Abstract
Background:
Although commonly used in anxiety and insomnia, recent guidelines recommend caution when prescribing benzodiazepines in the elderly. Here we examined rates of benzodiazepine prescribing to older adults in Ontario, Canada from 1998 to 2013 and impact of legislation that made prescribing regulations more strict.
Method:
Annual benzodiazepine prescription rates for Ontario residents aged 65 and over were examined using the Ontario Drug Benefit database which captures all publicly funded prescriptions. Since most drugs, including benzodiazepines, are funded for residents aged ⩾65, data are essentially population-based. Weighted least squares regression methods were used to examine trends in prescribing rates (all benzodiazepines, anxiolytics, hypnotics, short- and long-acting drugs and individual drugs) from 1998 to 2013 for all Ontario residents aged ⩾65 and by sex and 5-year age bands. Impact on monthly prescribing rates of legislative changes (November 2011) which aimed to promote appropriate prescribing and dispensing practices for controlled substances, including requiring prescribers to record specified information, was assessed by constructing an interrupted time-series model.
Results:
Benzodiazepines were prescribed to 23.2% of the 1,412,638 Ontario residents aged ⩾65 in 1998, declining to 14.9% of 2,057,899 residents aged ⩾65 in 2013 (p < 0.001 for trend). Rates were significantly greater throughout in older age bands (p < 0.001) and 1.54–1.62 times greater in females than males (p < 0.001). Lorazepam was the most prescribed benzodiazepine throughout, but rates declined from 11.4% in 1998 to 8.5% in 2013. Diazepam rates fell from 2.3% to 0.7%. However, clonazepam prescription rates increased until 2011, 1.7-fold overall. After the November 2011 legal changes, downward shifts were observed in total benzodiazepine prescription rates and for each drug individually. The step function, conditional on covariates, suggested benzodiazepine rates after November 2011 were 2.89 per 1000 (p < 0.001) below rates observed previously, representing a relative reduction of 4.8% compared to the year before the intervention.
Conclusion:
Benzodiazepine prescribing rates declined markedly in this population from 1998 to 2013. Targeted legislation may have reduced rates, but the effect, although statistically significant, was small.
Introduction
Benzodiazepines, introduced in the early 1960s, were for many years considered a first-line treatment, both for anxiety disorders and for insomnia. They additionally are employed in alcohol detoxification protocols, as muscle relaxants, for severe agitation and for their antiepileptic properties. Pharmacologically, benzodiazepines are positive modulators at the GABA-A benzodiazepine receptor, binding to a specific site which communicates with other receptor structures to allow opening of a central chloride channel in the presence of GABA, thereby contributing to inhibitory effects through neuronal hyperpolarization.
Anxiety disorders are very common and carry high costs to society. 1 They can be treated effectively with several drug classes, including many antidepressants across several subclasses, as well as pregabalin, buspirone and some atypical antipsychotics.2–4 Benzodiazepines are no longer considered the first-line treatment in anxiety disorders, in part due to concerns relating to tolerance and difficult withdrawal, especially on prolonged use, but remain a viable short-term treatment option especially where rapid relief from anxiety is required. While some guidelines advise against use beyond 4 weeks in the context they are addressing, 5 others specify circumstances in which they can be an appropriate longer-term treatment – for example in selected patients who have failed on other treatments, do not have a history of substance misuse and have not escalated their dose. 6 Some benzodiazepines such as temazepam and nitrazepam have been used primarily for their sleep-promoting properties. Zopiclone, its isomer eszopiclone and the related drugs zolpidem and zaleplon, collectively known as z-drugs have come to market more recently. 7 These drugs also bind to the GABA-A benzodiazepine receptor, but at a different site, and are therefore not considered to be benzodiazepines although they share many pharmacological properties with the benzodiazepine class.
