Abstract
We evaluated whether updated pulmonary hypertension definitive criteria proposed in sixth World Symposium on Pulmonary Hypertension had an impact on diagnosis of overall pulmonary hypertension and pre-capillary and combined pre- and post-capillary phenotypes as compared to those in European Society of Cardiology/European Respiratory Society 2015 pulmonary hypertension Guidelines. Study group comprised the retrospectively evaluated 1300 patients (age 53.1 ± 18.8 years, female 807, 62.1%) who underwent right heart catheterization with different indications between 2006 and 2018. Mean pulmonary arterial pressure ≥25 mmHg (European Society of Cardiology) and PAMP (mean pulmonary arterial pressure) >20 mmHg (World Symposium on Pulmonary Hypertension) right heart catheterization definitions criteria were used, respectively. For pre-capillary pulmonary hypertension, pulmonary artery wedge pressure ≤15 mmHg and pulmonary vascular resistance ≥3 Wood units criteria were included in the both definitions. Normal mean pulmonary arterial pressure (<21 mmHg), borderline mean pulmonary arterial pressure elevation (21–24 mmHg), and overt pulmonary hypertension (≥25 mmHg) were documented in 21.1, 9.8, and 69.1% of the patients, respectively. The pre-capillary and combined pre- and post-capillary pulmonary hypertension were noted in 2.9 and 1.1%, 8.7 and 2.5%, and 34.6 and 36.6% of the patients with normal mean pulmonary arterial pressure, borderline, and overt pulmonary hypertension subgroups, respectively. The World Symposium on Pulmonary Hypertension versus European Society of Cardiology/European Respiratory Society definitions resulted in a net 9.8% increase in the diagnosis of overall pulmonary hypertension whereas increases in the pre-capillary pulmonary hypertension and combined pre- and post-capillary pulmonary hypertension diagnosis were only 0.8 and 0.3%, respectively. The re-definition of mean pulmonary arterial pressure threshold seems to increase the frequency of the overall pulmonary hypertension diagnosis. However, this increase was mainly originated from those in post-capillary pulmonary hypertension subgroup whereas its impact on pre-capillary and combined pre- and post-capillary pulmonary hypertension was negligible. Moreover, criteria of pre-capillary pulmonary vascular disease and combined pre- and post-capillary phenotypes were still detectable even in the presence of normal mean pulmonary arterial pressure. The obligatory criteria of pulmonary vascular resistance ≥3 Wood units seems to keep specificity for discrimination between pre-capillary versus post-C pulmonary hypertension after lowering the definitive mean pulmonary arterial pressure threshold to 20 mmHg.
Keywords
Introduction
Since the first World Symposium on Pulmonary Hypertension (WSPH), pulmonary hypertension (PH) has been arbitrarily defined as mean pulmonary arterial pressure (mPAP) ≥25 mmHg at rest, measured by right heart catheterization (RHC).1–4 However, recent data from normal individuals revealed that normal mPAP mean value was 14.0 ± 3.3 mmHg, and two standard deviations (SDs) above this mean value would suggest mPAP > 20 mmHg as the upper limit of normal (ULN) (the 97.5th percentile).5,6 Furthermore, current data from longitudinal follow-up cohorts in some specific risk groups have suggest that even mPAP>20 mmHg has been significantly associated with increased risks for progression to overt pulmonary arterial hypertension (PAH), hospitalizations, and mortality.7–13 However, borderline elevations in mPAP solely are not considered to be sufficient to specify pulmonary vascular disease because of the fact that this can be due to an increase in cardiac output or pulmonary arterial wedge pressure (PAWP).5,14 Thus, sixth WSPH Task Force has proposed to include pulmonary vascular resistance (PVR) ≥3 Wood units into the definition of pre-capillary (pre-C) PH in addition to mPAP>20 mmHg. 5
However, several issues, whether the reducing the definitive cut-off value of PH to 20 mmHg significantly increases the “new” prevalence of the patients with pre-C PH or may lead to misdiagnosis, unnecessary RHC procedures, earlier initiation of aggressive PAH-targeted therapies in borderline pre-C PH subsets, and surgical endarterectomy in chronic thromboembolic disease remain to be determined.14–16
In this single-center retrospective study, we aimed to evaluate the characteristics of patients with normal mPAP, borderline elevation in mPAP and overt PH, and to assess the impact of the revised PH definitive mPAP threshold >20 mmHg on diagnosis rates of additional PH, pre-C PH, and combined pre- and post-capillary (co-pre-post-C) PH as compared to those with prior cut-off value of mPAP ≥25 mmHg.
