Abstract
Objective
To evaluate the prognostic value of baseline neutrophil-to-lymphocyte ratio (NLR) in the prediction of long-term mortality in patients with pulmonary arterial hypertension (PAH).
Methods
This prospective study recorded NLR during initial diagnostic right-sided cardiac catheterization in adult patients with PAH. Demographic, clinical, laboratory and haemodynamic variables were compared by NLR tertile. Univariate and multivariate Cox regression analyses were used to determine whether NLR was independently associated with mortality.
Results
Adults with PAH (n = 101) were followed-up for mean ± SD 36.8 ± 23.6 months. The number of deaths, New York Heart Association functional capacity (NYHA FC), levels of brain natriuretic peptide (BNP) or C-reactive protein (CRP) and presence of pericardial effusion increased as the NLR tertile increased, but haemoglobin and tricuspid plane annular systolic excursion (TAPSE) decreased. On univariate analysis, high NLR values were associated with mortality, but on multivariate analysis, NLR did not remain an independent predictor of mortality. Baseline NYHA FC, TAPSE, BNP level and pericardial effusion were independent predictors of mortality.
Conclusions
NLR was correlated with important prognostic markers in PAH such as NYHA FC, BNP and TAPSE. This simple marker may be useful in the assessment of disease severity in patients with PAH.
Introduction
Pulmonary arterial hypertension (PAH) is a relatively rare condition, often accompanied by a poor outcome due to right heart failure. 1 The median survival period of patients with idiopathic PAH (IPAH) was 2.8 years in the initial reports from a national US prospective registry. 2 In the past two decades, survival has improved as treatment options have increased. 3 Data from the US REVEAL registry suggest that the current median survival is 7 years for patients with any form of PAH. 4
Identifying clinically-relevant prognostic predictors has been a key goal for clinicians involved in the care of patients with PAH. Several prognostic models have been investigated by the large disease registries. For example, the latest update from the 5th PAH World Symposium (held in Nice, France, in 2013) outlined the multivariate predictors of survival as follows: male sex, age > 65 years, PAH secondary to connective tissue disease, high New York Heart Association functional class (NYHA FC), low 6-min walking distance (6MWD), high levels of brain natriuretic peptide (BNP) or the N-terminal of the prohormone brain natriuretic peptide, high creatinine levels, presence of pericardial effusion on echocardiography, low diffusing capacity of the lung for carbon monoxide (DLCO), high right atrial pressure (RAP), low cardiac output (CO) and high pulmonary vascular resistance (PVR). 5 Research has also identified several biomarkers to be prognostic predictors in PAH, including levels of bilirubin, platelets, uric acid, troponin or C-reactive protein (CRP, and red cell distribution width. 6
Inflammation has long been recognized as an important pathogenic element in PAH. 7 Stacher et al. 8 reported the accumulation of inflammatory cells in PAH for the first time in 2012. In this study, the amount of perivascular inflammatory infiltrate correlated with parameters of pulmonary vascular remodelling and haemodynamics in PAH. 8 Among several inflammatory markers, neutrophil-to-lymphocyte ratio (NLR) is a simple and popular marker, which has been shown to be correlated with the prognosis of several disease states in cardiology including heart failure (HF), acute myocardial infarction (AMI), coronary artery disease (CAD), infective endocarditis and acute pulmonary embolism.9–13 One study showed for the first time that the NLR was significantly increased in patients with PAH compared with control subjects. 14 To our knowledge, NLR has not been studied in terms of patient prognosis in PAH. This present study therefore evaluated the prognostic value of baseline NLR in patients with PAH.
Patients and methods
Patients
Consecutive adult patients with definitive PAH who attended the PAH Clinic, Department of Cardiology, School of Medicine, Dokuz Eylul University, Izmir, Turkey between January 2008 and June 2014, were prospectively screened for inclusion in this prospective study. All patients met the diagnostic criteria for the definitive diagnosis of PAH. 15 The Dokuz Eylul University Ethics Committee approved the study protocol (no. 2138-GOA). Verbal informed consent was obtained from all of the study participants. Patients with overt infectious disease at the time of PAH diagnosis (i.e. at the beginning of the screening process) were excluded from the study.
