Abstract
There are few randomised controlled data to guide management of patients with pulmonary arterial hypertension associated with congenital heart disease (PAH-CHD). In this clinical review, common areas of uncertainty in the management of PAH-CHD are identified, the literature is summarised and discussed and a suggested approach offered for each clinical dilemma.
Keywords
Introduction
Pulmonary arterial hypertension (PAH) may complicate different forms of congenital heart disease (CHD) associated with volume and/or pressure overload of the pulmonary circulation, including simple pre- and post-tricuspid shunts, corrected shunts and more complex disease. The clinical classification of PAH associated with CHD (PAH-CHD) is summarised in Fig 1.1–3
Clinical classification of PAH-CHD. Current guidelines define four subgroups ((a)–(d)) while a fifth subgroup (segmental PH) can also be described.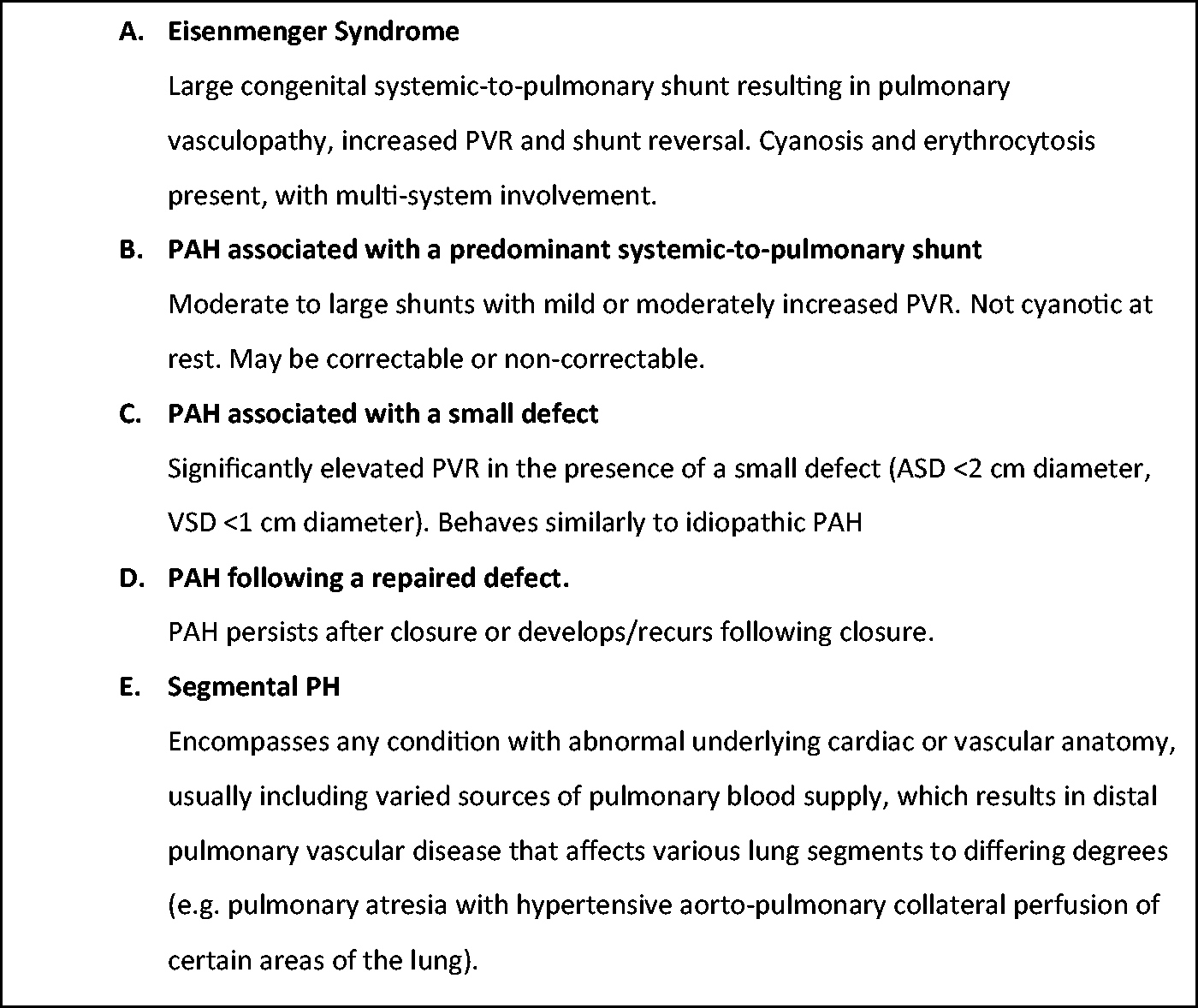
Data from randomised controlled trials (RCTs) including patients with PAH-CHD are limited. In practice, the clinician and patient are often faced with management choices which are not supported by RCT evidence. The CHAMPION (Congenital Heart disease And pulMonary arterial hyPertension: Improving Outcomes through education and research Networks) programme aims to improve the care of patients with PAH-CHD. 4 In this review, we discuss some of the most clinically challenging scenarios facing health care professionals who manage people with PAH-CHD.
Methods
The CHAMPION steering committee identified clinical dilemmas related to challenging issues in PAH-CHD. Each committee member performed a literature search on three or four dilemmas and drafted a suggested approach. The committee then held a further round-table discussion to achieve consensus.
