Abstract
While pulmonary hypertension (PH) has traditionally not been considered as a disease that is directly linked to or, potentially, even caused by inflammation, a rapidly growing body of evidence has demonstrated the accumulation of a variety of inflammatory and immune cells in PH lungs, in and around the wall of remodeled pulmonary resistance vessels and in the vicinity of plexiform lesions, respectively. Concomitantly, abundant production and release of various inflammatory mediators has been documented in both PH patients and experimental models of PH. While these findings unequivocally demonstrate an inflammatory component in PH, they have fueled an intense and presently ongoing debate as to the nature of this inflammatory aspect: is it a mere bystander of or response to the actual disease process, or is it a pathomechanistic contributor or potentially even a trigger of endothelial injury, smooth muscle hypertrophy and hyperplasia, and the resulting lung vascular remodeling? In this review, we will discuss the present evidence for an inflammatory component in PH disease with a specific focus on the potential role of the endothelium in this scenario and highlight future avenues of experimental investigation which may lead to novel therapeutic interventions.
Inflammatory cells and mediators in pulmonary hypertension
Specific subclasses of pulmonary arterial hypertension (PAH) have traditionally been linked to inflammation and immunity due to the inflammatory or infectious nature of their underlying or associated disease. Prototypic examples are PAH forms related to connective tissue diseases such as systemic sclerosis or lupus erythematosus, 1 but also PAH as a consequence of HIV infection or related to other viral etiologies. 2 The implication of inflammation and immunity in pulmonary hypertension (PH), however, is much older, and seems to reach far beyond these most striking associations.
Already in 1878, when Paul Ehrlich identified the mast cell, he reported that these cells were most abundant in “brown induration of the lung,” i.e. in hemosiderosis, which we nowadays would classify as type II PH, i.e. PH following left heart disease. 3 Subsequent clinical studies confirmed the accumulation of mast cells in lungs of patients with idiopathic PAH (iPAH)4–7 or “secondary” PAH (which nowadays would be considered associated PAH) 6 or in patients with PH owing to mitral stenosis and left heart disease. 8 Measurements of mast cell densities in lungs of native highlanders revealed that mast cell numbers were only increased in subjects with considerable muscularization of their pulmonary circulation, indicating a functional role for mast cells in lung vascular remodeling. 9 These clinical findings were paralleled by reports of similar mast cell accumulations in experimental models of PH, notably in chronic hypoxic rats10,11 as well as calves, pigs, and sheep, 12 in the rat monocrotaline model of PH,4,13,14 in rat models of left heart disease, 13 or in a combined model of monocrotaline and left-to-right shunt. 15
More recently, the recognition of immune cell abundance and infiltration in lung vascular lesions and remodeled vessels has expanded profusely (Fig. 1): innate immune cells such as macrophages and monocytes are characteristically detected in patients with iPAH,7,16 in PH secondary to congenital cardiac shunts
17
and in murine and rat lungs in response to chronic hypoxia or monocrotaline.18,19 Vascular lesions and the adventitial space of remodeled blood vessels in iPAH patients and monocrotaline-induced experimental PH are also infiltrated by immature dendritic cells.7,20 In addition to infiltrating innate immune cells, the adaptive immune response has recently become implicated in PH based on the fact that perivascular accumulations of B cells have not only been documented in PAH associated with connective tissue disorders or HIV infection,21,22 but also in plexiform lesions of patients with iPAH,
16
as well as in experimental PH.
23
Work by the groups of Perros et al.
24
and Colvin et al.
25
as well as from our own laboratory
26
has identified the formation of characteristic tertiary lymphoid tissue comprising B- and T-cell areas with high endothelial venules and dendritic cells in the vicinity of remodeled pulmonary arteri(ol)es and bronchi(oles) in iPAH patients as well as animal models of PH.
Infiltration of inflammatory and immune cells into the wall and perivascular space of pulmonary arteries in PH. A schematic cross-section shows a pulmonary artery with its different layers (intima, media, and adventitia) and the characteristic accumulation of inflammatory and immune cells, namely macrophages, dendritic cells, T cells, B cells, mast cells, and plasma cells, as well as the infiltration of fibroblasts and myofibroblasts and the production of (auto-)antibodies in PH disease.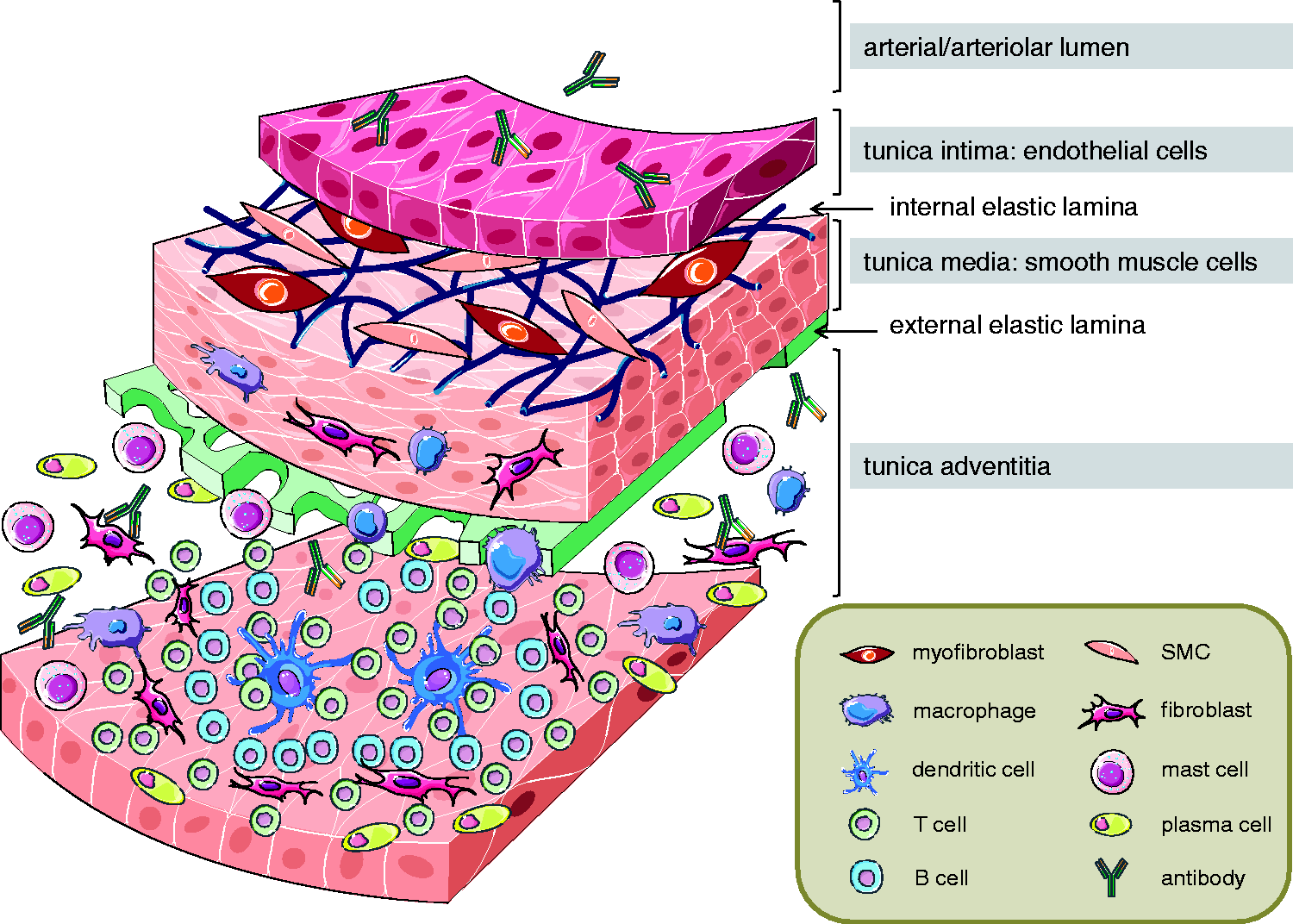
