Abstract
Evaluation of left ventricular filling pressure plays an important role in the clinical management of pulmonary hypertension. However, the accuracy of echocardiographic parameters for the determination of left ventricular filling pressure in the presence of pulmonary vascular lesions has not been fully addressed. We retrospectively investigated 124 patients with pulmonary hypertension due to pulmonary vascular lesions (noncardiac pulmonary hypertension group) and 113 patients with ischemic heart disease (control group) who underwent right heart catheterization and echocardiography. The noncardiac pulmonary hypertension group was subdivided into less-advanced and advanced groups according to median pulmonary vascular resistance. Pulmonary artery wedge pressure was determined as left ventricular filling pressure. As echocardiographic parameters of left ventricular filling pressure, the ratio of early- (E) to late-diastolic transmitral flow velocity (E/A), ratio of E to early-diastolic mitral annular velocity (E/e′), and left atrial volume index were measured. In the less-advanced noncardiac pulmonary hypertension and control groups, positive correlations were observed between pulmonary artery wedge pressure and late-diastolic transmitral flow velocity (R = 0.41, P = 0.002 and R = 0.71, P < 0.001, respectively) and left atrial volume index (R = 0.53, P < 0.001 and R = 0.41, P < 0.001), whereas in the advanced noncardiac pulmonary hypertension group, pulmonary artery wedge pressure was only correlated with left atrial volume index (R = 0.27, P = 0.032). In the controls, only pulmonary artery wedge pressure determined E (β = 0.48, P < 0.001), whereas both pulmonary artery wedge pressure and pulmonary vascular resistance were independent determinants of E (β = 0.29, P < 0.001 and β = –0.28, P = 0.001, respectively) in the noncardiac pulmonary hypertension group. In conclusion, in the presence of advanced pulmonary vascular lesions, conventional echocardiographic parameters may not accurately reflect left ventricular filling pressure. Elevated pulmonary vascular resistance would lower the E, even when pulmonary artery wedge pressure is elevated, resulting in blunting of echocardiographic parameters for the detection of elevated left ventricular filling pressure.
Introduction
Pulmonary hypertension (PH) has diverse causes and results from varying contributions of elevated pulmonary vascular resistance (PVR), pulmonary artery (PA) stiffness, and left ventricular (LV) filling pressure.1 Its etiology can be classified as post-capillary PH-left heart disease (PH-LHD) or pre-capillary due to pulmonary vascular lesions (noncardiac PH).2,3 As accurate differential diagnosis between these two entities is critical for the management of PH, evaluation of LV filling pressure plays an important role in related clinical practice.4–6 On the other hand, various studies have suggested that noncardiac PH substantially aggravates LV diastolic dysfunction due to intrinsic myocardial damage or through ventricular interaction.7,8 Although mortality rates have improved since the introduction of pulmonary vasodilator therapy,9,10 such therapy can be hazardous in populations with elevated LV filling pressure because of increased preload resulting in exacerbation of the rise in the filling pressure.11,12 Therefore, the estimation of LV filling pressure is essential in the management of noncardiac PH.
Although echocardiography is used as a first-line tool for the noninvasive estimation of LV filling pressure in patients with cardiovascular disease,3,13,14 the accuracy of echocardiographic parameters for the determination of LV filling pressure has not been addressed specifically for PH patients. Various researchers have discussed the inconsistency of Doppler echocardiographic parameters, compared to invasive measurements, for the determination of LV filling pressure in PH patients.15–17 Their results suggested that the severity of pulmonary vascular lesions might alter the association between Doppler echocardiographic parameters and LV filling pressure, the extent of which has not yet been elucidated. We, therefore, aimed to investigate the relationship between invasively measured pulmonary artery wedge pressure (PAWP) and echocardiographic parameters of LV filling pressure in noncardiac PH, with a particular focus on the effect of the severity of pulmonary vascular lesions. To this end, we compared noncardiac PH patients with ischemic heart disease patients without severe LV systolic dysfunction as controls.
Methods
Study protocol and population
The study protocol was approved by the institutional review board of our University Hospital (No. 015-0210). This investigation was designed as a retrospective, observational study in a single academic hospital. We enrolled 138 consecutive patients who had been diagnosed with PH due to abnormal pulmonary vasculature and underwent cardiac catheterization and echocardiography for hemodynamic evaluation within 10 days from January 2010 to September 2019. All PH diagnoses were made by expert physicians according to current Guidelines.2 Because this study was aimed to assess the reliability of echocardiographic LV filling pressure parameters to detect the elevated filling pressures in patients with PH caused by pulmonary vascular lesions, patients in whom pre-capillary PH were confirmed in the past and exhibited elevated PAWP (≥15 mmHg) at the time of the examination were not excluded. Patients who had been diagnosed with left heart disease, such as mitral stenosis (N = 2), severe mitral valve calcification (N = 1), or hypertrophic cardiomyopathy (N = 1), were excluded. Also, 10 patients who had been diagnosed as group 5 PH, which may cause pre- or post-capillary PH because of complex entity consisted of several disorders with multiple etiologies,18 were excluded. Accordingly, 124 patients with noncardiac PH were included for the final analysis. The noncardiac PH patients were subdivided into less-advanced and advanced groups by using the median PVR (5.3 Wood units). We also investigated 179 consecutive patients with ischemic heart disease who underwent the above-mentioned two tests within 10 days from March 2013 to December 2017, as a control group. To minimize the difference in frequency of patients with abnormal LV filling pressure between the groups, we excluded patients with a history of hospitalization due to worsening heart failure (N = 4), those with an LV ejection fraction (EF) of <40% (N = 61) from the control group. We also excluded patients showing elevated PAWP (≥15 mmHg) and elevated PVR (≥3 Wood Units), i.e. combined pre- and post-capillary PH (N = 1). Finally, 113 patients were analyzed as a control group (Fig. 1). For all patients, we carefully confirmed that hemodynamic status did not change between the two tests. The study was performed in accordance with the declaration of Helsinki and the ethical standards of the responsible committee on human experimentation (institutional and national).
