Abstract
About half of all patients with pulmonary hypertension (PH) experience psychological and emotional disturbances that affect their quality of life (QOL). There is a lack of studies exploring how psychiatric professionals can provide specific and effective mental health treatment to patients with PH. This study aimed to explore and understand the treatment experiences of patients with PH in Taiwan. We employed an exploratory qualitative design involving interviews with 17 patients with PH who were treated at Kaohsiung Veterans General Hospital in Taiwan. Participants were interviewed by a psychiatrist; the interviews were audiotaped and transcribed for thematic analysis by two researchers. We corroborate earlier findings showing that patients who have the rare disease PH often experience psychological or emotional disturbances throughout the treatment process. This study explored a model for psychiatric intervention based on patients’ experience of having PH. We find that assessing and strengthening links to external resources can enhance patients’ long-term coping abilities, and thereby help reduce their psychological and emotional disturbances and improve their QOL.
Introduction
Pulmonary hypertension (PH) is a rare disease, which has a poor prognosis and significantly impacts all physical, psychological, and social areas of the affected person’s life.1,2 The issue of quality of life (QOL) among patients with PH has received more attention recently. Numerous studies have investigated this important topic using different kinds of QOL questionnaires; the results of these studies have indeed shown that up to 50% of patients with PH experience adverse psychological and emotional disturbances that are significantly correlated with their QOL.3–5 Data on coping with or treatment for the psychological or emotional disturbances caused by PH is, however, still lacking. An earlier study shows that the viewpoints and expectations of patients and their medical teams differ. Medical teams focus on the effectiveness of the treatment, while patients are also concerned about real-life practical problems and personal feelings in addition to treatment efficacy. 6 Hence, the psychological and emotional problems that are a priority for patients may be overlooked by the treating team. Understanding the patients’ knowledge about their disease, their inner feelings, and their external, practical needs during treatment remain important to the patients’ QOL. The qualitative research that has been conducted to date exploring the experience of having PH7–12 is limited; to our knowledge, no qualitative study of the experience of patients with PH receiving treatment in an Asian setting has been published to date. This study aimed to explore and understand the experiences of patients with PH in Taiwan and also attempted to interpret patients’ experience and needs from a psychiatric perspective, in order to facilitate the formulation of a more specific psychiatric intervention model that meets the needs of patients with PH in the future.
Methods
Ethical statement
This study utilized an exploratory qualitative design involving interviews with patients with PH who were treated at Kaohsiung Veterans General Hospital (VGHKS) in Taiwan. The Institutional Review Board (IRB) at VGHKS reviewed and approved the study in 2015 (IRB no. VGHKS15-CT10-10).
Participants
Participants were consecutive patients who were treated at VGHKS from October 2015 to May 2016. The eligibility criteria for participation in this study were the following: (1) aged ≥ 20 years; and (2) patients diagnosed with PH by VGHKS physicians. Patients were excluded if they had any cognitive impairments, psychotic illnesses, severely debilitating physical illnesses, or were too ill to participate. Written consent from all participants was obtained at the time of the interview. The expected ratio of male to female participants is 1:4. 13
Data collection
Subject to confirmation of eligibility by the patient’s treating physician, patients were phoned by a research assistant and invited to participate. Willing participants were then interviewed in a private room at the cardiovascular department of VGHKS by one of the authors (Y-C Chiang) who is a psychiatrist. The length of interviews was in the range of 50–80 min and recruitment continued until data saturation was reached (i.e. 17 participants).
Interviews were semi-structured around the participants’ experiences of being diagnosed with and treated for PH. An interview schedule with standard probes was used to guide the dialogue and encourage participants to elaborate on their responses, but remained sufficiently flexible to follow new lines of inquiry raised by participants. All interviews were audio-recorded and transcribed for analysis.
Data analysis
Key themes present in the data were identified from the interview transcripts using thematic analysis. The analysis was undertaken by two of the authors (Y-C Chiang and L-Y Hu). Themes that were identified were discussed between the authors, ensuring that the derived meaning was consistent with the interviewers’ understanding of the participants’ experience. The key themes were progressively grouped, coded, and refined14,15 until agreement was reached. When new additional codes no longer emerged, the cohort was considered complete.