This infiltration of innate and adaptive immune cells is associated with—and likely orchestrated by—the activation of several key transcription factors such as the nuclear factor of activated T cells (NFAT) 27 and STAT328 contributing to the release of numerous cytokines. Patients with iPAH or associated PAH exhibit higher circulating levels and/or pulmonary expression of tumor necrosis factor (TNF),29,30 interleukins (IL) including IL-1β,31,32 IL-4,32,33 IL-6,31,32 IL-8, 32 IL-10, 32 IL-12p70, 32 and IL-13,33,34 and a series of chemokines including fractalkine (CX3CL1), 35 RANTES (CCL5), 36 monocyte chemotactic protein-1 (MCP-1; CCL2),37,38 and interferon γ-induced protein 10 (IP-10; CXCL10). 39 Of the characteristic cytokines, IL-6 seems of particular relevance in the context of PH as suggested by experimental studies and biomarker screenings: in PAH patients, plasma IL-6 levels predict five-year survival with a higher prognostic accuracy as functional or hemodynamic parameters. 32 Similarly, circulating IL-6 in PAH patients contribute to the development of co-morbidities in PAH such as coronary artery diseases through the activation of the Bromodomain-containing protein 4 (BRD4),40,41 while increased TNF contributes to right ventricular failure through a miR-208/myocyte enhancer factor 2 (MEF2)-dependent mechanism. 42 The importance of circulating cytokines especially IL-6 is reinforced by the fact that lung-specific overexpression of IL-6 in mice suffices to cause elevated right ventricular systolic pressures and right ventricular hypertrophy with corresponding pulmonary vascular changes. 43 Conversely, IL-6-deficient mice develop less PH, right ventricular hypertrophy, and lung vascular remodeling in chronic hypoxia compared to their corresponding IL-6+/+ wild type (WT). 44
In addition to classic inflammatory cytokines, immune responses in PH may also be triggered or aggravated by other pro-inflammatory mediators such as leukotrienes (LTs) or complement factors. Recent studies suggest an important role for LTB4 in the context of immune dysregulation in PAH. 45 LTs are lipid mediators derived from arachidonic acid. Following activation of 5-lipoxygenase (5-LO) by 5-LO-activating protein (FLAP), arachidonic acid is converted to LTA4, an unstable epoxide which is subsequently further metabolized by either LTA4 hydrolase or LTC4 synthase to LTB4 or LTC4, respectively. In rats exposed to chronic hypoxia, expression levels of 5-LO and FLAP are increased in alveolar macrophages and endothelial cells, 46 and in athymic rats treated with the VEGF receptor antagonist SU5416, which develop lethal PH even under normoxic conditions, LTB4 levels were found to be elevated in bronchoalveolar lavage fluid and serum. 47 Analogously in PAH patients, alveolar macrophages expressing 5-LO and FLAP are more frequently clustered in the vicinity of remodeled blood vessels, while endothelial cells in plexiform and concentric lesion similarly express both enzymes. 48 Pharmacological antagonization of 5-LO and FLAP by MK-866 was shown to prevent hypoxic pulmonary vasoconstriction and development of chronic hypoxia-induced PH, thus establishing a functional role of LTs in PH. 46
LTB4 exerts its chemoattractant and pro-inflammatory effects predominantly via its high affinity receptor BLT1 which is widely expressed on immune cells including granulocytes, T cells, and dendritic cells. 49 In vitro, LTB4 induces apoptosis of pulmonary artery endothelial cells via a signaling pathway that involves spingosine kinase 1 and endothelial nitric oxide synthase, and stimulates proliferation of human pulmonary artery smooth muscle cells, which is effectively blocked by the BLT-1 inhibitor U75302. 47 In addition, LTB4 may further promote PH by stimulating proliferation, migration, and differentiation of pulmonary arterial adventitial fibroblasts. 50 In vivo, inhibition of LTB4 formation by the LTA4 hydrolase inhibitor Ubenimex rescued PH rats from death. In PAH patients, LTA4 hydrolase expression was shown to be increased in CD68+ macrophages clustered around occluded vascular lumens of plexiform lesions, and circulating levels of LTB4 were found to be elevated in PAH patients with connective tissue disease though not in iPAH. 47 From these studies, LTB4 has emerged as an important inflammatory signal and, hence, also potential drug target in PH. In respect to the latter, the recent completion of the LIBERTY trial, a phase 2 study on the effectiveness of the LTA4 hydrolase inhibitor Ubenimex in patients with PAH (LIBERTY:NCT02664558), is expected to provide key insight into the therapeutic potential of this pathway.
