Abstract
Objectives:
Antipsychotic polypharmacy (APP) is common clinical practice. Theoretically, APP runs the risk of additional side effects, drug interactions, adherence and cost. A limited evidence base is emerging to support the effectiveness of APP in clinical practice. Our companion paper highlighted the extent of APP alongside commonly prescribed long-acting antipsychotic injections (LAIs). We aimed to examine the effects of APP on discontinuation rates and Clinical Global Impression (CGI) outcomes in patients commenced on risperidone long-acting injection (RLAI) and zuclopenthixol decanoate.
Method:
LAI-naïve patients commenced on RLAI (n = 102) and zuclopenthixol decanoate(n = 105) were identified using our electronic patient record (running from 2002) within NHS Lanarkshire, Scotland, UK. This was a retrospective, electronic case note review with an 18-month follow up. Patient groups were divided into those receiving the LAI as the sole antipsychotic and those who were receiving additional oral antipsychotic polypharmacy (APP) for at least 50% of the duration of the treatment with their LAI. Kaplan–Meier statistics were calculated for discontinuation rates. CGI severity and improvement scores were retrospectively assigned by the investigating team.
Results:
Antipsychotic polypharmacy occurred with RLAI (37%) and zuclopenthixol decanoate (46%) and was associated with lower discontinuation rates (statistical significant with zuclopenthixol for any cause and adverse effects discontinuation). APP had no adverse outcomes on hospital admissions or CGI ratings. Patients on APP did not have more severe, chronic or treatment resistant illnesses.
Conclusions:
For RLAI and zuclopenthixol decanoate, APP had some favourable outcomes when examining discontinuation rates for any cause, and adverse effects. This was unexpected as we had considered APP would signal illness chronicity and severity and be associated with increased adverse effects resulting in early discontinuation. APP had no adverse outcomes on assigned CGI improvement or mean end-point severity ratings for RLAI and zuclopenthixol decanoate.
Keywords
Introduction
The companion paper in this journal [Cordiner et al. 2015] described the effectiveness of three commonly prescribed long-acting antipsychotic injections (LAIs) within our health board organization. We noted in that study, and as seen elsewhere in various parts of the world [Correll and Gallego, 2012], rates of antipsychotic polypharmacy (APP) were significant, between 20% and 40%. Theory supports monotherapy over APP for primarily obvious concerns including the lack of a clear evidence base and potentially increased side effects; see Correll and Gallego for a comprehensive evaluation of this area [Correll and Gallego, 2012]. However, APP with LAIs is known to be common practice (up to 50%) in the UK [Barnes et al. 2009] and has been considered potentially useful from a pharmacological basis [Patel et al. 2009]. There is emerging evidence for the superior effectiveness of APP over monotherapy in specific clinical situations, for example clozapine augmented with another antipsychotic and coprescription of aripiprazole to reduce metabolic side effects [Fleischhacker and Uchida, 2014]. Once APP is established it is difficult to revert to monotherapy, despite some evidence that this can be successful in up to 50% of cases [Langan and Shajahan, 2009; Correll and Gallego, 2012]. Our companion paper showed some differences in clinical effectiveness between paliperidone palmitate, risperidone long-acting injection (RLAI) and zuclopenthixol decanoate (zuclopenthixol) [Cordiner et al. 2015]. We aimed to discern the effects of APP on clinical effectiveness measured by discontinuation rates [Goff et al. 2005; Kahn et al. 2008; McEvoy et al. 2014] and Clinical Global Impression (CGI) [Guy, 1976] outcomes for the larger two groups of patients. That is, LAI-naïve patients commenced on RLAI (n = 102) and zuclopenthixol decanoate (n = 105). Our hypothesis was that compared with LAI monotherapy those receiving additional oral APP would (1) have more severe, chronic and treatment refractory illnesses, (2) discontinue earlier due to inefficacy or adverse effects and demonstrate earlier hospitalization and (3) perform less favourably on CGI outcomes.