Results
Participant characteristics
Demographic data.
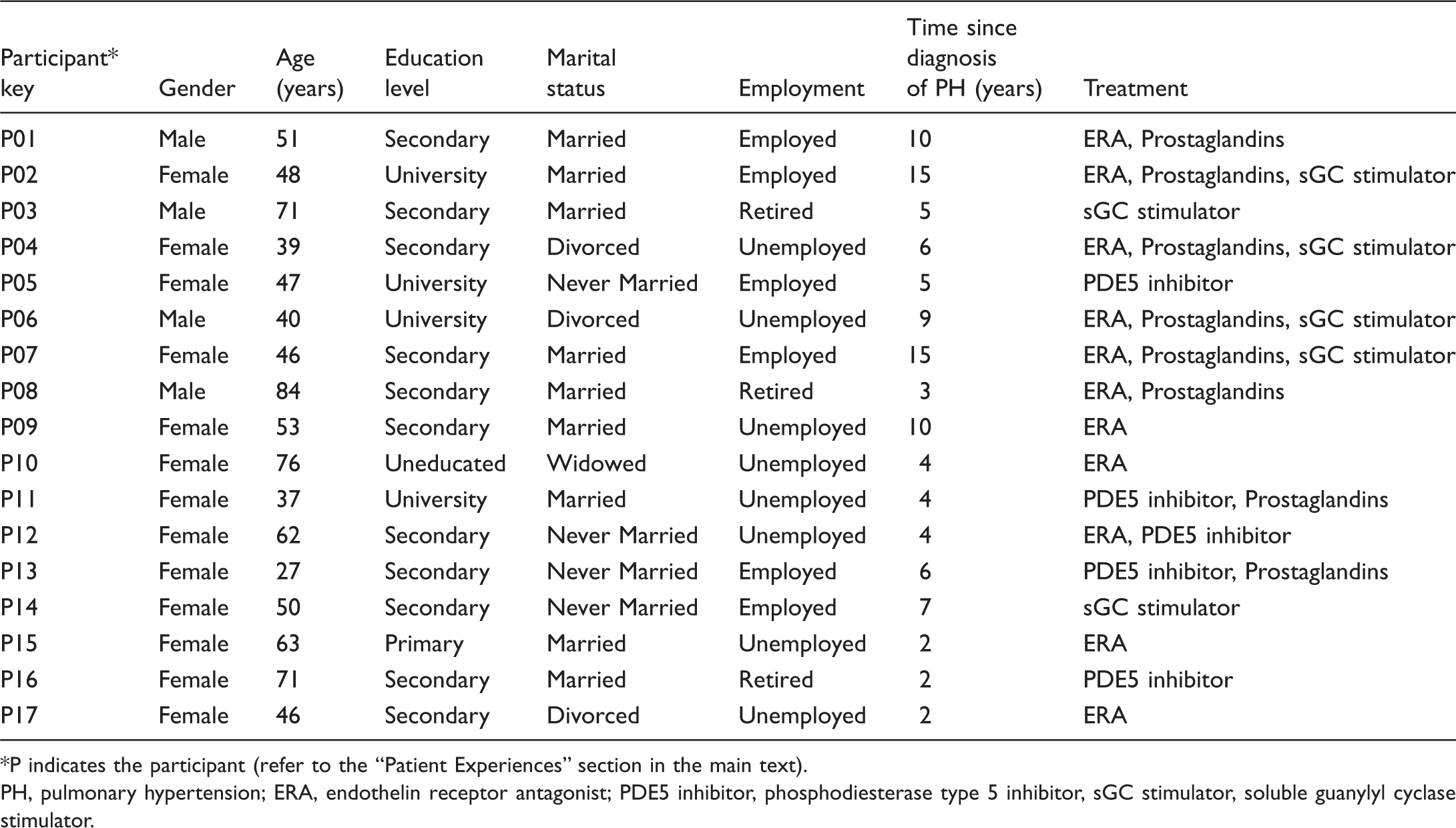
P indicates the participant (refer to the “Patient Experiences” section in the main text).