Considering that complement factors C3 and C4a have been identified as biomarkers of iPAH,51,52 it is surprising that the functional role of the complement system as a critical regulator of innate and adaptive immune responses in PH has thus far scarcely been addressed. In what is to our knowledge the only mechanistic study so far, Bauer et al. were able to demonstrate increased deposition of the C3 degradation product C3d in the pulmonary vessel wall in a murine PH model of chronic hypoxia and in human iPAH patients. 53 More importantly, C3-deficient mice developed less PH with no increase in pulmonary IL-6 or tissue factor, less P-selectin on platelets, and less pulmonary intercellular adhesion molecule 1 (ICAM-1) expression during chronic hypoxia compared to WT mice, suggesting that C3 plays an important role in the pathophysiology of PH, potentially by promoting inflammatory cell interaction and recruitment via adhesion molecules such as P-selectin and ICAM-1. Since various novel therapies targeting the complement system are presently tested in clinical trials,54,55 the functional role of the complement system in PH and its therapeutic exploitation pose intriguing topics for future research.
The functional relevance of immune responses in the initiation and/or progression of PH has recently become evident, in that pharmacological inhibition, depletion, or genetic deficiency in specific cell subsets such as mast cells4,13,15 or B cells26,56 has been shown to confer protection from the development of PH in a variety of animal models. Furthermore, IL-6 has been identified as a critical link between mast cells and B cells and, hence, between the innate and adaptive immune system in that mast cell-derived IL-6 promotes the formation of tertiary lymphoid tissue in PH lungs 26 in line with previous data demonstrating that mast cells synthesize and release IL-6.57,58 Originally identified as a B cell stimulatory factor that induces differentiation into antibody-producing plasma cells, 59 IL-6 production has also been linked to increased Ig secretion and production of autoantibodies. 60 A similar and potentially parallel pathway linking mast cells to B cells may act via another member of the IL-6 family, the pleiotropic cytokine oncostatin M. 61 Like IL-6, OSM is also secreted by mast cells 62 and upregulated in the bronchoalveolar lavage fluid of patients with idiopathic pulmonary fibrosis and scleroderma or in plasma of PAH patients.63,64 Endotracheal administration of an adenoviral vector expressing mouse oncostatin M promotes B cell activation and formation of tertiary lymphoid tissue independent of IL-6, 65 suggesting that mast cells may regulate adaptive (auto-)immunity and formation of tertiary lymphoid tissue via different pathways in PH.
Importantly, the emerging role of mast cells, B cells, and other inflammatory cells in PH is not a purely theoretical concept but of tremendous translational potential and, as such, has already reached the clinical setting. 66 Mast cell stabilizers have been shown to reduce inflammation and increase exhaled NO in PAH patients in a small pilot study, 67 while a clinical phase II trial on the effect of the B cell depleting anti-CD20 antibody rituximab for the treatment of systemic sclerosis-associated PAH is currently underway (NCT01086540). Care should, however, be taken with respect to existing immunosuppressive drugs, as poor safety profiles and potentials for drug–drug interactions with current PH therapies may present dangerous pitfalls for their implementations in clinics. 68
While mast cells and B cells promote the development of PH, CD4+CD25+FoxP3+ regulatory T cells (T regs), a subpopulation of T cells which maintains tolerance to self-antigens and downregulates autoimmune disease, seem to attenuate experimental PH. Athymic mice or rats lacking T cells characteristically develop more severe PH in response to monocrotaline or SU5416 compared to euthymic rodents.69,70 The beneficial effect of T regs in PH was particularly evident in a study in athymic rats in that the development of lung vascular remodeling and PH in response to SU5416 was attenuated in animals that had been reconstituted with CD4+CD25+ T regs. 71 This may at first seem contradictory, as B cells are considered to maintain 72 and expand73–76 T regs. Conversely however, a series of animal studies on autoimmune diseases show that depletion of B cells causes activation and proliferation of T regs which are associated with marked improvement of histological or functional parameters of disease severity.77–79 The clinical relevance of this scenario is highlighted by the fact that B cell depletion with rituximab restores T reg numbers in peripheral blood of patients with immune thrombocytopenia (ITP), an effect that is particularly evident in therapy responders. 80 Conversely, B cells may thus potentially promote inflammatory (auto-)immune responses by inhibiting T regs.
The differential involvement of innate and adaptive immune cells, the temporal sequence of their infiltration, their mutual crosstalk, and interdependency are exciting topics of ongoing and future research in PH of which the interaction between mast cells and B cells via cytokines of the IL-6 family as outlined above may only serve as prototypical example. At present, our insight into the individual mechanisms that trigger adaptive versus innate immune responses in PH is rudimentary, as is our understanding regarding their differential potential as therapeutic targets in PH. While an exhaustive discussion of this topic is beyond the scope of this manuscript, the dissection of innate and adaptive immune responses in PH clearly deserves deeper exploration in terms of experimental studies and state-of-the-art reviews.
