Abstract
Pulmonary hypertension currently has minimal guidelines for outpatient disease management. Congestive heart failure studies, however, have shown effectiveness of disease management plans in reducing all-cause mortality and all-cause and congestive heart failure-related hospital readmissions. Heart failure exacerbation is a common reason for readmission in both pulmonary hypertension and congestive heart failure. Our aim was to review individual studies and comprehensive meta-analyses to identify effective congestive heart failure interventions that can be used to develop similar disease management plans for pulmonary hypertension. A comprehensive literature review from 1993 to 2019 included original articles, systematic reviews, and meta-analyses. We reviewed topics of outpatient congestive heart failure interventions to decrease congestive heart failure mortality and readmission and patient management strategies in congestive heart failure. The most studied interventions included case management, multidisciplinary intervention, structured telephone strategy, and tele-monitoring. Case management showed decreased all-cause mortality at 12 months, all-cause readmission at 12 months, and congestive heart failure readmission at 6 and 12 months. Multidisciplinary intervention resulted in decreased all-cause readmission and congestive heart failure readmission. There was some discrepancy on effectiveness of tele-monitoring programs in individual studies; however, meta-analyses suggest tele-monitoring provided reduced all-cause mortality and risk of congestive heart failure hospitalization. Structured telephone strategy had similar results to tele-monitoring including decreased risk of congestive heart failure hospitalization, without effect on mortality. Extrapolating from congestive heart failure data, it seems strategies to improve the health of pulmonary hypertension patients and development of comprehensive care programs should include structured telephone strategy and/or tele-monitoring, case management strategies, and multidisciplinary interventions.
Keywords
Pulmonary hypertension (PH) is a progressive group of diseases that remains difficult to treat and carries significant morbidity and mortality despite available medical therapy. Currently, there are minimal guidelines on chronic outpatient management and prevention of hospitalization owing to the low number of patients and orphan status of the disease. In contrast, numerous studies and reviews in congestive heart failure (CHF) including the Cochrane review have shown effectiveness of disease management plans in reducing key endpoints including all-cause mortality, heat failure admissions, and all-cause and CHF-related hospital readmissions. A key similarity between PH and CHF is heart failure exacerbations which is a significant and common reason for readmission. Due to physiologic similarities, fluid management and patient compliance challenges, and the chronic nature of these two diseases, we believe applying similar disease management strategies in PH could be of patient benefit.
Methods
A comprehensive literature review was conducted utilizing original articles, meta-analyses, and systematic reviews from 1993 to 2019. We examined the interventions identified in the Cochrane review1–3 and limited our analysis to larger studies with these methodologies. Articles reviewed specifically included these outpatient CHF interventions and their effect on one or more of the following: all-cause admission or readmission, CHF admission or readmission, and all-cause or CHF mortality. Primary endpoints of our review were all-cause mortality, CHF hospitalization and readmission, and all-cause hospitalization and readmission. We included in our data analysis statistically significant studies that also provided a description of intervention(s) used, documentation of outcomes, and study population size greater than or equal to 150 persons. Articles were excluded if a specific diagnosis of CHF was not listed and if primary endpoints of interest did not reach statistical significance or were not reported.
Data collection
Literature search was performed using the following keywords: heart failure, readmission, admission, tele-monitoring, telecommunication, telemedicine, structured telephone support, structured telephone system, case management, and multidisciplinary. Referenced studies were searched as well. Review of individual articles and meta-analyses focused on study power, intervention, and primary and secondary outcomes.
Results
A total of 76 original trials, meta-analysis, and reviews were identified. Of these, 17 met our inclusion criteria, comprising 7681 patients. Each of the 17 studies showed statistically significant results favoring intervention for at least one primary endpoint. There were no statistically significant studies during our review that favored usual care over specified interventions.
