Abstract
Background:
Healthcare is challenged by a rapidly growing group of patients with multi-morbidity and polypharmacy. Increasing activity and specialization puts pressure on healthcare sectors. Medication errors in cross-sectoral transition of patients are often seen. The aim of the study was to explore drug-related problems (DRPs) in the transition of patients between sectors and to develop and pilot-test a cross-sectoral hospital pharmacist intervention to overcome some of these problems.
Methods:
DRPs in cross-sectoral transitions were explored from four perspectives; the literature, the primary and secondary healthcare sector and the patients. An intervention was developed from the findings through co-creation between pharmacists, doctors and a nurse. The intervention was piloted and evaluated from data on the included patients and the activities performed.
Results:
DRPs in transitions from general practice (GP) to hospital were caused by inadequate focus on updating the Shared Medication Record (SMR). For patients being discharged, DRPs were described with multiple facets; for example, missing information on medication changes, lacking patient involvement and problems with dose-dispensed medicine or electronic prescriptions. An intervention with a pharmacist in a shared employment between Hospital Pharmacy and GP was developed and piloted. The intervention included medication reconciliation and updating SMR for patients referred to hospital; and medication review, overview of medication changes and follow-up telephone calls for patients discharged from hospital. The intervention identified and solved several DRPs; in this way, medication errors were avoided. Access to health records in both sectors was important in the identification and resolution of DRPs.
Conclusion:
DRPs in cross-sectoral transitions are multifaceted and the experiences depend on the point of view. The cross-sectoral hospital pharmacist intervention identified and solved several DRPs and medication errors were avoided. The intervention made sense to both healthcare sectors and patients. Shared employment and unique access to health records in both sectors showed to be of importance in the identification and resolution of DRPs.
Plain language summary
For patients being discharged, drug-related problems were related to for example
missing information on medication changes
sparse involvement of the patient in their own treatment
problems with medicine dispensed on a dose dispensing machine at the local pharmacy.
An intervention with a pharmacist in a shared employment between Hospital Pharmacy and general practice was developed and piloted. The intervention included
talking to the patient about their medication and updating the Shared Medication Record for patients referred to hospital
medication review, overview of medication changes and follow-up telephone calls for patients discharged from hospital to general practice.
The intervention identified and solved several drug-related problems. Access to health records in both the general practice and at the hospital was important in the identification of drug-related problems.
Keywords
Introduction
Healthcare is challenged. Challenged by people living longer, by an increasing number of people of retirement age 1 and; therefore, by a rapidly growing group of patients with multi-morbidity (⩾2 chronic illnesses) treated with several concomitant drugs (polypharmacy; ⩾5 drugs). 2
General practice (GP) is the patient’s primary entrance to the healthcare system and is the central coordinator of the patient’s overall treatment across medical specialties. However, increasing specialization in the healthcare system has meant that patients are prescribed medication by different specialists, who primarily focus on illnesses within their own field of expertise. 2 The number of general practitioners (GPs) is declining and GPs must increasingly handle more and more complex patients per GP, which puts pressure on the primary healthcare sector. 1
Activity in Danish hospitals has increased over the years 3 and the length of hospital stay has concomitantly decreased. 4 The high activity and the faster patient flow in the hospitals give increased workload to the staff 3 and make it more difficult for the hospital doctors to focus on the patients’ current medical treatment which does not necessarily relate to the cause of hospitalization. In order to optimize patients’ medical treatment, many hospitals collaborate with hospital pharmacists on medication reconciliation and review. 5
In Denmark, we have a real time updated Shared Medication Record (SMR) for each patient in which both the primary and the secondary healthcare sector can see and update the patient’s current medication. 6 A regional guideline states that GPs must update the SMR in case of elective referral to the hospital and strives to update the SMR in case of emergency admissions. Likewise, regional guidelines state that the hospital doctor must update the SMR at discharge 7 and send discharge letter electronically to the GP within 1–2 days after discharge. 8 Knowledge of the patient’s current medication and reasons for medication changes are crucial prerequisites for being able to treat patients optimally and avoid medication errors–regardless of which direction the patient moves in cross-sectoral transitions. Medication errors in cross-sectoral transition of patients are often seen; an English study reports prescription errors in 20% of patients discharged from hospital. 9 Medication errors expose patients to an unnecessary risk and can increase hospital stay, healthcare costs and mortality.10–13
Patients are experts in their own lives and a valuable source of information for healthcare professionals when organizing medical treatment. 14 Many patients prefer greater involvement in their treatment and care, 15 and patient involvement has the potential to improve their knowledge, skills, adherence and confidence with managing their illness.16–18 Patient involvement helps ensure that the decisions made about medical treatment are executed into their daily lives at home.
Hospital pharmacists have in-depth knowledge of medication-related issues and a pharmacist with a shared employment between the hospital and the GP may be a link to ensure a good cross-sectoral transition and coherence of the medical treatment. Besides having prescription information in the SMR, GP and hospitals have separate electronic journals. In practice, this means that neither sector has easy access to explanations and thoughts that are the basis for treatment decisions. By having a shared employment, the pharmacist will have access to both electronic systems and therefore insight into the intentions of current and future treatments for the individual patients in the practice.
