Abstract
Anaplastic large cell lymphoma (BIA-ALCL) associated with rough textured breast implants was first reported in 1997. It is a non-Hodgkin’s lymphoma originating from a T lymphocyte which occurs on average 10.9 years after placement of the breast implant. BIA-ALCL mainly manifests as a periprosthetic seroma or a mass adjacent to the implant. To our knowledge, we describe the first case of BIA-ALCL with initial presentation by indurate erythematous plates located in both breasts and the progressive appearance of several asymptomatic metastatic nodular lesions that have been appearing on the right arm some weeks later.
Keywords
Introduction
Anaplastic large cell lymphoma associated with rough textured breast implants (BIA-ALCL) was first reported in 1997. It is a non-Hodgkin’s lymphoma originating from a T lymphocyte which occurs on average 10.9 years after placement of the breast implant. Its incidence is rare, estimated at 1 case per 500,000 to 3 million women with breast implants. The median age is 50 years old.1–3 BIA-ALCL mainly manifests as a periprosthetic seroma or a mass adjacent to the implant. Clinically, in more than half of patients, rapid and painless swelling of the chest occurs. Skin signs are rare but may be the first manifestation of the disease.
Case report
A 69-year-old woman came for consultation following indurate and erythematous plates on the infero-internal side of the two breasts more pronounced on the right than on the left (Figure 1) and the progressive appearance of several asymptomatic nodular lesions that have been appearing on the right arm and forearm for several weeks (Figure 2). The patient is in excellent condition and is not taking any medication. In her medical and surgical history, 30 years ago, she presented an infiltrating ductal carcinoma of grade II with lymph node invasion of the right breast treated by mammectomy, chemotherapy, radiotherapy, and hormone therapy. One year later, she got a breast reconstruction with textured implant. Twenty-five years later, for esthetic reasons, she benefited from a change in her right breast prosthesis with the fitting of another prosthesis on the left. These two new prostheses are also textured. The histology of an arm nodule shows an invasion of large pseudo-Sternberg-like tumor cells (Figure 3). The CD30 marker is positive (Figure 4). The T markers (CD2, CD5, CD3) as well as the expression of cytotoxic proteins (Granzyme B, perforin) are negative. ALK (anaplasic lymphom kinase) is negative. It is a CD 30 positive lymphoproliferative disorder with ALK negative. A mammogram shows a fleshy peri-prosthetic tumor mass of 43 mm at the right internal equator whose ponction-biopsy reveals the presence of a T-type monoclonal rearrangement. The FISH does not detect any translocation involving the ALK gene in 2p23 or the IRF4/DUSP22 gene in 6p25. The PET-CT shows an image of lymphoma, mainly of the right breast and the right arm with digestive extension and of the left lower limb. The diagnosis of anaplastic large cell CD 30+ Alk lymphoma—stage IV from a right breast implant is set down. The patient is treated with chemotherapy and surgical removal of breast implants with negative margins. The patient has been in complete remission 3 years later.

Indurate and erythematous plates on the infero-internal side of the two breasts.
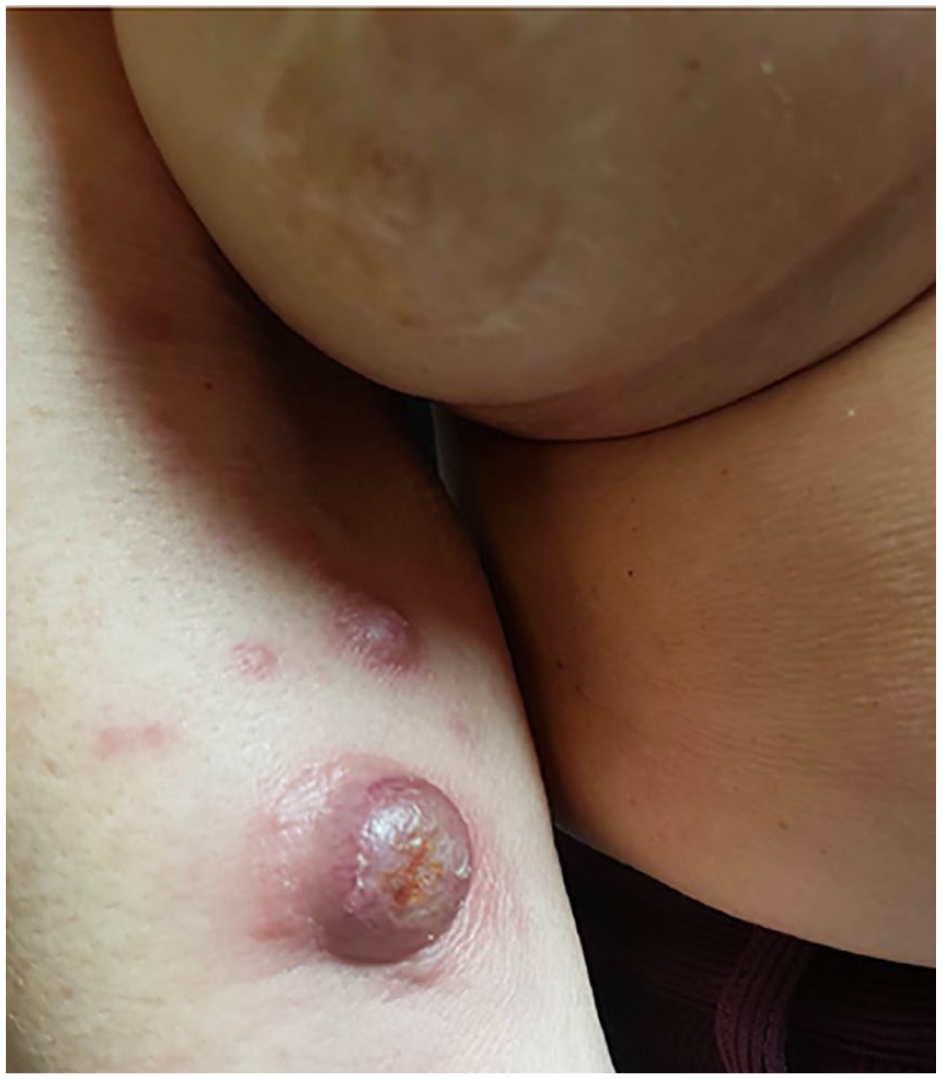
Asymptomatic nodular lesions of the right arm and forearm.