We were able to identify four primary categories of interventions consistent with those in the Cochrane review. Case management (CM), which was specialist nurse driven, included education pre/postdischarge, specialist nurse home visits, scheduled telephone calls for symptom management, and teaching for when to seek help.4–7 Multidisciplinary intervention (MI), which was also specialist nurse driven, was comprised of coordinated interventions and communications including patient–caregiver education regarding their disease, medication and diet, nurse clinic visits, regular telephone calls, individualized follow-up plan, and access to physician, nurse, dietician, pharmacist, and social worker.8–16
Remote monitoring programs consisted of structured telephone strategy (STS) which involved monitoring collected data via human–human or human–machine interactive response system.1,5,17–20 Lastly, tele-monitoring (TM) which comprised of physiologic data transmission of electrocardiogram (EKG), blood pressure, weight, respiratory rate digitally.1,5,7,16,17,19,21–33
CM showed decreased all-cause mortality (ACM) at 12 months, all-cause readmission (ACR) at 12 months, and CHF readmission at 6 and 12 months. MI resulted in decreased ACR and CHF readmission (Table 1). There was some discrepancy on effectiveness of TM programs alone in individual studies; however, large meta-analysis suggests TM provided a reduction in ACM and risk of CHF hospitalization and was a common factor of successful management plans. STS had similar results to TM including decreased risk of CHF hospitalization and ACM (Table 2).
Statistically significant Case Management and Multidisciplinary Intervention studies.
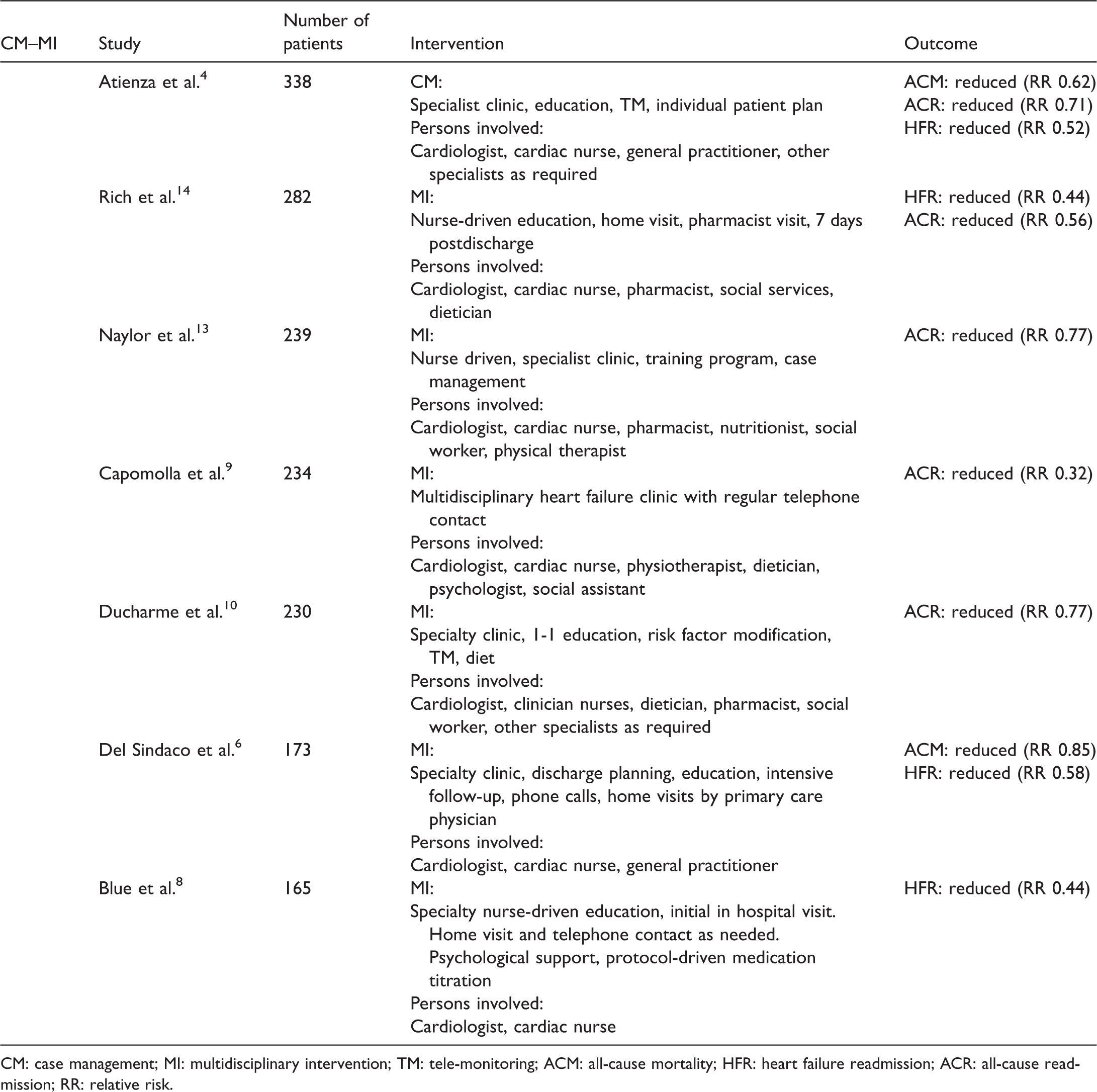
CM: case management; MI: multidisciplinary intervention; TM: tele-monitoring; ACM: all-cause mortality; HFR: heart failure readmission; ACR: all-cause readmission; RR: relative risk.
