarkable. A chest X-ray revealed bilateral enlargement of pulmonary artery with mild cardiomegaly (Fig. 1a). A repeat transthoracic echocardiogram now showed RA and RV enlargement. The estimated PASP was now 55–60 mm Hg (Fig. 1c and e). The tricuspid annular plane of systolic excursion was 15 mm demonstrating RV dysfunction. A moderately large pericardial effusion was also present. A pulmonary function test revealed low diffusing capacity with a diffusing capacity of the lungs for carbon monoxide of 35.2%, compared with 84.2% immediately following the first HSCT (Table 1).
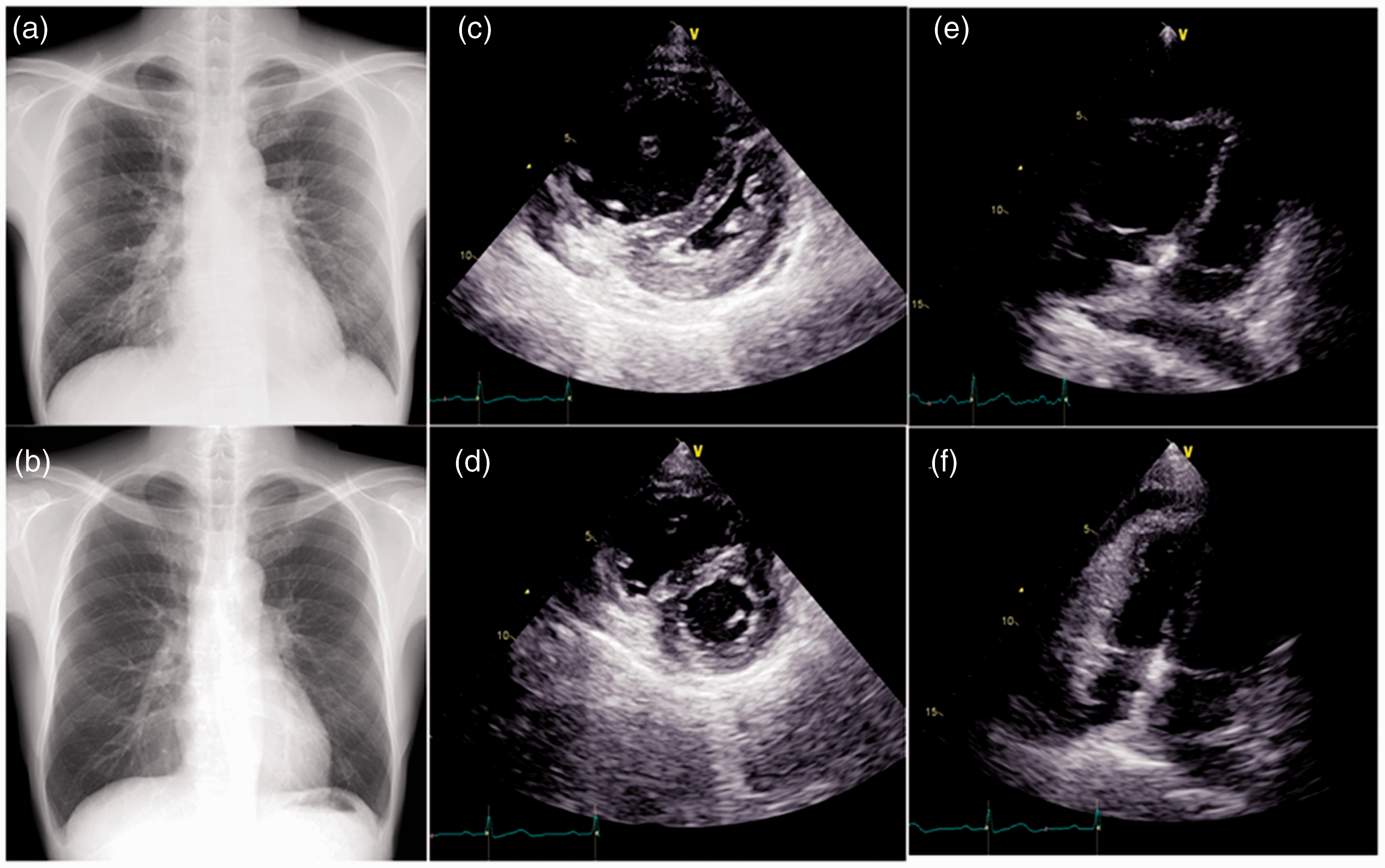
The findings of chest X-ray (CXR) and transthoracic echocardiogram (TTE) before and four weeks after tadalafil treatment. CXR on admission (Panel a) demonstrated cardiomegaly with pulmonary congestion. CXR after treatment (Panel b) demonstrated no cardiomegaly. The parasternal short axis and apical view of TTE before treatment (Panel c and e) showed severe enlargement of RV with a RVEDA of 15.3 cm2 and RVESA of 10.6 cm2, with an interventricular septum (IVS) bowing. TTE after treatment (Panel d and f) showed a mild enlargement of RV with a RVEDA of 11.9 cm2 and RVESA of 6.8 cm2, without IVS bowing or flattening.