Disadvantages of benzodiazepine use have emerged, not only through their associations with tolerance and difficult withdrawal, 8 but also through their propensity to cause sedation, motor impairment, falls and fractures, 9 accidents10,11 and cognitive impairment in long-term use.12–14 Many of the latter effects have the potential to be especially problematic in the elderly, where there is evidence of excess rates of hip fractures, 15 motor vehicle accidents 16 and cognitive impairment during hospitalization. 17 For these reasons, benzodiazepine use in older people is seen as presenting a greater burden of risk than in younger populations. Prescribers are advised to consider these risks before initiating treatment. 6 A recent Canadian Guideline described the widespread use of long-term benzodiazepine treatment in the elderly 18 as a ‘cause for concern’. 3
A previous retrospective population-based study using the same database 19 described temporal trends in benzodiazepine prescribing to Ontario residents aged 65 and over between 1993 and 1998. They reported a small but significant reduction in overall benzodiazepine prescription rates (25.1% versus 22.5%) over this period, greater use in females (relative risk = 1.5), and increasing rates of benzodiazepine prescription with increasing age. Tu and colleagues 19 also examined the ratio of the number of people to whom short-acting versus long-acting drugs were dispensed, citing literature from the period which suggested that, in general, short-acting benzodiazepines were thought to be safer than long-acting drugs in the class. A progressive increase in this ratio of over 60% from 1993 to 1998 was reported and was interpreted as implying improved prescribing practices. Tu and colleagues 19 projected that both the reduction in the overall prescription rates and the increase in the ratio of short-acting to long-acting benzodiazepine prescribing rates would continue in subsequent years. However, the thesis prevalent in the 1990s, that prescription of short-acting benzodiazepines should be considered inherently preferable to long-acting benzodiazepines, has lost credence in the interim. As early as 1999 a Canadian guideline 20 cited concerns that short-acting drugs were more likely to cause rebound and withdrawal. A more recent population-based longitudinal study 21 reported that people taking short-acting benzodiazepines were 2–5 times more likely to go on to long-term use than those taking long-acting benzodiazepines. In contemporary literature there is little enthusiasm for the suggestion that longer-acting drugs in the class should be replaced by shorter-acting benzodiazepines. Indeed, an American Psychiatric Association Guideline on treatment of panic disorder specifically highlights the potential desirability of using clonazepam over shorter-acting drugs due its potential for easier dosing and reduced likelihood of withdrawal symptoms after missed doses. 22
In November 2011, changes were made to the legal framework governing benzodiazepine prescribing in Ontario 23 through the Narcotics Safety and Awareness Act. 24 These changes were introduced with the aim of promoting appropriate prescribing and dispensing practices for a range of controlled substances, including requiring prescribers to record specified information (registration number and patient name, address, age, sex and government-issued identification number on prescriptions for ‘monitored drugs’, which included all benzodiazepines) and dispensers to verify that the necessary information was present.
Aims
The aims of the study were as follows:
To describe patterns of benzodiazepine dispensing in the Ontario population aged 65 and over, by year from 1998 to 2013, stratifying for gender and age (5-year bands).
To examine trends in benzodiazepines subdivided by (a) long-acting versus short-acting (as per Tu and colleagues) 19 and (b) by anxiolytic and hypnotic benzodiazepines; and (c) to examine trends specifically in the most commonly prescribed benzodiazepines, the anxiolytics diazepam, lorazepam, clonazepam, oxazepam and alprazolam, and the hypnotics temazepam and nitrazepam.
To examine the impact of the legal changes introduced in November 2011 on monthly benzodiazepine prescription rates.
Methods
Setting and design
The study employed standardized data registers in the province of Ontario, Canada to examine crude numbers of prescriptions and prescription rates for benzodiazepines. The design was cross-sectional, with observations repeated annually (and for one analysis, monthly) over a period of 16 years to allow prescribing trends to be described longitudinally.
The Institute of Clinical Evaluative Sciences (ICES) is a prescribed entity under section 45 of Ontario’s Personal Health Information Protection Act. Section 45 is the provision that enables analysis and compilation of statistical information related to the management, evaluation and monitoring of, allocation of resources to, and planning for the health system. Section 45 authorizes health information custodians to disclose personal health information to a prescribed entity, such as ICES, without consent for such purposes. Although projects conducted wholly under section 45, by definition, do not require research ethics board (REB) review, the REB at Sunnybrook Health Sciences Centre (ICES’ REB of Record) has agreed to help ICES achieve a higher ethical standard for the use of administrative and other data held at ICES. This is done using a retrospective review process whereby, at the end of each calendar year, ICES submits a report on the projects undertaken that year to the REB for review and approval. Accordingly, the present project was included in and approved under the 2015 Sunnybrook Health Sciences Centre REB annual review. In addition, ICES required a Privacy Impact Assessment, which was approved in September 2015 with the reference number 2016 0904 814 000.
Data sources
The Ontario Drug Benefit (ODB) program database records all government-supported prescription drugs dispensed to Ontario residents, except those used in a hospital inpatient setting. Since the government supports all prescriptions for drugs appearing on the provincial formulary for residents aged 65 or older, records are essentially population based for this age group. We identified benzodiazepine prescriptions using the ODB program database dispensed in each year from 1998 to 2013. Information on age, gender and date of death for Ontario residents were derived from the Registered Persons Database and linked to the prescribing data through the healthcare number. The population studied was made up of all people who were both (1) aged ⩾65 (including those reaching their 65th birthday by 30 June of that year); and (2) resident in Ontario at any point in the year and eligible for coverage through the Ontario Health Insurance Plan (OHIP). Any individuals with age missing were excluded. For each year, we assessed the total number of people to whom at least one prescription was dispensed for each of the categories in the list below. We used census data from Statistics Canada to derive Ontario population data for each year, to calculate the denominator of individuals resident in the province aged ⩾65, and were therefore able to express the figures for benzodiazepine use both as a crude number of individuals in each year and as a percentage of the population. For the analysis relating to the impact of legal changes in November 2011, we extracted the rate of benzodiazepine prescriptions dispensed for each month from January 1998 to December 2013. Data relating to long-term care-residence was ascertained from the Continuing Care Reporting System database.
