Abstract
Right ventricular (RV) function is an important determinant of the prognosis in patients with pulmonary arterial hypertension (PAH). In the context of recent therapeutic progress, there is an increasing need for better monitoring of RV function for management of PAH. We present the case of a 42-year-old woman with idiopathic PAH who was treated with three oral pulmonary vasodilators, i.e. tadalafil, ambrisentan, and beraprost. At the baseline assessment, the mean pulmonary arterial pressure (mPAP) was 45 mmHg, cardiac index (CI) was 1.36 L/min/m2, and pulmonary vascular resistance (PVR) was elevated to 21.3 Wood units (WU). However, three months after the start of combination treatment, mPAP and PVR decreased to 42 mmHg and 7.5 WU, respectively, and conventional indices of RV function, such as CI, right atrial area, and right atrial pressure also improved. Beyond three months, however, there were no further improvements in mPAP, PVR, or indices of RV function. In addition, we calculated three recently introduced indices of intrinsic RV function: end-systolic elastance (Ees; an index of RV contractility), Ees/arterial elastance ratio (Ees/Ea; an index of RV/pulmonary arterial coupling), and β (an index of RV stiffness) using cardiac magnetic resonance imaging and Swan-Ganz catheterization measurements. Notably, in contrast to conventional parameters, Ees, Ees/Ea, and β showed persistent improvement during the entire two-year follow-up. The application of Ees, Ees/Ea, and β may play an additional role in a comprehensive assessment of RV function in PAH.
Keywords
Assessment of right ventricular (RV) function has become an important element in the diagnosis and management of pulmonary arterial hypertension (PAH).1–3 Cardiac pressure–volume loop analysis is required for the evaluation of load-independent RV function; however, the application of this analysis is limited because it requires an invasive procedure with dedicated catheters.1,4,5 Recently, cardiac magnetic resonance imaging (CMRI)-derived metrics have been introduced for calculating load-independent indices of the RV systolic function, such as RV end-systolic elastance (Ees), 6 stiffness constant β, 7 and the Ees/arterial elastance (Ea) ratio, a measure of RV/pulmonary artery (PA) coupling. 6 The clinical relevance of these parameters is promising; however, no prior reports have demonstrated how the parameters change in PAH patients treated with multi-drug regimens. In the present case report, we document the remarkable time course of changes in the conventional and novel indices of RV morphology and function in a patient with idiopathic PAH who was treated with three classes of pulmonary vasodilating agents.
Case description
A 42-year-old woman was referred to Hokkaido University Hospital, Sapporo, Japan, for evaluation of presyncope and progressive exertional dyspnea (World Health Organization [WHO] functional class III). She had no family and life medical history associated with pulmonary hypertension (PH). Auscultation of the heart revealed a holosystolic murmur at the left third intercostal space and an accentuated pulmonary component of the second heart sound. Comprehensive blood test results did not indicate any risk factor for PH including autoimmune disorders. Electrocardiography showed right axis deviation and RV hypertrophy. Chest radiography indicated enlargement of the right atrium and ventricle. A ventilation/perfusion scan showed no mismatched perfusion defects. Echocardiography revealed right atrial and RV dilatation, severe tricuspid regurgitation, pericardial effusion, and dilatation of the inferior vena cava. The tricuspid annular plane systolic excursion (TAPSE) was decreased to 9.7 mm. Right heart catheterization (RHC) exhibited elevated mean PA pressure (mPAP) and pulmonary vascular resistance (PVR) values of 45 mmHg and 21.3 Wood units (WU), respectively, and a reduced cardiac index (CI) of 1.36 L/min/m2. Pulmonary arterial wedge pressure (PAWP) was 5 mmHg. These diagnostic workups indicated no underlying cause of PAH, and a diagnosis of idiopathic PAH was made.
This case report was approved by the ethical committee of Hokkaido University Hospital (014-0388) and the patient provided written informed consent.
