Abstract
The six-minute walk test is widely used to assess the severity and prognosis of pulmonary hypertension. However, the pathophysiology underlying a compromised six-minute walk distance is incompletely characterized. The purpose of this study is to evaluate the Fick principle and pulmonary hemodynamic determinants of the six-minute walk distance in patients with suspected pulmonary hypertension. Twenty-nine patients were retrospectively studied and underwent a right heart catheterization for the evaluation of suspected pulmonary hypertension. With the pulmonary artery catheter in place, patients were moved to a treadmill and completed a six-minute walk test. Fick cardiac output and indices of right heart afterload were calculated using continuous measurements of pulmonary vascular pressures, gas exchange, and mixed venous blood samples. Fifteen subjects who walked ≤ 348 m were compared to 14 subjects who walked > 348 m. Systemic oxygen delivery was impaired in six-minute walk distance ≤ 348 m compared to six-minute walk distance > 348 m (15.2 ± 6.2 vs. 23.2 ± 6.8 mL/kg/min, p < 0.01). Impaired oxygen delivery was due to a depressed cardiac index and decreased cardiac reserve demonstrated by the change in the stroke volume index (3.0 ± 14 vs. 17 ± 15 mL/min/m2, p = 0.02). The six-minute walk distance positively correlated with oxygen delivery (r = 0.501, p = 0.006) and inversely correlated with oxygen extraction (r = 0.369, p = 0.049). A decreased six-minute walk distance was associated with an increased total pulmonary resistance (r = 0.502, p = 0.006) and pulmonary vascular resistance (r = 0.530, p = 0.003). In patients with suspected pulmonary hypertension, a decreased six-minute walk distance is due to compromised oxygen delivery, decreased cardiac reserve, and increased right ventricular afterload.
Introduction
The six-minute walk test (6MWT) is a submaximum exercise test used for the evaluation of functional capacity in patients with heart failure and pulmonary hypertension.1,2 The widespread use of this test stems from its simplicity, low cost, and reproducibility. Along with its utility in determining prognosis,3–5 the 6MWT is frequently used as a study design end-point in trials evaluating treatment efficacy for pulmonary arterial hypertension (PAH). 6 However, criticism has been levied at this testing modality, such as what constitutes a meaningful change in six-minute walk distance (6MWD) in the setting of background PAH-specific therapy.7,8 Due to its nonspecific assessment of exercise capacity, changes in the 6MWD may reflect a wide range of pathology that include individual biomechanics, 9 changes in the pulmonary vasculature, cardiac output (CO), or peripheral limitations of the exercising muscle bed. 10 Additionally, correlations between 6MWD and maximum incremental cardiopulmonary exercise testing (CPET) results remain subjective 11 and may depend on the CPET experience of both the patient and the operator. 12
Although general aerobic capacity can be inferred from the 6MWT, the pathophysiology underlying a compromised 6MWD is difficult to determine in isolation. Unlike peak oxygen uptake (VO2), there are weak correlations between 6MWD and CPET variables such as ventilatory efficiency (VE/VCO2) and changes in end-tidal carbon dioxide. 13 Noninvasive measurements of cardiac hemodynamics using impedance cardiography have shown impaired stroke volume (SV) as the cause of a decreased 6MWD in patients with systemic sclerosis and pulmonary hypertension. 14 Inert gas rebreathing has also been used to assess central hemodynamics during the 6MWT with mixed results. 15
While noninvasive correlates may guide our understanding of exertional intolerance, measuring hemodynamics directly with a pulmonary artery catheter remains the gold standard in the assessment of pulmonary hypertension and can be used to explain the mechanisms underlying a decreased 6MWD. 16 Potential causes of a decreased 6MWD include decreased oxygen delivery (DO2) and its utilization. Other groups have shown correlations between a decreased 6MWD and invasive hemodynamics, but none has done so concurrently.17,18 Therefore, the purpose of this study is to evaluate the simultaneously measured Fick principle determinants of the 6MWT in patients with suspected pulmonary hypertension.
Methods
Twenty-nine patients were referred for a clinically indicated resting right heart catheterization (RHC) after evaluation in the Dyspnea Center at Brigham and Women’s Hospital for the evaluation of clinically suspected exercise or resting pulmonary hypertension. All patients had a transthoracic echocardiogram that did not show left heart disease and had a contemperanous noninvasive 6MWT. Systematic data collection for research purposes was approved by the Partners Human Research Committee (IRB 2011P000272).
Right heart catheterization
Vascular access of the internal jugular vein was obtained under ultrasound guidance using a micro-introducer kit (Teleflex Incorporated, Wayne, PA, USA). After venous access was confirmed with fluoroscopy, a 7 French, single-lumen pulmonary artery catheter was placed using Seldinger technique. A zero-reference level was set at the mid-thoracic level with the patient in the supine position. 19 Hemodynamic data were obtained in the usual fashion after confirming both catheter location on fluoroscopy and the presence of appropriate waveforms. 20 CO was calculated at rest using the Fick equation and an estimated oxygen consumption. Pulmonary vascular resistance (PVR) was calculated using the assumed Fick CO.
Invasive 6MWT
After the RHC was complete and the pulmonary artery catheter secured, patients were moved to an adjacent treadmill (SportsArt Fitness TR22F, Woodinville, WA) in the catheterization lab. The zero-reference point in the upright position was set at the fourth intercostal space in the mid-axillary line. 21 Baseline hemodynamic and gas exchange data were obtained in the upright position for two minutes prior to the start of exercise. Patients then walked for six minutes on the treadmill, with speed, but not grade, adjusted to patient tolerance. This was followed by one minute of recovery.
