Abstract
Cognitive Behavioural Therapy (CBT) for preadolescent children with obsessive compulsive disorder (OCD) is typically derived from adult cognitive behavioural models of OCD; however, it is unknown whether these adult models apply to preadolescent children. This systematic review examined whether 11 cognitive, behavioural and familial maintenance mechanisms identified from adult cognitive behavioural models of OCD and descriptions of how family factors may maintain OCD applied to preadolescent children with obsessive compulsive symptoms/disorder (OCS/OCD; Prospero:CRD42019153371). PsycINFO, MEDLINE and Web of Science Core Collection were searched in March 2019, with forward citation handsearching conducted in March/April 2020. Twenty-nine studies were synthesised. Studies were identified for only six of the 11 proposed maintenance factors. Of the cognitive and behavioural factors, only inflated responsibility and meta-cognitive beliefs showed evidence of independent and/or specific associations with childhood OCS. Of the family factors, only less frequent displays of parental confidence, positive problem solving and rewarding of children’s independence showed some evidence of specificity to childhood OCD. Notably, findings across studies were inconsistent and existing studies have considerable methodological limitations. Experimental and prospective longitudinal studies are needed to determine whether the proposed factors maintain childhood OCS/OCD, to improve the effectiveness and efficiency of CBT for preadolescent children with OCD.
Introduction
Obsessive compulsive disorder (OCD) is a highly debilitating mental health disorder characterised by the presence of obsessions (intrusive, unwanted thoughts, images or urges which cause significant distress or anxiety) and/or compulsions (repetitive behaviours or mental acts an individual feels compelled to perform to reduce distress or anxiety, or to prevent a feared outcome; American Psychiatric Association, 2013). OCD often has its onset between the ages of 7.5 and 12.5 years old (Geller et al., 1998) and is estimated to affect between 1% and 4% of the paediatric population (Flament et al., 1988; Heyman et al., 2001). Childhood OCD is also commonly comorbid with other mental health disorders (Heyman et al., 2001; Pediatric OCD Treatment Study (POTS) Team, 2004) and often continues into adulthood if appropriate treatment is not provided (Pinto et al., 2006).
Cognitive Behavioural Therapy (CBT) including Exposure and Response Prevention (ERP) is the recommended psychological treatment for childhood OCD (National Institute of Health and Care Excellence - NICE, 2005), and has been shown to be superior to pharmacological treatment (Ivarsson et al., 2015) and active psychological control conditions (Freeman et al., 2014). Despite this, up to 60% of children and adolescents do not experience clinical remission of obsessive compulsive symptoms (OCS) following CBT (Barrett et al., 2008; Pediatric OCD Treatment Study (POTS) Team, 2004). To date, treatment studies have often failed to distinguish between preadolescent and adolescent populations (e.g. Franklin et al., 2011; Piacentini et al., 2011; Williams et al., 2010) despite key differences among these populations (i.e. cognitive maturation, clinical presentation and family factors) which may influence the maintenance of the disorder. To improve the effectiveness of CBT for preadolescent children with OCD specifically, an understanding of the psychological processes which maintain the disorder in preadolescence is required.
There are a number of reasons to anticipate that the processes that maintain OCD in preadolescents may differ to those that occur in adolescence or adulthood. First, Farrell and Barrett (2006) suggested that the cognitive processes hypothesised to maintain OCD may be particularly important during adolescent and adult years – bringing a lack of clarity about the processes which maintain the disorder in preadolescence. For example, Farrell and Barrett (2006) found that adolescents and adults with OCD reported significantly higher responsibility beliefs, probability of harm beliefs, and engaged in more thought suppression than preadolescent children with OCD. However, ratings of thought-action fusion (TAF), doubt, severity of harm and cognitive control were comparable across preadolescents, adolescents and adults with OCD. Second, the clinical presentation of OCD differs with age. For example, Nakatani et al. (2011) found that children with early onset OCD (defined as <10 years old) reported significantly more repeating and ordering compulsions compared to children with late onset OCD (defined as 10 to 18 years old). Furthermore, Geller et al. (2001) found that preadolescent children (<12 years) with OCD reported significantly fewer aggressive and sexual obsessions than adults with OCD and were less likely to report multiple obsessions and compulsions than adults with OCD. Moreover, preadolescent children with OCD reported significantly fewer religious and sexual obsessions than adolescents (≥12 years) with OCD and had poorer ‘insight’. Similarly, Mancebo et al. (2008) found that preadolescent children (6–12 years) with OCD reported significantly fewer aggressive obsessions than adolescents (13–18 years) and adults with OCD, and significantly fewer mental rituals than adolescents with OCD. However, in this study, no significant age differences were found on reports of sexual or religious obsessions. Third, preadolescent children are immersed in the family in a distinct manner to adolescents and adults (Freeman et al., 2003). Children are heavily reliant on the family and spend considerable time in the family environment (Freeman et al., 2003). Thus, researchers have emphasised the importance of understanding the role of the family in the maintenance of OCD among preadolescent children specifically (Freeman et al., 2003; Smorti, 2012; Waters & Barrett, 2000).
To date, treatment for childhood OCD has typically involved CBT with ERP as the core treatment component – in line with the existing evidence base (NICE, 2005). However, there is evidence to suggest that the psychological processes implicated in cognitive models of adult OCD also apply to children and adolescents (Reynolds & Reeves, 2008), suggesting that cognitive approaches to CBT treatment for young people with OCD may add further value. The most widely cited cognitive behavioural model of adult OCD was proposed by Salkovskis (1985) which proposes that the central difference between individuals with and without OCD is the interpretation assigned to the incidence and/or content of normal intrusive cognitions. Individuals with OCD interpret intrusive cognitions as indicating that they may be responsible for harm and/or the prevention of harm to themselves and/or others (Salkovskis et al., 1996). This interpretation results in a plethora of effects, including (i) mood changes, such as increased distress, anxiety and low mood; (ii) attentional biases, whereby individuals place greater attention on intrusive cognitions and related stimuli; (iii) increased accessibility of intrusive cognitions and (iv) maladaptive cognitive and behavioural strategies, such as compulsive checking and/or washing, reassurance seeking, avoidance and thought suppression (Salkovskis, 1999). These effects are proposed to maintain the individual’s negative interpretation of the intrusive cognitions, prevent belief disconfirmation and increase the likelihood of future intrusive cognitions (Salkovskis, 1999).
Other cognitive models of adult OCD share the central feature that an individual’s interpretation of an intrusive cognition is crucial to the development and maintenance of OCD (Reynolds & Reeves, 2008). For example, Rachman (1993) proposed the construct of TAF, a cognitive process where individuals interpret thoughts and actions as equivalent. TAF consists of two elements; (i) likelihood TAF – the belief that experiencing an unwanted, intrusive cognition increases the probability of an adverse event occurring to oneself and/or others and (ii) morality TAF – the belief that experiencing an unwanted, intrusive cognition is morally equivalent to performing the action (Shafran & Rachman, 2004). A related construct, which has also been proposed to contribute to the maintenance of OCD (Bolton et al., 2002), is ‘magical thinking’, the belief that one’s thoughts or actions can affect causally unrelated events (Zusne & Jones, 1989). Furthermore, Wells and Matthews’ (1994) meta-cognitive model of adult OCD emphasises the role of beliefs about thinking in the maintenance of OCD. Specifically, this model highlights the potential maintaining role of (i) beliefs regarding the meaning and consequences of experiencing an intrusive cognition, and (ii) beliefs regarding the need to perform compulsions and the negative effects of not doing so (Fisher & Wells, 2008). To consolidate research examining cognitive models of OCD, the Obsessive Compulsive Cognitions Working Group (1997) identified six belief domains considered to be critical to the development and maintenance of adult OCD. These include (i) inflated responsibility – the belief that one has capability to cause or prevent negative outcomes; (ii) over importance of thoughts – the belief that the appearance of a thought means that the thought is important; (iii) importance of controlling thoughts – the belief that it is possible and desirable to have complete control over one’s thoughts; (iv) overestimation of threat – beliefs about the likelihood or severity of negative events; (v) intolerance of uncertainty – beliefs about the need to be certain, and one’s inability to cope in uncertain situations and (vi) perfectionism – beliefs about the necessity of perfectionism and the consequences of mistakes (Obsessive Compulsive Cognitions Working Group, 1997).