To the best of our knowledge, no studies in a Danish setting have been published identifying which DRPs are seen in cross-sectoral transitions and examining how a patient-centred collaboration between GPs and hospital pharmacists can be established to optimize the medical treatment among patients in cross-sectoral transitions.
Therefore, the aim of the study was to explore DRPs in the transition of patients between healthcare sectors and to develop a cross-sectoral hospital pharmacist intervention to overcome some of these problems.
Methods
This study is reported in accordance with the checklist of the Criteria for Reporting the Development and Evaluation of Complex Interventions in healthcare (CreDECI 2) (Items 1–5). 19
This study reflected two phases of a complex intervention design20,21: phase I, the development process and phase II, piloting.
The study group comprised three hospital pharmacists, two GPs and a medical doctor and a nurse from the hospital.
Setting
The study was performed at Randers Regional Hospital and a GP in Grenaa, Denmark.
Randers Regional Hospital has 190 beds, around 18,000 acute hospitalisations and 95,000 outpatient visits per year within a catchment area of 226,000 inhabitants including inhabitants in Grenaa. 22 The GP serves approximately 8700 patients, has five doctors (3,2 full-time equivalents), seven nurses (6,0 full-time equivalents) and a number of other healthcare professionals employed.
GPs are responsible for the update of the electronic SMR prior to a hospital visit whether it is an outpatient visit or an acute hospitalization.23,24 If the patient is referred by another doctor than their own GP, the SMR is not necessarily updated. GPs perform medication review in relation to chronic ill patients’ annual check-up visits in the clinic.
Some patients receive their oral medication dose-dispensed on a robot at the local pharmacy every 14 days. The dose-dispensing is primarily for patients in stable medication in agreement with the GP.
Medication reconciliation and updating the electronic Medication Administration Record (eMAR) in hospital is performed by hospital physicians at, for example, the Emergency Department, Randers Regional Hospital prior to referral to other departments.
Hospital pharmacists routinely perform medication review at Randers Regional Hospital on patients who are in high risk of medication errors assessed by using the validated algorithm MEdicine Risk Score (MERIS). MERIS calculates a score based on the patients’ medication and renal function. Patients in high-risk of medication errors have a score ⩾ 14. 25
When a patient is discharged from the hospital, the physician is responsible for the assessment and adjustment of the patient’s medication, medication reconciliation, SMR update, withdrawal plans and generating electronic prescriptions for new or lacking medication.
The physician is also responsible for writing a discharge letter to the GP including a description of the admission, treatment and possible follow-up plans. The discharge letter is sent electronically to the GP. 26
A nurse will print the medication list and discharge letter and talk to the patient about it. Medication is dispensed for 1–3 days if the patient or relatives are not able to go to the pharmacy on their way home or if the patient have nursing care for medication administration.
For patients in nursing homes or with municipal nursing care, a discharge report is written by a nurse and sent electronically. The discharge report includes information on the admission, treatment, care needs and possible follow-up plans. The nursing home or municipal nursing care is also contacted by telephone. 26
During the study a hospital pharmacist was partly employed at the Hospital Pharmacy and partly employed in the GP. This shared employment provided access to electronic patient records in both healthcare sectors.
Development and pilot-test of the intervention
The intervention was built upon the concept of interdisciplinary collaboration 27 and the hypothesis was that medication for patients in cross-sectoral transitions can be optimized through collaboration across healthcare professionals and across healthcare sectors.
The development of a cross-sectoral pharmacist intervention comprised a series of stages to develop and refine the intervention (see Figure 1).

Developing and piloting a cross-sectoral hospital pharmacist intervention—stages and timeline.
Stage 1: identification of the evidence base
In Stage 1, identification of the evidence base was performed by exploring the question: Which DRPs are seen in the transition of patients between healthcare sectors and how can a pharmacist intervention be used to solve some of these problems?
The question was explored from four points of view from April to July 2021 as four concurrent processes (see Stage 1, Figure 1).
i. What does the literature say?
Published evidence on medication-related pharmacist interventions to improve patient safety in, respectively, sector transitions and GP was explored by two literature searches.
In May 2021, the literature database PubMed was searched for reviews, systematic reviews, or meta-analysis, published in 2011 to 2021.
Both MESH terms and text words were used; for example, MESH terms as pharmacists, medication error, GP and transitional care or text words as medication reconciliation, medication continuity, primary healthcare and patient discharge. The full search queries can be seen in Supplemental Appendix 1.
Studies that did not only include pharmacists, not involved GP or care transitions, were written in other language than English and Nordic language or were without access, were excluded.
The last author (CO) performed the literature searches with the support of a librarian.
ii. What does the primary healthcare sector experience?
Observation in clinical areas: Two experienced hospital pharmacists (LJ, CAS) was placed in the GP clinic in May 2021 and performed observations in clinical areas in the GP, for example by participating in morning conferences, in two patients’ annual check-up visits with a nurse and in one of the weekly GP-visits at a nursing home. The observations were used to get an initial picture of how the GP clinic was organized.
Interviews with staff: Healthcare professionals in the primary healthcare sector (GPs, nurse, practice manager, secretary, care assistant, practice assistant, homecare nurse and a pharmacist at the local pharmacy) were interviewed (semi-structured) to uncover which DRPs they experience from their point of view. The interviews were performed in the GP clinic, the homecare’ office and the local pharmacy over seven dates in May 2021. An interview guide was developed to gain further knowledge of how the GP Clinic was organized, how the individuals worked with the patients’ medication, which DRPs they experienced and how these were related to healthcare transitions. The interview guide was adapted to each type of healthcare professional and was not pilot-tested. The interview guide can be seen in Supplemental Appendix 2.