Comparison of key hemodynamics with tadalafil therapy.
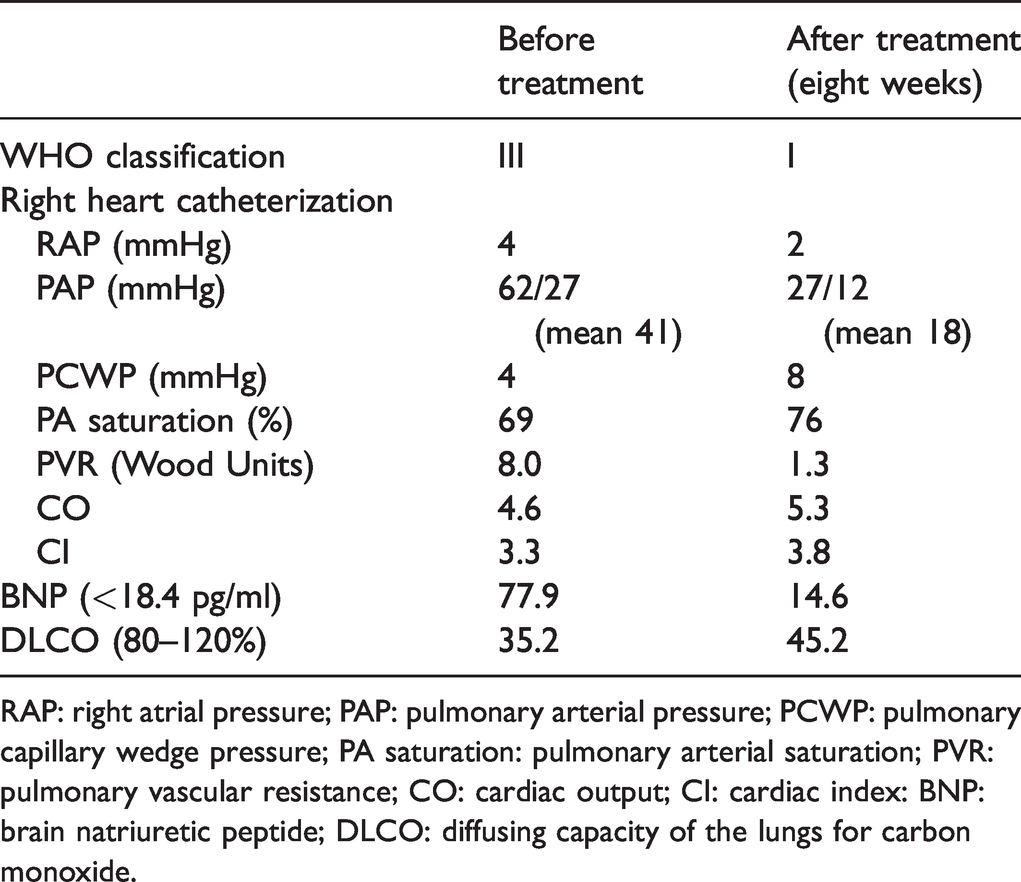
RAP: right atrial pressure; PAP: pulmonary arterial pressure; PCWP: pulmonary capillary wedge pressure; PA saturation: pulmonary arterial saturation; PVR: pulmonary vascular resistance; CO: cardiac output; CI: cardiac index: BNP: brain natriuretic peptide; DLCO: diffusing capacity of the lungs for carbon monoxide.