To date, there has been limited research to examine the applicability of adult cognitive behavioural models of OCD to childhood OCD, and studies have typically examined preadolescents and adolescents together. For example, Reynolds and Reeves (2008) conducted a systematic review examining the relevance of adult cognitive models of OCD to children and adolescents more broadly (aged < 18 years old), with a particular focus on inflated responsibility, TAF and meta-cognitive beliefs. Of 122 studies identified, only 11 met inclusion criteria. Ten studies provided preliminary support for the applicability of adult cognitive models of OCD among children and adolescents; however, many studies used cross-sectional designs and non-clinical samples. Only one study (with young people aged 7–17 years) used an experimental design, and as such was the only study able to examine directionality among a clinical sample, and failed to support the applicability of a causal role of responsibility beliefs on OCD-related constructs (e.g. avoidance and ritualising) in children and adolescents. Mantz and Abbott (2017) have since conducted a (non-systematic) literature review of research examining the Obsessive Compulsive Cognitions Working Group’s (1997) six key OCD belief domains which included (combined) child and adolescent populations. The authors highlighted that there is inconclusive evidence regarding the relationship between cognitive appraisals and the maintenance of OCD among children and adolescents. In addition to an absence of consideration of the specific evidence for preadolescent children, reviews to date have failed to examine other maintenance mechanisms identified in adult models of OCD such as attentional biases and maladaptive coping strategies. Furthermore, the role of the family in the maintenance of childhood OCD has been largely overlooked.
Despite the need to understand the role of family factors in the maintenance of OCD among preadolescent children specifically (Freeman et al., 2003), to our knowledge, there is no maintenance model which outlines the role of the family in the maintenance of childhood OCD. However, some family factors have been proposed to be relevant to the maintenance of childhood OCD and anxiety more broadly, including family members’ cognitions (Freeman et al., 2003) and behaviours (Smorti, 2012; Waters & Barrett, 2000). Family members’ cognitions (e.g. interpretations of anxious stimuli) may be relevant to the maintenance of childhood OCD (Freeman et al., 2003) through direct or indirect effects on family members’ behaviours (e.g. by reinforcing threatening interpretations of anxious stimuli or promoting avoidance behaviours; Barrett et al., 1996; Creswell et al., 2010). Moreover, family members’ behaviours, in particular, family accommodation (e.g. assistance/participation in rituals and/or modification of routines to minimise child distress; Waters & Barrett, 2000) are thought to maintain childhood OCD through inadvertently reinforcing children’s OCS and behaviours through attempts to provide symptom relief to the child (Waters & Barrett, 2000). Thus, the role of the family in the maintenance of OCD among preadolescent children warrants further attention.
Objectives
Hypotheses derived from adult cognitive behavioural models of OCD and descriptions of how family factors may maintain childhood OCD.

Note. Due to the conceptual overlap between neutralising actions and counterproductive safety strategies, for clarity, we have classified neutralising actions as restorative behaviours (i.e. behaviours which an individual performs to reduce harm that has been caused, such as washing compulsions) and have classified counterproductive safety strategies as verification behaviours (i.e. behaviours performed when an individual fears they may cause harm in the future, such as checking compulsions, Cougle et al., 2007).
Method
A systematic review was conducted in accordance with PRISMA guidelines (Moher et al., 2009) and was pre-registered with PROSPERO (ID: CRD42019153371, accessible from https://www.crd.york.ac.uk/PROSPERO/display_record.php?RecordID=153371).
Search strategy
Three electronic databases, PsycINFO, MEDLINE and Web of Science Core Collection, were searched from 1985 to March 25, 2019, with backward and forward citation hand searching conducted in March/April 2020 for all studies included in the review, to identify further papers of interest not identified from the electronic search. The former date was chosen to reflect the introduction of the adult cognitive behavioural model of OCD (Salkovskis, 1985). The following search strategy was implemented: (Obsessi* or compulsi* or OCD) AND (Child* or p?ediatric or juvenile or young or youth or school) AND (Cogniti* or belief* or thought* or threat or responsibility or perfect* or magic* thinking or uncertain* or safety behavio* or neutrali* or avoid* or coping or reassur* or ritual* or suppress* or emotion* or attention* or attend or family or parent or carer or guardian or accommodation or antagonising). No other restrictions were applied to the search strategy.
Eligibility criteria
The inclusion and exclusion criteria were piloted and refined by two review authors (CCh and BH) using a sub-sample of papers. Studies were deemed eligible for inclusion if they met the following criteria: The paper was available in English, in a peer-reviewed journal. The paper reported on humans. The paper reported novel findings. Papers reporting reviews, meta-analyses, biographies, clinical guidelines, commentaries or summaries of previously reported research were not included in this review. The paper reported on preadolescent children aged between 5 and 12 years old (inclusive). Due to the scarcity of research in the preadolescent population, studies including participants with an upper age limit of 14 years were included, if the average age of the sample was less than 13 years. Papers reporting on other age ranges (e.g. 7–17 years) were included, if sub-group analyses of preadolescent children (aged 5–14 years, with a mean <13 years) could be extracted. Where studies examined children and adolescents as one group, we contacted authors to request re-conducted analyses for participants who met our core age criteria (i.e. participants aged 5–12 years old). Authors were only contacted to re-conduct analyses when papers satisfied all other eligibility criteria and presented no extractable data for participants in our specified age range. The paper included a standardised measure of OCS/OCD. Papers were required to include a standardised measure of OCS/OCD. Diagnostic interviews were required to be structured or semi-structured and conducted with the child, parent or both. Questionnaire measures were required to show evidence of adequate psychometric properties and to have been designed specifically for children. Studies using a questionnaire subscale to measure OCS/OCD were included, if the above criteria were satisfied. The paper included a measure of one or more potential maintenance factors. This review focused on potential cognitive, behavioural and familial maintenance factors (i.e. children’s and/or family member’s specific cognitions and/or behaviours). Papers with questionnaire, observation or equivalent measures of potential maintenance factors were included. The paper was required to meet at least one of the following study designs: Study examining (i) associations between potential maintenance factors and continuous measures of OCS/OCD and (ii) independent or specific associations between potential maintenance factors and continuous measures of OCS/OCD, compared with other anxiety symptoms/disorders and/or non-anxious controls. Study examining (i) differences in potential maintenance factors and categorical measures of OCS/OCD and (ii) differences in potential maintenance factors and categorical measures of OCS/OCD, compared with other anxiety symptoms/disorders and/or non-anxious controls. Prospective or experimental study examining the direction of effects between potential maintenance factors and OCS/OCD, including experimental studies using treatment designs. Study examining change in a potential maintenance mechanism and change in OCS/OCD.
Papers were excluded if the study was a single case report, or if the study specifically examined OCS/OCD in the context of other comorbid conditions (e.g. autism spectrum disorders (ASDs), attention deficit hyperactivity disorder (ADHD), eating disorders or physical health conditions).
Study selection
A flow chart of the study selection process is shown in Figure 1. Electronic database searches retrieved 14,987 records. Backward and forward citation hand searching retrieved a further 255 potentially eligible papers. A total of 10,835 records were retained after duplicates were removed. The titles and abstracts of a subset of records (n = 200) retrieved from the electronic database searches were independently screened by two review authors (CCh and BH) to identify records for full text screening. Inter-rater reliability between the two review authors was calculated and classified as ‘almost perfect agreement’ (k = .86; Landis & Koch, 1977). The titles and abstracts of the remaining records were screened by one review author (CCh). Two review authors (CCh and BH) then independently screened 1627 full texts to determine eligibility for inclusion in the review. Ninety-nine records were identified which examined children and adolescents as one group (i.e. they presented no extractable data for participants in our specified age range). As these records met all other eligibility criteria, we emailed the authors of 96 records (n = 3 were not contactable) to request re-conducted analyses on participants within our age range. Seven authors responded with the requested analyses or provided data for re-analysis. Any disagreements among reviewers were initially discussed by the two review authors (CCh and BH) and if consensus was not reached, a third review author (CCr) was consulted to reach a final decision. PRISMA flowchart of study selection process.
Data extraction
A data extraction sheet was developed and refined through initial piloting. The data extraction sheet included: details of the publication (e.g. authors, title and year of publication); participant characteristics (e.g. number of participants, age range, gender, diagnostic information and comorbidity); study design (e.g. questionnaire, observation, prospective, experiment and intervention); standardised measure of OCS/OCD (e.g. questionnaire, interview, informant, evidence of construct validity and appropriateness for age of child); measure of potential maintenance factors (e.g. questionnaire, observation and informant); control/comparison group (if applicable); method of data analysis; sub-group analyses (if applicable, e.g., age); study results (including effect sizes); and information relevant to the quality assessment. Data extraction was independently conducted by two review authors (CCh and CGH) and reviewed to ensure accuracy. Any discrepancies were initially discussed by the two review authors (CCh and CGH), and if consensus was not reached, a third review author (CCr or BH) was consulted to reach a final decision. Authors were contacted for missing data where necessary.
Quality ratings
The quality of included studies was assessed using a modified version of the Checklist for Assessing the Quality of Quantitative Studies (Kmet et al., 2004). We modified the wording of the criterion ‘Outcome and exposure measures well defined and robust to misclassification bias?’ and measured this for both OCS/OCD measures (‘OCS/OCD measure(s) well defined and robust to misclassification bias?’) and proposed maintenance factor measures (‘Proposed maintenance factor measure(s) well defined and robust to misclassification bias?’). Two review authors (CCh and CGH) independently rated the quality of all included studies. Studies were only rated on the criteria which were applicable to the specific study design; thus, the possible total score for each study varied, so percentage scores were calculated to show the total score as a proportion of the potential total for each study. Studies where analyses were re-conducted to fit our specified age criteria were rated twice; once for the overall quality of the paper and once for the re-conducted analyses. This approach was chosen to reflect that re-conducted analyses may differ in quality (i.e. sample size, control for confounding variables and estimates of variance) from the original paper. Any discrepancies were initially discussed by the two review authors (CCh and CGH) and a third review author (CCr or BH) was consulted if consensus was not reached.
