Abstract
Exercise training was not traditionally recommended for patients with pulmonary hypertension. However, recent work has demonstrated that exercise improves endurance and quality-of-life in patients with pulmonary hypertension. Unfortunately, patients with pulmonary hypertension are often sedentary. While some studies have examined patient attitudes to exercise, none have investigated physician perspectives on exercise in patients with pulmonary hypertension. This multinational survey of physicians involved in treating patients with pulmonary hypertension sought to ascertain physician attitudes to exercise and physician-identified barriers and enablers of exercise in this patient population. We collected cross-sectional survey data from a cohort of 280 physicians, including rehabilitation physicians, cardiologists, respiratory physicians and rheumatologists. We found that overall, 86% physicians recommended exercise, in line with current guidelines, although there were differences in the rationale for prescribing exercise and in the type of exercise prescription. Barriers to exercise included patient-related factors, such as patient ill health preventing exercise; poor patient motivation and lack of understanding regarding the benefits of exercise. Systemic barriers included cost/funding issues and limited availability of appropriate services. Perceived enablers of exercise included access to appropriate programmes, provision of education and supportive treating clinicians. Further research is required to identify and implement interventions to promote physical activity in patients with pulmonary hypertension.
Introduction
Pulmonary hypertension (PH) is a chronic, disabling condition that often results in exercise limitation, reduced quality-of-life, progressive dyspnoea and increased mortality. The estimated global prevalence of PH is 1%, increasing to 10% for those aged over 65 years of age. 1 Pharmaceutical therapy and exercise based rehabilitation studies have focused predominantly on pulmonary arterial hypertension (PAH), a subtype of PH, or PAH and chronic thromboembolic pulmonary hypertension (CTEPH). Few studies have examined the effect of exercise in patients with PH from other groups, such as due to left heart disease. Historically, due to safety concerns, exercise was not routinely recommended for people with PAH. 2 However, mounting evidence suggests that supervised exercise is safe and beneficial for this population, with positive benefits on exercise capacity, endurance and quality-of-life.3–5 Exercise training and rehabilitation has now been recommended by the European Society of Cardiology and the European Respiratory Society (class II, level of evidence B). 6 An Expert Taskforce from the recent World Symposium on Pulmonary Hypertension (2018) strongly recommended an individually prescribed exercise training program for patients stable on medication, undertaken in PH expert centres and supervised by rehabilitation professionals. 7 They note that the focus of their task force was on PAH and CTEPH, which they referred collectively to as PH (despite many other different types of PH that can also occur).
Recent reviews of exercise training in PH have suggested supervised individualised outpatient exercise training sessions two-to-three times per week, each of 45–60 min duration.8,9 These recommendations have been based on a number of small studies demonstrating increased exercise capacity and quality of life in an outpatient setting.10–16 Despite recommendations, patients with PH are often sedentary or have low physical activity levels.17–20 Uptake of pulmonary rehabilitation is variable, 21 with low rates of independent exercise once the programme had finished. 22
It is well-recognised that physicians’ personal level of physical activity correlates with the likelihood of them encouraging exercise in their patients.23,24 Although potentially influenced by recall bias, doctors self-reported being more active than the general population, with a greater proportion of doctors meeting recommended national guidelines for levels of physical activity (78% of survey participants compared to 64.5% of the general US population). 25 Physicians’ discussion of their own physical activity with patients may improve their credibility as health-care professionals and increase patient motivation to exercise, compared to if a physician did not mention their own physical activity (p < 0.001). 26 It is therefore important to ascertain physicians’ level of physical activity as this may influence their attitude to exercise and the likelihood they will recommend exercise to patients as a therapeutic intervention.
Most research exploring physicians’ attitudes to exercise training has been done in the general practice setting.27–30 General practitioners (GPs) typically report positive attitudes towards exercise, with 73% of respondents agreeing or strongly agreeing ‘any amount of physical activity is beneficial to health’. 27 However, self-reported promotion of exercise by GPs was low, with only 8% of GPs reporting that they always gave advice regarding physical activity. 27 A study of 43 sports physicians similarly found that while these physicians had positive attitudes to exercise counselling, only 51% indicated they often discussed physical activity with patients. 31
Studies of exercise attitudes and adherence to exercise training have focused largely on patient perspectives32,33; few have considered treating clinician or implementers’ perspectives, although these may influence patient behaviour, and offer valuable insights into improving patient adherence. 34 To our knowledge, there are no published studies assessing physicians’ attitudes towards exercise or rehabilitation and their perspectives on perceived barriers and enablers of exercise for patients with PH.
This study sought to determine beliefs and patterns of exercise prescription among medical specialists of varying disciplines who treat patients with PH. We sought to determine the perspectives of treating medical specialists on exercise, exercise-related concerns, and exercise recommendations for people with PH.
Methods
Study design and participants
This was a cross-sectional, multinational voluntary survey of medical specialists from a range of disciplines who treated patients with PH or who were experts in rehabilitation.
Survey design
An English language survey was developed by the research team in accordance with the Checklist for Reporting Results of Internet training E-surveys (CHERRIES). 35 The survey was anonymous and comprised 20 items assessing demographic data (age, gender, specialist type, years since specialist qualification, country and postcode of practice); in addition to detailed descriptive data on exercise beliefs, practices and attitudes. Survey questions evaluated the personal exercise behaviour of respondents; their exercise recommendations/prescriptions given to patients with PH, based on patients’ World Health Organization (WHO) functional class; attitudes on the perceived importance and safety of exercise for patients with PH; as well as perceived barriers and enablers of exercise in patients with PH, from a physician’s perspective. Exercise was defined as exertion at, or above, the level of a brisk walk.
Most questions required answers that were dichotomous or categorical. There was also the option to provide comments and/or free text responses to some open-ended questions.