Patient cases: A total of 175 patient cases in GP were randomly selected and explored by the hospital pharmacist (LJ) in May 2021. The patient cases were reviewed in relation to the update of SMR according to the guideline.23,24 Seventy-five of these cases were patients from nursing home or with recent annual check-up visit and 100 cases were referred to an outpatient clinic.
In addition, 10 randomly selected patient cases in GP were explored to identify actual or potential DRPs through a pharmacist-led medication review. The pharmacist-led medication review comprised a critical examination of the patient’s clinical data and current medication according to doses, timing, formulation, interactions, side effects, biochemistry and guidelines.
iii. What does the secondary healthcare sector experience?
Interviews with staff: A medical doctor and a nurse working with cross-sectional collaboration, both from Randers Regional Hospital, were purposefully selected for the semi-structured interviews as they were considered able to provide in-depth and detailed information about which DRPs the secondary healthcare sector experience. Both interviews were held in June 2021 – in the doctor’s office and online with the nurse. An interview guide was developed to gain further knowledge of their daily work, which DRPs they experienced and how these were related to healthcare transitions. The interview guide can be seen in Supplemental Appendix 3.
Patient cases: Nine hospitalized patients from the GP in question were consecutively recruited at the hospital in June 2021. Hospital records and discharge letters were reviewed by the hospital pharmacist (LJ) in relation to medication changes during hospitalization including communication about these to the primary healthcare sector. Medication changes were defined as any change in the medication list when comparing lists from prior and after hospitalization. For example, an altering of dose, an addition of a medication or a withdrawal of a medication.
iv. What do the patients experience?
Patient cases: Seven patients associated to the GP in question were interviewed by CAS (semi-structured) by telephone after their discharge from hospital to uncover their knowledge about medication changes during hospitalization, how they were involved in their medication at the hospital and if they had missed a place to gain further knowledge about their medication after discharge. These patients were recruited at the hospital as described above in (iii). The interview guide can be seen in Supplemental Appendix 4.
Stage 2: development of the intervention
The information gained from Stage 1 was discussed by CAS, LJ and CO and the most important findings were identified. This synthesized information was presented for the study group in an inter-disciplinary workshop (Stage 2). During the inter-disciplinary workshop, the study group had brainstorms and discussions under the headings: (a) Pharmacist intervention for patients referred to an outpatient clinic; (b) Pharmacist intervention for patients acutely admitted to the hospital; (c) Pharmacist intervention for patients transferred from the hospital to the GP and (d) Possible ad hoc tasks in the GP clinic. At the end of the interdisciplinary workshop, the study group, decided which elements to be included in the first prototype of the intervention. Elements included: medication history, medication reconciliation, SMR update, medication review, overview of medication changes and follow-up telephone calls after discharge.
Stage 3: pilot-test of the intervention
The pharmacist intervention was delivered by LJ in the GP in October to November 2021. The intervention was delivered to patients referred to an outpatient clinic prior to their hospital visit and retrospectively to patients after their hospital visit. Hospitalized patients were identified by using a Business Intelligence report on hospitalized patients from the GP in question. The report was electronically generated each day at 5 p.m., sent out on email the next morning and informed consent was obtained afterwards.
The information gained from the pilot test was discussed by CAS and LJ, and the most important findings on the included patients and the activities performed were identified. This synthesized information was presented for the study group in an inter-disciplinary workshop (Stage 3). This aided to the final version of the intervention (Version 2). See Supplemental Appendix 5.
Participants
Pilot study participants were patients in transition between hospital and GP – both ways. The participants were consecutively recruited Monday to Friday at Randers Regional Hospital by hospital pharmacists (n = 30) or at the GP by the GP, a nurse or a hospital pharmacist (n = 14). Written informed consent was obtained prior to participation. Patients were eligible for inclusion if they were ⩾ 18 years old. Patients were excluded if they were hospitalized due to childbirth, a psychiatric diagnosis, were considered too ill (suicidal, cognitive impaired or with life-threatening illness) or were unable to speak Danish.
Data analysis and outcomes
Interviews during the development phase were performed by two experienced pharmacists (CAS and LJ). The interviews were audio-recorded. Due to time constraints, the interviews were not transcribed; therefore, citations were selected by listening to the audio-recorded interviews. Data from reviewing patient cases were analyzed by using numbers and percentages.
The overall information gained was presented from the four points of view in question; (a) the literature; (b) the primary healthcare; (c) the secondary healthcare; and (d) the patients.
The pilot study was evaluated by looking at data on the included patients and the activities performed by the pharmacist; including baseline characteristics, update of the SMR, medication discrepancies at referral, medication changes at discharge, electronic prescriptions, DRPs identified in the medication review or at the follow-up telephone call.
Numbers, mean, SD, minimum/maximum values, percentages, median and interquartile range were used when relevant.
DRPs were defined as events or circumstances involving drug therapy that actually or potentially interferes with desired health outcomes. 28
Results
Development of the intervention
Synthesis 1
A summary of the findings when exploring DRPs and interventions in the transition of patients between healthcare sectors seen from the four points of view is presented in Table 1.