Data collection and patient survival
Baseline evaluation of the patients included the following: NYHA FC assessment, 16 transthoracic echocardiography (TTE), routine laboratory tests, BNP, 6MWD, echocardiogram, and right-heart catheterization (RHC). BNP was measured using a chemiluminescence microparticle immunometric method (ARCHITECT c4000 Clinical Chemistry Analyser; Abbott Laboratories, Abbott Park, IL, USA). A Beckman Coulter LH 780 Haematology Analyser (Beckman Coulter, Brea, CA, USA) was used to undertake the haematological analysis, which was used to determine the baseline NLR for each patient at hospital admission. For haematological analysis, a sample (3 ml) of venous blood was collected from each patient in tubes containing 6% ethylenediaminetetra-acetic acid; samples were stored at room temperature for 20–25 min before analysis. Blood analyses undertaken during the diagnostic RHC were recorded as baseline biochemical data. RHC was performed at rest, without sedation, by an experienced cardiologist (B.A.). Measurements of pulmonary artery pressure (PAP), RAP and wedged PAP were taken at end-expiration. CO was measured by an indirect Fick method with an assumed O2 consumption of the patient. 17 Cardiac index (CI) was calculated as CO divided by body surface area. Pulmonary vascular resistance was calculated as mean PAP minus left atrial pressure divided by CO. The survival period was calculated as the number of months from initial diagnosis to June 2014, which was the end of the follow-up period in this study, or to patient death if that occurred first.
Two-dimensional Doppler echocardiography
All patients had a comprehensive two-dimensional Doppler echocardiography examination with a special focus on right heart functions and pressures. Echocardiograms were performed by two experienced cardiologists (B.A. and E.Ö.) using a Philips HD11 XE ultrasound system with a 3.2 MHz transducer (Philips Healthcare, Best, the Netherlands). The following parameters were measured during TTE: systolic PAP, right ventricular (RV) end-diastolic diameter, right atrial area, maximum systolic velocity of pulmonary outflow jet, tricuspid plane annular systolic excursion (TAPSE), RV tissue Doppler systolic velocity, RV fractional area change (RFAC) and RV Tei index. 18 RFAC was calculated as RV end diastolic area (RVEDA) minus RV end systolic area divided by RVEDA, in which measurements were obtained from the apical four-chamber view. At the apical four-chamber view, M-mode recording of the long axis was taken from the lateral side of the tricuspid annulus. The maximal distance of endocardial motion during the systolic phase was defined as TAPSE. The tissue Doppler imaging was used to obtain RV velocities in the apical four-chamber view with a 2-mm sample volume placed at the lateral segment of the tricuspid annulus during early diastole and systole. The isovolumetric contraction time (IVCT) and isovolumetric relaxation time (IVRT) were measured from the end of the tricuspid annular velocity pattern to the onset of the systolic wave, and from the end of the systolic wave to the onset of the tricuspid annular velocity pattern, respectively. The ejection time (ET) was defined as the duration of the systolic wave. The RV Tei index was calculated according to the formula: Tei index = (IVCT + IVRT)/ET. Using the modified Bernoulli equation, an estimate of the RAP is added to the peak systolic gradient of the tricuspid regurgitant jet to approximate systolic PAP (sPAP) in the absence of pulmonary valve stenosis. The presence of pericardial effusion during TTE was also noted.
Patients were followed-up periodically at 3-month intervals. Follow-up visits included a physical examination, NYHA FC assessment, BNP testing, 6MWD, routine laboratory testing and comprehensive TTE. Based on the NLR upon admission, patients were stratified into tertiles: 1st tertile: ≤ 2.2; 2nd tertile: 2.3–3.5; and 3rd tertile: ≥ 3.6.
