Abstract
Pulmonary arterial hypertension (PAH) is a type of pulmonary hypertension that is a progressive, fatal disease. Multiple underlying mechanisms for PAH have been identified, including vasoconstriction, intimal proliferation, medial hypertrophy, inflammation, mitochondrial dysfunction, and in situ thrombosis. Because it is an uncommon disease, it has been challenging to identify a specific treatment that targets the dominant disease mechanism in a given patient. Early success demonstrating that some patients (approximately 10%) possess pulmonary vasoreactivity at diagnosis has driven the development of pulmonary vasodilators as the mainstay of treatment. However, while they improve exercise tolerance in clinical trials, their effect on survival is limited. Therapies that target underlying disease mechanisms that affect a majority of patients are clearly needed if we are to significantly improve overall survival.
In the actual guidelines, chronic anticoagulation is no longer recommended in patients with idiopathic, hereditary, and drug-induced PAH although there is much indirect evidence for this.
There are data from over 40 years which include: (1) pathology studies showing the presence of thrombotic lesions in a majority of patients with PAH, both idiopathic and associated with many other conditions; (2) a similar frequency of thrombotic lesions in patients treated with pulmonary vasodilators as was seen in the years before their use; (3) mechanistic studies showing that procoagulant conditions predispose to the development of intraluminal thrombosis that contributes to vascular remodeling and the progressive nature of the pathologic changes; and (4) observational studies that, with one exception, have demonstrated a substantial survival advantage in patients with PAH treated with oral anticoagulation.
Acknowledging that no prospective randomized trial with anticoagulants has ever been done, we recommend a pragmatic approach to the use of anticoagulants in PAH. We suggest that the risks and benefits of chronic anticoagulation be considered in individual patients, and that warfarin be prescribed in patients with PAH, unless they have an increased risk of bleeding.
The question of whether direct oral anticoagulants (DOACs) would provide the same benefit as vitamin K antagonists is valid, but presently there are no data at all regarding their use in PAH. However, in patients with PAH in whom warfarin anticoagulation management proves problematic, it is reasonable to switch the patient to a DOAC as is current practice for other conditions.
Introduction
Pulmonary arterial hypertension (PAH) is a type of pulmonary hypertension (PH) that is a progressive, fatal disease. Multiple underlying mechanisms for PAH have been identified, including vasoconstriction, intimal proliferation, medial hypertrophy, inflammation, mitochondrial dysfunction, and in situ thrombosis. Because it is an uncommon disease, it has been challenging to identify a specific treatment that targets the dominant disease mechanism in a given patient. Early success demonstrating that some patients (approximately 10%) possess pulmonary vasoreactivity at diagnosis has driven the development of pulmonary vasodilators as the mainstay of treatment. However, while they improve exercise tolerance in clinical trials, their effect on survival is limited. Therapies that target underlying disease mechanisms that affect a majority of patients are clearly needed if we are to significantly improve overall survival.
In contrast, chronic thromboembolic pulmonary hypertension (CTEPH) is a type of PH that can mimic PAH, but one where the disease mechanism, pulmonary vascular thrombosis, is known. Life-long anticoagulation is an undisputed treatment even though there have never been randomized clinical trials proving that anticoagulation improves outcomes. Interestingly, pathologic, functional, and molecular studies have shown that IPAH and CTEPH have many features in common, and anticoagulation has been previously recommended for both diseases, aside from different international normalized ratio (INR) target values.
The presence of pulmonary vascular thrombosis in PAH
Anticoagulation has been recommended to treat PAH in the era before the use of pulmonary vasodilators. 1 Early justification came from several pathology studies in patients with PAH showing widespread evidence of intraluminal thrombosis. Intimal fibrosis has a more prominent role than medial and adventitial hypertrophy in the luminal obstruction. 2 The large series by Wagenvoort from 1970 noted in situ thrombosis a likely mechanism in many patients. The commonly found eccentric intimal fibrosis lesions are believed to represent organized intraluminal thrombus. 3
The definitive pathology study describing idiopathic PAH (IPAH) came from the pathology sub-study of the NIH PPH Registry, 4 which showed that 33% of patients with IPAH had thrombotic lesions. In addition, eccentric intimal fibrosis was seen in the majority of patients. A more recent systematic comparison of intimal lesions from patients with CTEPH and IPAH found that these lesions have the same cell composition and arrangement. The major difference was that CTEPH involved larger vessels, whereas the size of the affected vessels was considerably smaller in IPAH. 5
The classification of PAH from 1998 now has several subgroups, which have similarities and differences. However, from pathology studies, patients with IPAH, hereditary PAH, drug- and toxin-associated PAH (I/H/DPAH), congenital heart disease-associated PAH, pulmonary veno-occlusive disease, and pulmonary capillary hemangiomatosis all have evidence of widespread pulmonary vascular thrombosis.