Statistically significant Structured Telephone Strategy and Tele-Monitoring studies
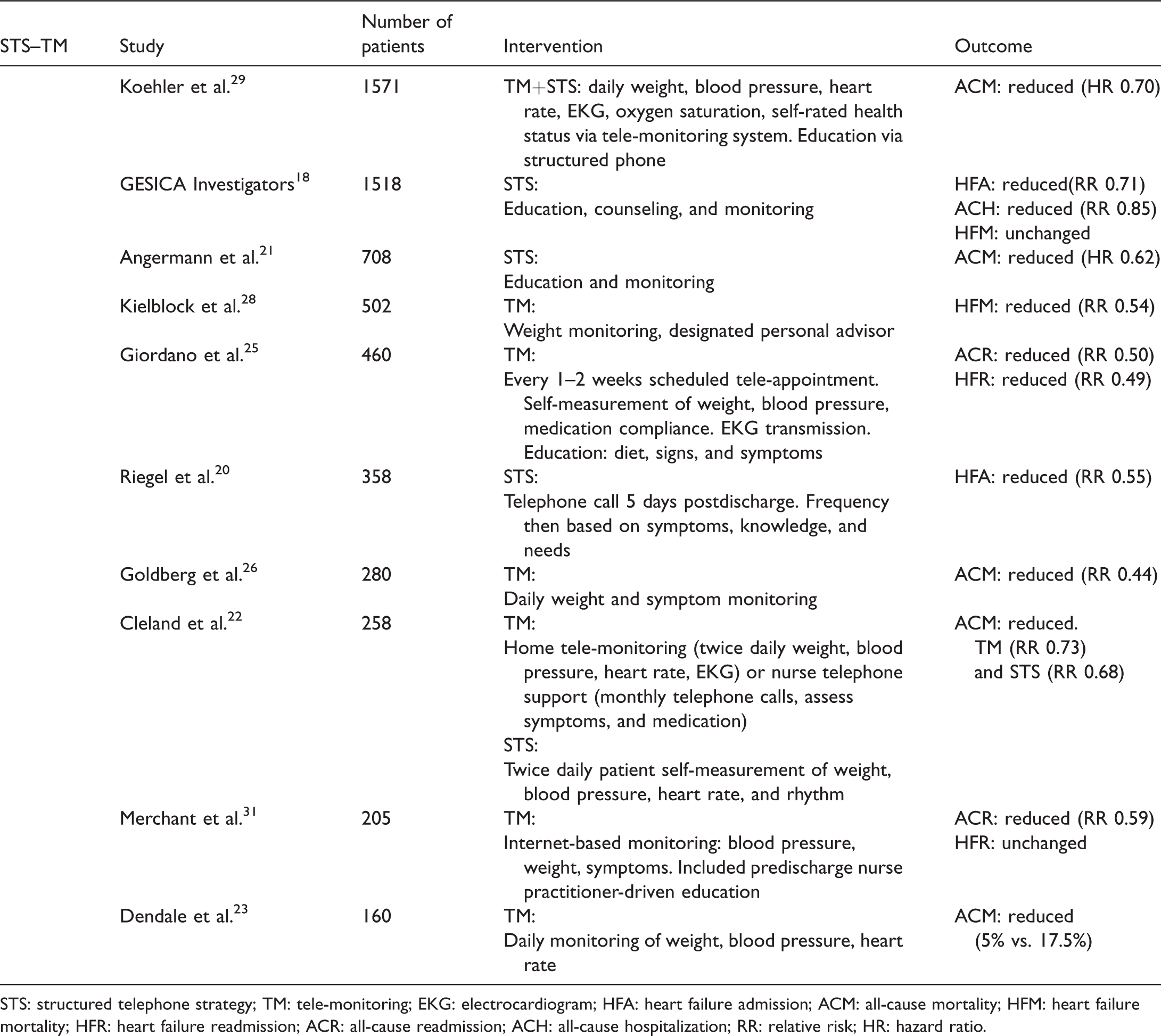
STS: structured telephone strategy; TM: tele-monitoring; EKG: electrocardiogram; HFA: heart failure admission; ACM: all-cause mortality; HFM: heart failure mortality; HFR: heart failure readmission; ACR: all-cause readmission; ACH: all-cause hospitalization; RR: relative risk; HR: hazard ratio.
Cochrane’s review identified a reduction in ACM and heart failure admissions with STS and TM. In addition, CM probably reduced heart failure readmissions and all-cause readmissions, while MI may have reduced heart failure readmissions and all-cause readmissions. There was some evidence that CM and MI may reduce ACM.
Even though the above conclusions were found, no specific recommendations have been developed to guide implementation of these interventions.
CM versus MI
The primary difference between CM and MI is coordination of care. Although both models focus on providing individualized patient care, MI encourages providers from multiple specialties to liaise with one another with the purpose of optimizing the efficiency and quality of patient–provider and provider–provider visits. Providers have direct communication with one another through either contemporaneous multidisciplinary visits with patients or individual visits which are reported and reviewed by a centralized specialist physician and/or nursing in charge of coordinating care. MI also expanded the patient management team to include social workers, dieticians, and pharmacists. CM had similar management, and intervention components, however, did not employ multidisciplinary patient visits. Specialist physician and nursing were typically in charge of coordinating additional care, generating referrals, and follow-up visits in conjunction with the patient’s primary care physician.
Implantable hemodynamic monitors