PH, pulmonary hypertension; ERA, endothelin receptor antagonist; PDE5 inhibitor, phosphodiesterase type 5 inhibitor, sGC stimulator, soluble guanylyl cyclase stimulator.
Patient experiences
The patients’ reaction towards their diagnosis of a rare disease: facing a diagnosis of a rare disease, most patients feel lonely, helpless, and unable to understand and cope with the situation. Participant 15 (P15): It is as if the world is “falling apart all of a sudden.” Being one of the 200–300 people nationwide to have contracted the disease!?
P4: According to the doctor, there is a one-in-a-million chance to have this disease. Just as others say, “Why me!”
Challenges the patients have faced during treatment:
Patients feel depressed about the fact that PH treatment can only alleviate symptoms but not cure the disease, as well as about the countless treatment sessions and side effects arising from the treatment.
P13: If discomfort is felt after taking the medication, it will be difficult to continue working. If medication is required throughout life, I might give up.
Medication fees are costly. Most patients obtain medication by filing case applications or joining clinical trials. Patients are worried about whether or not medication can continuously be obtained.
P14: What most frightens me is that the medication I am taking now is not covered by national health insurance. I have seriously thought about the burden on my family… How can any patient with PH afford it when a jar of medicine costs tens of thousands of dollars?
P3: A project assistant told me, “The doctor said the medicine you took the first time is not necessarily an effective one, as at this stage we are still performing a blind match.” It sounds as if it the drug efficacy was a matter of “sheer luck.” I happened to be blind matched with the so-called “placebo.”
Several patients have trouble making treatment decisions regarding organ transplantation, which seems to be associated with the state of communication with their physician before the transplant, and with uncertainty regarding the outcome.
P2: My doctor told me a lung transplant was the only solution for me. After being sick for 10 months, it was finally my turn on the waitlist! I remember crying and shouting, fiercely resisting the idea of undergoing a transplant. My doctor was at a loss for words, but to me, I had not the faintest idea whether the transplant was a good idea at all.
Wide-range impacts brought about by the disease:
The disease affects cardiopulmonary function, resulting in limited mobility and functional impairments, and further leading to changes of the patient’s role in their family and in society.
P9: There was basically nothing I could do according to my own will. I would need to gasp for breath, even after doing some simple house chores. Sometimes the shortness of breath would get so bad that I could not even move.
P14: I have often thought about what I can do or what I cannot do for my family every now and then. I cannot help with the house chores or work… I just do not know what I can do anymore.
After having the disease, the patient is likely to experience helplessness, hopelessness, uncertainty, anxiety, low self-esteem, guilt, depression, and suicidal thoughts, which likely affect their interpersonal interactions and lead to increased interpersonal conflicts and social withdrawal.
P11: The fact that I know I will not live for long saddens me. I am clueless as to how long my heart will hold out. I need to hang on long enough to see the possibility of new drugs being developed. We know for a fact that medicine has its limitations. Now I am taking it one step at a time, but I must say that I do not like this feeling at all.
P7: When my body deteriorates, I tend to complain why it happened to me. I have no one to blame, so I cry in my bed to release my emotions and hopefully go on the next day.
P9: I used to enjoy talking on the phone and going places. Now, I am too lazy to go out. I do not like going out or talking on the phone now, neither do I welcome people coming for a visit. I have become a loner of some sort.
P4: Whenever I think about my disease, I am drawn to the idea of killing myself. The problem is, I do not have the courage to commit suicide, and yet I have to bear the torture of the disease and financial pressure. I also think about my parents and my child.
Coping with the disease and needs:
Coping with the variety of impacts brought about by the disease, for most patients, is a painstaking process that takes time to adapt to.
P1: After more than one year, I thought about why I should lead an unhappy life. After all, the currently available medication can control the disease well. Therefore, I had a change of mindset. I now believe that despite my physical condition, I can still live a long life.