Thrombosis and pulmonary vascular remodeling
In IPAH, mechanistic studies have implicated arterial thrombosis as being involved in the development of intimal fibrosis and progression of the pulmonary vascular disease. A procoagulant state exists in patients with IPAH. One study reported that the increase in t-PA that is normally found after venous occlusion in controls was severely decreased and almost blunted in patients with CTEPH and IPAH, 6 suggesting that patients with IPAH and CTEPH had a comparable prothrombotic state. In addition to the procoagulant changes, fibrinolytic activity is diminished in IPAH.7,8
Hassoun et al. showed that heparin had anti-remodeling effects in animal models of PH, 9 which could be explained by its specific antiproliferative effects on pulmonary arterial smooth muscle cells (PASMCs). 10 Eisenberg et al. showed markedly elevated fibrinopeptide A levels, indicative of increased activity of the coagulation product thrombin, in patients with severe IPAH. 11 Yuan et al. found that thrombin causes a strong proliferative response in PASMCs from patients with both CTEPH and IPAH but not from normal controls, and that the response depends on mTOR activation and calcium influx into the cells, mediated by thrombin. 12 The conclusion from all of these findings is that thrombin plays a major role in the genesis of both CTEPH and IPAH.
As depicted in Fig. 1, thrombin has a number of effects beyond fibrin formation which are mediated by its specific target Protease-Activated Receptor (PAR)-1. 13 Many cells such as thrombocytes, fibroblasts, and smooth muscle cells express PAR1, and its cleavage by thrombin causes activation of thrombocytes,14,15 activation of rho kinase, 16 activation of phospholipase C, 17 inhibition of adenylyl cyclase, and activation of Protein Gßγ 18 and PI3 kinase 19 in smooth muscle cells, all resulting in vasoconstriction. Of importance, thrombin also increases permeability and migration in endothelial cells 20 and causes transition of fibroblasts into myofibroblasts, 21 known for their extensive production of matrix proteins such as collagen 18.
The cleavage product of collagen 18, endostatin, is massively overexpressed in the intimal fibrosis of pulmonary arteries in PAH patients 2 and may even serve as a biomarker for collagen 18 deposition and a bad prognosis. 22 The effects of thrombin might also account for cardiac fibrosis in heart failure23,24 and atrial fibrillation. 25
Survival advantage with anticoagulation
Multiple observational studies have reported a survival advantage in those patients receiving vitamin K antagonists, mostly warfarin or phenprocoumon. The impact of anticoagulation in appetite suppressant-induced and IPAH was acknowledged from a retrospective assessment of the Austrian experience with aminorex-induced PAH (DPAH) and IPAH which showed a significant improvement in survival and quality of life in patients treated with anticoagulation compared to those who were not.26,27
A similar observation was made from a retrospective review of patients with PAH seen at the Mayo Clinic over several decades which demonstrated that patients treated with warfarin had better survival than those who were not. 28 Autopsies showed the frequent presence (57%) of thrombotic lesions in the patients who died. In 1992, the only prospective study of anticoagulation validated the improvement in survival in patients with IPAH who were treated with warfarin compared to those who were not. 29
Based on the totality of information from all of these studies, including pathology studies demonstrating widespread thrombotic lesions, coagulation studies showing the procoagulant state in PAH, and observational studies consistently showing a survival advantage in patients with PAH treated with warfarin, global treatment guidelines for PAH recommended the use of vitamin K antagonists.
The current treatment era
It is reasonable to ask whether the survival advantage from anticoagulation in the era before the use of pulmonary vasodilators remains. One might speculate that pulmonary vasodilators may in some way diminish the procoagulant state via their effects on the pulmonary vascular endothelium. If this is the case, one would expect to find fewer thrombotic lesions on pathology and the loss of survival advantages from recent observational studies.
