Abstract
The effect of pulmonary venous hypertension (PVH) on the pulmonary circulation is extraordinarily variable, ranging from no impact on pulmonary vascular resistance (PVR) to a marked increase. The reasons for this are unknown. Both acutely reversible pulmonary vasoconstriction and pathological remodeling (especially medial hypertrophy and intimal hyperplasia) account for increased PVR when present. The mechanisms involved in vasoconstriction and remodeling are not clearly defined, but increased wall stress, especially in small pulmonary arteries, presumably plays an important role. Myogenic contraction may account for increased vascular tone and also indirectly stimulate remodeling of the vessel wall. Increased wall stress may also directly cause smooth muscle growth, migration, and intimal hyperplasia. Even long-standing and severe pulmonary hypertension (PH) usually abates with elimination of PVH, but PVH-PH is an important clinical problem, especially because PVH due to left ventricular noncompliance lacks definitive therapy. The role of targeted PH therapy in patients with PVH-PH is unclear at this time. Most prospective studies indicate that these medications are not helpful or worse, but there is ample reason to think that a subset of patients with PVH-PH may benefit from phosphodiesterase inhibitors or other agents. A different approach to evaluating possible pharmacologic therapy for PVH-PH may be required to better define its possible utility.
As a perfect example of how clinical imperative can drive basic physiological investigation, studies of the effect of pulmonary venous hypertension (PVH) on the lung's circulation were in full swing by the very early 1950s, 1 close on the heels of the development of surgical relief of mitral valve stenosis. Cardiac catheterization of patients with mitral valve disease has characterized the physiology of PVH, and histological investigations demonstrated the microvascular changes provoked by PVH. Just as important, the effect of relief of left atrial (LA) hypertension on the circulation has been extensively reported, usually for patients who have had mitral valve intervention. We have learned that the circulatory alterations provoked by PVH share some characteristics with other forms of pulmonary hypertension (PH), such as the idiopathic variety, PH due to chronic alveolar hypoxia, and PH secondary to congenital cardiac shunting lesions. For example, acute “reactivity” to vasodilators may be observed, and there is overlap in the microarchitectural abnormalities seen. On the other hand, the “natural history” of PVH-PH is very different than that of the idiopathic variety or that seen with shunting defects: in the former (as demonstrated with mitral valve disease), PH is likely to largely or completely resolve if PVH is relieved, even with long-standing and severely increased pulmonary vascular resistance (PVR),2,3 while in the latter two, PH is more likely to inexorably increase. PVH-PH is therefore one of the very few “models” of increased PVR in which removal of the stimulus is often possible, which is followed by substantial reduction of PVR. (PH caused by chronic alveolar hypoxia shares this quality, but the vascular pathology and elevation of PVR are usually much less severe).4–7
This review will discuss (1) anatomic and physiologic abnormalities that cause PVH; (2) how PVH impacts the pulmonary microvascular architecture and physiology, with emphasis on its effect on PVR; (3) the effect of reduction of pulmonary venous pressure on PVR; (4)mechanical forces, especially increased wall stress, as the putative proximate cause of increased PVR with PVH; and (5) issues related to evaluating pharmacologic therapy aimed at reducing PVH-PH. The effect of PVH on lung water is an important but somewhat distinct issue and is not explored. Clinical presentation and diagnostic evaluation are not discussed, nor are specific therapeutic recommendations offered.
CAUSES OF PVH
Multiple abnormalities increase pulmonary venous pressure. One can, and probably should, separate the causes of PVH into two types: (i) those involving increased pressure in the left atrium or extrapulmonary pulmonary veins are referred to as category 1 (corresponding to Dana Point group 2, PH due to left heart disease), and (ii) conditions with primary stenosis/occlusion of intrapulmonary veins (but with normal LA pressure), referred to as category 2 in this review. The Dana Point classification does not specifically accommodate stenosis of the large intrapulmonary veins, although pulmonary veno-occlusive disease is classified as group 1. Both categories share certain characteristics. For example, PH of variable magnitude and some tendency for pulmonary vasodilators to provoke pulmonary edema are seen with both LA hypertension and pulmonary veno-occlusive disease.8–11 On the other hand, the biology of pathological vascular remodeling originating within the lung (rather than in response to increased LA or proximal pulmonary venous pressure) 12 must be in some ways different from that seen with category 1 PVH. Discussion in this review refers to observations made in and pertinent to category 1 PVH.
Category 1: anatomic and physiologic abnormalities which increase LA or extrapulmonary vein pressure
There are many varieties of these abnormalities, the most important of which include the following:
Anomalously connected pulmonary veins and cor triatriatum.13,14 Anomalous connection of the pulmonary veins (to the right atrium, systemic or hepatic veins, or the coronary sinus) can occur with or without obstruction to egress of blood from the veins. In the former, pulmonary vein pressure is usually elevated, and PH can be severe after birth.
Congenital and acquired structural abnormalities of the mitral valve, including supravalvar mitral ring.15–18 Rheumatic mitral valve disease is the most common of these abnormalities.
