Abstract
Patients with end-stage heart failure (HF), pulmonary hypertension and elevated pulmonary vascular resistance (PVR) despite medical therapy are not eligible for heart transplantation (HTx). In this ‘proof of concept’ case series, we demonstrate the feasibility and efficacy of the MitraClip procedure as ‘bridge to list’ in end-stage HF patients not eligible for HTx. In fact, in the three patients reported, who were initially excluded from the HTx list because of elevated PVR, the MitraClip procedure was followed by a sustained improvement of PVR, allowing the patients’ risk to be reclassified, and they were then considered eligible for HTx.
Introduction
Heart transplantation (HTx) is the treatment of choice for patients with end-stage heart failure (HF). 1 However, patients with severe pulmonary hypertension (PH) and elevated pulmonary vascular resistance (PVR) > 6 Wood Units (WU) are not eligible for HTx list due to the risk of post-operative right ventricular failure and unacceptably poor outcome.2,3 Furthermore, in the case of concomitant severe bi-ventricular dysfunction, a left-ventricular (LV) assist device is not indicated, 4 leaving these patients with no therapeutic opportunities.
End-stage dilated cardiomyopathy (DCM) is often associated with severe functional mitral regurgitation (MR) secondary to dilative LV remodelling. Functional MR reduces antegrade cardiac output and increases LV filling pressure, leading to PH, which may progressively become pre-and post-capillary. In high surgical risk patients, trans-catheter mitral valve repair with the MitraClip procedure (Abbott Vascular, Menlo Park, CA, USA) is a safe procedure to reduce Functional MR and PH and improve the quality of life. 5
Case series
We present a case series of three patients, mean age 57 years, two males and one female, affected by end-stage DCM, HF and severe Functional MR, who were excluded from the HTx programme due to PH associated with elevated PVR and an unsatisfactory response to a vasodilator challenge. Patients underwent MitraClip implantation under general anaesthesia with real-time echocardiographic and fluoroscopic guidance. After a follow-up period of six months, we found a remarkable haemodynamic improvement, which allowed all three patients to be included in the HTx list.
Characteristics of patients before MitraClip procedure.
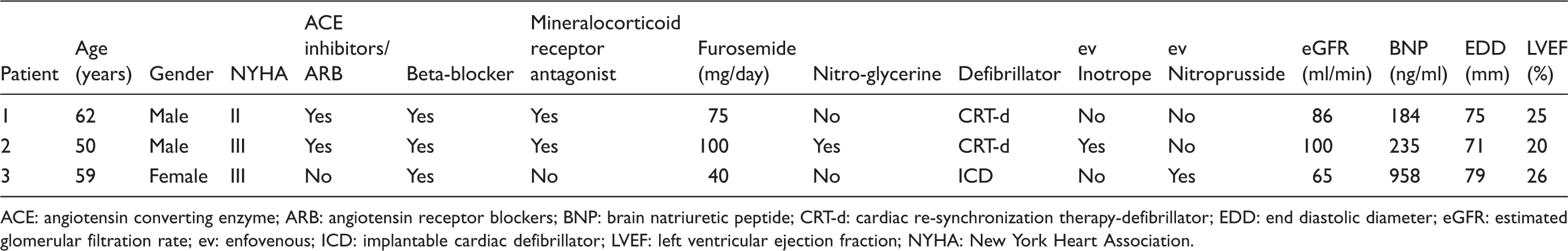
ACE: angiotensin converting enzyme; ARB: angiotensin receptor blockers; BNP: brain natriuretic peptide; CRT-d: cardiac re-synchronization therapy-defibrillator; EDD: end diastolic diameter; eGFR: estimated glomerular filtration rate; ev: enfovenous; ICD: implantable cardiac defibrillator; LVEF: left ventricular ejection fraction; NYHA: New York Heart Association.
Baseline and six-month follow-up echocardiographic and haemodynamic parameters.