The survey was piloted with a focus group of physicians (cardiologist, rheumatologist and rehabilitation physicians (n = 5), and refined according to their feedback. The survey was available in either paper-based or electronic format, via the secure, web-based electronic data capture system, REDcap (Research Electronic Data Capture).36,37 Participants who completed the survey online provided electronic consent via a ‘yes/no’ question, while those who completed the paper-based form were advised that survey completion indicated consent to participate. No incentives were given to participate.
Ethical approval was obtained from the Human Research Ethics Committee of St Vincent’s Hospital, Sydney, Australia (2018/ETH00430).
Survey dissemination and data collection
Advertisement of the study and survey link was conducted online via social media platforms (Twitter™, LinkedIn™, Facebook™) and the St Vincent’s Hospital, Sydney, Australia website. The study was also advertised via the following stakeholders: the Pulmonary Vascular Research Institute (PVRI; United Kingdom); Australasian Faculty of Rehabilitation Medicine (AFRM); American Academy of Physiatrists (AAPMR); International Society of Physical Medicine and Rehabilitation (ISPMR); Pulmonary Hypertension Association of Australia and New Zealand (PHSANZ); Australian Rheumatology Association (ARA); Cardiac Society of Australia and New Zealand (CSANZ); Australian NZ Thoracic Society; European Society of Cardiology (ESC); European Respiratory Society (ERS); American College of Cardiology; American Thoracic Society; Pulmonary Hypertension Clinicians and Researchers (USA); and the American College of Rheumatology. These organisations were invited to review study documentation and to disseminate study information and the survey link to members. The decision whether or not to disseminate study information was voluntary and at the discretion of each organisation.
Physicians attending the following Annual Society Scientific Meetings were also invited to complete the survey: the PHSANZ (Melbourne, Australia, October 2018); the Indian Society of Physical Medicine and Rehabilitation (Vellore, India, October 2018); the Asia-Oceanian Conference of Physical Medicine and Rehabilitation (Auckland, New Zealand, November 2018); and the International Society of Physical Medicine and Rehabilitation (Kobe, Japan, June 2019). The members of the research team (K. S. W. C. and S. G. F.) were present at each meeting to facilitate study enrolment.
Survey responses were collected over a 12-month period (October 1, 2018 to October 1, 2019). Data management was via the REDcap electronic data capture system,36,37 hosted at St Vincent’s Hospital, Sydney, Australia.
Statistical analysis
Data were extracted and analysed via simple descriptive statistics using IBM SPSS v23. Participants who provided valid responses to any part of the survey were included in the analysis. However, respondents who did not indicate their specialist discipline were excluded from analysis.
Results
Demographic data
Participant demographics.
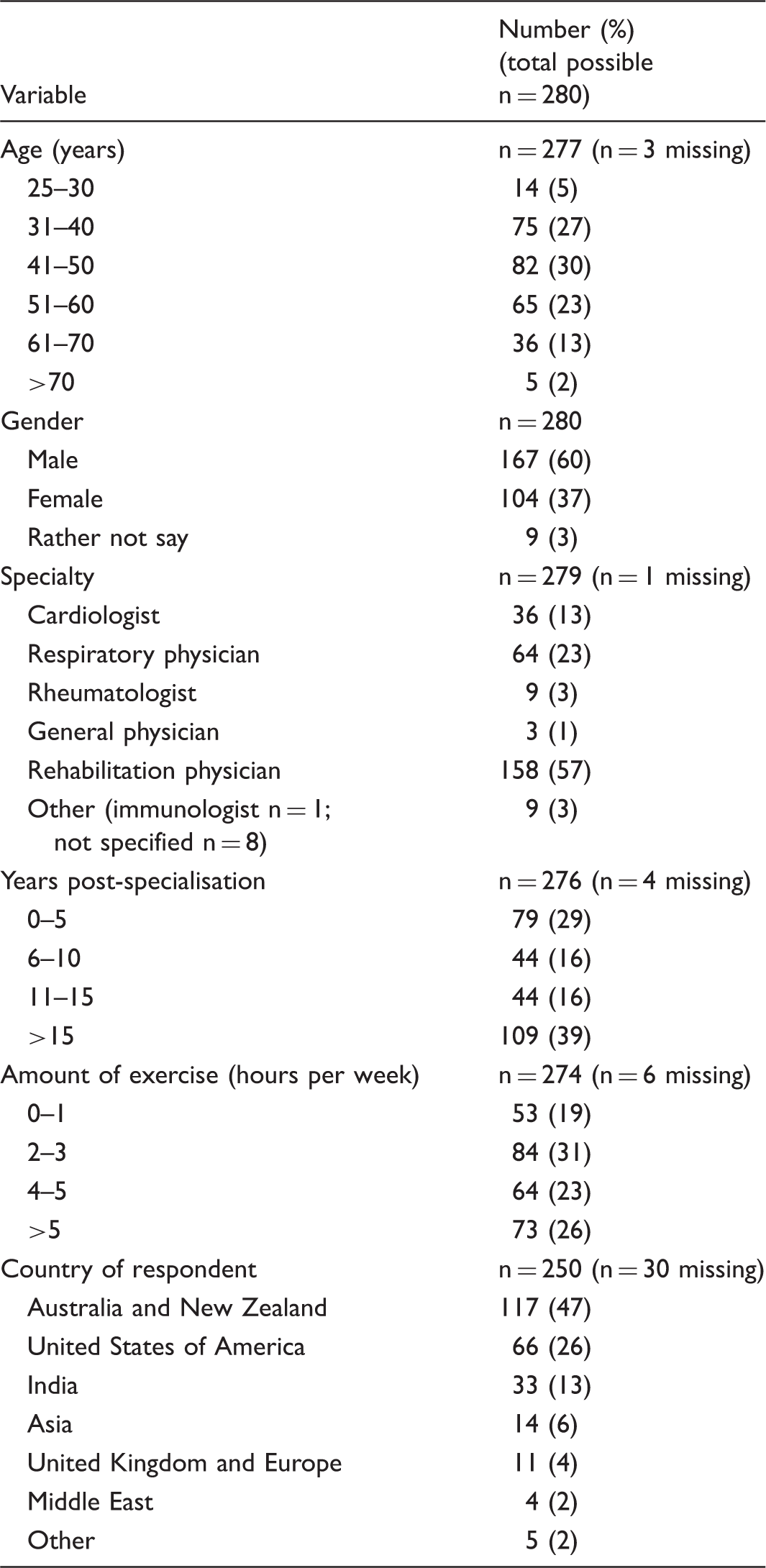
Participants from 22 different countries were represented, with the majority from Australia (109/250, 44%), followed by the United States (66/250, 26%) and India (33/250, 13%). Respondents from Australia were mostly rehabilitation medicine physicians (67/109, 61%), followed by cardiologists (15/109, 14%), respiratory medicine physicians (15/109, 14%) and rheumatologists (8/109, 7%). In contrast, US respondents were predominantly respiratory physicians (43/66, 65%) and cardiologists (19/66, 29%) with only two rehabilitation physicians (2/66, 0.03%). Indian respondents were mostly rehabilitation physicians (32/33, 97%).