Methods
Our study group comprised of the retrospectively evaluated 1300 patients (age 53.1 ± 18.8 years, female 807, 62.1%) who underwent RHC with different indications between 2006 and 2018. In accordance with recommendations of European Society of Cardiology (ESC)/European Respiratory Society (ERS) 2015 PH Guidelines, 4 all patients underwent RHC following the echocardiographic assessments showing findings suggestive for increased PH probability. Indications for RHC were as follows: as a part of the our single-center EvalUation of Pulmonary Hypertension Risk factors AssociaTEd with Survival (EUPHRATES) study in 491 patients, for hemodynamic confirmation and/or risk-based management for heart failure in 677 patients, and before percutaneous interventions or surgical operations for valvular heart diseases in 127 patients. For hemodynamic definitions of PH on RHC according to the ESC/ERS 2015 PH Guidelines and sixth WSPH PH definitions, mPAP ≥25 mmHg and mPAP >20 mmHg cut-off values have been utilized as diagnostic criteria, respectively.4,6 For pre-C PH definitions, PAWP ≤15 mmHg and PVR ≥3 Wood units criteria have been included in both the definitions. 6 Overall study population have been subclassified according to the invasively measured normal mPAP (<21 mmHg), borderline elevation in mPAP (21–24 mmHg), and overt PH (≥25 mmHg), and baseline demographics, clinical, echocardiographic, and hemodynamic characteristics were compared. Written informed consent was obtained from each participant, if needed, and the study protocol was reviewed and approved by the Institutional Ethics Committee. This study was conducted in accordance with the Declaration of Helsinki.
Statistical methods
Continuous variables were represented as mean and SD, and categorical variables were represented as % and number. Numerical differences across the three groups were tested by variance analysis, and categorical variables were tested by chi-square analysis. In cases where statistically significant differences were detected between the groups, post-hoc test (Tukey test) was also utilized for more detailed analysis. A p value of <0.05 was considered statistically significant. All analyzes were performed with SPSS Statistical Package for the Social Sciences program.
Results
Normal mPAP, borderline mPAP, and overt PH were documented in 275 (21.1%), 127 (9.8%), and 898 (69.1%) out of the 1300 patients, respectively (Fig. 1a). According to the definitive criteria of mPAP ≥25 mmHg and mPAP >20 mmHg, PH was diagnosed in 69.1 and 78.9%, pre-C PH in 23.9 and 24.7%, and co-pre-post-C PH in 25.1 and 25.4%, respectively (Fig. 1b).
