Abstract
Coronavirus disease (COVID-19) is associated with pulmonary hypertension due to pulmonary embolism, which affects subsequent outcomes. However, definitive diagnosis of pulmonary hypertension is difficult because of the risk of spreading the infection. Here, we assess the utility of plane computed tomography in noninvasively predicting the clinical severity of COVID-19.
To the Editor
The coronavirus disease (COVID-19) pandemic continues to spread worldwide. In severe cases, cytokine storm causes microvascular failure and a hypercoagulable state, resulting in deep vein thrombosis and pulmonary embolism with pulmonary hypertension (PH). 1 , 2 Pulmonary artery (PA) dilatation in relation to the ascending aorta (Ao) (PA/Ao ratio) calculated from computed tomography (CT) scans has been reported to be associated with the clinical severity of chronic lung disease and idiopathic PH. 3 , 4 In this study, we aimed to determine whether the PA/Ao ratio on a plain CT scan is predictive of the clinical severity of COVID-19.
Methods
Between 1 January 2020 and 31 May 2020, 130 patients diagnosed with COVID-19 in our hospital were retrospectively enrolled; 103 of these patients underwent a plain chest CT on admission. The PA diameter was measured at the level of the PA bifurcation, and the Ao diameter was averaged from two perpendicular measurements taken from the same CT image as previously reported. 5 The main outcome was a combined endpoint consisting of oxygen inhalation ≥4 L/min, intubation, or death. Continuous measures were compared using a Wilcoxon matched-pairs signed rank test or t test if the paired data were normally distributed. Two-sided p < 0.05 defined statistical significance. All statistical analyses were performed with SPSS statistical software, version 24. The study was approved by the local Ethics Committee (NCGM-G-003472-03); written informed consent was obtained from all patients.
Results
The mean (±standard deviation) age among 103 COVID-19 patients was 53 ± 18 years; the proportion of men was 68%. Twenty (19%) of the 103 COVID-19 patients had severe respiratory exacerbation. Significant differences were observed in PA diameter (31.1 ± 2.7 mm vs. 25.4 ± 3.5 mm, p < 0.001) and PA/Ao ratio (0.97 ± 0.11 vs. 0.82 ± 0.10, p < 0.001) between groups with and without severe respiratory exacerbation, respectively. This PA/Ao ratio difference was also significant in 74 patients aged ≤65 years (1.03 ± 0.1 vs. 0.84 ± 0.09, p < 0.001). The group with a PA/Ao ratio of >0.9 had more severe respiratory exacerbation (p < 0.001) than the group with a PA/Ao ratio of ≤0.9 of the median cutoff point. Kaplan–Meier curves stratified by PA/Ao ratio demonstrated a significant separation for severe respiratory exacerbation and mortality during the hospitalization period. Patients with a PA/Ao ratio of >0.9 had a higher rate of event in the log-rank test from admission (p < 0.001; Fig. 1).
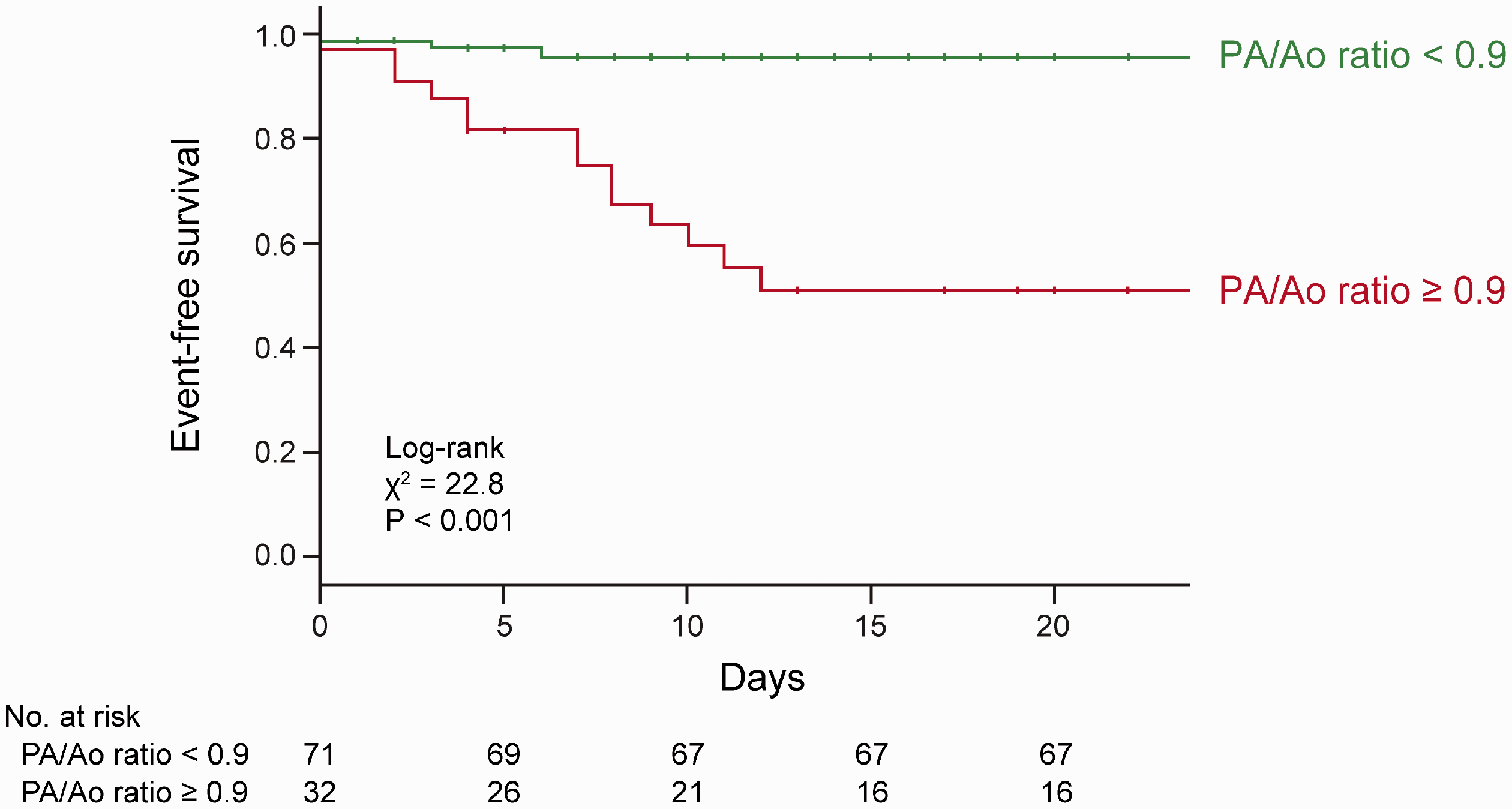
Kaplan–Meier curves for severe respiratory exacerbation and mortality during the hospitalization period. Patients with a PA/Ao ratio >0.9 had a higher event rate in the log-rank test.
Discussion
