Abstract
A 49-year-old man with CTEPH (pre-procedural mean pulmonary artery pressure: 36 mmHg) underwent balloon pulmonary angioplasty. Chronic total occlusion of the left inferior pulmonary artery trunk was observed. To evaluate the collateral vessels of the chronic total occlusion, 4D-CTA was performed. The examination was performed using a 256-row detector CT system using the test bolus tracking method. 4D-CTA showed the bronchial artery-to-left inferior pulmonary artery collateral supply, which was confirmed by a selective bronchial artery angiography. The patient’s symptoms improved with balloon pulmonary angioplasty of the other stenotic lesions. 4D-CTA can noninvasively evaluate the anatomy and hemodynamics of multiple systemic collaterals simultaneously. This technique can support interventions in systemic artery-to-pulmonary artery collaterals, such as embolization, and could be helpful in challenging balloon pulmonary angioplasty interventions for chronic total occlusion to identify vessel structures distal to the chronic total occlusion and collateral channels for a retrograde approach.
Keywords
Case description
A 49-year-old man with chronic thromboembolic pulmonary hypertension (CTEPH) (pre-procedural mean pulmonary artery pressure: 36 mmHg) underwent balloon pulmonary angioplasty (BPA). Chronic total occlusion (CTO) of the left inferior pulmonary artery trunk was observed (Fig. 1a). To evaluate the collateral vessels of the CTO, time-resolved 4D CT angiography (4D-CTA) was performed. The examination was performed using a 256-row detector CT system (Revolution CT; GE Healthcare, Milwaukee, WI, USA) using the test bolus tracking method.
1
First, the test bolus was injected for 2 s, followed by a 0.9% saline solution for another 4 s. Then, after waiting for 20 s, the main bolus injection for 18 s was automatically started, followed by the injection of a saline solution for 4 s. The CT operator then manually pressed the acquisition trigger button at the beginning of the enhancement of the right ventricle in the test bolus (the trigger point), visually assessing the monitor images along with the enhancement curve measured in the region of interest (ROI) placed on the right ventricle. After the subsequent scan delay of 23 s from the trigger point, an intermittent image acquisition was automatically started. This image acquisition consisted of an initial 24 intermittent volume scans with a rotation time of 0.28 s and a scan interval of 0.6 s (scan duration: 20.52 s), followed by a secondary 13 intermittent volume scans with a rotation time of 0.28 s and a scan interval of 1.47 s (scan duration: 21.28 s). The CT operator manually stopped the image acquisition when the contrast medium had sufficiently reached the systemic collaterals and the distal pulmonary arteries of the targeted CTO. In this patient, the acquisition was performed until the 31st scan. A 0.9% saline solution and an iodine contrast medium with an iodine concentration of 370 mg/mL were delivered via a 20-gauge catheter inserted into the right antecubital vein with an injection flow rate of 5 mL/s. The acquisition was performed under automatic exposure control (tube current modulation) with a noise index of 30 (for a slice thickness of 5 mm), and the tube current ranged from 10 mA to 200 mA. Other scanning parameters were as follows: peak tube voltage, 100 kVp; rotation speed, 0.28 s; scan coverage, 160 mm; a matrix size of 512 × 512 pixels; and reconstruction section thickness and section interval, 0.625 mm. The CT dose index volume for this examination was 28.84 mGy, and the dose-length product was 461.46 mGy*cm. Consequently, the effective dose estimate was 6.46 mSv, which was determined by the dose-length product measurements and appropriate normalized coefficients for chest CT (0.014 mSv/(mGy*cm)).
2
4D-CTA showed the bronchial artery-to-left inferior pulmonary artery collateral supply, which was confirmed by a selective bronchial artery angiography (Fig. 1b and c; Video 1 in supplementary material). The patient’s symptoms improved with BPA of the other stenotic lesions.