(a) Normal mean pulmonary pressure (mPAP), borderline mPAP, and overt PH were documented in 275 (21.1%), 127 (9.8%), and 898 (69.1%) out of the 1300 patients, respectively and (b) according to the definitive criteria of mPAP ≥25 mmHg and mPAP >20 mmHg, PH was diagnosed in 69.1 and 78.9%, pre-C PH in 23.9 and 24.7%, and combined pre-post-capillary (co-pre-post-C) PH in 25.1 and 25.4%, respectively. mPAP: mean pulmonary artery pressure, PH: pulmonary hypertension.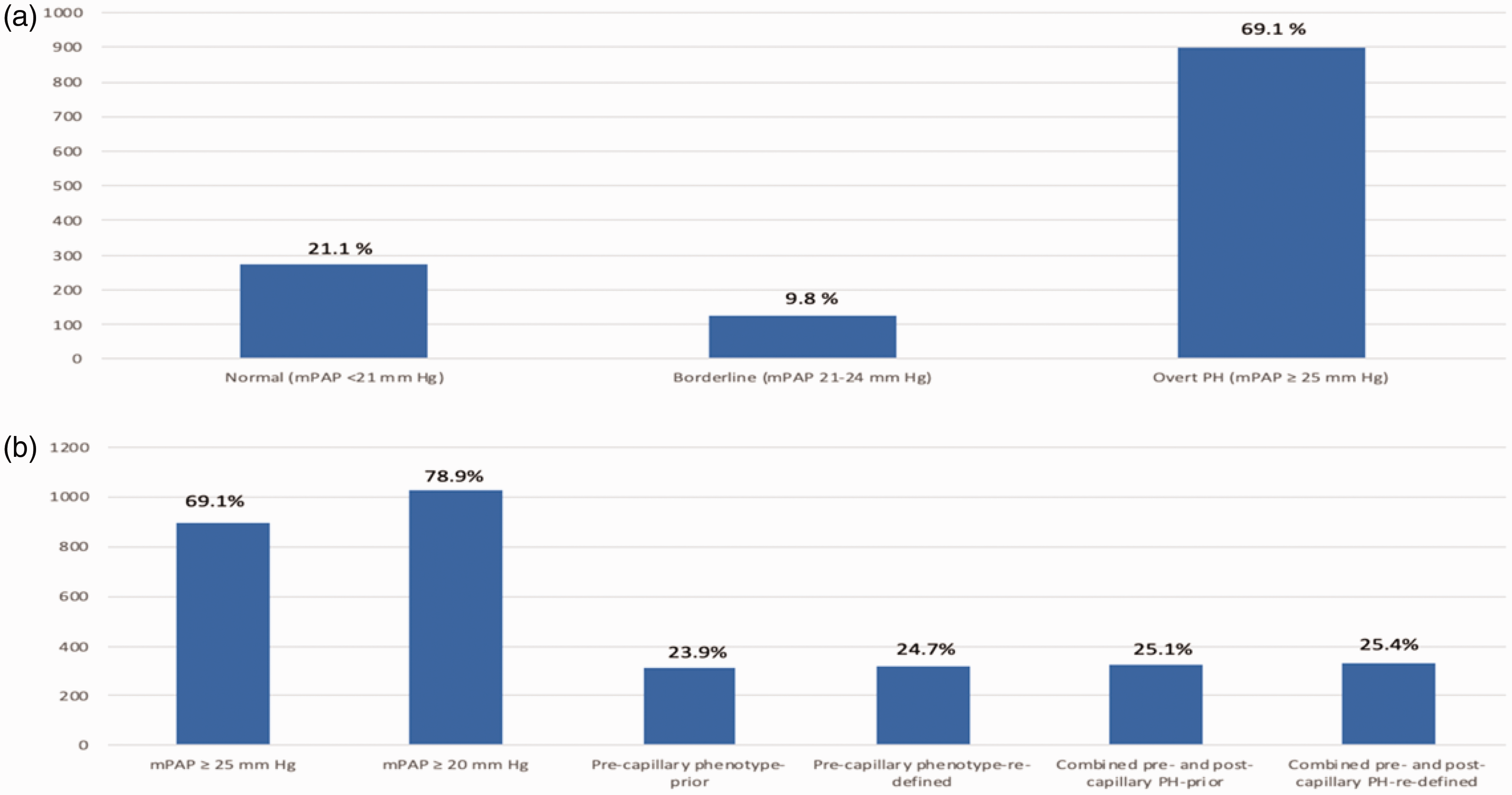
Comparison of basal characteristics, echocardiographic measures, and hemodynamic parameters among three thresholds for mean pulmonary pressure.
