Abstract
Despite the significant mortality and mobidity benefits being obtained with the targeted therapies in patients with pulmonary arterial hypertension (PAH), mid- to long-term survival of patients with this disease has remained unsatisfactory. For earlier and reliable risk stratification in PAH and tailoring the dynamic management strategies, various risk assessment models have been developed. Currently available risk reduction strategy recommended by the European Society of Cardiology (ESC)/European Respiratory Society (ERS) 2015 Pulmonary Hypertension Guidelines has been utilized in three recent registries. In this review, we evaluated the risk prediction models and management algorithms in this setting and propose an alternative parametric display, a bull’s eye, dart table scheme for ESC/ERS goal-orientated risk reduction strategy in patients with PAH.
Although advances in the treatment opportunities of pulmonary arterial hypertension (PAH) with targeted therapies (TT) have provided significant mortality and morbidity benefits in this relentlessly progressive disease for the last two decades compared to those in the pre-TT era, mid- to long-term survival of patients with severely symptomatic PAH has remained poor.1–16 Therefore, earlier and reliable risk stratification in PAH is crucial for the individualization of management strategies by selecting patients who are prone to rapidly progessive deterioration and need more aggressive TTs such as upfront or sequential dual or triple drug combinations including parenteral prostacyclins.1–16
Cumulated real-life data which have been derived from multiple registries and other cohorts in the PAH population have enriched our understanding and widened perspectives for this disease regarding the reliable risk prediction model, the appropriate cohort designs, i.e. retrospective versus prospective or incident versus prevalent cohorts, the reliable statistical models to overcome the limitations of cohort data such as left truncation, survival, and immortal time biases, and varying risk hazards at different time sequences of the disease course.1–10,17–25 The ideal risk assessment model in PAH should meet several needs. It should be as simple as possible to increase the availability in routine daily practice.1,2,10,11,16–27 On the other hand, it has to cover the complexity of the multiple requirements of the course of this disease; it should incorporate evidence-based measures with precise cut-off limits and “weighted” predictive ability derived from sizable well-defined cohorts; and finally, it should be validated internally and externally for all spectra of PAH subgroups, clinical settings such as incident versus prevalent patients, treatment-naive versus on-treatment status, regardless of the time point during the course of disease.1,2,10,11,17,18,20–27
Since the development of the first and classical survival estimation model, the National Institutes of Health (NIH) equation representing the survival status of PAH before entry of TTs to clinical practice, several prediction models such as Pulmonary Hypertension Connection (PHC), French Pulmonary Hypertension Network (FPHN) Registry, and Registry to Evaluate Early and Long-Term Pulmonary Arterial Hypertension Disease Management (REVEAL) risk calculators have also been proposed for risk stratification at baseline evaluation and during follow-up.1,10,11,18,20–25 The NIH and PHC survival models have been based on three identical hemodynamic (HD) measures, mean pulmonary artery pressure (mPAP), cardiac index (CI), and mean right atrial pressure (mRAP), but survival estimates (SEs) have been calculated by two different equations.1–18 The PHC equation has been proposed as a novel approach addressing the advances within the two decades of the TT era in