Abstract
Exercise rehabilitation is underutilized in patients with pulmonary arterial hypertension despite improving exercise capacity and quality of life. We sought to understand the association between (1) patient characteristics and (2) patient-perceived barriers and referral to exercise rehabilitation. We performed a cross-sectional survey of patients with pulmonary arterial hypertension or chronic thromboembolic pulmonary hypertension attending an International PAH meeting. Predictors of referral considered included gender, body mass index, subjective socioeconomic status, insurance type, age, and World Health Organization functional class and perceived barriers assessed using the Cardiac Rehabilitation Barriers Scale. Among 65 participants, those in the lowest subjective socioeconomic status tertile had reduced odds of referral compared to the highest tertile participants (odds ratio 0.22, 95% confidence interval: 0.05–0.98, p = 0.047). Several patient-perceived barriers were associated with reduced odds of referral. For every 1-unit increase in a reported barrier on a five-point Likert scale, odds of referral were reduced by 85% for my doctor did not feel it was necessary; 85% for prefer to take care of my health alone, not in a group; 78% many people with heart and lung problems don’t go, and they are fine; and 78% for I didn’t know about exercise therapy. The lack of perceived need subscale and overall barriers score were associated with a 92% and 77% reduced odds of referral, respectively. These data suggest the need to explore interventions to promote referral among low socioeconomic status patients and address perceived need for the therapy.
Introduction
Patients with pulmonary arterial hypertension (PAH) have reduced exercise capacity1–3 and report burdensome symptoms that reduce their overall health-related quality of life (HRQOL).4–6 Exercise rehabilitation has been shown to improve exercise capacity and HRQOL in PAH. 7 , 8 In recognition of the benefits, current guidelines recommend supervised exercise training as part of the management of patients with PAH by centers with experience taking care of patients with PAH and rehabilitation of compromised patients.9–11 In the United States, access to supervised exercise training is most readily available as a component of exercise rehabilitation performed during enrollment in cardiac or pulmonary rehabilitation.
Despite the guideline recommendations, the extent to which PAH patients are utilizing exercise rehabilitation is currently limited. 12 Studies in chronic cardiopulmonary illnesses where patients receive a similar benefit from exercise have identified unique predictors of referral13–19 and barriers to the uptake of exercise rehabilitation.20–23 While some overlap may exist, these challenges may differ in PAH patients due to their unique pathophysiology and barriers such as travel to specialized centers with experience performing exercise rehabilitation with PAH patients. Recognizing the underutilization and lack of information about the optimal program, experts have called for a better understanding of the practical implementation of exercise therapy, 24 including the need to identify barriers to referral. 25
Identification of patient characteristics and perceived barriers is critical for the development and implementation of exercise rehabilitation programs tailored for patients with PAH.20–22, 26 As a first step toward this goal, we examined the association between both patient characteristics and patient-reported barriers and referral for exercise rehabilitation by surveying patients with PAH or chronic thromboembolic pulmonary attending a large International PAH conference.
Methods
We performed a cross-sectional survey of patients with PAH or chronic thromboembolic pulmonary hypertension (CTEPH) recruited from the voluntary research room at the Pulmonary Hypertension Association International Conference from 29 June–1 July 2018 held in Orlando, FL. The Pulmonary Hypertension Association International Conference is the largest gathering of pulmonary hypertension patients in the world. 27 The study was deemed exempt by the University of Michigan Institutional Review Board, and written informed consent was obtained from all patients (HUM00146004). This study was conducted in accordance with the amended Declaration of Helsinki. Permission was obtained for the use of the survey instruments.
Study population
Participants in the research room were eligible if age ≥18 and if they were diagnosed with PAH or CTEPH by right heart catheterization according to guideline recommendations. Patients were excluded if they were unable to exercise due to orthopedic or other nonpulmonary hypertension-related limitations, lived outside the United States, or unable to speak or read English.
Measures
All participants in the research room completed a universal data collection questionnaire, which included information on demographic characteristics, etiology of pulmonary hypertension, World Health Organization (WHO) functional class symptoms, and medications.
