Abstract
Prostacyclins are the mainstay treatment for patients with severe pulmonary arterial hypertension. This case highlights the transition from selexipag to oral treprostinil. Our patient improved both subjectively and objectively. Cardiac output and index, as measured by the echocardiogram, improved 12% and 7.7%, respectively. Invasive hemodynamic data revealed greater improvements: cardiac output improved by 25% and cardiac index by 28%. Mixed venous oxygen saturation improved from 65% to 71%. A possible explanation is that selexipag has a maximal dose, whereas there is no recommended maximum dose of oral treprostinil. Another theory is oral treprostinil has higher affinity to the IP receptor, though selexipag has a higher specificity. However, there are no bio-equivalency data, and data comparing pharmacodynamics of both drugs are lacking. Furthermore, no head-to-head trials comparing these agents exist.
Introduction
Despite the availability of multiple treatment options for pulmonary arterial hypertension (PAH), this disease has a poor prognosis. Approximately 10 to 15 patients per million are diagnosed with PAH every year and the number of patients living in the U.S.A. with pulmonary hypertension is noted to be between 10,000 and 20,000. 1 Current mainstay PAH treatment consists of drugs that target nitric-oxide, endothelin and prostacyclin pathways. 2 Selexipag is the first oral selective IP prostacyclin-receptor agonist with a higher affinity for IP receptor than for other PG receptors. On the other hand, oral treprostinil is a stable, non-selective, synthetic analogue of prostacyclin with a high affinity for the DP1, EP2, and IP receptors. We report a case of a patient who was transitioned from selexipag to oral treprostinil due to clinical worsening and dose limiting side effects.
Case presentation
Transition table and invasive hemodynamic parameters.
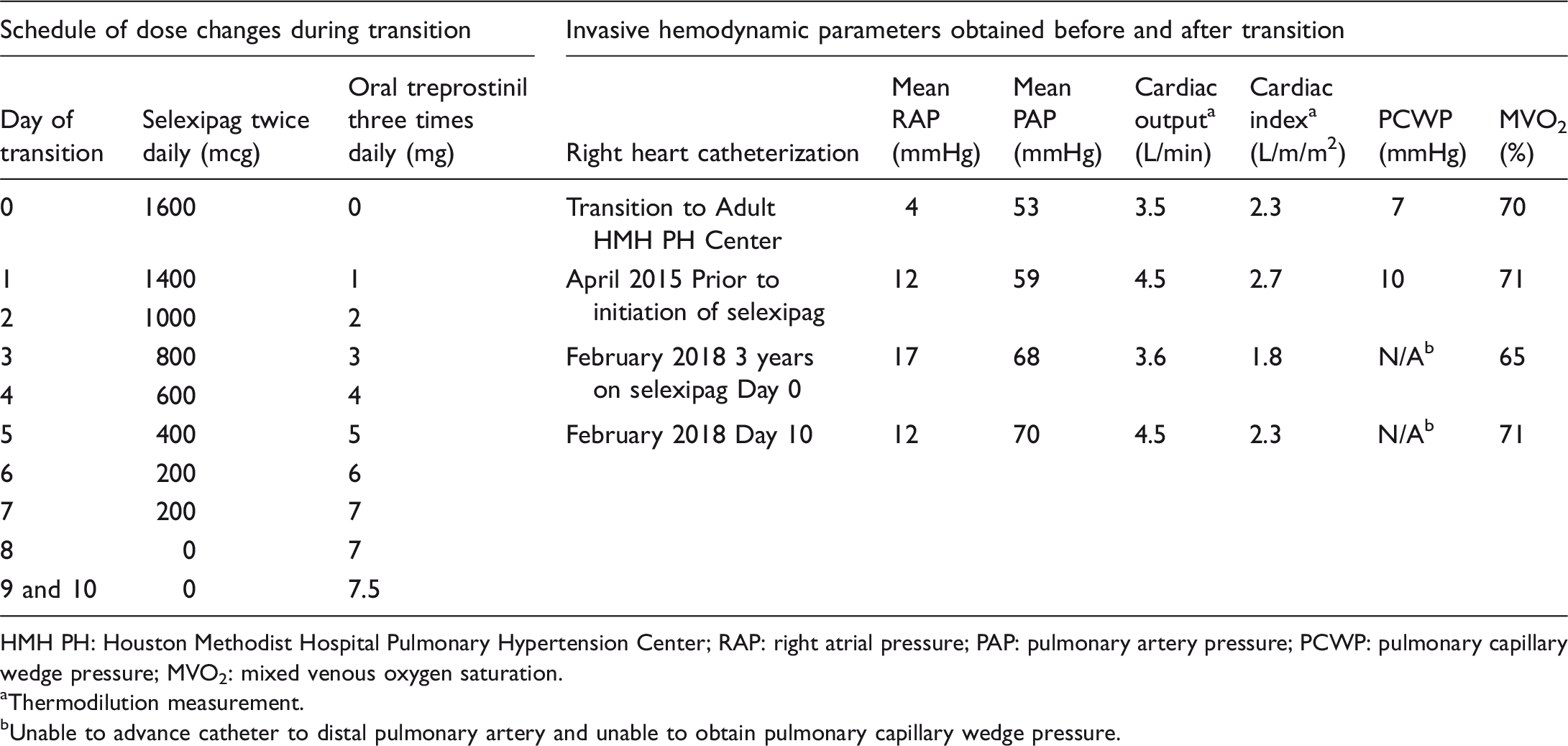
HMH PH: Houston Methodist Hospital Pulmonary Hypertension Center; RAP: right atrial pressure; PAP: pulmonary artery pressure; PCWP: pulmonary capillary wedge pressure; MVO2: mixed venous oxygen saturation.
