Abstract
Our objective was to establish the impact of wearing a face mask on the outcome of six-minute walk test in healthy volunteers. In a study of 20 healthy volunteers who each completed two 6MWTs, one with a mask and one without, there was no difference in distance walked. However, there was a significant difference in perception of dyspnea between the two groups.
Introduction
The 6-minute walk test (6MWT) is a common and reproducible test of exercise capacity used in the initial assessment and surveillance of many cardiopulmonary conditions. The 6MWT has prognostic value as part of the initial patient assessment, and changes in 6MWT over time also have prognostic importance.1–3 The 6MWT has been used as a common outcome in therapeutic trials of pulmonary arterial hypertension (PAH), and it is incorporated into models that commonly help to determine next steps in patient management.4–8 The SARS-CoV-2 pandemic has changed the way we perform routine in-office testing. Since the beginning of the pandemic, the CDC has recommended that a mask be worn in public settings. The importance of wearing a face mask (FM) is heightened in those with underlying lung disease, especially in a healthcare setting. As the 6MWT is routinely performed within a healthcare facility, the impact of wearing a FM on 6minute walk distance (6MWD) must be better understood. The 2002 ATS or 2014 ERS/ATS Statement on 6MWT does not provide guidance as to how to perform or adjust for walks done with face coverings.9,10 As a first step to understanding this, we evaluated the impact of FM on 6MWT performance in healthy volunteers.
Methods
This study has been approved by our University IRB, HM20019672.
Inclusion/exclusion criteria
Health Employees and healthcare professions students who identified with the term ‘healthy volunteer’ were asked to participate. Those with underlying cardiopulmonary illness were excluded from participation.
Subject recruitment
Health employees and healthcare professions students were identified through publicly available hospital websites. An e-mail was sent notifying them of the study and inviting participation. For those interested, an electronic link was included, which allowed subjects to complete electronic consent form. Once informed consent was obtained, e-mail instructions for 6MWT and a form for electronic self-reporting of results were automatically sent. The invitation e-mail was re-sent daily, for three consecutive days, to those who had not yet consented. Once a participant completed the consent (but not yet data entry into REDCap), they received daily e-mail reminders for three days.
6-minute walk course and instructions
We used a large, uncrowded outdoor patio (flat surface with good traction) on the hospital campus, in order to permit social distancing to reduce risk from COVID-19. Here, three separate corridors of 100 feet each were marked at 10-foot intervals. Participants were asked to avoid outdoor temperatures that could impact their performance. Participants were asked to bring a coin; on arrival, a self-administered coin flip was used to randomize participants into the “mask first” group (heads) or “mask second” group (tails). Participants were asked to wear comfortable clothing and shoes, and to bring their own mask. Electronic instructions explained the objective of the test, as well as other standard 6MWT instructions. Participants were asked to walk with a cellular device and to use the ‘Stopwatch’ option within the ‘Clock’ app to keep time and count laps completed. They were also asked to measure incomplete laps using the marked corridor, and to use the ‘Measure’ app on their cellular device to measure the remaining distance between 10-foot markings. Participants then add the completed laps to the distance from the incomplete lap to calculate their total distance.
Self-reported data
Using REDCap anonymously, participants were asked to enter their gender, approximate weight and height, type of mask used during the 6MWT, and results from each of their 6MWTs (distance and self-reported Borg Dyspnea Score).
Statistical analysis
For our primary outcome, change in 6MWD with and without a FM, as well as all secondary outcomes, we used a paired t-test. Significance was set at p ≤ 0.05 with power (1-B) set at 0.90.
Results
Our study recruited 20 healthy volunteers, 15 female and 5 male participants. The participants had a body mass index ranging from 17.9 to 33.9, with an average of 23.3. Of the 20 participants, 10 wore droplet masks and 10 wore cloth masks. Average distance walked (Fig. 1) with a mask was 1986.1 ft ± 130 ft, and without a mask 2002.8 ft ± 111 ft (mean difference 26.5 ft, p = 0.58). BDS average with a mask was 1.2 ± 0.44, and without a mask 0.73 ± 0.37 (mean difference 0.4, p = 0.002).