Summary of the findings in the literature searches, staff interviews, patient cases and patient interviews.
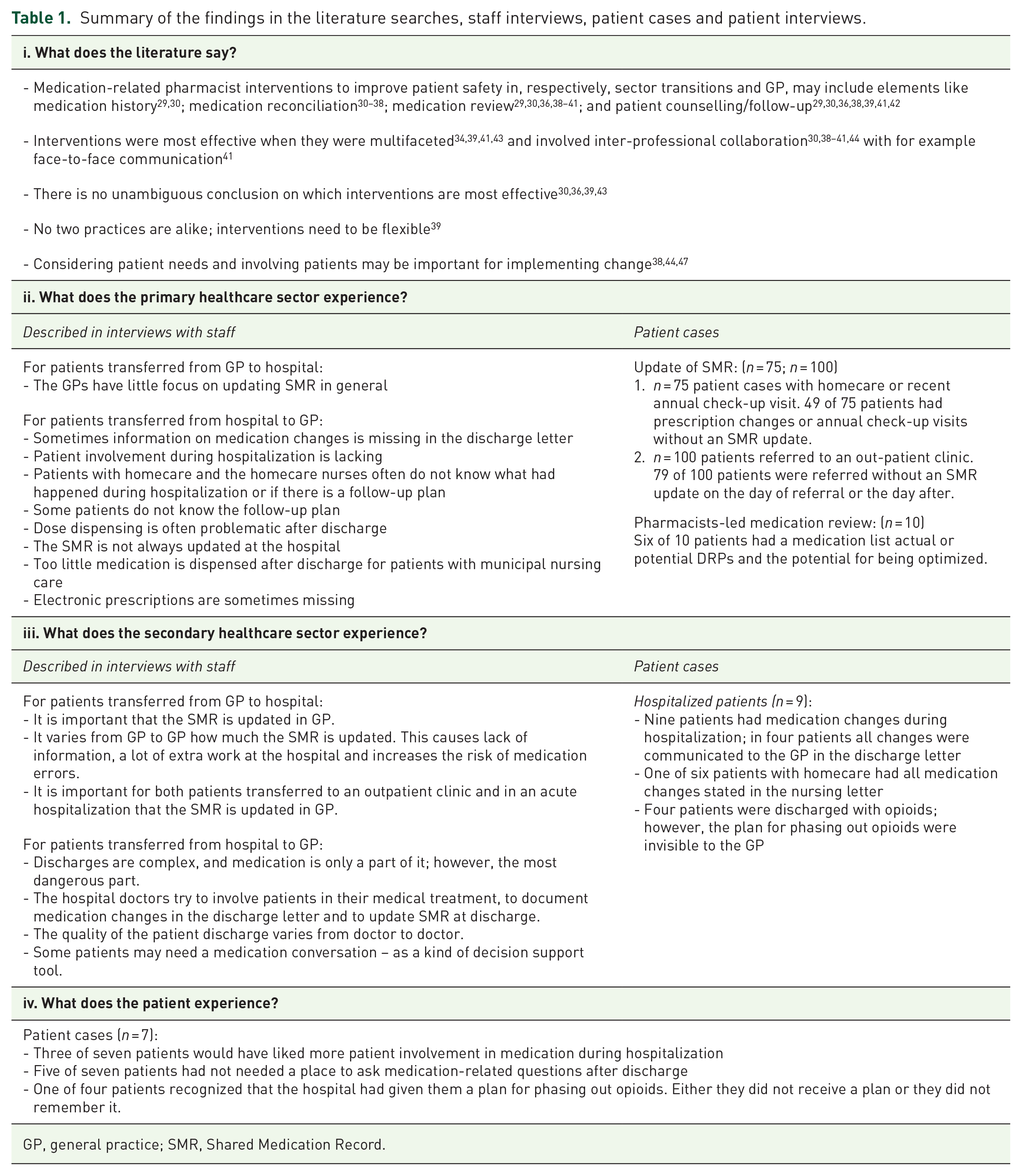
GP, general practice; SMR, Shared Medication Record.
i. What does the literature say about medication-related pharmacist interventions in sector transitions and in GP?
In the two literature searches, respectively 63 and 64 articles were identified. A total of 113 were removed after title and abstract screening (n = 84) and full-text screening (n = 29) leaving 14 articles for inclusion. In addition, four articles found by random search were included. For further information; for example reasons for exclusion, see Supplemental Appendix 1.
The findings from the included articles showed that many different pharmacist interventions have been explored, for example medication reconciliation in healthcare transitions, medication review, patient counselling and follow-up.29–46 The literature reviews showed positive effects on medication discrepancies, DRPs, potential adverse drug events and hospital revisits related to adverse drug events;31,34,39,40 however, no single preferred, effective pharmacist-led intervention or a consensus for best practice has been identified. 40
Medication-related pharmacist interventions in GP were most effective when they were multifaceted and involved patient follow-up and interdisciplinary collaboration with face-to-face communication. 41 No two GPs are alike, so the role of the pharmacist should be flexible and meet local needs. 39 Patient involvement is important for a long-term effect and for motivation to change. 44
ii. What does the primary healthcare sector experience?