An interesting and upcoming technology from CHF trials are implantable hemodynamic monitors (IHMs). Initially investigated in several CHF studies comprised of patients ranging from New York Heart Association (NYHA) class II–IV, these devices have been met with mixed results primarily based on potential study bias, blinding, and protocol-guided therapy challenges. The CardioMEMS Heart Sensor Allows Monitoring of Pressure to Improve Outcomes in NYHA Class III Heart Failure Patients (CHAMPION) trial study,34,35 however, showed statistically significant reductions in CHF-related hospitalizations (hazard ratio (HR) 0.72, 95% confidence interval (CI) 0.60–0.85,
Raina et al.
37
performed a retrospective analysis of the CHAMPION trial data and found improved risk stratification of patients with the use of IHM in addition to right heart catheterization (RHC). Those patients with no PH on RHC or IHM had lower HF hospitalization rates than those patients with no PH on RHC but did have PH on IHM (0.25 vs. 0.49, Incidence Rate Ratio (IRR) 0.51, 95% CI 0.33–0.77,
All positive interventions are listed in Tables 1 and 2.
Examples of strategies of each type of intervention that showed positive outcomes are listed below.
Structured telephone strategy
GESICA Investigators 18 employed a strategy consisting of specialist nurse-led education, counseling, and monitoring through frequent telephone follow-up in addition to usual care. Patients were treated by their attending cardiologist and follow-up at least every three months. Nurses trained specifically in heart failure performed telephone follow-ups. Telephone calls were initiated within seven days of discharge. The purpose of telephone calls was to educate and monitor the patient. Data included adherence to diet, drug treatment, monitoring of symptoms (particular attention to disease progression, i.e. dyspnea, edema), control of signs of fluid retention, and daily physical activity. Predetermined questionnaires were provided for nurses along with standardized intervention procedures. Nurses were able to adjust the dose of diuretics and also determine if nonscheduled or emergent medical attention was needed. The outcome of this intervention strategy was a significant reduction in CHF and all-cause hospital admissions.