Narrowing of the extrapulmonary veins. This can be congenital, develop for occult reasons postnatally, 19 or develop after surgery to correct anomalously connected veins. 20
Left ventricular (LV) noncompliance. LV diastolic dysfunction is seen in multiple settings: with dilated, hypertrophic or restrictive cardiomyopathy; structural lesions causing increased LV pressure or volume load (e.g., aortic stenosis); systemic hypertension; in patients with congenital cardiac defects and a small LV.21,22 Heart failure and preserved ejection fraction and heart failure with reduced ejection fraction are the most frequent causes of PH due to reduced LV compliance. 21
Category 2: pulmonary venous stenosis/obstruction within the lung parenchyma
Acquired stenosis or atresia of the intrapulmonary veins. This occurs in several settings: idiopathic, in prematurely born infants with bronchopulmonary dysplasia, after surgical repair of anomalously connected pulmonary veins (including those not obstructed at time of repair), in patients with congenital heart defects without anomalous pulmonary vein connection, and under other circumstances.19,20,23–25 It seems unlikely that a single stenotic pulmonary vein can cause significant PH, 26 although manifest obstruction of one or more pulmonary veins in one lung can exist with occult obstruction of small veins in the contralateral lung, and additional obstructed veins can develop over time. 27
Pulmonary veno-occlusive disease. In this rare disease, there is stenosis and occlusion of venules and small veins and generally severe and progressive PH. 9
THE IMPACT OF PVH ON PVR: STRUCTURE, PHYSIOLOGY, AND REVERSIBILITY
Pulmonary arterial pressure (PAP) is increased with PVH, often only due to passive transmission of pulmonary venous pressure (i.e., PVR is unchanged), although PVR in this setting is highly variable and is frequently much increased (see the upper right panel of Fig. 1 in this article and Fig. 2 in Kulik et al. 31 ). In 5 reports of adults undergoing intervention for mitral valve disease (n = 96 patients), mean PAP ranged from 25 to 104 mmHg (mean ± standard deviation, 47 ± 12 mmHg), and 41% had mean PAP ≥50 mmHg.32–36 Most patients had little or no increase in PVR, but 4 large series reported 23%–29% of adults with mitral valve disease to have PVR ≥5 units.28,37–39 Data from Guazzi and Borlaug 37 indicate roughly the same for patients with LV noncompliance, and variability in PVR is also the case for children with pulmonary vein obstruction (personal observations), indicating that variability in PVR with PVH is a general phenomenon and not limited to mitral valve disease. The fact that many patients have normal PVR may be partly due to passive distention of pulmonary resistance vessels due to pulmonary venous hypertension.41,42
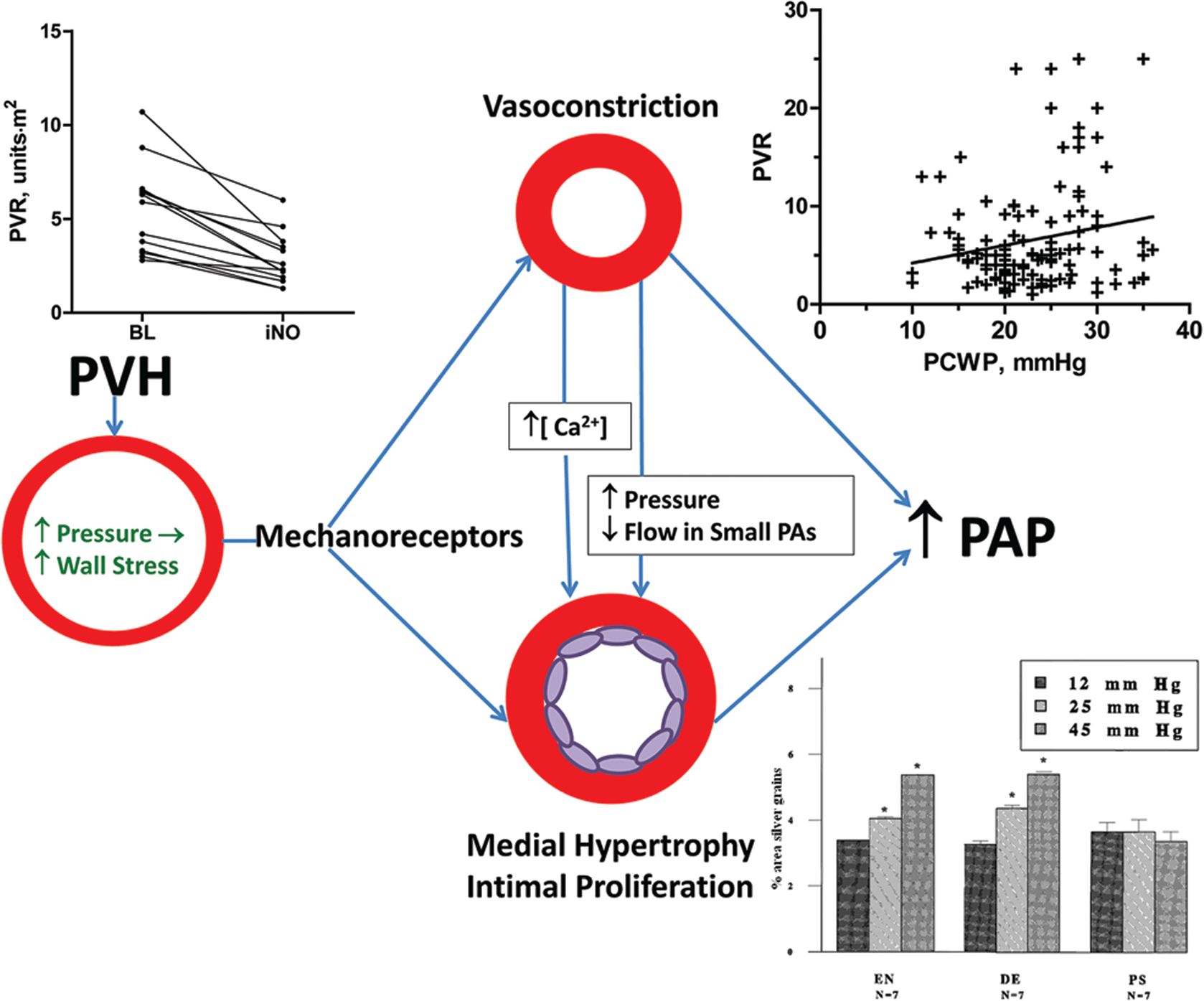
How pulmonary venous hypertension (PVH) causes increased pulmonary vascular resistance (PVR). Increased intravascular pressure increases wall stress in resistance-level pulmonary arteries (PAs), increasing stretch/tension in medial smooth muscle cells (SMCs). This stimulates mechanoreceptors in these cells, causing vasoconstriction, which reversibly increases PVR and also provokes structural changes. The latter may result from shared pathways for smooth muscle contraction and growth and/or reduction in blood flow in very small end and branch PAs. Increased stretch/tension may also directly (independent of vasoconstriction) stimulate medial hypertrophy and intimal hyperplasia. In the upper right panel, pulmonary capillary wedge pressure (PCWP) is plotted against PVR (pulmonary vascular resistance) in 114 adult patients with mitral stenosis (data from Wood et al. 28 ); PVR ranges from normal, despite very high left atrial pressure, to markedly elevated, despite only a modest increase in pulmonary venous pressure. The upper left panel shows the effect of inhaled nitric oxide (iNO) on PVR in 13 children with left atrial hypertension (data from Atz et al. 29 ), demonstrating that a component of increased PVR with PVH is often acutely reversible. BL: baseline, before iNO. The lower right panel shows the relative rate of protein synthesis in the media of rabbit PA strips in tissue culture was measured at wall stresses equivalent to various mean PA pressures using quantitative autoradiography. Protein synthesis increased with wall stress in an endothelium-independent manner; hydrostatic pressure did not alter protein synthesis. Adapted from Kolpakov et al. 30 DE: endothelium removed; EN: endothelium present; PS: hydrostatic pressure.