Methods
The methodology of this study is largely described in detail in the companion paper. For the specific purposes of APP analysis, RLAI and zuclopenthixol decanoate were chosen due to the greater number of LAI-naïve patients commenced on these two LAIs since the commencement of our electronic patient record. Those records that contained insufficient information to allow analysis were excluded, RLAI (n = 3), zuclopenthixol decanoate (n = 15), χ2 = 7.1, degrees of freedom (d.f.) = 1, p < 0.01.
Demographic and clinical variables were obtained from the electronic patient records and can be seen in Table 1. Coprescription with adjunctive oral antipsychotics was recorded if it was a regular (not an ‘as required’ or ‘prn’ prescription) and was present for greater than 50% of the time the patient was on the LAI of interest. Among our study population, no patients received clozapine to augment their LAI. Our proxy marker of chronicity of illness was duration of contact with psychiatric services and treatment refractoriness was measured by a record of clozapine being trialled before the prescription of the LAI of interest.
Clinical and demographic details of patients commenced on long-acting injections.

χ2 = 16.7, d.f. = 3, p < 0.001.
F(3,203) = 6.6, p < 0.001.
χ2 = 10.3, d.f. = 6, p = 0.11.
χ2 = 7.6, d.f. = 3, p = 0.054.
χ2 = 6.1, d.f. = 3, p = 0.11 (psychotic versus nonpsychotic disorders).
χ2 = 4.4, d.f. = 3, p = 0.23.
χ2 = 13.1, d.f. = 3, p = 0.005.
χ2 = 9.4, d.f. = 3, p = 0.02.
χ2 = 6.4, d.f. = 3, p = 0.09.
χ2 = 5.0, d.f. = 3, p = 0.17.
χ2 = 7.2, d.f. = 3, p = 0.06 (second-generation versus all other groupings).
χ2 = 5.0, d.f. = 6, p = 0.53.
t = 1.0, d.f. = 84, p = 0.34.
χ2 = 3.8, d.f. = 2, p = 0.15.
For RLAI alcoholic hallucinosis (n = 2), avoidant personality disorder (n = 1). For zuclopenthixol decanoate schizotypal disorder (n = 1).
BNF, British National Formulary; CI, confidence interval; d.f., degree of freedom; LAI, long-acting injection; RLAI, risperidone long-acting injection.
Discontinuation and hospitalization rates were calculated using Kaplan–Meier statistics. Time to hospitalization was chosen as a further proxy marker of effectiveness for analysis in that if there were differences, the more effective strategy, either LAI or LAI with APP, should prolong the time before admission to psychiatric hospital [Kishimoto et al. 2013; McEvoy et al. 2014].
The patient records had CGI severity scores assigned at the outset of treatment with the LAI and after 18 months or the date of discontinuation, whichever came sooner. The CGI scores were assigned retrospectively, according to information within the clinical records. All CGI scoring was assigned by four of the authors, all clinical psychiatrists (MC, PS, SM and MB) working within NHS Lanarkshire. Individual patient records were assigned randomly to the investigators, to reduce possible inter-rater discrepancy. Throughout data collection, there were regular discussions and joint assessments to reduce this further.
Raters involved clinically and directly in patients records were asked to give the CGI assignment to author MC who repeated all CGI measures independently of the other three assessors. We aggregated CGI improvement scores into three categories, (A) = (1) very much improved and (2) much improved, (B) = (3) minimally improved and (4) no change, and finally category (C) = (5) minimally worse, (6) much worse and (7) very much worse. The reason for this being that all LAIs are powerful, long-term psychotropic medications with significant adverse effects and some are potentially costly compared with others. As clinicians, we should strive for the best gains (an ‘A’ rating) in terms of CGI improvement, that is, CGI-I (1) and (2) from interventions such as LAIs and cautiously review all other ‘improvement’ categories, particularly if harm is being done. It was felt that a CGI improvement of category (B) = (3) minimally improved and (4) no change, were of low clinical utility as they reflected patients exposed to medications they had little control over, risk of adverse effects and the possibility of no significant clinical gain.