contrast to those in NIH model. The comparisons between NIH and PHC equations showed the that second model provided a more realistic SE consistent with observed survival (OS), whereas the NIH equation tended to underestimate the recent improvements in PAH survival with TTs.1–18 Moreover, the other approach, the FPHN registry equation comprising three variables—gender, 6-min walking distance (6MWD), and CI—has been reported to provide SE consistent with OS in patients with PAH.10,11 A comparison between FPHN and PHC equations showed that the OS was similar to the SE predicted by PHC equation whereas the FPHN equation overestimated OS. 18
The more complicated REVEAL risk stratification model has included 15 high-risk and four low-risk variables, and has also provided a risk calculator internally validated for one-year SE in patients with PAH.19–25 This calculator has been shown to discriminate risk strata at baseline and at re-evaluation at one-year control visit.19–25 The application of this score to a pivotal PAH trial database, the 12-week PATENT-1 and open-label PATENT-2 extension studies of riociguat, also showed that risk scores both at baseline and week 12 and change in this score were significant predictors of survival and clinical worsening-free survival. 23 These results support the long-term prognostic value of this model in a controlled study population. However, inclusion of the pulmonary vascular resistance (PVR) cut-off value as high as > 32 Wood units into the high-risk variables has remained the most criticized limitation of this comprehensive model.19–25
The assessment for the external validity of the FPHN equation and the REVEAL risk score calculator for SEs showed that application of FPHN parameters to REVEAL and REVEAL risk scores to FPHN demonstrated high probabilities of concordance for hazard ratio (HR) (HR = 0.72; 95% confidence interval [CI] = 0.64–0.80, and HR = 0.73; 95% CI = 0.70–0.77), respectively. 25 Each model provided good discrimination and calibration for SEs in the other cohort. These results also suggest the prognostic generalizability of two different models in geographically different PAH populations. 25
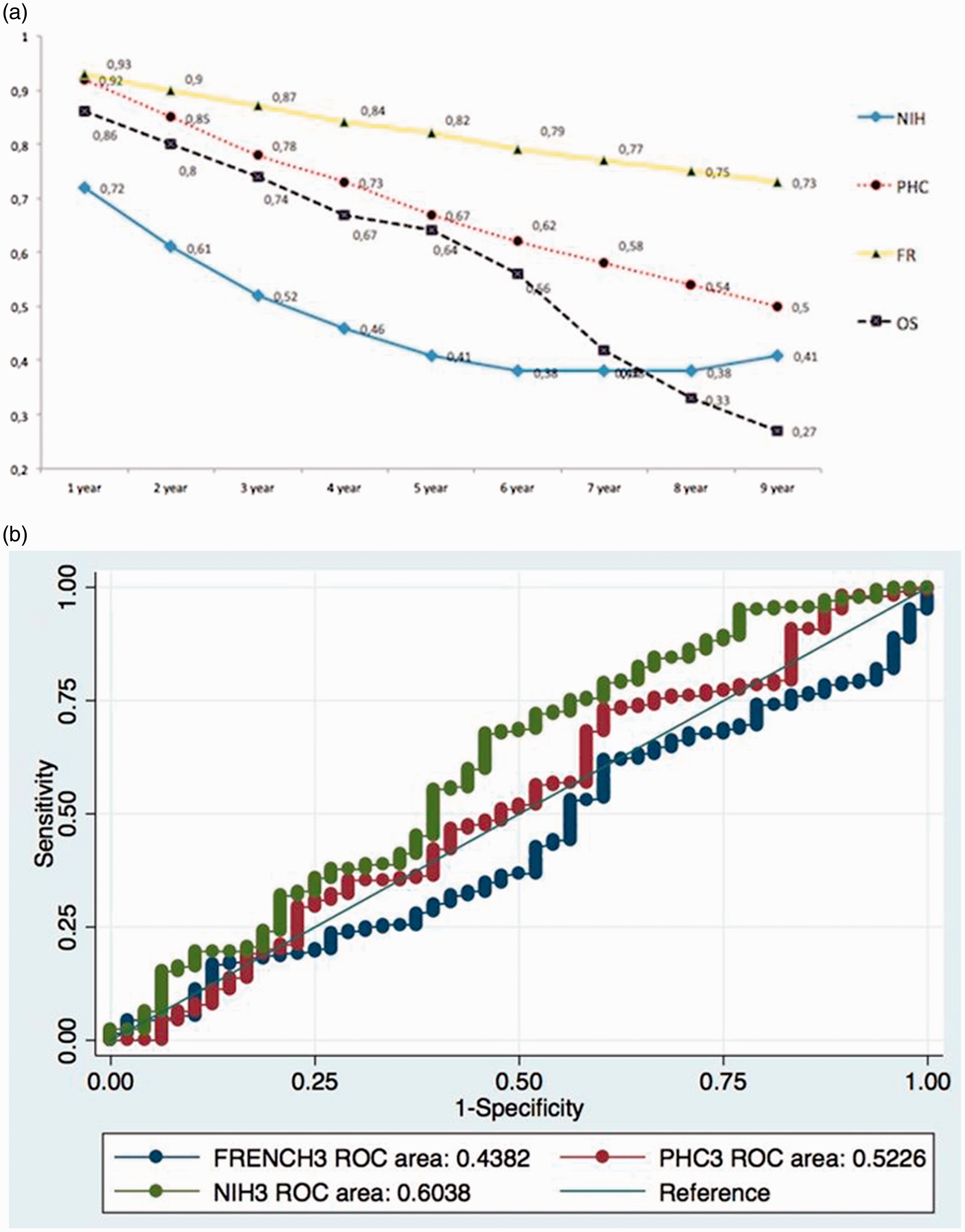
Although both NIH and PHC equations have been validated for SEs up to a three-year period, we compared the SEs predicted by the NIH, PHC, and FPHN equations for more extended durations up to nine-year follow-up periods in our single-centre study, EvalUation of Pulmonary Hypertension Risk factors AssociaTEd with Survival (EUPHRATES) (Fig. 1a).
28
The FPHN model was found to overestimate the OS at each time point of the follow-up in our PAH cohort (Fig. 1). Although the NIH versus the PHC equation underestimated the OS for seven years of follow-up, the NIH model was documented to successfully predict the trend of progessive decrease in OS after this time point (Fig. 1).
28
However, the consistency of the PHC equation was found to attenuate after five years of follow-up despite the utilization of TTs including dual or triple combinations (Fig. 1).
28
These results seem to suggest the failure of the currently available treatments in PAH and the necessity of more efficient, tailored, and dynamic management strategies.
(a) Comparisons of three survival estimate (SE) models including National Institutes of Health (NIH), Pulmonary Hypertension Connection (PHC) and French Pulmonary Hypertension Network Registry (FR) in relation to observed survival (OS).
28
(b) The receiver operating curves (ROC) and area under curve values of the SEs by NIH, PHC and French Pulmonary Hypertension Network Registry for OS.
28