Gas exchange, heart rate, and arterial pulse oxygen saturation (SpO2) were continuously measured using a portable metabolic cart (Shape Medical Systems, MN, USA). Systemic blood pressure was measured every minute of exercise using a cuff sphygmomanometer. Pulmonary artery pressures (PAP) were continuously monitored during the 6MWT (Xper Cardio Physiomonitoring System, Philips, Melbourne, FL, USA). Pulmonary arterial wedge pressures (PAWP) were obtained every minute during exercise. 22 Averages of at least three waveforms across the respiratory cycle were used to account for swings in intrathoracic pressure that could lead to overestimation with end-expiratory pressure measurements. 23
Arterial oxygen content was calculated from SpO2 × [Hb] × 1.34. Mixed venous content was calculated from mixed venous oxygen saturation (SvO2) × [Hb] × 1.34. 24 Indirect Fick CO was calculated as VO2/(CaO2 – CvO2), using pulse oximetry as a surrogate for directly measured arterial oxygen saturation. 25 Total pulmonary resistance (TPR) was calculated as mean pulmonary arterial pressure (mPAP)/CO. PVR was calculated as (mPAP – PAWP)/CO. Pulmonary arterial compliance (PAC) was calculated as (SV)/(systolic – diastolic PAP). SV was calculated from CO/heart rate. Oxygen extraction was calculated as (CaO2 – CvO2)/[Hb], based on the concept that peak systemic oxygen extraction during exercise should approach the hemoglobin concentration. 26 All included patients had complete monitoring of peripheral oxygen saturations and hemodynamic data.
Statistical analysis
Data are presented as mean ± standard deviation unless otherwise stated. Comparisons between groups were made using a Student’s t-test or a Mann–Whitney test. Categorical variables were compared using a Chi-squared test or a Fisher’s exact test. Correlations between variables were calculated using the Pearson’s correlation coefficient or the Spearman’s rank correlation coefficient. A p-value < 0.05 was considered significant. SPSS (IBM Corp., Released 2010, IBM SPSS Statistics for Windows, Version 19.0. Armonk, NY: IBM Corp) was used for all statistical analysis.
Results
Baseline characteristics according to the 6MWD.
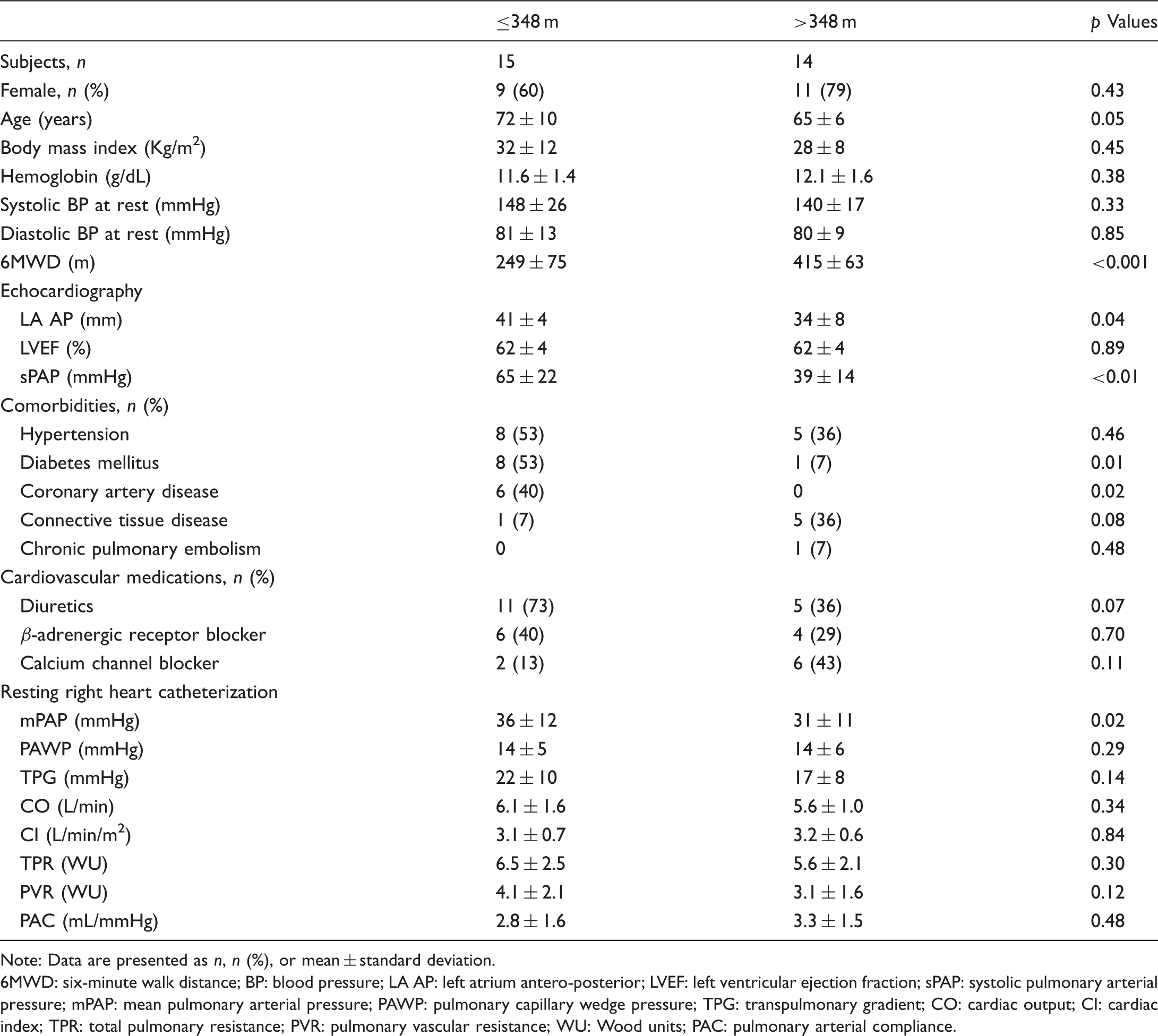
Note: Data are presented as n, n (%), or mean ± standard deviation.