Analysis
The results were tabulated using Microsoft Excel 2007, which was used for the majority of statistical analysis. Histograms were created to assess the distribution of numerical data. Continuous data was reported as means with 95% confidence intervals (CIs) and compared using analysis of variance and two-tailed t tests as appropriate. Categorical data was analysed by way of χ2 tests, with significance levels requiring p < 0.05. Kaplan–Meier survival curves were computed using MedCalc (http://www.medcalc.org) statistical software for Microsoft Windows, to calculate percentages, censored data and to demonstrate time to discontinuation or, hospitalisation. Overall differences within the two groups (LAI versus LAI plus additional antipsychotic) were assessed for significance using the log-rank test [Bland and Altman, 2004]. Differences between LAIs were presented as hazard ratios (HRs) with 95% CIs.
Results
From our electronic document management system we identified all patient records in secondary psychiatric health services in NHS Lanarkshire showing patients commenced on RLAI (n = 102) and zuclopenthixol decanoate (n = 105) and who were previously LAI naïve. As reported in the companion paper [Cordiner et al. 2015], APP was more common with zuclopenthixol decanoate at 46% compared with RLAI at 37%. This was not statistically significant χ2 = 2.7, d.f. = 1, p = 0.1.
Table 1 shows demographic and clinical features for the four different patient cohorts. There was a statistically significant increased proportion of female patients commenced on zuclopenthixol decanoate (42–49%) compared with RLAI (64–82%), χ2 = 16.7, d.f. = 3, p < 0.001. Within the RLAI group, more males were on antipsychotic polypharmacy, although this was not statistically significant, χ2 = 3.5, d.f. = 1, p = 0.06. Within the zuclopenthixol decanoate groups there were no gender differences, χ2 = 0.5, d.f. = 1, p = 0.47. Patients commenced on zuclopenthixol decanoate tended to be around 7 years older, F(3,203) = 6.6, p < 0.001. There were no significant differences in length of contact with psychiatric services, χ2 = 10.3, d.f. = 6, p = 0.11. Patients treated with zuclopenthixol decanoate who required APP were less likely to be treated using compulsory (legislative) measures, although this just failed to reach statistical significance, χ2 = 3.7, d.f. = 1, p = 0.053. A higher proportion of patients with bipolar affective disorder received treatment with zuclopenthixol decanoate as the sole antipsychotic. For RLAI and zuclopenthixol decanoate, APP was associated with increased coprescription with mood stabilizers χ2 = 13.1, d.f. = 3, p = 0.005. For both LAIs, APP was not associated with different levels of alcohol or substance misuse. However, compared with RLAI, patients prescribed zuclopenthixol decanoate had significantly (almost 50% less) recorded comorbid alcohol misuse at 24–25%, χ2 = 9.1, d.f. = 2, p = 0.01, and drug misuse around 20–24%, χ2 = 8.2, d.f. = 2, p = 0.01. Few patients had previously been prescribed clozapine and this did not differ between groups, χ2=5.0, d.f. = 3, p=0.17. Immediately prior to commencing the LAIs, the majority of patients had been on second-generation oral antipsychotic medications. There was suggestion that patients treated with zuclopenthixol decanoate plus APP were more likely to been on first-generation oral antipsychotic and combination medications beforehand (χ2 = 7.2, d.f. = 3, p = 0.06).
High rates of nonconcordance as the reason for commencing a LAI were seen for RLAI plus APP (55%) and zuclopenthixol decanoate plus APP (36%). For the RLAI group with APP, chlorpromazine was the only first-generation antipsychotic used, n = 13 (100%). The second-generation antipsychotics used were oral risperidone, n = 8 (36%), quetiapine, n = 8 (36%), amisulpride, n = 2 (9%), aripiprazole, n = 2 (9%), olanzapine, n = 2 (9%), and unknown for n = 1. For the zuclopenthixol decanoate group with APP, the additional first-generation antipsychotics used were chlorpromazine, n = 16 (69%), oral zuclopenthixol, n = 5 (22%), thioridazine, n = 1 (4%) and trifluoperazine, n = 1 (4%). The second-generation antipsychotics used were oral risperidone, n = 8 (36%), quetiapine, n = 8 (36%), amisulpride, n = 2 (9%), aripiprazole, n = 2 (9%) and olanzapine, n = 2 (9%). The daily dose of LAIs did not differ within the RLAI (t = 0.2, d.f. = 100, p = 0.81), or zuclopenthixol groups (t = 1.5, d.f. = 103, p = 0.15). The additional mean daily dosages of APP (expressed as a percentage of the maximum allowed by the British National Formulary [BNF] and logarithmically transformed) were not significantly different, 23% extra for RLAI and 27% extra for zuclopenthixol decanoate (t = 1.0, d.f. = 84, p = 0.34). Where APP was observed, the mean combined dosages (expressed as a percentage of the BNF maximum) for RLAI plus APP were higher than for zuclopenthixol decanoate with APP (93% versus 55%).