Autoimmunity in pulmonary hypertension
The recognition of B cell activation and tertiary lymphoid tissue formation has recently fueled the intriguing hypothesis of a relevant autoimmune component in the pathogenesis and/or pathophysiology of PH. This view is supported by genomic analyses which identified a distinct RNA expression profile in peripheral blood B cells, indicative of their activation in patients with iPAH compared to healthy controls. 81 Notably, while differentiation of B cells to antibody-producing plasma cells was originally considered to be restricted to lymph nodes, 82 the recent recognition of functional ectopic lymphoid tissues adjacent to remodeled vessels in lungs of patients with iPAH clearly demonstrates that B cell differentiation and subsequent antibody production can occur and may be regulated at the local level in PH lungs. 83 Many of these ectopic lymphoid tissues form germinal centers where somatic hypermutation and class-switching occur, thereby providing an optimal environment for the generation of pathogenic autoantibodies. 83 Formation of autoantibodies has long been recognized as a key factor that is assumed to account for the high prevalence of PAH in patients with connective tissue diseases (CTDs) such as systemic sclerosis84,85 or Sjögren's syndrome 86 where antibody deposits have been found localized in the pulmonary artery walls.87,88 However, the presence of tertiary lymphoid tissue in patients with iPAH as well as in various animal models of hypoxia- or monocrotaline-induced PH suggests a much broader relevance of autoimmunity in the pathogenesis of PAH. Along these lines, increased levels of various circulating autoantibodies have been detected in patients with non-CTD PAH: It is estimated that 10–15% of iPAH patients are positive for antiphospholipid antibodies, 89 30–40% express antinuclear antibodies,90,91 40% anti-fibroblast antibodies, 92 62% anti-endothelial cell antibodies,93,94 and up to 93% anti-fibrillin-1 antibodies. 95 In recent collaborative work, we furthermore identified the prevalence of circulating agonistic autoantibodies against endothelin receptor type A (ETAR) and the angiotensin receptor type-1 (AT1R), which not only predicted the development of PAH and PAH-associated mortality in patients with systemic sclerosis, but were also present in 11% and 21% of patients with iPAH, respectively. 96 The functional relevance of these autoantibodies was recently elegantly demonstrated, in that passive transfer of either autoantibody-rich plasma or purified immunoglobulin (Ig) G from rats with monocrotaline-induced PH was sufficient to induce the de novo formation of lung ectopic lymphoid tissue and the development of PH in naïve rats. 97 Notably, increased production of autoantibodies does not seem to be restricted to PAH patients or the monocrotaline model of PH, as increased levels of circulating immunoglobulin G were similarly detected in a rat model of PH with left heart disease, 26 in which moreover immunoglobulin-encoding genes were found to be the most mast cell-dependent regulated genes in lung tissue. 26 While these findings point to an overarching relevance of pathogenic autoantibodies in the development of PH that is not restricted to CTDs, the mechanisms that drive this acquired autoimmunity remain unclear.
Autoimmunity emerges when the fragile balance between self-recognition and protection from non-self-pathogens is lost. 98 It has been estimated that 50–75% of newly produced human B cells are autoreactive and must be eliminated by tolerance mechanisms. 99 This B cell tolerance is established at multiple checkpoints throughout B cell development, both in the bone marrow and in the periphery by mechanisms such as receptor editing, clonal deletion, and anergy, which serve to eliminate autoreactive B cells.100–102 The actual development of autoimmunity is driven via the activation of distinct pro-inflammatory signaling pathways, which have accordingly emerged as potential novel therapeutic targets for individual autoimmune diseases, including transcription factors such as STAT4, 103 cytokines such as interleukin-17, 104 or alarmins such as high mobility group box 1 (HMGB1).105–107 HMGB1 gains particular relevance as a potential link between inflammation/autoimmunity and pulmonary vascular disease through its recent implication in both clinical and preclinical PAH. HMGB1 is abundant both in serum and in vascular lesions of patients with iPAH,108,109 and the increase in circulating HMGB1 correlates with mean pulmonary artery pressure. 108 Evidence for a functional role of HMGB1 in PAH comes from rodent models of chronic hypoxia and monocrotaline, respectively, where treatment with anti-HMGB1 antibodies attenuated the development of PH108,110 as did a non-specific inhibitor of HMGB1, glycyrrhizin. 111 Notably, the fact that actively secreted HMGB1 is primarily derived from macrophages 112 provides an intriguing link to a series of recent publications which attribute a key role for macrophages in the initiation of PAH.113–117 Indeed, remodeled vessels in lung samples of patients with iPAH are often surrounded by HMGB1-positive cells in the adventitia 109 where perivascular macrophages accumulate in PAH. 118 Of particular relevance in the context of autoimmunity, extracellular HMGB1 in isolation or in complex with DNA promotes the proliferation and activation of autoreactive B cells.119–121 Consistent with this view, autoantibody production was recently found to correlate with HMGB1 serum levels in patients with systemic lupus erythematosus. 122 Conversely, blockade of extracellular HMGB1 suppresses xenoreactive B cell responses, autoantibody production, and delays acute vascular rejection following heterotopic heart xenotranplantation. 123 Additionally, HMGB1, as a part of DNA-anti-DNA immune complexes, can interact with the receptor for advanced glycation endproducts (RAGE) on the surface of plasmacytoid dendritic cells and B cells leading to TLR9-dependent interferon-α release and activation of autoreactive B cells. 124 The latter aspect may be of particular relevance in the context of PH as RAGE activation is increased in PAH patients and systemic vascular diseases.125,126 Thus, HMGB1 emerges as a potent trigger and promoter of autoimmunity via both direct and indirect effects on B cells and as a trigger or promoter of vascular remodeling in PH; yet although it is tempting to postulate a functional link between these two effects a direct causal interrelationship remains to be shown.