As a general rule, statistical validation of intermediate endpoints for chronic diseases has been adopted to require an explanation of 50–75% of the exposure-outcome relationship of interest with these variables.2,26,27 Although the vast majority of the available TTs for PAH have been approved according to the change (Δ) in 6MWD as a clinically important surrogate end-point, validity of Δ6MWD has remained unproven.30–32 Baseline and final 6MWD, but not Δ6MWD, have been documented to predict clinical outcome of PAH.30–32 A pooled analysis revealed that TTs decreased the probability of a clinical event (summary odds ratio [OR] = 0.44; 95% CI = 0.33–0.57) and Δ6MWD accounted for only 22.1% (95% CI = 12.1–31.1%) of the treatment effect (P < 0.001). 30 Although the average difference in Δ6MWD favoring TTs over placebo was 22.4 m (95% CI = 17.4–27.5 m), meta-regression conducted among 21 drug/dose-level combinations showed a significant threshold value of 41.8 m. 30 Therefore, Δ6MWD has not been adopted as a reliable surrogate for PAH outcome.29–31 Similarly, an analysis from the REVEAL cohort also showed that no 6MWD improvement threshold, but worsening of the 6MWD, was significantly associated with prognosis. 30 Moreover, validity of TT-induced improvements in pulmonary HD measures as the possible surrogates for short-term clinical outcomes in PAH has also been questioned. A patient-level pooled analysis of four randomized, placebo-controlled PAH trials revealed that TTs significantly improved the mRAP, mPAP, PVR, and CI at 12 weeks (P < 0.01 for all), but these changes accounted for only 1.2–13.9% of the overall treatment effect. 32 Another study-level meta-analysis also yielded similar results and showed that risk reduction in the composite outcome (OR = 0.3; 95% CI = 0.3–0.5) with TTs could not be predicted by HD improvements. 31
In our EUPHRATES study comprising 481 patients with pulmonary hypertension (PH), baseline functional class (FC), PVR, and history of clinical worsening episode (CWE) after initial assessment, but not other baseline clinical and biochemical and treatment characteristics, diastolic pulmonary gradient, or other HD measures, were found to predict survival. 33
In another study investigating the prognostic impact of changes in HD, functional and biochemical variables after initiation of TT, changes in FC, CI, mixed venous oxygen saturation (SvO2), and N-terminal pro-brain natriuretic peptide (NT-proBNP) at first evaluation compared with baseline measures were proved to be independent predictors of subsequent outcome. 34 According to the change and satisfaction status in each variable at first evaluation, four clinical conditions were defined: group 1 = persistently satisfactory; group 2 = improved; group 3 = deteriorated; and group 4 = persistently unsatisfactory. 34 Although the strata of groups 3 and 4 versus groups 1 and 2 for each measure were associated with significant differences in survival, the incremental prognostic impact of various combination probabilities of the on-treatment changes have not been tested in this study. 34
A practical approach for risk stratification and definition of treatment goals in PAH has been recommended in the European Society of Cardiology (ESC)/European Respiratory Society (ERS) 2015 PH Guidelines. 35 This model comprises three risk columns according to the estimated annual mortality—low-risk (<5%), intermediate-risk (5–10%), and high-risk (>10%) status—and has incorporated measures of clinical status, exercise capacity, neurohumoral, cardiac imaging, and invasive HD variables. 35 However, non-modifiable risk factors have not been included into this algorithm targeted to achieve the low-risk status. Moreover, diversity of the source of variables is one of the crucial shortcomings of this risk reduction strategy. 