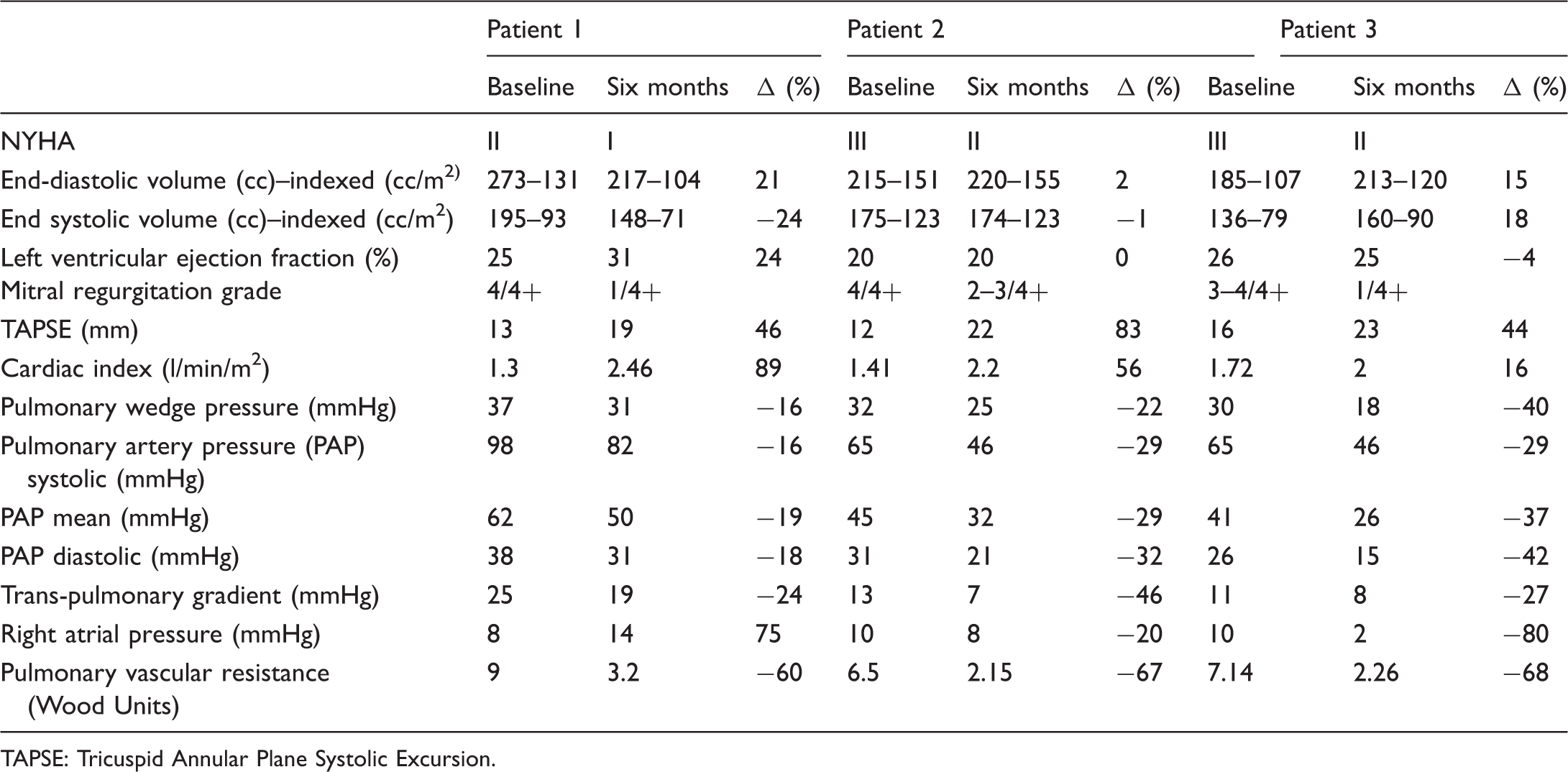
TAPSE: Tricuspid Annular Plane Systolic Excursion.
Patient 1 (SB)
A 62-year-old male with post-ischaemic DCM, INTERMACS classification 7 and bi-ventricular dysfunction. RHC showed very poor cardiac index (CI) =1.3 l/min/m2 and severe PH with PVR = 9.0 WU, dropping to 3.6 WU after vasodilator challenge. MitraClip was successfully performed with the implantation of two clips (post-implant mitral regurgitation (FMR) 1+/4+). After six months’ follow-up, the patient was in New York Heart Association (NYHA) functional class I, residual MR was 1+/4+, and there was favourable LV remodelling (Table 2). CI improved to 2.46 l/min/m2 and PVR was reduced to 3.2 WU, which allowed inclusion on the HTx list. Importantly, he was readmitted to hospital for acute decompensated HF 746 days after the procedure.
Patient 2 (BMT)
A 50-year-old male with idiopathic DCM and bi-ventricular dysfunction and multiple hospitalizations for HF in the last six months, INTERMACS classification 3. RHC showed poor CI = 1.4 l/min/m2 and severe PH with PVR = 6.5 WU, substantially unchanged (6.2 WU) after vasodilator challenge (Fig. 1). The MitraClip procedure was successfully performed with the implantation of one clip (post-implant MR 2/4+). After six months’ follow-up, the patient was in NYHA class II. We found right ventricular (RV) function improvement, while there were no significant changes in LV volume or function. CI improved to 2.2 l/min/m2 and PVR was reduced to 2.15 WU; therefore the patient became eligible and was listed for HTx. The patient was readmitted for HF for the first time 514 days after the procedure.