Management dilemmas
Selected therapeutic studies in patients with Eisenmenger syndrome.
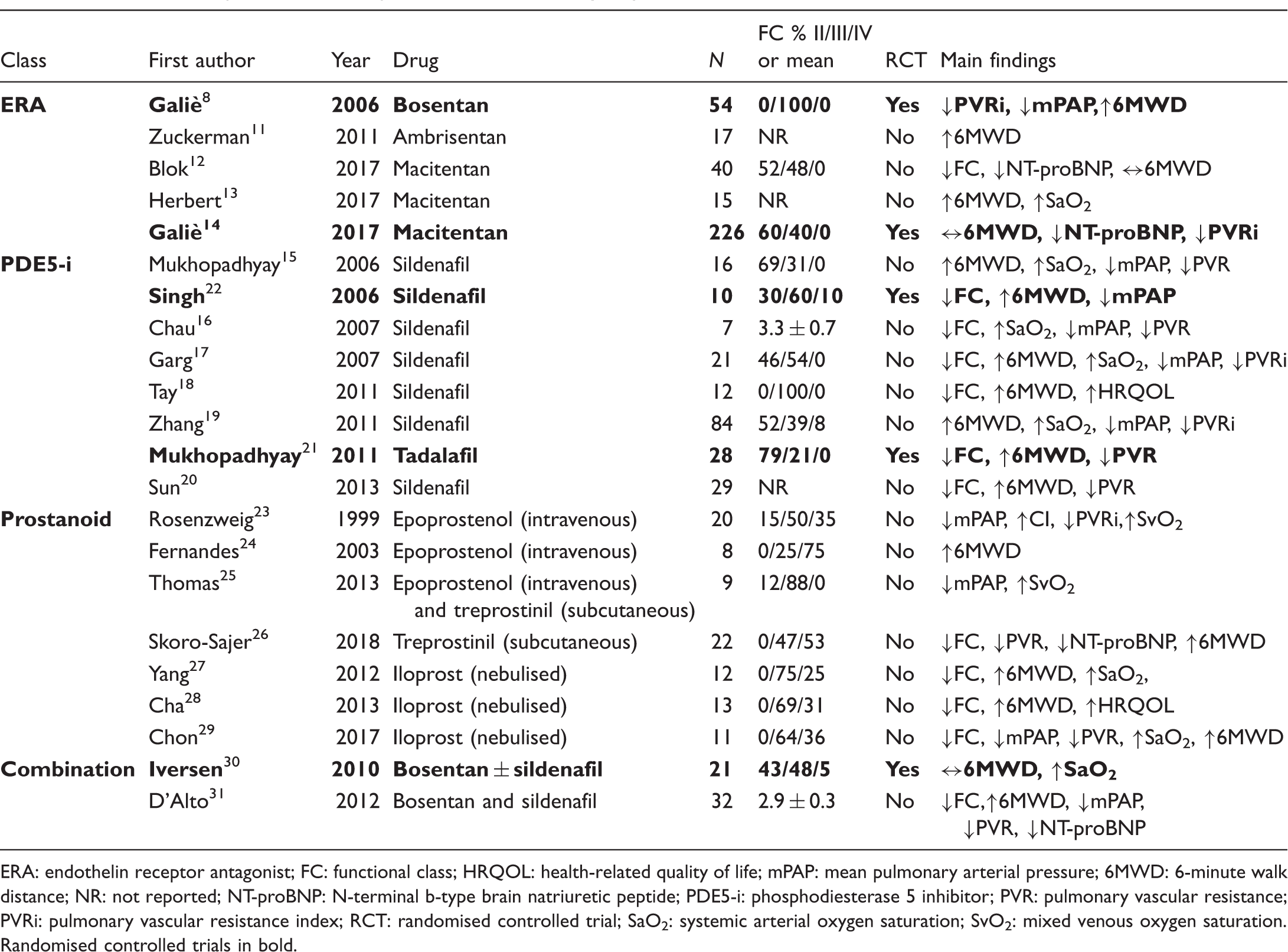
ERA: endothelin receptor antagonist; FC: functional class; HRQOL: health-related quality of life; mPAP: mean pulmonary arterial pressure; 6MWD: 6-minute walk distance; NR: not reported; NT-proBNP: N-terminal b-type brain natriuretic peptide; PDE5-i: phosphodiesterase 5 inhibitor; PVR: pulmonary vascular resistance; PVRi: pulmonary vascular resistance index; RCT: randomised controlled trial; SaO2: systemic arterial oxygen saturation; SvO2: mixed venous oxygen saturation.
Randomised controlled trials in bold.