The endothelium in inflammation and immunity
What remains obscure and has not been addressed in either preclinical or clinical studies so far is the origin of these inflammatory and immune cells in PH, and the mechanisms that trigger and regulate their recruitment to the lung parenchyma and into the vicinity of the remodeling pulmonary blood vessels. At later stages of the disease, some of these cells may expand locally within the tissue and the newly formed lymphoid tissues, yet it seems fair to assume that at least initially the inflammatory cells infiltrate the lung largely from the circulating blood. This notion is supported, for example, by flow cytometric analyses in chronic hypoxic mice demonstrating the mobilization of cells positive for the mast cell (and stem cell) marker c-kit from the bone marrow into the circulation and their subsequent accumulation in remodeled pulmonary artery vessel walls.127,128 In neonatal rats and calves, development of chronic pulmonary hypertension required the recruitment of a monocyte/macrophage precursor from the circulating blood into the pulmonary perivascular space. 129 Similarly, flow cytometric analyses in various organs of rats with monocrotaline-or SU5416/hypoxia-induced PH revealed an increase in B cells abundance in virtually all organs including lung, lymph nodes, spleen, and circulating blood with the notable exception of bone marrow. 26
It remains unclear whether the inflammatory and immune cells that migrate into the lungs in PH are recruited directly from the pulmonary arteries or arterioles, from the vasa vasorum and the perivascular capillary network,
130
or from the lymphatic vasculature. That notwithstanding, the recruitment will have to occur along the lines of the classic leukocyte adhesion and migration cascade that has been extensively studied and described in the past (Fig. 2). In brief, in order for circulating leukocytes to leave the blood stream and enter the perivascular space and the lung parenchyma, they first need to interact, adhere, and ultimately migrate through the vascular (or, alternatively, lymphatic) endothelium in a tightly controlled sequence of events.131,132 This cascade comprises initial steps of tethering and rolling, followed by firm arrest and occasional crawling along the vessel wall until the inflammatory cell exits the vessel by ways of paracellular or, occasionally, transcellular migration. The sequential steps of this adhesion cascade are mediated by the interaction of adhesion molecules expressed on the vascular endothelium with their respective counterligands on circulating leukocytes or platelets that may in turn form aggregates with leukocytes.
133
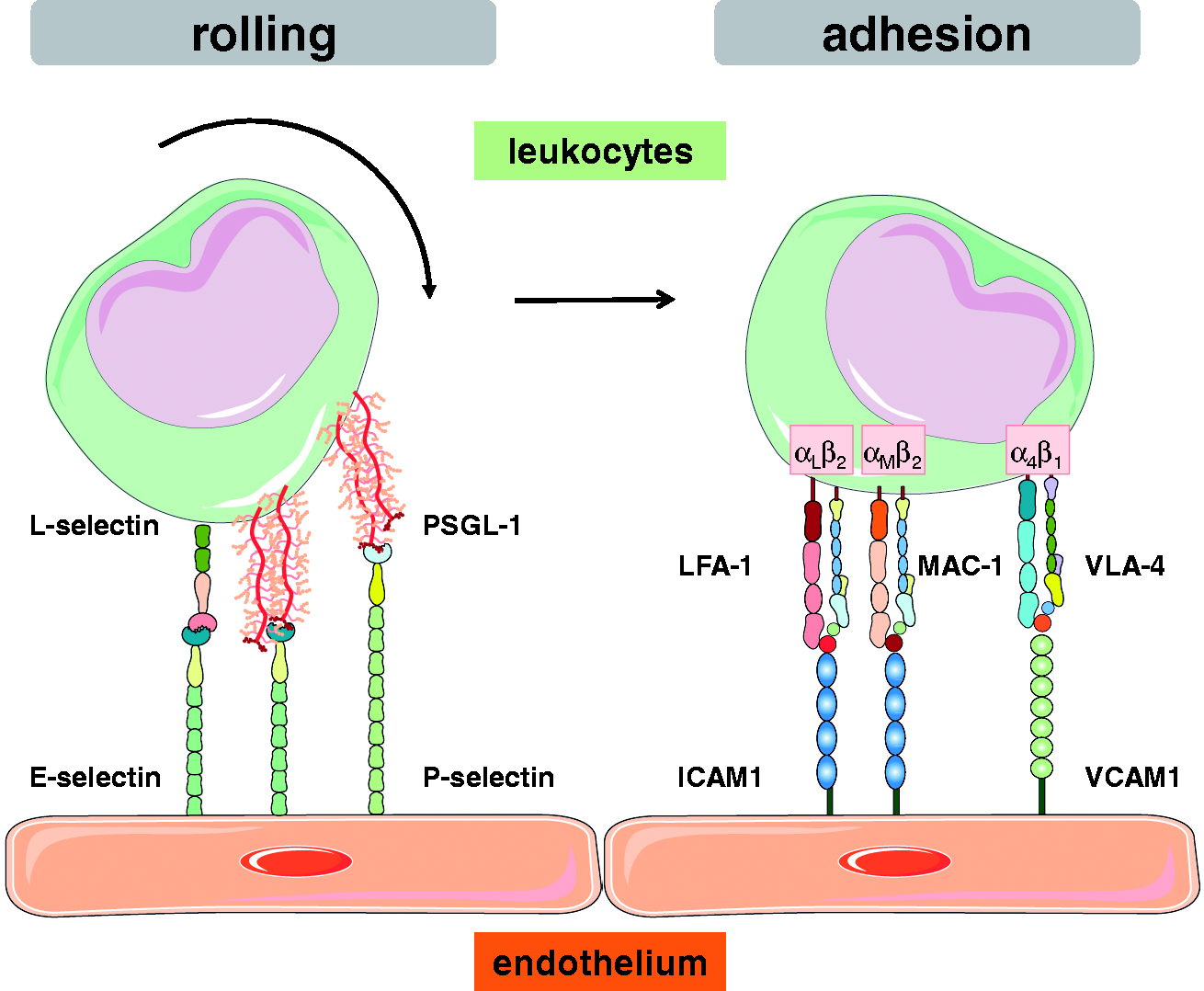
In what has become known as the classic paradigm of the leukocyte adhesion cascade, leukocytes first start to role via the interaction of leukocytic L-selectin and P-selectin glycoprotein ligand-1 (PSGL-1) with P- and E-selectin expressed on the vascular endothelium, and may subsequently adhere via CD11a/CD18 (lymphocyte function-associated antigen 1, LFA-1) or CD11b/CD18 (macrophage-1 antigen, Mac-1) interacting with ICAM-1, or integrin α4β1 (very late antigen-4, VLA-4) interacting with vascular cell adhesion protein 1 (VCAM-1) (Fig. 3). This general concept applies not only for neutrophils, but equally for migrating mast cells,134,135 B cells,
136
and mononuclear cells.