Statistical analyses
All statistical analyses were performed using the SPSS® statistical package, version 15.0 (SPSS Inc., Chicago, IL, USA) for Windows®. To test the distribution pattern, the Kolmogorov–Smirnov method was used. Data are summarized as the mean ± SD, median (minimum, maximum), or n of patients (%). Analysis of variance was used to compare data between the tertiles displaying normal distribution. Kruskal–Wallis test was applied to compare the data without normal distribution between the tertiles. Mann–Whitney U-test was used to compare the data without normal distribution between patients who had died and patients who had survived during follow-up. Categorical parameters were compared with χ2-test. Spearman's rank correlation coefficient analysis was used to analyse the correlation between numeric variables. The effects of different parameters on clinical outcomes were calculated by univariate analysis for each. Parameters for which the unadjusted P-value was <0.10 in the univariate analysis were identified as potential risk markers, and were included in the multivariate Cox logistic regression model. A P-value ≤0.05 was considered to be statistically significant.
Results
Comparison of baseline demographic, clinical and laboratory parameters in adult patients with pulmonary artery hypertension (n = 101), stratified according to baseline neutrophil-to-lymphocyte ratio (NLR) tertiles.
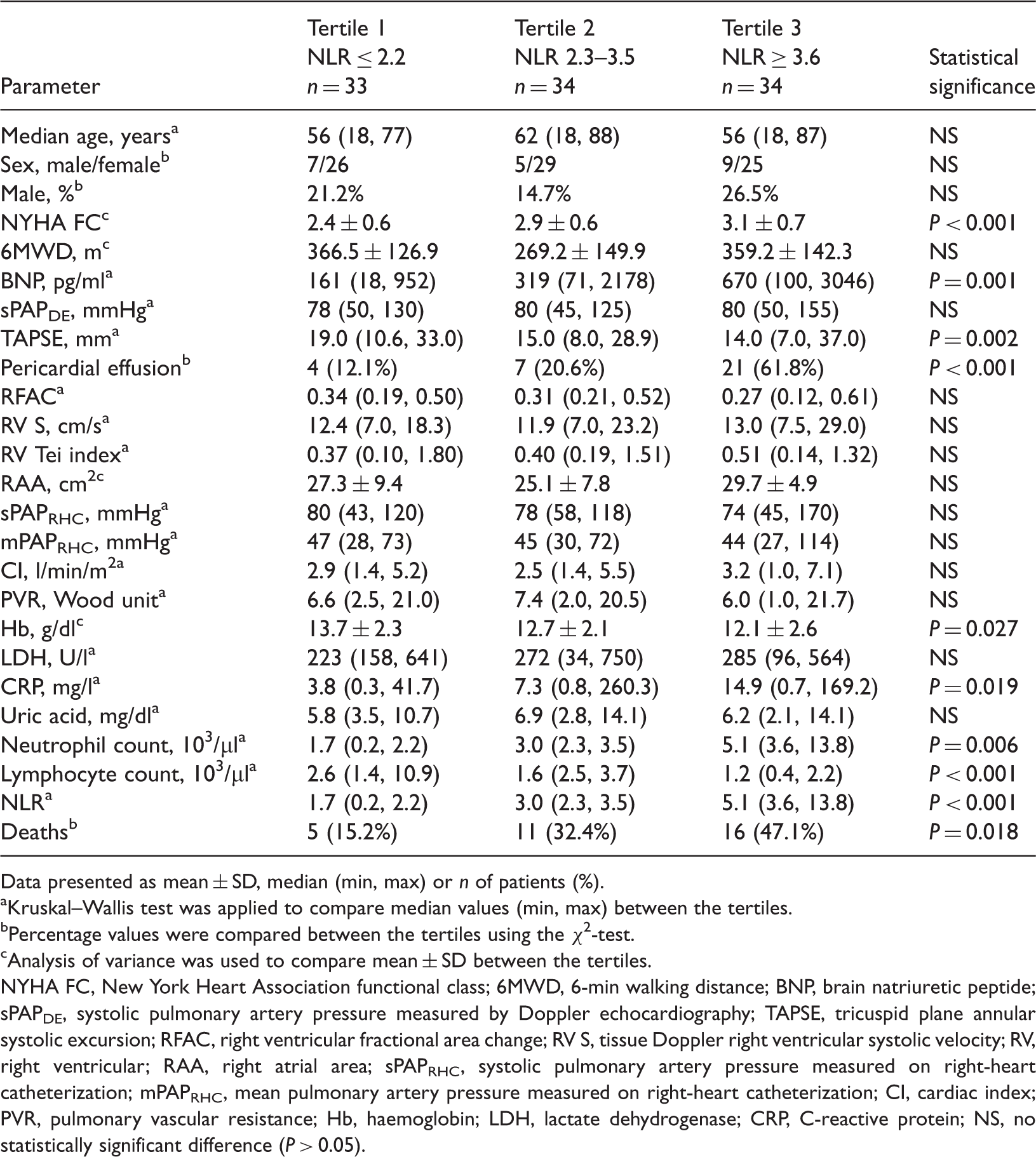
Data presented as mean ± SD, median (min, max) or n of patients (%).