Assessment of the RV function using CMRI and calculations of Ees, Ees/Ea, and β
CMRI was performed using a 1.5-T Philips Achieva magnetic resonance imaging system (Philips Medical Systems, Best, The Netherlands) with a five-channel coil, equipped with Master gradients (maximum gradient amplitude, 33 mT/m; maximum slew rate, 100 mT/m/ms). We used a protocol reported in a previous study. 8 In brief, a total of 12 axial slices were acquired using a steady-state free precession pulse sequence (TR = 2.8 ms; TE = 1.4 ms; flip angle = 60; acquisition matrix = 192 × 256; field of view = 380 ms; slice thickness = 10 mm; 0 mm inter-slice gap; and 20 phases/cardiac cycle), which were analyzed using a dedicated software (Extended MR Work Space ver. 2.6.3; Philips Medical Systems, Amsterdam, The Netherlands). In axial datasets, the endocardial contours of the right ventricle were manually traced, and RV and left ventricular (LV) end-diastolic volume (EDV) and end-systolic volume (ESV) were computed. RV and LV stroke volume (SV) and ejection fraction (EF) were calculated using SV = EDV − ESV and EF = SV/EDV × 100%, respectively.
Ees and Ea were approximated with the following formulas based on a method reported by Sanz et al.
6
Ees/Ea is the ratio of Ees to Ea.



To solve Eq. 3, the following three datasets of P and V were used: (P, V) = (0, 0), (minimal RV diastolic pressure, end-systolic RV volume), and (RV end-diastolic pressure, end-diastolic RV volume). Here, as reported by Rain et al., minimal RV pressure was normalized at 1 mmHg to avoid measurement errors caused by the positioning of RV catheter and to construct pressure–volume curve and calculate α and β. For similar reasons, RVEDP was calculated using the following formula: 1 + (RVEDP – minimal RV diastolic pressure). 7
Clinical course