Figure 1 demonstrates Kaplan–Meier survival curves calculated for discontinuation due to any cause, inefficacy, side effects and rates of hospitalization for RLAI. The statistics for this are shown in Table 2. The log rank chi-squared test result is given to show overall differences within the groups and Cox model treatment comparisons using HRs with 95% CIs are given to show the differences between the LAI on their own and with APP using the lone LAI as the comparator. No significant differences were seen for RLAI versus RLAI plus APP although the graphs suggested possible lower discontinuation rates for RLAI plus APP. Figure 2 demonstrates Kaplan–Meier survival curves calculated for discontinuation due to any cause, inefficacy, side effects and rates of hospitalization for zuclopenthixol decanoate. The statistics for this are also shown in Table 2. Significant differences were seen for RLAI versus RLAI plus APP with reduced likelihood of any cause discontinuation (HR = 0.4 [95% CI 0.2–0.6], p = 0.01) and discontinuation due to side effects (HR = 0.2 [95% CI 0.1–0.6], p = 0.005).

Kaplan–Meier graphs for discontinuation events: effects of additional antipsychotic on risperidone.
Kaplan–Meier tests for LAI discontinuation: effects of antipsychotic polypharmacy.
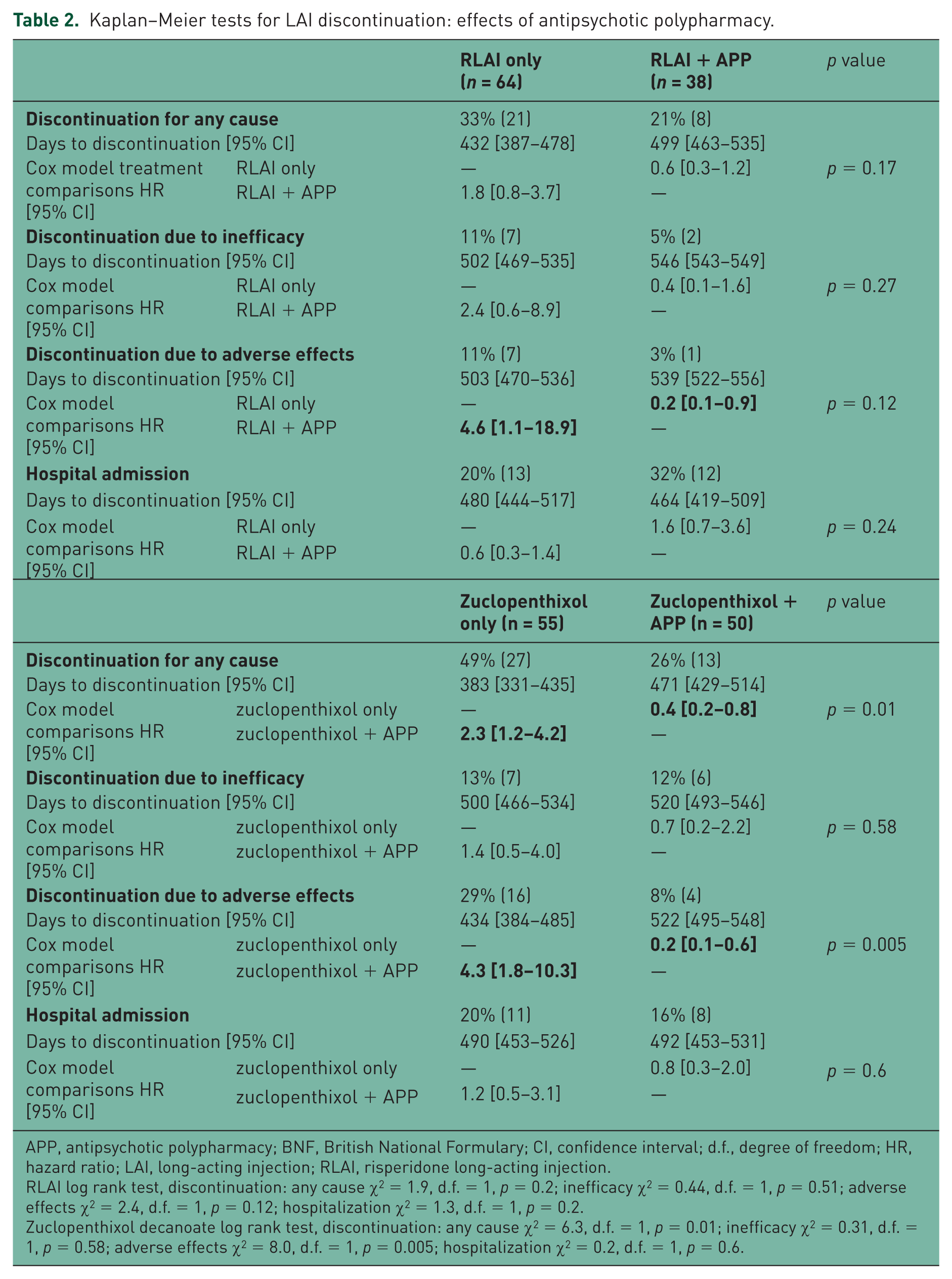
APP, antipsychotic polypharmacy; BNF, British National Formulary; CI, confidence interval; d.f., degree of freedom; HR, hazard ratio; LAI, long-acting injection; RLAI, risperidone long-acting injection.
RLAI log rank test, discontinuation: any cause χ2 = 1.9, d.f. = 1, p = 0.2; inefficacy χ2 = 0.44, d.f. = 1, p = 0.51; adverse effects χ2 = 2.4, d.f. = 1, p = 0.12; hospitalization χ2 = 1.3, d.f. = 1, p = 0.2.