Tele-monitoring
Giordano et al. 25 developed a TM strategy with two specialty nurse-driven procedures. The first consisted of scheduled weekly TM appointments (TM). A standardized interview includes evaluation of patient’s diet (fluid management, weight monitoring, salt intake, and smoking habits), weight, blood pressure, medication knowledge and compliance, and EKG. At future appointments, nursing reinforced education and patient compliance strategies. The second procedure consisted of occasional appointments (tele-assistance), escalated from TM. This was done if the patient was experiencing signs or symptoms of decompensation or had a concern about therapeutic plan. Further intervention included drug modification (predetermined or nurse contacting specialist physician or primary care physician) or new scheduled appointment. Nursing was required to consult the physician to determine if emergency room or additional specialist clinic follow-up was required. This intervention strategy was successful and resulted in significant reduction in all-cause and heart failure readmissions.
Case management
Atienza et al. 4 created a three-phase CM program. The first phase was disease education for patients and families. Before discharge, a specialist nurse interviewed patient and family to determine disease knowledge base, ability to identify signs and symptoms of disease worsening, and how to respond to deterioration. Education included importance of self-monitoring, diet and exercise, signs and symptoms of heart failure, and medication compliance. The second phase included a primary care physician visit within 2 weeks of discharge. During visit, the patient’s clinical progress was assessed to determine risk of deterioration. If deterioration was anticipated, medication modification was performed, and primary care had the option to refer to hospital for reassessment. The third phase included specialist clinic follow-up visits every three months for routine clinical assessment, where patient performance was analyzed and strategies to improve treatment adherence employed. In addition, reinforcement of disease knowledge and self-management, referral to other specialist, diagnostic tests, and treatments if needed was performed. The end of the study concluded with telephone communication. This leads to a significant reduction in ACM, heart failure admissions, and ACRs.
Multidisciplinary intervention
Rich et al.14,15 chose an MI model. This included intensive disease education by experienced specialist nurse using teaching booklets, individual diet assessment, and instructions given by a registered dietician, social services evaluation to facilitate discharge planning and posthospitalization care, and medication analysis by specialist physician focusing on eliminating unnecessary medications and regimen simplification. Individualized education included specialist nurse-led daily visits while hospitalized addressing diagnosis, symptoms, treatment, follow-up and prognosis. Emphasis placed on importance of self-monitoring and instructions of when to call should monitoring parameters exceed limits provided. An intensive discharge follow-up schedule was created via the hospital’s home care services which were supplemented with nursing home visits and telephone contacts with study team members. First follow-up home visit occurred within 48 h of hospital discharge. Home environment assessment, additional education and teaching materials, and activity guidelines were addressed by the home-care nurse. Three visits were performed during week 1 postdischarge. Routinely scheduled nursing telephone calls were done to assess patient progress and address questions or concerns. Similar to prior intervention strategies, the goals of follow-up were education reinforcement, medication and diet compliance, and identifying symptoms amenable to outpatient treatment. This management plan leads to a reduction in heart failure admission rates.
Stewart et al. 38 discussed in excellent detail the components of a multidisciplinary PH center including its members, their functional roles, work flow of patients from diagnosis to treatment, as well as the importance of patient education and empowerment.
Implantable hemodynamic monitors
Benza et al. 39 performed IHM implantation in 14 pulmonary arterial hypertension (PAH) patients with NYHA class III/IV symptoms and recent hospitalization for heart failure. Mean duration of follow-up was 14 months. They found statistically significant hemodynamic improvements in mean pulmonary artery pressure, total pulmonary resistance, cardiac output, and stroke volume. In addition, brain natriuretic peptide (BNP) levels <340 pg/ml were maintained or achieved in 75% of patients after one month, patient functional class improved, and annual CHF hospitalization was decreased. Of note, there were no reported periprocedural complications or device-related serious adverse events postimplantation. This data suggest that IHM may be a safe adjunct therapy in PAH patients to reduce hospitalizations, improve functional status, and facilitate optimization of hemodynamics (Table 3).