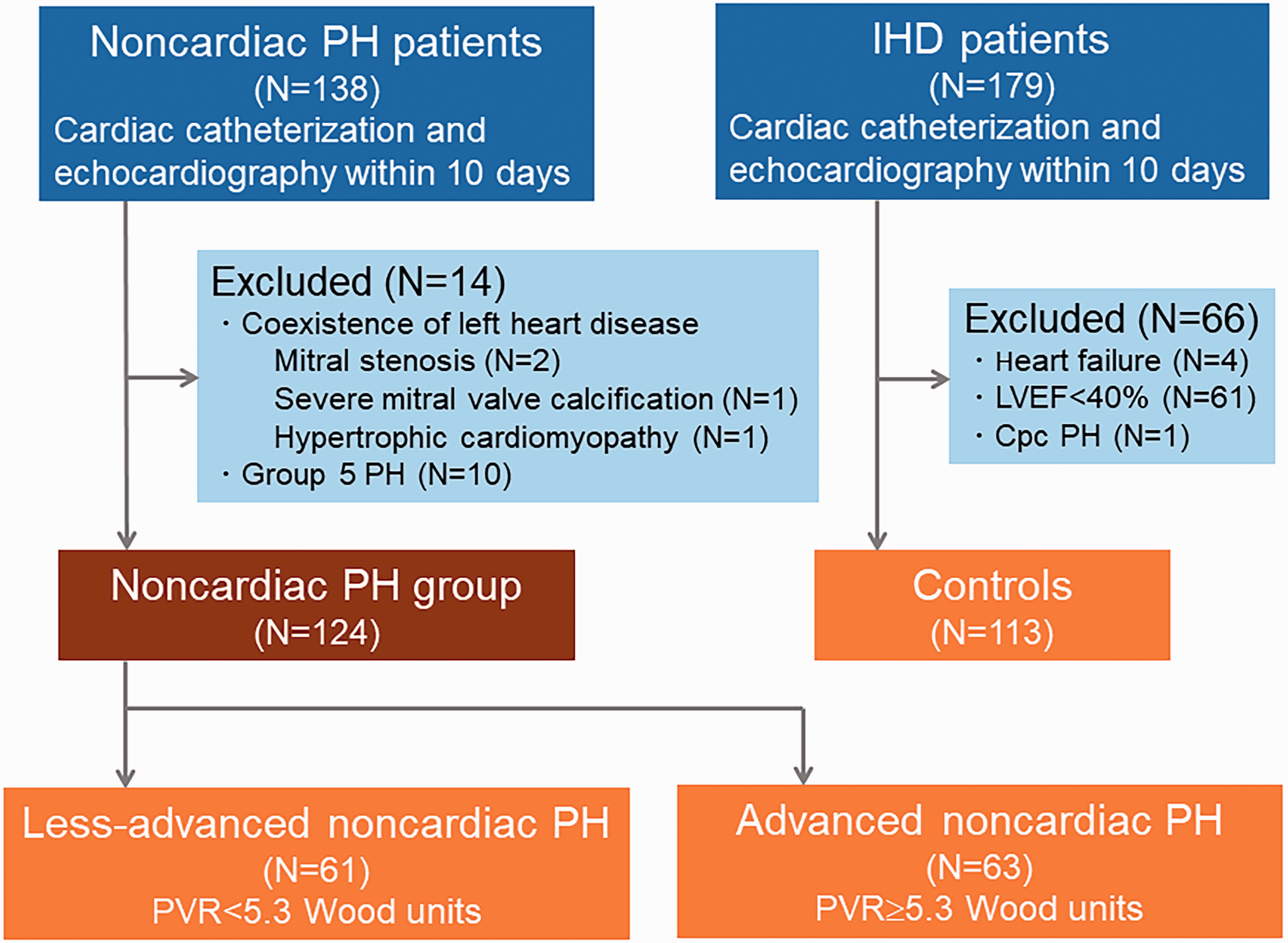
Flowchart of patient enrollment.
Cardiac catheterization
Right heart catheterization was performed by trained physicians using a 7F, fluid-filled, balloon-tipped catheter. After calibration, with the 0 point at the mid-thoracic line, the catheter was inserted through the internal jugular vein or common femoral vein to the PA, and waveforms of PAWP, main PA pressure, right ventricular (RV) pressure, and right atrial (RA) pressure were recorded during a breath-hold at shallow expiration or at the intermediate expiratory position under quiet respiration. The wedge position was confirmed by fluoroscopy, or if needed, by oxygen saturation of the blood aspirated from the tip of the wedged catheter. From the pressure waveforms, PAWP, mean PA pressure, and mean RA pressure were determined at end expiration. Cardiac output (CO) was measured using the thermodilution method and corrected for body surface area to determine the cardiac index (CI). PVR was calculated using the following formula: PVR (Wood units) = (mean PA pressure – PAWP)/CO.
Echocardiography
Echocardiography was performed using commercially available systems: an Aplio Artida system equipped with a PST-25BT probe (Canon Medical Systems, Otawara, Japan), a Vivid E9 ultrasound system with an M5S probe (GE Healthcare, Chicago, IL, USA), an iE33 ultrasound system with an S5-1 probe (Philips Medical Systems, Andover, MA, USA), or a Prosound F-75 system with a 2.5MHz probe (Hitachi Ltd., Tokyo, Japan), with the patient in the left lateral decubitus position. LV end-diastolic diameter, LV end-systolic diameter, and proximal RV outflow tract diameter were measured in the parasternal long-axis view, and inferior vena cava diameter was measured in the subcostal view according to international guidelines.19 LV EF and left atrial (LA) volume were measured in the apical four- and two-chamber views using the biplane method of disks. LV mass was calculated using the Devereux formula.20 Tricuspid annular plane systolic excursion (TAPSE) and right ventricular fractional area change (RVFAC) were measured from the apical four-chamber view. Well-recognized Doppler parameters of LV filling pressure were obtained as follows. Transmitral Doppler flow was recorded in the LV long-axis view, and peak early-diastolic velocity (E), late-diastolic velocity (A), and the E/A ratio were measured. Pulmonary venous Doppler flow was recorded in the apical four-chamber view, and peak systolic velocity (PVS), peak diastolic velocity (PVD), and the PVS/PVD ratio were measured. Septal and lateral early-diastolic mitral annular velocities (e′) were measured from the apical four-chamber view using pulsed-wave tissue Doppler imaging, and the E/e′ ratio was calculated for the septal e′, lateral e′, and average of the septal and lateral e′ values. Estimated PAWP was then calculated as 1.91 + 1.24⋅E/lateral e′ (mmHg) according to the previous report.14 The LV eccentricity index, reflecting the degree of ventricular interaction due to RV pressure overload, was calculated as D2/D1, where D1 was the diameter of the left ventricle perpendicular to the interventricular septum and D2 was the diameter perpendicular to D1 in the LV basal short-axis view at end systole (Supplemental Figure 1).21
Statistical analysis
All statistical analyses were performed using JMP software version 13.1.0 (SAS Institute Inc., Cary, NC, USA). The Shapiro–Wilk test was performed to test the normality of continuous variables. The continuous variables were summarized as mean ± standard deviation or medians (interquartile range) and compared using an unpaired Student t test or Wilcoxon rank sum test as appropriate. Invasive and estimated PAWP were compared by Bland–Altman analysis to derive bias, agreement, and confidence intervals.22 Categorical variables were expressed as a number (percentage) and compared between the groups using chi-square analysis. Linear regression analysis was used for the detection of correlation between two continuous variables based on their normal distributions. The correlations were adjusted by the patient characteristics that were different between the control and noncardiac PH groups using multivariable linear regression analyses in which each characteristic was added as an explanatory variable. To investigate independent determinants of echocardiographic parameters of LV filling pressure, multivariable linear regression analyses were performed. For all tests, a P value of <0.05 was considered as significant.