Zuclopenthixol decanoate log rank test, discontinuation: any cause χ2 = 6.3, d.f. = 1, p = 0.01; inefficacy χ2 = 0.31, d.f. = 1, p = 0.58; adverse effects χ2 = 8.0, d.f. = 1, p = 0.005; hospitalization χ2 = 0.2, d.f. = 1, p = 0.6.

Kaplan–Meier graphs for discontinuation events: effects of additional antipsychotic on zuclopenthixol.
Table 3 depicts CGI scores for illness severity and consequent improvement with treatment. The mean CGI at start of treatment was similar for all four LAI groups (F(3,203) = 1.6, p = 0.2) between 4 and 5 suggesting that patients were moderately to severely unwell. The mean end-point CGI severity was similar for all four LAI groups (F(3,203) = 0.3, p = 0.8). The mean CGI improvement scores did not differ significantly (F(2,203) = 1.9, p = 0.14). However, following stratification of CGI improvement into aggregated groups, (A = 1 + 2), (B = 3 + 4) and (C = 5, 6 + 7), RLAI was associated with a higher proportion of patients being assigned CGI improvement category C (5, minimally worse, or 6, much worse; no patients were assigned to be 7, very much worse), χ2 = 30.8, d.f. = 6, p < 0.001. There were no differences in the A, B and C score categories within the RLAI groups, χ2 = 0.22, d.f. = 2, p = 0.9 or the zuclopenthixol decanoate groups, χ2 = 4.9, d.f. = 2, p = 0.08.
CGI severity and improvement outcomes: LAI monotherapy versus antipsychotic polypharmacy.

F(3,203) = 1.6, p = 0.2, bF(3,203) = 0.3, p = 0.8, cF(3,203) = 1.9, p = 0.14, dχ2 = 30.8, d.f. = 6, p < 0.0001.
APP, antipsychotic polypharmacy; CGI, Clinical Global Impression; CI, confidence interval; d.f., degree of freedom; RLAI, risperidone long-acting injection.