6MWD: six-minute walk distance; BP: blood pressure; LA AP: left atrium antero-posterior; LVEF: left ventricular ejection fraction; sPAP: systolic pulmonary arterial pressure; mPAP: mean pulmonary arterial pressure; PAWP: pulmonary capillary wedge pressure; TPG: transpulmonary gradient; CO: cardiac output; CI: cardiac index; TPR: total pulmonary resistance; PVR: pulmonary vascular resistance; WU: Wood units; PAC: pulmonary arterial compliance.
Resting RHC results
mPAP from the resting supine RHC was higher in 6MWD ≤ 348 m compared to 6MWD > 348 m (36 ± 12 vs. 31 ± 11 mmHg, p < 0.02). CO, PVR, TPR, and PAC were not significantly different (Table 1). Among the studied patients, 83% (n = 24/29) had a resting mPAP > 20 mmHg. Of the 24 patients with pulmonary hypertension, 33% (n = 8/24) had precapillary PH, 25% (n = 6/24) had postcapillary PH, and 25% (n = 6/24) had combined pre- and postcapillary PH. Of the five patients who did not meet the 6th World Symposium Definition of pulmonary hypertension, 27 all either had borderline resting mPAPs or PVRs that fit an exercise pulmonary hypertension phenotype. 28
Fick variables during the invasive 6MWT
Gas exchange measurements during invasive 6MWT according to the 6MWD.
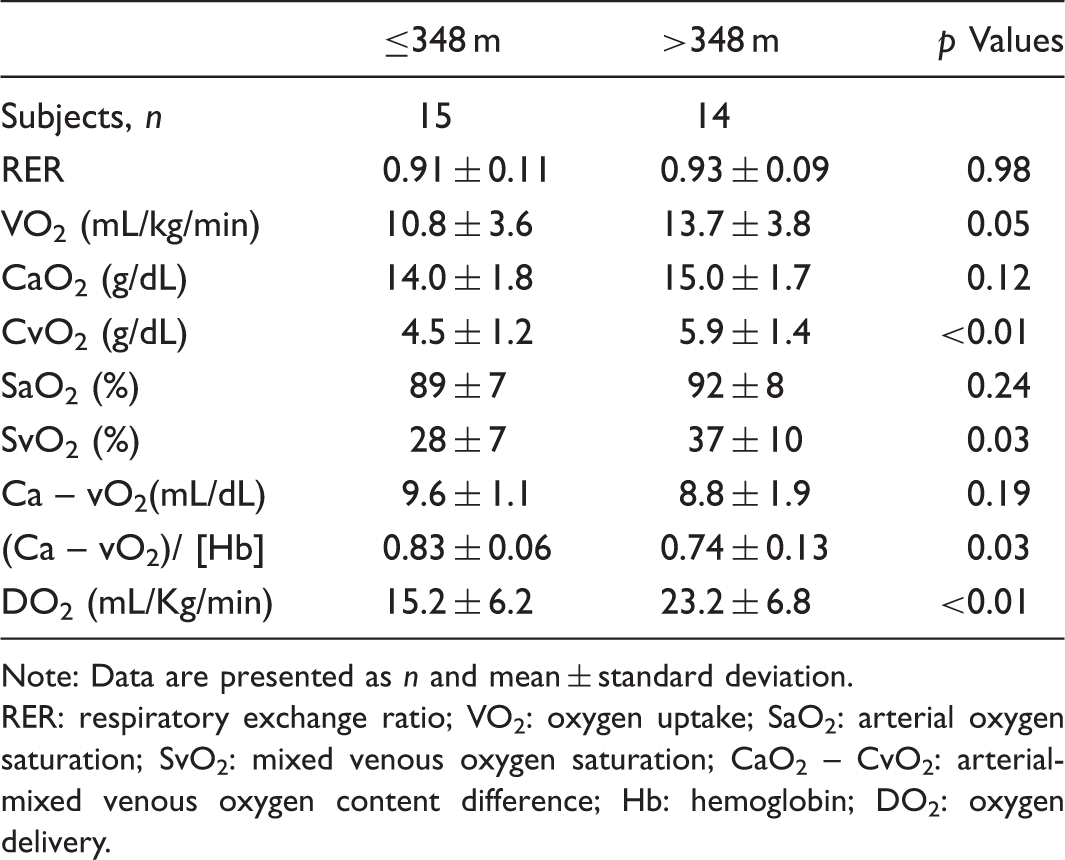
Note: Data are presented as n and mean ± standard deviation.
RER: respiratory exchange ratio; VO2: oxygen uptake; SaO2: arterial oxygen saturation; SvO2: mixed venous oxygen saturation; CaO2 – CvO2: arterial-mixed venous oxygen content difference; Hb: hemoglobin; DO2: oxygen delivery.
Hemodynamics during invasive 6-MWT according to the 6-MWD.