Data synthesis
Due to considerable heterogeneity among the studies included in this review, we adopted a descriptive approach to data synthesis. Studies are organised according to (i) specific hypotheses identified from adult cognitive behavioural models of OCD, and descriptions of how family factors may maintain childhood OCD; (ii) sample characteristics (e.g. non-clinical and clinical populations); and (iii) methodological approach, to indicate the extent to which findings aid our understanding of whether the proposed maintenance factors are independently and/or specifically associated with childhood OCS/OCD. Thus, we presented studies examining the association between childhood OCS/OCD and proposed maintenance factors (i.e. studies examining differences between children with OCD and non-clinical controls on proposed maintenance factors, or associations between childhood OCS/OCD and proposed maintenance factors). If the study provided evidence of a significant association between childhood OCS/OCD and the proposed maintenance factor, we then presented study findings (where applicable) on the independent association between childhood OCS/OCD and the proposed maintenance factor (i.e. associations between childhood OCS/OCD and the proposed maintenance factor whilst controlling for other psychiatric symptoms) and/or the specific association between childhood OCS/OCD and the proposed maintenance factor (i.e. differences between children with OCD and psychiatric controls on the proposed maintenance factor or lack of associations between other psychiatric symptoms and the proposed maintenance factor). If the study provided no evidence for a significant association between childhood OCS/OCD and the proposed maintenance factor, then no analyses regarding independent or specific associations from that study were presented. A summary of the strength of the existing evidence for each proposed maintenance factor is shown in Figure 2. Summary of the strength of the available evidence. Note. Studies are represented once for each investigated maintenance factor, for the highest degree of evidence shown. Red = The study has found no evidence to support the hypothesised association between childhood OCS/OCD and the proposed maintenance factor; Orange = The study has found some evidence to support the hypothesised association between childhood OCS/OCD and the proposed maintenance factor; Green = The study has found some evidence to support the hypothesised independent and/or specific association between childhood OCS/OCD and the proposed maintenance factor.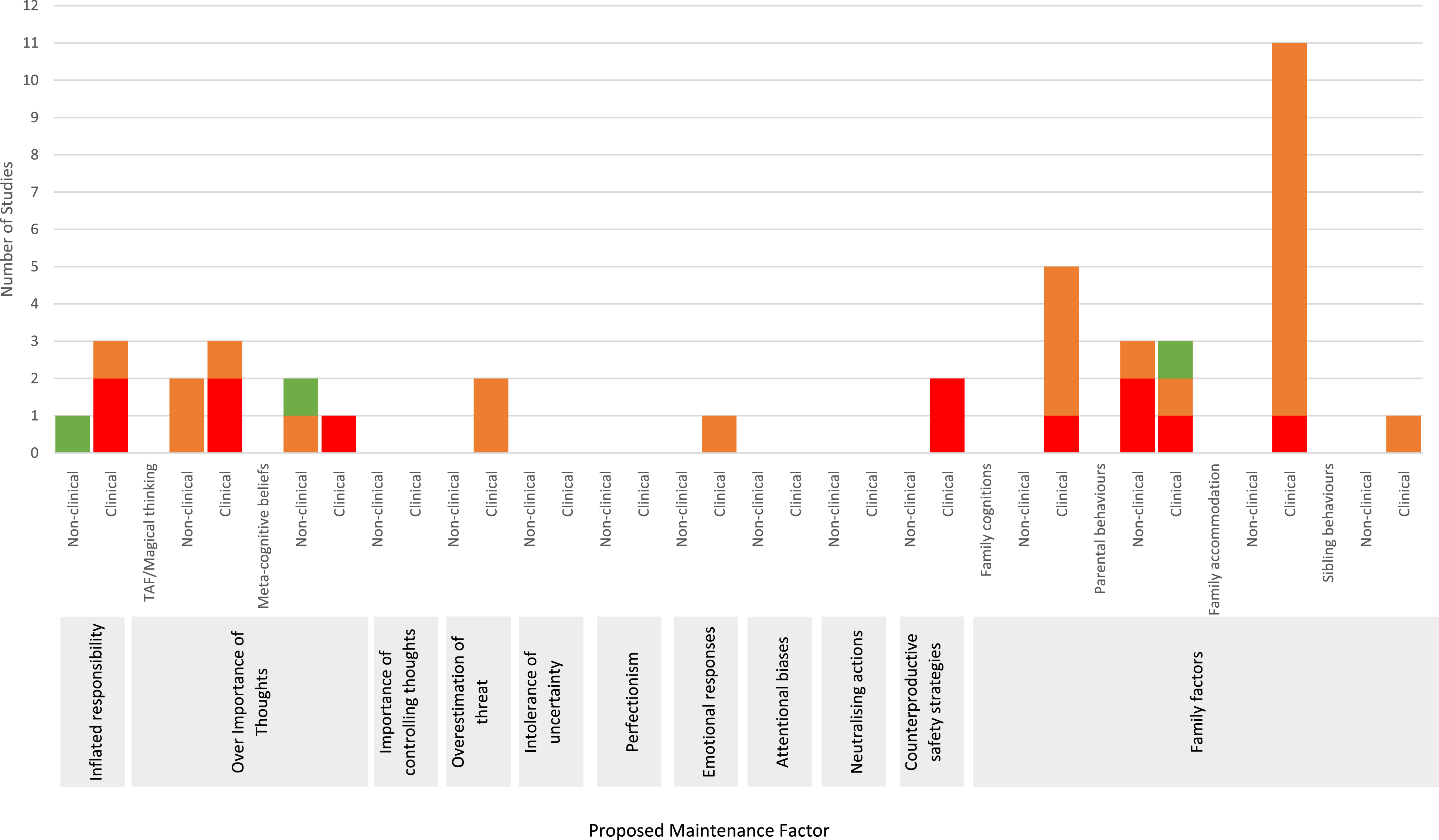
The results of this review are evaluated based on significance testing and effect sizes. In recognition that many studies used small sample sizes and/or were insufficiently powered to detect potentially meaningful effects, effect sizes (Cohen’s d) were calculated to aid interpretation of the results in the discussion section. Cohen’s d is reported for all studies where this could be extracted, calculated or converted (using https://www.psychometrica.de/effect_size.html). Where effect sizes were not reported, Cohen’s d was calculated using means and standard deviations. If this data was not available, effect sizes were calculated using F values or t-statistics. Where there was insufficient information to calculate effect sizes, authors were contacted to provide the required data. However, the required data was not always available to calculate effect sizes; in these circumstances, we interpreted the results based on significance testing only. For consistency, the effect sizes reported in this paper were calculated by the review authors unless indicated. Any discrepancies between review authors’ calculations and the original papers are indicated. Effect sizes were coded as positive or negative to aid interpretation of the data. For correlational studies, a positive effect size indicates that increases in childhood OCS/OCD are associated with increases in the proposed maintenance factor. For studies examining between-group differences, a positive effect size indicates that children with OCD have a higher score on the proposed maintenance factor than the control group. For treatment studies examining the statistical association between change in childhood OCS/OCD and change in proposed maintenance factors, a positive effect size shows the measures changed in the same direction (e.g. reductions in both childhood OCS/OCD and the maintenance factor). Where treatment studies did not directly examine this association, but just reported change in childhood OCS/OCD and proposed maintenance factors over time, a positive effect size indicates increases in childhood OCS/OCD or the proposed maintenance factor across time. Effect sizes were interpreted using Cohen’s (1988) conventions of small (d = 0.20), medium (d = 0.50) and large (d = 0.80). Where there was insufficient information to determine the direction of the effect, this is indicated.
Results
Description of included studies
Study characteristics.