Although more than one-quarter of ES patients are in FC I or II at time of diagnosis or presentation to a pulmonary hypertension (PH) centre,5,32,33 there are few published RCT data which have specifically investigated ES patients with FC II (Table 1).14,21,22 The merits of PAH treatment in FC II PAH patients were established with the EARLY study, a placebo-controlled RCT of bosentan in FC II PAH (21% PAH associated with small septal defects or patent ductus arteriosus (PDA)). 34 A significant reduction in PVR and clinical worsening after six months of bosentan was observed. The mortality in ES patients in FC I or II, although lower than in those in FC III or IV, is still substantial. 5 Furthermore, even mildly symptomatic ES patients have significantly impaired exercise capacity: In one study, peak oxygen consumption in 20 ES patients (70% in FC I or II) was only 11.5 ± 3.6 ml/kg/min. 35 PAH is a progressive disease and delays in instituting therapy may be detrimental. FC underestimates the severity of limitation in adult congenital heart defect (ACHD) patients who have been affected since birth and are likely to have adapted their “ordinary” activities to their ability. There is, therefore, a rationale for the use of PAH therapy in ES patients in FC II but given the lack of specific evidence in this population, this cannot yet be routinely recommended. Routine assessment of ES patients should include risk stratification, either using the criteria recommended by current European Society of Cardiology guidelines, and/or ES-specific predictors or outcome including BNP, C-reactive protein, platelet count and 6MWD.2,36–38 In a multicentre study of 1098 ES patients, five independent predictors of mortality were identified: age, pre-tricuspid shunt, lower systemic oxygen saturations (SaO2), presence of pericardial effusion and absence of sinus rhythm. 39 Patients at increased risk of death should be considered for PAH therapies, independent of FC.
The role of combination therapy in PAH has evolved significantly over recent years. The AMBITION trial of upfront combination therapy with ambrisentan and tadalafil in 500 PAH patients (including 13 patients with previously closed defects) and the SERAPHIN study of macitentan in 742 PAH patients (including 62 patients with previously closed defects, 64% of whom were on background PDE5-i) demonstrated an improvement in time to clinical worsening and 6MWD in those receiving combination therapy (upfront or early sequential).40,41 The COMPASS-2 study of 334 PAH patients on background sildenafil (including 20 patients with previously closed defects) who were given bosentan or placebo failed to demonstrate improvement in time to clinical worsening, but significant improvements in 6MWD and NT-proBNP were observed. 42 On the basis of these studies, current guidelines recommend upfront or sequential oral combination therapy for PAH patients in FC II or III. 43
There are, however, few data to support this approach in ES. In one study, 21 ES patients were randomised to receive sildenafil or placebo in addition to background bosentan. 30 No significant effect on 6MWD was observed, although a significant increase in resting SaO2 was noted (Table 1). In another study of 32 ES patients receiving bosentan, addition of sildenafil resulted in significant improvements in FC, 6MWD, NT-proBNP and haemodynamics (Table 1). 31 Diller et al. reported outcomes in 153 ES patients, 26 (17%) of whom received sequential combination therapy with bosentan and sildenafil: No difference in long-term mortality between those treated with mono- as opposed to dual therapy was observed. 6 Finally, the MAESTRO study randomised 226 ES patients, 61 of whom were on background PDE5-i therapy, to receive macitentan or placebo. 14 While the primary endpoint of change in 6MWD was not met, detailed results are awaited.
Several observational studies have reported improvement in exercise capacity and haemodynamics following intravenous, subcutaneous or inhaled prostanoid therapy (Table 1).23–29 Intravenous therapy is associated with a risk of paradoxical embolic events; where available, subcutaneous treprostinil may be an attractive option. Owing to the complexities of prostanoid therapies, their role in ES is limited to patients deteriorating despite PDE5-i/ERA combination therapy, especially when they are candidates for transplantation. Currently there are no data to support the use of oral therapies acting on the prostacyclin pathway, even though PAH patients with repaired CHD were included in the GRIPHON study. 44
Current international PH guidelines recommend right heart catheterisation (RHC) to confirm a diagnosis of PAH, assess haemodynamic severity and, in cases of suspected idiopathic, heritable or drug-associated PAH, assess acute vasoreactivity. 2 Cardiac catheterisation, including acute vasoreactivity, is also used to assess operability in CHD patients. Therefore, all PAH patients, including ES, should in principle undergo cardiac catheterisation to establish the diagnosis of PAH.
In adult clinical practice, however, echocardiography can provide sufficient information to establish the presence of severe pulmonary artery (PA) pressures in patients with post-tricuspid shunts (e.g. VSD, PDA, aortopulmonary window), which, together with clinical features such as hypoxaemia, clubbing and secondary erythrocytosis, are highly suggestive of ES. Cardiac catheterisation is, however, indicated in patients with pre-tricuspid shunts or those who present with left-to-right shunting and may be candidates for defect closure. Similarly, cardiac catheterisation is indicated for patients with PAH associated with small or repaired defects and those with associated lesions (e.g. pulmonary stenosis), suspected segmental PH or other complex anatomy.
Hypoxaemia in patients with ES results not from alveolar hypoxia but rather from right-to-left shunting as a result of increased PVR. Hence, a proportion of deoxygenated blood leaving the right heart bypasses the alveolar-capillary interface. The rationale for the use of supplemental oxygen is, therefore, not immediately apparent. Early studies on the use of oxygen in patients with ES did, however, demonstrate a reduction in PVR and increase in pulmonary blood flow (Qp). 45 A significant improvement in SaO2 was observed in 29 patients with cyanotic CHD following 10 minutes of 40% oxygen. 46 More recently, a significant improvement in 6MWD, heart rate recovery, dyspnoea and lower limb fatigue was seen in 30 ES patients who received acute 40% oxygen supplementation. 47 There was, however, no benefit after two years of nocturnal oxygen therapy on mortality, exercise capacity, erythrocytosis or quality of life in an RCT involving 23 patients with ES and a post-tricuspid defect. 48 The routine prescription of oxygen therapy is, thus, not supported by the current literature, and the use of oxygen should be considered on a case-by-case basis and continued only if there is clear subjective or objective benefit.