Benzodiazepine ascertainment
We examined prescription rates (having at least one dispensed prescription in the calendar year) for each of the following categories: (1) Any benzodiazepine prescription dispensed. (2) Any anxiolytic benzodiazepine prescription dispensed – alprazolam, bromazepam, chlordiazepoxide, clonazepam, clorazepate, diazepam, lorazepam, oxazepam (Table 1). The classification described by Ashton 8 considers all of these drugs to be primarily anxiolytic and, with the exception of bromazepam, have all received FDA approval for treatment of anxiety or of a specific anxiety disorder. (3) Any hypnotic benzodiazepine prescription dispensed – flurazepam, nitrazepam, temazepam, triazolam (Table 1) [since the non-benzodiazepine ‘z-drugs’ are either not available in Ontario (eszopiclone), not on the ODB formulary (zolpidem, zaleplon) or funded only in exceptional circumstances (zopiclone), we did not examine the use of these drugs in the current study]. (4) Any ‘long-acting’ benzodiazepine prescription dispensed – chlordiazepoxide, clorazepate, clonazepam, diazepam, flurazepam, nitrazepam (Table 1). (5) Any ‘short-acting’ benzodiazepine prescription dispensed – alprazolam, bromazepam, lorazepam, oxazepam, temazepam, triazolam (Table 1). (As in Tu and colleagues, 19 midazolam, a short-acting benzodiazepine used for status epilepticus, injected as part of operative premedication and anesthesia or in intensive care, and infused for sedation in palliative care settings, was not included in this analysis). (6) Any prescription dispensed of the following most commonly prescribed benzodiazepine drugs considered individually: (a) alprazolam, (b) clonazepam, (c) diazepam, (d) lorazepam, (e) oxazepam, (f) temazepam and (g) nitrazepam. The above categories were tabulated for each year from 1998 and 2013 and were then stratified by sex and age (in 5-year bands). The ratio of the proportion of individuals in the population aged ⩾65 prescribed at least one short-acting benzodiazepine to that of individuals prescribed at least one long-acting benzodiazepine was examined for each calendar year.
Benzodiazepines available through the Ontario Drug Benefit (ODB) program that were included in this study, divided as (a) anxiolytic versus hypnotic and (b) short-acting versus long-acting.

Includes ‘Chlordiazepoxide HCL’.
Statistical analysis
Weighted least squares regression methods were used to examine trends in prescribing rates from 1998 to 2013 for the whole sample of Ontario residents aged over 65 and by sex and 5-year age bands. The weighted least squares regression gave weight to the population in each year, since the variability in the rate of benzodiazepine prescription over the 16-year period was not the same as the population increases in each year.
To determine the impact of intervention of November 2011, which altered benzodiazepine prescription requirements, on prescription rates, we examined impact on monthly benzodiazepine prescribing rate by constructing an interrupted time-series model. Data from January 1998 up to December 2013 were used to estimate the effect of the legislative change by calculating a step function where a dummy variable for the intervention date is included in the regression model. Seasonal differencing was also used to account for seasonal variation in prescribing rates. A Ljung–Box test 25 was used to test for stationarity of the trend.
Results
Overall the number of individuals prescribed at least one benzodiazepine/calendar year declined from 23.2% of the Ontario population aged ⩾65 (n = 1,412,638 residents) in 1998, to 14.8% in 2013 (n = 2,057,899 residents) (p < 0.001 for trend) (Table 2, Figure 1), a reduction of 36.1%. Similar trends were observed in both males and females. Prescribing rates in females were consistently between 1.54 and 1.62 times that observed in males (p < 0.001). In every year, individuals with a single benzodiazepine prescription in the calendar year accounted for around one-quarter (between 25.0% and 26.5%) of those prescribed benzodiazepines, with the remaining 73.5–75% of those prescribed benzodiazepines having more than one prescription.
Prescription rates for benzodiazepines (BDZs) 1998–2013 in the Ontario population aged ⩾65, stratified by sex and illustrating rates for >1 BDZ prescription/year, anxiolytic BDZ prescription and hypnotic BDZ prescription.

p < 0.001 for trend.