Vasodilator challenge during right heart catheterization.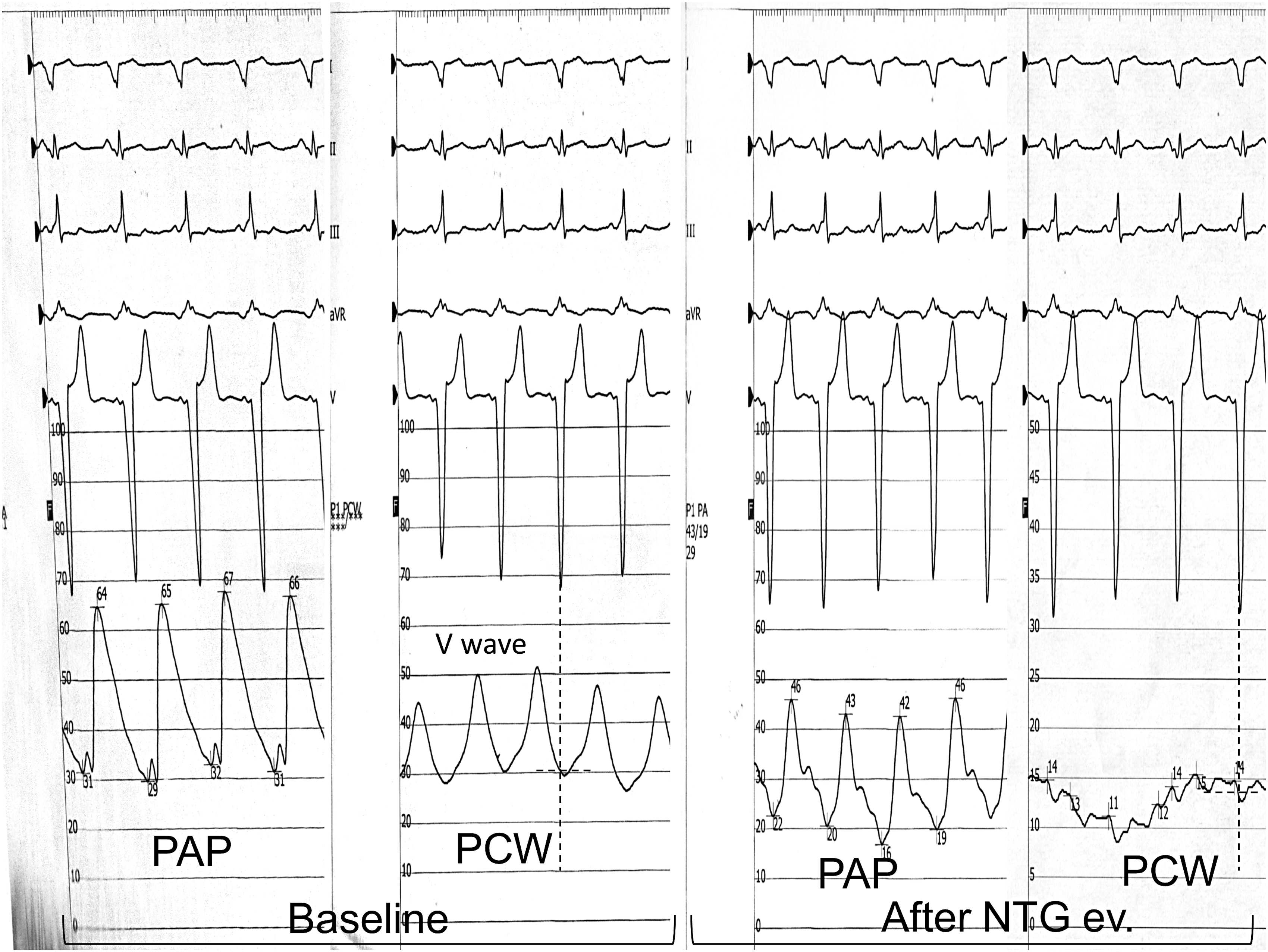
Patient 3 (GM)
A 61-year-old female with post-ischaemic DCM, single hospitalization for HF in the last 6 months, INTERMACS classification 6 ‘frequent-flyer’. Baseline RHC showed poor CI = 1.72 l/min/m2, with prevalent post-capillary PH and PVR = 7.14 WU; no acute vasodilator challenge was performed as the patient was already under infusion with nitroprusside. She underwent the MitraClip procedure with the implantation of two clips (post-implant residual RM 1+/4+). At RHC at six months, CI had improved to 2.0 l/min/m2 and PVR was reduced to 2.26 WU. Because of worsening symptoms of HF, but still acceptable PVR, she was added to the HTx list two years after the procedure.
Discussion
Although the role of MitraClip as ‘bridge to transplant’ has already been reported,5–7 this is a proof of concept case series demonstrating, for the first time, the role of the MitraClip procedure as ‘bridge to list’ in end-stage HF patients not eligible or at high risk for HTx due to elevated PVR with unsatisfactory response to vasodilator challenge. In all three patients, the MitraClip procedure was followed by a sustained reduction of PVR, allowing them to become eligible for HTx. Also, none of the three patients was re-hospitalized for HF in the year after the procedure, and all were in a lower NYHA functional class as compared with baseline. This finding may be a consequence of the increase in antegrade cardiac output and the decrease of LV filling pressure following mechanical reduction of Functional MR. Consistently, increased RV performance was found in all patients (ranging from +44% to 83%). Nonetheless, favourable LV remodelling was observed only in patient 1 (who likely had less advanced disease), which is in agreement with previous reports showing this phenomenon in fewer than half of advanced HF patients. 5
Footnotes
Conflict of interest
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Informed consent
All patients have signed an informed consent for research purposes.