The percentage of inspired oxygen in most pressurised airlines at cruising altitude is 15% compared with 21% at sea level. 49 Hypoxia has the potential to cause pulmonary vasoconstriction and, thus, current PH guidelines recommend the use of supplementary oxygen in idiopathic PAH patients in FC III or IV or with a arterial oxygen pressure <8kPa. 2 Broberg et al. surveyed the flight history of 53 ES patients over a 10-year period. 50 The majority of flights were taken without supplementary oxygen and no adverse events of significance were observed. It, therefore, seems reasonable for most stable ES patients to fly without supplemental oxygen. Measures to reduce the risk of other complications around flights, such as keeping well hydrated and mobilising regularly, should be advocated.
Data regarding treatment outcomes in ES associated with complex anatomy are extremely limited. Ten patients with complex anatomy received two years of bosentan therapy and demonstrated significant improvements in 6MWD and WHO FC. 51 Baptista et al. treated 14 patients with ES and complex anatomy (including four with truncus arteriosus, two with transposition of great arteries and five with tetralogy and pulmonary atresia) and demonstrated a significant improvement in 6MWD after six months of bosentan. 52 Significant improvements in WHO FC and 6MWD were seen in response to bosentan therapy in seven patients with pulmonary atresia and segmental PAH. 53 Yamamura et al. subsequently reported beneficial effects of bosentan on haemodynamics and BNP in two paediatric patients with surgically treated tetralogy of Fallot with pulmonary atresia and major aorto-pulmonary collaterals. 54 There are currently no data on the use of PAH therapies in patients with unoperated single ventricle physiology with an unprotected pulmonary circulation and Eisenmenger complex. While an increase in Qp may improve oxygenation, close monitoring of systemic ventricular function is recommended for the potential detrimental effects of the additional volume load.
In CHD, PH as conventionally defined (mean pulmonary arterial pressure (mPAP) ≥ 25mmHg) is not synonymous with pulmonary vascular disease (PVD). A large left-to-right shunt may result in elevation of mPAP due to increased flow rather than a pulmonary vasculopathy. It is widely accepted that cardiac defects should not be closed in patients who have developed “significant” PVD. 55 Indeed, while the defect may have been instrumental in the development of PVD, it thereafter acts as a “relief valve” for the pressure-overloaded right ventricle (RV), which can fail acutely or over time if the defect is repaired. The above considerations become even more complex in patients with pre-tricuspid shunts, i.e. various types of ASD, in whom the development of PVD is a rather unexpected phenomenon and suggests an intrinsic predisposition of the pulmonary vasculature towards PVD, and a phenotype resembling idiopathic PAH.