Results
Patient characteristics
Patient characteristics are summarized in Table 1. Patients in the noncardiac PH group were younger and contained a smaller proportion of males than the control group, the latter being an explanation for the smaller body size of patients in the noncardiac PH group. Due to the difference in indications for cardiac catheterization between the groups, the comorbidity rate was higher and renal function was lower in the control group than in the noncardiac PH group, whereas plasma brain natriuretic peptide level was comparable between the groups. Among the noncardiac PH group, group 1 (pulmonary arterial hypertension) was the most common subtype, followed by groups 4 (chronic thromboembolic PH) and 3 (PH associated with lung disease). The mean duration between cardiac catheterization and echocardiographic examination was 1.7 days longer in the noncardiac PH group than in the control group. As expected, mean PA pressure and PVR were higher in the noncardiac PH group, whereas PAWP and mean RA pressure were higher in the control group. There was no statistical difference in CI between two groups. Patients in the control group had a larger LV diameter and lower LV EF than those in the noncardiac PH group, whereas patients in the noncardiac PH group had a larger PA diameter, RV diameter, and inferior vena cava diameter. TAPSE was comparable between the two groups, whereas RVFAC was reduced in noncardiac PH. Although the E and septal e′ values were comparable between patients in the control and noncardiac PH groups, septal E/e′ was slightly higher in controls. The lateral e′ value was higher in noncardiac PH group, resulting in higher lateral and averaged E/e′ in the control group.
Patient characteristics.
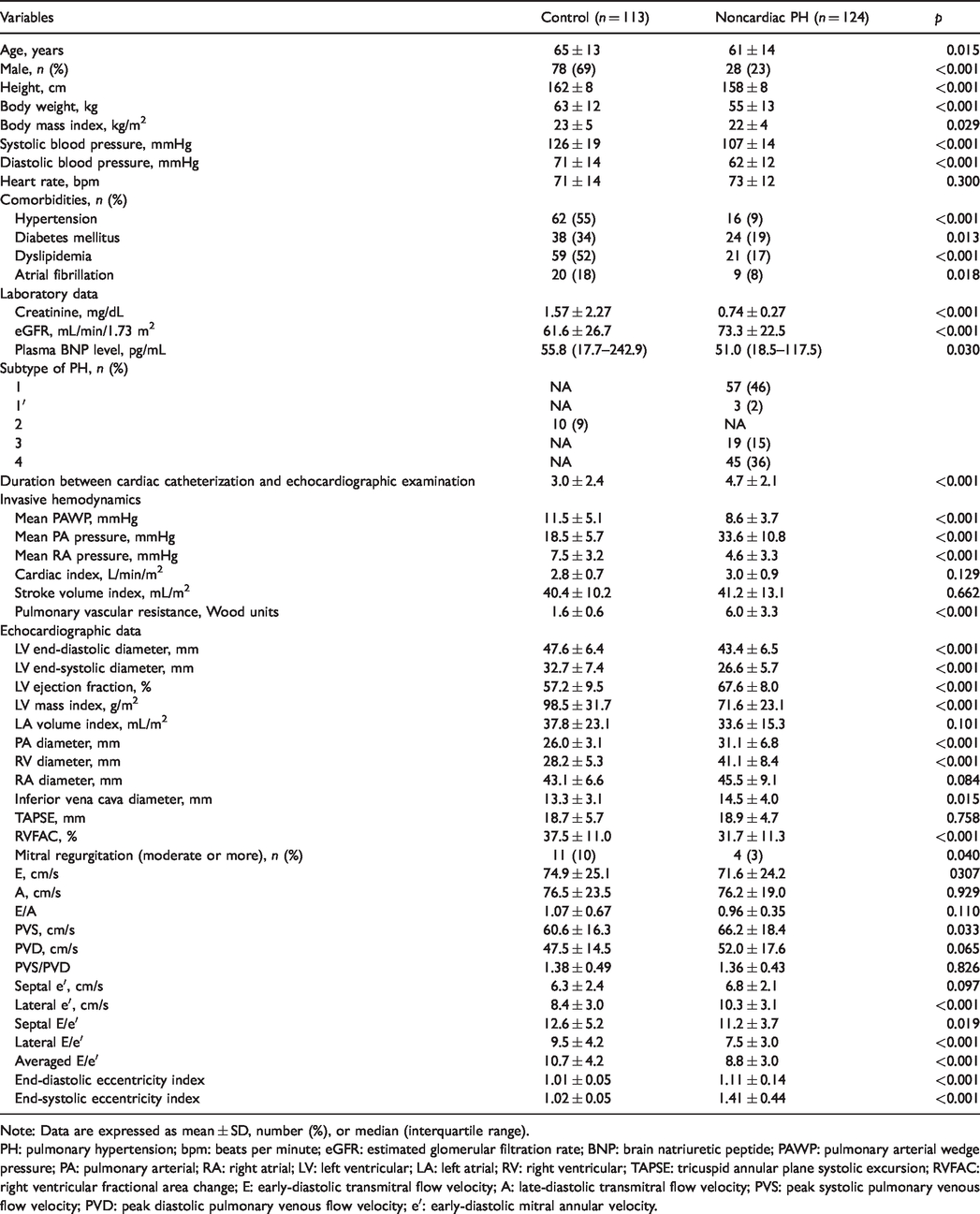
Note: Data are expressed as mean ± SD, number (%), or median (interquartile range).
PH: pulmonary hypertension; bpm: beats per minute; eGFR: estimated glomerular filtration rate; BNP: brain natriuretic peptide; PAWP: pulmonary arterial wedge pressure; PA: pulmonary arterial; RA: right atrial; LV: left ventricular; LA: left atrial; RV: right ventricular; TAPSE: tricuspid annular plane systolic excursion; RVFAC: right ventricular fractional area change; E: early-diastolic transmitral flow velocity; A: late-diastolic transmitral flow velocity; PVS: peak systolic pulmonary venous flow velocity; PVD: peak diastolic pulmonary venous flow velocity; e′: early-diastolic mitral annular velocity.
Relationships between echocardiographic parameters and PAWP
Linear regression analysis results of echocardiographic parameters and PAWP are summarized in Table 2 and Fig. 2. In the control group, all Doppler parameters besides e′ and the LA volume index (LAVI) exhibited a weak to modest correlation with PAWP. However, the correlations of E and E/A to PAWP was attenuated and those of E/e′ to PAWP disappeared in the noncardiac PH group. Notably, when the noncardiac PH group was stratified based on PH severity, there was no correlation between E or E/A and PAWP in the advanced noncardiac PH group (Table 2). In contrast, LAVI significantly correlated with PAWP in both the noncardiac PH groups. These results did not change after adjusting for patient characteristics that were different between the control and noncardiac PH groups (data not shown).
Correlation of echocardiographic parameters and mean PAWP.
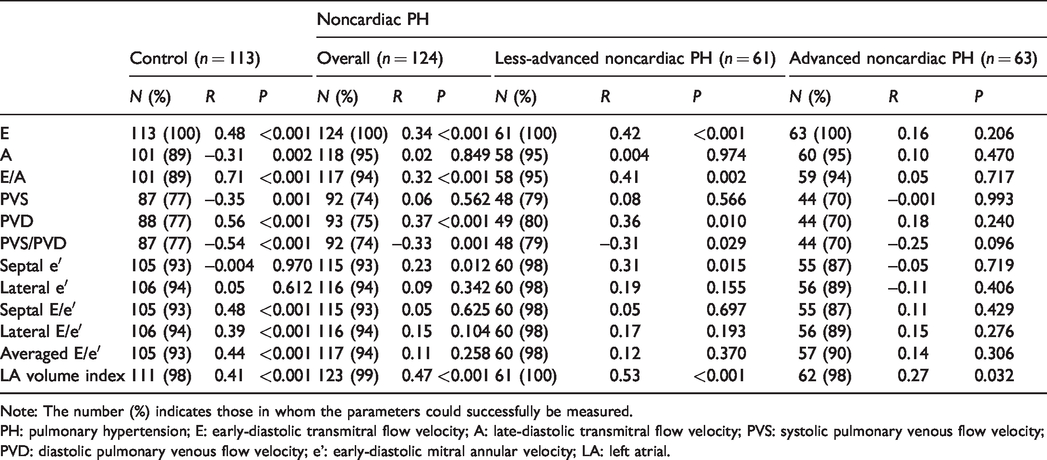
Note: The number (%) indicates those in whom the parameters could successfully be measured.