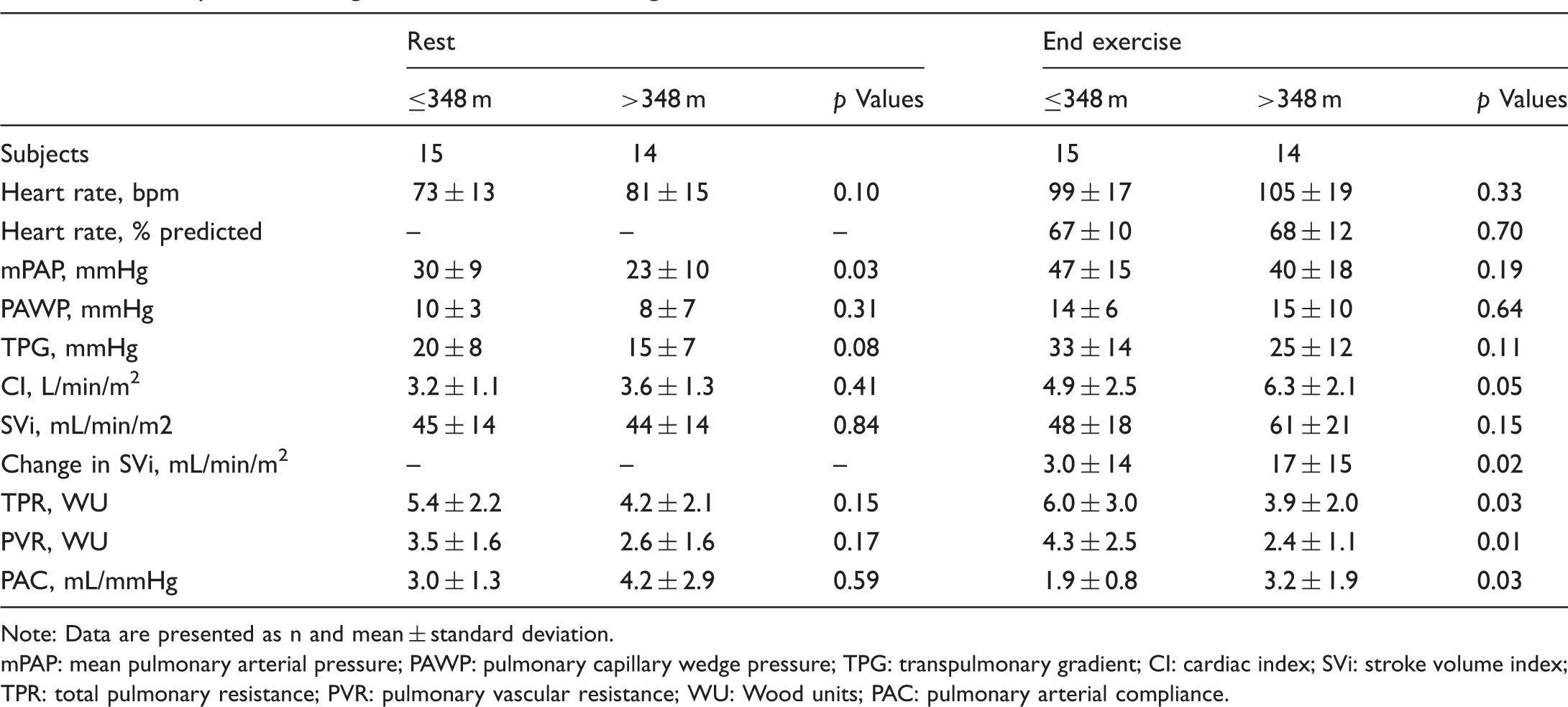
Note: Data are presented as n and mean ± standard deviation.
mPAP: mean pulmonary arterial pressure; PAWP: pulmonary capillary wedge pressure; TPG: transpulmonary gradient; CI: cardiac index; SVi: stroke volume index; TPR: total pulmonary resistance; PVR: pulmonary vascular resistance; WU: Wood units; PAC: pulmonary arterial compliance.
Upright, resting mPAP was higher in 6MWD ≤ 348 m compared to 6MWD > 348 m (30 ± 9 vs. 23 ± 10 mmHg, p < 0.05). mPAP and PAWP at end exercise were not different (Table 3, Fig. 1).
Minute by minute (a) mPAP, (b) PAWP, (c) CO, (d) TPR, (e) PVR, and (f) PAC during the invasive 6MWT in patients who walked (•) ≤ 348 m and (⋄) > 348 m.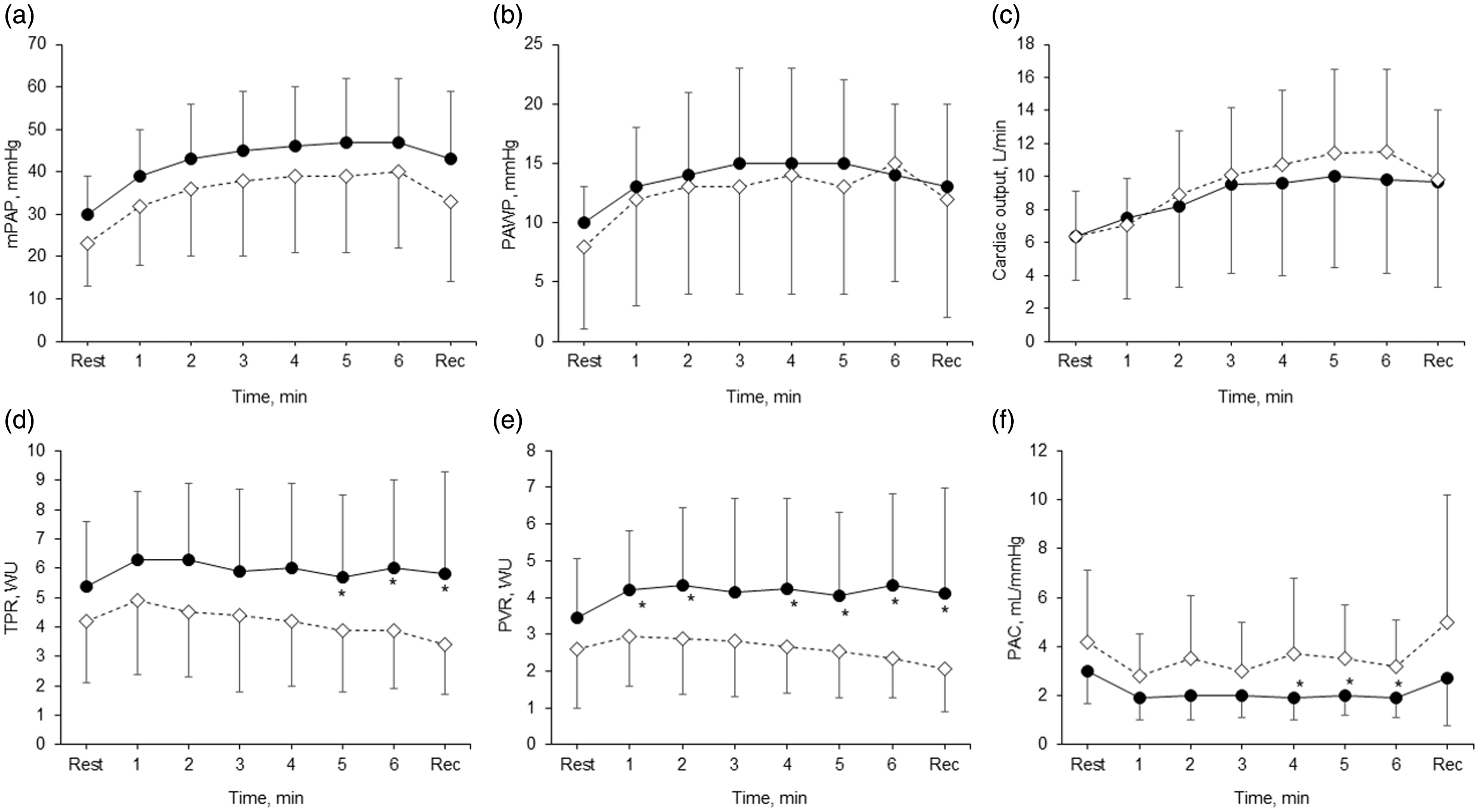
Right ventricular afterload