Predictors of referral
Patients were specifically asked information on characteristics previously associated with referral to either cardiac or pulmonary rehabilitation, including age,13–15 gender, 14 , 16 body mass index (height and weight), 17 subjective socioeconomic status, 18 insurance type, 18 and WHO functional class. 19 Subjective socioeconomic status was determined using the MacArthur Scale of Subjective Social Status (Supplemental Fig. 1). 28 The MacArthur Scale of Subjective Social Status is a validated scale used to quantify a person’s sense of social standing incorporating multiple socioeconomic status dimensions including education, income, and occupation. 29 Participants were asked to rate where they were on a ladder ranging from 1 to 10 in regards to income, occupation, or education compared to other people in the United States. Participants were split into tertiles to define low, middle, or high subjective socioeconomic status. Participants’ primary insurance type was classified as private or public (Medicaid or Medicare).
Patient-perceived barriers to referral
Patient-perceived barriers to rehabilitation were determined using the Cardiac Rehabilitation Barriers Scale (Supplemental Fig. 2). 30 The survey was designed to assess the impact of patient, provider, and health-system barriers on the utilization of rehabilitation in patients regardless of whether they have been referred to or attended rehabilitation. The survey was modified to include “exercise therapy” defined as either cardiac or pulmonary rehabilitation in place of “cardiac rehabilitation” for the pulmonary hypertension population with approval from the instrument developer. The survey is a 21-item questionnaire that includes statements of factors that influence participation in exercise rehabilitation rated on a five-point Likert scale ranging from “1 = strongly disagree” to “5 = strongly agree.” A mean barrier score was calculated from the average of all the questions, and four average subscale scores were created using the questions related to perceived need/healthcare factors, logistics, work/time conflicts, and comorbidities/functional status. The survey has previously been shown to be a reliable and valid measure of perceived barriers. 30
Primary outcome
The primary outcome was a previous referral to exercise rehabilitation. Exercise rehabilitation was defined as a supervised rehabilitation program that required referral by a healthcare provider.
Statistical analysis
Patient demographic characteristics, etiology of pulmonary hypertension, WHO functional class profile, medication use, and survey results are reported using frequencies for categorical variables and means ± standard deviations (SD) for continuous variables, as appropriate.
The association of (1) patient characteristics and (2) patient-perceived barriers and referral to exercise rehabilitation was assessed using univariable and multivariable analyses with adjustment for age and WHO functional class in the multivariable models. Age and WHO functional class were adjusted for as both have previously been shown to be associated with increased interest in exercise rehabilitation. 12 Referral to exercise rehabilitation was the primary dependent variable.
The first analyses sought to determine patient characteristics associated with referral. Separate logistic regressions were performed with gender, body mass index, subjective socioeconomic status, insurance type, age, and WHO functional class as the primary independent variables. Multivariable models were next done adjusted for age and WHO functional class. Using the final multivariable regression model, the predicted percent referral and 95% confidence interval was determined using the Stata (version 15) margins command.
The second analysis explored the association of patient-perceived barriers and referral to exercise rehabilitation. The frequency of barriers to rehabilitation categorized as low (Likert score 1–2), neutral (Likert score 3), or high (Likert score 4–5), and referral rates were determined for descriptive purposes. Univariable analysis was performed to compare reported barriers among those not referred and referred to exercise rehabilitation. Next, multivariable logistic regression models were conducted again adjusted for age and WHO functional class. Additional multivariable adjustments were not performed because of sample size limitations. In these models, separate multivariable logistic regressions were performed using the mean barrier score (patient average of the barriers), the four subscale categories (perceived need/healthcare factors, logistics, work/time conflicts, and comorbidities/functional status), and the score of the 21 barrier questions as the primary independent variables. A p value of <0.05 was used to determine statistical significance. Analyses were conducted using Stata 15 (College Station, TX).
Results
Of the 82 people screened, 12 met an exclusion criterion and 5 had incomplete survey data, leaving 65 participants in the current analysis. Participant demographic characteristics, etiology of pulmonary hypertension, WHO functional class, subjective social status, insurance type, and medication use are shown in Table 1. Among the 65 participants, 52% (n = 34) had been referred to exercise therapy. Most of the participants were female (87%), had PAH (97%), and WHO functional class 2 symptoms (55%). Rates of referral among low, middle, and high socioeconomic status participants were 39%, 58%, and 71%, respectively.
Characteristics of the 65 participants.