35 The components of this algorithm and their specific cut-off limits have been derived from different registries or cohorts, and measures of overall model have not been validated with a single multivarable analysis. More importantly, there is no logical reason to assume all of these variables have equal weights for risk prediction. As a potential solution to compensate the weakness of this model, the weighting of the cut-off values of a variable might be defined as assigning their individual HR. Interestingly, despite the inclusion of many variables of the REVEAL model with their original cut-off limits into this algorithm, utility of overall REVEAL risk model seemed to be ignored in the ESC/ERS PH Guidelines. Finally, as another critically important limitation, this recommendation oversimplificating the complexity of the natural course of PAH has been supported by the level C evidence based on consensus of expert opinion rather than any statistical modelling of validated parameters. 35
Three recently published PAH registries including over 3000 incident PAH patients from eight European countries have utilized some simplified modifications of the risk stratification and reduction strategy recommended in the ESC/ERS PH Guidelines.36–38 In the Swedish PAH registry (SPAHR), FC, 6MWD, NT-proBNP, right atrial (RA) area, mRAP, pericardial effusion (PE), CI, and SvO2 have been used, and each was graded from 1 to 3 according to the severity of risk. 36 A patient’s mean grade was obtained by dividing the sum of all grades by the number of available variables, and the “low risk” at baseline and at one-year follow-up were found to predict a better survival. 36 In the treatment-naive and incident PAH population of the COMPERA registry, a similar set of variables (except PE) and a similar grading method have been utilized, and mortality rates one year after diagnosis were 2.8%, 9.9%, and 21.2% in the low-risk, intermediate-risk, and high- risk cohorts, respectively. 37 In the French registry including the incident patients with idiopathic, heritable, or drug-induced PAH, the low-risk criteria derived from four variables (FC I or II, 6MWD > 440 m, mRAP < 8 mmHg, and CI ≥ 2.5 L/min/m2) were assessed at diagnosis and at first re-evaluation within one year of follow-up; the number of low-risk criteria at diagnosis and at first re-evaluation were found to predict the risk of death or lung transplantation. 38 Moreover, a subgroup analysis including three non-invasive criteria (FC, 6MWD, and BNP or NT-proBNP) revealed that a number of these variables at low-risk at first re-evaluation discriminated prognostic groups, significantly. 38
Although these three registries have seemed to highlight the potential prognostic advantage of achieving low-risk status as a treatment goal in “real world” practice, these consistent results can not be considered to be sufficient for validation of current ESC/ERS risk reduction tables suffering from aforementioned limitations.20,36–40 However, the results of these registries seem to confirm the utility of the ESC/ERS PH risk table in daily practice. As the common shortcomings, the study populations did not cover all the spectra of PAH subgroups, all ages, and prevalent cohorts, and non-modifiable risk factors were not considered in the analyses.20,36–38 A recent report from the authors of the SPAHR group also highlighted the additional impacts of age and specific co-morbidities as prognostic markers of outcome in patients with incident PAH. 39 A significant number of patients have been reported to improve in the two youngest age groups (18–45 years, P < 0.001 and 46–64 years, P = 0.034), but not in the older patients. Five-year survival was highest in the youngest patients (88%), while the survival rates were 63%, 56%, and 36% for patients in the age groups 46–64, 65–74 and ≥75 years, respectively (P < 0.001). 