Interviews with staff. From the perspective of the primary healthcare sector, a total of nine interviews were performed. Interviews (n = 7) in the GP included two GPs, one nurse, one practice manager, one secretary, one care assistant, one practice assistant (medical student). In addition, an interview with one homecare nurse and a pharmacist at the local pharmacy was performed.
For patients transferred from GP to hospital, the interviews showed that updating SMR had not been in focus in the GP: We are expected to update SMR before admitting a patient. In the acute situation we do not have time to get an overview of a patient’s medication if, for example, it is a long time since their last annual check-up. In addition, the patient can be followed by various specialists, so you are not responsible for the full medication. (General practitioner 1) I think that updating SMR is a really good idea. We do it in relation to patients’ annual check-up and we should also do it before we admit people, but we are just not good enough at doing that. We know very well that it can take on average an extra 15 minutes to assess a patient in the Emergency Department if SMR is not updated. We are not doing it well enough. I would like to make that a focus point. (General practitioner 2)
For patients transferred from hospital to GP, the interviews showed experiences that information on medication changes is sometimes missing. The SMR is not always updated, sometimes electronic prescriptions are missing and some patients do not know the follow-up plan: The worst thing is when the patient is discharged and SMR is not updated. It is not always clear in the discharge letter why a medication change has been made. Sometimes I have to look in the e-record because I need an explanation or if there is a follow-up plan. The patient, especially those with homecare nursing, is not always involved in their own treatment. (Nurse) The discharge letters are of very variable length. Some are easy to read and are written with a clear and distinct conclusion. Others are difficult to read and it is unclear what is relevant to me and what is done at the hospital. Sometimes information about medication is adequate and other times it is not. (Practice assistant) The discharge letters contain information about medication changes; however, the minor adjustments are not always mentioned. We will then capture that in the SMR. I could call the hospital to find out if the little things are mistakes or correct changes. Also, we often find that there is a lack of electronic prescriptions for new medicines. (Homecare nurse)
Patient cases. A total of 175 patient’s SMR were audited in relation to their update. Of these, 75 cases were patients from a nursing home or with a recent annual check-up visit. Prescriptions changes or annual check-up visits without a SMR update were found in 65% of the patients (49/75). One of the patients had a SMR with 1456 days (4 years) since the last SMR update and was receiving dose-dispensed medication from the local pharmacy. An example of a misleading SMR was a patient with a prescription of 300 mg Gabapentin in the SMR; however, in the patients’ GP record, it was stated that the dose was increased to 300 mg three times daily.
In addition, 100 cases were patients referred to an outpatient clinic. Of these, 79% (79/100) were referred without an SMR update on the day of referral or the day after.
Pharmacist-led medication review was performed on 10 randomly selected patients in the GP.
Six of 10 patients had a medication list with actual or potential DRPs and the potential for being optimized. An example was a patient with Amlodipine, Bisoprolole, Acetylsalicylic acid and Nitroglycerine spray prescribed during a previous hospitalization; however, heart problems had since been ruled out.
iii. What does the secondary healthcare sector experience?
Interviews with staff. From the perspective of the secondary healthcare sector, two interviews were performed; one with a medical doctor and one with a nurse with experience on cross-sectoral collaboration.
For patients transferred from the GP to the hospital, the interviews showed the experience of SMR not always being updated. Both for patients referred to an outpatient clinic and for acutely admitted patients: It may have major consequences for patients if the SMR is not updated. When a patient has several diseases, then no one ‘dares’ take responsibility. Many hospital physicians say, well, the doctor responsible for the patient must then be his doctor in GP. But no, not if the patient also goes to a COPD outpatient clinic. Then your doctor in GP will never bother with it. (Nurse) It has a huge significance that the medication list is correct and SMR is being updated. This applies to both patients referred to an outpatient clinic and for patients referred for acute care. (Doctor)
For patients transferred from the hospital to the GP, the interviews reflected that the discharge process is really complex and involves several parties. Medication is only a part of the discharge process; however, ‘It [medication] is the most dangerous part’ (Nurse).
The hospital has an ambition to involve patients in their medical treatment, to document medication changes in discharge letters and to update the SMR at discharge; however, the interviews also indicated that this is not always the case.
I have a lot of attention around medication. I make sure the medication lists are correct, to update SMR, and to contact the GP when I am in doubt about something. I pay attention to justify medication changes and talk to patients about what has changed. I am aware of writing about medication changes in the discharge letters. I probably do more than most doctors due to my particular interest in the field. (Doctor) The discharge process is too fast and you completely forget to involve the patient. At discharge, they [nurses] have much more focus on how to inform the municipality; but how do they prepare the patient for him to be discharged?. (Nurse) I have often thought that one should introduce a medication conversation at patient level. What is the consequence if you do not take your medication? The doctors just assume that of course they are taking their medication. The medication conversation could be like a kind of decision support tool. You have this choice and that choice. And these choices have consequences if you choose this or that. There are some places where one forgets to involve the patients. (Nurse)
Patient cases. A total of nine hospital records and discharge letters were audited in relation to medication changes during hospitalization and communication about them to the primary healthcare sector. The patients were admitted to the Orthopaedic Surgical Department (n = 4), to the Gastrointestinal Surgical Department (n = 1) or the Medical Department (n = 4). All of the patients had medication changes during hospitalization; in four of the cases all of their medication changes were communicated to the GP in the discharge letter. A total of six of the patients had homecare nursing after discharge; medication changes were noted in the discharge letters for the homecare nurses in one of the six cases.