(a) Selective pulmonary angiography. (b) Time-resolved 4D CT angiography. (c) Selective bronchial artery angiography. A selective pulmonary angiography revealed a totally occluded left inferior pulmonary artery trunk (arrow); the distal branches were not visualized. Time-resolved 4D CT angiography showed the collaterals, which developed from the bronchial artery (arrow) to the distal branches of the pulmonary artery in the left lower lobe (arrowhead). This finding was confirmed by a selective bronchial artery angiography.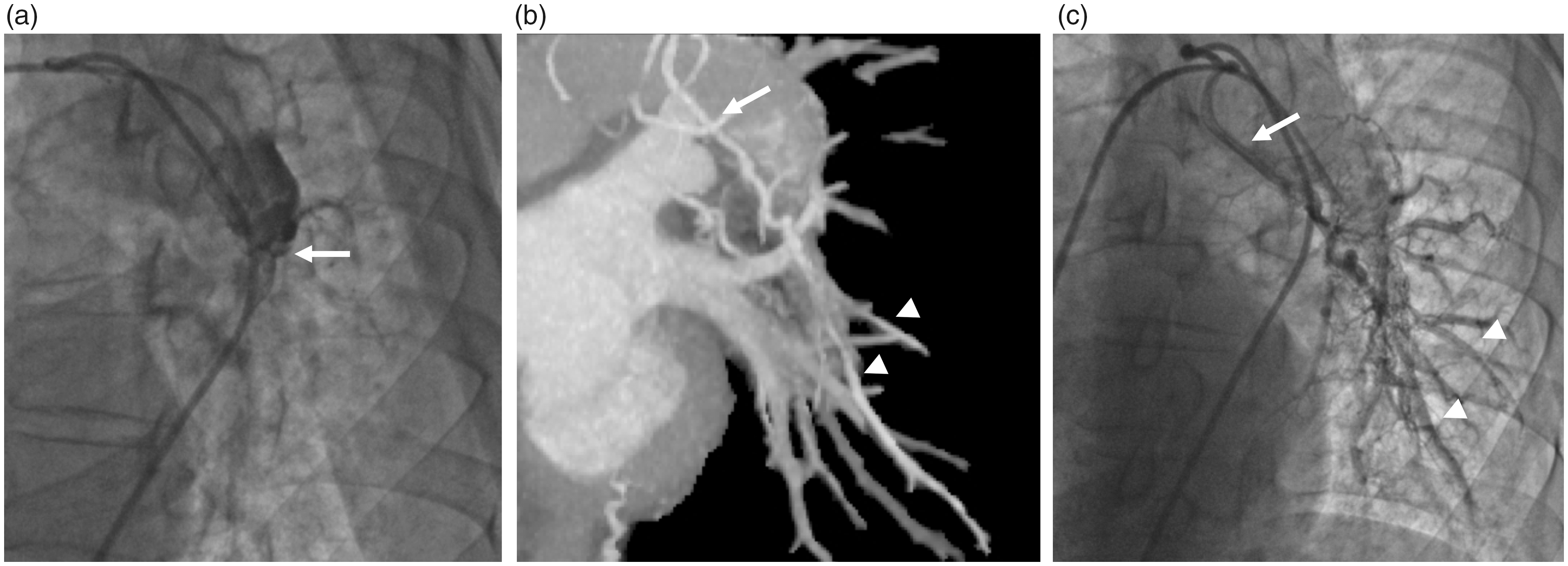
Discussion
In patients with CTEPH, abnormal enlargement of systemic arteries develops due to the development of systemic-to-pulmonary anastomoses, which help to maintain pulmonary blood flow. 3 These systemic collaterals are generally evaluated using conventional single-phase CT angiography (CTA). To the best of our knowledge, this case report is the first successful depiction of the systemic collateral supply to the pulmonary artery using 4D-CTA, which showed a good agreement with a selective angiography. A previous study using conventional single-phase CTA showed the enlargement of both bronchial artery and non-bronchial systemic arteries, such as inferior phrenic artery, intercostal artery, internal mammary artery, and so on, in 56% of the CTEPH patients. 3 However, this report did not confirm the accuracy of the CTA depiction using a conventional angiography. A single-phase CTA provides only a snap shot in time and cannot evaluate the hemodynamics of these enlarged arteries; such images can thus lead to a misunderstanding of the origin or the extent of collateral vessels. In contrast, although a conventional angiography can evaluate the hemodynamics of the collateral vessels, it is an invasive procedure and multiple collaterals cannot be evaluated simultaneously, potentially leading to important collaterals being overlooked. For example, intrapulmonary collaterals, which are observed in some CTEPH patients and through which a successful retrograde approach can reportedly be used to cross the CTO during BPA, 4 cannot be evaluated using systemic arterial angiography. However, 4D-CTA can noninvasively evaluate the anatomy and hemodynamics of multiple systemic collaterals simultaneously. This technique can support interventions in systemic artery-to-pulmonary artery collaterals, such as embolization, 5 and could be helpful in challenging BPA interventions for CTO to identify vessel structures distal to the CTO and collateral channels for a retrograde approach. In addition, 4D-CTA, which covers both the pulmonary arterial phase and systemic arterial phase, has the potential capability of quantifying the systemic arterial perfusion of the lung in CTEPH patients. Nowadays, Lung Perfused Blood Volume using dual-energy CT or Lung Subtraction Iodine Mapping CT using the subtraction technique are being used for evaluating lung perfusion in CTEPH patients.6,7 However, these techniques have the limitation that they cannot completely separate pulmonary and systemic arterial perfusion of the lung, which can lead to overestimation of lung perfusion. 6 Thus, it is now necessary to evaluate lung perfusion by 99mTc-MAA Single Photon Emission Computed Tomography (SPECT) or SPECT/CT, which evaluates pulmonary arterial perfusion alone. On the other hand, 4D-CTA, which enables time-resolved quantitative analysis, is considered to be capable of distinguishing, to some extent, between pulmonary and systemic arterial perfusion by using the method of perfusion CT analysis. 8 At present, in current CT scanners, the scan range of 4D-CTA is limited to 16 cm, however, with the development of more advanced CT scanners, there is a possibility that in the near future, it might become possible to quantify pulmonary and systemic arterial perfusion of the lung by 4D-CTA. Further studies in larger patient populations are required for the validation and evaluation of the clinical utility of 4D-CTA in CTEPH patients.
Footnotes
Conflict of interest
The author(s) declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