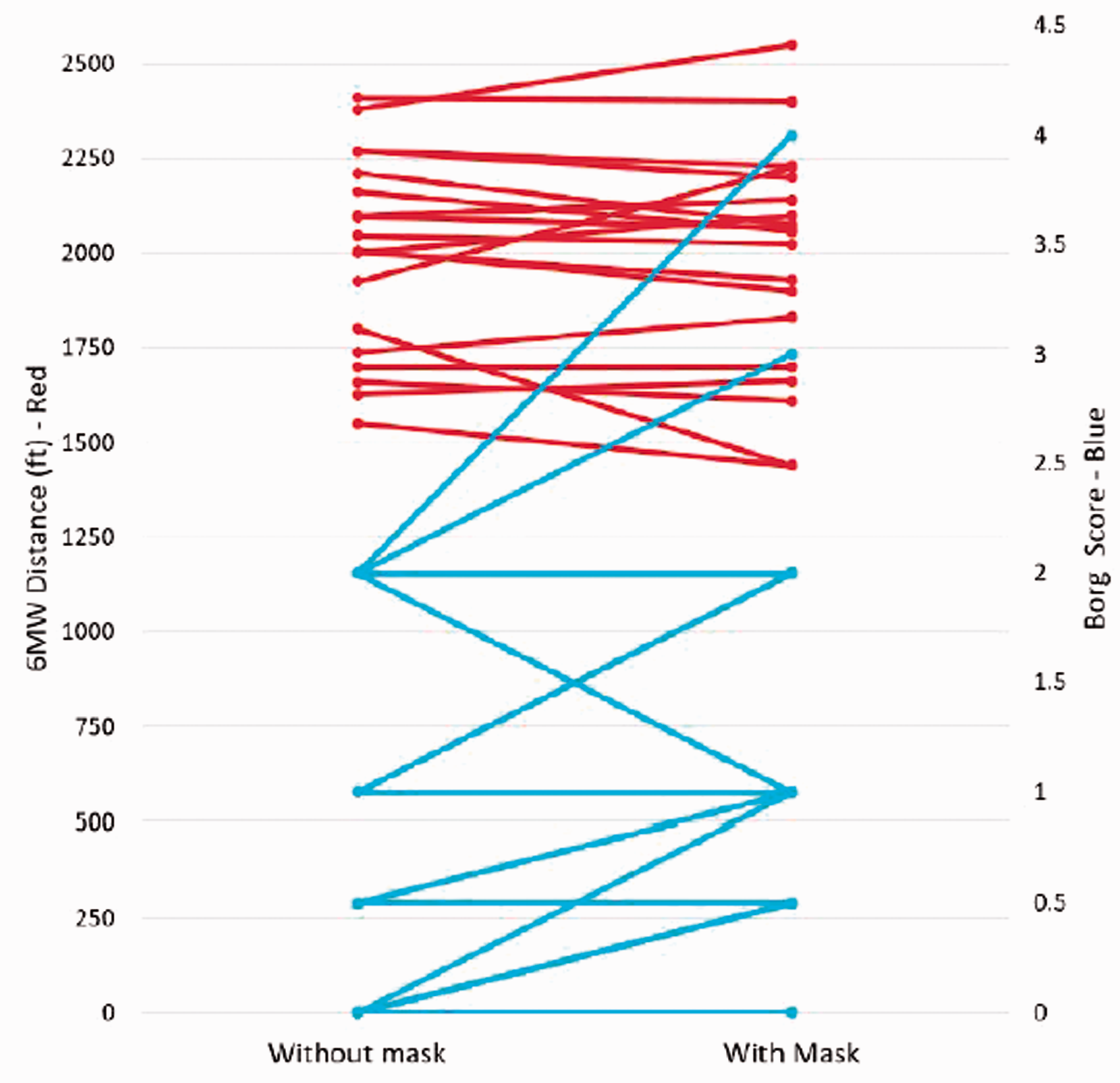
Impact of Facemask on 6MWD and Borg Score.
Discussion
In the present study assessing the effect of a FM on 6MWT performance in healthy volunteers, we found no significant difference in the distance walked with or without a mask, but we did find a significant increase in dyspnea (as measured by BDS) with use of a mask. We would note that the limited number of participants may have underpowered our assessment of the change in 6MWD, and we would anticipate that changes in 6MWT performance are likely to be heightened in patients with cardiopulmonary illness in comparison to healthy volunteers.
Dyspnea on exertion is the initial symptom in more than 80% of patients with pulmonary arterial hypertension. 7 In patients living with PAH, fatigue and dyspnea remain the most common (>90% in both cases) symptoms. 11 The BDS is a standard component of the 6MWT, and the ATS recommends that patients provide a subjective 0 to 10 score to describe their fatigue at the conclusion of the walk.9,10 The BDS is reproducible and can be followed over time, and the minimally important difference in BDS for those with PAH is thought to be around 1. 12 The BDS is an important clinical outcome in those with PAH. Thus, changes in BDS when using a facemask suggest that a facemask alone may be an independent factor, regardless of underlying disease or severity.
Samannan and colleagues recently evaluated the effect of FM on healthy and COPD patients by measuring vital signs, end tidal carbon dioxide, and partial pressure of oxygen and carbon dioxide. 13 Although their sample size was small, their results are complementary to ours: there was no significant difference in the objective measurements with a FM in healthy individuals. The authors do not comment on the distance walked or Borg score.
Our results are also comparable to results from a study of 44 healthy volunteers from France. 14 The researchers found no difference in distance walked, heart rate, or oxygen saturation between group with a surgical mask and without. However, they did find a clinically and statistically significant variation in reported dyspnea score (5.6 with a surgical mask vs. 4.6 without a surgical mask, p ≤ 0.001). 14 Given the importance of the 6MWT in determining patients’ prognosis and management, changes in 6MWT related to the use of a FM are important to better understand during the COVID-19 pandemic or subsequent epidemics. Limitations of our study include its small size and healthy patient population. Future steps might include enrollment of a larger study population and standardization of mask type in order to limit variability.
Prospective studies in patients with underlying cardiopulmonary illness are needed.
Footnotes
Authors’ contribution
Kevin Swiatek – protocol development, implementation of study, article preparation; Saahil Golia – protocol development, implementation of study, article preparation; Nicole Ng – protocol development, implementation of study, article preparation; Janet Pinson – protocol development, implementation of study, article preparation; Charnetta Lester – protocol development, implementation of study; Dan Grinnan – protocol development, implementation of study, data analysis, article preparation.
Conflict of Interest
The author(s) declare that there is no conflict of interest.
Ethical approval
This study was approved by our University Institutional Review Board, HM20019672.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