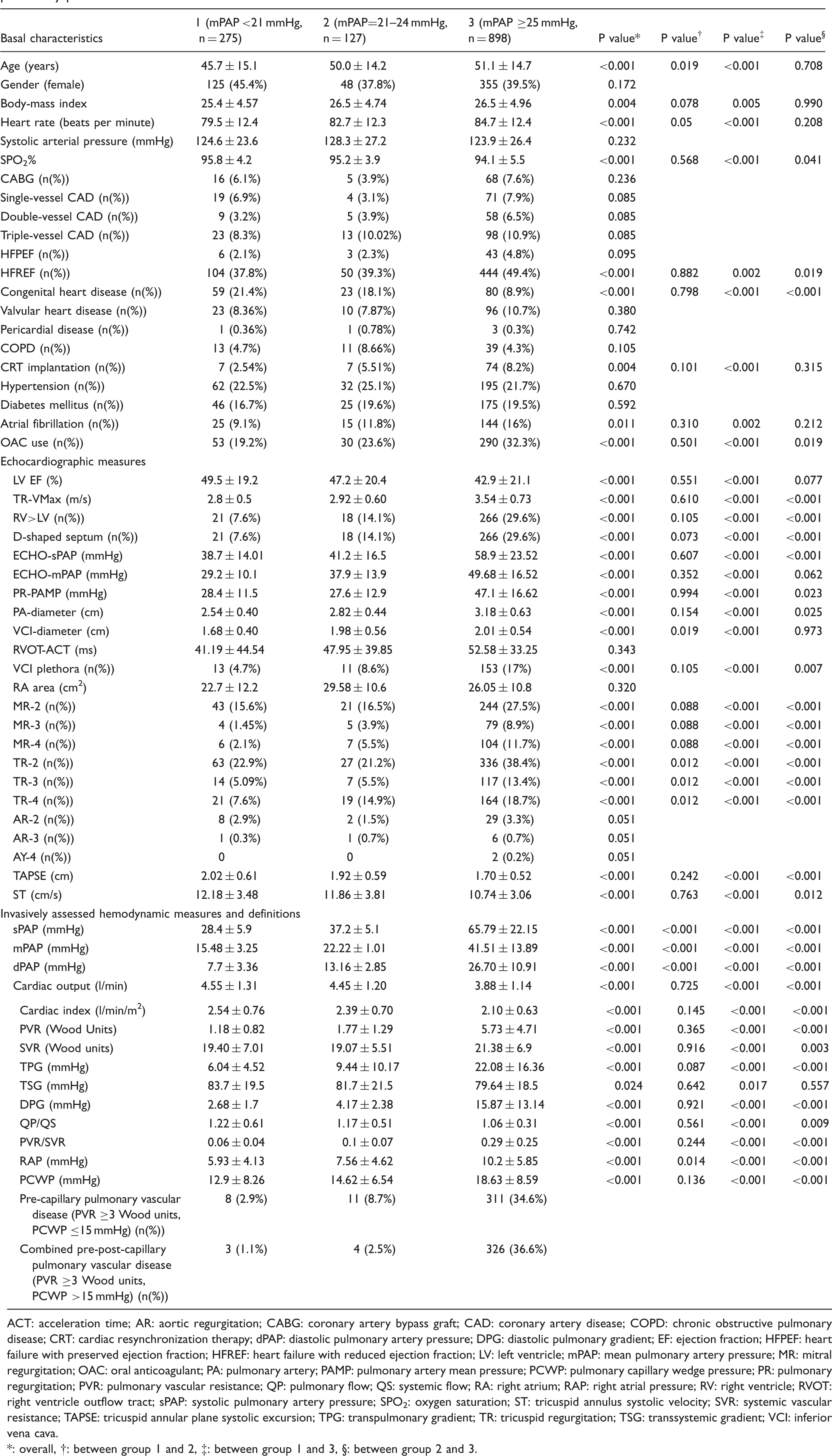
ACT: acceleration time; AR: aortic regurgitation; CABG: coronary artery bypass graft; CAD: coronary artery disease; COPD: chronic obstructive pulmonary disease; CRT: cardiac resynchronization therapy; dPAP: diastolic pulmonary artery pressure; DPG: diastolic pulmonary gradient; EF: ejection fraction; HFPEF: heart failure with preserved ejection fraction; HFREF: heart failure with reduced ejection fraction; LV: left ventricle; mPAP: mean pulmonary artery pressure; MR: mitral regurgitation; OAC: oral anticoagulant; PA: pulmonary artery; PAMP: pulmonary artery mean pressure; PCWP: pulmonary capillary wedge pressure; PR: pulmonary regurgitation; PVR: pulmonary vascular resistance; QP: pulmonary flow; QS: systemic flow; RA: right atrium; RAP: right atrial pressure; RV: right ventricle; RVOT: right ventricle outflow tract; sPAP: systolic pulmonary artery pressure; SPO2: oxygen saturation; ST: tricuspid annulus systolic velocity; SVR: systemic vascular resistance; TAPSE: tricuspid annular plane systolic excursion; TPG: transpulmonary gradient; TR: tricuspid regurgitation; TSG: transsystemic gradient; VCI: inferior vena cava.