After diagnosis, administration of ambrisentan (10 mg/day) was commenced, followed by an addition of tadalafil (40 mg/day) and then of beraprost (120 µg/day) within three weeks. During this treatment intensification, the patient reported mild headache and facial flushing but otherwise tolerated the medication well. Subsequently, the dose of beraprost was increased up to 360 µg/day. However, the patient reported a slight worsening of dyspnea on exertion and her mPAP and PVR increased at the 1.5-year follow-up. Thus, the treatment was intensified by adding inhaled iloprost (incremental increase up to 30 µg/day).
Clinical data before and after the start of oral combination treatment.
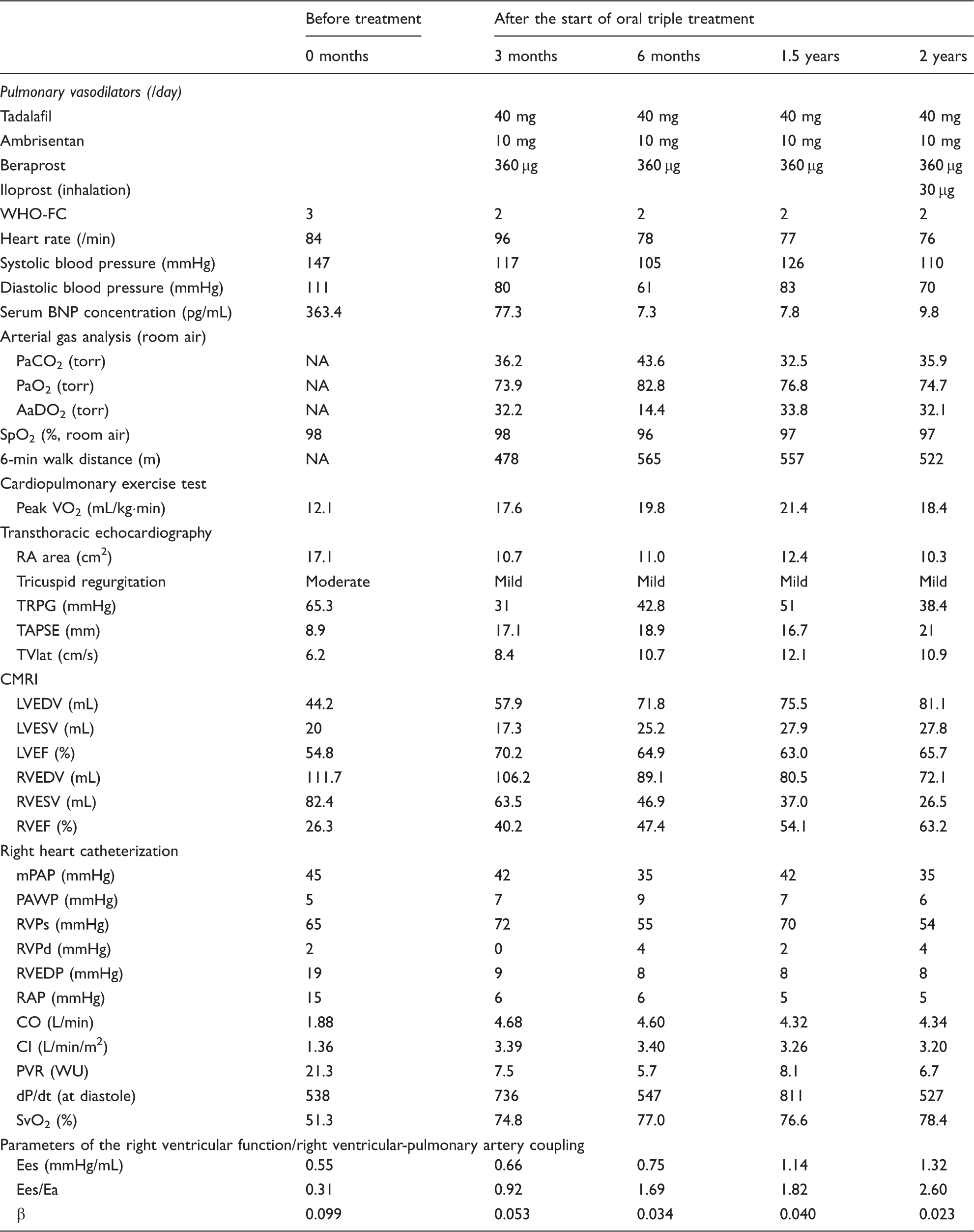
BNP, brain natriuretic hormone; CI, cardiac index; CMRI, cardiac magnetic resonance imaging; CO, cardiac output; LVEDV, left ventricular end-diastolic volume; LVEF, left ventricular ejection fraction; LVESV, left ventricular end-systolic volume; MPAP, mean pulmonary arterial pressure; PAWP, pulmonary arterial wedge pressure; PVR, pulmonary vascular resistance; RA, right atrial; RAP, right atrial pressure; RVEDP, right ventricular end-diastolic pressure; RVEDV, right ventricular end-diastolic volume; RVEF, right ventricular ejection fraction; RVESV, right ventricular end-systolic volume; RVPd, diastolic right ventricular pressure; RVPs, systolic right ventricular pressure; TAPSE, tricuspid annular plane systolic excursion; TRPG, maximum tricuspid regurgitation pressure gradient; TVlat, lateral tricuspid valve annular motion velocities in systole.
Figure 1 shows the change in PVR and conventional indices of the RV function over time. As illustrated in Fig. 1a, CI, TAPSE, and RA pressure significantly improved as PVR decreased during the three months after the start of combination treatment, and this improvement was maintained throughout the two years of follow-up. In contrast, as shown in Fig. 1b, the three indices of intrinsic RV function, i.e. Ees, Ees/Ea, and β, showed improvement at three months and, in contrast to the indices shown in Fig. 1a, they continued to improve during the entire follow-up.