Thermodilution measurement.
Unable to advance catheter to distal pulmonary artery and unable to obtain pulmonary capillary wedge pressure.
In February 2018, he was admitted for this transition. He was afebrile, heart rate of 85 per minute, respiratory rate of 16 per minute, blood pressure of 135/70 mmHg, oxygen saturation was 95% on room air, and euvolemic on physical exam. Selexipag was slowly tapered, while oral treprostinil was increased to a final dose of 7.5 mg three times daily without any significant side effects except for slight headaches. He noticed improvement in nausea, headache, diarrhea, facial flushing, and jaw pain. The total duration of the transition was 10 days as outlined in Table 1. During the hospital course, echocardiogram and RHC were performed before and after completing this transition with improvement in hemodynamics (Table 1). He was completely off selexipag and taking oral treprostinil 7.5 mg three times daily at the time of discharge (11th day).
Discussion
Prostacyclin and prostacyclin analogues are the mainstay of PAH therapy for patients with severe PAH. Prostacyclins exert their effect primarily through the IP receptor with vasodilatory effect on pulmonary arteries and smooth muscle, inhibition of platelet aggregation, in addition to anti-inflammatory and antiproliferative properties. 3
This patient was initially started on selexipag, which is the first orally available selective agonist of the prostacyclin IP receptor and structurally distinct than prostacyclin. 4 The GRIPHON trail, a phase 3 clinical trial in 2015, demonstrated that patients with PAH treated with selexipag has significantly lower risk of the composite endpoint of death or complication related to PAH versus placebo. However, there was no significant difference in mortality between the two groups. 5 In contrast, treprostinil is a stable, prostacyclin analogue which is not specific to the IP receptor like selexipag and has been shown to improve exercise capacity in PAH patients. 3 Freedom trials also show that a combination of oral treprostinil with endothelin receptor antagonist and/or phosphodiesterase is efficacious, safe and results in a significant reduction in clinical worsening when compared to placebo.6,7
Our case focuses on the transition from selexipag to oral treprostinil. By comparing the echocardiogram indices before and after, cardiac output and index improved by 12% and 7.7%, respectively. Invasive hemodynamic data revealed a 25% and 28% increase in cardiac output and cardiac index, respectively. Mixed venous oxygen saturation improved from 65% to 71% post-transition. These are objective results in the setting of the patient’s subjective report of feeling better after the transition. Oral treprostinil has been available for a long time with less specific mechanism of action and reportedly with poor tolerance. However, our case shows it to be more efficacious and more tolerable in this patient. A possible explanation may be that selexipag has a maximal dose (1600 mcg twice daily), whereas there is no recommended maximum dose of oral treprostinil. Although no treatment guideline for the number of days or frequency for increasing oral treprostinil dose exists, a recommendation to consider 12-month target of 8 mg three times daily has been presented. 8 As our patient was titrated off selexipag while being up-titrated on oral treprostinil, the initial dose of the latter drug was higher and the up-titration was faster than what is described in the literature. Another possibility is perhaps oral treprostinil has a higher affinity for the DP1, EP2, and IP receptors, whereas selexipag has a high specificity for IP receptors. However, there exist no bio-equivalency data of selexipag and oral treprostinil, and no head-to-head trials comparing these agents.
Conclusion
Our case of a young adult male with idiopathic PAH with worsening symptoms and hemodynamics highlights the transition methodology of selexipag to oral treprostinil. Invasive hemodynamics showed some improvement and demonstrated better tolerance. The reason for the subjective and objective improvement noted is unclear but may relate to the higher dose of treprostinil or perhaps the receptor affinity of oral treprostinil in contrast to the more specific IP receptor binding of selexipag. The long-term effects of this transition need to be carefully monitored with long-term follow-up.
Footnotes
Acknowledgements
This case report was presented at the annual meeting of American College of Chest Physicians on 9 October 2018.
Conflict of interest
The author(s) declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