Four patients were discharged with opioids and a plan for phasing out opioids were prescribed in the eMAR at the hospital; however, the phasing out plans were not visible for the GP in either the discharge letters or the SMR.
iv. What does the patient experience?
Seven of the nine audited patients were reached by telephone after discharge. In general, the patients were satisfied by their treatment at the hospital.
Three of seven patients would have liked more patient involvement in their medical treatment during hospitalization.
There was no doctor who told me why all those changes were made. (Patient 4) They did not tell anything by themselves. But they were willing to answer when I asked. I want to know what I am taking. (Patient 6)
Four patients were discharged with opioids; one of them recognized that she was discharged with a plan for phasing out opioids after discharge.
The doctor told me what was going to happen and I also got a note with the phasing out plan to take home. (Patient 1)
Five of seven patients had not needed a place to ask medication-related questions; two of the patients had check-up visits at the hospital twice a week.
Synthesis 2 (Figure 1)
During the inter-disciplinary workshop, the information gained was further synthesized and informed the development of the first prototype of the intervention (see Table 2).
Components of piloted intervention (version 1).

Intervention components are described in the table as well as the basis of rationale.
GP, general practice; SMR, Shared Medication Record.
Piloted cross-sectoral pharmacist intervention
Synthesis 3 (Figure 1)
A total of 14 patients referred to an outpatient clinic were included in the GP Clinic by a GP or a nurse. In addition, 30 hospitalized patients were included by a pharmacist in the hospital (see Table 3).
Descriptive data for included patients.

GP, general practice; IQR, interquartile range; SMR: Shared Medication Record
Reason unknown: GPs did not register why a patient was not recruited.
Medication review not performed in patients with no or only a few medications.
Considered too ill: suicidal, cognitive impaired or with life-threatening illness.
The SMR was not updated by the GP in 14% of patients referred to an outpatient clinic; however, despite the update, the pharmacist-led medication history revealed 22 medication discrepancies in 9 of 14 patients. Most of them were minor (n = 20) and were easily solved by correction in the SMR by the pharmacist.
The SMR was not updated by the GP in 63% of acutely hospitalized patients. At discharge, the SMR was not updated by the hospital in 10% of the patients.
Medication changes during hospitalization were seen in 79% of the patients. Twenty-nine percent of the medication changes were not communicated to the GP and 58% not to the homecare nurses.
A total of 24 missing electronic prescriptions in 13 patients were seen.
A pharmacist-led medication review was performed for 36 patients. DRPs were found in 24 patients; 55 comments in total. Most of these were related to medication reconciliation, dose, or interactions.
Seven of the 44 patients were included without consent according to the study permissions; therefore, a follow-up telephone call was planned for 37 patients. Follow-up telephone calls were performed for 23 patients; in 14 cases we missed the follow-up call of various reasons (see Table 3). The pharmacist discovered seven patients with DRPs related to the transition between the hospital and the GP. An example was a patient, who was discharged with high dose of morphine and an abrupt discontinuation date. Another example was a patient who were used to take isosorbide-mononitrate 30 mg daily. The patient was discharged with 60 mg; however, the new dose was not prescribed in the SMR or mentioned in the discharge letter for the GP or the homecare nurse. With access to electronic records in both healthcare sectors, the pharmacist was able to participate in the identification and/or resolution of these problems.
Most patients liked the initiative with a follow-up telephone call; however, some mentioned that it was more relevant for others than themselves.
Ad hoc tasks included preparation of a guideline for updating SMR in the GP in question, presentation of the guideline at morning conferences and a few medication reviews on patients chosen by the GP. One week after the implementation of the SMR guideline, 57% of the referred patients had an updated SMR on the day of referral or the day after.
An interdisciplinary workshop was held after the pilot study. Overall it was considered that the different elements of the intervention made sense to both healthcare sectors and to the patient. The timing of the follow-up telephone call was clarified to be performed ideally the day after discharge. No further changes were made to the design of the intervention (Version 2, see Supplemental Appendix 5).
Discussion
In this study, we aimed to explore DRPs in the transition of patients between healthcare sectors and to develop and pilot-test a cross-sectoral hospital pharmacist intervention to overcome some of these problems. In our thorough coverage of the perspectives from healthcare professionals, patients and the literature, we found that DRPs in cross-sectoral transitions are multi-faceted. Especially GPs not updating SMR regularly and at referral and lacking information on medication changes after discharge was noticed. Also, we saw lacking patient involvement, problems with dose-dispensed medicine after discharge and dispensing of too little medicine after discharge. Transitional care is complex and thus; the cross-sectoral hospital pharmacist intervention was developed with the purpose to overcome only some of the problems. With the intervention, we wanted a pharmacist with a shared employment between the Hospital Pharmacy and the GP, to keep an extra eye on patients’ medication on their way into the hospital as well as home again.