The most authoritative pathology study of PAH in the current treatment era is from the Pulmonary Hypertension Breakthrough Initiative which detected thrombi (recent and old) in 50% of PAH lungs. 30 All of the patients were treated with multiple pulmonary vasodilators. Of the patients with thrombi, 42% received anticoagulation, whereas in the patients without thrombi, 68% were anticoagulated. Thus, the presence of thrombotic lesions does not seem to be diminished by the use of pulmonary vasodilators, but by the use of warfarin.
Two large recent observational studies again looked at the influence of anticoagulation in PAH. When IPAH patients from the COMPERA registry (2007–2013) with and without anticoagulation were compared, there was a significant survival benefit for the anticoagulated patients. Even a matched-pair analysis, correcting for disease severity and other confounding factors, confirmed this conclusion. 31
The REVEAL registry (2006–2009) was the first study to report a lack of benefit of anticoagulation. 32 This was based on an analysis of four sub-groups within the registry, representing approximately 20% of the patients. These included: IPAH, never on warfarin but started after enrollment, versus IPAH, never on warfarin and no warfarin after enrollment; and SSc-PAH, never on warfarin but started after enrollment versus SSc-PAH, never on warfarin and no warfarin after enrollment. When the effects of warfarin on survival between the groups were compared, the IPAH patients showed no significant difference in survival (P = 0.17) and the scleroderma patients showed a significant survival disadvantage for the warfarin group (P = 0.03). However, unlike the COMPERA registry, there was a noticeable imbalance between the groups regarding baseline characteristics of disease severity, with the anticoagulated patients having features of more severe disease than the ones who were not.
Conclusions
We believe that chronic anticoagulation is still warranted in patients with PAH, based on the totality of available data from over 40 years which includes: (1) pathology studies showing the presence of thrombotic lesions in a majority of patients with PAH, both idiopathic and associated with many other conditions; (2) a similar frequency of thrombotic lesions in patients treated with pulmonary vasodilators as was seen in the years before their use; (3) mechanistic studies showing that procoagulant conditions predispose to the development of intraluminal thrombosis that contributes to vascular remodeling and the progressive nature of the pathologic changes; and (4) observational studies that, with one exception, have demonstrated a substantial survival advantage in patients with PAH treated with oral anticoagulation.
Acknowledging that no prospective randomized trial with anticoagulants has ever been done, we recommend a pragmatic approach to the use of anticoagulants in PAH. We suggest that the risks and benefits of chronic anticoagulation be considered in individual patients and that warfarin be prescribed in patients with PAH, unless they have an increased risk of bleeding. Since the ideal INR target value is unknown, it seems reasonable to use the same range that is used in preventing venous thromboembolism, a range of 2.0–3.0.
In patients who are anticoagulated, we suggest that it is not necessary to bridge them with heparin before invasive or surgical procedures, but to discontinue the anticoagulant 5–10 days before the procedure and restart it after all related risks of bleeding have resolved.
The question of whether direct oral anticoagulants (DOACs) would provide the same benefit as vitamin K antagonists is valid, but presently there are no data at all regarding their use in PAH. However, in patients with PAH in whom warfarin anticoagulation management proves problematic, it is reasonable to switch the patient to a DOAC as is current practice for other conditions.