PH: pulmonary hypertension; E: early-diastolic transmitral flow velocity; A: late-diastolic transmitral flow velocity; PVS: systolic pulmonary venous flow velocity; PVD: diastolic pulmonary venous flow velocity; e': early-diastolic mitral annular velocity; LA: left atrial.
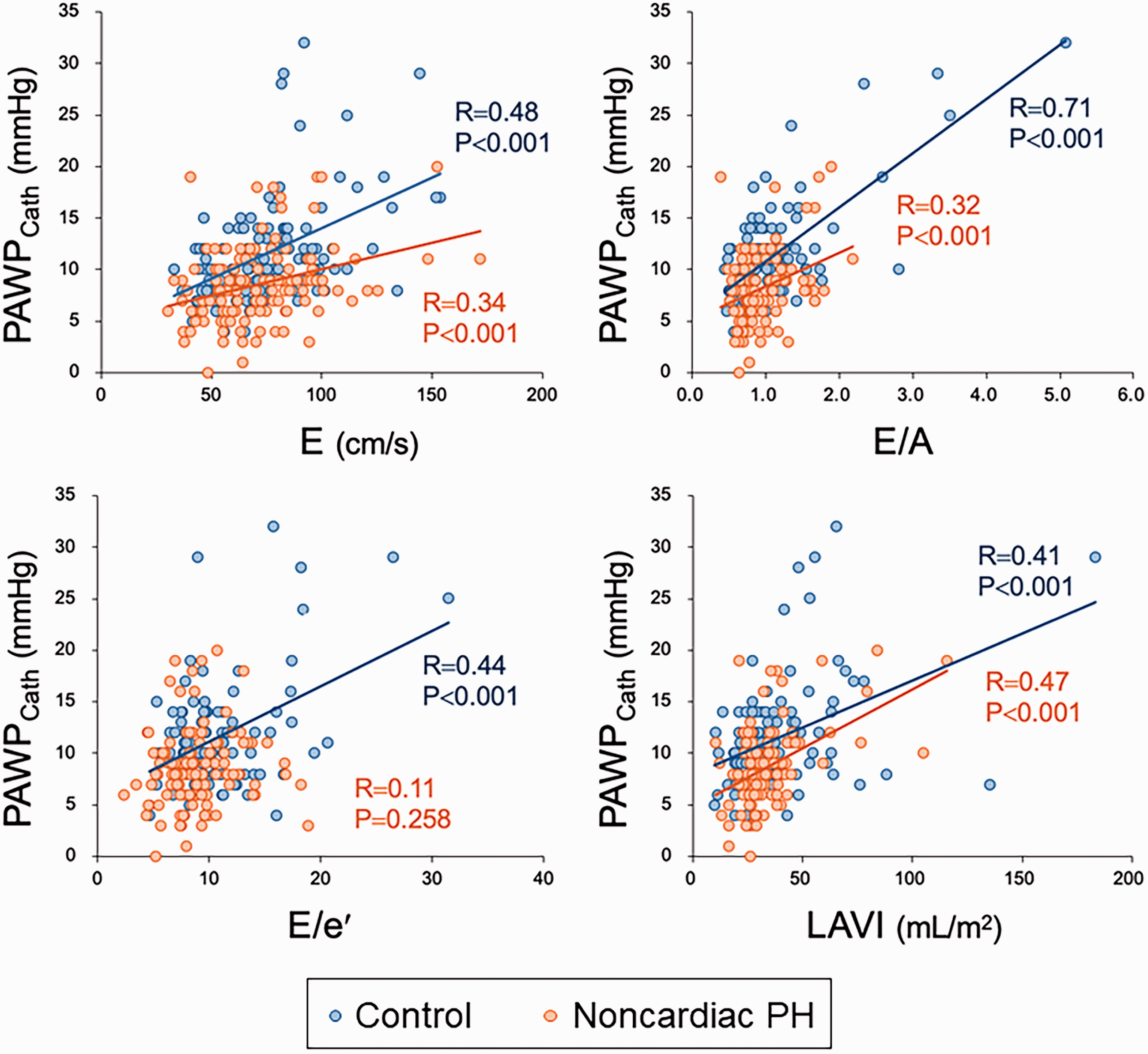
Correlation of echocardiographic parameters and PAWP.
Fig. 3 illustrates the Bland–Altman plots showing the agreement between the invasive and estimated PAWP. In patients with a PAWP <12 mmHg, positive fixed bias was similarly observed in both controls and noncardiac PH patients. In contrast, in patients with elevated PAWP (≥12 mmHg), a negative fixed bias was observed in noncardiac PH patients, suggesting an underestimation of the estimated PAWP.