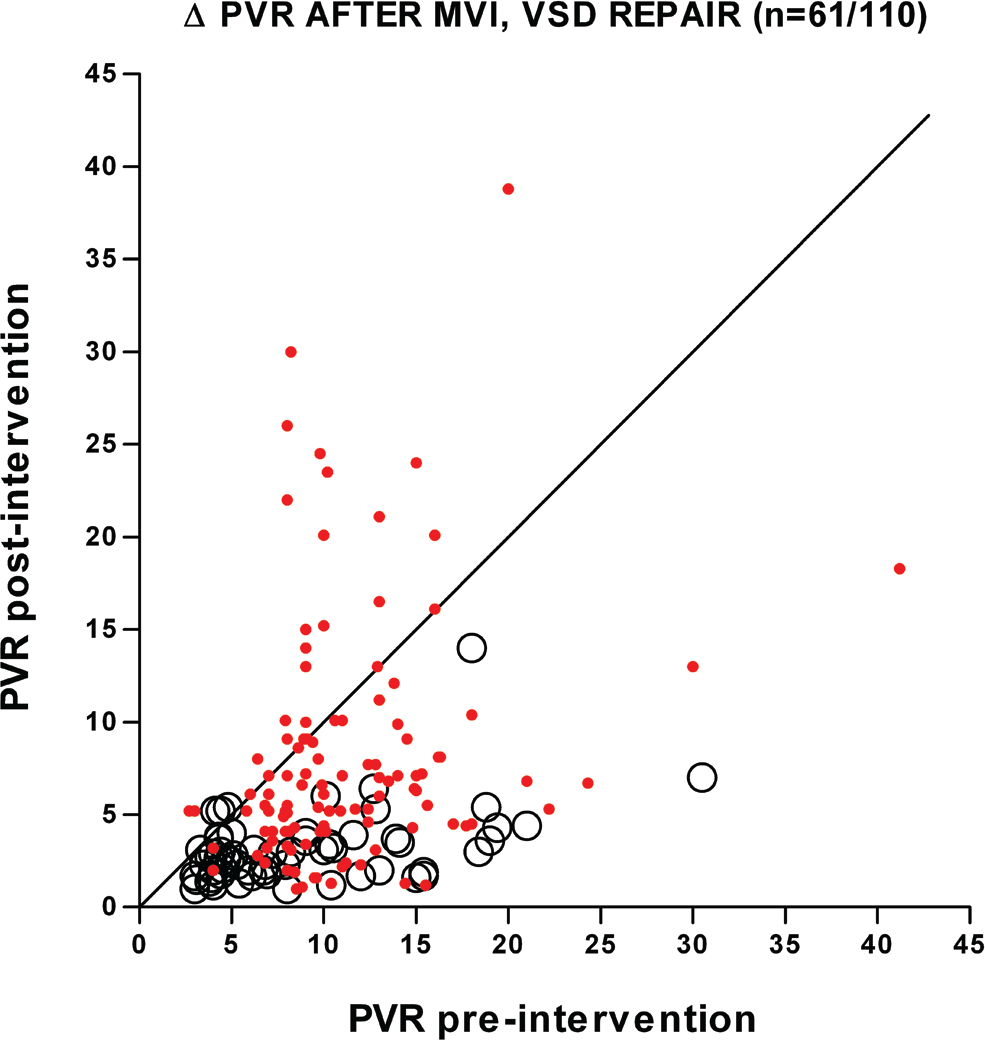
Change in pulmonary vascular resistance (PVR) after mitral valve intervention to effect relief of mitral stenosis/regurgitation (circles; n = 61 patients) or closure of ventricular septal defect (VSD; dots, n = 110 patients). Nearly all patients with mitral valve disease had a large decrease in PVR after relief of left atrial hypertension. Conversely, for patients with a VSD, the response was quite variable, and many had unchanged or increased PVR after repair. Adapted from Kulik. 3 MVI: mitral valve intervention.