137
While the exact molecular players that orchestrate this sequence will vary between different vascular beds and leukocyte subsets, it is a fundamental paradigm that each of these steps is mediated by the intimate interaction of adhesion molecules expressed on the infiltrating leukocyte on the one, and the vessel outlining endothelium on the other hand.
137
Schematic representation of the classic leukocyte adhesion cascade. Following initial tethering at the endothelial cell surface, leukocytes start to roll and ultimately may firmly arrest on the vessel surface to finally migrate into the subendothelial space, typically via a paracellular but occasionally also via a transcellular route. Schematic representation of central adhesion molecules mediating rolling and firm adhesion of circulating leukocytes on the vascular endothelium. Rolling is mediated by interaction of endothelial E- and P-selectin with L-selectin and P-selectin glycoprotein ligand-1 (PSGL-1) on the surface of the leukocyte, while firm adhesion involves interaction of endothelial intercellular adhesion molecule (ICAM)-1 with αLβ2 (lymphocyte function-associated antigen 1 [LFA-1]) or αMβ2 (macrophage-1 antigen [MAC-1]) integrin, or interaction of vascular cell adhesion molecule 1 (VCAM-1; CD106) with α4β1 integrin (very late antigen 4 [VLA-4]) on the leukocyte.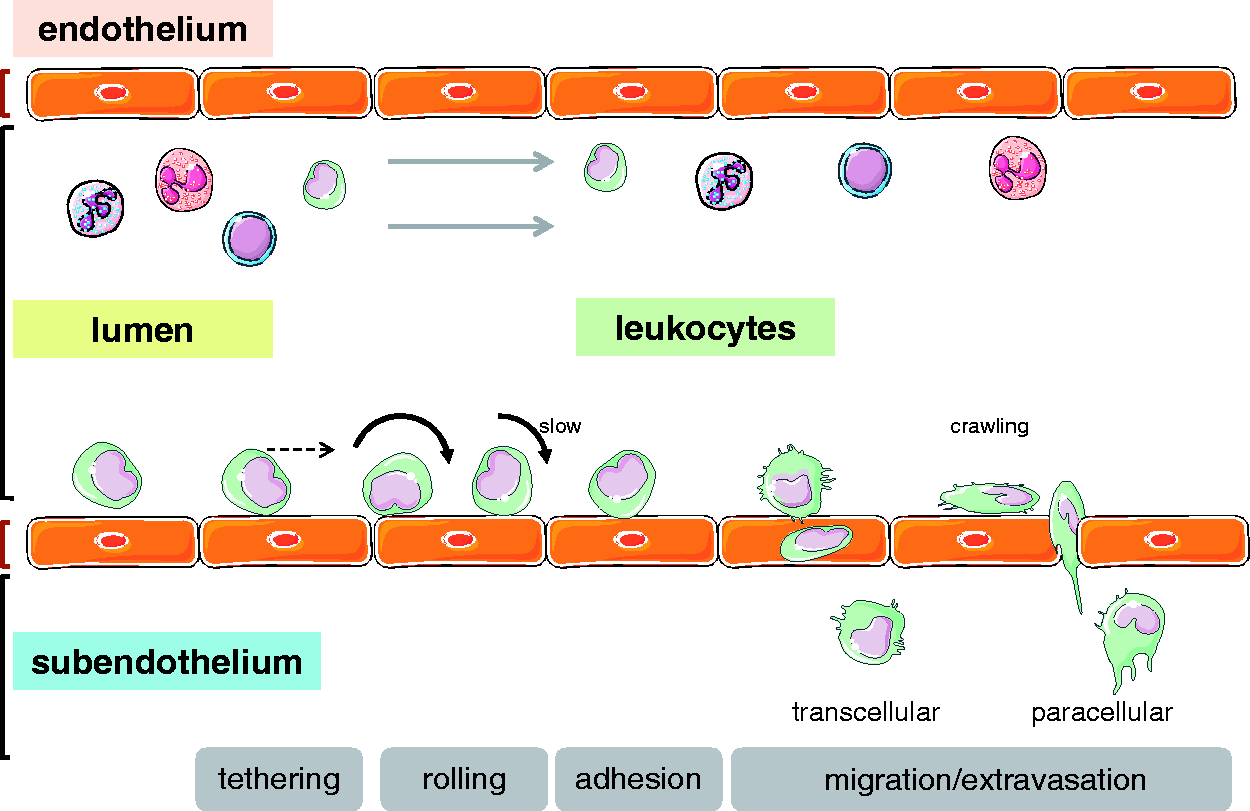
With that in mind it must come as a surprise that so far no clinical or preclinical studies have to our knowledge addressed the role of specific adhesion molecules in PH, either by pharmacological or antibody blockade or by genetic deletion strategies. There is, however, an abundance of studies that have reported elevated levels of circulating soluble adhesion molecules in PH patients. As such, marked increases in the plasma concentration of soluble P-selectin have been detected in PAH patients with either idiopathic138,139 or non-idiopathic disease. 138 Similarly, patients with PH due to left heart disease have been found to exhibit higher circulating levels of soluble P-selectin, although this finding did not reach significance, 138 and P-selectin expression on platelets as an indicator of their activation is increased in patients with chronic thromboembolic pulmonary hypertension (CTEPH). 140 In patients with congenital heart disease (CHD), P-selectin genotype polymorphism of -825T/C differs significantly between patients with and without PH, suggesting a potential contributory role of the P-selectin genotype in the development of PH in this patient population. 141 Circulating levels of soluble P-selectin did, however, not correlate with World Health Organization functional class (FC) or transplant-free survival in a recent biomarker study in 65 PAH patients, 142 and were not associated with changes in 6-min walk distance or FC in response to PAH therapy by trepostinil. 143
For soluble E-selectin, elevated levels have been reported in iPAH patients compared to healthy controls. 144 Likewise, soluble intercellular adhesion molecule-1 (ICAM-1) levels in serum are significantly higher in children with PAH secondary to CHD compared to children with CHD without associated PAH, or in a healthy control group.145,146 ICAM-1 levels are also increased in iPAH patients and patients with PAH associated with connective tissue disease (PAH-CTD), whereas circulating levels of soluble vascular cell adhesion protein 1 (VCAM-1) were elevated in PAH-CTD only. 147 Conversely, soluble ICAM-1 levels decreased when young patients with CHD and PH were treated with the phosphodiesterase 5 inhibitor sildenafil. 148 Interestingly, ICAM-1 expression on pulmonary arterial but not microvascular endothelial cells can be increased when endothelial cells are exposed to microparticles isolated from PH rats. 149 In line with their proposed role as disseminators of inflammatory signaling in the lung, 150 circulating microparticles may thus specifically promote inflammatory responses in the pulmonary arterial compartment in PAH.