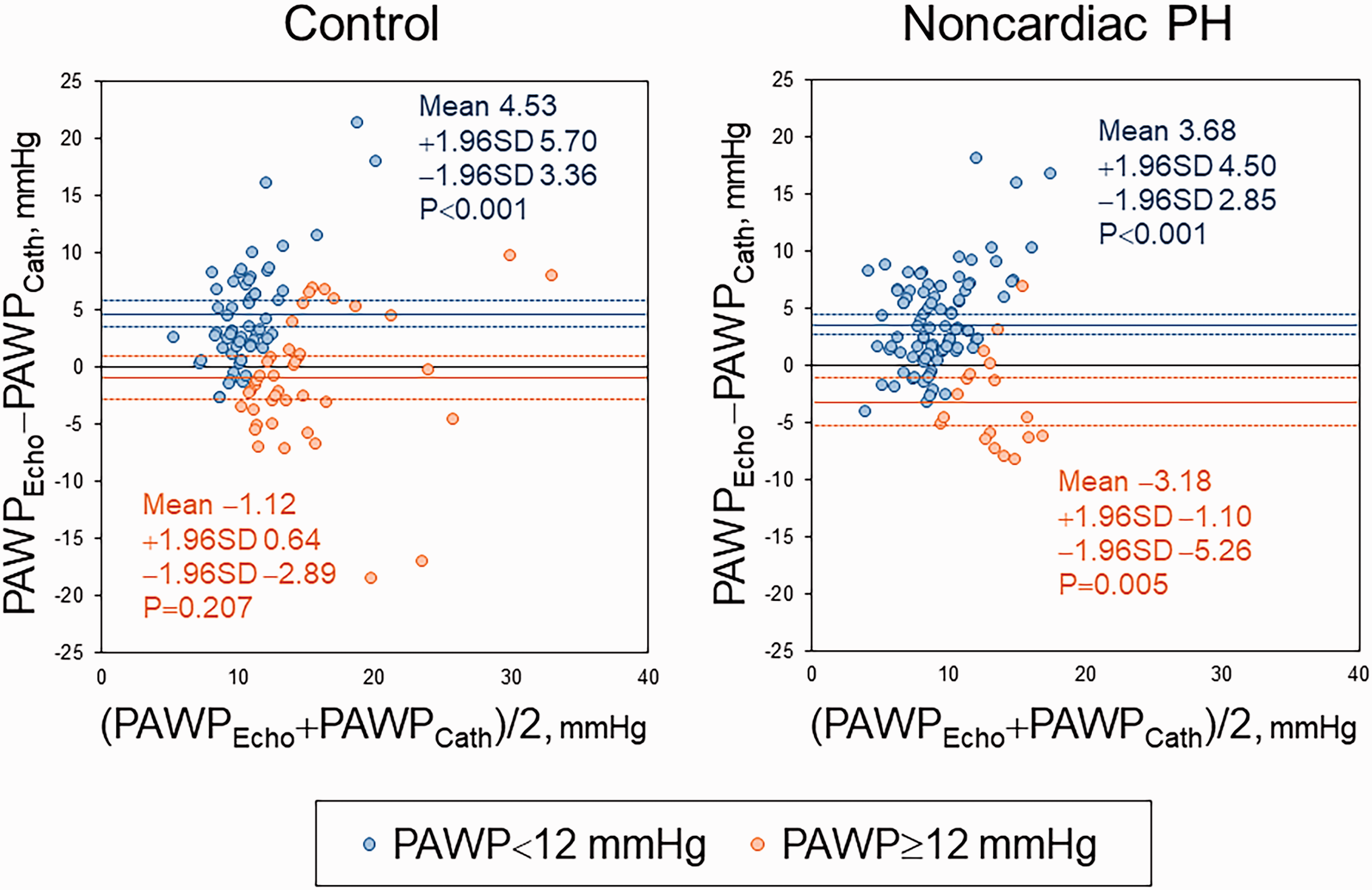
Bland–Altman plots showing the agreement between invasive and estimated PAWP. In patients with pulmonary artery wedge pressure (PAWP) <12 mmHg, similar positive fixed bias was observed both in controls and noncardiac PH patients. In contrast, in patients with PAWP ≥12 mmHg, negative fixed bias was observed in noncardiac PH patients, whereas there was no bias in controls, suggesting an underestimation of estimated PAWP in noncardiac PH.
Differences in hemodynamic determinants of E and LAVI between the control and noncardiac PH groups
To assess the influence of PVR on the correlation between the E value and PAWP, we performed multivariable linear regression analysis in both the groups (Table 3). In the control group, PAWP was an independent determinant of the E value, and PAWP and PVR were independently associated with LAVI in this group (β = 0.38 and 0.21, respectively). In contrast, they independently determined the E value and LAVI in the noncardiac PH group (Table 3). Importantly, the standard partial regression coefficient for PVR was negative, suggesting a negative influence of PVR on these parameters in noncardiac PH patients. When the influence of CI and the eccentricity index on these parameters was assessed, we discovered that CI correlated with the E value, whereas both indices correlated with LAVI in the noncardiac PH group (Fig. 4).
Determinants of Doppler parameters in each group (multivariable analysis).
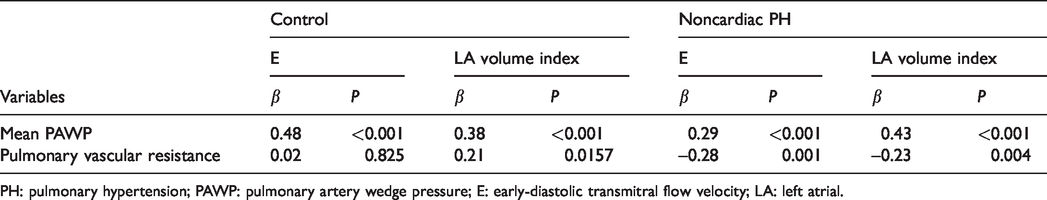
PH: pulmonary hypertension; PAWP: pulmonary artery wedge pressure; E: early-diastolic transmitral flow velocity; LA: left atrial.
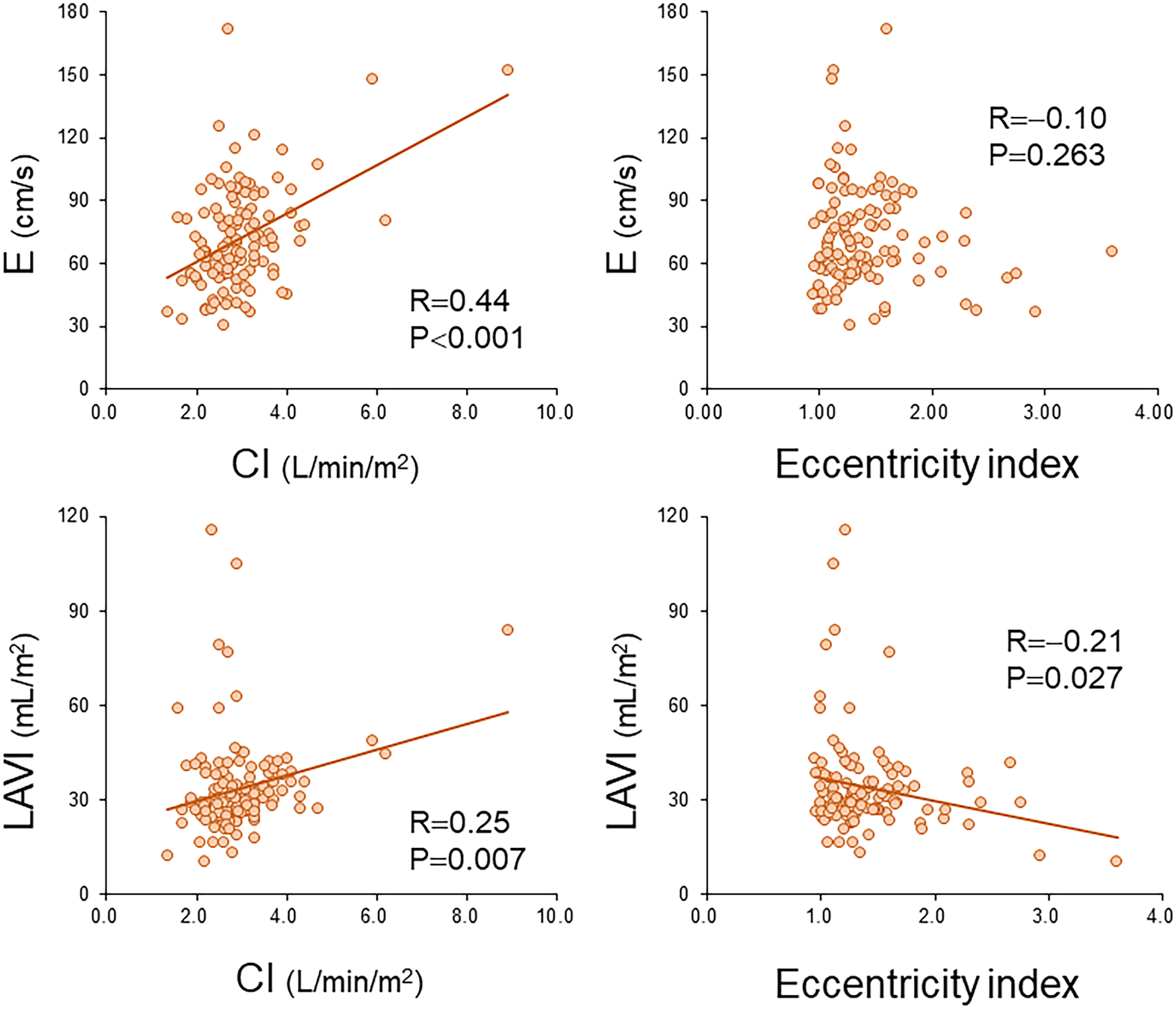
Correlation of the cardiac and eccentricity indices with echocardiographic parameters in the noncardiac PH group.