Considerable note has been made of PH “out of proportion” to the magnitude of LA pressure (i.e., a transpulmonary gradient >12 mmHg).40,43 Some observers even suggest that this disproportionate increase in PAP may be due to factors independent of the PVH. 44 Although this notion may be useful in thinking about which patients might most likely benefit from pulmonary vasodilators (see below), it seems likely that “out of proportion” is actually a reflection of garden variety biological variability. Indeed, it has been long appreciated 45 that the lung's circulation demonstrates considerable variability in its response to multiple stimuli, including acute and chronic hypoxia,46,47 and chronic elevation of flow and pressure due to congenital shunting lesions 45 (Fig. 2). That is not to say that there is no cellular or molecular basis for this marked variability, just that it is not limited to the response of the pulmonary circulation to PVH. Comparing the genetic, proteomic, and metabolic characteristics of patients with striking elevation in PVR with PVH with those of patients evincing normal PVR despite severe PVH may someday yield insights into the mechanisms involved.
Increased PVR with PVH is due to pathological remodeling and active vasoconstriction
Wagenvoort and Wagenvoort 57 found little correlation between pulmonary hemodynamics and histological changes, although others have. I am aware of no information regarding the time course of remodeling, although, as noted above, intimal lesions have been described in young children, and pathological remodeling of PA and venous vessels occurs in utero with obstructed pulmonary venous return. 58
Evolution and resolution of PH
As previously noted, despite having PH for many years, adults and older children52,54,56,64 with mitral valve disease who have reduction of LAP with valve repair usually (albeit not invariably) show a substantial decrease or even normalization of PVR (Fig. 2); even patients with mean PAP >50 mmHg generally show a large reduction in PAP and PVR.28,63,65,66 Most available hemodynamic data are for ≤1 year of follow-up, but one large series demonstrated that the reduction in PVR lasts at least several years. 67
Reliable reduction of PVR with mitral valve replacement or repair probably also occurs in the first few years of life,31,54,56 although the available data are limited and far from definitive. (Published long-term follow-up data for patients with significant and isolated [i.e., without left-to-right shunting] PVH and PH at birth are scant, which is surely a reflection of the tendency of these patients to die early absent relief of the PVH.) This is noteworthy, because it is possible that long-standing PH since birth may be much less likely to resolve with relief of the cause than PH commencing after the pulmonary circulation has matured. 3
Remodeling and “reversibility” of increased PVR with PVH
The fact that PVR decreases over a matter of months after mitral valve intervention suggests that the decrease is partly due to favorable remodeling. Unfortunately, there is little documentation of what actually happens with the decrease in PVR, but one can speculate: smooth muscle hypertrophy/hyperplasia presumably regresses, and edema in the vessel walls is perhaps reduced. What happens to the intimal proliferation is unclear. Intimal proliferation and fibrosis do not imply a fixed increase in PVR with mitral stenosis,50–52,54 even though such lesions often portend an unfavorable outcome with shunting lesions. 68 This may be mostly a matter of degree: perhaps the fraction of the vascular bed occluded by intima is smaller with PVH than other forms of PH; the observation by Wagenvoort and Wagenvoort 50 that intimal lesions are rarely occlusive with PVH is consistent with this. Possibly the pattern of intimal proliferation is relevant. Using three-dimensional reconstruction, Yaginuma and co-workers 69 found that, with cardiac shunting malformations, intimal occlusion mostly affected small (100–150-μm diameter) PAs at branch points or at the terminal end of very small vessels. If, with PVH, intimal proliferation is mostly confined to arteries with somewhat larger diameters, it would have less impact on the cross-section area of the vascular bed, and favorable remodeling would therefore be mostly due to reduction of smooth muscle mass.
One investigator's analysis of data sets of hemodynamic information obtained at cardiac catheterization suggests that the hydrodynamics of PVH-PH differ from those of PH without venous hypertension: with PH, mean PVR and PA compliance are consistently inversely related when LAP is normal, but with elevated LAP (>20 mmHg), compliance decreases as PVR increases. 70 The reasons for this are unclear, but it could be that PVH stimulates changes in the geometry and mechanical properties of small pulmonary vessels different from those that occur in other forms of PH. The fact that plexiform lesions are seldom seen with PVH, even with long-standing and severe PH, also suggests that the architecture of vascular disease with PVH is, at least in some ways, distinct from that of some other forms of PH. Future investigations will hopefully better define the microanatomic and biological characteristics that distinguish PVH-related PH from other varieties of the condition.
WALL STRESS AND PVH-PH
Many molecules and pathways have been identified as being possibly relevant to pulmonary vascular remodeling and vasoconstriction, but it is still unknown for any type of PH to what extent these pathways are actually relevant, how they interact with other pathways, and which biological components have yet to be uncovered. 71 Abnormalities observed with other forms of PH have been demonstrated with PVH-PH (e.g., increased circulating endothelin-1 levels), but the meaning of this is unclear. For example, the fact that plasma endothelin-1 levels correlate with PAP in heart failure 72 does not establish a role for the peptide in the genesis of the PH. I will thus refrain from speculation regarding the usual PH molecular suspects, recognizing that some pathways that are relevant in other forms of PH will ultimately be shown to be involved in PVH-PH. Focus will be directed on the hypothesis that the fundamental cause of PVH-increased PVR is increased intravascular pressure, leading to increased wall stress and/or stretching of PAs and veins. This hypothesis has intuitive appeal, given that increased intravascular pressure is the obvious consistent consequence of PVH. The fact that relief of PVH usually substantially reduces PVR also powerfully suggests that increased intravascular pressure plays a signal role. Finally, increased wall stress causes pathologic remodeling in systemic arteries.73–77
Note that intravascular pressure is not the only plausible relevant mechanical force. The cross-sectional area of the pulmonary vascular bed is presumably reduced with PVH-increased PVR, implying (absent lower flow) that shear stress is increased. A general discussion of the effect of shear on vascular biology is left to previous reviews,78,79 although attention will be given to a specific way that endothelial shear may modulate the effect of increased wall stress.