In situ thrombosis and eccentric intimal fibrosis in PAH. In PAH patients, systemic factors such as low cardiac output and dilated central veins, right atrium (RA), right ventricle (RV), and pulmonary arteries (PA) cause blood stasis and increase the thrombosis risk. Chronic intravenous catheters or other devices represent an additional risk factor. The thrombosis risk is further increased by a disbalance between fibrinolytic and thrombotic capacity. There are reduced levels of tissue plasminogen activator (t-PA) while increased thrombin activity, indicated by increased fibrinopeptide A levels, causes increased thrombosis formation. Thrombin, by cleaving the protease activating receptor (PAR)-1 of different target cells has additional effects: thrombocytes become activated, fibroblasts are turned into matrix-secreting myofibroblasts, and smooth muscle cells are constricted by activation of rho kinase (ROKK) and IP3. Independent of PAR-1, inhibition of adenylyl cyclase (AC) and potassium channels (IK) add to the vasoconstrictive effects. In addition, thrombin activates the mechanistic Target of Rapamycin (m-Tor) causing calcium influx and proliferation. The cleavage product of collagen 18 (col18), endostatin, is deposited in the intimal fibrosis but is also found at an elevated level in the circulation of PAH patients where it represents as a marker of a poor prognosis (for references, see text).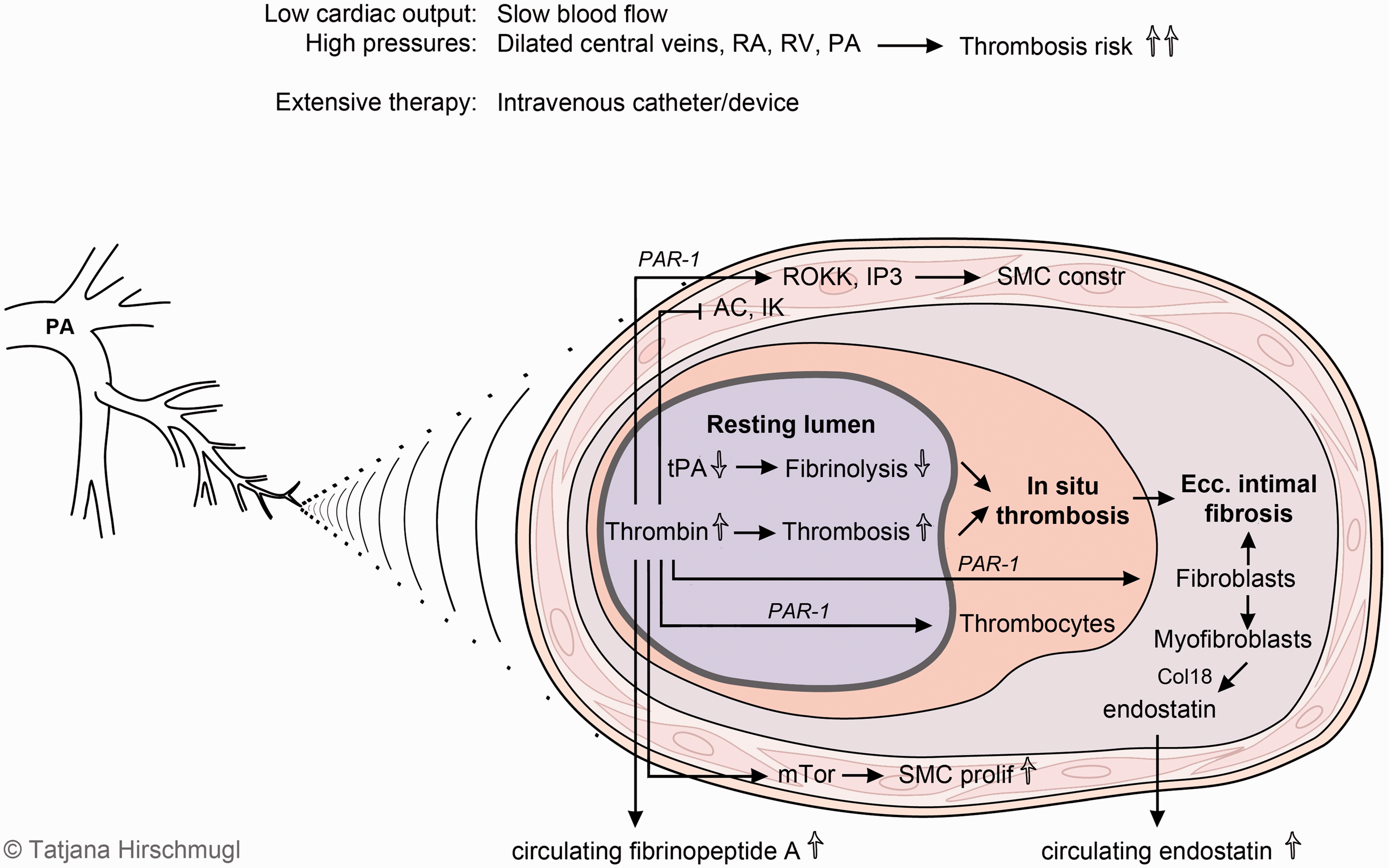
Footnotes
Acknowledgements
The authors thank PD Grazyna Kwapiszewska, PhD, for her scientific input and discussion and Prof. Dr. Johannes Mlczoch for his support.
Conflict of interest
The author(s) declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