In sickle cell patients, circulating levels of soluble vascular cell adhesion protein 1 (VCAM-1) show the most consistent correlation with PAH, while ICAM-1, E- and P-selectin show correlations and/or linearity in some but not all studies.151,152 In systemic sclerosis, circulating levels of soluble P-selectin, ICAM-1, VCAM-1 and platelet endothelial cell adhesion molecule-1 (PECAM-1) were found markedly elevated. While this effect was seemingly independent from the presence or absence of PAH, treatment of PAH with the endothelin-1 receptor antagonist bosentan significantly reduced the levels of all four adhesion molecules by up to 80%. 153 Notably, since PECAM-1 acts as important endothelial shear sensor, increased cleavage of PECAM-1 from the endothelial surface may not only result in elevated levels of circulating soluble PECAM-1, but also impair microvascular adaptation to shear and thus, promote the development of occlusive vascular lesions in PAH. 154
In addition to analyses of circulating soluble adhesion molecules, a few studies have addressed the expression of endothelial adhesion molecules in human tissue samples or primary endothelial cells, respectively. As such, Vengethasamy et al. showed that pulmonary microvascular endothelial cells isolated from lungs of transplanted PAH patients show an elevated ICAM-1 expression in BMPR2 mutation carriers compared to patients without mutations. 155 Consistent with this finding, pulmonary microvascular endothelial cells from BMPR2 mutation carriers showed an enhanced adhesiveness for monocytes in response to inflammatory mediators, suggesting that BMPR2 mutations could increase the susceptibility to inflammatory cell recruitment in PAH. 155 In line with these data, Le Hiress et al. detected an increased expression of the adhesion molecules ICAM-1, VCAM-1, and E-selectin on the endothelium of pulmonary arteries in human iPAH compared to controls that was associated with a higher number of peripheral blood mononuclear cells adhering to the endothelium. 156
Taken together, these studies at large demonstrate an association of increased levels of circulating or endothelial adhesion molecules with PH, whereby the individual adhesion molecules may vary based on severity, time course, or underlying cause/class of the disease. Expectedly, adhesion molecule expression correlates with leukocyte interaction with the pulmonary endothelium in PH; importantly, however, experiments on the functional role of adhesion molecules in PH in vivo are to our knowledge lacking as of now.
The potential triggers of endothelial inflammation and adhesion molecule expression in PH are likely manifold, and would exceed the purpose of this review. It must suffice to point out that, for example, endothelial expression of P-selectin is stimulated by most of the classic triggers of PH in animal models, including monocrotaline, 157 hydrostatic stress, 158 or hypoxia159,160 (modelling clinical PH of groups 2, 3, and—arguably in case of MCT—group 1, respectively). Similarly, environmental stresses, endothelial dysfunction, or injury will inevitably upregulate endothelial adhesion molecules and, thus, facilitate inflammatory cell infiltration into the vessel wall and perivascular space as well as trigger formation and release of pro-inflammatory cytokines. Finally, it is tempting to speculate that DNA damage, mosaic chromosomal abnormalities, and microsatellite instabilities as previously detected in pulmonary arterial endothelial cell cultures from PAH lungs161–164 may facilitate expression of adhesion molecules and inflammatory cell recruitment, yet this concept remains to be experimentally tested.