There are at least three ways that increased pressure in pulmonary blood vessels may increase PVR: myogenic vasoconstriction, pathological remodeling induced by increased wall stress, and vasoconstriction induced by distention of large (main and proximal branch) PAs.
Myogenic vasoconstriction
Contractile activation of smooth muscle can be elicited by increased stretch or tension in smooth muscle itself (although it is modulated by endothelial cells) and plays an important role in adjusting tone in at least some systemic vascular beds. 80 There is ample reason to think that myogenic constriction can also occur in the lung: first, stretch or increased intraluminal pressure stimulates constriction in segments of small PAs in vitro in multiple species,81–85 and second, myogenic tone, at physiologically relevant pressures, has been demonstrated in the in situ lung of the ovine fetus86,87 and (pace assertions that this response is lacking in normoxic mature animals 88 ) mature feline, canine, and ovine lungs.42,89,90
An apparent objection to the pulmonary myogenic tone hypothesis is the observed effect of exercise on PVR (it generally decreases it). Passive distention of small pulmonary vessels at least partly accounts for the flow-mediated decrease in PVR, 91 which seems inconsistent with the notion of distention-mediated vasoconstriction. Storme and colleagues, 86 however, showed that, in the fetal lung, vasoconstriction with ductal compression occurs only when endothelial release of NO is blocked using NO synthase inhibition. They surmise that increased PA flow with ductal constriction causes endothelial release of NO, which prevents smooth muscle activation, but when NO production is inhibited, myogenic contraction is made manifest. Inhibition of myogenic contraction by flow-stimulated NO release could also occur with exercise,92–94 explaining why distention of small PAs in this setting does not cause vasoconstriction. In fact, the magnitude of endothelial modulation of myogenic tone could at least partially account for variability in PVR with PVH: Cooper and colleagues, 95 using NG-monomethyl-l-arginine to inhibit NO production, found that, in adults with PH due to left ventricular noncompliance, those with increased PVR had less baseline NO modulation of PVR than patients with normal PVR. Whether this is due to a limited capacity to generate NO or reduced production for other reasons is unclear, but some patients with PVH and increased PVR show substantial vasodilation with acetylcholine infusion,28,96 indicating that the endothelium can have the capacity to produce NO but not generate it maximally at baseline.
The myogenic tone hypothesis as an explanation for PVH-related pulmonary vasoconstriction is currently mostly that. There is still much to be learned about this phenomenon in the lung. To what extent does it occur in humans? Is the magnitude of stretch caused by PVH-related increased intraluminal pressure enough to stimulate myogenic contraction? Does it operate in the setting of chronically increased intraluminal pressure? What non-smooth-muscle cells and circulating or paracrine factors modulate the response? Why do vasodilators only partly abolish increased PVR with PVH and have no effect at all in some people? Presuming myogenic tone is present and important in the pulmonary circulation, is its mechanism sufficiently distinct from that in systemic vessels that specific inhibition is a possibility? Definitive confirmation and characterization of the role—and possible pharmacologic modulation—of myogenic tone in PVH-PH will likely have to wait until selective antagonists for stretch-operated channels and/or other components of the machinery of mechanically induced contractile activation are developed.74,80
Alas, our fragmentary understanding of the molecular mechanisms underlying the SMC stretch response seriously constrains our ability to better characterize it in vivo and manipulate it. Although investigators have learned a lot about how mechanical forces are translated into biological effect in SMC, a granular picture of the mechanisms involved has yet to evolve. Transmembrane Ca2+ flux and Ca2+ release from intracellular stores are key early events, but exactly what mediates them is unclear. Stretch-responsive elements in vascular SMC likely include ion channels, possibly including nonselective cation channels dubbed stretch-activated channels (SACs) and multiple others (e.g., transmembrane receptor potential channels, BKCa channels, Kv channels, ENaC channels, and ClCa channels). Some of these channels (e.g., SACs) increase [Ca2+] via membrane depolarization, whereas others modulate the increase (e.g., BKCa channels). Alternatively, or in addition to stretch-sensitive channels, cytoskeletal elements may serve as mechanotransducers. For example, integrins, binding to matrix proteins and cytoskeletal elements, induce changes in the latter and have received much attention as putative primary mechanotransducers. Multiple other structures or molecules (e.g., caveolae and G proteins) may also serve as mechanosensors in SMC.76,80,97,98 Considerably more work remains before we learn enough to allow the stretch response to be selectively manipulated toward investigative and therapeutic ends.
Pathological remodeling induced by increased wall stress
Pathological remodeling induced by increased wall stress can occur either as a direct consequence of increased vascular tone or as a reaction to increased stress per se. One possible explanation for increased vascular resistance in systemic hypertension is that contraction of small arteries becomes “entrenched.” With this “eutropic” remodeling, the lumen of the arteries is reduced in diameter without increasing smooth muscle mass.99,100 In an analogous way, might myogenic contraction directly lead to the structural changes seen with PVH and other forms of PH? Perhaps the first question one might ask is whether pathologic remodeling in the lung is eutrophic, or whether there is increased smooth muscle mass in remodeled small vessels? We are not aware of information for PVH-PH (most reports describe medial hypertrophy but do not comment on vessel diameter), but with a large ventricular septal defect, the external diameter of small (generally intraacinar) PAs is normal or reduced much more often than it is dilated, and the luminal diameter is reduced by virtue of increased medial thickness.101–104 Likewise, in multiple experimental models of increased pulmonary blood flow with or without increased PAP, small PAs are usually of normal or reduced diameter.105–107 Whether smooth muscle mass is normal or increased cannot be determined from the data presented, but reduced vessel diameter (and thickened media) is consistent with eutropic remodeling. Although such remodeling would not directly account for dilation lesions (which are not seen with PVH-PH but are seen with other forms of PH), increased PAP due to narrowed resistance vessels could lead to other microarchitectural abnormalities.