Discussion
We demonstrated that in the presence of advanced lesions in the pulmonary vasculature, echocardiographic Doppler parameters of the LV filling pressure did not correlate with invasively measured PAWP. We further found that these results could be explained by the opposite action of PVR and PAWP on E, i.e. a higher PVR corresponded to a lower E value in noncardiac PH patients. To the best of our knowledge, this is the first study to demonstrate the influence of the severity of pulmonary vascular lesions on the correlation between echocardiographic LV filling pressure parameters and PAWP, including another population as a control group.
Left-sided heart failure in pre-capillary PH
Historically, little attention has been paid to LV diastolic dysfunction in populations with noncardiac PH because of the conventional knowledge that LV function is not affected in such populations. However, in the past decade, it has been discovered that specific subsections of this population, such as those with connective tissue disease-related PH or pulmonary arterial hypertension with severe decline in RV function, often experience an elevated PAWP.4,5,7,8 LV diastolic dysfunction has been increasingly detected even in mild pre-capillary PH cases and is associated with symptoms and survival in PH patients.7,8 More recently, noncardiac PH patients with multiple cardiovascular risk factors have been recognized as the midpoint of a continuum between noncardiac PH and heart failure with preserved LV EF complicating PH.6 As the tolerance of therapies targeting the pulmonary vasculature decreases with the progression of LV diastolic dysfunction,6 detection of a slight increase in LV filling pressure could play a key role in the estimation of the risk of lung congestion after initiating targeted therapies.
Echocardiographic assessment of LV diastolic function in PH
Echocardiography is currently the first-line tool for the noninvasive assessment of LV diastolic function in patients with cardiovascular disease.3 Among the various echocardiography parameters, the ASE/EACVI recommends the use of transmitral Doppler flow velocity, e′ value, peak velocity of tricuspid regurgitation, and LAVI for diastolic grading.3 Among these parameters, the diagnostic value of E/e′ in pre-capillary PH has been confirmed by some researchers.23–26 However, because previous studies mainly focused on the differentiation of pre-capillary PH and PH-LHD, the differences in relationships between E/e′ and LV filling pressure between patients with and without pulmonary vascular lesions have not yet been addressed. As mentioned above, a recently recognized population with complicated pulmonary vascular lesions and LV diastolic dysfunction suggests the need for precise assessment of the LV filling pressure even in patients with apparent pulmonary vascular lesions. Recently, Leung et al.17 demonstrated that ASE algorithms often produce indeterminate results in patients with suspected pulmonary arterial hypertension, probably because it does not incorporate the tricuspid regurgitation velocity. Ran et al.27 further demonstrated an improved accuracy with a significant number of wrong classifications of the 2016 ASE algorithms compared to the 2009 algorithms in PH patients. Cameron et al.16 also applied the algorithm to PH patients and illustrated that it was accurate only in patients with advanced LV diastolic dysfunction and elevated LV end-diastolic pressure. These data suggest that conventional echocardiographic parameters do not highly predict LV filling pressure in PH patients. In the present study, we further found a blunted sensitivity of E/e′ in detecting elevated PAWP in noncardiac PH patients (Fig. 3), which could be associated with the negative effect of elevated PVR on E velocity (Table 3). In the present study, various Doppler echocardiographic parameters were associated with PAWP in the control group and in patients with less-advanced noncardiac PH but not in patients with advanced noncardiac PH, suggesting that these parameters could be an implausible marker of LV filling pressure in patients with apparent pulmonary vascular lesions.
Physiological determinants of echocardiographic parameters of LV filling pressure
In the presence of PH, an increase in RV volume causes a leftward shift of the interventricular septum, resulting in impaired LV filling because of a reduced diastolic pressure fall in the left ventricle.28–30 At the same time, this diastolic ventricular interaction elevates LV diastolic pressure in the absence of LV myocardial disease.31 As the E value is determined based on the LA–LV pressure gradient in early diastole,32 this interventricular interaction can lower the E value even in the presence of elevated LV diastolic pressure. We accordingly found that the E value was determined not only by PAWP but also by PVR in noncardiac PH. In contrast, advanced RV systolic dysfunction causes a reduced blood flow through the pulmonary vasculature, resulting in a reduced LV preload, lowered LV diastolic pressure, and subsequent reduction of the E value.33–35 In fact, an observation in patients with severe PH during staged balloon atrial septostomy, in whom CO was severely decreased, showed normal LV end-diastolic pressure despite elevated RV diastolic pressure.36 Therefore, diastolic ventricular interaction and reduced LV preload can have opposing effects on LV diastolic pressure, and the LV diastolic pressure can change in accordance with the factor that strongly influences hemodynamics. If the ventricular interaction is stronger, the increased LV filling pressure owing to the diastolic shift of the interventricular septum would be relieved by pulmonary vasodilator therapy. Therefore, the therapy does not always result in a further increase in the LV filling pressure. From this perspective, it would be more valuable to determine the cause of LV filling elevation, intrinsic myocardial damage, or exaggerated ventricular interaction in PH patients.
As mentioned above, in patients with advanced noncardiac PH, the E value remained low even with a mild elevation in PAWP (Figs 3 and 5). The same phenomenon has been observed in hypertrophic cardiomyopathy patients, in whom severely impaired LV relaxation prevented an increase in the E value.37 In addition, we found that the CI positively correlated with the E value in noncardiac PH, whereas LV eccentricity did not, suggesting that the reduced E value in our study cohort may have been caused mainly by a reduction in the LV preload rather than by ventricular interaction. Conversely, the lateral and septal e′ were significantly correlated with age of the controls and noncardiac PH patients (Supplemental Figure 2). Nevertheless, E/e′ did not correlate with PAWP in noncardiac PH, suggesting that the interaction between the E value and PAWP is blunted, rather than a loss of relationship between the e′ value and LV relaxation.