P6: Over the past 10 years or so, I managed to adjust and suppress my feelings instead of taking it out on the people around me.
Many patients lower their expectations of life and set reachable goals as a way to adapt and seek internal strength or meaning.
P3: I only feel I have to gasp for breath, but my mobility is not restricted. I still do things I want to do, as I know it will do my body good.
P4: I think I can still keep on working. The fact that I can still go to work to make money makes me happy. As long as I do not suffer frequent attacks, I cannot ask for more.
P9: At least, as long as I can still participate in some house chores… I do not dream of a complete recovery as it is impossible. All I ask for is stabilization.
External support including family, workplace, and medical environment support is very important for patients, especially the support of their family being the most crucial:
Family support.
P2: My family, husband, father-in-law, and mother-in-law have all been very considerate since they found out about my disease. I do not have to do house chores, as my husband does all of them. My father-in-law and mother-in-law attended the Pulmonary Hypertension Society patients’ group educational meeting. They are aware of my pant symptoms and poor stamina but, not knowing the reason, they all attended to learn and understand the disease.
P6: My family is very concerned about how I feel, because I had heart palpitations and was hospitalized after a fight once. Ever since that incident, they handled most things by themselves… Now, when I am in need or when I am sad, they encourage me; when I am happy, they laugh with me.
Workplace support.
P14: My colleagues repeatedly asked me not to quit my job. I was a little embarrassed, but I had to quit. I worked until I could no longer climb stairs or do certain things. A colleague of mine was very kind and helped me perform my chores. I said, “This cannot be right. You do my job for me, and I get paid.” She said it was fine.
P11: I am grateful to my boss at work. She time and again asked me to return to my job, but I was reluctant to do so whenever I got sick. She insisted that I went back, likely because she was concerned about my financial situation.
Medical environment support.
P4: I am truly grateful to my doctor for his encouraging words. I often asked the doctor for the availability of a euthanasia drug. He would reply, “If you knew how many of us have tried our best to help you live longer, then, you would never want to end your life as your way of repaying us.” The nurses by the doctor’s side occasionally called me over the phone to ask me how I was feeling.
Most patients, to some extent, experience psychological or emotional disturbances, but few patients express a need for psychiatric intervention and some even refuse to accept it:
P11: Personally, I do not believe that I have depression, but I do lack the confidence normal people have. I do not need help, because it will do me no good. The disease itself is the problem.
P14: My problem is that I am sick. I do not know what you can do to help me, considering you cannot cure me or relieve my pain.
Discussion
This study collects and presents the subjective experiences of patients diagnosed with PH in Taiwan. Through this study, we also attempt to explore specific psychiatric intervention models to meet the needs of these patients. The study shows that the majority of the patients were in shock after being diagnosed with PH. Even though the medical team had already explained the disease to the patients at the disease onset, most of the patients still had trouble understanding it. Recent studies have shown that patients with PH had some difficulties in understanding the disease and related treatment as well as in accepting medical information.16,17 This difficulty can perhaps explain patients being in such a state of helplessness and isolation. Since PH has a low prevalence rate, it is more difficult for patients with PH to find “peers” in their community, to learn from others’ experiences of the disease and its treatment, as is the case for patients with more common diseases. This may have a potential impact on the patients’ ability to cope with the disease psychologically during the early stage after diagnosis. Thus, assisting patients with PH in reducing their feelings of isolation, both psychologically and in their social environment, is an important issue. In this case, patient group meetings or group psychotherapy might be helpful and should be considered.
PH treatment is challenging for patients, especially when it comes to major treatment interventions involving transplant surgery. If a patient has inadequate knowledge of the disease and its treatment, great difficulties will be encountered when making treatment decisions. Therefore, when a medical team is offering to perform surgery, psychiatric professionals could offer assessments to ensure the patients fully understand the disease and the treatment options, and give patients the opportunity to grapple with the medical information with appropriate psychological and emotional support. Additionally, patients with PH are faced with a rare major disease that cannot be cured, which means they will be burdened with long-term treatment expenses as well as enduring side effects, which may affect their QOL. 18 Due to limited medical resources, patients with PH are in a “passive” situation during treatment, which can easily lead to a sense of helplessness. This also indicates that the patients’ financial capabilities and the availability of medical resources have an impact on how the patients cope with the disease. Psychiatric professionals are able to assess the patients’ psychosocial status and integrate available external resources into the treatment, in order to reduce internal adjustment problems, and to enable the patient and their PH medical team to be fully aligned as to the goals of treatment.