Intimal proliferation is a feature of pathological remodeling in some patients with PVH-PH, and there are at least two ways that this might be linked with myogenic vasoconstriction. First, reduced flow in systemic arteries, or vascular grafts, can cause neointimal proliferation.99,108 Because the pulmonary microvascular bed branches dichotomously (and also has lateral branches), distal constriction of the small branches will reduce flow in those vessels; reduced flow in these very small arteries could possibly stimulate neointimal proliferation. The pattern of intimal hyperplasia demonstrated by Yaginuma and colleagues 69 in patients with congenital cardiac shunting defects and PH—that is, occlusion of very small branches arising from an unaffected larger artery—is consistent with this notion.
Second, systemic veins and arteries subject to high intraluminal pressure develop intimal hyperplasia. Although vascular injury and inflammation may account for some of this effect, stretch probably also causes neointima independently of these factors.77,109–111 By increasing PAP via constriction of small PAs, myogenic contraction might thus serve as the inciting stimulus for intimal hyperplasia of more proximal arteries. To what extent the biology of relatively large systemic veins and arteries applies to very small PAs is unclear, but it is noteworthy that, in a murine model of veins subjected to high pressure, neointimal formation is in part dependent upon expression of early growth response factor-1, 77 a transcription factor associated with intimal lesions in at least 2 forms of PH;112,113 similar observations have been made for tissue inhibitor of metalloprotinease-1.111,114
Finally, because myogenic contraction involves transmembrane Ca2+ flux,80,115,116 and SMC growth and migration require increased intracellular [Ca2+],117,118 these cellular events related to contraction might simultaneously augment pathological remodeling stimulated by other factors.
Whether or not myogenic contraction is an inciting stimulus for pathological remodeling in the lung, multiple studies of in vitro systemic and (to a much lesser extent) PA SMC and vascular segments have shown that stretch increases SMC growth and matrix protein synthesis,30,119–123 stimulates intimal hyperplasia, 77 and has multiple other remodeling-relevant effects (e.g., apoptosis and migration).73,74 Over the last 30 years, many studies have been published regarding the impact of mechanical forces on many types of cells and tissues, and it now is axiomatic that wall (and shear) stress are important regulators of vascular architecture.
There is still much to be learned. (i) Most studies compare stretched with unstretched cultured cells, but in vivo, it is the magnitude of mechanical stimulus—not its presence versus absence—that is relevant. If an SMC subjected to a 5% periodic strain (due to pulsatile expansion of the artery) is subjected to an 8% strain due to higher intraluminal pressure, how does it respond? (ii) Stretched cultured cells are almost always attached to a two-dimensional surface, but they behave differently when embedded in a three-dimensional matrix, which better reflects their in situ geometrical arrangement. 74 (iii) In experiments using vessel segments, they are usually statically stretched,30,121,122,124 whereas cyclical stretch pertains in vivo. (iv) Cells from large, rather than resistance, arteries are used, and the vast majority of experiments use systemic SMC; there are few studies of PA SMC or vascular segments. Because at least some PA SMC characteristics differ according to the size of the vessel, 125 experiments using small (<300-μm diameter) vessels or cells from them would be required to know how the body of work noted above applies to the PAs that control PVR. (v) Upon which cells does wall stress act, and how do they modulate contractility and growth? Although most studies have focused on SMC, cultured systemic endothelial cells respond to pulsatile stretch by increasing production of angiotensin II and superoxide. 126 Adventitial cells could also be involved.
More studies of the impact of mechanical forces on cellular and molecular events in whole tissues and the in vivo pulmonary circulation are needed, but this is challenging. PVH is the only definable stimulus that increases PAP without increased flow, alveolar hypoxia, genetic modification, toxins, or other pharmacological agents, but these studies are technically more difficult than other models of PH. Few have addressed cellular and molecular mechanisms involved in pathologically remodeling.127–129 Ultimately, however, a deeper comprehension of the mechanisms of all types of PH must include a more precise reckoning of how increased wall stress regulates vascular biology.
Vasoconstriction induced by distention of large (main and proximal branch) PAs
Multiple investigators have found that distention of the main or proximal branch PAs acutely increases PVR, presumably via neutrally mediated constriction of resistance vessels. These studies have used closed130–136 and openchest137,138 canine and ovine preparations, and there is one report involving human infants undergoing cardiac catheterization. 139 The magnitude of PAP increase is variable, generally being modest but sometimes considerable. Infiltration of the large PAs with xylocaine distal to the distended segment130,133 and surgical disruption of the adventitia 134 reduce or abolish the vasoconstriction, as does 6-hydroxydopamine,133,134 suggesting that nerves running from large to resistance PAs mediate the vasoconstriction. If so, the nerves are apparently not catecholaminergic, because alpha receptor blockade does not abolish the response.131,133 Ganglionic blocking agents, sympathectomy, and vagotomy do not abolish the vasoconstriction.130,131
Not all investigators have found large PA distention to cause distal vasoconstriction.140–142 Indeed, one investigator responsible for multiple articles describing this vasoconstrictor response (Juratsch) subsequently collaborated on a study suggesting that the technique used by him (inflation of a “Laks” catheter in the main PA to cause distention) may occlude a branch PA and hence increase PAP due to increased flow rather than vasoconstriction. 141 However, given that multiple investigators have demonstrated distention-mediated vasoconstriction using multiple techniques, it is hard to discount the possibility that this “reflex” is an important feature of the lung's circulation. That said, the magnitude of distention required to cause vasoconstriction is rarely quantified, and it is unknown whether the surely gradual increase in PA diameter accompanying the gradual onset of PH with PVH would be sufficient to stimulate much, if any, vasoconstriction. It seems more likely that the stretch vasoconstrictor response mediates or augments acute increases in PAP occasioned by exercise or other stimuli in people with preexisting PH rather than being an important factor in the genesis of PH.