*: overall, †: between group 1 and 2, ‡: between group 1 and 3, §: between group 2 and 3.
The echocardiographic data revealed a decrease in left ventricular ejection fraction and increase in the number of measures consistent with severe right ventricular and right atrial pressure overloading, and clinically relevant moderate and severe mitral and tricuspid regurgitation in association with increasing mPAP (Table 1). The step-wise increases in PAWP, diastolic transpulmonary gradient, right atrial pressure, PVR and PVR/SVR ratio, and decrease in cardiac index across the spectrum of mPAP were also statistically significant (Table 1).
The pre-C disease phenotype (PVR ≥3 Wood units and PAWP ≤15 mmHg) and co-pre-post-C PH (PVR ≥3 Wood units and PAWP >15 mmHg) were noted in 2.9 and 1.1%, 8.7 and 2.5%, and 34.6 and 36.6% of the cases in normal and borderline mPAP, and overt PH groups, respectively (Table 1 and Fig. 2a). The re-definition was found to result in a net 9.8% increase in the diagnosis of overall PH, 0.8% increase in the pre-C PH, and 0.3% increase in the co-pre-post-C PH diagnosis (Fig. 2b).
(a) The pre-capillary disease phenotype (PVR ≥3 Wood units and PAWP ≤ 15 mmHg) and co-pre-post-C (PVR ≥3 Wood units and PAWP >15 mmHg) were noted in 2.9 and 1.1%, 8.7 and 2.5%, and 34.6 and 36.6% of the normal and borderline mPAP, and overt PH groups, respectively and (b) the re-definition was found to result in a net 9.8% increase in the diagnosis of overall PH, 0.8% increase in the pre-C PH, and 0.3% increase in the co-pre-post-C PH diagnosis. mPAP: mean pulmonary artery pressure, PH: pulmonary hypertension.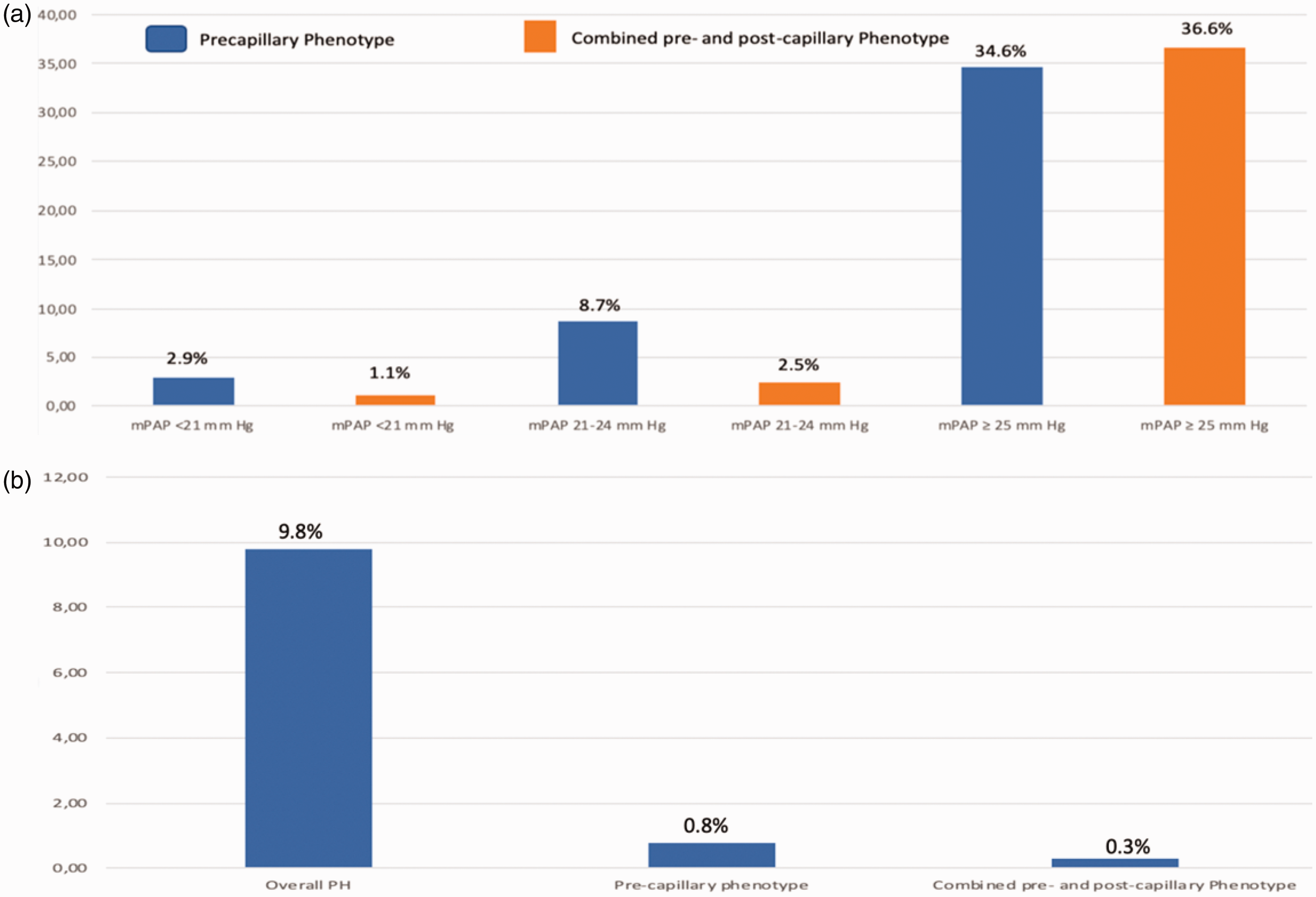
Discussion
Although updated sixth WSPH definition based on mPAP>20 mmHg compared with prior hemodynamic definition as mPAP ≥25 mmHg resulted in a net 9.8% increase in the diagnosis of overall PH, increases in the pre-C PH and co-pre-post-C PH diagnosis were only 0.8 and 0.3%, respectively. More importantly, even in the presence of the mPAP < 21 mmHg, criteria of pre-C and co-pre-post-C phenotypes were still detectable in 2.9 and 1.1% of the patients, respectively.