39 Moreover, ischemic heart disease and kidney dysfunction were found to be independent predictors of survival. 39 The results of the SPAHR and French registry have been based on the analyses of retrospective cohorts.36,38 Moreover, low-risk status was achieved in only a minority of patients in each cohort at follow-up which may be due to unexpectedly low utilization rates of dual or triple combinations of TTs (especially in COMPERA and SPAHR).36–38 These failure rates suggest a kind of “Cassandra desperation” for patients persistently remaining at intermediate or high risk in the absence of the maximal combination TTs including drugs having evidence for mortality or combined mortality/morbidity benefits. An important loss rate of patients at follow-up was another limitation of these three cohorts.36–38 Moreover, these measures seemed to discriminate high risk from low risk whereas the lack of separation for those “in between” has remained an unresolved issue.36–38 Furthermore, the possibility of survival benefits from upfront dual or triple combinations of TTs versus goal-oriented sequential combinations guided by any serial risk stratification model in patients with PAH has not been tested in a registry or randomized controlled trial. The utilization of the “Rubik’s cube” approach integrating the multiple risk measures as proposed by some authors may result in approximately 729 combinations of various risk factors and can not serve as a practical risk reduction tool for guidance to PAH management.20,40
Moreover, recently published analyses yielded the importance of reassessing the dynamic changes in various measures for risk stratification along the course of PAH.42–46 A study from the REVEAL registry showed that a simple biomarker, declining renal function as defined by the presence of a ≥10% decrease in estimated glomerular filtration rate (eGFR) from baseline over ≥1 year, significantly increased the risk of death and the composite of all-cause hospitalization and death, independently of changes in 6MWD and FC. 42 However, a ≥10% increase in eGFR was not associated with either end-point. 42 An updated REVEAL score with the addition of eGFR (<60) and hospitalization within the last year to the classical model showed that both the updated score at 24 months and change in this score at 12–24 months predicted survival from this time point. 44 Among the components of the overall model, change in hospitalization and change in systolic blood pressure were found to be most influential risk factors for survival. 44 C-index for updated score indicated slightly better discrimination (0.762) than the original model (0.741) for three-year survival from one year post enrollment. 44 In another analysis from the REVEAL cohort, low (≤340 pg/mL) versus high (>340 pg/mL) BNP levels have been defined and assessed at baseline and last follow-up evaluation. 45 Baseline high versus low BNP predicted a significantly higher mortality (HR = 3.6; 95% CI = 3.0–4.2) up to the five-year period. Moreover, according to BNP change at ≤1 year post-enrollment control, the low-low BNP group had the lowest and the high-high BNP group had the highest five-year mortality risk. Changes in BNP score also correlated with change of risk of death. 45 Another recently published study showed that none of the baseline HD variables, but FC, 6MWD, stroke volume index (SVI), and RAP at first follow-up, and right heart catheterization were independently associated with death or lung transplantation, adjusted for age, gender, and etiology of PAH. 46 Even in the presence of two or three low-risk criteria at follow-up, including a CI ≥ 2.5 L/min/m2, 6MWD > 440 m, and either FC I or II, a lower SVI still predicted higher risk for adverse outcome (P < 0.01). 46 These results highlighted the potential importance of SVI in the management of PAH.