In Denmark, we have a SMR for each patient with access from both healthcare sectors. The electronic record was implemented with the purpose to reduce the number of medication errors that occur due to lack of information about patient’s medication, reduce the number of readmissions due to medication errors and to reduce the time spent clarifying patients’ current medication. 6 To fulfil this purpose, it is important that physicians in both sectors focus on updating SMR on an ongoing basis and when medication changes are made. Especially in cross-sectoral transitions where treatment-responsibility shifts. Our study found, that updating SMR had been given little focus at the GP; however, the intervention and the implementation of a guideline for the update of SMR had an impact on GPs behaviour updating SMR. Many GPs are not aware of the increased risk of medication errors when the SMR is not updated. GPs in Denmark normally do not have a pharmacist in the clinic. The presence of the pharmacist in the GP helped to focus on updating SMR which may have reduced the number of potential medication errors and extra work at the hospital.
In line with our study, it is well known that discrepancies between registered prescriptions and patients’ actual use of medication are frequent and the majority of discrepancies are caused by the healthcare system (53%) or the patient (32%; 70% intentional non-adherence). 49 Therefore, the intervention included medication history and focus on updating SMR at referral from the GP to the hospital.
For patients discharged from hospital, we found DRPs in many of the patients. Most of the patients had an updated SMR; however, 50% of the patients with new prescriptions missed an electronic prescription, and 30% of medication changes were not communicated to the GP in the discharge letter. This number was even higher for medication changes communicated to the homecare nurses. In addition, the pharmacist identified DRPs in two thirds of the reviewed patients. Most of the DRPs were related to medication reconciliation, dose or interactions.
This is in line with a newly published study from Aalborg University Hospital 50 in which 22 discharged patients were audited. In their study, they found DRPs in 20 (91%) of the patients including DRPs in SMR, dispensing errors at hospital and missing electronic prescriptions in SMR. The handling of these DRPs was very time-consuming for the healthcare professionals in both healthcare sectors, therefore; they recommend more resources to prevent DRPs instead of solving the single problems – for instance by practising cross-sectoral interdisciplinary ‘Shared Care’. 50
It was not possible for the pharmacist to be physically present at the hospital and in the GP at the same time. Therefore, it was not possible to intervene at the hospital before discharge, so that for example all medication changes were described in the discharge letter. The pharmacist was physically present in the GP twice a week, and this part of the intervention was designed to follow-up on patients after their hospital contact aiming to clarify questions from the patients and identifying DRPs before they became huge problems.
In our study, we found that patients thought it was a good idea to be followed up by telephone after discharge; however, not everyone thought it was necessary for themselves. We did not see any particular relation between this opinion and, for example, age or the number of drugs, so from the pilot study, it is not possible to describe inclusion and exclusion criteria for the telephone follow-up.
A total of 87% of the people living in the specific municipality has low socioeconomic status due to low educational level, job situation and low income. 51 Low educational level and low income are also related to low health literacy, 52 therefore; it is assumed that many of the included patients have low socioeconomic status as well as low health literacy. Maybe that is why many of the included patients did not see their own need for a follow-up telephone call after discharge? People with higher health literacy have a greater ability to find, understand, and use information and services to inform health-related decisions and actions. 53
Interestingly; the pharmacist discovered DRPs as part of the follow-up telephone call in 30% of the cases. The follow-up telephone calls may prevent DRPs as well as extra and time-consuming 50 telephone calls to the GP and the hospital. To do so, we found that the timing of the follow-up telephone call was important and ideally should be done the day after discharge or as quickly thereafter.
Overall, the intervention in this study made sense to both healthcare sectors and patients and the overall design of the intervention was not changed after the pilot study; only the timing of the telephone call was specified. Therefore, the final version of the intervention included the following elements: medication history, medication reconciliation, SMR update, medication review, overview of medication changes and follow-up telephone calls after discharge. This is in line with previous published literature reviews in which elements like medication reconciliation, medication review, patient follow-up and physically presence at the GP were considered effective in optimizing patient medication.31,39,41,44 The shared employment and the unique access to health records in both healthcare sectors were the most different, innovative and value-creating elements in the identification and resolution of DRPs in cross-sectoral transitions.
The intervention was tested in a large GP Clinic with many different healthcare professionals employed; thus, the GPs were used to interdisciplinary work. It would be interesting to explore the acceptability of the intervention in GP Clinics with differing characteristics.
Strengths and limitations
This study has some strengths and limitations that merit further discussion.
The identification of evidence was performed by exploring the question: Which drug-related problems are seen in the transition of patients between healthcare sectors and how can a pharmacist intervention be used to solve some of these problems? The question was explored thoroughly from four points of view. Interview participants were selected with inspiration from the ‘Snowball’ principles, and it was considered a strength that the question has been explored from different perspectives; however, we only included participants from one GP and only two participants from the hospital. The experiences may have been different if more participants had been involved.
The intervention was developed before the new Medical Research Council (MRC) guidance 54 on complex interventions was published; thus, the former guidance on complex intervention research was used. 20 We refined the intervention once. According to the new guidance, it is important to revisit the core elements of the intervention and refine the intervention accordingly. 54
The intervention was developed based on no other theoretical basis than the concept of inter-disciplinary collaboration. The intervention may have been different if another theoretical approach had been used.
The intervention was developed from the findings through co-creation between pharmacists, doctors and a nurse. This was considered a strength as an intervention developed together with participation of both healthcare sectors and different professionals, may be more relevant and take the context into account. Ideally, patients are involved as research partners in the development of an intervention. 55 It was our ambition from the beginning to have a patient representative on board in the project group; however, we did not succeed with this. Patient and public involvement in research was new to the project group and we did not have any experience with user panels. Instead, we decided to explore the relevance of the follow-up telephone call by simply asking the patients. In this way, we gained knowledge of the issue from several patients instead of a single or two participants in a user panel.