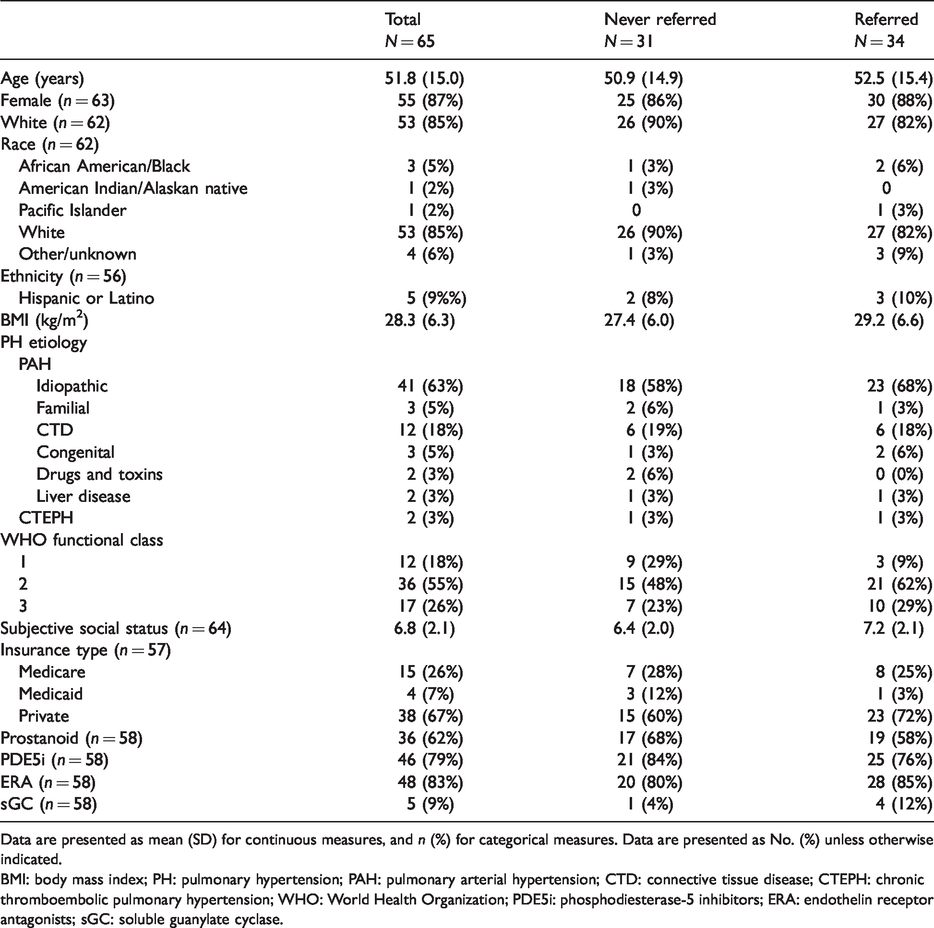
Data are presented as mean (SD) for continuous measures, and n (%) for categorical measures. Data are presented as No. (%) unless otherwise indicated.
BMI: body mass index; PH: pulmonary hypertension; PAH: pulmonary arterial hypertension; CTD: connective tissue disease; CTEPH: chronic thromboembolic pulmonary hypertension; WHO: World Health Organization; PDE5i: phosphodiesterase-5 inhibitors; ERA: endothelin receptor antagonists; sGC: soluble guanylate cyclase.
The results of the univariable and multivariable analyses exploring the association between patient predictors and referral to exercise rehabilitation are shown in the supplementary table (Supplemental Table 1) and Table 2, respectively. In the multivariable analysis adjusted for age and WHO functional class, low subjective socioeconomic status was associated with reduced odds of referral to exercise rehabilitation compared to participants with high subjective socioeconomic status (odds ratio (OR) 0.22, 95% confidence interval (CI): 0.05–0.98, p = 0.047). There was no association between insurance type, body mass index, or gender. The predicted percentage referral for participants with low and high subjective socioeconomic status adjusted for age and WHO functional class is shown in Fig. 1. Using the final multivariable model, 36% (95% CI: 18%–53%) of participants with low socioeconomic status were predicted to be referred compared to 69% (95% CI: 45%–92%) of participants with high subjective socioeconomic status.
Results of multivariable logistic regression adjusted for age and WHO functional class.
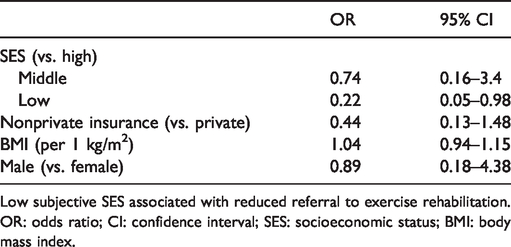
Low subjective SES associated with reduced referral to exercise rehabilitation.