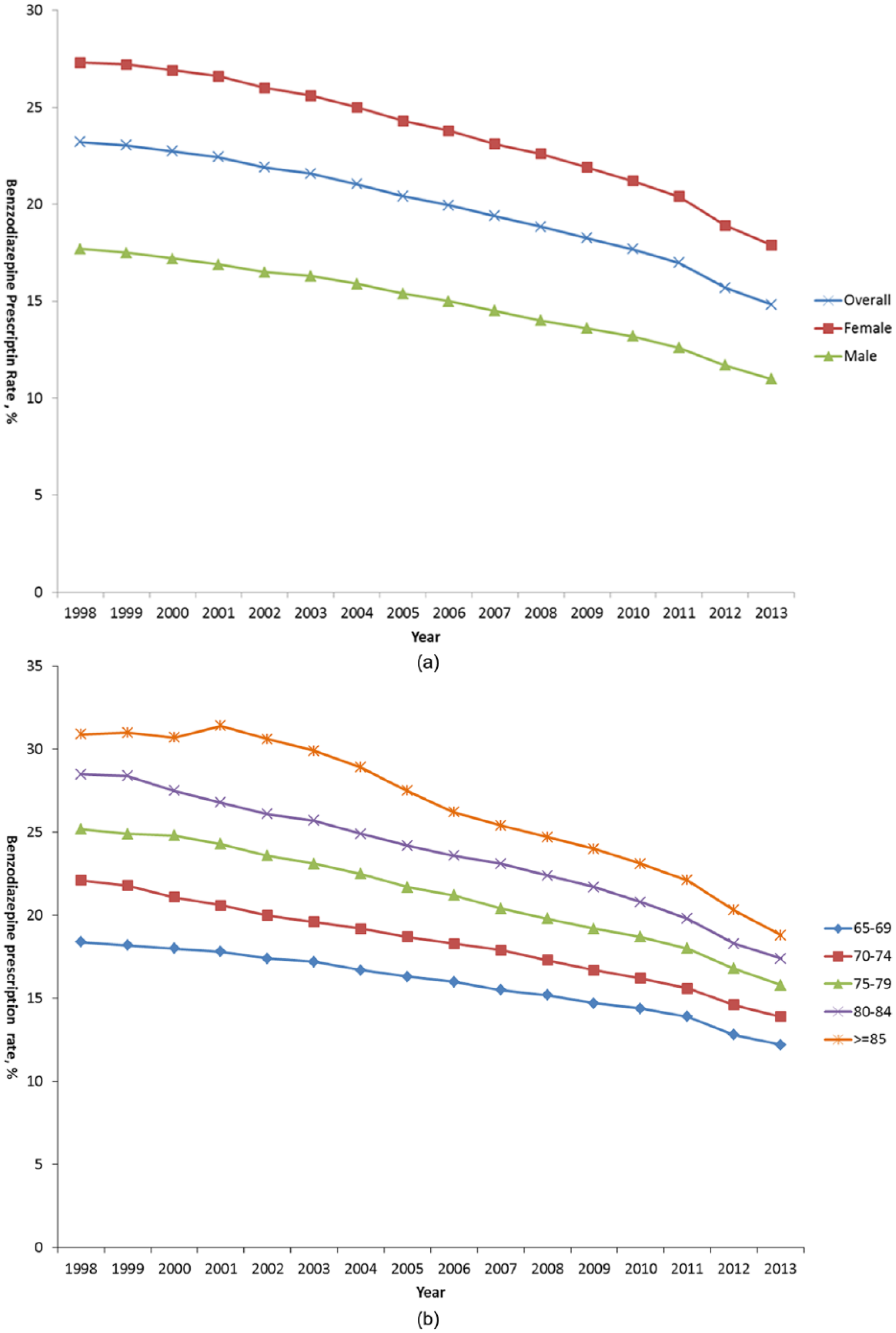
Percentage of Ontario population aged ⩾65 having at least one benzodiazepine prescription in 1998–2013. (a) Overall and stratified by sex. (b) Stratified by age group.
Benzodiazepine prescriptions were dispensed more frequently to those in older age bands; in all 16 years examined, the increasing prevalence in increasing age groups was highly significant (p < 0.001) (Figure 1). In the oldest age band (⩾85 years) the rate of benzodiazepine prescription fell progressively from 30.9% in 1998 to 18.8% in 2013 (p < 0.001), while the rate in the youngest age band (65–69 years) saw sustained but less pronounced reductions from 18.5% in 1998 to 12.2% in 2013 (p < 0.001). Thus, over the course of the observation period the disparity between prescribing rates in the youngest and oldest age bands was reduced. The proportion of individuals residing in long-term care facilities out of the total number of benzodiazepines users was 8.0% in 1998, and this decreased to 7.1% in 2013 (p < 0.001). This change mirrored the similar reduction in long-term care-residence rates among all individuals prescribed any medication covered by the ODB program – the figures being 5.5% in 1998 and falling to 4.9% in 2013.
Hypnotic benzodiazepine prescription declined markedly over the study period, with 5.1% of residents aged ⩾65 receiving hypnotics in 1998 compared with 1.7% in 2013 (p < 0.001). For anxiolytic benzodiazepines the rate declined substantially, from 22.7% in 1998 to 14.4% in 2013 (p < 0.001) (Table 2).
The ratio of individuals receiving short-acting to long-acting benzodiazepine prescriptions (Figure 2) rose from 1998 to 2003, as had been observed in the earlier study in the period from 1993 to 1998, 19 reaching a peak of 4.06 in 2003. In males the peak was observed 1 year later in 2004. Overall, the subsequent decline in the years up to 2013 took the ratio to 3.43, a lower value than the 3.69 observed in 1998. As had been observed between 1993 and 1998, older age groups had a higher short-acting to long-acting benzodiazepine prescription ratio across all 16 years (Figure 2).