Whilst the decision to repair a congenital heart lesion should rely on the overall clinical picture, PVR is the single best indicator of the severity of PVD.
10
International guidelines suggest that patients with a PVR indexed (PVRi) < 4 WU.m2 (or PVR < 2.3 WU) should be considered for repair and those with a PVRi greater than 8 WU.m2 (or PVR > 4.6 WU) should not (Fig. 2).
2
A “grey” area of patients with “borderline” haemodynamics remains; these should be considered individually in expert PAH and CHD centres. Fenestrated closure of large ASDs is recommended in borderline cases deemed suitable for repair, hence preserving a “relief valve” for the RV, whilst significantly reducing left-to-right shunting.
The importance of calculating PVRi in assessing suitability for closure of atrial septal defects. A mean left atrial pressure of 10 mmHg is assumed in this example. Patients with a left-to-right shunt and significantly raised pulmonary blood flow may have pulmonary hypertension (mPAP ≥ 25 mmHg) in the absence of an increase in PVR (green zone); in these cases, defect closure is advisable. Patients with PVRi > 8 WU.m2 are deemed to have established PVD and the defect should not be closed. Those with PVRi > 4 but < 8 WU.m2 are in the “grey” zone and the decision on whether to repair the defect should be taken in expert centres. PA: pulmonary artery; PAH: pulmonary arterial hypertension; PVD: pulmonary vascular disease; PVR: pulmonary vascular resistance; PVRi: pulmonary vascular resistance index; mPAP: mean pulmonary arterial pressure.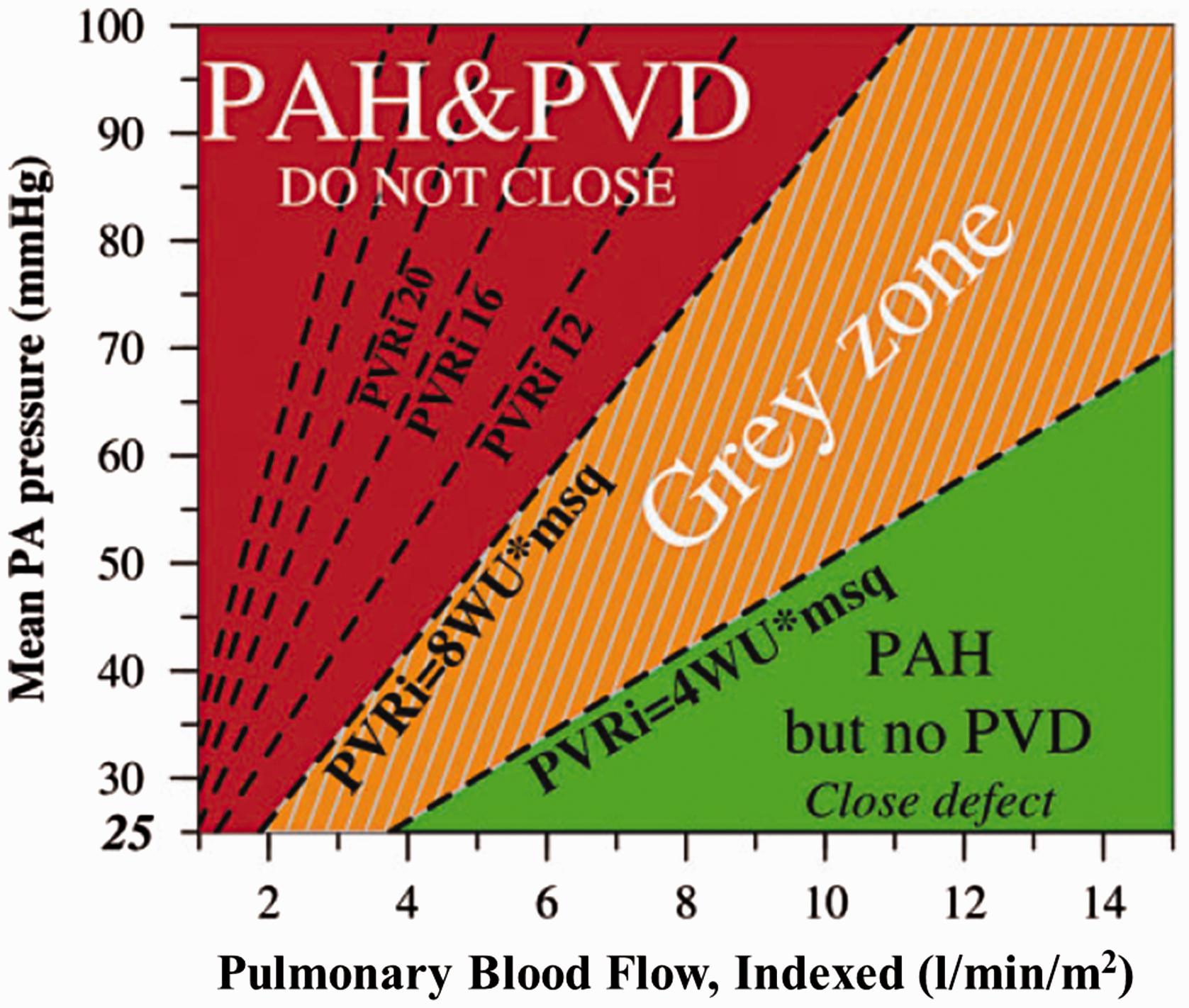
Data to support pretreatment of patients with borderline or prohibitive haemodynamics with PAH therapies, followed by intervention (the “treat-and-repair” approach) are lacking, with concerns persisting regarding the long-term response of the pulmonary vascular tree and RV to defect closure. 6 Certainly, no patients with ES (i.e. those with very high PVR and reversal of the shunt) should undergo repair, regardless of the treatment received.
Computed tomography thorax demonstrating anomalous pulmonary venous connection of the right middle lobe pulmonary vein (horizontal arrow) into the superior vena cava (vertical arrow). Note the dilated pulmonary artery (PA) compared with adjacent ascending aorta (Ao).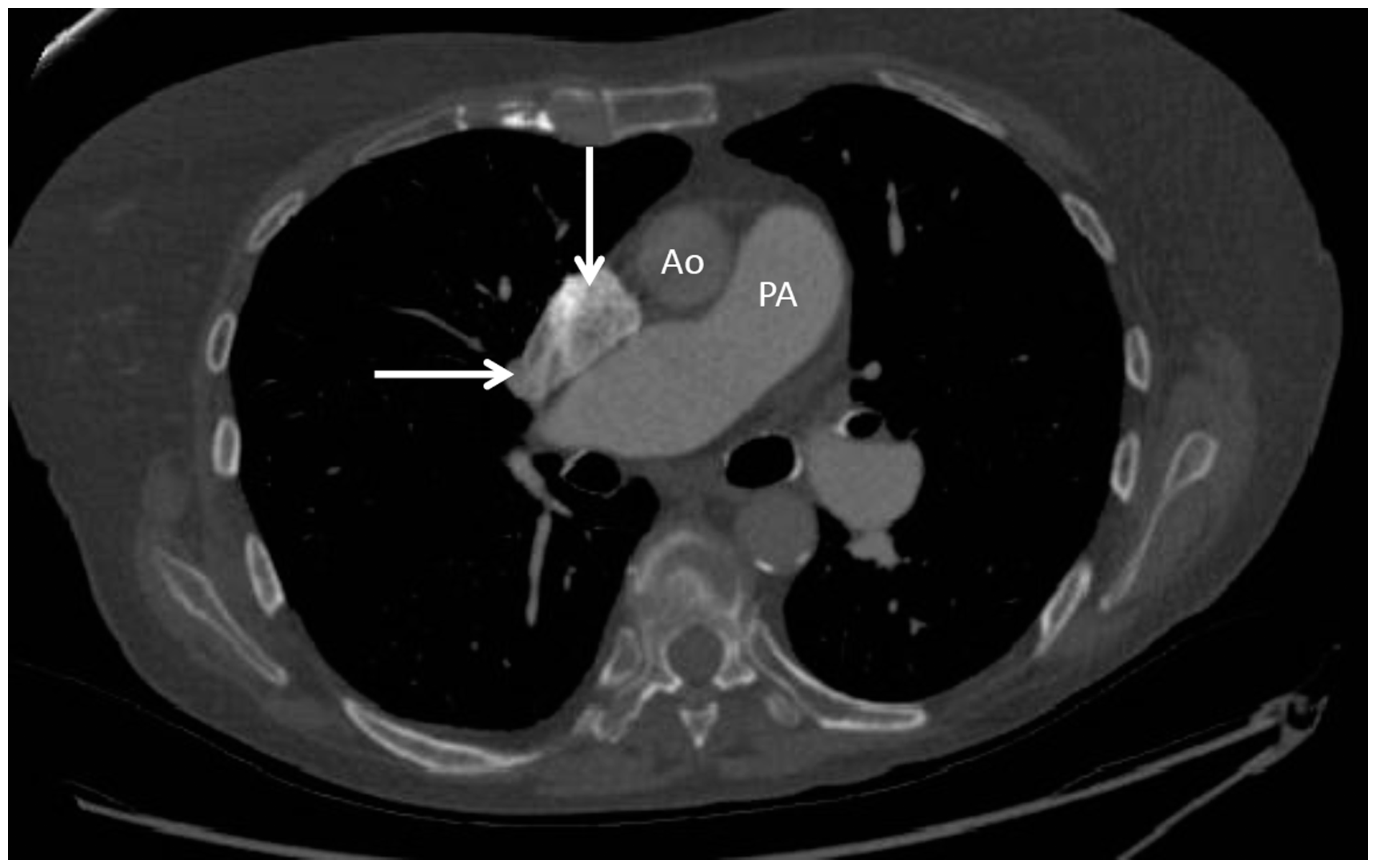
Partial anomalous pulmonary venous return of the right upper pulmonary veins to the superior vena cava (SVC) may be associated with a sinus venosus ASD, both of which are very difficult to identify on transthoracic echocardiography in adults. Pulmonary venous drainage should be, therefore, systematically evaluated on cross-sectional imaging in patients with suspected or proven PH. Cardiac catheterisation also provides an opportunity to avoid misdiagnosis, by routinely sampling SaO2 in the upper and lower SVC and identifying the “step-up” in saturations.