Kruskal–Wallis test was applied to compare median values (min, max) between the tertiles.
Percentage values were compared between the tertiles using the χ2-test.
Analysis of variance was used to compare mean ± SD between the tertiles.
NYHA FC, New York Heart Association functional class; 6MWD, 6-min walking distance; BNP, brain natriuretic peptide; sPAPDE, systolic pulmonary artery pressure measured by Doppler echocardiography; TAPSE, tricuspid plane annular systolic excursion; RFAC, right ventricular fractional area change; RV S, tissue Doppler right ventricular systolic velocity; RV, right ventricular; RAA, right atrial area; sPAPRHC, systolic pulmonary artery pressure measured on right-heart catheterization; mPAPRHC, mean pulmonary artery pressure measured on right-heart catheterization; CI, cardiac index; PVR, pulmonary vascular resistance; Hb, haemoglobin; LDH, lactate dehydrogenase; CRP, C-reactive protein; NS, no statistically significant difference (P > 0.05).
A higher prevalence of pericardial effusion was observed as the NLR tertile increased (P < 0.001 for trend across the three NLR tertiles). Among the RV echocardiographic parameters, only TAPSE differed significantly across the tertiles, with TAPSE being lower with increasing NLR tertile (P = 0.002).
Right-heart catheterization parameters were similar among the three NLR tertiles, including systolic pulmonary artery pressure measured on right-heart catheterization (sPAPRHC), mean pulmonary artery pressure measured on right-heart catheterization (mPAPRHC), PVR and CI. Among the biochemical parameters, BNP levels were significantly higher (P = 0.001) and haemoglobin levels were significantly lower with increasing NLR tertile (P = 0.027). The CRP level significantly increased as the NLR tertile increased (P = 0.019). There was a significant correlation between CRP and NLR (r = 0.702, P < 0.001; Spearman's rank correlation coefficient analysis).
A total of 32 deaths occurred during the study period, the majority (n = 30) of which were confirmed to be related to worsening right heart failure; for the remaining two patients, cause of death was undetermined from the relatives. When patients were stratified into two groups according to the occurrence of death, those who had died had a significantly higher median NLR value (3.9 versus 2.7, respectively; P = 0.003), higher median neutrophil counts (6.8 versus 5.0 × 103/µl, respectively; P = 0.001) and similar median lymphocyte counts (1.4 versus 1.8 × 103/µl, respectively) compared with those who survived (Figure 1).