Although cumulated data suggest a significant relationship between elevations in mPAP and morbidity and mortality irrespective of the pre-C or post-C physiopathologies, the normal range of the mPAP has not been determined until some recent studies.6–14 A systematic review based on healthy individuals from 47 studies in 13 countries revealed that mean mPAP at rest was less than 21 mmHg, two SDs above the normal mean values, regardless of the gender, age, geographical distribution, and supine or upright position. 5 A proposal for the term “borderline PH” to define patients with mPAP of 21–25 mmHg was already made 10 years ago at Dana Point WSPH, but this was not agreed until sixth WSPH.6,14 It has been considered that definitive cut-off value of mPAP ≥25 mmHg was also an arbitrary choice, and lowering it to 20 mmHg as ULN assures a scientific approach.6,14 Furthermore, even mPAP above the 1SD limit (17.3 mmHg) may have prognostic relevance in chronic obstructive pulmonary disease and idiopathic pulmonary fibrosis.6,17,18
In a large longitudinal cohort, borderline PH with mPAP 21–24 mmHg was noted in 18% of the individuals who underwent RHC, and after adjusting for 34 covariates in a Cox proportional hazards model, borderline elevation in mPAP predicted a higher mortality compared with those with normal mPAP, and the this hazard increased incrementally with increasing mPAP, without a threshold. 9 The 61% of these patients with borderline PH had developed overt PH at follow-up RHC, with a median increase in mPAP of 5 mmHg. 9 In a retrospective analysis 7 and a systematic review and meta-analysis, 10 mPAP >19 mmHg was shown to increase the risk of mortality. In a multivariate model considering age and comorbidities, not only overt PH, but also borderline elevations in mPAP were independently associated with a poor survival. 11 On the other hand, only 36% of patients in borderline PH group had a PVR ≥3 Wood units at baseline RHC. These results imply the contributions from post-C physiopathologies in this subset. 11
However, this revised cut-off value of mPAP solely neither characterize a clinical condition, nor define the pathological process per se,6,14 and this rigor is not consistent with the PAWP and PVR remaining unchanged despite the fact that an ULN (above 2SDs) being 12 mmHg for PAWP and 2 Wood units as suggested by some recent studies, 14 Therefore, all three definitive measures of the pulmonary hemodynamics seem to suffer from the gaps between ULN values and those defining pre-C PH. 14 Although the gap related with revised mPAP definition might be considered as a protective buffer zone against premature diagnosis of PH, the gaps in PVR and PAWP values might not serve the same purpose concordantly against overdiagnosis or misclassification of PH in the presence of their unchanged definitive cut-off values. 14 A PVR ≥3 Wood units can still be possible even after a mPAP cut-off reduced to 20 mmHg in cases of low PAWP and cardiac output. Underestimating these technically vulnerable measures may increase PVR and result in misclassification of a patient as having pre-C PH.
The data from the Veterans Affairs Clinical Assessment, Reporting, and Tracking Program might provide important evidence against straightforward mechanistic implications for the causal relationship between mPAP and morbidity or mortality. 7 Individuals have been stratified into the normal (≤18 mmHg), borderline (19–24 mmHg), and overt PH groups according to their mPAP values on RHC. The post-C PH was reported in 78.2% of patients with overt PH, in 22% of individuals with borderline mPAP, and in 2.5% of the individuals with normal mPAP. 7 Moreover, 38.2% of the patients with overt PH, 7.7% of the individuals in borderline group, and even 2.1% of the individuals with normal mPAP had a PVR ≥3 Wood units addressing to pre-C pulmonary vascular disease. 7 In our study confirming these findings, criteria of pre-C phenotype was noted in 34.6% of the patients with overt PH, 8.7% of the patients with borderline mPAP, and even in 2.9% of the patients with normal mPAP while co-pre-post-C PH was noted in 36.6% of the patients with overt PH, 2.5% of the patients with borderline mPAP, and 1.1% of patients with normal mPAP. These PVR data might raise the questions concerning the possibility of significant pulmonary vascular disease even in the presence of the normal mPAPs, and imply the need for more reliable hemodynamic definitions. 7 We noted a step-wise increase either in PAWP and the severity of the pre-C physiopathology marked by higher PVR with increasing mPAP (p<0.001 for both). Incidence of heart failure with reduced ejection fraction, atrial fibrillation, echocardiographic meas-ures of severe right ventricular and right atrial pressure overloading, clinically relevant mitral and tricuspid regurgitation, and utilization rates of oral anticoagulant and cardiac resynchronization therapies were found to be increased in association with increasing mPAP. However, congenital heart disease showed an inverse relation to increasing mPAP while incidence of heart failure with preserved ejection fraction, valvular heart diseases, and chronic obstructive pulmonary disease were comparable among three mPAP subsets.