Despite the several aforementioned limitations of the currently available scheme of ESC/ERS risk-based treatment goals, the unpublished Task Force Report for Risk Stratification and Medical Therapy of Pulmonary Arterial Hypertension presented in 6th World Symposium on Pulmonary Hypertension (WSPH) has highlighted simplified prognostic criteria as the components of a road-map derived from this algorithm. These four prognosticators inspired from ESC/ERS 2015 PH Guidelines and utilized in the SPAHR, COMPERA, and French registries are WHO FC, 6MWD, NT-proBNP/BNP or RAP, and CI or SvO2, and original cut-off values for measures of three risk status remain unchanged.35–38 However, there is no convincing evidence for deleting the PE from the original model and the position of the RAP separated from two other invasive HD parameters of category D and proposed as an alternative for NT-proBNP/BNP in measures of the category C. Low-risk status has been arbitrarily defined as at least three low-risk criteria and no high-risk criteria while high-risk status has been defined as at least two high-risk criteria including deteriorated CI or SvO2. Intermediate risk has been defined as the conditions not fulfilling the low- or high-risk criteria. However, critical weakness of the ESC/ERS risk prediction table due to the lack of validation seems to persist even after this update. Moreover, arbitrary definitions of three risk status have not been based on any symmetry for ranges of measures included.
Despite these drawbacks of the currently available ESC/ERS risk management table, the potential for the generalizability of the simplified version of this goal-oriented risk reduction strategy in daily PAH practice should be taken into account. Accordingly, we propose an alternative parametric display for the original ESC/ERS 2015 PH Guidelines risk reduction table and its simplified version by using three concentrically layered circles from high-risk at the periphery to low-risk at the centre as a dart table order instead of columns of risk cohorts (Fig. 2). The simplicity of this bull’s eye display seems to demonstrate the concept of goal-oriented risk reduction strategy better than shifting among the colums. Therefore, this easy-to-use demonstration of the management model should aim to hit the bull’s eye, the lowest risk status as highlighted in the current PH management algorithms. However, even this scheme remains a parametric display of an unvalidated but widely used risk stratification approach. This 360° pictorial display can serve as a practical tool either for the average score method of the SPAHR and COMPERA registries or method of achieving the low-risk status used in the French registry. Ideally, relative contribution of sectors in the overall area of circle can demonstrate the weight of each risk factor validated as independent variable for clinical outcome, and the distance from the green centre can indicate the achieved level of satisfaction in risk reduction according to the ranges of precisely defined HR values of each measure. Moreover, potential developments in risk parameters and their cut-off values may enrich the utility and reliability of this approach and dart table simplification may evolve to more comprehensive and dynamic radar graphical displays in the near future.