Comparison of neutrophil-to-lymphocyte ratio (NLR), neutrophil count (×103/µl) and lymphocyte count (×103/µl) between adult patients with pulmonary artery hypertension who died and those who survived during follow-up. *P = 0.003, †P = 0.001 for patients who died compared with those who survived; Mann–Whitney U-test.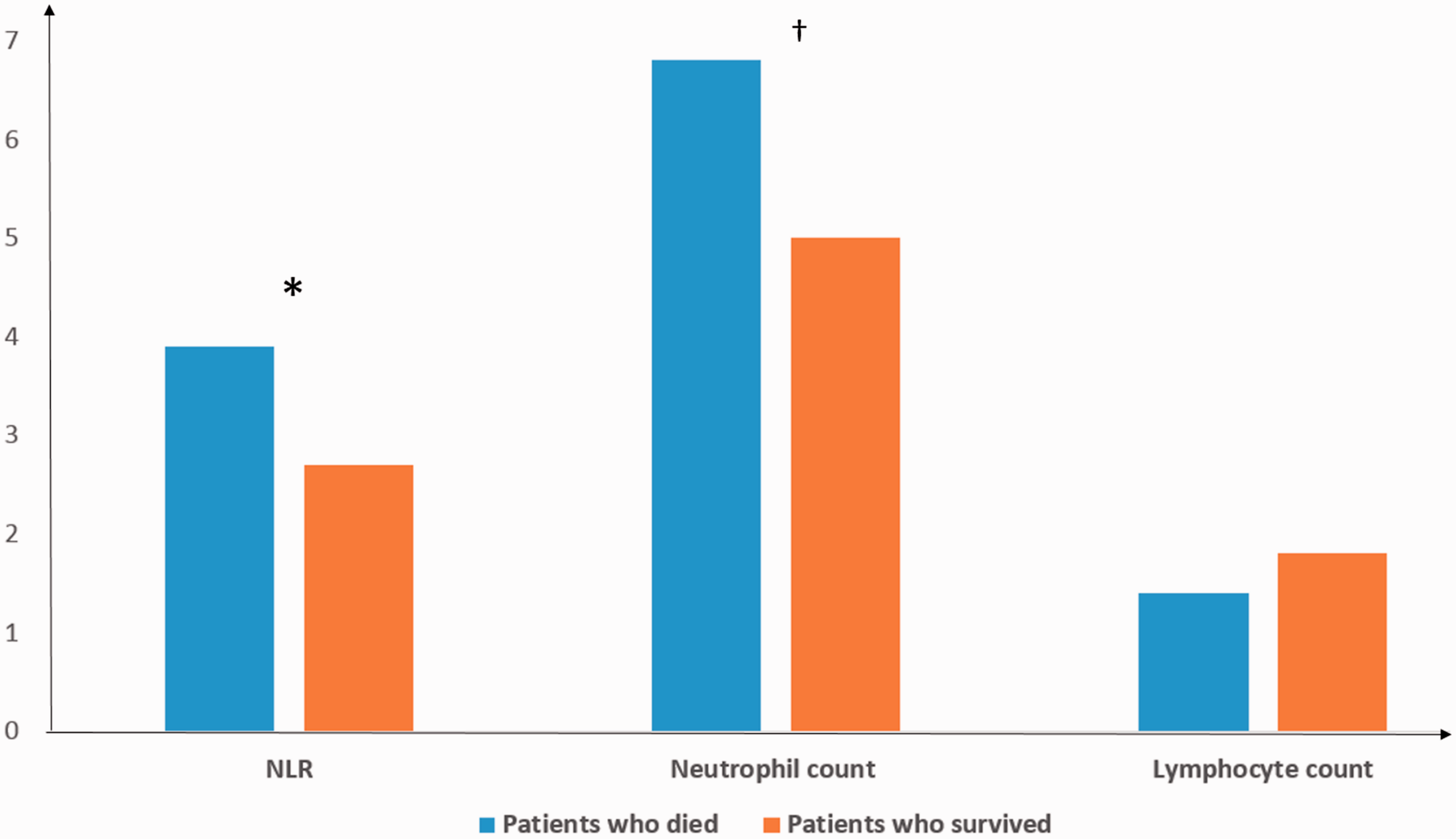
Univariate and multivariate analyses of the effects of multiple baseline parameters on long-term mortality in adult patients with pulmonary artery hypertension (n = 101).