In the intervention, we had an experienced pharmacist with a shared employment between the Hospital Pharmacy and the GP. As far as we know, this constellation has not been tested prior. The pharmacist was physically present at the GP twice a week in the acknowledgement of the importance of verbal inter-professional and face-to-face communication. 41
It was difficult to collect informed consent from referred patients at the GP. When the pharmacist was physically present at the GP is was often easier; however, many patients were referred without a physically meeting at the GP. Some were referred after a video consultation (popular during the COVID-19 pandemic) or after X-ray consultation. Since the pharmacist during the pilot study found many discrepancies between registered prescriptions and patients’ actual use of medication, it was considered relevant to keep this part of the intervention.
Conclusion
DRPs in cross-sectoral transitions are multifaceted and the experiences depend on the point of view. The cross-sectoral hospital pharmacist intervention identified and solved several DRPs; in this way, medication errors were avoided. The shared employment and the unique access to health records in both healthcare sectors were important in the identification and resolution of DRPs. The intervention made sense to both healthcare sectors and patients, and the overall design of the intervention was not changed after the pilot study. A feasibility test with focus on acceptability of the intervention in GP Clinics with differing characteristics is considered as the next step.
Supplemental Material
sj-docx-1-taw-10.1177_20420986231159221 – Supplemental material for Developing and piloting a cross-sectoral hospital pharmacist intervention for patients in transition between hospital and general practice
Supplemental material, sj-docx-1-taw-10.1177_20420986231159221 for Developing and piloting a cross-sectoral hospital pharmacist intervention for patients in transition between hospital and general practice by Charlotte Arp Sørensen, Linda Jeffery, Jannik Falhof, Philipp Harbig, Klaus Roelsgaard, Solveig Gram and Charlotte Olesen in Therapeutic Advances in Drug Safety
Supplemental Material
sj-docx-2-taw-10.1177_20420986231159221 – Supplemental material for Developing and piloting a cross-sectoral hospital pharmacist intervention for patients in transition between hospital and general practice
Supplemental material, sj-docx-2-taw-10.1177_20420986231159221 for Developing and piloting a cross-sectoral hospital pharmacist intervention for patients in transition between hospital and general practice by Charlotte Arp Sørensen, Linda Jeffery, Jannik Falhof, Philipp Harbig, Klaus Roelsgaard, Solveig Gram and Charlotte Olesen in Therapeutic Advances in Drug Safety
Supplemental Material
sj-docx-3-taw-10.1177_20420986231159221 – Supplemental material for Developing and piloting a cross-sectoral hospital pharmacist intervention for patients in transition between hospital and general practice
Supplemental material, sj-docx-3-taw-10.1177_20420986231159221 for Developing and piloting a cross-sectoral hospital pharmacist intervention for patients in transition between hospital and general practice by Charlotte Arp Sørensen, Linda Jeffery, Jannik Falhof, Philipp Harbig, Klaus Roelsgaard, Solveig Gram and Charlotte Olesen in Therapeutic Advances in Drug Safety
Supplemental Material
sj-docx-4-taw-10.1177_20420986231159221 – Supplemental material for Developing and piloting a cross-sectoral hospital pharmacist intervention for patients in transition between hospital and general practice
Supplemental material, sj-docx-4-taw-10.1177_20420986231159221 for Developing and piloting a cross-sectoral hospital pharmacist intervention for patients in transition between hospital and general practice by Charlotte Arp Sørensen, Linda Jeffery, Jannik Falhof, Philipp Harbig, Klaus Roelsgaard, Solveig Gram and Charlotte Olesen in Therapeutic Advances in Drug Safety
Supplemental Material
sj-docx-5-taw-10.1177_20420986231159221 – Supplemental material for Developing and piloting a cross-sectoral hospital pharmacist intervention for patients in transition between hospital and general practice
Supplemental material, sj-docx-5-taw-10.1177_20420986231159221 for Developing and piloting a cross-sectoral hospital pharmacist intervention for patients in transition between hospital and general practice by Charlotte Arp Sørensen, Linda Jeffery, Jannik Falhof, Philipp Harbig, Klaus Roelsgaard, Solveig Gram and Charlotte Olesen in Therapeutic Advances in Drug Safety
Supplemental Material
sj-docx-6-taw-10.1177_20420986231159221 – Supplemental material for Developing and piloting a cross-sectoral hospital pharmacist intervention for patients in transition between hospital and general practice
Supplemental material, sj-docx-6-taw-10.1177_20420986231159221 for Developing and piloting a cross-sectoral hospital pharmacist intervention for patients in transition between hospital and general practice by Charlotte Arp Sørensen, Linda Jeffery, Jannik Falhof, Philipp Harbig, Klaus Roelsgaard, Solveig Gram and Charlotte Olesen in Therapeutic Advances in Drug Safety
Footnotes
Acknowledgements
This study could not have been performed without the participation of patients and staff in the primary and the secondary healthcare sector. Thanks to the General Practice in Grenaa (DK) and Randers Regional Hospital (DK) for active participation in the study phases. Thanks also must be given to the steering committee for their support throughout the study. Thanks to the funders for seeing the potential of the study.
Declarations
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