Indices of right ventricular afterload were all significantly different during 6MWT. TPR (6.0 ± 3.0 vs. 3.9 ± 2.0 Wood units, p < 0.05) and PVR (4.3 ± 2.5 vs. 2.4 ± 1.1, p < 0.05) were both increased in 6MWD ≤ 348 m during 6MWT. PAC was lower in 6MWD ≤ 348 m during the 6MWT (1.9 ± 0.8 vs. 3.2 ± 1.9 mL/mmHg, p < 0.05). TPR and PVR were both significantly increased and remained elevated throughout exercise into recovery in 6MWD ≤ 348 m, as compared to the normal decline in 6MWD > 348 m. PAC decreased at the first minute of the 6MWT and remained at this level for the duration of exercise (Fig. 1).
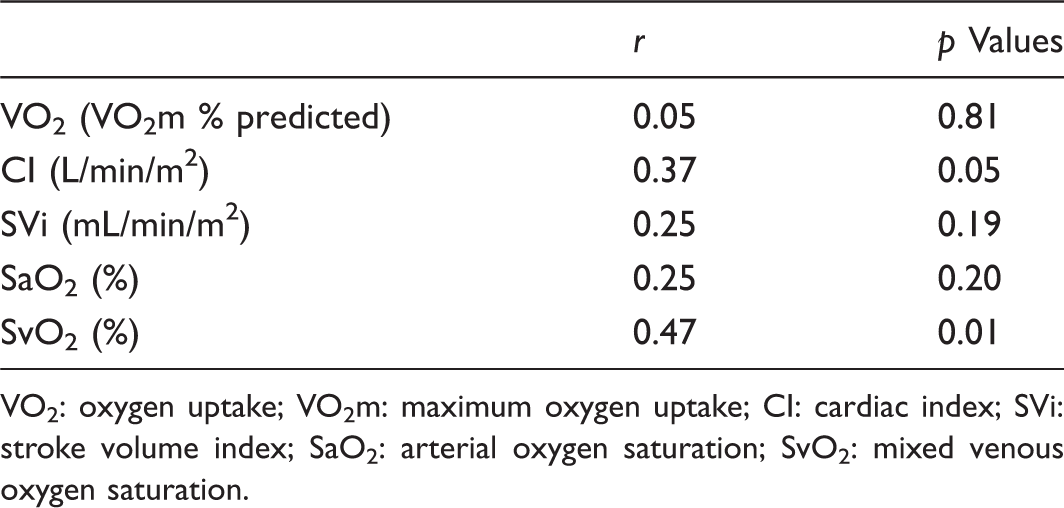
Among gas exchange and hemodynamic variables measured during the 6MWT, VO2, cardiac index, and SV did not correlate with the 6MWD (Table 4). However, both DO2 and systemic oxygen extraction ratio correlated with the 6MWD (Fig. 2). Additionally, indices of right ventricular afterload correlated with the 6MWD (Fig. 3) and correlated with changes in SV and SVi (Fig. 4).
