Abstract
Malignant mesothelioma is a rare and devastating form of cancer with an increasing economic burden. We sought to describe the direct cost burden of mesothelioma to the US health system. A systematic literature review was performed to locate published estimates of the medical cost of mesothelioma. In addition, we performed an analysis of hospital discharge data from the National Inpatient Sample, Healthcare Cost and Utilization Project, Agency for Healthcare Research and Quality. We also reviewed publicly available legal settlements. We found that published estimates of the cost of medical care for mesothelioma are sparse, and differ with respect to nation, timeframe, and types of cost included. For the year 2014 in the United States, we estimated a mean cost per mesothelioma hospitalization of US$24,124 (95% confidence interval: US$20,819–US$28,983) and a total cost for hospital care of US$44,214,835. In conclusion, we found that reports describing the direct medical cost of care for mesothelioma in the United States are lacking, yet the per-patient cost of care is substantial, as evidenced by analyses of inpatient care and legal settlements.
Introduction
Mesothelioma is a rare and fatal form of cancer that is linked to occupational exposure to asbestos. The disease arises from the mesothelial cells of the pleura, but can also occur in the pericardium, peritoneum, and tunica vaginalis testis.1,2 Asbestos mining and use in the United States peaked in 1973 and started to decline over the next two decades. 3 Mining of asbestos finally ended in the United States in 2002. 3
Approximately 2,750 mesothelioma deaths occurred annually in the United States during 2011–2015. 4 Roughly 80% of these deaths were among males, and approximately 95% were Caucasians. 4 The prevalence of mesothelioma in the United States is estimated to have peaked around 2007, and is projected to decline over the next several decades.5,6
Mesothelioma has a very poor prognosis. The latency between development of mesothelioma after exposure to asbestos ranges from 20 to 50 years, but some cases occur as late as 70 years after.3,7,8 A higher intensity of exposure is associated with a shorter latency period. 9 The median age of diagnosis for mesothelioma is approximately 72 years.10,11 Patients with mesothelioma have a mean survival of approximately 1 year after diagnosis.10,11 Diagnosis is often made at an advanced stage, which is reflected in the low survival rates. 12 While a small subgroup of patients may survive for many years beyond diagnosis, for most patients, the prognosis is bleak with only limited treatment options available to mitigate the cancer.
Treatment options generally depend upon the patient’s clinical status and prognosis upon being diagnosed. First-line chemotherapy includes different combinations and regimens of the following chemotherapy agents: pemetrexed, cisplatin, bevacizumab, carboplatin, gemcitabine, or vinorelbine. 11 For patients who are suitable candidates, surgical procedures might include pleurectomy/decortication (P/D) or extrapleural pneumonectomy (EPP).11,13 Patients who receive either P/D or EPP are also recommended to have a mediastinal node dissection. 11 Radiation therapy may also be used in patients postoperatively after EPP, for palliative care, or as prophylaxis to prevent surgical tract recurrence. 11 Due to the advanced stage of disease at diagnosis, treatment options, which are often very costly, include extensive surgery, systemic therapy, and radiation therapy.
Given the long latency period of the disease, mesothelioma cases will continue to develop in the United States over the next several decades, adding to the cost burden of cancer care overall. Published data regarding the direct medical costs of mesothelioma in the United States are lacking. The objective of this study was to describe the direct cost burden of mesothelioma to the US health system.
Material and methods
Literature review
A systematic literature search was performed using PubMed and Embase, the International Society for Pharmaco‑economics and Outcomes Research (ISPOR) scientific presentation database, and the International Pharmaceutical Abstracts (IPA) database to locate published estimates of the cost of mesothelioma in the United States and throughout the world. The review of PubMed and Embase consisted of the search term “mesothelioma AND cost.” The review of the ISPOR scientific presentation database consisted of the search term “mesothelioma” in abstracts. The review of the IPA database consisted of the search terms “mesothelioma AND cost.” Articles and presentations that only discussed the cost of specific medications, chemotherapy, or surgery were excluded.
Inpatient cost burden
We analyzed the National Inpatient Sample (NIS), Healthcare Cost and Utilization Project (HCUP; US Agency for Healthcare Research and Quality) for the year of 2014 using the International Classification of Diseases, 9th Revision (ICD-9) diagnosis codes of 163.0 (malignant neoplasm of parietal pleura), 163.1 (malignant neoplasm of visceral pleura), 163.8 (malignant neoplasm of other specified sites of pleura), and 163.9 (malignant neoplasm of pleura unspecified). 14 We determined overall and mean costs and mean length of stay for hospitalizations having a primary diagnosis of mesothelioma, overall and according to patient demographics. We also evaluated the cost of procedures performed during a hospital stay, which included 32.30 video-assisted thoracic surgery (VATS), 32.50 EPP, 34.51 P/D, 33.20 thoracoscopic biopsy, 34.20 thoracoscopic pleural biopsy, and 34.91 thoracentesis.
Cost of chemotherapy
The cost of chemotherapy was estimated for two common first-line chemotherapy regimens, as recommended by the National Comprehensive Cancer Network Clinical Practice Guidelines in Oncology (NCCN Guidelines) for malignant pleural mesothelioma. 11 The first chemotherapy regimen considered was pemetrexed 500 mg/m2 on day 1, plus cisplatin 75 mg/m2 on day 1, administered every 3 weeks. The second chemotherapy regimen considered was both drugs and dosages included in the first regimen plus bevacizumab 15 mg/kg administered on day 1, administered every 3 weeks. The cost of chemotherapy was calculated using the wholesale acquisition cost (WAC) for 2017. 15 Dosing was calculated using a patient weight of 72 kg and a body surface area (BSA) of 2 m2 which assumed a typical BSA for a male cancer patient of 1.91 m2 and rounding up to account for non-used chemotherapy from open vials which must be discarded. 16 Costs were reported in 2017 dollars.