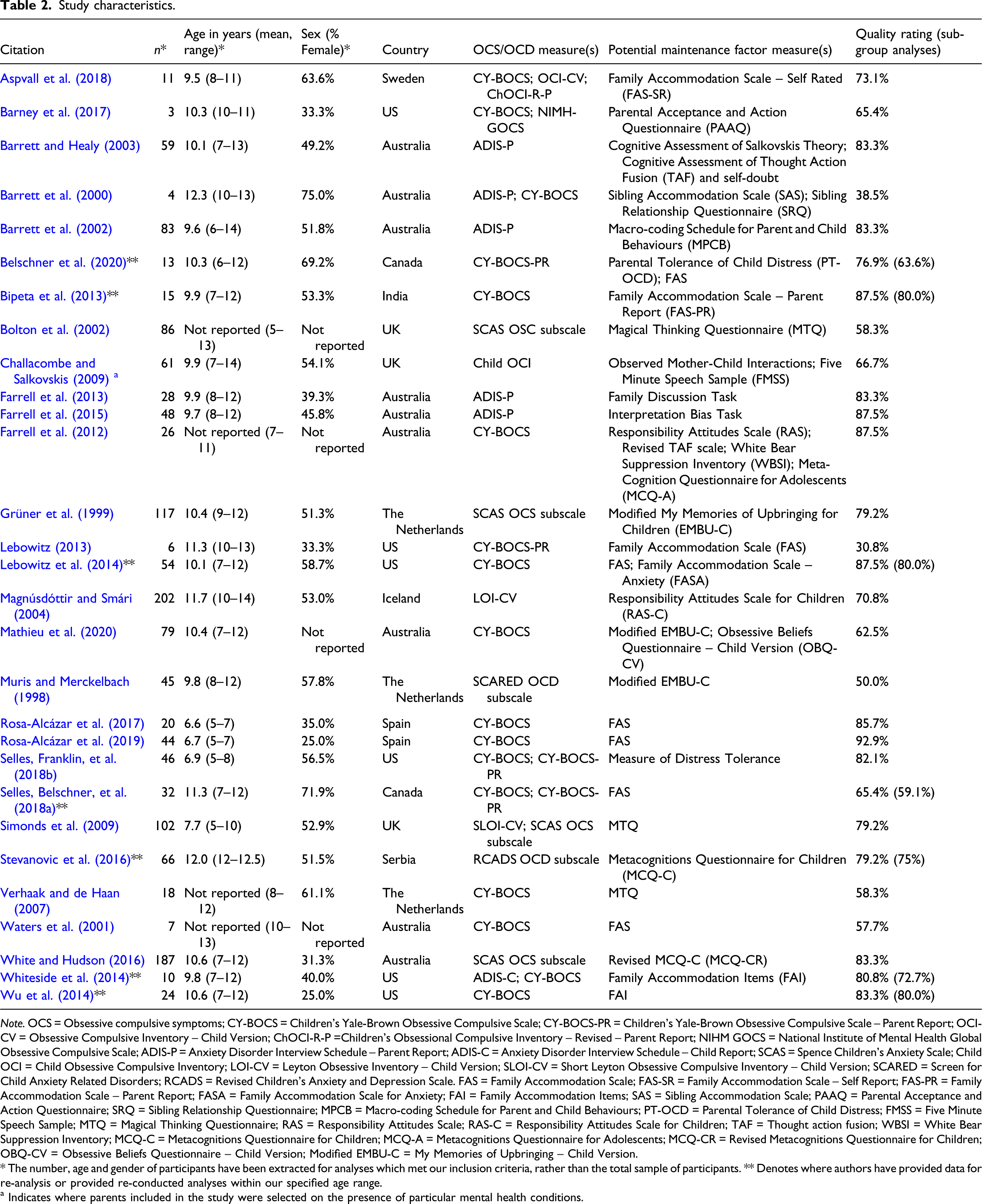
Note. OCS = Obsessive compulsive symptoms; CY-BOCS = Children’s Yale-Brown Obsessive Compulsive Scale; CY-BOCS-PR = Children’s Yale-Brown Obsessive Compulsive Scale – Parent Report; OCI-CV = Obsessive Compulsive Inventory – Child Version; ChOCI-R-P =Children’s Obsessional Compulsive Inventory – Revised – Parent Report; NIHM GOCS = National Institute of Mental Health Global Obsessive Compulsive Scale; ADIS-P = Anxiety Disorder Interview Schedule – Parent Report; ADIS-C = Anxiety Disorder Interview Schedule – Child Report; SCAS = Spence Children’s Anxiety Scale; Child OCI = Child Obsessive Compulsive Inventory; LOI-CV = Leyton Obsessive Inventory – Child Version; SLOI-CV = Short Leyton Obsessive Compulsive Inventory – Child Version; SCARED = Screen for Child Anxiety Related Disorders; RCADS = Revised Children’s Anxiety and Depression Scale. FAS = Family Accommodation Scale; FAS-SR = Family Accommodation Scale – Self Report; FAS-PR = Family Accommodation Scale – Parent Report; FASA = Family Accommodation Scale for Anxiety; FAI = Family Accommodation Items; SAS = Sibling Accommodation Scale; PAAQ = Parental Acceptance and Action Questionnaire; SRQ = Sibling Relationship Questionnaire; MPCB = Macro-coding Schedule for Parent and Child Behaviours; PT-OCD = Parental Tolerance of Child Distress; FMSS = Five Minute Speech Sample; MTQ = Magical Thinking Questionnaire; RAS = Responsibility Attitudes Scale; RAS-C = Responsibility Attitudes Scale for Children; TAF = Thought action fusion; WBSI = White Bear Suppression Inventory; MCQ-C = Metacognitions Questionnaire for Children; MCQ-A = Metacognitions Questionnaire for Adolescents; MCQ-CR = Revised Metacognitions Questionnaire for Children; OBQ-CV = Obsessive Beliefs Questionnaire – Child Version; Modified EMBU-C = My Memories of Upbringing – Child Version.
* The number, age and gender of participants have been extracted for analyses which met our inclusion criteria, rather than the total sample of participants. ** Denotes where authors have provided data for re-analysis or provided re-conducted analyses within our specified age range.
a Indicates where parents included in the study were selected on the presence of particular mental health conditions.
Results and effect sizes.
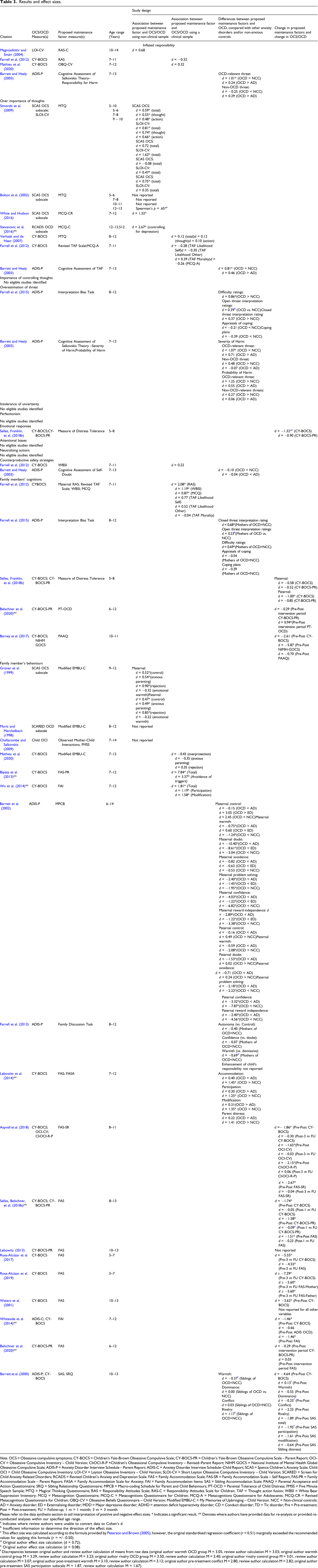
Note. OCS = Obsessive compulsive symptoms; CY-BOCS = Children’s Yale-Brown Obsessive Compulsive Scale; CY-BOCS-PR = Children’s Yale-Brown Obsessive Compulsive Scale – Parent Report; OCI-CV = Obsessive Compulsive Inventory – Child Version; ChOCI-R-P =Children’s Obsessional Compulsive Inventory – Revised–Parent Report; NIHM GOCS = National Institute of Mental Health Global Obsessive-Compulsive Scale; ADIS-P = Anxiety Disorder Interview Schedule – Parent Report; ADIS-C = Anxiety Disorder Interview Schedule–Child Report; SCAS = Spence Children’s Anxiety Scale; Child OCI = Child Obsessive Compulsive Inventory; LOI-CV = Leyton Obsessive Inventory – Child Version; SLOI-CV = Short Leyton Obsessive Compulsive Inventory – Child Version; SCARED = Screen for Child Anxiety Related Disorders; RCADS = Revised Children’s Anxiety and Depression Scale. FAS = Family Accommodation Scale; FAS-SR = Family Accommodation Scale – Self Report; FAS-PR = Family Accommodation Scale – Parent Report; FASA = Family Accommodation Scale for Anxiety; FAI = Family Accommodation Items; SAS = Sibling Accommodation Scale; PAAQ = Parental Acceptance and Action Questionnaire; SRQ = Sibling Relationship Questionnaire; MPCB = Macro-coding Schedule for Parent and Child Behaviours; PT-OCD = Parental Tolerance of Child Distress; FMSS = Five Minute Speech Sample; MTQ = Magical Thinking Questionnaire; RAS = Responsibility Attitudes Scale; RAS-C = Responsibility Attitudes Scale for Children; TAF = Thought action fusion; WBSI = White Bear Suppression Inventory; MCQ = Metacognition Questionnaire; MCQ-C = Metacognitions Questionnaire for Children; MCQ-A = Metacognitions Questionnaire for Adolescents; MCQ-CR = Revised Metacognitions Questionnaire for Children; OBQ-CV = Obsessive Beliefs Questionnaire – Child Version; Modified EMBU-C = My Memories of Upbringing – Child Version. NCC = Non-clinical controls; AD = Anxiety disorder; ED = Externalising disorder; MDD = Major depressive disorder; ADHD = attention deficit hyperactivity disorder; CD = Conduct disorder; TD = Tic disorder; Pre = Pre-treatment; Post = Post-treatment; FU = Follow-up; 1 m = 1 month; 3 m = 3 month.