Discussion
LAI treatment with RLAI and zuclopenthixol decanoate when combined with additional oral antipsychotic polypharmacy was not given to more severely ill or treatment refractory patients. There was suggestion that patients with APP may have been in contact with services for longer. Discontinuation rates were generally less in the APP groups reaching statistical significance for zuclopenthixol decanoate for any cause discontinuation and discontinuation due to adverse effects. Hospitalization rates and CGI improvement outcomes did not differ significantly with APP.
Our first hypothesis was that those receiving an LAI who required APP would have more severe, chronic and treatment refractory illnesses. Severity of illness was rated using the CGI (severity scale) which showed no differences across the four patient cohorts. The mean CGI (S) score at 4.5 suggested moderate-to-severe illness at the start of treatment. Chronicity of illness was measured by duration of contact within our NHS psychiatric services. This suggested that at least three quarters of all patients commenced on an LAI had been in contact with services for 3 or more years. A slightly higher percentage was seen for both RLAI with APP and zuclopenthixol with APP where this proportion approached 9 out of 10. Treatment refractoriness was assessed by recording those trialled on clozapine beforehand, as in the UK the licensed indication for clozapine is treatment resistant schizophrenia. The number of patients previously tried on clozapine was small and no statistically significant differences were seen between the four groups. From a clinical perspective, comorbid alcohol and substance misuse result in patients less likely to respond to treatment and could be considered markers of potential treatment resistance. There were differences in comorbid alcohol and substance misuse between RLAI and zuclopenthixol but no differences due to APP. Treatment failure may also arise from non-concordance with antipsychotic medications. It was surprising to see that although the main indication for starting a LAI was nonconcordance with oral medication, there was still a sizeable proportion prescribed oral APP. A total of 55% of patients prescribed RLAI with APP had been commenced on the LAI for problems with medication nonconcordance. A mechanism for understanding this may be that patients become well enough with the LAI component of their treatment to understand the potential benefits of not only additional antipsychotics, but also other psychotropic medications, including antidepressants and mood stabilisers, the latter prescribed at a significantly higher rate in the APP groups (p = 0.005).
The second hypothesis was that patients with APP would discontinue earlier due to inefficacy or adverse effects and demonstrate earlier hospitalization. This hypothesis was not supported. There was evidence that compared with zuclopenthixol as the sole antipsychotic, patients on zuclopenthixol with APP were less likely to experience any cause discontinuation (HR = 0.4 [95% CI 0.2–0.6], p = 0.01) and discontinuation due to adverse effects (HR = 0.2 [95% CI 0.1–0.6], p = 0.005). This was surprising as clinically more adverse effects are likely with any degree of polypharmacy. Our results were, however, consistent with those from a large meta-analysis of oral antipsychotics showing lower discontinuation rates for patients prescribed more than one antipsychotic [Correll et al. 2009]. The mechanism by which antipsychotic polypharmacy may improve outcome for staying on an LAI is unclear. Potential reasons include beneficial multiple neurotransmitter effects, which occur when more than one antipsychotic is prescribed. This may, for example, be useful sedative properties, including promotion of sleep and reduction of anxiety and agitation, particularly seen with agents such as chlorpromazine which was commonly used. It was surprising that discontinuation due to adverse effects was also reduced with APP, again raising questions about the mechanism by which antipsychotics actually help in schizophrenia and related disorders. Perhaps a broader scope of drug action is associated with a more favourable outcome on these particular discontinuation measures, particularly relevant to the heterogeneity of schizophrenia and related disorders. As mentioned, the most popular choice for augmenting RLAI and zuclopenthixol was chlorpromazine which, although sedative, may exacerbate potential extrapyramidal side effects of both RLAI and zuclopenthixol. However, we considered that the potential increase in such side effects and thereby lowered tolerability was mitigated by the broad spectrum of effects from such antipsychotic combinations allowing for more effective and continuous treatment. Interestingly, the oral forms of the LAIs were popular choices as APP, 36% of all second-generation antipsychotics for oral risperidone with RLAI and 22% of all first-generation antipsychotics for oral zuclopenthixol with zuclopenthixol decanoate.