Summary
Intriguingly, the recognition of an inflammatory and autoimmune component in PH sheds new light on the pivotal role of the endothelium in this disease that extends beyond classic concepts of endothelial damage or dysfunction, endothelial apoptosis and proliferation, or anti-endothelial antibodies,26,165 but points to a key role of the endothelium and its adhesion molecules as first line in the regulation of inflammatory and immune cell recruitment and infiltration (Fig. 4). While respective mechanistic studies seem long overdue, premature enthusiasm for potential translational benefits should be cautioned. Some 25 years ago, therapeutic targeting of adhesion molecules for the treatment or prevention of inflammatory disorders such as sepsis or the adult respiratory distress syndrome (ARDS) had already received a huge surge of attention both from the scientific community and industry; yet, to this date no approved therapy based on these concepts has materialized. That notwithstanding, a better understanding of the how, where, and when of immune cell adhesion and recruitment in PH may provide important novel insights into the mechanisms of disease, and—potentially—identify new therapeutic targets.
Schematic summary of the proposed role of the endothelium and its adhesion molecules in PH. Endothelial adhesion and subsequent emigration of monocytes, mast cells, T cells, and B cells is an essential step for inflammatory and immune cell recruitment and infiltration. Following migration into the vascular wall and adventitial space, emigrated cells will further promote perivascular abundance of immune cells by perivascular differentiation and proliferation as well as by additional recruitment of immune cells via the release of pro-inflammatory and chemotactic mediators such as cytokines, alarmins, or leukotrienes. Perivascular accumulations of T cells, B cells, plasma cells, and dendritic cells organize into ectopic lymphoid tissue, which acts as source of autoantibodies and immune-cell derived mediators such as cytokines driving intimal and medial proliferation and, thus, vascular remodeling in PH.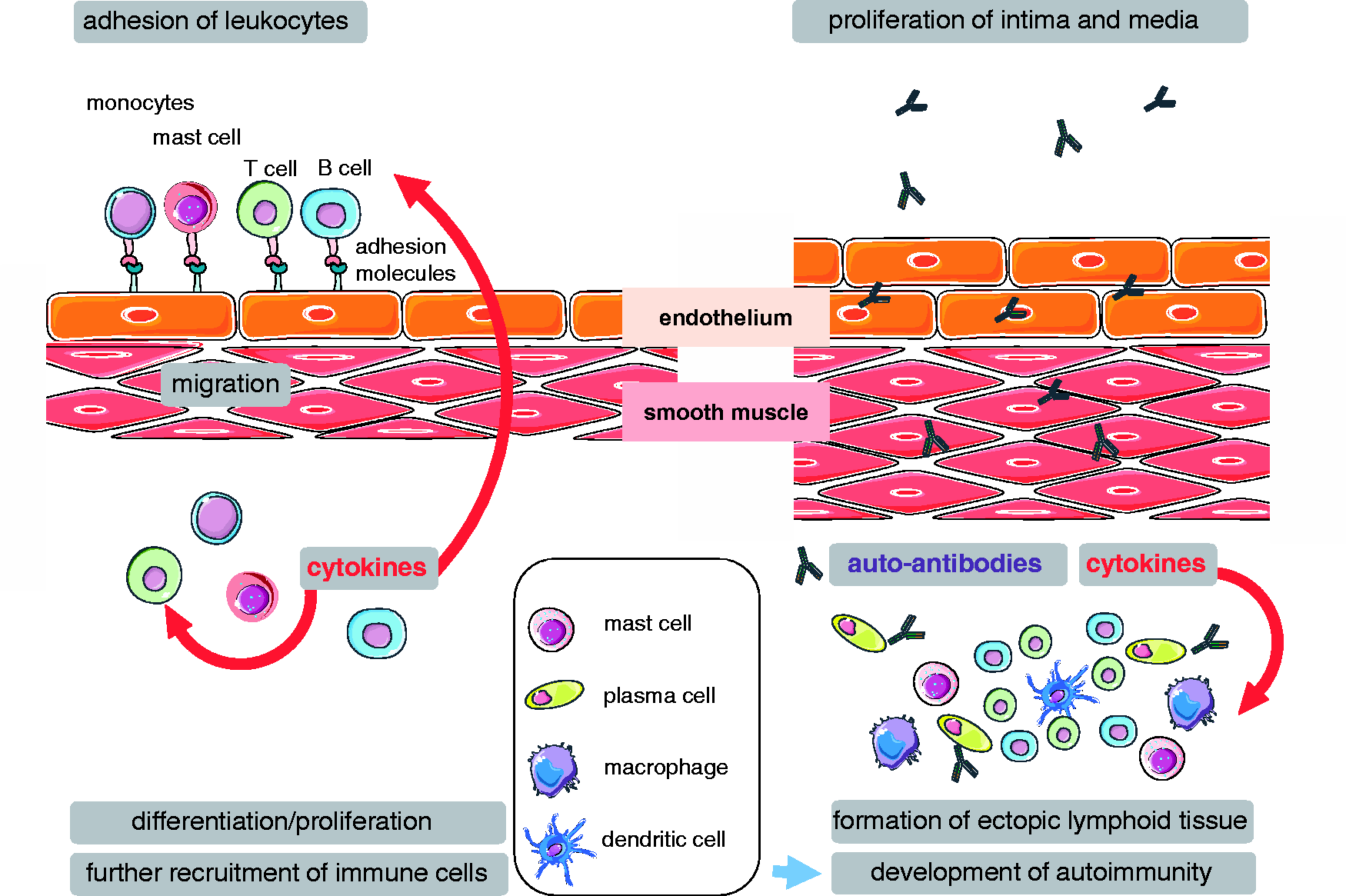
2017 Grover Conference Series
This review article is part of the 2017 Grover Conference Series. The American Thoracic Society and the conference organizing committee gratefully acknowledge the educational grants provided for the support of this conference by Actelion Pharmaceuticals US, Inc., Gilead Sciences, Inc., and United Therapeutics Corporation. Additionally, the American Thoracic Society is grateful for the support of the Grover Conference by the American Heart Association, the Cardiovascular Medical Research and Education Fund, and the National Institutes of Health.