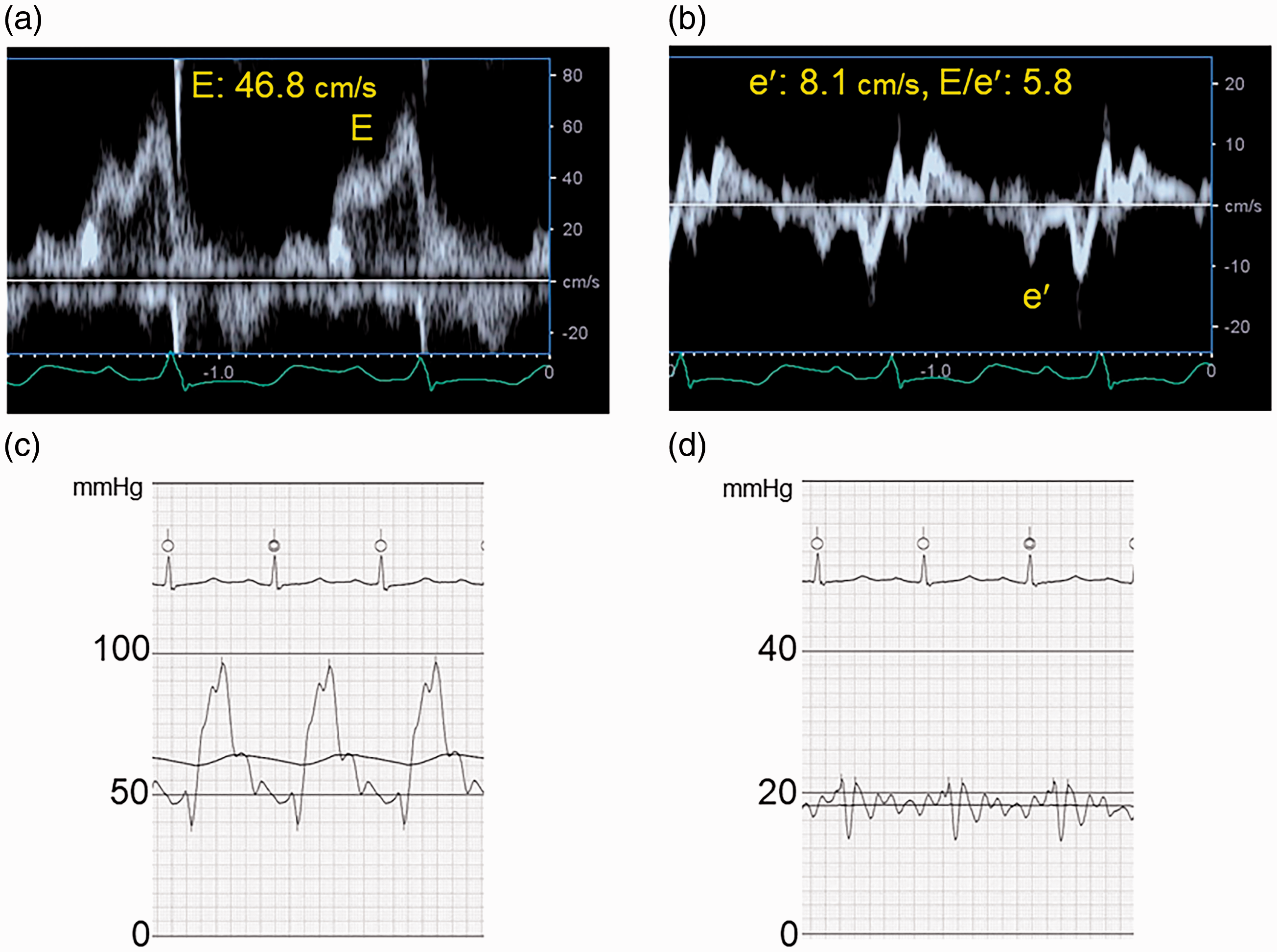
Discrepancy between echocardiographic findings and invasively measured pulmonary artery wedge pressure observed in a case of noncardiac pulmonary hypertension. Transmitral Doppler flow (a), lateral mitral annular Doppler velocity (b), pulmonary artery pressure waveform (c), and pulmonary arterial wedge pressure (PAWP) waveform (d), obtained from a 30-year-old man with portopulmonary hypertension. His pulmonary vascular resistance was 5.4 Wood units. Note the elevated PAWP despite low early-diastolic transmitral velocity (E) as well as low E/e′.
In contrast to the E value, LAVI linearly correlated with PAWP even in the presence of high PVR. Therefore, we considered LAVI to be a potentially reliable marker of elevated LV filling pressure in advanced noncardiac PH patients, although it does not directly represent the instantaneous LV filling pressure. Enlarged left atrium regardless of reduced blood return owing to pulmonary vascular lesion could suggest cumulative load on the left atrium due to elevated LV filling pressure.
Clinical implications
Because of newly established therapies targeting the pulmonary vasculature, detecting a mildly elevated LV filling pressure before treatment is an important issue. Our data suggest that LAVI is the most reliable echocardiographic parameter to identify elevated LV filling pressure in patients with advanced noncardiac PH. It is crucial to recognize that the E value may be blunted by elevated LV filling pressure in advanced noncardiac PH patients, and this Doppler echocardiographic finding may be misleading (Fig. 6). Invasive assessment of LV filling pressure would be recommended in patients showing a large LA volume, even if the patient did not show abnormal Doppler echocardiographic findings. Future studies are expected to elucidate further novel parameters to estimate LV filling pressure in these patients by utilizing recently developed echocardiographic methods.