Hematological studies showed no evidence of connective tissue disease or human immunodeficiency virus infection. A lung ventilation perfusion scan did not demonstrate segmental/subsegmental perfusion defects. A contrasted chest CT scan was also negative for evidence of pulmonary thromboembolism and also revealed bilateral pleural effusions and a pericardial effusion. A separate high-resolution chest CT (HRCT) demonstrated mild bilateral lower lobe interlobular septal thickening, but no mediastinal lymph node enlargement or ground glass opacity. Due to severity of his dyspnea, the patient was unable to perform a six-minute walk test. A right heart catheterization was performed which demonstrated hemodynamics consistent with group 1 pulmonary arterial hypertension (PAH) (Table 1). Because the clinical suspicion for idiopathic/heritable PAH was low at the time of the procedure, a vasoreactivity test was not performed.
While we felt the diagnosis was consistent with PAH after HSCT, the interlobular septal thickening raised concerns for pulmonary veno-occlusive disease (PVOD), thus we decided to cautiously start treatment with the phosphodiesterase type 5 (PDE-5) inhibitor tadalafil with the expectation that if he tolerated it but remained symptomatic, we would include additional pulmonary vasodilator therapy.
With oral tadalafil, which he tolerated without any side effects or exacerbation of symptoms, his shortness of breath and fatigue improved. A repeat transthoracic echocardiogram showed that the estimated PASP had decreased to 40–45 mm Hg with improvement in the RA and RV sizes as well as RV function (Fig. 1d and f). A repeat chest X-ray revealed no cardiomegaly or pulmonary edema (Fig. 1b). Subsequently, the patient was discharged in a month. Eight weeks after discharge, right heart catheterization was performed to evaluate the efficacy of tadalafil and revealed now normalized hemodynamics (Table 1). Now, two years later, the patient has been stable with WHO functional class I symptoms (none to minimal) with routine physical activity; as he has tolerated the medication well, we have elected to continue him on tadalafil to prevent recurrence of pulmonary hypertension (PH).
Discussion
In this case, a middle-aged Japanese man who had undergone HSCT twice because of acute lymphoblastic leukemia with recurrence presented with dyspnea, leading to a diagnosis of PAH which was quickly and effectively treated with the monotherapy of PDE-5 inhibitor tadalafil. To our knowledge, PAH related to hematologic malignancies requiring HSCT is rarely reported. This case represents an even more unusual case of either successful treatment with tadalafil or eventual resolution over time.
Hematopoietic stem cell transplantation is a viable treatment for many patients with various hematologic diseases. However, several toxicities associated with HSCT limit its widespread use. A case of HSCT-related PH complication was first reported in 1984 in a 12-year-old boy who had undergone HSCT for acute lymphoblastic leukemia. 1 However, because few cases of PH following HSCT have been reported, much remains unclear about the cause, incidence, and risk factors. The types of PH most commonly reported after HSCT are PAH and PVOD, depending on the location of vascular injury. 2
According to European Society of Cardiology and European Respiratory Society guidelines, in the present case, the hemodynamic findings on right heart catheterization were consistent with group 1 PAH. 3 Theoretically, PVOD and PAH cannot be differentiated on the basis of only clinical symptoms or the results of cardiac catheterization. While adverse events to pulmonary vasodilator (e.g. acute pulmonary edema, worsened dyspnea) may suggest PVOD as opposed to pre-capillary disease, definitive diagnosis of PVOD requires a wedge resection lung biopsy. However, due to the morbidity of wedge resection lung biopsy and because the chest HRCT was not highly suggestive of PVOD, empiric treatment and close monitoring with a single pulmonary vasodilator, the PDE-5 inhibitor tadalafil, was the decided course in this case. Evidence for the medical treatment of HSCT-PAH is limited to a few case reports. These cases reported a favorable outcome of HSCT-PAH with oral therapeutic regiments consisting of either PDE-5 inhibitor with inhaled and oral prostacyclin analogues 4 or endothelin receptor antagonist with steroid therapies. 5 Our case differs from these two prior reports in our decision to initiate monotherapeutic pulmonary vasodilator therapy with tadalafil alone due to worries that interlobular septal thickening might represent a variant of PVOD. Not only did he tolerate the tadalafil monotherapy but there was a rapid clinical improvement in hemodynamics and clinical course. Thromboembolic disease was ruled out by imaging studies. PVOD more frequently takes a progressive course, and ultimately it was felt that this patient’s PAH was caused by a pre-capillary abnormality following HSCT.