TREATING PVH-PH
Over half a century ago, cardiologists caring for and performing hemodynamic studies involving people with mitral stenosis appreciated that LA pressure can exceed serum oncotic pressure, putting these patients at risk for pulmonary edema. They suggested that increased resistance to flow through precapillary arteries may be protective, shielding capillaries from high pressure at the cost of limiting cardiac output.1,28 Paul Wood, the acerbic “gale force wind of British cardiology,”143,144 concluded that pulmonary edema, congestive hemoptysis, and paroxysmal orthopnea were less common in patients with mitral stenosis and high PVR than in those with lower resistance. 34 Reducing precapillary constriction with vasodilators can indeed provoke pulmonary edema in some patients with PVH.8–11 On the other hand, at least one clinician, practicing early in the days of mitral valve palliation, concluded that those with mitral valve disease and high PAP had increased risk of dyspnea attacks relative to those with lower pressure, 60 and it is certainly plausible that, for some patients, limitation of right ventricular output due to PH, not lung water, is what causes most symptoms. Pharmacologic modulation of the body's (apparently excessive) response to myocardial dysfunction (diuretics, angiotensin converting enzyme inhibitors, and beta blockers) is foundation therapy for congestive LV failure, and one could argue analogously that carefully monitored use of agents aimed at reducing excessively increased PVR could be useful for some patients with PVH.
However, defining what role PH-targeted therapy may play in the context of PVH-PH is complicated by the current demographic characteristics associated with this derangement. Because mitral valve disease is now largely susceptible to mechanical alleviation, PVH (at least in adults) is mostly a consequence of LV dysfunction. Clinical trials of PH-targeted therapy have therefore involved patients with an additional and often severe physiological liability related to the left heart. So far, at least, there is little to suggest that vasodilators are helpful in patients with LV dysfunction and PVH-PH, and some appear to be harmful. As has been well-reviewed by Guazzi and Arena, 21 trials of prostacyclin and endothelin receptor antagonists in patients with congestive heart failure have not yielded significant clinical or hemodynamic benefit or have actually exacerbated heart failure or hastened death. Calcium channel blockers have received little attention in this regard, perhaps because of early studies showing them, with congestive heart failure, to not confer survival benefit and safety concerns regarding their use in this context.145,146 A recently reported 16-week randomized, placebo-controlled trial of riociguat in 201 patients with heart failure with LV systolic dysfunction and PH (baseline mean PAP, ***?40 mmHg) found that this guanylate cyclase stimulator had no significant effect, relative to placebo, on the primary end point of PAP (although cardiac output was increased, and there was improvement in a health-related quality of life index). 147
The story may be different for sildenafil. Multiple small studies of patients with heart failure and systolic dysfunction suggest that this medication improves pulmonary vascular hemodynamics and sometimes functional status (reviewed in Guazzi and Arena, 21 Cooper et al., 148 and Redfield et al. 149 ). For example, Lewis and colleagues, 150 in a randomized 12-week placebo-controlled trial, found that sildenafil decreased PVR, increased peak oxygen consumption with exercise, and had other salutary clinical effects in patients with systolic heart failure and PH. More information is pending: the Sildenafil in Heart Failure (SilHF) trial, a multicenter, randomized, placebo-controlled clinical trial of sildenafil for patients with heart failure and systolic LV dysfunction, is enrolling patients (October 2014). 148 In this 6-month trial, inclusion criteria include (among others) a systolic PAP >40 mmHg (by echocardiography), and the co-primary end points are patient global assessment and 6-minute walk test.
On the other hand, two studies involving patients with heart failure but preserved LV systolic function had disparate findings. Guazzi et al. 151 reported that sildenafil significantly improved LV compliance and pulmonary hemodynamics after 6 and 12 months. (The patients had baseline mean PAP of ?38 mmHg and PVR of ?3.6 Wood units.) However, the much larger RELAX trial demonstrated no difference in peak VO 2 , 6-minute walk distance, or mean clinical status rank score. 149 (The median systolic PAP by echocardiography was 41 mmHg, considerably lower than in the Guazzi trial, assuming that the noninvasive estimate was accurate.)
Lacking clear benefit, and with evidence of unfavorable effects with some agents, routine use of targeted PH therapy to treat PVH-PH is currently discouraged.21,43,147,152 However, the question of whether pharmacologic therapy could be beneficial is a complex one and is not fully answered by existing studies. It is perhaps useful to speculate on possible reasons why these medications have not appeared to be helpful in the context of PVH-PH, despite their utility in class 1 PH.
The drugs tested are ineffective in reducing PVR in PVH-PH. Although this is likely true for some patients and some drugs (e.g., riociguat), studies have shown that epoprostanol and sildenafil effected at least as much reduction in PVR in patients with heart failure as with idiopathic pulmonary arterial hypertension (PAH).150,151,153,154 The fact that many patients with PH due to mitral valve disease are “reactive” when tested with acute vasodilators also suggests that, as a group, patients with PVH-PH should be at least as likely to reduce PVR with chronic vasodilator therapy as other patients with PH.