OR: odds ratio; CI: confidence interval; SES: socioeconomic status; BMI: body mass index.
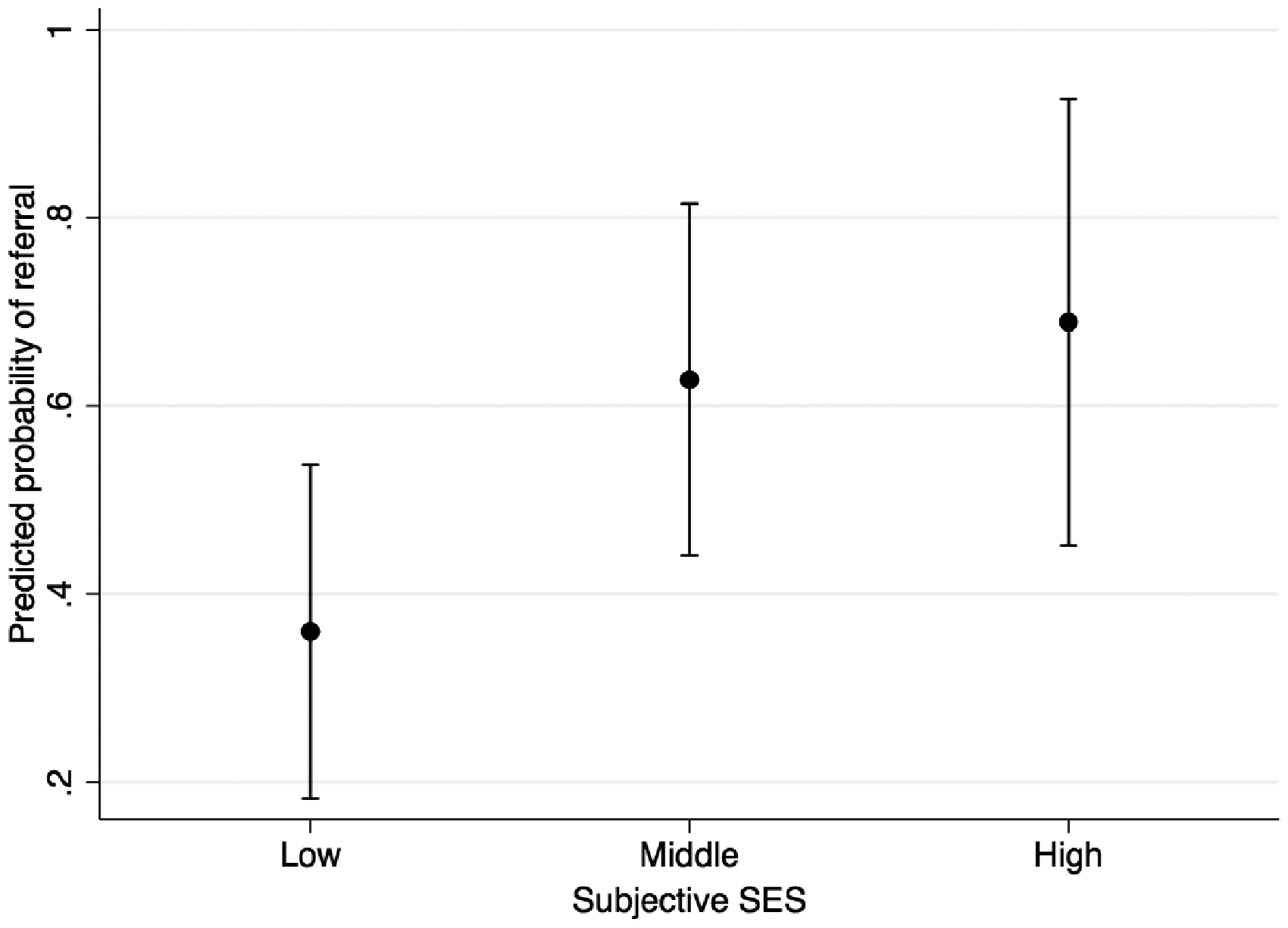
Predicted probability of referral to exercise rehabilitation by tertile of subjective socioeconomic status. Low subjective SES patients have a lower predicted probability of being referred to exercise rehabilitation. Among low subjective SES participants, 36% (95% CI: 18%–53%) were predicted to be referred to exercise rehabilitation compared to 69% (45%–92%) of high subjective SES participants.