Our results showed that high PA/Ao ratio (>0.9) is a predictive marker for severe respiratory failure. In previous studies on PH, a PA/Ao ratio reflecting the mean PA pressure ranging between >0.9 and 1.0 was associated with a poor prognosis and was considered a more useful marker than the tricuspid regurgitation peak gradient measured by echocardiography. 3 Some studies have showed that one of the causes of severe cases of COVID-19 is pulmonary embolism, including microembolism. 6 The World Health Organization interim guidance statement 7 states that for patients with COVID-19 administration of prophylactic low-molecular-weight heparin once a day or subcutaneous unfractionated heparin twice a day is recommended; however, the use of anticoagulants for all COVID-19 patients still remains controversial. Although it might be difficult to perform contrast-enhanced CT, echocardiography, and Swan-Ganz catheterization in COVID-19 patients in a clinical setting, plain CT is used to diagnose COVID-19 pneumonia in many patients. It is easy to calculate the PA/Ao ratio, as a surrogate marker of PH, from plain CT scans for evaluating the clinical severity of COVID-19. In fact, a 36-year-old man without obvious past illness had mild pneumonia (Supplementary Fig. S1b) and PA/Ao ratio was 1.2 (Supplementary Fig. S1a) on the admission, but his respiratory condition severely worsened with extra-corporeal membrane oxygenation on hospital day 30 (Supplementary Fig. S1c). The limitations of our study were the small number of patients, univariate analysis, and the lack of direct evidence of PH and pulmonary embolism by a contrast CT, Swan-Ganz catheterization, or echocardiography. Despite these limitations, our study showed that a PA/Ao ratio >0.9 on plain CT scans might be predictive of the clinical severity of COVID-19. This method is non-invasive and will be useful in resource-limited settings.
Supplemental Material
sj-pdf-1-pul-10.1177_2045894020969492 - Supplemental material for Association of plain computed tomography-determined pulmonary artery-to-aorta ratio with clinical severity of coronavirus disease 2019
Supplemental material, sj-pdf-1-pul-10.1177_2045894020969492 for Association of plain computed tomography-determined pulmonary artery-to-aorta ratio with clinical severity of coronavirus disease 2019 by Hiromasa Hayama, Masahiro Ishikane, Rubuna Sato, Kohei Kanda, Noriko Kinoshita, Shinyu Izumi, Norio Ohmagari, Yukio Hiroi and NCGM COVID-19 clinical team in Pulmonary Circulation
Footnotes
Acknowledgments
We thank all the clinical staff at our hospital for their dedication to clinical practice and patient care. This work was supported in part by the National Center for Global Health and Medicine Clinical Research (NCGM-CR) grant (20A-3002).
Conflict of interest
The author(s) declare that there is no conflict of interest.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Own funding of National Center for Global Health and Medicine, Japan.
Ethical approval
The study was approved by the local Ethics Committee (NCGM-G-003472-03); written informed consent was obtained from all patients.
Authors’ contributions
HH designed and performed experiments, analysed data, and co-wrote the paper. RS, KK, NK, SI, NO: performed experiments. MI, YH: designed experiments and co-wrote the article.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