Implantable Hemodynamic Monitor studies

IHM: implantable hemodynamic monitor; HFM: heart failure mortality; HFR: heart failure readmission; HR: hazard ratio; CI: confidence interval; ICD: implantable cardioverter defibrillator; CRT-D: cardiac resynchronization therapy with a defibrillator device; NYHA: New York Heart Association; PAH: pulmonary arterial hypertension.
CM versus CM plus TM
To further identify which interventions were most beneficial, a randomized control trial (RCT) by Wade et al. 7 compared CM and CM plus TM. The result was no significant difference in hospital admission, death, or emergency department visits, suggesting the addition of TM to CM may not provide additional patient benefit.
MI versus MI plus TM
Vuorinen et al. 16 performed an RCT that compared MI and MI plus TM. The combined intervention of MI plus TM did not improve the primary outcome of HF-related hospital days. Of note, health care resources in the combined group were significantly higher including contacts between nurse and patient, visits to nurse reception, and unplanned cardiology clinic visits.
We were not able to identify studies directly comparing STS to CM or STS to MI.
Based on review of available literature and intervention strategies, we suggest a comprehensive care plan (CCP) that enlists a combination of STS, home TM and MIs. A list of interventions and their components is available in Table 4. First and foremost, prior to implementing these strategies, it is imperative that CCP team members are adequately educated regarding disease process, prognosis, medication, and provider-specific treatment goals.
Summary of comprehensive care plan components
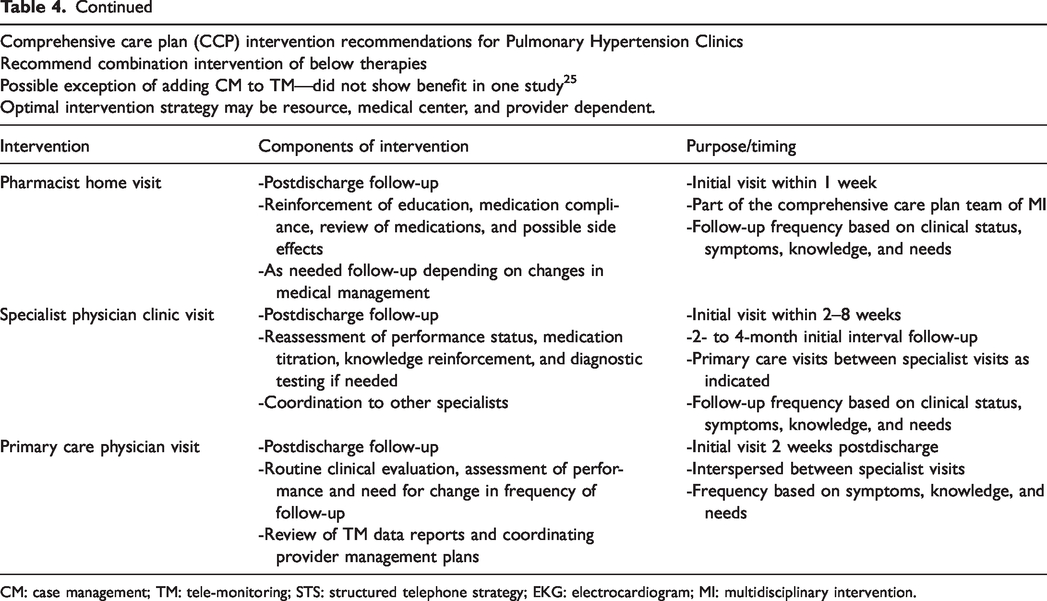
CM: case management; TM: tele-monitoring; STS: structured telephone strategy; EKG: electrocardiogram; MI: multidisciplinary intervention.