Please refer to the data synthesis section to aid interpretation of positive and negative effect sizes. * Indicates a significant result. ** Denotes where authors have provided data for re-analysis or provided re-conducted analyses within our specified age range.
a Indicates where review authors were unable to convert data to Cohen’s d.
b Insufficient information to determine the direction of the effect size.
c This effect size was calculated according to the formula provided by Peterson and Brown (2005); however, the original standardised regression coefficient (r = 0.51) marginally exceeded the recommended values for applying this formula (r = +/−0.50).
d Original author effect size calculation (d = 0.72).
e Original author effect size calculation (d = 0.08).
f Discrepancies between original author and review author calculation of means from raw data (original author warmth OCD group M = 3.05, review author calculation M = 3.03; original author warmth control group M = 3.29, review author calculation M = 3.23; original author rivalry OCD group M = 3.50, review author calculation M = 3.40; original author rivalry control group M = 3.01, review author calculation M = 3.07; original author post-treatment warmth M = 3.10, review author calculation M = 3.12; original author pre-treatment conflict M = 2.80, review author calculation M = 2.82; original author pre-treatment SAS participation subscale M = 1.87, review author calculation M = 1.67).
Eligible studies were identified for six of the 11 proposed maintenance factors. Among the cognitive and behavioural mechanisms, studies most commonly examined inflated responsibility beliefs (n = 4) and over importance of thoughts (n = 7). Studies were also identified for overestimation of threat (n = 2), emotional responses (n = 1) and counterproductive safety strategies (n = 2). No eligible studies were identified which examined the association between childhood OCS/OCD and the remaining cognitive/behavioural mechanisms, that is, importance of controlling thoughts, intolerance of uncertainty, perfectionism, attentional biases or neutralising actions. Among the familial mechanisms, studies most commonly examined family members’ behaviours (n = 18) – including 12 different parental behaviours, family accommodation and sibling behaviours. Five studies examined family members’ cognitions. The strength of the available evidence for each proposed maintenance factor is summarised in Figure 2.
Quality ratings
As shown in Table 2, the quality of included studies varied considerably (from 30.8% to 92.9%). Studies often scored highly for sufficiently described research questions, study design, participant characteristics and appropriate conclusions. Lower scores were typically allocated for participant recruitment (recruitment strategies were often unclear/could introduce bias); sample size (studies often failed to provide power analyses); data analysis (studies provided little evidence statistical assumptions were met) and estimates of variance (confidence intervals and/or standard errors for results were infrequently reported).
1. Inflated responsibility
Four studies (three with clinical samples) used cross-sectional designs to examine the association between inflated responsibility and childhood OCS/OCD.
Non-clinical populations
Magnúsdóttir and Smári (2004) provided evidence of a significant positive association between childhood OCS and inflated responsibility in a non-clinical sample (N = 202, 10–14 years, d = 0.68). Regarding specificity, although a significant association between children’s depression symptoms and inflated responsibility was found (d = 0.63), there was a significant independent association between childhood OCS and inflated responsibility after controlling for children’s depression symptoms (d = 0.45).
Clinical populations
There is some, albeit limited, evidence that inflated responsibility is significantly associated with childhood OCS/OCD in clinical samples but no evidence that inflated responsibility is independently associated with, or specific to, children with OCD. While there was not a significant association between OCD severity and responsibility beliefs in general within groups of children with OCD (N = 26, 7–11 years, d = −0.32, Farrell et al., 2012; N = 79, 7–12 years d = 0.32, Mathieu et al., 2020), Barrett and Healy (2003) found that children with OCD (N = 28, 7–13 years) reported significantly higher responsibility ratings for OCD-relevant (but not non-OCD-relevant) threats compared to non-clinical controls (N = 14, d = 1.01 and d = −0.25, respectively). However, regarding specificity, Barrett and Healy (2003) found no evidence that children with OCD (N = 28) reported significantly higher responsibility ratings for OCD-relevant threats compared to children with anxiety disorders (N = 17, d = 0.24).
2. Over importance of thoughts
Five studies (three with clinical samples) employed cross-sectional designs to examine the association between over importance of thoughts and childhood OCS/OCD. Specifically, three studies examined ‘magical thinking’ and two studies examined TAF. Additionally, three studies (one with a clinical sample) were identified which examined the association between meta-cognitive beliefs and childhood OCS/OCD. Although meta-cognitive beliefs are not fully encompassed by the construct of over importance of thoughts, the meta-cognitive model of adult OCD emphasises beliefs about the meaning and importance of intrusions in the maintenance of OCD (Wells & Matthews, 1994); thus, these studies are also presented here.
Non-clinical populations
Magical thinking and thought-action fusion
There is evidence that ‘magical thinking’ is significantly associated with childhood OCS in non-clinical populations; however, the size of the associations differs depending on child age and the OCS measure used. Furthermore, there is no evidence that this association is independent or specific to childhood OCS. For example, Simonds et al. (2009) found that increased ‘magical thinking’ beliefs were significantly associated with increased OCS on two measures of OCS (N = 102, 5–10 years, SLOI-CV and MTQ total d = 0.81, MTQ thought subscale d = 0.74, MTQ action subscale d = 0.66; SCAS OCS subscale and MTQ total d = 0.59, MTQ thought subscale d = 0.55, MTQ action subscale d = 0.48). However, when analyses were conducted for three specific age groups (i.e. 5–6 years, 7–8 years and 9–10 years), the magnitude of the effect varied considerably dependent on the measure of OCS used (d’s ranged from d = −0.08 to d = 1.62, see Table 3 for further details), with significant positive associations found between ‘magical thinking’ and SLOI-CV scores for 5–6 year olds (d = 1.62), and ‘magical thinking’ and SCAS OCS subscale scores for 9–10 year olds (d = 0.75). Consistent with these findings, Bolton et al. (2002) also only found significant positive associations between ‘magical thinking’ and OCS for older children (i.e. 10–11 years and 12–13 years, Spearman’s p = .65 1 ) and not for younger children (i.e. <10 years old) when using the SCAS OCS subscale. Regarding independence, ‘magical thinking’ has not been found to significantly predict higher scores on two measures of OCS after controlling for other anxiety symptoms (male participants only, SLOI-CV d = 0.56; SCAS OCS subscale d = 0.49, Simonds et al., 2009). Similarly, ‘magical thinking’ does not appear to be specific to childhood OCS as significant associations between ‘magical thinking’ and other anxiety symptoms have been found for 12–13 year olds (Bolton et al., 2002) and 5–10 year olds (d’s ranged from d = 0.50 to d = 0.68, Simonds et al., 2009).
Meta-cognitive beliefs
Meta-cognitive beliefs
There is evidence that meta-cognitive beliefs are significantly and independently associated with childhood OCS in non-clinical populations. However, evidence of specificity in this relationship is mixed. White and Hudson (2016) found that increased meta-cognitive beliefs were significantly associated with increased OCS (N = 187, 7–12 years, d = 1.32). Extending this, Stevanovic et al. (2016) provided evidence of independence in this relationship, as increased meta-cognitive beliefs were significantly associated with increased OCS, after controlling for children’s depression symptoms (N = 66, 12 years old, d = 2.67). Regarding specificity, although children’s depression symptoms were not significantly associated with children’s meta-cognitive beliefs (after controlling for anxiety symptoms, d = −0.18), significant associations have been found between meta-cognitive beliefs and all RCADS anxiety subscales (after controlling for depression symptoms, d’s ranged from d = 0.75 to d = 2.14, Stevanovic et al., 2016) and all SCAS subscales (d’s ranged from d = 0.68 to d = 1.28, White & Hudson, 2016).
Clinical populations
Magical thinking and thought-action fusion
There is limited evidence of an association between ‘magical thinking’ or TAF and childhood OCS/OCD in clinical populations, and there is currently no evidence that ‘magical thinking’ or TAF is independently associated with, or specific to, children with OCD. While there was not a significant association between OCD severity and ‘magical thinking’ or TAF within groups of children with OCD (N = 18, 8–12 years, MTQ Total d = 0.12, MTQ Thought d = 0.12, MTQ Action d = 0.10, Verhaak & de Haan, 2007; N = 26, 7–11 years, TAF Likelihood Self d = −0.28, TAF Likelihood Other d = −0.30, TAF Morality d = 0.39, Farrell et al., 2012), Barrett and Healy (2003) found that children with OCD reported significantly higher levels of TAF than non-clinical controls (d = 0.81). However, concerning specificity, no significant differences between children with OCD and anxiety disorders on ratings of TAF have been shown (d = 0.46; Barrett & Healy, 2003).