Respondents were from six different medical specialties (Table 1). Respondents who recorded ‘other’ for type of specialty, or did not specify what type of specialty (n = 8) only had demographic data analysed; no data were used from this cohort for sub-group analyses. One respondent who noted ‘other’ specialist type and specified their sub-speciality as immunology was included in the acute care specialist cohort.
Rehabilitation physicians comprised over half the cohort (158/280, 56%). Most respondents were male (167/280, 60%), <50 years old (171/280, 61%) and were >10 years post-specialisation (153/280, 55%) (Table 1). According to self-reported exercise levels, approximately 50% of participants exceeded the recommended guidelines for aerobic physical activity (137/274). 38. Among rehabilitation physicians, 75% (n = 116/155) reported personal activity levels of ≥2 hours of exercise per week, with 48% (n = 75/155) reporting ≥4 hours of exercise per week. Acute care specialists reported similarly high levels of personal physical activity, with 88% (n = 97/110) reporting exercise of ≥2 h/week and 52% (n = 57/110) reporting ≥4 h of exercise per week.
Patterns of PH practice
i) Rehabilitation physicians
Of the 158 rehabilitation physicians who responded, 47% (n = 74) were involved in cardiac and/or pulmonary rehabilitation, and 29% (n = 46) were directly involved in managing PH (Fig. 1). Those who were not involved in managing patients with PH were only asked to complete survey sections scoping their demography and personal exercise habits; they were not asked to complete survey questions related to PH exercise recommendations or prescriptions. The number of PH patients seen per specialist for rehabilitation was low; 85% (39/46) of respondents saw <20 PH patients per year, mostly as inpatients (n = 25/44, 57%); followed by outpatients (n = 17/44, 39%), with a few patients seen in private consulting rooms. Only five rehabilitation physicians reported working as part of a PH specialist centre.
Respondents.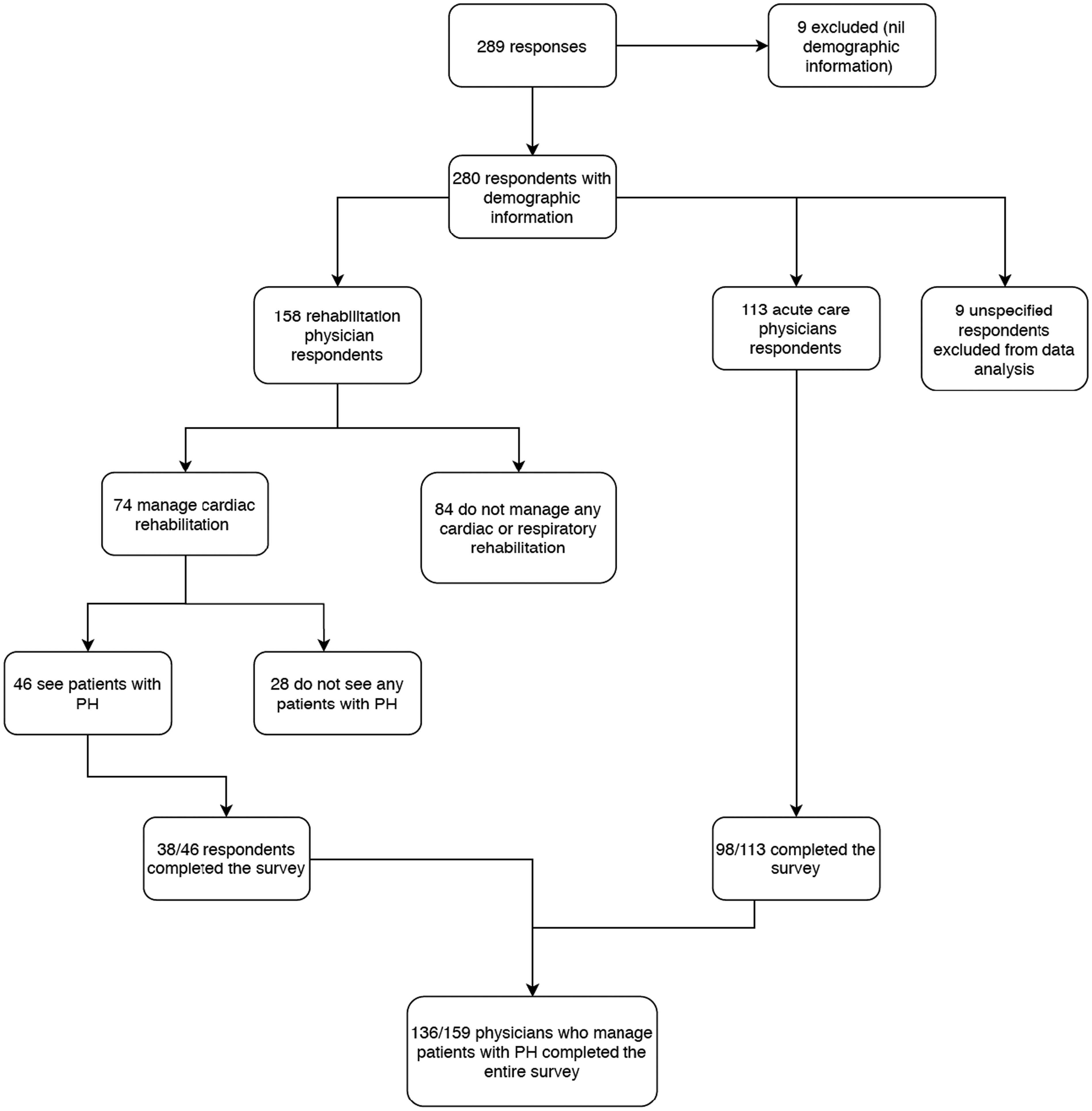
Acute care physicians
Overall, 113 acute care physicians (cardiologists, respiratory physicians, rheumatologists and general medicine physicians and an immunologist) responded to the survey (Fig. 1). Of these, 96% (n = 108/113) were involved in management of PH patients. Seventy percent (n = 72/103) of respondents saw >50 PH patients per year, mostly as outpatients in a PH specialist centre (n = 85/103, 83%). Forty-three percent (n = 49/113) of acute care respondents were directly involved in delivery of cardiopulmonary rehabilitation.