Unfavorable effects of the medications may be more important than any hemodynamic benefit. Increased lung water is an obvious possible pernicious adverse effect, but there could be any number of others, some known (i.e., fluid retention with endothelin receptor antagonists 155 ) and others not yet identified. The Flolan International Randomized Survival Trial trial, in which epoprostanol was given to patients with LV dysfunction, is illustrative. 153 Both PAP and PVR were significantly reduced, but the study was halted early because of increased mortality among treated subjects.
In patients with left heart failure, the physiological liability related to LV dysfunction overwhelms that contributed by PH. This seems likely to be the case when PAP is only modestly elevated and right ventricular (RV) function is adequate, and it could be true even with markedly elevated PAP and severe LV dysfunction. Janicki et al. 156 found that patients with pulmonary vascular disease were able to generate similar cardiac outputs with exercise as patients with heart failure despite having considerably higher PAP, suggesting that LV rather than RV function can be rate-limiting in patients with LV failure and PH. Also, consider that, even when targeted agents are used for patients with PH and normal LV function (e.g., idiopathic PAH), their effect on hemodynamic parameters and exercise capacity is usually quite modest. 154 With severe LV systolic or diastolic dysfunction, the LV may not be up to increasing its output or reserve on account of a small increment in RV performance.
Also, surely patients in any clinical trial who have little elevation in PVR (especially with good RV function) have much less, if anything, to gain from a reduction in that variable compared with those patients with markedly elevated PAP. Data from the trials noted above are consistent with this. The Lewis study 150 found that the change in oxygen consumption with sildenafil correlated with baseline PVR—those with the highest pretreatment PVR had the greatest increase in oxygen consumption with the drug. In the Guazzi trial of sildenafil with left heart failure, 151 the absolute decrease in PVR was (not surprisingly) greatest in those with the highest baseline resistance. With a few exceptions, clinical trials of pulmonary vasodilators with left heart failure have not specified a minimum PAP for inclusion or required only modest elevation, meaning that, a priori, some fraction of subjects stood relatively little to gain from a reduction in PVR. In fact, the difference in findings between the RELAX and Guazzi sildenafil trials might, at least in part, relate to the fact that patients likely had higher PAP (and more RV dysfunction) in the latter trial. 149 The greater the percentage of patients with relatively low PAP, the less likely that benefit will be demonstrated, even if some people with higher pressure have significant improvement.
Uncovering what, if any, role targeted PH pulmonary therapy can play in people with PVH may therefore require clinical trials with enrollment limited to patients with substantial PH (and perhaps RV dysfunction); alternatively, a subanalysis of outcomes among patients with high PAP could be performed for large studies that contain subjects with a range of PAP, assuming a sufficient number of patients. However, this poses practical problems. First, accurate determination of baseline pulmonary vascular hemodynamics, given the limitations of echocardiography in accurately estimating PAP, 157 requires cardiac catheterization, with the attendant expense and logistical complications. Second, enrollment of an adequate number of subjects is more challenging if entry criteria are more stringent and subjects need to consent to invasive studies. Alternatively, n-of-1-like trials, in which a smaller number of patients are more intensively monitored, 158 may yield generalizable information and be a means of tailoring therapy to individual patients. Echocardiographic screening (for PAP and RV and LV function) and clinical characteristics could identify patients most likely to benefit from targeted PH therapy, and these people could be carefully evaluated for clinically meaningful improvement with therapy. The medication would be discontinued absent positive effect; reevaluation after being switched to placebo could be undertaken for those who appeared to derive benefit. Although expensive and cumbersome, this sort of approach may be a way to rationally use agents that, while showing sufficient promise (e.g., sildenafil) in small trials, do not prove helpful when applied to a mixed (in terms of PAP/PVR and RV function) population of patients. Alternatively (or additionally), the response of the pulmonary circulation to exercise may better stratify patients relative to the likelihood of a favorable response to targeted therapy. 159
SUMMARY
Increased PVR due to PVH is a clear demonstration of the effect of increased pressure per se on pulmonary vascular tone and structure and is therefore of special interest: the impact of any process that increases PAP (e.g., hypoxia, toxins, and genetic causes) may be magnified by the inherent tendency for PH to beget more PH. Even were the mechanisms involved in the genesis of, for example, idiopathic PAH to be distinct from those operative in PVH-PH, understanding the latter could lead to therapies to ameliorate the effects of the former. PVH-PH confirms the huge variability in the pulmonary circulation's response to vasoconstrictive/pathological remodeling stimuli and offers up a relatively clean model to investigate the biology of this variability. It also shows that, more palpably than in any other form of PH, even long-standing and severely increased PVR can abate with elimination of the inciting stimulus. We do not know what fraction of this resolution is attributable to release of vasoconstriction, reduction of medial hypertrophy with or without intimal hyperplasia, or other structural vascular changes, but this favorable physiological/structural remodeling might serve as a paradigm for pulmonary vascular healing with other forms of PH.
We need much better characterization of the molecular mechanisms of stretch/tension transduction on SMC, including delineation of any differences specific to pulmonary blood vessels. This may lead to means of interfering with mechanically stimulated contraction and remodeling in the pulmonary circulation, which would be invaluable for better defining the role that increased pressure plays, and to developing new types of therapy for all forms of PH.
Despite its capacity for reversal, PVH-PH is an important clinical problem, especially because LV diastolic dysfunction lacks definitive therapy. Clinical studies thus far mostly suggest that currently available targeted PH therapy is not useful—or worse—for the general population of patients with PVH related to left heart dysfunction. However, there are a few reports suggesting that a subset of patients may benefit from such therapy, and the question of whether current or future medications used to alleviate other forms of PH can be safe and useful in this context still hangs fire. It may be that a different way of answering this question is needed, in which patients whose pulmonary vascular phenotype drives their physiology as much as their left ventricular phenotype are treated and evaluated.