Meta-cognitive beliefs
Meta-cognitive beliefs
There is no evidence that meta-cognitive beliefs are significantly associated with childhood OCS/OCD in clinical samples. For example, Farrell et al. (2012) did not find a significant association between increased meta-cognitive beliefs and increased OCD severity within a sample of children with OCD (7–11 years, d = −0.26).
3. Importance of controlling thoughts
No studies were identified which met our eligibility criteria and examined the association between importance of controlling thoughts and childhood OCS/OCD in non-clinical or clinical samples.
4. Overestimation of threat
Two studies (with clinical samples) employed cross-sectional designs to examine the association between overestimation of threat and childhood OCS/OCD
Clinical populations
There is mixed evidence regarding the association between overestimation of threat and childhood OCS/OCD in clinical samples, and no evidence of an independent or specific association to children with OCD. Farrell et al. (2015) found that children with OCD (N = 22, 8–12 years) interpreted ambiguous scenarios (including mildly-positive, neutral and mildly-aversive scenarios) as significantly more difficult than non-clinical controls (N = 26, d = 0.86). However, no significant between-group differences were found for children’s open or closed threat interpretations (d = 0.39 2 and d = 0.37, respectively) appraisals of coping (d = −0.21) or coping plans (d = −0.39) for ambiguous scenarios. Further, Barrett and Healy (2003) found that children with OCD (7–13 years) reported significantly higher severity of harm ratings for OCD-relevant threats compared to non-clinical controls (d = 1.07), yet there were no significant between-group differences for children’s ratings of the probability of harm for OCD-relevant threats (d = 1.25). As expected, there were no significant differences for children’s ratings of the probability or severity of harm for non-OCD-relevant threats (d = 0.27 and d = 0.48, respectively). Regarding specificity, children with OCD did not report significantly higher severity of harm ratings for OCD-relevant threats compared to children with anxiety disorders (d = 0.71, Barrett & Healy, 2003). Similarly, regarding independence, no significant differences were found between children with OCD and non-clinical controls’ difficulty ratings for ambiguous scenarios when controlling for children’s comorbid anxiety symptoms (d = 0.17, Farrell et al., 2015).
5. Intolerance of uncertainty
No studies were identified which met our eligibility criteria and examined the association between intolerance of uncertainty and childhood OCS/OCD in non-clinical or clinical populations.
6. Perfectionism
No studies were identified which met our eligibility criteria and examined the association between perfectionism and childhood OCS/OCD in non-clinical or clinical populations.
7. Emotional responses
One study (with a clinical sample) examined the association between emotional responses and childhood OCS/OCD.
Clinical populations
Selles, Franklin, et al. (2018b) provided evidence of a significant association between improvements in children’s (N = 46, 5–8 years) distress tolerance throughout treatment and reductions on clinician (but not parent) reported OCD severity at post-treatment (d = −1.32 and d = −0.90, respectively). No research has examined whether this association is independent or specific to children with OCD.
8. Attentional biases
No studies were identified which met our eligibility criteria and examined the association between attention to intrusive, unwanted cognitions or related stimuli and childhood OCS/OCD in non-clinical or clinical populations.
9. Neutralising actions
No studies were identified which examined the association between neutralising actions and childhood OCS/OCD in non-clinical or clinical populations.
10. Counterproductive safety strategies
Two studies (with clinical samples) employed cross-sectional designs to examine the association between counterproductive safety strategies and childhood OCS/OCD.
Clinical populations
There is no evidence that counterproductive safety strategies are significantly associated with childhood OCS/OCD in clinical samples. For example, Farrell et al. (2012) did not find a significant association between OCD severity and thought suppression within a group of children (7–11 years) with OCD (d = 0.22). Similarly, Barrett and Healy (2003) found no evidence that children with OCD (7–13 years) had significantly higher ratings for responses to self-doubt (i.e. by repeating rituals/checking) compared to non-clinical controls (d = −0.10).
11. Family factors
Family member’s cognitions
Five studies (with clinical samples) examined the association between family member’s cognitions and childhood OCS/OCD; two studies employed cross-sectional designs and three studies used treatment designs.
Clinical populations
There is mixed evidence regarding the association between family members’ cognitions and childhood OCS/OCD in clinical samples, and no research has examined whether these associations are independent or specific to children with OCD. For example, when examining the association between family members’ cognitions and OCD severity within a sample of children (N = 26, 7–11 years) with OCD, Farrell et al. (2012) found significant positive associations for maternal responsibility attitudes (d = 2.08), thought suppression (d = 1.19) and meta-cognitive beliefs (d = 0.87) but not for maternal TAF (TAF Likelihood Self d = 0.77; TAF Likelihood Other d = 0.52; TAF Morality d = −0.04). Furthermore, Farrell et al. (2015) found that mothers of children (8–12 years) with OCD perceived ambiguous scenarios (including mildly-positive, neutral and mildly-aversive scenarios) as significantly more threatening (on responses to closed, but not open questions, d = 0.68 and d = 0.23 2 , respectively) and more difficult (d = 0.69) than mothers of non-clinical controls. However, the between-group differences in mother’s appraisals of coping (d = −0.54) or coping plans (d = −0.29) for ambiguous scenarios were not significant.
Regarding the association between parents’ distress tolerance or acceptance of their child’s emotions and childhood OCS/OCD specifically, inconsistent findings have been found. For example, whilst Selles et al. (2018b) found that improvements in fathers’ tolerance of their child’s distress throughout treatment was significantly associated with reductions on clinician (but not parent) report of children’s (5–8 years) OCD severity at post-treatment (d = −1.00 and d = −0.85, respectively), no significant associations between improvements in mother’s distress tolerance and children’s post-treatment OCD severity were shown (CY-BOCS d = −0.58; CY-BOCS-PR d = −0.52). Similarly, although Belschner et al. (2020) did not directly examine the association between changes in parental distress tolerance and changes in children’s (N = 13, 6–12 years) OCS/OCD across treatment, analyses showed that despite parents’ tolerance of their child’s distress significantly increasing through a caregiver-focussed, mindfulness-based intervention (d = 0.94), children’s OCD severity did not significantly decrease across this period (d = −0.29). In contrast, Barney et al. (2017) found mean improvements in both parents’ acceptance of their child’s (N = 3, 10–11 years) emotions and children’s OCD severity following Acceptance and Commitment Therapy (ACT; CY-BOCS d = −2.61; NIMH-GOCS d = −5.87; PAAQ d = −0.70).
Family member’s behaviours
Eighteen studies (15 with clinical samples) examined the association between family member’s behaviours (including 12 different parental behaviours, family accommodation and sibling behaviours) and childhood OCS/OCD. Nine studies employed cross-sectional designs and nine studies used treatment designs to examine the association of interest.
Non-clinical populations
Parental behaviours
There is limited evidence of a significant association between parental behaviours and childhood OCS in non-clinical populations, and there is no evidence that particular parental behaviours are independently or specifically associated with childhood OCS. For example, Grüner et al. (1999) found significant positive associations between children’s (N = 117, 9–12 years) reports of maternal and paternal control, anxious parenting and rejection (but not emotional warmth) and children’s OCS, after controlling for children’s age and gender (maternal control d = 0.52; anxious parenting d = 0.54; rejection d = 0.90; emotional warmth d = −0.32; paternal control d = 0.47; anxious parenting d = 0.49; rejection d = 0.85; emotional warmth d = −0.22). In contrast, Muris and Merckelbach (1998) found no evidence that children’s (N = 45, 8–12 years) reports of maternal and paternal behaviours (i.e. warmth, rejection, control or anxious parenting) were associated with children’s OCS when using the SCARED OCS subscale. Similarly, Challacombe and Salkovskis (2009) found no evidence that maternal promotion of autonomy, maternal warmth or high levels of expressed emotion were significantly associated with children’s (N = 61, 7–14 years) OCS. Regarding specificity, it is noted that significant positive correlations were also found between parental control, anxious rearing and rejection, and all other SCAS subscales (d’s ranged from d = 0.39 to d = 0.93, Grüner et al., 1999).
Family accommodation
Family accommodation
No eligible studies were identified which examined the association between family accommodation and childhood OCS in non-clinical populations.