Most reported cases of PH complicating HSCT have occurred in children, but under reporting of cases in adults may be a factor of under recognition in adults or reporting bias favoring pediatric cases. With the case series of PH after HSCT in children, the findings emphasized the importance of the early diagnosis of HSCT-PAH because aggressive and timely treatment improves the likelihood of hemodynamic normalization and survival. 6 When PH has occurred in older adults, the presentation and mechanisms of PH seem to differ from those in children and younger adults. 2 Because of these possible differences, we conducted and summarized a literature search for reported cases of PH, including PVOD7–13 and PAH, 4 , 5 , 14 in adults (20 years and older) after HSCT (Table 2). With respect to the onset of PAH, except for a case related to graft-versus-host disease, the present case is consistent with other cases occurring within four months after HSCT. Of note, the prognosis differs significantly between patients with PVOD and PAH following HSCT. Regardless of the small number of patients, all four patients (including ours) developing PAH were alive after treatment and four out of seven patients developing PVOD died (one due to relapse of their hematologic malignancy). This finding is consistent with a previously reported one-year mortality rate in cases of PVOD of as high as 70%. 15 As PH is a severe complication after HSCT, early accurate diagnosis and subsequent prompt treatment is important to ensure a favorable outcome.
Cases of PH, including PVOD and PAH, in adults (20 years and older) after HSCT.
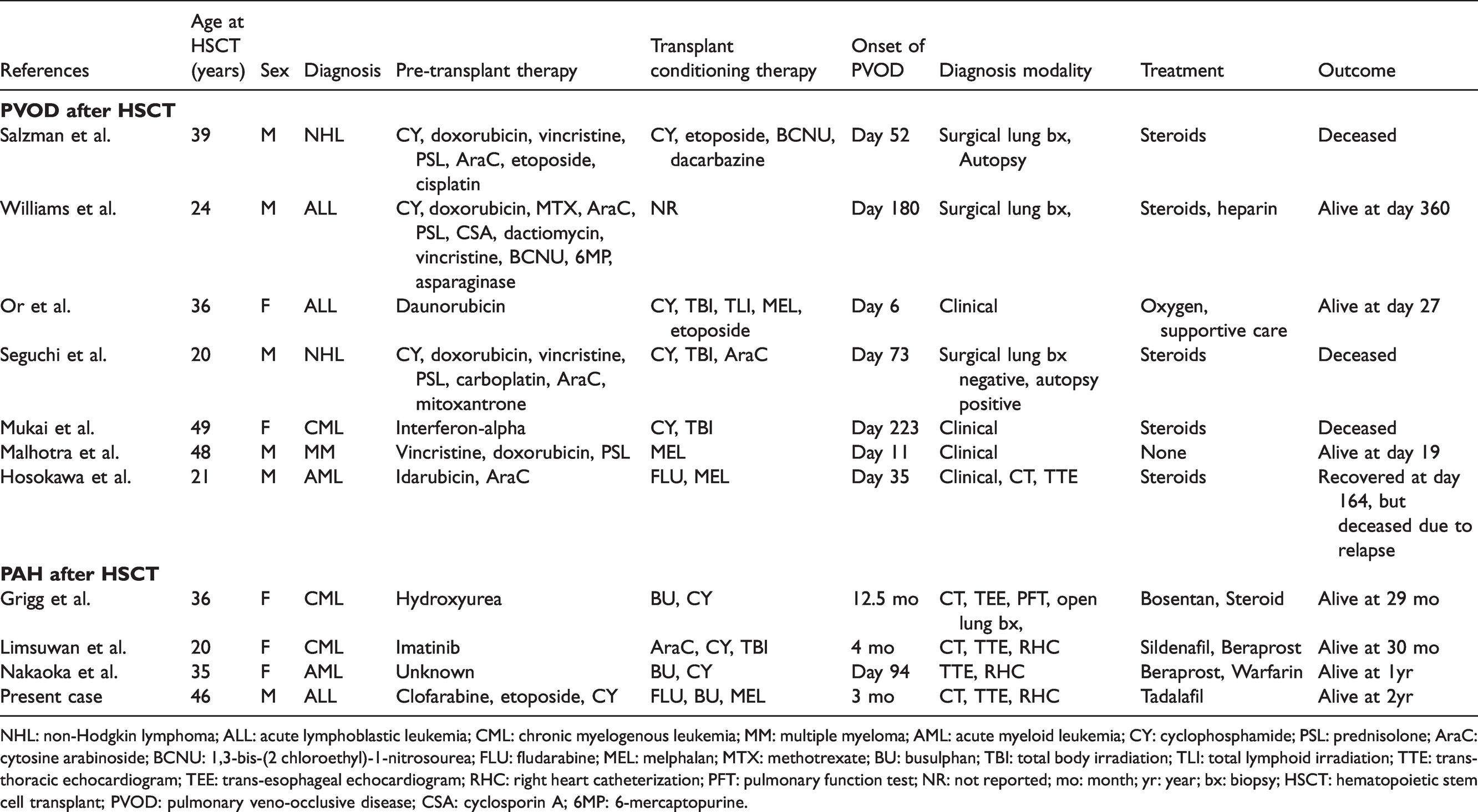
NHL: non-Hodgkin lymphoma; ALL: acute lymphoblastic leukemia; CML: chronic myelogenous leukemia; MM: multiple myeloma; AML: acute myeloid leukemia; CY: cyclophosphamide; PSL: prednisolone; AraC: cytosine arabinoside; BCNU: 1,3-bis-(2 chloroethyl)-1-nitrosourea; FLU: fludarabine; MEL: melphalan; MTX: methotrexate; BU: busulphan; TBI: total body irradiation; TLI: total lymphoid irradiation; TTE: trans-thoracic echocardiogram; TEE: trans-esophageal echocardiogram; RHC: right heart catheterization; PFT: pulmonary function test; NR: not reported; mo: month; yr: year; bx: biopsy; HSCT: hematopoietic stem cell transplant; PVOD: pulmonary veno-occlusive disease; CSA: cyclosporin A; 6MP: 6-mercaptopurine.