Discussion
Clinical implications
Presently, there is no consensus on the most effective outpatient management of PH or strategies to reduce hospital readmission. Successful CHF interventions can provide us with a starting point as we aim to develop and validate PH-specific interventions and comprehensive care programs.
Important factor that likely contribute to the success of these management programs is determining which patient information is most beneficial to monitoring and decision making. Although this article did not investigate which specific data points would be helpful, other articles have. Kane et al. 40 showed an improved concordance statistic (c-index) of 0.84 for predicting mortality when predominantly noninvasive clinical parameters (gender, age, disease duration, 6-min walk test, hemoglobin, glomerular filtration rate, BNP, echocardiography, pulmonary function tests, RHC) were used in addition to World Health Organization functional class. The c-index for functional class alone was 0.60, and when the Registry to Evaluate Early and Long-Term PAH Disease Management (REVEAL) score was validated in their cohort, the c-index was 0.71. These parameters along with multifaceted CCP may further enhance patient management.
Limitations
There were some limitations identified during this review. They include the extrapolation of data and interventions from CHF to PH based on disease and patient similarities. Secondly the duration of time between the original articles (1993–2019). While comprehensive, it should also be considered that medical and interventional techniques for heart failure management have changed, and standards of care improved over time. Another consideration is the proportion of PH patients managed with parenteral therapies. They are often managed by expert PH centers and may already have a system in place which provides close monitoring of their clinical status. It would need to be determined if those current management systems would benefit from modification or replacement with the above alternative systems. Lastly, individual patient’s familiarity and ability to interact with the technology being used to monitor and collect data may be a limiting factor. Those with more technological aptness may be able to provide data more consistently and reliably. In an era of smart devices, this opens the door to development of applications and monitoring programs that could more easily integrate into the daily lives of patients.
Conclusion
In conclusion, we have identified a gap in the current outpatient care and management of PH patients that may be amenable to the implementation of CHF interventions described by our cardiology colleagues given possible patient similarities within the two disease states. The relatively benign nature of these interventions is also particularly attractive. Based on our review, management plans must focus on predischarge, discharge, and postdischarge education for the patient and family members with specific attention to disease process, medication, diet, and self-monitoring. Patients from the community who do not require hospitalization and are able to be seen in the specialist clinic initially should begin their evaluation in similar sequence to that of postdischarge patients. We suggest that strategies to improve the health of PH patients should include STS and TM in addition to the patient-centered approach of multidisciplinary intervention (MI). Regarding IHM devices, the evidence presented in cardiology trials and early data in PAH trials suggest there may be benefit in extrapolating their routine use to PAH patients. However, due to their invasiveness, such an intervention requires further validation prior to being recommended. Which intervention or combination of interventions implemented may require tailoring to the individual institution depending on patient needs and resource availability. Further follow-up studies are needed to identify which interventions are most beneficial to this particular patient population in addition to cost effectiveness of care.
Disclaimer
The views expressed in this article are the view of the authors listed and not the official position of the institutions.
Footnotes
Author contributions
FR conceived of the presented idea. JD developed the theory and performed the data search and interpretation. FR and JD investigated outpatient congestive heart failure management strategies. All authors discussed the results and contributed to data analysis and development of the final manuscript.
Conflict of interest
JD, JPM, VN, and SM have nothing to disclose. JT reports personal fees from United Therapeutics, personal fees and nonfinancial support from Medtronic, Inc., and personal fees and nonfinancial support from United Therapeutics, outside the submitted work. MC reports grants and personal fees from Actelion, grants and personal fees from Bayer, personal fees from United Therapeutics, grants and personal fees from Reata, grants from Eiger, grants from Novartis, grants from Liquidia, grants from Complexa, grants and personal fees from Phase Bio, grants and personal fees from Arena, grants from Medtronic, personal fees from Gilead, personal fees from Express Scripts, and personal fees from Akros, outside the submitted work. FR is a researcher, consultant, and speaker for Actelion, Bayer, and United Therapeutics. He is also a researcher and consultant for Acceleron. He reports grants and personal fees from Actelion, grants and personal fees from Bayer, personal fees from United Therapeutics, and grants and personal fees from Acceleron, outside the submitted work.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