On the other hand, increased mortality in borderline group, as compared to those in normal mPAP group, was not limited to pre-C PH subset, but was also noted in patients with post-C physiopathology. 7 Whether “borderline PH” defines the severity of underlying pulmonary vascular disease or represents hemodynamic status related to a poor outcome regardless of the pre- or post-capillary physiopathology remains to be determined. 14
A lot of questions raised for gray zone of borderline pre-C PH in patients with scleroderma, family members of hereditary PAH or asymptomatic carriers of gene mutations related with PAH, prevalent systemic to pulmonary congenital shunts, or chronic thromboembolic disease.6,14 Two scleroderma series from same center showed a time-dependent increase (nearly 1.1 mmHg per year) in mPAP with a 17.7% rate of PAH development in this setting.12,13 However, transpulmonary gradient and a high PVR were independent predictors of progression to PH in these series, and transpulmonary gradient ≥11 mmHg in first series, and significant lung disease, but not borderline PH, in second series independently predicted survival.12,13 These results suggest the need for further studies before any re-definition of PH in scleroderma.
The predictive value of the echo screening criteria to identify patients who are potential candidates for RHC needs to be re-evaluated.6,14 The issue whether exercise-induced increase in mPAP could help for closing the gap between borderline and overt PAH in potential risk groups remains to be determined.6,14 Although the revised threshold of mPAP highlights the critical importance of close monitoring in specific risk settings rather than treating all these patients at gray zone, whether this re-definition provides a starting point for earlier initiation of PAH targeted treatments needs to be clarified in prospective trials.6,14 In this kind of newly defined gray zone, no PAH treatment can be justified on the basis of current evidence, despite the willingness of patients and their families to initiate off-label targeted therapies without any delay.6,14,19 Moreover, defining the targets for hemodynamic and clinical benefit from treatments or possibility of spontaneous stabilization along the course of patients with borderline PH remains as another unresolved issue.6,14,19 On the other hand, current standpoint of PH pathologist's view suggests that a clear-cut categorization into pre-C and post-C PH/vascular remodeling appears more and more difficult, and perhaps rather different conditions in
The impact of the mPAP >20 mmHg as definitive threshold was tested in different unpublished cohorts of the Sao Paulo and Giessen series, respectively. 6 The combination of mPAP >20 mmHg with PVR ≥3 Wood units resulted in 2 and 6% increase in the pre-C PH in first and second cohorts, respectively. 6 As given in an editorial, other two unpublished series from Poland and UK also reported pre-C PH in 18.8 and 17.5% of the patients with borderline PH, respectively. 14 We found that mPAP >20 mmHg compared with mPAP ≥25 mmHg cut-off value resulted in net increases of 9.8% in the overall PH diagnosis, but only 0.8 and 0.3% in the pre-C and co-pre-post-C diagnosis. Although the obligatory criterium of PVR ≥3 Wood units seems to keep specificity for discrimination between pre-C versus post-C PH even after lowering the definitive mPAP threshold to 20 mmHg, detection rates of pre-C phenotype in 2.4% and co-pre-post-C in 1.2% of our patients with mPAP ≤20 mmHg seem to suggest that these dichotomizations might be unreliable.
Limitations
The lack of the analysis on prospective follow-up data should be considered as the major limitation of this study. Integrated registry data addressing the sources of the gaps in the evidence, and potential solutions, such as the impact of this re-definition on management algorithms including appropriateness of RHC procedures, timing of targeted therapies in borderline PAH or surgical endarterectomy in chronic thromboembolic disease, and benefit from these goal-oriented strategies across the different settings and ages seem to be required.
In conclusion, the re-definition of mPAP threshold seems to increase the frequency of the overall PH diagnosis which is mainly originated from those in post-C PH subgroup whereas its impact on pre-C and co-pre-post-C PH was negligible. The obligatory criterium of PVR ≥3 Wood units seems to keep specificity for discrimination between pre-C versus post-C PH after lowering the definitive mPAP threshold to 20 mmHg.
The detection rates of pre-C disease and co-pre-post-C phenotypes even in patients with normal mPAP seem to imply the need for reappraisal of currently used arbitrary thresholds of hemodynamic measures definitive for these phenotypes.