As mentioned above, PH has extensive physical, psychological, and social impacts. 19 Past studies also showed that the work competency of almost all patients with PH was affected, which in turn affected their household income, lifestyle, and even interactions with their partners, 20 ultimately leading to a state of social isolation. 7 The results of our study reveal that in addition to the multiple impacts mentioned above, patients with PH are also likely to experience psychological states of anxiety, depression, worthlessness, uncertainty about the future, and hopelessness.5,21,22 Although past studies have pointed out the importance of psychiatric referrals in patients with PH,20,23 one study has shown that the percentage of patients with PH with psychological and emotional disturbances undergoing psychiatric treatment is low. 24 Our study finds that the underlying cause of the low percentage of psychiatric treatment involved is not that the medical team fails to notice the patients’ psychological and emotional disturbances. Instead, patients with PH do not expect, or may even refuse, the assistance of psychiatric professionals, even when they are experiencing significant psychological or emotional disturbances. They think their emotional distress stems from the impact of PH on their physical abilities, daily life, and other aspects. Nearly all patients with PH emphasise that what they need is an effective treatment and assistance in practical aspects of their life. Therefore, we suggest that the recommended psychiatric intervention strategy should include an assessment of the patient’s practical problems, possibilities of strengthening family interactions, and links to social resources. It may then be possible to effectively help with the emotional and psychological aspects of their care. Moreover, the medical team should be patient enough to give the patient time to adjust psychologically during the early stage of their PH diagnosis, which will be conducive to the establishment of rapport and will favorably reduce resistance possibly encountered during future psychiatric interventions if needed.
This study shows that patients with PH need sufficient time to gradually adjust mentally after the disease onset. In addition to externally overcoming difficulties in daily life, they also try to develop inner-stress coping abilities, and to reflect on the significance of their experience with the disease on the value of their lives. The current study is in accordance with past literature that reports that patients with PH need to understand the limitations of their disease, gradually adjust their lifestyle, 20 learn to cope with uncertainty, 11 and redefine the meaning and value of their lifestyle after the disease onset. 10 Psychiatric intervention strategies should coordinate the experiences of disease trajectories in most patients, strengthen the patients’ psychological coping abilities, and further encourage patients to find meaning or strength in their experience of the disease.
Our study has several limitations. The participants in this study were recruited from a major medical center. In consideration of variations in medical or other relevant resources provided by hospitals of different levels, the experiences described in this study may not be representative of all patients with PH in Taiwan. In addition, the time since diagnosis confirmation in the participants in our study was in the range of 2–12 years. The PH treatment received thus varied during this time; however, we found that participants’ reflections were similar despite the differences in disease onset times.
In summary, this study shows that PH greatly affects patients in Taiwan regarding physical, psychological, and social aspects of their lives. In the face of such a rare disease, patients are faced with challenges in terms of an informed diagnosis, an understanding of the disease, and treatment decisions. We find that medical resources and external support have a great impact on the patients’ coping with the disease. Considering that the disease is incurable and that medical resources are limited, it is especially important to strengthen the patients’ own abilities to cope with the disease. Patients with PH experience a variety of psychological and emotional disturbances that are closely related to the multiple impacts the disease brings upon their body and their daily life. Therefore, psychiatric care remains an indispensable part of patient care in PH. This study attempted to explore the space for psychiatric intervention based on patients’ individual experience of having PH. Future long-term studies will be needed to understand whether these recommended psychiatric intervention strategies will be beneficial to the clinical care of patients with PH.
Footnotes
Acknowledgements
The authors are grateful to all patients who took time to take part in this study.
Conflict of interest
The author(s) declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