Invasion of large pseudo-Sternberg-like tumor cells (Hematoxyline Eosine ×400).

The positive CD30 marker (Immunoperoxydace CD30 ×200).
Discussion
The aetiology of BIA-ALCL is unclear. It may be found in patients with rough-textured breast implants. These implants have concavities which predispose to chronic inflammatory stimulation of the textured surface itself, ultimately causing lymphoma. Furthermore, there is no difference between implants made of silicone and implants filled with saline or between patients who have undergone reconstructive surgery after breast neoplasia or for aesthetic reasons. 4 BIA-ALCL is not a disease of the breast parenchyma, it comes in the form of a peri-implant seroma in two thirds of the cases and in the form of a mass derived from the fibrous capsule in the remaining third. 5 The most common symptoms are swelling of the chest, pruritus, pain, capsular contracture manifested by abnormal tension.5–7 Some cases have skin signs along with a seroma and/or a lump. The localized skin manifestations on the breasts and chest are mainly indurate erythematous plates, urticary or eczema flares, papular-nodular lesions as well as skin erosions or ulcers. 5 Finally, cutaneous T cell lymphomas (CTCL), cases of mycosis fungoides, and Sézary syndrome have been reported in patients with breast implants. 8 Lymph node invasion is present in 30% of patients including axillary lymphadenopathy. Twenty percent of the patients show a real lymph node invasion from a distance, 90% of which are from the axillary site. Metastases are very rare.1–3 To our knowledge, we describe the first case of BIA-ALCL with initial presentation by indurate erythematous plates located in both breasts accompanied some weeks later by asymptomatic metastatic skin nodules on the homolateral arm to the primary tumor. During diagnosis, the majority of the cases described are at the stage limited to the seroma, that is to say confined to the space surrounding the prosthesis. Recently, a TNM classification separates a very low risk group characterized by a localized disease limited to the seroma and a higher risk group characterized by an infiltration beyond the fibrous capsule in the breast tissue or a breast mass. 9 In the low-risk group, treatment consists of complete surgical excision of the implant and capsule with negative margins. A radical mastectomy and a sentinel lymph node biopsy are not indicated. If there are several lymph node metastases, total axillary dissection is then recommended. Chemotherapy or radiotherapy is only recommended in advanced or metastatic cases after consulting the oncologist. The prognosis of the disease usually depends on the extent of the disease at the time of diagnosis and all relapses after any treatment have occurred in the first 3 years. This highlights the importance of early diagnosis and the fact that complete surgical excision is essential. The risk of recurrence is uncertain. Replacement with a smooth prosthesis or with autologous tissue is recommended, replacement with a textured prosthesis should preferably be avoided. In conclusion, clinicians should include BIA-ALCL in the differential diagnosis of breast erythema in a woman with an implant. In conclusion, clinicians have an important role to play for the diagnostic because the prognosis is excellent if diagnosed at an early stage.
Footnotes
Author contributions
The content of the paper “Breast erythema and nodular skin metastasis as the first manifestation of breast implant-associated anaplastic large cell lymphoma” N Ducastel, MD, I Cimpean, MD, I Theate, MD, O Vanhooteghem, MD, has not been published or submitted for publication elsewhere. All authors have read and approved the manuscript. In keeping with the latest guidelines of the International Committee of Medical Journal Editors, each author’s contribution to the paper is to be quantified.
Declaration of conflicting interest
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Informed consent
Patient give written informed consent to publish the case including clinical image (available on request).