Clinical populations
Parental behaviours
There is mixed evidence regarding the association between parental behaviours and childhood OCS/OCD in clinical samples, and no research has examined the independence of these associations. However, there is some evidence that particular parental behaviours are specifically associated with childhood OCS/OCD. When parental behaviours have been examined within a sample of children (7–12 years) with OCD, no significant associations have been found between children’s OCD severity and children’s reports of parental overprotection (d = −0.43), anxious parenting (d = −0.35) or rejection (d = 0.35, Mathieu et al., 2020). In contrast, Barrett et al. (2002) found that compared to parents of non-clinical controls (N = 22, 7–13 years), mothers and fathers of children with OCD (N = 18; 8–14 years) displayed significantly less warmth (d = −1.24, d = −2.08, respectively), confidence (d = −6.82, d = −7.87, respectively), positive problem solving (d = −1.95, d = −2.22, respectively) and rewarding of children’s independence (d = −3.38, d = −4.56, respectively) based on observations of a Family Discussion Task. However, there was no evidence that parents of children with OCD significantly differed from non-clinical controls on observations of maternal/paternal control (d = 2.45, d = 0.49, respectively), maternal/paternal doubt (d = −3.04, d = 0.02, respectively) or maternal/paternal avoidance (d = −0.53, d = 0.24, respectively). Furthermore, Farrell et al. (2013) found no evidence that mothers of children (8–12 years) with OCD significantly differed to mothers of non-clinical controls on displays of autonomy granting (vs. control d = −0.40) confidence (vs. doubt d = −0.07) or warmth (vs. dismissiveness d = −0.69). However, Farrell et al. (2013) did show that mothers of children with OCD displayed significantly greater enhancement of their child’s (rather than their own) responsibility for action during a Family Discussion task, compared to mothers of non-clinical controls (who did not differ in enhancement of their own or their child’s responsibility for action 1 ).
Regarding specificity, although Barrett et al. (2002) found that mothers of children with OCD (N = 18, 8–14 years) displayed significantly less warmth than mothers of children with anxiety disorders (N = 22, 6–14 years, d = −0.75), no significant differences were found between mothers of children with OCD and externalising disorders (N = 21, 7–12 years, d = 0.60). Furthermore, no significant differences in paternal warmth were found for fathers of children with OCD and anxiety disorders (d = −0.59). Overall, only less frequent displays of parental confidence, positive problem solving and rewarding of children’s independence were specific to parents of children with OCD, compared to parents of children with anxiety disorders (maternal confidence d = −4.03; problem solving d = −2.40; reward independence d = −2.89; paternal confidence d = −3.32; problem solving d = −2.18; reward independence d = −2.40) and externalising disorders (maternal confidence d = −1.22; problem solving d = −1.45; and reward independence d = −1.22, Barrett et al., 2002).
Family accommodation
Family accommodation
Family accommodation has consistently been found to be significantly associated with childhood OCS/OCD in clinical samples; however, no research has examined the independence of this association, and in the only study to examine disorder specificity, there was no evidence that this association was specific to children with OCD. For example, Lebowitz et al. (2014) found that compared to mothers of non-clinical controls (N = 16, 7–12 years), mothers of children with OCD (N = 21) reported significantly greater levels of overall family accommodation (d = 1.45), participation in rituals (d = 1.25), modification of family routines (d = 1.35) and parental distress when accommodating (d = 1.41). Similarly, when examining the association between OCD severity and family accommodation within groups of children (7–12 years) with OCD, strong significant associations have been found (N = 15, FAS Total d = 7.84, FAS Avoidance of Triggers d = 3.37, Bipeta et al., 2013; N = 24, FAS total d = 1.81, FAS Participation d = 1.19, FAS Modification d = 1.58, Wu et al., 2014). Furthermore, although no eligible treatment studies have statistically examined the association between changes in children’s OCD severity and changes in family accommodation across treatment, studies have consistently shown significant improvements in both children’s OCD severity and family accommodation from pre-to post-treatment, including following internet-delivered CBT (N = 11, 8–11 years, CY-BOCS d = −1.86, OCI-CV d = −1.65, ChOCI-R-P d = −2.15, FAS d = −2.67, Aspvall et al., 2018); group CBT (N = 32, 7–12 years, CY-BOCS d = −1.74, CY-BOCS-PR d = −1.58, FAS d = −1.51, Selles et al., 2018a); parent-led CBT (N = 6, 10–13 years, Lebowitz, 2013; N = 20, 5–7 years, Rosa-Alcázar et al., 2017; N = 44, 5–7 years, Rosa-Alcázar et al., 2019); and family-based CBT treatments (N = 7, 10–13 years, CY-BOCS d = −3.62, Waters et al., 2001; Rosa-Alcázar et al., 2017; Rosa-Alcázar et al., 2019), with some studies showing maintenance of these effects at 1-month (CY-BOCS d = −0.05, CY-BOCS-PR d = −0.09, FAS d = −0.23, Selles et al., 2018a) and 3-month follow-up periods (CY-BOCS d = −0.30, OCI-CV d = −0.03, ChOCI-R-P d = 0.06, FAS d = −0.04, Aspvall et al., 2018; Rosa-Alcázar et al., 2019; Rosa-Alcázar et al., 2017). Furthermore, Whiteside et al. (2014) also found significant improvements in both children’s CY-BOCS (but not ADIS OCD severity) and family accommodation scores following intensive CBT treatment (N = 10, 7–12 years, CY-BOCS d = −1.46; ADIS OCD d = −0.66; FA d = −1.46). In contrast to this overall pattern, Belschner et al. (2020) found no evidence that children’s (6–12 years) OCD severity or family accommodation significantly improved across the intervention period of a caregiver-focussed, mindfulness-based intervention (CY-BOCS-PR d = −0.29; FAS d = 0.03). Regarding specificity, Lebowitz et al. (2014) found that mothers of children with OCD (N = 21) did not report significantly greater levels of overall family accommodation (d = 0.40), participation in rituals (d = 0.30), modification of family routines (d = 0.31) or parental distress (d = 0.22) than mothers of children with anxiety disorders (N=17).
Siblings’ behaviours
Siblings’ behaviours
There is some evidence of an association between siblings’ behaviours and childhood OCS/OCD in clinical samples; however, no research has examined the independence or specificity of this association to childhood OCS/OCD. Barrett et al. (2000) found that on average, siblings of children with OCD (N = 4, 10–13 years) reported less warmth and greater rivalry in their sibling relationship compared to siblings of non-clinical children (N = 5, 8–12 years; d = −0.37 and d = 1.17, respectively); however, there were no mean differences in sibling dominance or conflict (d = 0.00 and d = 0.03, respectively). Furthermore, Barrett et al. (2000) also found evidence of mean improvements in both children’s OCD severity (d = −4.64) and sibling warmth (d = 0.13), dominance (d = −0.55), conflict (d = −0.25), rivalry (d = −2.25), overall accommodation (d = −1.89), participation in rituals (d = −1.95), modification of routines (d = −1.61) and distress when accommodating (d = −0.64) following CBT treatment.
Robustness of data synthesis
According to liberal thresholds suggested by Kmet et al. (2004), three studies were defined as poor quality (i.e. <55% quality ratings; Barrett et al., 2000; Lebowitz, 2013; and Muris & Merckelbach, 1998). Although studies were not excluded on this basis, re-examination of the results without these studies provides greater confidence that some parental behaviours (i.e. parental control, anxious parenting and rejection) are significantly associated with childhood OCS in non-clinical populations. However, there continued to be a lack of evidence that this association was specific to childhood OCS. Furthermore, without the inclusion of Barrett et al. (2000) there is no evidence on the potential role of sibling behaviours in the maintenance of childhood OCS/OCD. Overall, the main results of this review remain unchanged.
Discussion
This review synthesised 29 studies examining the association between childhood OCS/OCD and proposed maintenance factors identified from adult cognitive behavioural models of OCD, and descriptions of how family factors may maintain childhood OCS/OCD.
As shown in Figure 2, no eligible studies were identified for the importance of controlling thoughts, intolerance of uncertainty, perfectionism, attentional biases or neutralising actions. Furthermore, although there was evidence of cross-sectional associations between childhood OCS/OCD and all other cognitive and familial maintenance factors (but not behavioural factors, i.e., counterproductive safety strategies), findings were often inconsistent between and within studies. Notably, however, there were large, independent associations between childhood OCS and two cognitive factors, that is, inflated responsibility and meta-cognitive beliefs, after controlling for children’s depression symptoms (Magnúsdóttir & Smári, 2004; Stevanovic et al., 2016, respectively). Similarly, large, specific associations between childhood OCS/OCD and three (of the 12) parental behaviours examined were found (i.e. less frequent displays of parental confidence, positive problem solving and rewarding of children’s independence; Barrett et al., 2002). However, the association between parental confidence and childhood OCS/OCD was not consistently found across studies, with Farrell et al. (2013) not finding a significant association between reduced maternal confidence and childhood OCS/OCD. Finally, there was some, albeit limited evidence, that meta-cognitive beliefs may be specific to childhood OCS, on the basis that there was a significant association between children’s meta-cognitive beliefs and OCS (whilst controlling for depression symptoms), but no evidence of a significant association between children’s meta-cognitive beliefs and depression symptoms (whilst controlling for anxiety symptoms, Stevanovic et al., 2016). Crucially, there were no experimental studies and no studies which examined longitudinal associations directly, limiting any conclusions which can be drawn about the direction of any associations identified.