Ratio of short-acting (SA) to long-acting (LA) benzodiazepine prescriptions in the Ontario population aged ⩾65 in 1998–2013. (a) Overall and stratified by sex. (b) Stratified by age group.
Lorazepam was the benzodiazepine prescribed to the greatest proportion of Ontario residents aged ⩾65 throughout the period of observation (Figure 3). During this time the lorazepam prescription rate declined by over 25%, from 11.4% of the population in 1998 to 8.5% in 2013 (p-value for trend, p < 0.001). However, since the total benzodiazepine prescription rate declined more sharply than was observed for lorazepam, lorazepam’s share of the gradually shrinking total of benzodiazepine prescriptions markedly increased, with 40.9% of individuals prescribed a benzodiazepine receiving lorazepam in 1998, increasing to 51.7% in 2013. Diazepam declined the most rapidly of the seven most commonly prescribed benzodiazepines, a 70% reduction being observed, from 2.3% in 1998 to 0.7% in 2013 (p-value for trend, p < 0.001). By 2013, people receiving lorazepam outnumbered those receiving diazepam by a factor of 12.

Percentage of the Ontario population aged ⩾65 having at least one prescription for each of seven common benzodiazepines in 1998–2013.
After the changes in the Ontario law relating to prescription of benzodiazepines, which was introduced in November 2011, the changes observed year-to-year both in total prescription rates and in prescription rates for each drug individually tended more toward reduction than was observed prior to this time-point. This was observable both in the figures for use of all benzodiazepines (Figure 1) and those for individual drugs, most notably for lorazepam and temazepam (Figure 3). After consistent annual increases in the crude number of people prescribed lorazepam each year between 1998 and 2010, there was a reversal of this trend in 2011, when a small reduction in the crude number of individuals receiving lorazepam prescriptions was observed [from 183,991 (10.1% of the population aged over 65) to 183,870 (9.7%)]. After 2011 the reduction was more substantial, to 177,145 individuals (9.0%) in 2012 and 174,836 individuals (8.5%) in 2013.
Examination of monthly data for total benzodiazepine prescribing rates (Figures 4 and 5) revealed that after the November 2011 changes, observed rates for most months were below the lower 95% confidence limit predicted from data prior to November 2011 (Figure 5). The step function, conditional on covariates, suggested benzodiazepine rates after November 2011 were 2.89 per 1000 (p < 0.001) below rates observed prior to the change (Figure 4). While this sustained downward shift amounts to an absolute reduction of under 0.3% in the rate of monthly benzodiazepine prescriptions in the population aged ⩾65, it represents a relative reduction of 4.8% compared to the year before the intervention.

Benzodiazepine prescribing rates to Ontario residents aged ⩾65 by month (number of individuals with one or more prescription over total population aged ⩾65).

Actual benzodiazepine prescribing rates (per 1000 population of Ontario aged ⩾65) by month, for November 2010 to December 2013 and forecast rates by month, for November 2011 to December 2013.
Of all the commonly prescribed benzodiazepines, only clonazepam use increased consistently over the observation period in terms of the crude number of individuals receiving prescriptions (20,115 in 1998 versus 49,911 in 2013), a 2.5-fold increase (Figure 3). The proportion of the population aged ⩾65 prescribed the drug each year saw a consistent increase until 2011 [1.4% in 1998 versus 2.5% in 2011, a 1.7-fold increase (p-value for trend, p < 0.001)]. Following the change in Ontario law in 2011, the year-on-year increases in proportion of individuals filling at least one clonazepam prescription ceased, there being a slight decline from 2.54% in 2011 to 2.46% in 2012 and 2.43% in 2013. In terms of clonazepam’s share of total benzodiazepine prescribing, 5.1% of individuals prescribed a benzodiazepine received clonazepam in 1998; this increased to 14.8% in 2013.
Discussion
Benzodiazepine prescribing rates declined markedly in the Ontario population aged ⩾65 from 1998 to 2013. The overall reduction reported in the 16 years of this study was a continuation of the trend observed from the same data source in the period 1993–1998. 19 Another Ontario-based study of benzodiazepine prescribing rates in the elderly which examined more recent data 26 described a slight reduction in the rate of new chronic benzodiazepine prescription to the elderly following hospitalization between 1992 and 2005. In focusing on the post-hospitalization period, however, this study is limited to examining a subset of elderly patients over a limited period of follow up. The overall reduction in benzodiazepine prescription observed in Ontario was similar to the data from the neighbouring province of Manitoba, 27 where a population-based study reported a reduction in benzodiazepine prescription rates in the over 65s from 56 to 30 users per 1000 people between 1996 and 2012. Standardized datasets from primary care in the United Kingdom (which has a government-funded health service similar to that in Ontario) revealed a similar trend from 1991 to 2009, albeit in the general population rather than specifically in the elderly, 28 as did data from Australia identified from the period 1992–2011, which examined both number of prescriptions and total defined daily dose on an annual basis across the general population. 29 Meanwhile in France a recent population-based study examining incident rates of new benzodiazepine users from 2006 to 2012 reported a small reduction overall, the effect being more prominent in younger people aged 18–44 than in those aged ⩾65. 30 The limited change over the 6-year study period may be explained by the fact that z-drugs were included alongside standard benzodiazepines, although surprisingly clonazepam was excluded on the grounds that it was specifically indicated as an anticonvulsant. While clonazepam is approved only for epilepsy in Canada, Canadian guidelines 3 and textbooks 31 recognize its widespread use as an anxiolytic, while in the United States it has formal approval for panic disorder.