We next examined self-reported barriers to exercise therapy grouped by referral status (Table 3). The highest average barriers for the entire cohort were don’t have the energy (mean ± SD: 2.9 ± 1.4), already exercise at home, or in my community (2.8 ± 1.4), time constraints (2.7 ± 1.4), travel (2.6 ± 1.3), and cost (2.6 ± 1.4). Compared to participants referred, those not referred reported a higher barrier score to several barriers including: cost; didn’t know about exercise therapy; don’t need exercise therapy, already exercise at home, or in my community; doctor did not feel it was necessary; many people with heart and lung problems don’t go, and they are fine; can manage my heart and lung problem on my own; think referred, but the rehab program didn’t contact; and prefer to take care of my health alone, not in a group. In addition, those not referred reported increased barriers in the perceived need subscale, healthcare subscale, and overall mean barrier score. The frequency of barriers described as low, neutral, or high and referral is shown in Table 4. No barriers had a higher percentage of referral among those participants who reported a barrier as high as opposed to low. The results of the univariable logistic regression are shown in the online supplement (Supplemental Table 2).
Average of barriers to exercise therapy grouped by referral status.
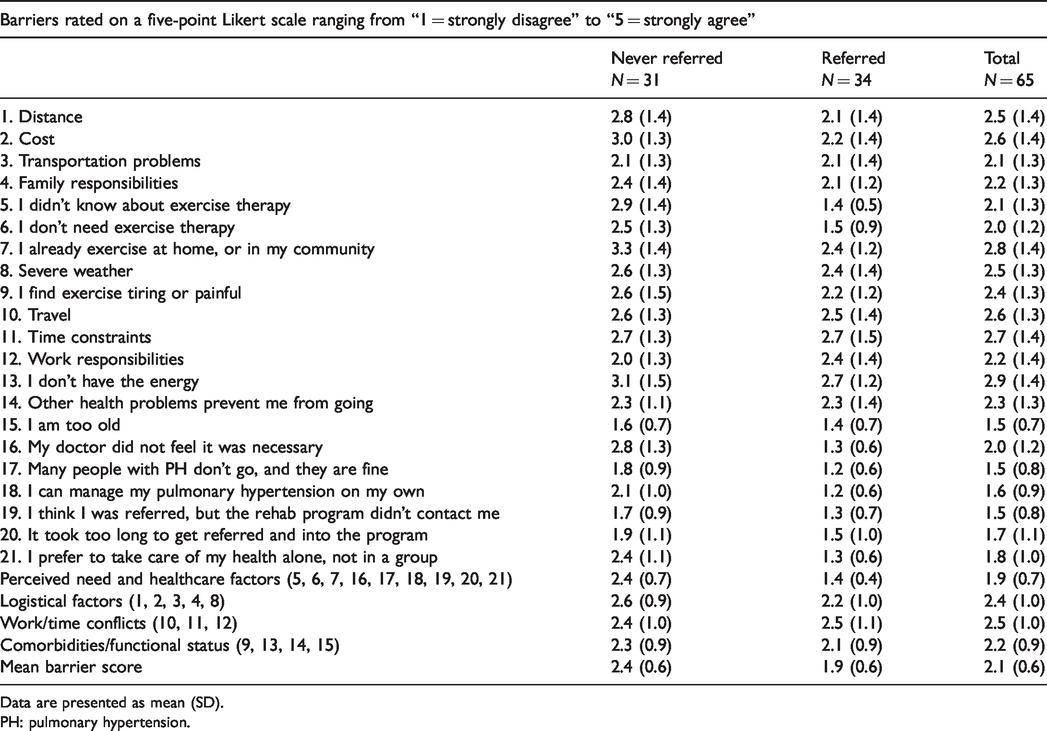
Data are presented as mean (SD).
PH: pulmonary hypertension.
Summary of rates of referral to pulmonary rehabilitation by severity of barrier.

Barriers were rated on a five-point Likert scale ranging from “1 = strongly disagree” to “5 = strongly agree.” The frequency of a barrier categorized as low (Likert 1–2), neutral (Likert 3), or high (Likert 4–5), and rates of referral are shown. Data are presented as the percentage of those referred divided by all participants who similarly rated the barrier.
PH: pulmonary hypertension.