In this case, mean PA pressure was indeed high (30 mmHg), as was the transpulmonary gradient (17 mmHg). It can be argued that Qp should be calculated using the direct Fick method rather than thermodilution, which is not recommended in the presence of a shunt (even though this shunt occurs proximal to the right atrium where the cold saline is injected). An indexed Qp of 7 l/min/m2 suggests a significant left-to-right shunt, and PVRi is estimated as 2.4 WU.m2. Hence there is no evidence of PVD and, with a Qp:Qs well above 1.5 and RV dilatation, the patient should be referred for surgical repair. Transoesophageal echocardiography is indicated to determine the presence of a sinus venous ASD or other CHD prior to surgery.
Correctly identifying an intracardiac shunt may mean the difference between a wrong diagnosis of idiopathic PAH (with years of inappropriate treatment), and cure by repairing the defect.
Secundum ASDs are, in their vast majority, easily repairable through percutaneous device implantation, while others are amenable to surgery. However, no ASDs should be closed unless there is clear evidence of a normal PVR (see Case 8, Fig. 2). Closing the defect in a patient with established PVD can have detrimental effects, as the ASD may act as a “relief valve” for the RV. Adult PAH-CHD patients with previously repaired defects have the worse prognosis of all PAH-CHD (including ES), underscoring the need to avoid inappropriate CHD repair. 56
This patient has severe PAH, with a severely raised PVR of 8.8 WU and significant symptoms of dyspnoea and presyncope on effort. Even though we do not know the haemodynamics before ASD closure, it is likely that PVD was pre-existent and closure of the defect (perhaps associated with progression of the PVD or other predisposing factors) has led to progressive deterioration of RV function, transforming this into a condition akin to idiopathic PAH. For this reason, patients with repaired PAH-CHD have been included in major PAH trials,41,57 and this patient should be treated aggressively with PAH therapies in view of her severe symptoms. Other causes of PH should, of course, be considered and excluded.
Balloon atrial septostomy, which boosts systemic cardiac output by allowing right-to-left shunting at the expense of SaO2, is a potential therapeutic option if the patient fails to respond to PAH therapies. Guidelines suggest avoiding septostomy if mRAP > 20 mmHg or resting SaO2 are < 85%. 2 However, it is better to avoid closing the defect in the first place if there is PVD, or at least allow a fenestration in borderline cases.
Chronic hypoxaemia stimulates compensatory erythrocytosis with the aim of preserving oxygen delivery (DO2, Fig. 4). In a study on 171 ES patients, there was a significant inverse relationship between SaO2 and haemoglobin in those who were iron replete, which was weaker in those who were iron deficient.