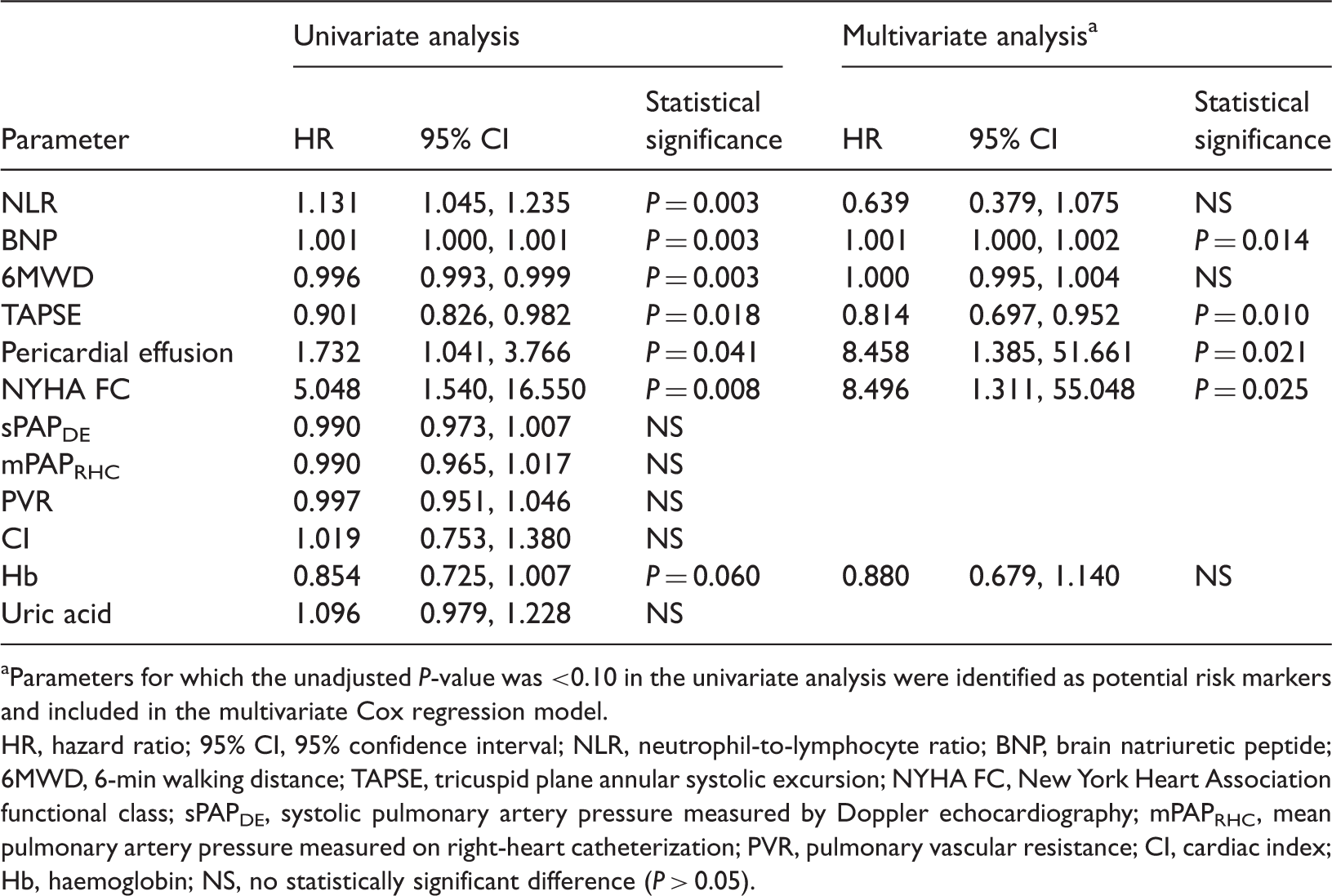
Parameters for which the unadjusted P-value was <0.10 in the univariate analysis were identified as potential risk markers and included in the multivariate Cox regression model.