Time course of changes in pulmonary vascular resistance (PVR) and indices of right ventricular (RV) function. (a) PVR and conventional indices of RV function improved three months (M) after the start of combination treatment with three pulmonary vasodilators. After three months of follow-up, no further changes in these indices were observed up to two years of follow-up. (b) The three indices of intrinsic RV function continued to improve throughout the two-year follow-up.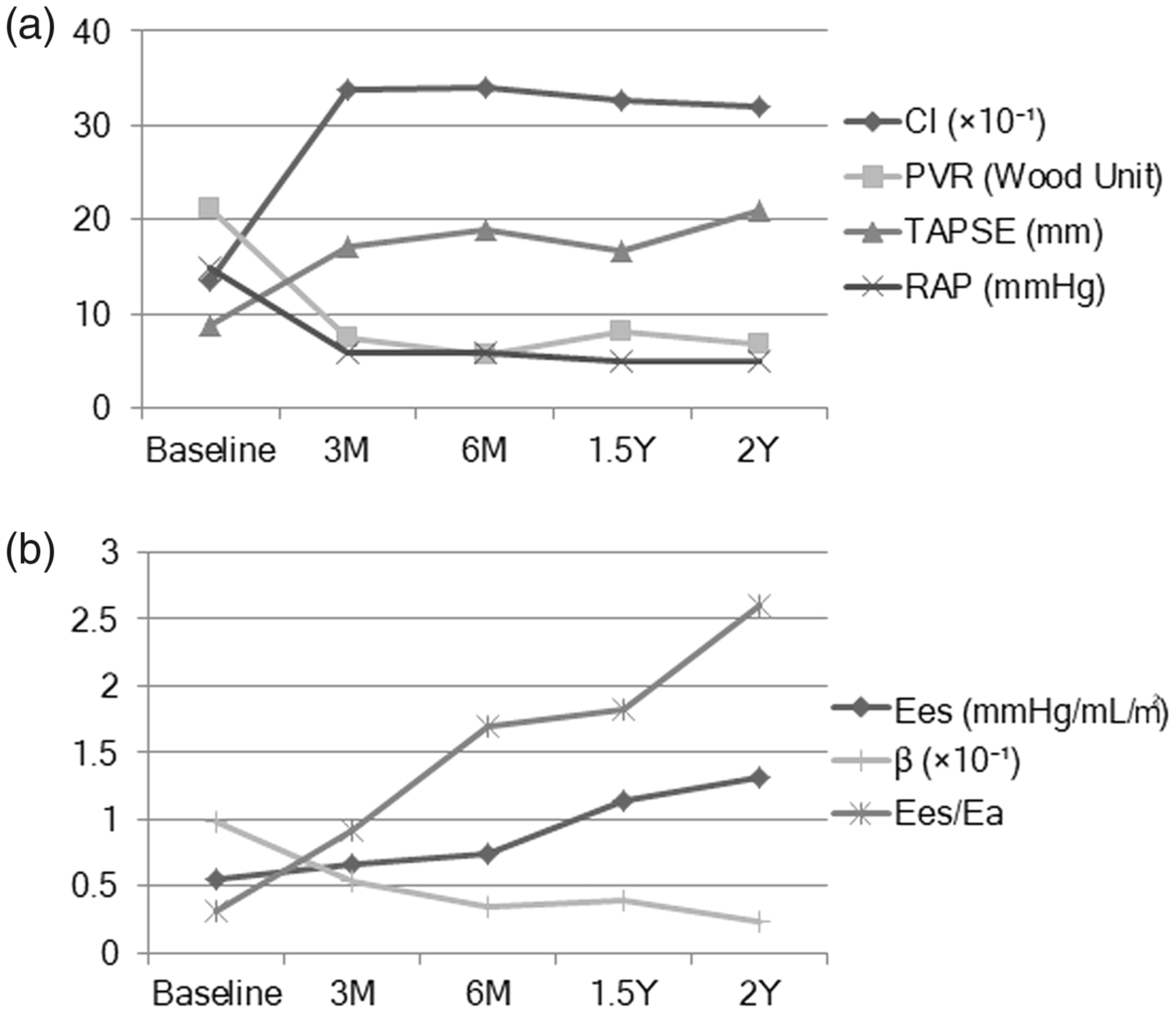
Discussion
Our patient was a 42-year-old woman with idiopathic PAH who showed significant improvements in functional class, exercise capacity, and conventional RV parameters after the start of combined therapy with a total of four oral pulmonary vasodilators. Notably, after these indices improved and became stable, three novel RV indices, i.e. Ees, Ees/Ea, and β, continued to improve, which suggested further amelioration in the RV function in response to the early and combined use of pulmonary vasodilators.
RV systolic function
RV contractility refers to the load-independent contractility of the right ventricle, and the gold standard index for this function is maximum elastance (Emax) or Ees.1,9 Ees can be measured using a pressure–volume relation loop recorded with a dedicated catheter and system.10,11 Recently, non-invasive parameters of the RV systolic function, such as TAPSE and CMRI-derived RV EF, have been introduced;12,13 however, these indices are pre- and afterload-dependent. Regarding load-independent indices of the RV systolic function, MPAP/RVESV has been proposed. In a pivotal report published in 2012, Sanz et al. measured Ees (MPAP/RVESV) in 124 patients with PH and showed that, compared with 27 individuals without PH, patients with PH had higher Ees (0.61 in PH versus 0.47 in control,
In our patient, we monitored changes in load-dependent and load-independent indices of the RV systolic function and observed continuous improvement exclusively in Ees after the administration of oral PAH drugs. Currently, Ees is not a widely used parameter in the management of PAH, whereas data in our case suggest that Ees, calculated as MPAP/RVESV, is an index that assesses RV contractility with sensitivity superior to that of currently used parameters.