Exercise recommendations and prescription patterns
Rehabilitation physicians
Eighty percent of rehabilitation physicians who managed PH patients (n = 36/45) recommended exercise for these patients, most commonly for its general health benefits, positive impact on physical function and quality-of-life. This was expressed in the following representative statements: ‘because of the enormous benefit to function and wellbeing’; exercise ‘improves functional outcomes… improve(s) general ADL (activities of daily living) function… improves tolerance and fitness’; ‘it is essential’. Specific physiological benefits of exercise for PH were also noted by three respondents: ‘exercise increases cardiac output’; ‘improves exercise tolerance and functional capacity in PH’; and can help ‘to avoid deconditioning and maintain cardiopulmonary capacity’. Only two rehabilitation medicine physicians mentioned evidence as a reason for recommending exercise in PH: ‘clinical practice/evidence’; and ‘evidence of efficacy exists in the literature’, while another stated it was a ‘generic recommendation – because I’m a Rehab Physician’.
Approximately one third of rehabilitation physician respondents (n = 16/45, 36%) identified a preferred setting for exercise training. This was predominantly an inpatient setting (n = 6/16, 38%), with the top three reasons being that it facilitated the most appropriate intensity of exercise training (29% n = 23); ease of access (27%, n = 21); and safety (24%, n = 19).
PH exercise recommendations by acute care physicians (n = 103).
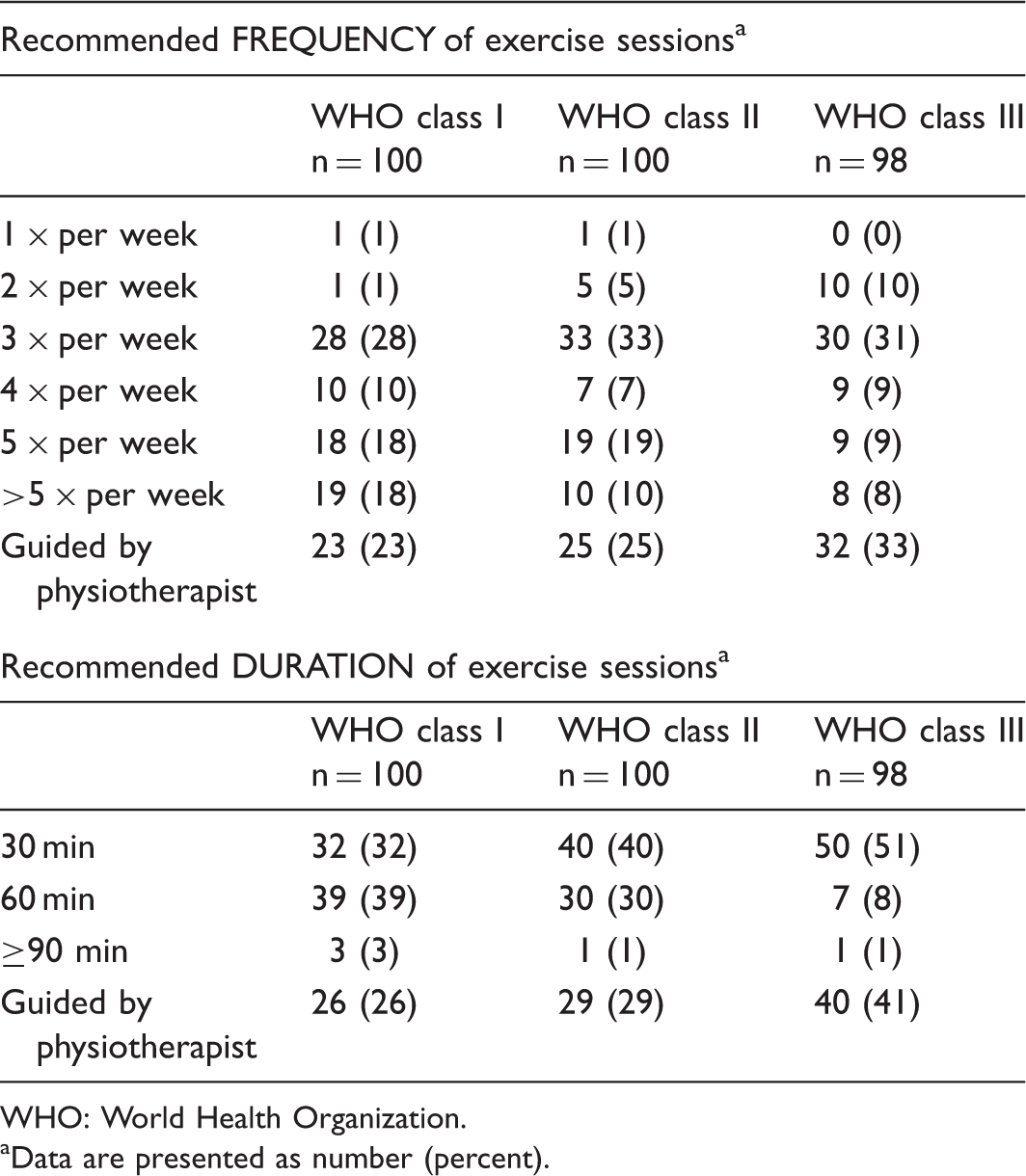
WHO: World Health Organization.