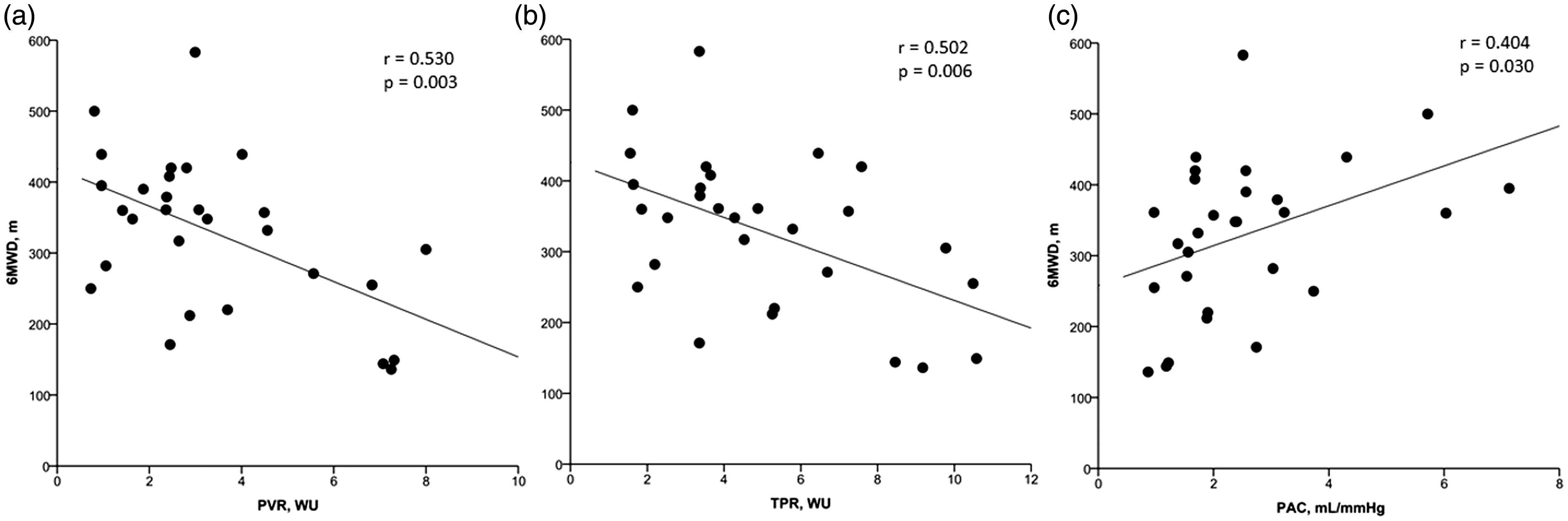
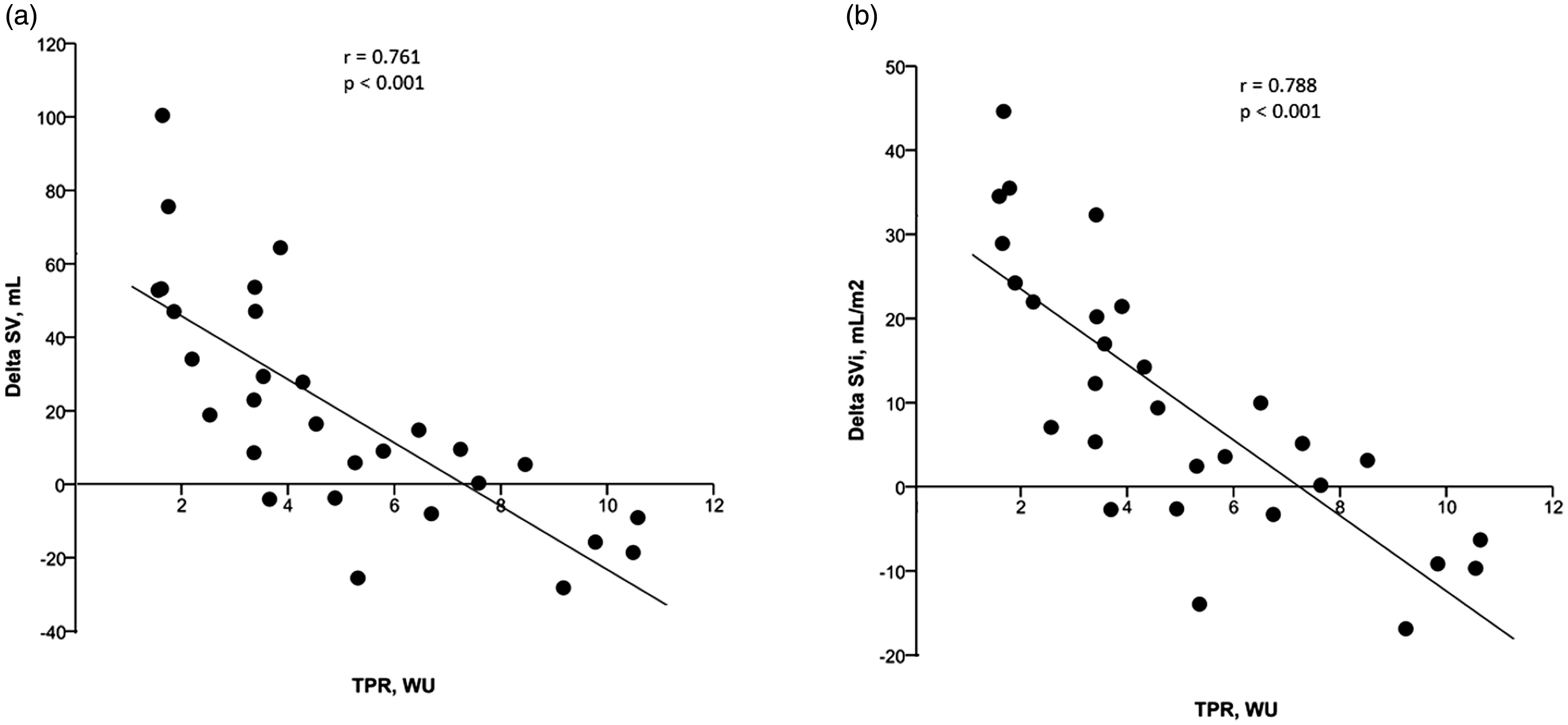
Correlations between 6MWD and (a) DO2 and (b) (Ca-vO2)/[Hb] during the invasive 6MWT. Correlations between 6MWD and (a) PVR, (b) TPR, and (c) PAC during the invasive 6MWT. Correlation between TPR and (a) change in SV and (b) change in SVi during the invasive 6MWT. Correlation between exercise variables and 6MWD. VO2: oxygen uptake; VO2m: maximum oxygen uptake; CI: cardiac index; SVi: stroke volume index; SaO2: arterial oxygen saturation; SvO2: mixed venous oxygen saturation.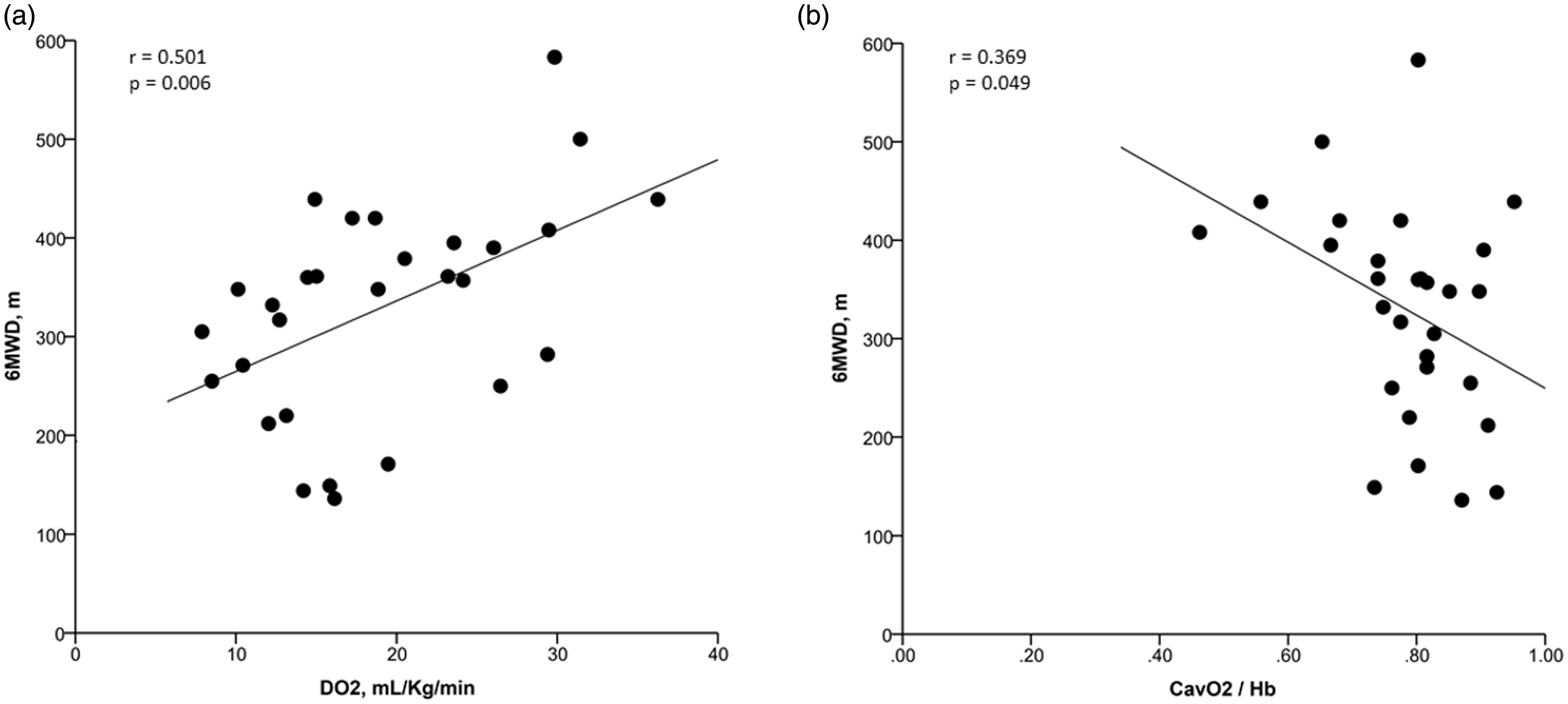
Discussion
The purpose of the current study was to evaluate simultaneously measured Fick principle determinants of the 6MWT in patients with suspected pulmonary hypertension. While correlations among aerobic capacity, pulmonary hemodynamics, and the 6MWD have been previously described, these measurements have never been made concurrently. The current study findings show that a decreased 6MWD in pulmonary hypertension is due to impaired DO2 rather than its uptake and utilization, which in turn is due to decreased cardiac reserve from increased right ventricular afterload.
For the last 30 years, the 6MWT has been used in the evaluation of patients with pulmonary hypertension and as an endpoint in numerous clinical trials.8,29 Its widespread use as a primary outcome has been called into question as meta-analyses show that it does not fully explain treatment effects or correlate with clinical outcomes.30,31 In spite of this uncertainty, the 6MWT remains an integral part of the assessment of a patient with pulmonary hypertension, as seen in the recent update of the REVEAL 2.0 risk calculator. 3
Field testing correlating with aerobic capacity was first studied half a century ago. Originally described as a simple, low cost method to assess aerobic capacity in aviation officers, 32 the 15-min run was eventually shortened to a 12-min run that was shown to have good correlation with peak VO2. 33 This was adapted to a 12-min walk test in patients with chronic bronchitis and again demonstrated good correlation with peak VO2 along with forced vital capacity. 34 Because of the potential for exhaustion for the patient and the time consumption for the provider, 2 -, 6 -, and 12-min walking tests were compared in respiratory disease and showed high correlation coefficients between all exercise durations. 35 Since that study, the 6MWT became the standard in the assessment of functional status in respiratory disease before also being studied in chronic heart disease.36,37 While other measurements of cardiovascular fitness have been shown to have similar values at peak exercise compared to submaximum exercise, 38 the 6MWT remains the standard in the assessment of disease state in patients with pulmonary hypertension.