58
Broberg et al. subsequently studied 65 ES patients in more detail and derived an equation to predict haemoglobin levels for a given SaO2, in the absence of iron, B12 or folate deficiency:
59
Oxygen delivery is the product of cardiac output and the oxygen content of blood. In patients with hypoxaemia and impaired cardiac output, maintenance of oxygen delivery relies on a compensatory erythrocytosis. The minute amount of oxygen dissolved in plasma is not included.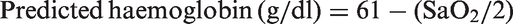
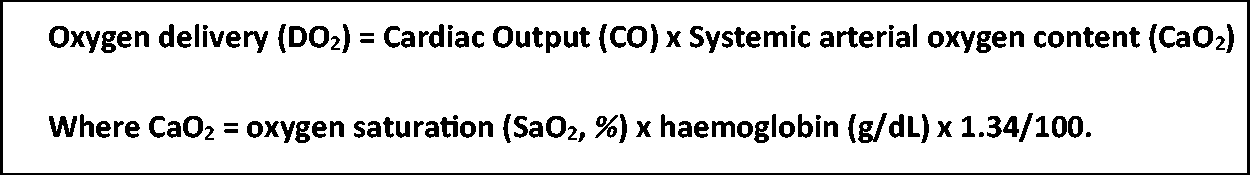
This equation has not, however, been prospectively validated.
Iron deficiency occurs in up to one-third of ES patients and is likely multifactorial, due to reduced absorption and increased consumption due to the erythrocytosis and chronic bleeding. The most widely used parameters to assess iron status in clinical practice are transferrin saturation and serum ferritin. Importantly, microcytosis is uncommon in the iron-deficient cyanotic patient, and a normal mean cell volume cannot be used to exclude iron deficiency. 60
Iron deficiency is associated with poorer survival in ES. 61 Three months of oral iron replacement (ferrous sulphate 200 mg three times daily, few instances of intravenous iron) given to 25 cyanotic CHD patients resulted in significant improvements in haemoglobin and iron stores, together with improved 6MWD and quality of life. 62 Although there were instances of symptomatic hyperviscosity in previous studies following iron replacement, no significant symptoms of hyperviscosity were observed in this study. 63 When patients cannot tolerate oral iron, intravenous iron replacement should be offered.
In previous decades, routine venesections were used in ES to keep the haematocrit below an arbitrary target, with the aim of reducing the risk of thrombotic events and other hyperviscosity symptoms. However, iron deficiency and venesections have been associated with an increased risk of cerebrovascular events 64 and venesection is, nowadays, reserved for iron-replete patients with high haematocrit (well above 0.65) and severe symptoms of hyperviscosity (such as headaches and lethargy), in the absence of dehydration.
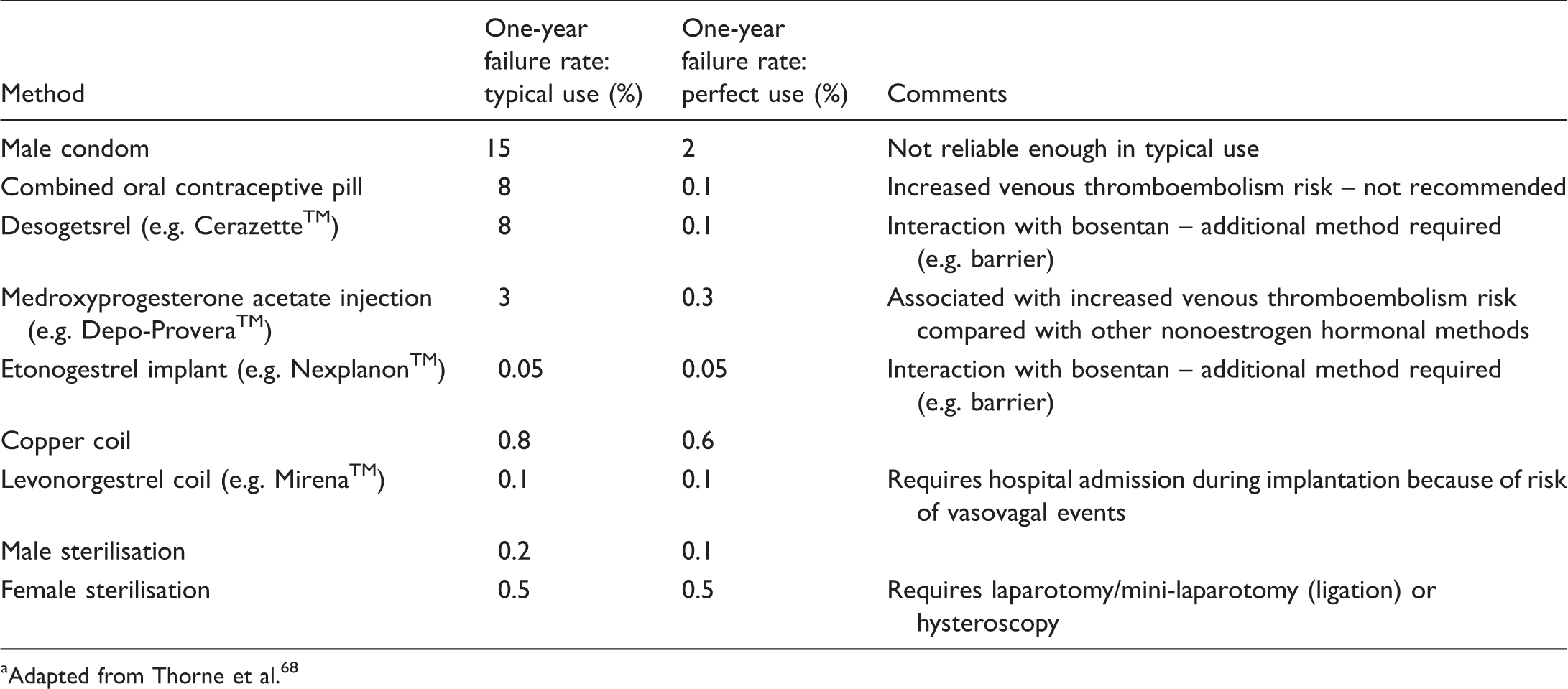
Some women with PH decide to proceed with pregnancy despite extensive counselling. Other women are first diagnosed with PH during pregnancy and choose to continue. A multidisciplinary approach to pregnancy in PH is essential, and requires a multidisciplinary team of health care professionals experienced in the management of pregnant women with PAH-CHD (PH and CHD physicians and nurses, obstetricians and midwives, anaesthetists, intensivists and access to ECMO/transplant services). 69 Endothelin receptor antagonists are potentially teratogenic and should be discontinued either prior to conceiving or as soon as pregnancy is confirmed. 70 Sildenafil appears to be safe in pregnancy, while the addition of prostanoid therapy (also safe) may be required. Close monitoring, with early elective delivery depending on the clinical status of the mother and level of maturity of the foetus, are recommended. 71 Close post-partum monitoring in a critical care environment is essential.