Data are presented as number (percent).
Acute care physicians
Eighty eight percent of acute care physicians (n = 91/103) recommended exercise for patients with PH. The small minority who did not routinely recommend exercise cited reasons such as: ‘patients too sick’; ‘not in protocol previously’, ‘no idea if there are evidence-based prescription guidelines’; and ‘don’t think about it’.
Among those who did recommend exercise, common reasons included general benefits of exercise ‘to optimise health’, ‘prevent deconditioning’ and ‘improve quality of life’. These were similar to reasons noted by rehabilitation physicians: ‘It has (positive) effects on body-mind interaction, general well-being, self-image, and has so many other positive impacts’; exercise ‘improves endurance, improves (patient’s) sense of independence, and self-satisfaction’. ‘exercise improves physical conditioning, maintains functional capacity, helps reduce co-morbid risks (e.g. hypertension, obesity, etc.)’, ‘Reduces falls risk. And helps with depression, anxiety and quality of life’.
Acute care physicians cited published evidence of benefit as a major driver of exercise prescription in PH. Respondents noted that exercise was the ‘most beneficial intervention known’, with ‘well established clinical benefits’ and ‘Level 1 evidence (to) support benefit’. Respondents recognised exercise as ‘evidence-based’ and ‘recommended by guidelines’ for PH, with two respondents citing the landmark German study of Mereles et al. 39 Respondents also noted that the magnitude of exercise benefit compared favourably to that achieved with PH-specific pharmacotherapies: ‘trials and research have shown that exercise improves 6 minute walk test to a magnitude greater than the best PAH drugs we have available’, ‘it is better than a drug in efficacy’, ‘it is as effective as many medications for maintaining functional status and capacity’. Because of the efficacy of exercise training, some respondents noted it was an integral part of PH management: exercise is an ‘essential part of my treatment plan’, ‘I’m convinced it’s an essential part of therapeutic regimen’, and [I recommend it] to ‘all my patients’.
The most common exercise setting prescribed by acute care physicians was outpatient pulmonary rehabilitation (n = 41/81, 51%), followed by a home exercise programme (n = 13/81, 16%) and outpatient cardiac rehabilitation (n13/81, 16%). The most common reasons for choosing these settings were safety (n = 54/81, 67%); provision of the appropriate exercise intensity (n = 49/81, 60%) and ease of access (n = 48/81, 59%). The importance of providing a ‘medically safe environment’ and having required facilities available such as ‘access to supplemental oxygen’ were noted.
Perceived barriers to exercise.
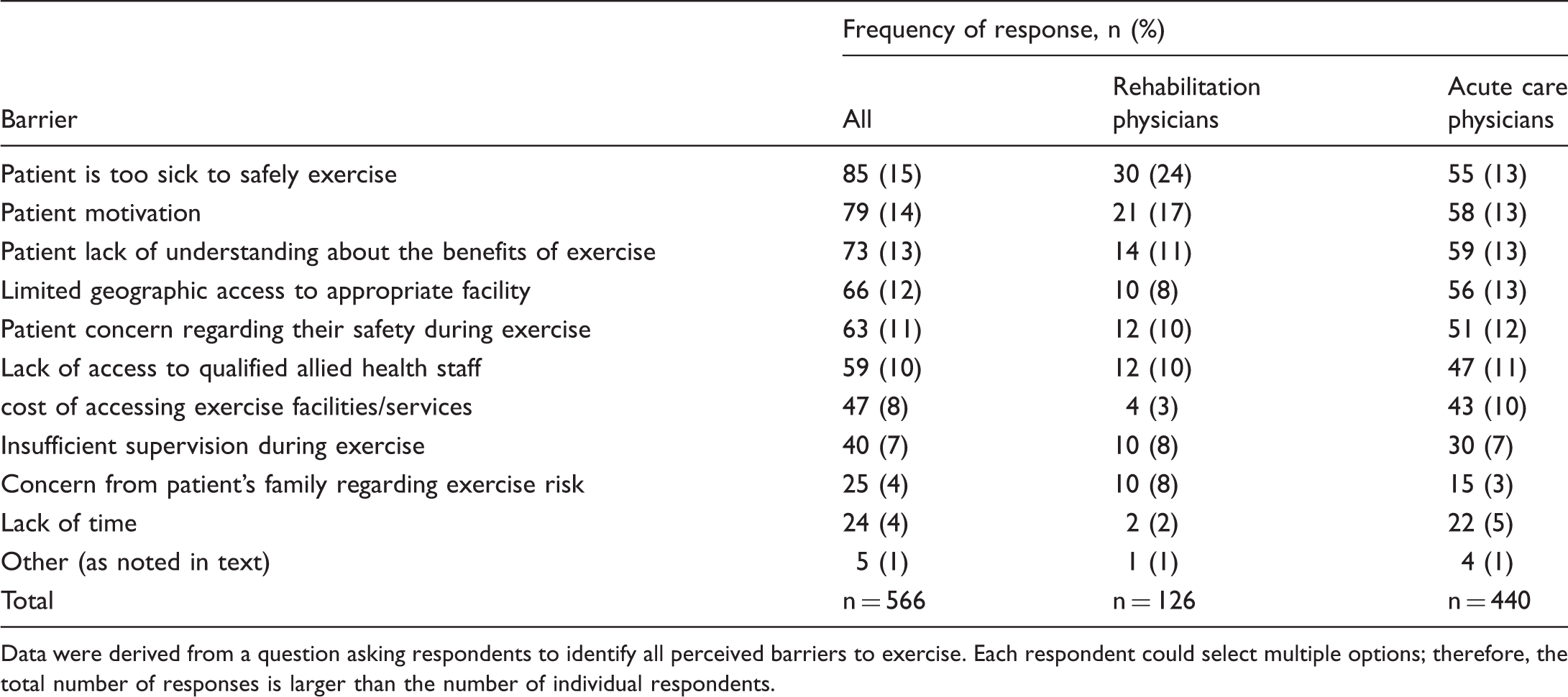
Data were derived from a question asking respondents to identify all perceived barriers to exercise. Each respondent could select multiple options; therefore, the total number of responses is larger than the number of individual respondents.