The present study identified a small but persistent decline in prescription rates of anxiolytic benzodiazepines over the 16 years studied. This may be attributable to a combination of better physician education and increasing availability of alternative drug treatments for anxiety disorders, such as SSRIs, SNRIs, pregabalin and buspirone, all of which have evidence of efficacy for generalized anxiety disorder in multiple randomized controlled trials, and in some cases evidence in other anxiety disorders, such as panic disorder, social anxiety disorder and post-traumatic stress disorder. A small number of double-blind randomized trials have reported efficacy of these drugs over placebo specifically in the elderly, including one using an SSRI 32 and one using pregabalin. 33 All of these drugs are recommended by recent guidelines originating in Canada, 3 the United Kingdom 2 and Germany 4 for generalized anxiety disorder prior to considering benzodiazepines. Similarly, in panic disorder, social anxiety disorder and post-traumatic stress disorder, SSRIs and the SNRI venlafaxine are given higher priority than benzodiazepines.2–4
Hypnotics showed a more rapid decline. The introduction of z-drugs may partly explain the greater reduction in prescription of hypnotic benzodiazepines compared with anxiolytics. In both the Manitoba-based study where data were available specifically for those over 65 27 and the UK adult primary care data described by Lader, 28 marked declines in hypnotic benzodiazepine use were matched by an increase in z-drug prescription from the mid-1990s onwards. However, in Ontario zopiclone is the sole ‘z-drug’ for which funding for prescriptions is available, but this is limited to ‘exceptional circumstances’ requiring a written application for special consideration. Otherwise, individuals may be prescribed zopiclone, zolpidem or zaleplon only if they will pay the costs themselves, or else request a drug that is financially supported (e.g. a traditional benzodiazepine or trazodone) or an over-the-counter alternative (e.g. melatonin or an antihistaminergic agent). In the UK, zopiclone, zolpidem and zaleplon prescriptions are all supported by the government. Thus, although z-drug prescribing trends could not be examined in ODB data, restrictions in governmental support compared with alternative drug treatments suggests that in Ontario reductions in hypnotic benzodiazepines may not be entirely attributable to prescribers switching to z-drugs.
While declining benzodiazepine prescription rates may be explained by the increasing utilization of alternative drugs for anxiety disorders or insomnia, there remains the possibility that changes in drugs costs or service provision patterns might have contributed. However, the cost of ODB prescriptions to the user is very small and has remained static throughout the period studied – a reduction in real terms – and thus cost is unlikely to explain the trends described. Data from the Canadian Chronic Disease Surveillance System 34 suggest that in Ontario the proportion of the adult population receiving treatment for mood or anxiety disorders fell from just over 12% to just over 10% between 1996/1997 and 2009/2010, a relative reduction of 16%, so it is possible that with the elderly population increasing markedly over the period studied, reduced access to services may have contributed to the trends we have described.
The finding that benzodiazepine prescribing rates were greater in older age bands matches that reported from the Ontario data from the 1990s by Tu and colleagues. 19 Lader 28 described a consistent finding across several studies19,35–37 that observed that prescription rates are greater in older populations.