Such findings highlight the mechanism of the origin of APP which includes incomplete cross-titration schedules in keeping with colleagues suggesting that some APP may be idiosyncratic or unfounded [Correll and Gallego, 2012]. APP was not associated with excessive or earlier hospitalization. This was of interest as we had considered the potential for adverse effects, drug interactions and nonconcordance would be higher with APP. However, these potential adverse factors did not translate to treatment failure resulting in poorer discontinuation outcomes and increased or earlier hospital admission.
Our third hypothesis was that compared with monotherapy, APP would be associated with less-favourable outcomes on CGI measures. Mean CGI severity scores at the start of treatment were similar, indicating moderate (score = 4) to severe (score = 5) illness across the four patient groups. There was no suggestion that APP was associated with less favourable outcomes on either mean end-point CGI Severity ratings, mean CGI improvement scores or CGI categorized scores according to our methods section (Table 3). These CGI findings are consistent with the position that APP did not result in a less-favourable clinical outcome. Interestingly, unlike the discontinuation data it does not support the position that patients on APP do better than those on monotherapy. Although we considered potential mechanisms by which APP may be associated with reduced discontinuation, this did not translate to differences noted by practising clinicians on relatively simple and robust illness severity and improvement markers, that is, CGI scores.
We considered whether the dosing of the LAI was implicated in the potential reason for APP. From the companion paper we can identify that, compared with RLAI, zuclopenthixol decanoate was used at a significantly lower dose (in terms of maximum allowed BNF dose), 74% versus 29%. When examining those patients who were on APP, the doses of the LAI of interest did not differ significantly, i.e. APP was not associated with inadequate dosing of the original LAI. There were interesting differences between the dosing strategies for RLAI and zuclopenthixol. The two LAIs had quite different mean daily dosages prescribed, when transformed to maximum allowed by BNF. When augmented with APP, similar mean dosages were used for augmentation for both LAIs: 23% for RLAI, 27% for zuclopenthixol decanoate. For those on RLAI with APP, this elevated the total mean antipsychotic dose to 93%, towards implications for high dose monitoring. This was less likely with zuclopenthixol where mean combined dosages were at 55%.
Limitations
These are broadly the same as in our companion paper which employed a similar methodology. We reiterate that due to the retrospective nature of this study, there is reliance on quality documentation of clinical findings. In most cases, it was possible to make a reasoned judgement about patient details and illness severity. In some, there was a dearth of information and these patients were excluded (as outlined in the methods section). There is also a risk that descriptions about illness severity were not conveyed accurately in the records available. However, this is unlikely to be unique to one particular LAI or subgroup and thus should not bias findings. However, this may influence the magnitude of effect detected. We also make the assumption that patients were compliant with any APP prescribed: it is possible that those prescribed an LAI for reasons of noncompliance remained noncompliant for their additional oral antipsychotic. In addition, it is possible that patients may under-report side effects for reasons such as embarrassment (as with sexual side effects) or through a willingness to tolerate side effects for improved symptom control. Again, this is unlikely to unduly influence results in one direction.
Our marker for illness chronicity was duration of contact with our secondary psychiatric care services, thus creating a potential error if patients were migrating to and from different areas. Our population in NHS Lanarkshire is, however, considered stable, with less net migration than, for example, larger cities across the UK. The population studied was almost exclusively White Scottish, with a mean age of 35 to 44 and most having had contact with our services for over 3 years. Therefore findings may not be generalizable to areas where there are more mixed populations, or to patients in their first episode of psychosis. In the UK, the cost of medications is not directly paid by the patient or their relatives. Where cost is more of a direct issue for the likelihood of treatment, findings related to relatively inexpensive medications such as zuclopenthixol decanoate are arguably as important as those showing the effectiveness of new compounds. This is not to understate the potential clinical effectiveness of all currently available LAIs in the UK and we welcome the addition of new products to help clinicians optimise the health patients suffering from psychosis.
Footnotes
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Conflict of interest statement
All the authors are employed by the NHS. MT has received hospitality and fees from Janssen; Lundbeck; Otsuka; and Roche in the last 3 years.