Perceived barriers to exercise
Rehabilitation medicine physicians
The most significant barrier to exercise identified by rehabilitation physicians was that patients were too sick to exercise (n = 16/31, 52%), followed by patient concerns regarding safety during exercise (n = 6/31, 19%), and poor patient motivation (n = 5/31, 16%).
Acute care physicians
According to acute care physicians, the most important barrier to exercise for patients with PH was poor patient motivation (n = 17/91, 19%), patients being too sick to exercise (n = 17/91, 19%) and limited geographic access to an appropriate facility (n = 15/93, 16%). When asked to identify all factors that limited exercise in patients with PH, there were a total of 440 responses (Table 4), with lack of understanding of the benefits of exercise (n = 59), patient motivation (n = 58) and limited geographic access (n = 56) most frequently chosen.
Other barriers to exercise noted in free text responses included ‘debilitating fatigue, which may be related to skeletal muscle metabolic dysfunction’; [exercise] is ‘not recommended/reinforced’; ‘[connective tissue disease] patients have physical morbidities that can impact’; ‘fear/anxiety regarding breathlessness’; and patients being ‘too breathless’.
Perceived enablers of exercise
These were thematically identified from free-text responses. As the same themes were identified from acute and rehabilitation physicians (thematic saturation), these results were pooled.
Access
The availability of transport services and subsidised financial cost were identified as important enablers of exercise participation. Access to ‘supervised, activity-based exercise classes’, ideally in an experienced cardiac rehabilitation centre and/or a PH-dedicated service was noted by many respondents as a key enabler. Long-term availability and follow-up were deemed important: ‘accessibility to a facility for initial instruction and monitoring, ideally followed by less monitored but structured exercise routine in a staffed local gym setting’, and ‘availability of long-term exercise program after the acute program is over’. Telehealth was also suggested ‘to provide close observation, e.g., through telehealth program in order to follow their home exercise program’. One respondent suggested a ‘telemedicine link with a “hub” centre’ for ongoing supervision.
Funding issues were mentioned frequently, with ‘better and affordable access to qualified allied health staff’, having ‘private health insurance or independent willingness to pay own money’ or ‘good financial resources’.
Experience of treating clinicians
The experience and attitudes of treating clinicians were identified as important exercise enablers – ‘the attitude of the physician/team caring for them’, ‘encouragement from doctor’, ‘physician guided reassurance’ and ‘continuous positive feedback’. Respondents noted that supportive, collaborative team environments where experienced clinicians encouraged exercise and tailored programs to individual needs were most conducive to exercise: ‘sympathetic therapists who are willing to vary the intensity of exercise based on patients’ anxiety levels’, and ‘more qualified therapists’ were noted enablers.
Education
Patient education regarding the benefits and limitations of exercise was important – ‘appropriate discussion with a doctor and/or nurse regarding potential benefits for PH and general fitness optimization; and approach/limitations/expectations to exercise’, ‘time spent emphasising safety and benefits’. Education with ‘formalized, evidence-based home programs that can be given as a guidebook’.
Other exercise enablers included family support, patient premorbid interest in exercise, patient motivation and ‘starting early in their diagnosis and maintaining at proper intensity and duration as their disease course shifts’.
Discussion
This is the first study to explore physicians’ attitudes towards exercise and exercise prescription patterns for patients with PH. We canvassed a broad spectrum of physician sub-specialities involved in the management of patients with PH, ranging from acute care physicians (cardiologists, respiratory physicians, rheumatologists and general physicians) to sub-acute rehabilitation physicians. In line with recent clinical guidelines, 40 most respondents recommended and prescribed exercise for patients with PH, due to the general health benefits of exercise, as well as the growing evidence base supporting exercise in this population. However, there was variability in the exercise recommendations made by specialist groups, including the optimal setting, frequency and duration of exercise. The recommended setting reflected physicians’ practice, with most rehabilitation medicine physicians recommending inpatient rehabilitation and most acute care physicians recommending outpatient therapy. A large number of respondents noted they would be guided by a physiotherapist with regard to exercise frequency and duration.
Exercise patterns
Self-reported exercise levels among physician respondents were generally high, with 50% (n = 137/274) exceeding recommended guidelines for aerobic activity. It was therefore not surprising that most physicians noted exercise was ‘very important’ and prescribed exercise for patients with PH. However, there were differences in the reasons given according to speciality; with rehabilitation physicians citing more general benefits of exercise for overall function, well-being and activities of daily living, in contrast to acute care physicians who noted evidence of specific benefits for the PH population. Rehabilitation physicians also tended to recommend inpatient rehabilitation, likely due to them seeing patients with PH as a comorbidity, rather than being referred for rehabilitation solely for PH. Rehabilitation physicians cited appropriate intensity, ease of access and safety as the main reasons for recommending an inpatient setting. Interestingly, most published exercise training programs have utilised an intensive inpatient protocol,15,39,41–48 such that rehabilitation physicians are in line with the current evidence base. However, inpatient rehabilitation is expensive and may not be widely available. It is also has more limited long-term utility than outpatient models due to cost.