Noncardiac surgery and anaesthesia in PAH patients is associated with a mortality of 3.5% to 18%, with the risk being higher in emergency and prolonged surgery.72–75 Other predictors of outcome around surgery include the severity of PH, degree of exercise intolerance and requirement for inotropic or pressor support.72–75
Perioperative management should include measures to reduce blood loss, avoid sudden reduction in systemic vascular resistance (SVR) or rise in PVR, and minimise the negative cardiovascular effects of airway instrumentation and positive airway pressure support. 76 Where possible, regional anaesthesia may be preferred, using regional nerve blocks and low-dose spinal or combined spinal/epidural techniques to minimise the drop in systemic pressure. Patients with intracardiac defects may be prone to right-to-left shunting secondary to the fall in SVR during anaesthesia, resulting in worsening hypoxaemia. Pressor agents to maintain SVR and intravenous prostanoid therapy to reduce PVR may, therefore, be required. Established PAH therapies should be continued; an intravenous formulation of sildenafil is available and preoperative commencement of intravenous prostanoid therapy may be considered. Care should be taken to reduce the risk of air emboli by using air filters and automated giving sets.
Close postoperative cardiovascular monitoring is essential. PA catheters are not routinely used because of concerns regarding complications such as PA trauma; however, noninvasive methods of cardiac output measurement may be considered.
Patients with ES commonly have few, less-effective platelets and may, therefore, have an increased requirement for platelets and clotting products. Given the importance of haemoglobin levels to maintain DO2, a higher threshold for transfusion (10–14 g/dl, depending on baseline haemoglobin concentration) should be considered. Finally, surgery is best performed in an elective manner with an experienced multidisciplinary team of anaesthetists, intensivists, surgeons, ACHD and pulmonary vascular physicians.
CHD is present in up to 43% of people with DS, with atrioventricular septal defects being most common. 77 Historically, few people with DS were offered corrective surgery and, as a consequence, the prevalence of ES in adults with DS is currently high. While randomised data on the use of PAH therapies in DS are lacking, there are some observational data suggesting efficacy. Significant improvements in WHO FC, 6MWD, Qp and PVRi were observed in a prospective study on 18 people with DS and ES after 12 months of bosentan therapy. 78 Similarly, 6MWD, SaO2 and pulmonary acceleration time significantly improved in seven people with DS and ES who received bosentan for more than four years. 79 Conversely, no improvements were observed in a study of 30 ES patients with DS following four months of bosentan, although the reproducibility of the 6MWD in patients with DS has been questioned.80,81 Furthermore, the recent Sildenafil in Treatment-Naive Children, Aged 1–17 Years, with Pulmonary Arterial Hypertension (STARTS-1) dose-finding trial of sildenafil in paediatric PAH failed to demonstrate a significant haemodynamic improvement in 48 people with DS. 82 The choice of PAH therapy depends on various parameters. The requirement for monthly blood monitoring with bosentan therapy can be problematic for some. In these cases, PDE5-i therapy or alternative ERAs with less-intensive blood monitoring requirements can be considered. A common concern regarding PDE5-i therapy is increased frequency of erections, but in practice this rarely leads to discontinuation.
Many people with DS lack full capacity to make informed treatment decisions. Family members sometimes have concerns regarding new medications which can result in a patient being denied effective therapy. In these situations, a best-interests meeting should be held including members of the multidisciplinary team, the family, the patient and an independent advocate.
Conclusion
The suggested approaches are based on interpretation of the published literature, guidelines and clinical experience. Management decisions in an individual patient require clinical assessment of risks and benefits.
Footnotes
Acknowledgements
The CHAMPION group has received an unrestricted educational grant from Actelion Pharmaceuticals. Actelion had no input into the writing of this manuscript.
Author contributions include the following: R.C. conceived the manuscript. All authors drafted sections of the paper and approved the final paper for submission.
Conflicts of interest
R.C. has received honoraria from Actelion, Bayer, GSK, and MSD. P.C. has received honoraria from Actelion and Bayer. K.D. has received grants and honoraria from Actelion, Bayer, GSK, MSD, and Pfizer. R.M.R.T. has received honoraria from Actelion, Abbott International, Bayer, and GSK.
Funding
The CHAMPION programme is supported by an unrestricted educational grant from Actelion Pharmaceuticals.