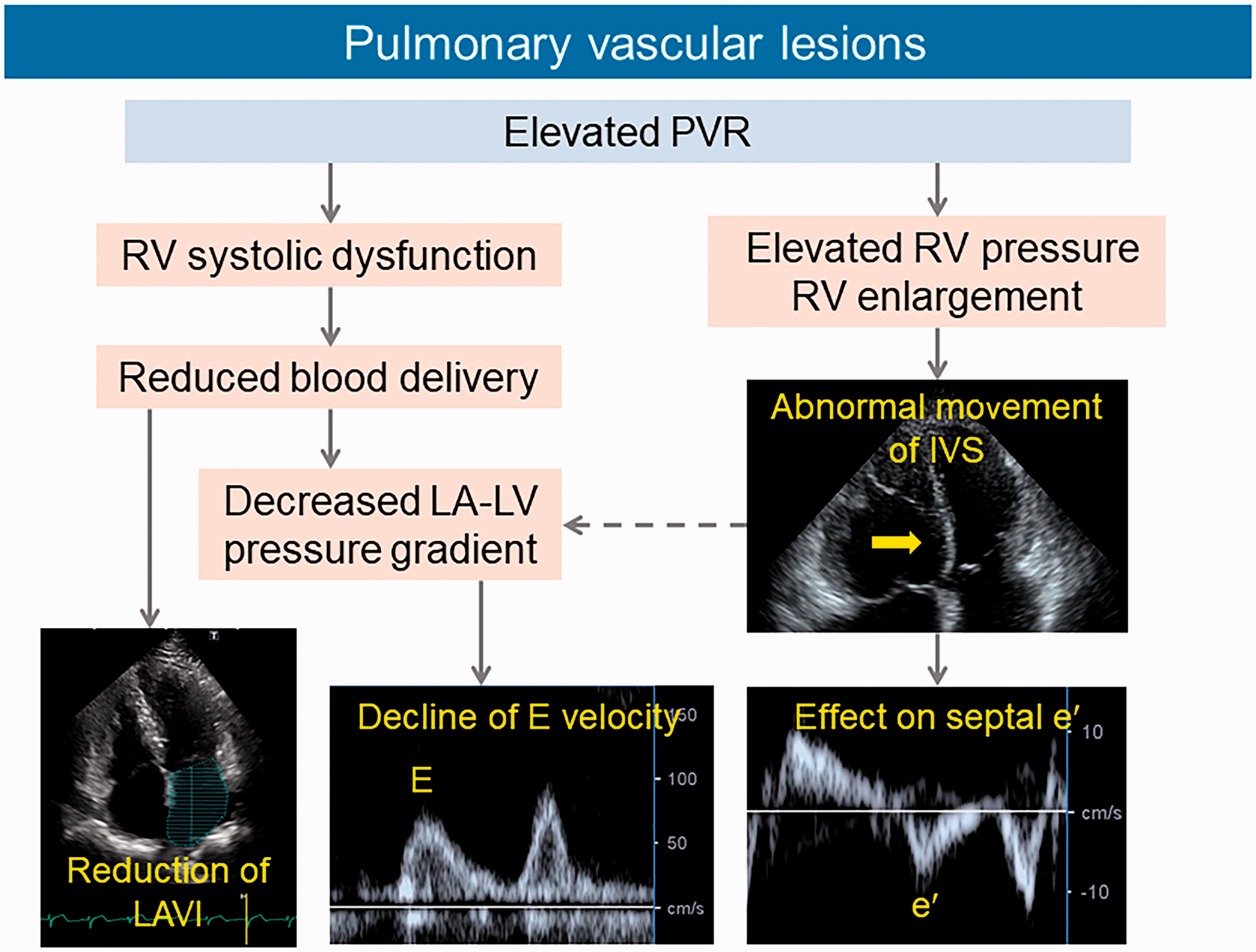
Schematic interpretation of the hemodynamic consequences of pulmonary vascular lesions. Elevated PVR caused by pulmonary vascular lesions decreases LV preload via the pulmonary vasculature, resulting in a decreased LA–LV pressure gradient and subsequent decline in the E value. In addition, elevated RV pressure and RV enlargement cause a shift in the interventricular septum, resulting in an alteration of the septal e′ value, but less so of the lateral e′ value. This abnormal septal motion may also prevent the early LV diastolic pressure drop, which would reduce the E value and reduce LV preload. Further, the reduced inflow to the LA results in a reduction of the LAVI.
Study limitations
This study had several limitations. First, the classification of noncardiac PH included PAH with an elevated PAWP during follow-up. As we recently noticed, patients with pre-capillary PH sometimes have comorbid LV diastolic dysfunction in their clinical course. In these patients, elevated PVR values are due to primary pulmonary vascular lesions but not due to elevated pulmonary venous pressure. However, if we automatically classify the type of PH without considering the causal relationship, these patients are classified as PH-LHD, which does not precisely reflect the pathophysiology of a patient. Nevertheless, we have to acknowledge that our classifications do not completely follow the classification recommended by the guidelines. In addition, we could not completely exclude the possibility of including a small number of HF patients with preserved EF, although we carefully included well-confirmed patients with a history of pre-capillary PH. Second, because of the purpose of setting as homogeneous controls as possible, patients with ischemic heart disease were considered controls. Although well-controlled heart failure with preserved EF could be more suitable as controls, we could not enroll these patients because of their limited number. Furthermore, substantial differences in patient characteristics owing to different disease entities between the noncardiac PH and control groups should be considered even after adjusting for these factors. Third, because of a limited number of patients who underwent LV pressure recordings, we could not obtain the data of LV end-diastolic pressure. Although LV end-diastolic pressure provides information on end-diastolic LV operating stiffness, which is somewhat different from LV filling pressure, a combination of the mean PAWP and LV end-diastolic pressure could provide a more accurate estimation of LV filling pressure because mean PAWP is potentially at a risk of significant error, especially in patients with high LA pressure.38 Finally, echocardiography and pressure measurements were not performed simultaneously, which may have weakened the relationship between echocardiographic parameters and PAWP. However, a comparison to a control group with a similar time lapse between the two examinations (although slightly shorter in the control group) may support the accuracy of the present results.
Conclusions
Doppler echocardiographic parameters of LV filling pressure were not highly predictive of invasively measured LV filling pressure in patients with advanced lesions of the pulmonary vasculature. Among conventional parameters, LAVI may be the most reliable parameter for estimating LV filling pressure in patients with advanced noncardiac PH.
Supplemental Material
sj-pdf-1-pul-10.1177_2045894020983723 - Supplemental material for Influence of advanced pulmonary vascular remodeling on accuracy of echocardiographic parameters of left ventricular filling pressure
Supplemental material, sj-pdf-1-pul-10.1177_2045894020983723 for Influence of advanced pulmonary vascular remodeling on accuracy of echocardiographic parameters of left ventricular filling pressure by Yasuyuki Chiba, Hiroyuki Iwano, Sanae Kaga, Mio Shinkawa, Michito Murayama, Hiroshi Ohira, Suguru Ishizaka, Miwa Sarashina, Shingo Tsujinaga, Shinobu Yokoyama, Masahiro Nakabachi, Hisao Nishino, Kazunori Okada, Kiwamu Kamiya, Toshiyuki Nagai and Toshihisa Anzai in Pulmonary Circulation
Supplemental Material
sj-pdf-2-pul-10.1177_2045894020983723 - Supplemental material for Influence of advanced pulmonary vascular remodeling on accuracy of echocardiographic parameters of left ventricular filling pressure
Supplemental material, sj-pdf-2-pul-10.1177_2045894020983723 for Influence of advanced pulmonary vascular remodeling on accuracy of echocardiographic parameters of left ventricular filling pressure by Yasuyuki Chiba, Hiroyuki Iwano, Sanae Kaga, Mio Shinkawa, Michito Murayama, Hiroshi Ohira, Suguru Ishizaka, Miwa Sarashina, Shingo Tsujinaga, Shinobu Yokoyama, Masahiro Nakabachi, Hisao Nishino, Kazunori Okada, Kiwamu Kamiya, Toshiyuki Nagai and Toshihisa Anzai in Pulmonary Circulation
Footnotes
Author contributions
Yasuyuki Chiba, Hiroyuki Iwano, Sanae Kaga, Mio Shinkawa, Michito Murayama, Hiroshi Ohira, and Toshihisa Anzai contributed to the conception and design of the study. Yasuyuki Chiba, Hiroyuki Iwano, Sanae Kaga, Mio Shinkawa, Michito Murayama, Hiroshi Ohira, Suguru Ishizaka, Miwa Sarashina, Shingo Tsujinaga, Shinobu Yokoyama, Masahiro Nakabachi, Hisao Nishino, Kazunori Okada, Kiwamu Kamiya, and Toshiyuki Nagai contributed to the investigation and acquisition of resource. Yasuyuki Chiba and Hiroyuki Iwano analyzed the data, drafted the manuscript, and critically revised it. All authors gave final approval and agree to be accountable for all aspects of work ensuring integrity and accuracy.
Conflict of interest
The author(s) declare that there is no conflict of interest.
Ethical approval
The study was performed in accordance with the declaration of Helsinki and the ethical standards of the responsible committee on human experimentation (institutional and national). The study protocol was approved by the institutional review board of Hokkaido University Hospital (No. 015-0210).
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