HR, hazard ratio; 95% CI, 95% confidence interval; NLR, neutrophil-to-lymphocyte ratio; BNP, brain natriuretic peptide; 6MWD, 6-min walking distance; TAPSE, tricuspid plane annular systolic excursion; NYHA FC, New York Heart Association functional class; sPAPDE, systolic pulmonary artery pressure measured by Doppler echocardiography; mPAPRHC, mean pulmonary artery pressure measured on right-heart catheterization; PVR, pulmonary vascular resistance; CI, cardiac index; Hb, haemoglobin; NS, no statistically significant difference (P > 0.05).
Spearman's rank correlation coefficient analysis demonstrated that baseline NLR was significantly correlated with NYHA FC (r = 0.421, P < 0.001), BNP (r = 0.362, P < 0.001), and TAPSE (r = −0.275, P = 0.007). Echocardiographic parameters (other than TAPSE), right-heart catheterization parameters and 6MWD were not correlated with baseline NLR.
Discussion
This present study investigated the value of baseline NLR in the prediction of mortality in patients with PAH. These present results showed that although NLR was a significant predictor of long-term mortality in the univariate analysis, the multivariate Cox logistic regression analysis did not support its significance in the prediction of long-term mortality. Baseline NLR was significantly correlated with baseline NYHA FC, BNP and TAPSE of patients with PAH. In this present study, independent predictors of long-term mortality were baseline NYHA FC, TAPSE, BNP and presence of pericardial effusion on echocardiography. Significant correlations between the baseline NLR and these well-known prognostic factors limited its value as an independent predictor of death in patients with PAH. However, these results suggest that NLR may be useful in the assessment of disease severity in patients with PAH.
The prognostic value of NLR has been studied in many disease states including AMI, CAD, HF, infective endocarditis, acute pulmonary embolism, type 2 diabetes mellitus and several cancers.9–13,19–22 This present study was the first to investigate the prognostic role of baseline NLR in patients with PAH. Inflammation has been long recognized as an important pathogenic element in PAH. 7 It has become increasingly clear that early and persistent inflammation is present and contributes to pulmonary vascular disease, as documented in tissue-based studies and in studies of circulating inflammatory cells and chemical mediators.23–25 A wide range of cytokines has been shown to be elevated and to correlate with survival in PAH; such cytokines include interleukin-6, monocyte chemoattractant protein-1, tumour necrosis factor-α, transforming growth factor-β and 5-hydroxytryptophan. 26 At the tissue level, traditional cellular components of inflammation are described in the hypertensive pulmonary circulation. 27 The cells involved have been shown to be mostly T cells, macrophages, and, to a lesser extent, B cells. 27 Although T cell infiltrates are increased in patients with IPAH, it appears that there is a decrease in CD8+ cytotoxic T cells and an increase in regulatory T cells. 27 Regulatory T cells are now believed to play a pivotal role in the development of PAH. 28 Although T cells have been one of the major points of focus in PAH pathophysiology, little is known about the role of neutrophils in PAH development. 29 Neutrophils are the most abundant white blood cells; they release various enzymes and cytokines, and activate other cells of the immune system to trigger and enhance inflammatory reactions. 30 After an acute infection or tissue destruction, the lymphocyte count declines and the neutrophil count rises, which leads to an increase in the NLR. 31 Previous studies reported that both lymphopenia and neutrophilia were independently associated with severity of infectious disease and degree of tissue damage. 32 Recent evidence suggests that the NLR provides a higher predictive value than the stand-alone leukocyte differential because by itself the NLR can reflect, in a synergistic manner, more about disease severity than either of the former leukocyte subgroups alone.32,33 Currently, the NLR has also been proposed as a strong prognostic indicator for worse cardiovascular outcomes in a variety of settings. For example, studies investigating the NLR in patients with cardiovascular disease showed that a higher preprocedural NLR was an independent predictor of adverse outcomes in patients undergoing coronary angiography, percutaneous coronary intervention, and coronary bypass grafting.34–36 A higher NLR predicts mortality in stable coronary heart disease, acute coronary syndromes, and HF.9–11