This review focused specifically on preadolescent children with OCD, and the results are both consistent with and contradictory to previous reviews examining the relevance of adult cognitive models of OCD to child and adolescent populations. Consistent with our findings, Mantz and Abbott (2017) concluded there was insufficient evidence to support a link between children (and adolescents’) cognitive beliefs and the maintenance of OCS/OCD. In contrast, Reynolds and Reeves (2008) concluded that there was broad support for the application of adult cognitive models of OCD to child and adolescent populations. Several reasons for these contradictory conclusions exist. First, Reynolds and Reeves (2008) placed less emphasis on whether cognitive beliefs were independently or specifically associated with OCS/OCD in young people than the current review. For example, correlational studies (not controlling for other psychopathological symptoms) were used as evidence to support the application of adult cognitive models of OCD to young people. Second, Reynolds and Reeves (2008) considered a broader age range of participants (i.e. <18 years old) and notably the older samples within this range provided greater evidence that cognitive beliefs are specific to young people with OCD (i.e. Libby et al., 2004) than was available for preadolescent samples. Finally, in contrast to the current review, Reynolds and Reeves (2008) included a broader range of papers (i.e. papers which did not examine the association between a measure of childhood OCS/OCD and a proposed maintenance factor measure) to inform their conclusions.
Limitations of the existing literature
The studies included in this review have several limitations to consider, including the heterogeneity of measures used, research designs employed and study power. These will now be considered in turn.
Variability in OCS/OCD measures
There was considerable variability in the measures of OCS/OCD employed, and their psychometric properties. Ten different measures of childhood OCS/OCD were used, which may account for the inconsistent findings both between and within studies (Brakoulias et al., 2014). This was illustrated by Simonds et al. (2009) who found substantially different effect sizes for the association between children’s OCS and ‘magical thinking’ when using two different OCS measures. Furthermore, the psychometric properties of the OCS/OCD measures varied. For example, whilst some studies have shown the LOI-CV significantly correlates with the CY-BOCS (e.g. Scahill et al., 1997) – which is considered the gold standard measure of OCD for young people (Lewin & Piacentini, 2010), other studies have not (e.g. Stewart et al., 2005; Storch et al., 2011). Future research would benefit from using measures of OCS/OCD which are specifically designed and validated for preadolescent children.
Variability in maintenance measures
There was also considerable diversity in the measures of proposed maintenance factors used, limiting our ability to compare and synthesise existing knowledge in the field. For example, of the four studies examining inflated responsibility, four different measures were used, including assessments individualised to children’s most frequent intrusions (e.g. Barrett & Healy, 2003); RAS (e.g. Farrell et al., 2012); RAS-C (e.g. Magnúsdóttir & Smári, 2004); and OBQ-CV (e.g. Mathieu et al., 2020). Furthermore, the cognitive measures used (e.g. RAS; revised TAF scale; WBSI) were often adapted from adult cognitive measures and lack sufficient validation for younger populations (Mantz & Abbott, 2017). As such, it is unclear whether these measures examined the intended mechanisms, due to differences in adults’ and children’s cognitive development (Casey et al., 2005). The development and validation of valid and reliable measures that can be used consistently to examine the proposed maintenance factors specifically among preadolescent children is urgently required.
Research design
Our knowledge of the mechanisms which maintain childhood OCS/OCD is limited by the research designs employed. Critically, no experimental or prospective longitudinal studies were identified in this review, which are crucial to determine the direction of effects between childhood OCS/OCD and proposed maintenance factors. Instead, studies most commonly used correlational designs. This was particularly problematic in studies where the sample consisted only of children with OCD, as there was a restricted range of OCS. This meant that the non-significant associations found between children’s OCS and proposed maintenance factors within samples of children with OCD may have resulted from insufficient variability in OCS, rather than the absence of a maintenance effect. Furthermore, few treatment studies statistically examined the association between changes in children’s OCS and changes in proposed maintenance factors, considerably limiting the conclusions which can be drawn from these studies. Finally, few studies compared children with OCD to children with other mental health disorders, such as anxiety disorders, limiting our understanding of whether the proposed maintenance factors are specifically associated with OCD in children.
Study power
Studies conducted with clinical populations often had small sample sizes and either failed to report power analyses or were insufficiently powered to detect potentially clinically meaningful effects. This limits our understanding of whether the proposed maintenance factors apply to preadolescent children, as non-significant associations could often be attributed to limited power. Thus, researchers need to ensure future studies are sufficiently powered to detect meaningful effects.
Strengths and limitations of the review
This is the first review to examine the applicability of adult cognitive behavioural models of OCD exclusively to preadolescent children and extends previous reviews by examining a broader range of mechanisms in the maintenance of childhood OCS/OCD. An extensive electronic search using broad search terms was conducted, and forward citation handsearching was carried out to identify recently published papers. Furthermore, the authors of 96 papers were contacted to request re-conducted analyses for participants within our specified age range. Nonetheless, a number of limitations need to be considered. First, of the studies where data was re-analysed (n = 7), sample sizes were often small and/or insufficiently powered to detect potentially meaningful differences through significance testing, limiting the conclusions which can be drawn from these studies. For example, where the results of re-conducted analyses differed to the original papers (e.g. Belschner et al., 2020; Whiteside et al., 2014), it is unclear whether this was due to the age of the participants. Second, the scope of this review was limited by our classification of maintenance measures during the screening stages (see Prospero CRD42019153371 for full details). For example, the CY-BOCS was only classed as a measure of OCS/OCD and not a measure of maintenance. This meant that papers using specific items of the CY-BOCS (e.g. avoidance and doubt) to measure maintenance were not included in this review. Furthermore, given that some of the proposed maintenance factors identified from adult models of OCD are also core features of the disorder (e.g. emotional and behavioural responses), there was overlap in the measures of OCS/OCD and some of the maintenance factor measures used (e.g. measures of counterproductive safety strategies) – limiting the conclusions which can be drawn. Third, this review was limited by our study design criteria. We required studies to examine the association between a proposed maintenance factor and a measure of childhood OCS/OCD, and not, for example a measure of an element of OCS/OCD. This meant that we did not include studies such as Reeves et al. (2010), who experimentally manipulated non-clinical youths’ perceived responsibility for a task and examined the effect on variables including checking, hesitation and state anxiety. Thus, some studies which may contribute to our understanding of the relevance of adult models of OCD to youth were not eligible for the review. Fourth, we used effect size calculators which assumed statistical independence between proposed maintenance factor and OCS/OCD scores at different timepoints (i.e. pre- and post-treatment study scores), which may have resulted in inaccurate calculations in some circumstances. We also extrapolated the recommended values for converting standardised regression coefficients to Pearson’s r. Finally, this review focused on proposed maintenance factors derived from theoretical accounts of the development and maintenance of OCD – however, it may be necessary to derive hypotheses about the mechanisms which maintain childhood OCD directly from children themselves, for example, through qualitative research. This approach has facilitated the understanding of other psychological disorders (e.g. psychosis, Isham et al., 2019) and has the potential to advance clinical interventions (Isham et al., 2019).
Conclusion
This systematic review examined the putative maintenance mechanisms for childhood OCS/OCD as identified from theoretical models of adult OCD and descriptions of how family factors may maintain childhood OCS/OCD. While there was some evidence of cross-sectional associations between childhood OCS/OCD and certain proposed maintenance factors, there is currently limited evidence that these associations are independently or specifically associated with childhood OCS/OCD. Inflated responsibility and meta-cognitive beliefs have been shown to be independently associated with childhood OCS (when controlling for children’s depression symptoms). Similarly, meta-cognitive beliefs may be specific to childhood OCS, as significant associations have been found between children’s meta-cognitive beliefs and OCS but not between children’s meta-cognitive beliefs and depression symptoms (when controlling for children’s anxiety symptoms). Finally, certain parental behaviours (e.g. reduced confidence, positive problem solving and rewarding of children’s independence) have showed evidence of specificity to children with OCD (when compared to children with anxiety disorders and children with externalising disorders). However, findings are often inconsistent both between and within studies and there is currently no evidence that can allow conclusions about the direction of these associations, and, as such, whether these factors do in fact have a maintaining role. Given the detrimental impacts of childhood OCD, future research urgently needs to use experimental and prospective longitudinal designs to elucidate whether the proposed maintenance mechanisms maintain childhood OCD, to improve the efficacy of CBT for preadolescent children with OCD.
Footnotes
Acknowledgments
The authors would like to thank Dr Alice Farrington, Berkshire Healthcare NHS Foundation Trust, for comments on a draft of this manuscript.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the Economic and Social Research Council [ES/P00072X/1]. Brynjar Halldorson and Cathy Creswell received funding from the National Institute for Health Research (NIHR) Applied Research Collaboration Oxford and Thames Valley at Oxford Health NHS Foundation Trust. The views expressed are those of the author(s) and not necessarily those of the NHS, the NIHR or the Department of Health and Social Care.