Several barriers were associated with decreased odds of referral in the multivariable model adjusting for age and WHO functional class (Fig. 2). For every 1-unit increase in a barrier, odds of referral were reduced by 85% for my doctor did not feel it was necessary; 85% for prefer to take care of my health alone, not in a group; 78% for many people with heart and lung problems don’t go, and they are fine; and 78% for didn’t know about exercise therapy. A 1-unit increase in the lack of perceived need and healthcare subscale was associated with a 92% reduced odds of referral. The overall barriers score was additionally associated with reduced odds of referral (OR 0.23, 95% CI: 0.08–0.69).

Odds of referral to exercise rehabilitation adjusted for age and World Health Organization functional class. Odds ratio (95% confidence interval) representing change in odds for referral for every 1-unit increase in a reported barrier adjusted for age and WHO functional class. The subscales are separated by the solid lines. The odds ratio summarizing each subscale is denoted by a dashed line.
Discussion
Among patients with pulmonary hypertension attending a national meeting, patient characteristics, and perceived barriers to rehabilitation were inversely associated with referral to exercise rehabilitation. Low subjective socioeconomic status was associated with a reduced odds of referral to rehabilitation compared to high subjective socioeconomic status. Compared to participants who were referred to exercise rehabilitation, those who weren’t referred prefer to take care of health alone, not in a group; had a doctor did who did not feel it was necessary; believed many people with heart and lung problems don’t go, and they are fine; didn’t know about exercise therapy; and/or had a higher perceived need subscale score and overall barriers score. Taken together, these findings suggest opportunities to increase referral to rehabilitation through advocacy and improving patient and physician understanding of the benefits of exercise rehabilitation.
Our study sought to look at the association between several common predictors of referral in other chronic cardiopulmonary processes and referral to exercise rehabilitation among PAH and chronic thromboembolic pulmonary patients. We found lower subjective socioeconomic status was associated with reduced referral while age,13–15 WHO functional class, 12 gender, 14 , 16 body mass index (height and weight), 17 and insurance type 18 were not. Disparities in access to care secondary to low socioeconomic status, including exercise rehabilitation, have previously been described in other chronic cardiopulmonary diseases.31–33 A recent statement from the American Thoracic Society highlighted the lack of and need for systematic investigation of health disparities in the diagnosis, treatment, and outcomes of patients with pulmonary hypertension. 34
The limited prior work in pulmonary hypertension has highlighted disparities in care among patients with low socioeconomic status. Patients with low socioeconomic status present with more advanced disease 35 and have worse outcomes including mortality. 36 Differences in access to therapies used to treat pulmonary hypertension is not well described and could explain some of the observed differences in outcomes. The confirmation of reduced referral confirms the existence of a modifiable disparity in access to an important therapy among patients with pulmonary hypertension and is a necessary first step in reducing such healthcare disparities. 32 The next, more difficult task remains the development of interventions aimed at promoting rehabilitation in lower socioeconomic status patients, which thus far have also been limited in the cardiac and pulmonary rehabilitation literature. 37 Recent work suggests financial incentives have the potential to increase participation among low socioeconomic status patients. 38
An improved understanding of patient-perceived barriers also has important implications and was a point-of-emphasis in a recent American Thoracic Society and European Respiratory Society Policy Statement. 25 Logistical barriers such as distance or work/time conflict have often by cited as the reason why people are unable to go and has led to a push for novel delivery methods. 25 , 39 While these barriers were often encountered in our cohort (i.e. time constraints), there was not a strong association with referral patterns. Rather, higher barriers related to perceived need or expected benefit from either the provider or patient perspective were associated with reduced odds of referral in our study.
Specifically, the finding of the strong associations between both the patient knowing about exercise rehabilitation and provider perceived benefit of exercise rehabilitation and referral is important as there has been interest in the potential to address low referral rates by increasing provider and patient knowledge about the benefits of rehabilitation. 40 Such targeted educational interventions may more easily be implemented than process changes in care delivery in the short term and have been shown to have impact in increasing access to rehabilitation. 41 This is supported by the recognition that one of the strongest predictors of referral to exercise rehabilitation in cardiac rehabilitation is the physician’s perceived benefit of rehabilitation. 42 Guidelines have been vague in recommendations for exercise training despite increasing evidence. 8 The recent World Symposium recommends supervised exercise training for physically deconditioned patients. 11 A first step toward increasing provider knowledge of populations who may benefit could be further clarification in consensus statements or guidelines on the patient population to target similar to the well-defined risk stratification used in recommendations around PAH-specific mediactions. 11 Importantly, our study only involved the patient perspective. The logical next necessary step is to understand the provider’s perspective of barriers.