Fick principle determinants of the 6MWD
In the present study, we demonstrate that impaired DO2, rather than its systemic uptake and utilization, underlies the decreased 6MWD in patients with suspected pulmonary hypertension. In turn, an impaired cardiac index drives decreased DO2 as hemoglobin concentration and oxygen saturation were not different between 6MWD ≤ 348 m and 6MWD > 348 m. This is consistent with prior studies showing a central cardiac limitation in patients with exercise pulmonary hypertension and exercise heart failure with preserved ejection fraction.28,39 This central cardiac limitation appears at minute 3 of the 6MWT, as seen with the plateau in CO in 6MWD ≤ 348 m compared to 6MWD > 348 m (Fig. 1c). Consistent with a central cardiac limitation, both the change in the SV and SVi were decreased in 6MWD ≤ 348 m compared to 6MWD > 348 m, signifying decreased cardiac reserve. Exercise performed during the 6MWT was performed near the anaerobic threshold as evident by a RER above 0.90, supporting the idea of impaired DO2 during the 6MWT. 40
Oxygen uptake and utilization
The second component of the Fick equation, systemic oxygen extraction, was evaluated in this study. Patients with a decreased 6MWD had a lower SvO2 and a higher arterial–venous oxygen content difference when normalized to hemoglobin (extraction ratio), signifying increased systemic oxygen extraction in 6MWD ≤ 348 m. This suggests that there is a peripheral, compensatory mechanism in the setting of impaired DO2 described above.
These findings contrast with studies suggesting abnormalities in capillary density and microcirculatory alterations in patients with PAH.41,42 While impaired oxygen utilization in PAH is not completely understood, it is thought to be due to a chronic inflammatory state leading to striated muscle atrophy and decreased contractility in both the diaphragm and peripheral muscles. 43 Additionally, vastus lateralis muscle biopsies from patients with PAH show a decreased ratio of slow twitch/type I muscle fibers to fast twitch/type II muscle fibers, increased proteolysis of muscle, and decreased levels of mitochondrial fusion protein. 44 Contrary to these studies, we identified that not only is there no peripheral limitation underlying a compromised 6MWD, there is a compensatory increase in peripheral oxygen extraction in the face of decreased DO2. Our finding of preserved and adaptive systemic oxygen extraction may be explained by our study of a less severe pulmonary hypertension population.
Pulmonary vascular response
The central cardiac limitation observed in 6MWD ≤ 348 m was related to an abnormal pulmonary vascular response to exercise. Both systolic PAP estimated from the transthoracic echocardiogram and upright, resting mPAP were higher in the 6MWD ≤ 348 m group. During the 6MWT, TPR and PVR were increased and PAC was lower in 6MWD ≤ 348 m. Abnormalities of all three indices of right ventricular afterload were associated with a compromised 6MWD (Fig. 3). Both the change in SV and SVi correlated with TPR (Fig. 4).
We have previously shown that in normal individuals TPR, PVR, and PAC decrease during upright, maximum exercise on a cycle ergometer. 45 Prior work has also shown that peak VO2 is decreased in exercise pulmonary hypertension due to depressed CO associated with increased right ventricular afterload including an elevated PVR and decreased PAC.28,46,47
In conclusion, while aerobic capacity has been loosely correlated with 6MWD, this is the first study to investigate Fick variables and their relationship to directly and simultaneously measured pulmonary hemodynamics during a 6MWT. In patients with suspected pulmonary hypertension, a decreased 6MWD is due to decreased DO2 from a depressed cardiac index and decreased cardiac reserve as demonstrated by the change in the SVi. This cardiac limitation is associated with abnormal indices of right ventricular afterload such as PVR and pulmonary arterial compliance. As previously suspected, but not proven, cardiac index and indices of right ventricular afterload correlate with the 6MWD. We suggest a similar invasive approach can be used in future studies to validate and better understand the 6MWT in other diseases.
Limitations
Limitations of this study include a small sample size and a lack of healthy controls. Despite our small sample size and given the lack of invasive hemodynamic data for the 6MWT, our study provides useful insights underlying a compromised 6MWD in pulmonary hypertension. Testing healthy individuals is generally not possible in invasive studies due to the potential risks of invasive testing. The study population was older in age compared to subjects with early PAH. Univariate and multivariate analysis of key Fick principle determinants was not feasible due to the small sample size. However, the analysis using the 6MWD median value of 348 m is clinically relevant given that the value is similar to the 6MWD in clinical trials of pulmonary hypertension and also approximates the 6MWD that separates functional class II from III. 8
Additionally, this was a nontraditional way to perform a 6MWT as these are not routinely performed on a treadmill as treadmill testing can decrease the 6MWD. 48 However, we encouraged treadmill walking with ATS guidelines for the 6MWT with standardized phrases of encouragement.
Indirect Fick measurements of the CO were used due to using pulse oximetry as a surrogate for directly measured arterial oxygen saturation using an arterial catheter.
The RER for both groups was above 0.9, which supports the idea that exercise during the 6MWT is performed at or near the gas exchange anaerobic threshold. However, we do not have lactate measurements to directly confirm this. We do not have average walking speeds to make correlations with physiologic variables.
Supplemental Material
sj-pdf-1-pul-10.1177_2045894020957576 - Supplemental material for Fick principle and exercise pulmonary hemodynamic determinants of the six-minute walk distance in pulmonary hypertension
Supplemental material, sj-pdf-1-pul-10.1177_2045894020957576 for Fick principle and exercise pulmonary hemodynamic determinants of the six-minute walk distance in pulmonary hypertension by Phillip Joseph, Rudolf K.F. Oliveira, Roza B. Eslam, Manyoo Agarwal, Aaron B. Waxman and David M. Systrom in Pulmonary Circulation
Footnotes
Acknowledgments
We thank Julie A. Tracy (Heart and Vascular Center, Brigham and Women’s Hospital) for her technical expertise.
Conflict of interest
The author(s) declare that there is no conflict of interest.
Contributions
All authors gave final approval and agree to be accountable for the work presented in this submission.
Ethical approval
Systematic data collection for research purposes was approved by the Partners Human Research Committee (IRB 2011P000272).
Funding
Roza B. Eslam, MD was supported by Erwin Schrödinger grant J 3522-B13. Departmental funds from Brigham and Women’s Hospital were used.
Guarantor
David M. Systrom, MD.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