(a, b) Bull’s eye parametric display of currently available ESC/ERS 2015 Pulmonary Hypertension Guidelines risk stratification table (a) and its simplified version (b). The red, yellow, and green circular zones indicate high-risk, intermediate-risk, and low-risk status, respectively. (b) Measures of pericardial effusion and RA area are deleted fron original model. CI, cardiac index; RAP, right atrial pressure; FC, functional class; 6MWD, 6-min walking distance; NT-pro BNP and BNP, N-terminal pro brain natriuretic peptide and brain natriuretic peptide, respectively; RA, right atrium; SVO2, mixed venous oxygene saturation %.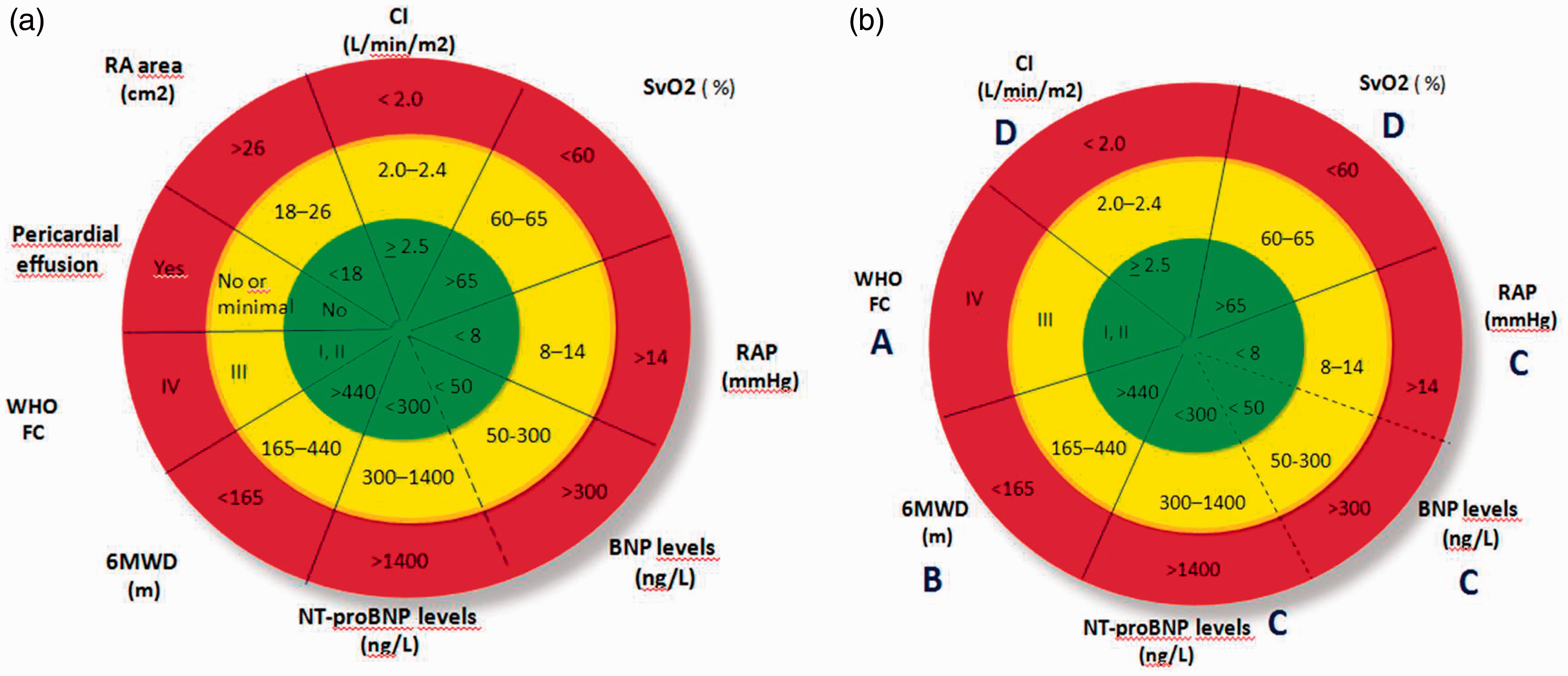
Another emerging and revolutionary approach, the “Redefining Pulmonary Hypertension through Pulmonary Vascular Disease Phenomics” (PVDOMICS) program, has been designed as a collaborative, protocol-driven network to develop new strategies and master clinical trials protocols based on precision medicine principles and applicable for future clinical trials and all phenotypes of pulmonary vascular diseases (PVD). 47 The adoption of smaller clinical trials using adaptive and innovative statistical models, the development of novel or updated variables in imaging, HD, cellular, genomic, proteomic, and metabolomic assessments to identify differentiating and common features of PVD as the standpoints for novel management strategies seem to imply new frontiers in the twilight airglove. 47
Footnotes
Conflict of interest
The author(s) declare that there is no conflict of interest.
Funding
Article processing procedure is financially supported by Actelion Pharmaceuticals – Turkey as an unrestricted scientific grant.