At the same time, improving patient knowledge of the benefits is critical. Face-to-face interventions with a healthcare provider emphasizing the potential benefits of rehabilitation is an important component of successful referral and, most importantly, subsequent utilization. 43 , 44 At the very least, providing an adequate understanding of the potential benefits of rehabilitation will allow more informed shared decision making empowering the patient to make the optimal decision for themselves. 45 Future work aimed at increasing referrals should consider the impact of perceived need and build on the above prior work to continue to develop targeted strategies that address this barrier.
Our study has limitations. This is a cross-sectional study that is unable to determine causality. The study design is often used to inform future work, 46 particularly when there is a sparsity of data regarding both the impact of patient characteristics 34 and perceived barriers to referral. 45 The diagnosis of PAH and chronic thromboembolic pulmonary relied on patient report. All participants were specifically asked about having had a right heart catheterization, and the high use of PAH-specific medications suggests at least some component of precapillary pulmonary hypertension in the participants though the presence of participants with PH due to left heart disease or chronic lung disease is possible. Given the data collection methods, we were unable to interview the patients’ providers to understand the physician’s perspective on the recent disease course and whether the timing was optimal for referral. Physician perceptions regarding rehabilitation are important for future intervention development and thus warranted in future studies. Patients who attend a national scientific meeting may be unlike other patients with PAH, and thus, selection bias is likely for our study. These participants are likely highly involved and informed in their care and may not be representative of the PAH population in general. The total number of patients who attended the conference and would have been eligible for our study is uncertain. This may also represent a selection bias that limits the generalizability of the study. Additionally, while the prevalence of PAH in the United States by race and ethnicity is uncertain, 47 the high percentage of white participants in our study is likely an overrepresentation compared to the population of people with PAH in the United States. Lastly, despite being a comparatively large survey of patients with pulmonary hypertension, the sample size is not large and includes only two patients with CTEPH. This limits the ability to adjust for multiple comparisons and generalize the results to patients with CTEPH. A p value of 0.05 was used to determine significance given the likelihood of missing real associations due to the small sample size if a lower p value was used.
Conclusion
We found that lower subjective socioeconomic status and barriers related to the perceived need for exercise rehabilitation were associated with decreased referral to rehabilitation. Future work should explore interventions to promote referral to exercise rehabilitation among low socioeconomic status patients and specifically address the perceived need for therapy among patients with pulmonary hypertension.
Supplemental Material
sj-pdf-1-pul-10.1177_2045894020974926 - Supplemental material for Impact of patient characteristics and perceived barriers on referral to exercise rehabilitation among patients with pulmonary hypertension in the United States
Supplemental material, sj-pdf-1-pul-10.1177_2045894020974926 for Impact of patient characteristics and perceived barriers on referral to exercise rehabilitation among patients with pulmonary hypertension in the United States by Thomas M. Cascino, Carmel Ashur, Caroline R. Richardson, Elizabeth A. Jackson and Vallerie V. McLaughlin in Pulmonary Circulation
Footnotes
Author contributions
TMC takes responsibility for (is the guarantor of) the content of the manuscript, including the data and analysis. CA, CRR, EAJ, and VVM contributed substantially to the study design, data analysis and interpretation, and the writing of the manuscript.
Acknowledgments
We would like to thank Susie McDevitt, Catherine Knight, Cindy Alsamarraie, and Jennifer Alford for their assistance in administering the survey.
Conflict of interest
TMC: The University of Michigan has received research funding from Actelion Pharmaceuticals US, Inc.; CA, CRR, and EAJ have no disclosures. VVM has served as a consultant and/or advisor for Actelion Pharmaceuticals US, Inc., Bayer, Gilead Sciences, Inc., Medtronic, Merck, St. Jude Medical, and United Therapeutics Corporation. The University of Michigan has received research funding from Actelion Pharmaceuticals US, Inc., Arena, Bayer, and Sonovie. Dr Jackson reports research funding from NIH, and Amgen; editorial board membership: Circulation: Cardiovascular Quality and Outcomes; consulting: American College of Cardiology and McKesson, Inc.; Expert witness for DeBlase Brown Everly LLP.; and royalties for UpToDate.
Funding
Dr Cascino was supported by a National Institutes of Health T32 postdoctoral research training grant (T32-HL007853).
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