The increasing use of clonazepam bears examination as this is the only benzodiazepine drug that saw a progressive year-on-year increase not only in gross number of prescriptions but also, despite the increasing population of individuals aged ⩾65, in the proportion of individuals prescribed the drug. Indeed the latter was as much as a two-fold increase. It is conceivable that clonazepam has become increasingly attractive due to the publication in the last 25 years of several successful randomized trials for anxiety disorders and related conditions, in a period where societal concerns and regulatory changes 28 have reduced enthusiasm to undertake trials on the other existing benzodiazepines. Randomized trials of clonazepam conducted during this period report effectiveness in panic disorder as monotherapy38–40 and as an adjunct to sertraline, 41 efficacy as monotherapy in social anxiety disorder in monotherapy 42 and benefits on some outcomes as an adjunct to SSRI antidepressants in this disorder,43,44 and efficacy in depression with or without anxiety as an adjunct to fluoxetine.45,46 Whereas alprazolam, diazepam, lorazepam and oxazepam have longstanding United States FDA approvals for ‘Management of Anxiety’ or ‘Management of Anxiety Disorders’, the manufacturer of clonazepam, which was first marketed for other indications in 1975, did not secure FDA approval for its use in any anxiety disorder until the late 1990s, eventually receiving approval for panic disorder in 1998. Nevertheless, it appears that Ontario prescribers and their patients are increasingly selecting clonazepam while other more established anxiolytic benzodiazepines, such as diazepam and alprazolam, have declined markedly. Even the most prescribed agent, lorazepam, has seen a reduction both in crude number of prescriptions/year and proportion of individuals in the population prescribed the drug. Increasing use does not necessarily imply superior efficacy or tolerability, but does at least suggest that an increasing proportion of prescribers were willing to view clonazepam as a preferred benzodiazepine. In the absence of high-quality comparative studies it remains possible that the increasing enthusiasm for clonazepam over the remaining benzodiazepines has emerged for reasons unrelated to its actual clinical attributes, most obviously the tendency of prescribers to favour a drug where trial evidence has emerged more recently. A parallel situation involving a different benzodiazepine was described in the Australian dataset, 29 in which prescription rates of alprazolam were reported to have increased markedly while those for all other drugs remained steady or declined. Alprazolam’s increasing popularity in Australia may similarly be for a reason that is not fully related to its true clinical attributes, in that it is the only benzodiazepine with a Pharmaceutical Benefits Scheme authority indication for a specific anxiety disorder – that is ‘panic disorder where other treatments have failed or are inappropriate’. Comparative studies for benzodiazepines are few in number, but in 2016 a naturalistic study in patients already taking antidepressants for anxiety disorders 47 compared the efficacy and tolerability of clonazepam with lorazepam and alprazolam. Although efficacy was similar, mean doses (by dose equivalence conversion) and incidence of side effects were significantly lower in participants prescribed clonazepam. It must be noted, however, that this study lacks randomization and blinding, and was limited to 180 subjects, so it should be seen as offering only preliminary evidence in favour of clonazepam over other drugs in the class. On the other hand, another recent study, which employed Canadian data, 48 reported that clonazepam was associated more frequently with dose escalation than any other benzodiazepine, although the possibility of this finding being attributable to confounding by indication (i.e. clonazepam being preferred in patients with baseline characteristics which represent risk factors for escalation) cannot be excluded.
There was a clear reversal of the progressive increase in the ratio of short- to long-acting benzodiazepines which had been reported in the same database for the period 1993–1998. A peak in this ratio was reached in 2003, but the projections made by Tu and colleagues 19 of continued increases in this ratio were not sustained, with a subsequent decline by 2013 to a lower value than that observed in 1998. This change appears to have been driven by declining use of the dominant short-acting benzodiazepine, lorazepam, and by other previously commonly used short-acting drugs such as oxazepam and temazepam, and is accentuated by the rise in prominence of the longer-acting clonazepam. The reversal of the trend which had been observed by Tu and colleagues 19 reflects the change in the prevailing opinion described earlier, whereby short-acting drugs are no longer considered preferable to long-acting compounds in contemporary literature.
Given the concerns and controversies relating to widespread benzodiazepine use, governmental initiatives have attempted to reign in benzodiazepine prescribing. A restriction on government reimbursement for benzodiazepine prescriptions introduced in the Netherlands in 2009 resulted in an 8% reduction in new prescriptions of benzodiazepines to patients newly diagnosed with an anxiety disorder and a corresponding 12% reduction for those newly diagnosed with a sleep problem. 49 An earlier example was the decision by the State of New York to substantially increase the administrative requirements for doctors prescribing benzodiazepines. 50 In the year after this intervention, benzodiazepine prescriptions were reduced by 60% in the state’s Medicaid prescribing data, compared with a 4% reduction in the year before. Substantial reductions were also observed in two other large New York State prescription databases, including a 33% reduction in IMS America data for benzodiazepine prescribing in the state, while no reduction was observed in this time period in the comparison states of New Jersey, North Carolina and California. However, the study illustrates a pitfall with stricter interventions in that an unexpected increase occurred in prescription rate of barbiturates, a drug class sharing some properties with benzodiazepines, but considered to be much more dangerous due to having a high rate of fatality in overdose. The legal changes introduced in Ontario in November 201123,24 required physicians to record more information on prescriptions than previously, but differed from the New York intervention in that all controlled substances, not specifically benzodiazepines, were targeted and benzodiazepine prescribing was not made more arduous than, for example, prescribing a drug from the barbiturate class, none of which are routinely supported in the ODB program. In Ontario, barbiturates can only be obtained through ODB via the ‘exceptional access program’, which is much more time-consuming for prescribers than prescribing benzodiazepines even after the November 2011 changes. The impact of this legislation on potentially inappropriate controlled drug prescribing (defined by number of tablets prescribed, time to repeat prescription or prescription from three or more physicians or pharmacies within a specified period) in the general Ontario population has been examined through a time-series analysis. 51 Following the legislative change, potentially inappropriate benzodiazepine prescription was markedly reduced. In the present study, from November 2011 onwards there was a sustained downward shift representing an absolute reduction of 0.3% in the overall monthly prescription rate in the population, or a 4.8% reduction relative to the year prior to the legislative change. The elimination of a proportion of benzodiazepine prescriptions was in line with one of the stated aims of the Narcotics Safety and Awareness Act 24 of ‘improving health and safety of Ontarians’, but there remains the limitation that there were no data ascertained from a comparison jurisdiction, such as another Canadian province where the intervention did not occur. Although the before and after comparison illustrates that the reduction in rates observed was statistically significant, the relative and absolute reductions were small. It can be seen as a well-calibrated change which may have made some prescribers re-examine the need for benzodiazepines in a minority of elderly patients.