Acute care physicians noted evidence of PH-specific benefits as the main drivers for exercise prescription, including increased walking distance and endurance, comparable efficacy of exercise to common PH drug treatments for improving quality-of-life, and increased right ventricular function. The predominant exercise setting recommended by acute physicians was outpatient pulmonary rehabilitation, perhaps reflecting the larger number of pulmonary medicine physician respondents. While most exercise training trials have been conducted in the inpatient setting, a number of small outpatient studies10–14,49 have also shown improvements in 6-min walk distance and quality-of-life. We postulate that acute care physicians were more comfortable recommending outpatient exercise programs due to this being the predominant setting in which they frequently see PH patients, greater experience with PH patients (reflected in the larger patient numbers seen per year) and their frequent association with a PH specialist centre. They may also recommend the outpatient setting due to practical reasons such as cost to the patient and lack of access to inpatient beds for rehabilitation.
Guidance by physiotherapist
The proportion of both rehabilitation medicine and acute care physician respondents who indicated they would be guided by a physiotherapist with regard to duration and frequency of exercise in WHO class III PH patients was similar at nearly 40%. Reasons for this were not explored, but may be due to physicians deferring exercise prescription to the treating therapist who is able to tailor a program to patient, or due to a lack of experience in prescribing exercise to this patient group, who are often symptomatic and have functional exercise limitations.
However, knowledge and confidence among physiotherapists in dealing with PH patients may also be limited. 50 While not explored in the present study, a previous study of 63 physiotherapists working with PH patients found that nearly 2/3 of physiotherapists self-rated their confidence in managing patients with PH ≤ 6/10 (where 10 was maximal confidence), demonstrating a notable gap in confidence among physiotherapists treating this patient population. 50 However, there remained high motivation to translate current exercise training evidence into outpatient service provision. 50
Detailed clinical guidelines on exercise prescription would be a helpful support to both physiotherapists and medical specialists recommending exercise. 50 General guidelines on how to adapt pulmonary rehabilitation to chronic pulmonary conditions have been published. 51 Detailed clinical practice suggestions for rehabilitation in PH patients have also recently been published 8 ; however, these were not formal guidelines. No formal guidelines currently exist, as the optimal duration, frequency and format for exercise in PH remains unclear. 40
Barriers to exercise
Both patient-related and systemic factors were identified by physicians as barriers to exercise, with the most commonly cited barriers being patient-related: patient ill health, poor patient motivation and lack of patient understanding regarding exercise benefits. Limited service availability, especially limited geographic access to exercise facilities and a low availability of qualified allied health staff, was the most common external barrier identified.
A recent study looked at barriers to exercise in patients with PH from a physiotherapist perspective. 50 Barriers noted were patient and carers’ anxiety, and patient uncertainty regarding exercise limitations. 50 This contrasts with physician respondents, who noted major barriers to exercise were patient ill health and poor patient motivation. In our study, family member/carer concern was not reported to be a major barrier, from the physician perspective.
A recent study of patient-identified barriers to exercise in 40 patients with PH and CTEPH concurred that patient internal factors played an important role, especially lack of self-discipline, poor energy and low self-interest. 33 These factors correlated significantly with reduced physical activity levels as measured by step counts. 33
External barriers such as limited geographic availability and access to qualified healthcare professionals were also noted by physicians to pose significant challenges. Our survey responses reflect what is reported in the literature that access to pulmonary rehabilitation due to financial constraints is generally poor, particularly in low to middle-income countries (defined as gross national income of <3995 USD per capita).52,53 In higher income countries, the format of pulmonary rehabilitation varies, based on differences in resource allocation and national healthcare policy. 54 In Europe, pulmonary rehabilitation tends to be inpatient-based, compared to outpatient rehabilitation in the United States and Australia. 54 Regardless of the setting, access to pulmonary rehabilitation is sub-optimal and increasing access to pulmonary rehabilitation is a key message from the American Thoracic Society and European Respiratory Society joint policy statement. 54 Similarly, global access to cardiac rehabilitation is poor, with cardiac rehabilitation only available in approximately half of the countries, globally. 55 Methods of funding included public, private and hybrid funding, all varying by country, with financial constraints the greatest barrier to cardiac rehabilitation, globally. 55 Lack of funding for PH programs, particularly in the outpatient setting, was noted in the present study and by Keen et al. 50 This reflects the current funding climate in Australia and overseas, 40 where a large proportion of health resources are directed towards the acute care (inpatient) setting.
Enablers
Identified enablers of exercise were similar among rehabilitation and acute care physicians and included easy geographical access to services, affordable cost and availability of qualified allied health staff, similar to what is reported in the literature. 54 Encouragement from all members of the multi-disciplinary clinical team was important. Prior research suggests that support must also come from peers, family and the patient’s social network. 56 A supervised, group exercise setting was reported to be important. This may reflect a desire for an empathic environment with peer support or positive role-modelling by others with the same condition. 34 The ultimate goal of any formal rehabilitation program is to progress patients beyond dependence on an external program, to an intrinsic motivation to continue self-directed exercise and integration into everyday life. 34 This may occur when patients move onto maintenance classes or form their own peer exercise groups, for example, a social walking group. 34 This is more likely to occur when enablers of exercise are present at multiple levels; including adequate resources and funding. 32
Telehealth
A number of respondents mentioned telehealth as a potential enabler to allow remote supervision of exercises classes – thereby overcoming access barriers. To our knowledge, there are no published trials examining the effectiveness of a telehealth exercise intervention in the PH population. However, a small number of trials have shown potential benefit in patients with chronic obstructive pulmonary disease.57,58
Methodological considerations
As this was a voluntary survey by a self-selected convenience cohort, selection and recall/response bias may limit the generalisability of results. In particular, response rates from the four conferences as a proportion of total registrants was low (189/3146, 6%), suggesting that it was mainly physicians with an active interest in PH who responded. Respondents might therefore have been more favourably disposed towards exercise as a therapeutic intervention. In addition, survey items were not compulsory, resulting in some missing data. However, a major strength of our study is that it canvassed a wide cross-section of clinical specialists, including those from across five different medical specialities and from 22 different countries.