Among the inflammatory mediators produced by neutrophils, superoxide anions, elastase and 5-lipooxygenase products of arachidonic acid potentially have important effects on lung vascular inflammatory and remodelling processes.37,38 To the authors’ knowledge, only one study in the literature has investigated the role of neutrophils in PAH. 29 This study demonstrated that neutrophils isolated from patients with IPAH and patients with chronic thromboembolic pulmonary hypertension showed an enhanced mediator release (superoxide anion, elastase, leukotriene A4, leukotriene B4 and 5-hydroxyeicosatetraenoic acid) compared with healthy control subjects when challenged with different stimulatory agents. 29 The exact role played by neutrophils in the PAH process remains unknown. Research has demonstrated that hypoxia causes a profound inhibition of neutrophil apoptosis. 39 Hence, the neutrophil appears to be remarkably well adapted to survive and function under oxygen-depleted environments such as those experienced in PAH. Regarding the value of NLR and circulating leukocyte subtypes in PAH, there appears to be only one study in the literature: 14 this study showed that NLR was significantly higher in patients with PAH compared with the healthy control subjects. 14 When examined separately, patients with PAH showed similar neutrophil counts but lower lymphocyte counts compared with healthy control subjects, but this study did not investigate the prognostic value of NLR in PAH. 14 The present study is therefore the first to be published in the literature investigating the role of NLR in predicting survival in patients with PAH. The results from our study showed that the baseline NLR was significantly higher in patients who died during the follow-up period compared with those who survived, and that this higher NLR was due to a higher neutrophil count and a similar lymphocyte count compared with the survivors. The NLR was significantly correlated with important prognostic factors such as NYHA FC, BNP and TAPSE. Multivariate Cox logistic regression analysis did not demonstrate the predictive role of NLR in the long-term mortality of patients with PAH. This was most likely due to the significant correlation between NLR and other significant predictors of mortality in PAH (such as NYHA FC, BNP and TAPSE). In this current study, the independent predictors of long-term mortality were baseline NYHA FC, TAPSE, BNP and the presence of pericardial effusion on echocardiography. These mortality predictors in PAH were consistent with those previously reported in the published literature. 3 At the 5th PAH World Symposium held in 2013, prognostic markers in PAH were outlined according to data from large registries and were reported as follows: male sex, age > 65 years, PAH secondary to connective tissue disease, high NYHA FC, low 6MWD, high BNP or the N-terminal of the prohormone brain natriuretic peptide, high creatinine levels, presence of pericardial effusion in echocardiography, low DLCO, high RAP, low CO and high PVR. 5 As a consequence of the limited size of the patient population in the current study, the mortality predictors did not include all of the above parameters, but those that were evaluated were among the most powerful predictors of mortality, as demonstrated by many large studies and registries.5,40
This present study had a number of limitations. First, it was a single-centre study, which meant that the study sample comprised patients cared for by a single tertiary referral practice. In addition, the sample size was small and there was a limited number of deaths during the follow-up period. Secondly, the study was designed to assess the relationship between the baseline NLR at the time of diagnosis and long-term mortality, so analyses were based solely on blood-test results measured on hospital admission, at the point of diagnosis. Despite adjusting for multiple risk factors, it is possible that there might have been residual confounding conditions and medications.
In conclusion, the present study showed that NLR, a promising marker of inflammation in other disease states, was correlated with important prognostic markers (such as NYHA FC, BNP and TAPSE) in patients with PAH. NLR was also significantly associated with long-term mortality, however it was not found to be an independent predictor of long-term mortality in this PAH population due to its correlation with other prognostic factors. Significant correlations between baseline NLR and other prognostic factors suggests that this simple marker may be useful in the assessment of disease severity in patients with PAH; this would be an easy, widely available and inexpensive test to undertake. These current data suggest that the level of inflammation may be directly associated with disease severity and prognosis in PAH, but this needs to be confirmed in larger prospective studies. Understanding the exact role of the inflammatory pathway in the PAH pathogenesis may lead to new therapeutic approaches.
Footnotes
Declaration of conflicting interest
The authors declare that there are no conflicts of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