Strengths and limitations
The strengths of the study include the population-based dataset for residents of Ontario aged ⩾65, whose numbers had grown to 2.06 million by the end of the study period, and the longitudinal element in which the data examined were available (on both an annual and monthly basis) over 16 years, following on from a previous study that examined an earlier 6-year period. A further strength is the ability to capture reliably all dispensed government-funded benzodiazepine prescriptions (other than the small number of those provided in an inpatient setting) in a context in which funding is available for all of the commonly used compounds. The study has some general limitations. Data derived from the ODB database reflect drug prescriptions which were dispensed by a pharmacy, but we cannot be certain that medications were taken. This issue is especially pertinent for medication prescribed on a pro re nata (PRN) basis, with, for example, residents of long-term care facilities often having PRN medications delivered on a regular basis but subsequently returned if unused. However, long-term care residents accounted for only 8% of benzodiazepine users at the start of the study and the proportion declined only slightly to 7.1% by 2013, so it is unlikely that prescribed but unused benzodiazepines in long-term care settings had a material influence on the trends described. While the Ontario government supports all of the benzodiazepines described in this study, the non-benzodiazepine drug zopiclone, is financially supported only in a small number of cases in which ‘exceptional access’ was granted, while two other z-drugs – zolpidem and zaleplon – cannot be financed by the province. Therefore, as most z-drug prescriptions must be funded by the patient themselves or by other sources, it was not possible to assess z-drug prescribing using the ODB database.
There were two further important issues which could not be addressed in the present design, but require future study. These questions relate to how appropriate are the benzodiazepines prescribed to the 15% of the population aged ⩾65 identified in Ontario as receiving these drugs in the final year of the observation period, and the extent to which benzodiazepine prescribing is associated with adverse outcomes in the elderly population taking these drugs. In future studies we will attempt to address these questions and to differentiate short- and long-term benzodiazepine usage, noting the concerns that have been raised in relation to long-term benzodiazepine usage.
Conclusions
In a continuation of the trend observed by Tu and colleagues, 19 benzodiazepine prescription rates among Ontario residents aged ⩾65 years declined progressively from 1998 to 2013, with only clonazepam seeing increased prescribing rates during the period studied. Clinically, advantages of clonazepam over other commonly used benzodiazepines are not clear-cut, and we speculate that its rise may relate to its FDA approval for panic disorder in the neighbouring United States in 1998, mirroring the increasing use of alprazolam in Australia, which may again be due to the breadth of its approved indications in that jurisdiction rather than any true pharmacological advantage. The predicted increase in the ratio of prescription of short-acting to long-acting benzodiazepine drugs continued to 2003 only, after which there was a reversal in the trend that brought the ratio down to below the 1998 level. Changes in the legal framework relating to the regulations around benzodiazepine prescription in November 2011 coincided with a small but significant and sustained downward shift in the monthly prescribing rate. Other factors which may have contributed to the progressive decrease in prescribing rates include the possibility of prescribers switching to other drugs for anxiety disorders (e.g. SSRIs, SNRIs and pregabalin) and for insomnia (e.g. z-drugs) or preferring non-pharmacological approaches, and perhaps the possibility that access to prescribers was slightly reduced in the context of the greatly expanding population of individuals aged ⩾65 during the time period studied.
The ODB database and linked registers provide wide-ranging opportunities for further study, in particular the possibility to characterize outcomes relating to an individual’s pattern of benzodiazepine use over periods of many years. In future research we will examine the association of patterns of benzodiazepine usage (e.g. intermittent versus continuous use), accounting for dose, and outcomes from linked registers such as falls, fractures and mortality.
Footnotes
Funding
This study was supported in part by the Medical Psychiatry Alliance, a collaborative health partnership of the University of Toronto, the Centre for Addiction and Mental Health, the Hospital for Sick Children, Trillium Health Partners, the Ontario Ministry of Health and Long-Term Care (MOHLTC) and an anonymous donor. The Institute for Clinical Evaluative Sciences (ICES) is funded by the Ontario MOHLTC. The study results and conclusions are those of the authors, and should not be attributed to any of the funding agencies or sponsoring agencies. No endorsement by ICES or the Ontario MOHLTC is intended or should be inferred.
Conflict of interest statement
The authors declare that there is no conflict of interest.