RV/PA coupling
The inter-relationship between RV contractility and afterload is called RV/PA coupling. In a setting of preserved RV/PA coupling, RV contractility increases to the level at which right heart function is maintained. However, when RV contractility cannot rise to match the elevated RV afterload, RV/PA uncoupling occurs and leads to RV dysfunction and right heart failure. Previous studies have reported that RV/PA coupling can be expressed as Emax/Ea, in which Ea is effective arterial elastance. 6 Optimal coupling of the right ventricle and pulmonary circulation occurs at an Emax/Ea of 1.5–2.0.1,9,14 In our case, Emax/Ea at diagnosis was 0.31. After the start of the combination treatment, however, Emax/Ea continuously increased to 2.6 during the two-year follow-up. Similar to Ees, Emax/Ea may have been an indicator of improved RV systolic function in our patient.
RV diastolic function
RV diastolic function can be divided into two phases, active and passive. The active phase describes relaxation of the myofibers that consume ATP and is assessed with tau(τ) or dP/dt.15,16 The passive phase describes the compliance of the RV walls, which reflects the capacity of the walls to expand when RV is fully dilated. Stiffness is an alternative concept that reflects passive components of RV diastolic function. The gold standard parameter representing compliance/stiffness of the RV walls is the EDP–volume relationship (EDPVR), 17 and an invasive procedure is required for its calculation.
In our case, we calculated β based on the method reported by Rain et al. 7 and found a linear improvement from 0.099 to 0.023 during two years of treatment with PAH drugs. Right atrial area and atrial area pressure also reflect RV compliance/stiffness, but unlike β, they did not change after the three-month follow-up. This outcome suggests that β has promising sensitivity in monitoring RV compliance/stiffness in patients with PAH treated with pulmonary vasodilating agents.
Limitations of this study include the substantial assumptions required for the calculation of Ees, Ees/Ea, and β. First, the gold standard indices of RV function are derived from multiple-beat pressure–volume curves, whereas, in the present study, we applied simplified single-beat methods for calculating Ees, Ees/Ea, and β. In addition, the normalization of RV diastolic pressure (minimal RV diastolic pressure and RVEDP) was employed for the calculation of β, which may have hampered its accuracy in assessing RV stiffness. Second, a reversibility test was not performed in this study. Thus, on the basis of the current guidelines for PH, the standard treatment for this case could have been high-dose calcium channel blockers rather than PAH-specific agents. Third, the regimens applied to this case were not prevalently used. For example, we introduced three pulmonary vasodilators within three weeks and also added iloprost along with beraprost. We followed this treatment regimen based on the severity of the disease and the drug availability in Japan; however, the unusual use of the vasodilators made application/interpretation of the presented data difficult. Fourth, the patient did not have the 6-min walk distance test before treatment, which precluded the comparison of the data before and after the multiple drug therapy. Lastly, the improvement of Ees, Ees/Ea, and β after three months of follow-up was not accompanied by ameliorations of patient’s symptoms/signs, functional capacity, and/or indices of cardiopulmonary exercise test as shown in Table 1. Therefore, it is still unknown whether the improvement of Ees, Ees/Ea, and β surely reflects an amelioration of RV function and is meaningful in the clinical practice.
Conclusions
In this case report, we document the time course of changes in promising indices of RV function, i.e. Ees, Ees/Ea, and β, in a 42-year-old woman with idiopathic PAH. The results suggested the promising potential of these indices as sensitive markers of the change in RV function in PAH. Further evaluation in prospective well-powered clinical studies is needed to verify the clinical relevance of these indices.
Footnotes
Acknowledgments
The authors thank Crimson Interactive Pvt. Ltd. (Tokyo, Japan) for the scientific English editing.
Conflict of interest
All diagnostic workups, treatments, and follow-ups were performed, and all authors were employed, at Hokkaido University Hospital.
Funding
All medical expenses were covered by the national insurance system of the Japanese government.