Future directions
While this study focused on physicians’ attitudes to exercise and their perception of barriers and enablers, we note the importance of patients’ attitudes towards exercise and the unique barriers and enablers they may perceive. To this end, we are currently undertaking a similar international survey to address this gap in the literature and supplement the current findings with patient perspectives.
Conclusion
PH exercise recommendations by rehabilitation medicine physicians (n = 41).
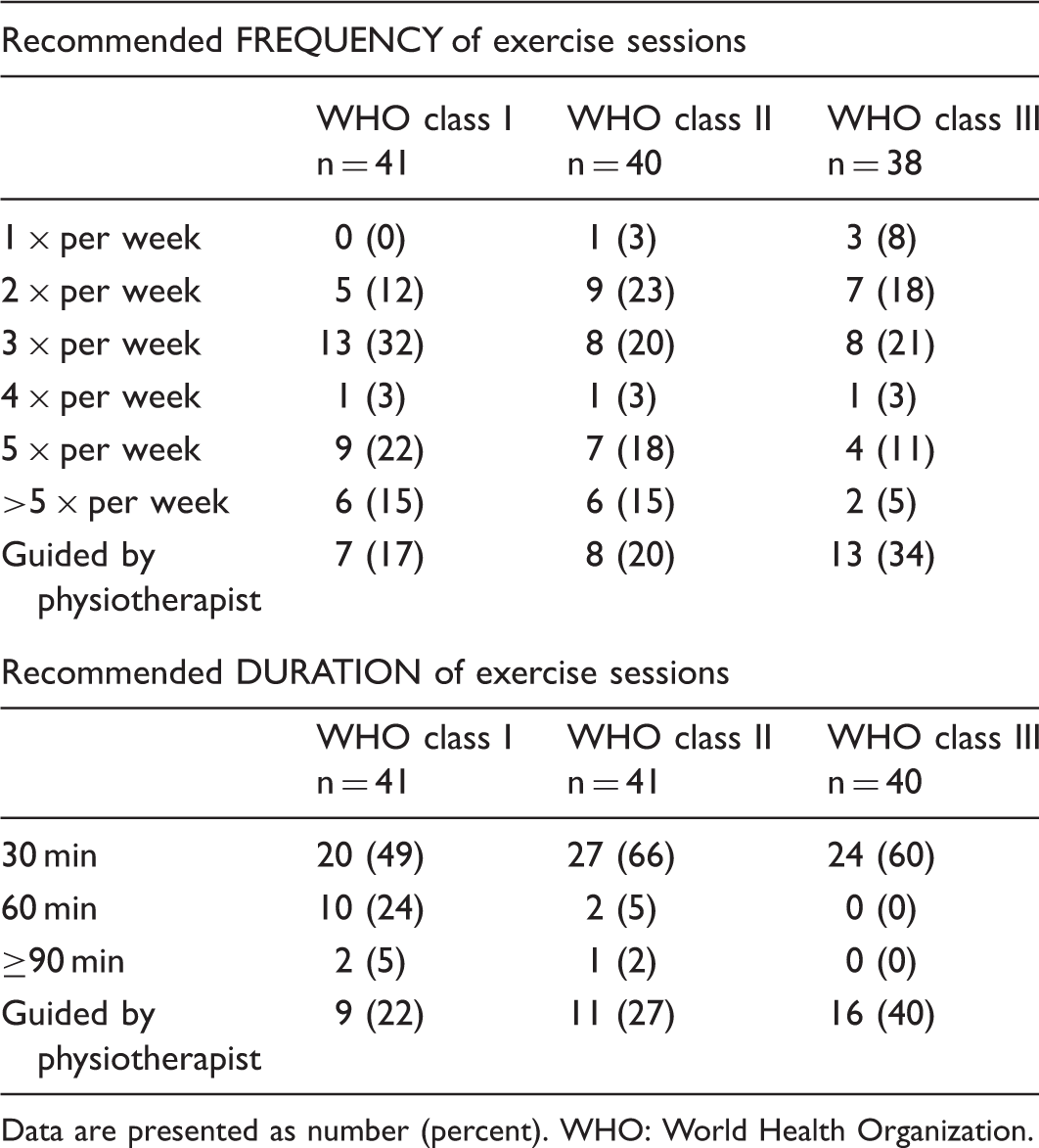
Data are presented as number (percent). WHO: World Health Organization.
Footnotes
Acknowledgements
The authors gratefully acknowledge Karen Brown (Pulmonary Hypertension Nurse, St Vincent’s Hospital Sydney) for her support of the study and assistance with data collection.
Contributorship
Study conception and design: K. S. W. C. and C. T. S. Funding acquisition: K. S. W. C. and C. T. S. Project administration: K. S. W. C. and C. T. S. Data acquisition/survey dissemination: K. S. W. C., P. K. K. W., S. G., S. G. F., E. K. and C. T. S. Data analyses: K. S. W. C., C. T. S. and P. K. K. W. Interpretation of results: K. S. W. C. and C. T. S. Drafting of manuscript: K. S. W. C. Critical revision and approval of final manuscript: all authors.
Conflict of interest
The author(s) declare that there is no conflict of interest.
Ethical approval
This project was approved by St Vincent’s Hospital Sydney HREC, approval number 2018/ETH00430.
Funding
K. S. W. C. was supported by the RACP Research Entry Scholarship.
Guarantor
K. S. W. C. guarantees the originality and veracity of this manuscript.