Concerning medical treatment, our patient has remained clinically well with normalization of his hemodynamics and continued relief of exertional dyspnea on tadalafil monotherapy over the past two years. Compared to other reported pulmonary vasodilator regiments (Table 2), tadalafil monotherapy is generally well tolerated without need for monthly liver function test (LFT) monitoring (as in the case of bosentan), reduced side effect profiles compared to prostacyclin analogues (as in the case of beraprost), and also less costly compared to the other reported pulmonary vasodilator treatment regiments. Based on this clinical context, the decision was made to continue tadalafil for a longer time period in the case that tadalafil itself was likely the reason for the improvement of pulmonary vascular disease/dysfunction.
In this present report as well as the prior reported cases, the exact mechanisms by which PH develops after HSCT is unknown and the possible diagnosis of drug-induced PAH and PVOD cannot be excluded. While it is impossible to completely exclude the possibility of chemotherapy-induced damage to the pulmonary vascular endothelium in our case, his chemotherapeutic regimen (busulphan–melphalan–fludarabine) is a widely used conditioning regimen and was not previously used in the reported cases of HSCT-associated PAH (Table 2). Furthermore, our patient did not manifest other evidence of endothelial damage such as veno-occlusive disease or microangiopathy. While our present case suggests that early diagnosis and treatment with a pulmonary vasodilator, such as tadalafil, can improve the hemodynamics and symptoms in patients with severe PAH after HSCT, we caution that this is still an isolated case. By reporting it, we hope to add to the existing body of cumulative case reports from which future clinicians can base their clinical judgment as the paucity of cases makes treatment trials unlikely. Moreover, because pulmonary complications after HSCT are common and have various causes, PH should not be overlooked. Accordingly, PH should be considered if respiratory symptoms develop following HSCT, and careful diagnostic work-up to diagnosis and differentiate PAH from PVOD should be taken because treatment with pulmonary vasodilator may lead to significant clinical improvement in PAH.
Footnotes
Consent
Informed consent was obtained to publish.
Author contributions
T.D.T.: study conception, design, analysis, interpretation of data, and drafting of manuscript; D.C.I. and T.S.: edition of manuscript and critical revision; A.Y.: acquisition of data; and M.Y.: critical revision.
Conflict of interest
The author(s) declare that there is no conflict of interest.
Acknowledgements
The authors are grateful to Prof. Masao Okazaki at The Jikei University School of Medicine for his editing contribution.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