LexisNexis academic review
To supplement our analyses of direct medical costs, we also reviewed published settlements from mesothelioma legal cases in the United States, using the cataloging resource LexisNexis Academic to find legal settlements and lawsuits where the total estimated direct cost of care for mesothelioma was reported. Our query consisted of three different search terms: “mesothelioma,” “mesothelioma treatment costs,” and “mesothelioma medical expenses.” For the legal settlements and lawsuits identified, we only considered the amount of monetary award that was specifically for medical expenses and omitted amounts for non-medical damages.
Results
The systematic literature review of PubMed returned 167 hits for the search terms “mesothelioma AND cost,” with five studies meeting our inclusion criteria.17–21 The review of the ISPOR scientific presentation database returned 11 matches for the search term “mesothelioma” of which two were applicable.22,23 The review of the IPA database returned six matches for the search terms “mesothelioma AND cost,” but none were applicable. The review of Embase returned 349 matches, and two additional results were applicable.24,25 In total, we identified nine relevant articles, abstracts, and presentations regarding the direct medical cost of mesothelioma.
We identified 1 abstract which addressed the cost of mesothelioma-related care by Babcock et al. which examined overall and per episode costs for mesothelioma for the inpatient setting in the United States during 2012. 23 They reported an aggregate US hospital cost of US$50,473,622, and a mean per-episode cost of US$25,566, which differed for hospitalizations involving a major procedure (mean cost of US$30,734) versus those without a major procedure (US$13,493). 23
We identified several other cost of illness studies conducted in other nations. Zocchetti examined the annual economic impact in Italy where the average pleural mesothelioma case costs approximately €67,000 overall, with €37,000 spent on medication. 18 Serrier et al. described the social cost of occupational respiratory cancers in France during 2010, reporting an average annual direct cost per patient for mesothelioma of €33,422 overall, 19 of which €19,500 was for hospital care.
Gomez et al. examined direct medical cost for job-related cancers in Spain in 2008, 20 finding that total annual hospital costs for males with mesothelioma were €498,110, and total hospital costs for females were €66,766. Cost per hospitalization, however, was similar between males and females (€6,731 vs €6,676). Among cost components, specialized care costs accounted for €566,292, primary care costs were €20,386, pharmacy costs were €294,472, and the overall annual sanitary cost for mesothelioma was €881,150.56. 20 Lee et al. estimated the financial savings of preventing occupational cancer from the perspective of the Taiwanese health system during 1997–2005, finding that averting a case of mesothelioma would yield an average lifetime cost savings of US$14,900. 17 Soeberg et al. 25 found that direct medical costs in Taiwan were approximately US$18,812 following a diagnosis of malignant pleural mesothelioma; whereas the direct medical costs in Australia were approximately US$20,573. 25 Watterson et al. 21 reported mesothelioma costs in Scotland for the year 2000 as £942,038, with inpatient care accounting for £906,965 and day cases accounting for £35,073 of total spending. Tournier et al. 22 estimated malignant pleural mesothelioma costs in France for 2011 and 2012, finding that the total cost during these 2 years was €52,000,000, with medications comprising 31% of total cost, while diagnosis-related group tariffs represented 66% of total expenditure, with a mean cost per patient of €27,624. 22
Ak et al. determined the lifetime cost by treatment regimen and prognosis for patients with malignant pleural mesothelioma in Turkey during 2005–2014. 24 The average cost for patients who received basic supportive care was US$1,355 while the average cost for patients who received only chemotherapy was US$6,595. 24 The average cost for patients who received both chemotherapy and radiation was US$8,962. 24 For patients receiving P/D, chemotherapy, and radiation the average cost was US$11,691, while mean cost for patients receiving EPP, chemotherapy, and radiation was US$13,788. 24
Our analysis of the 2014 NIS identified 1,675 hospital discharges in the United States having a primary diagnosis of mesothelioma (Table 1). The estimated aggregate US hospital inpatient cost associated with a primary diagnosis of mesothelioma in 2014 was US$41,709,687. The mean cost per hospitalization was US$24,901 (95% confidence interval (CI): US$20,819–US$28,983) and the mean length of stay was 7.7 days (95% CI: 7.0–8.4). The Northeast had the highest mean cost per region at US$33,396 per episode (95% CI: US$23,045–US$43,748), and the Midwest had the lowest mean cost of US$18,206 per episode (95% CI: US$15,523–US$20,888). Patients aged 65–84 years comprised two-thirds of the discharges. Patients 45-64 years of age incurred the highest mean cost per episode (US$30,845; 95% CI: US$22,431–US$39,258), while the lowest mean cost per episode was among patients aged 85 years and older (US$15,534; 95% CI: US$12,717–US$18,352). Mean cost per episode was similar among Medicare, private, and other insurance types; except for Medicaid which accounted for a lesser number of cases (n = 60) and a lower mean cost per episode (US$18,754; 95% CI: US$14,803–US$22,706). The mean cost per episode was substantially greater among hospitalizations associated with a mesothelioma-related procedure (Table 1) (US$29,344; 95% CI: US$24,349–US$34,340), as compared with hospitalizations where such procedures were not performed (US$10,263; 95% CI: US$8579– US$11,946). The mean cost per procedure ranged from US$16,089 for drainage of pleural cavity (95% CI: US$12,883–US$19,296) to US$62,408 for pneumonectomy, NOS (95% CI: US$48,385–US$76,431). Higher mean costs per stay were generally associated with longer lengths of stay (Table 2).
Mean and total hospital expenditures for mesothelioma in the United States, 2014.
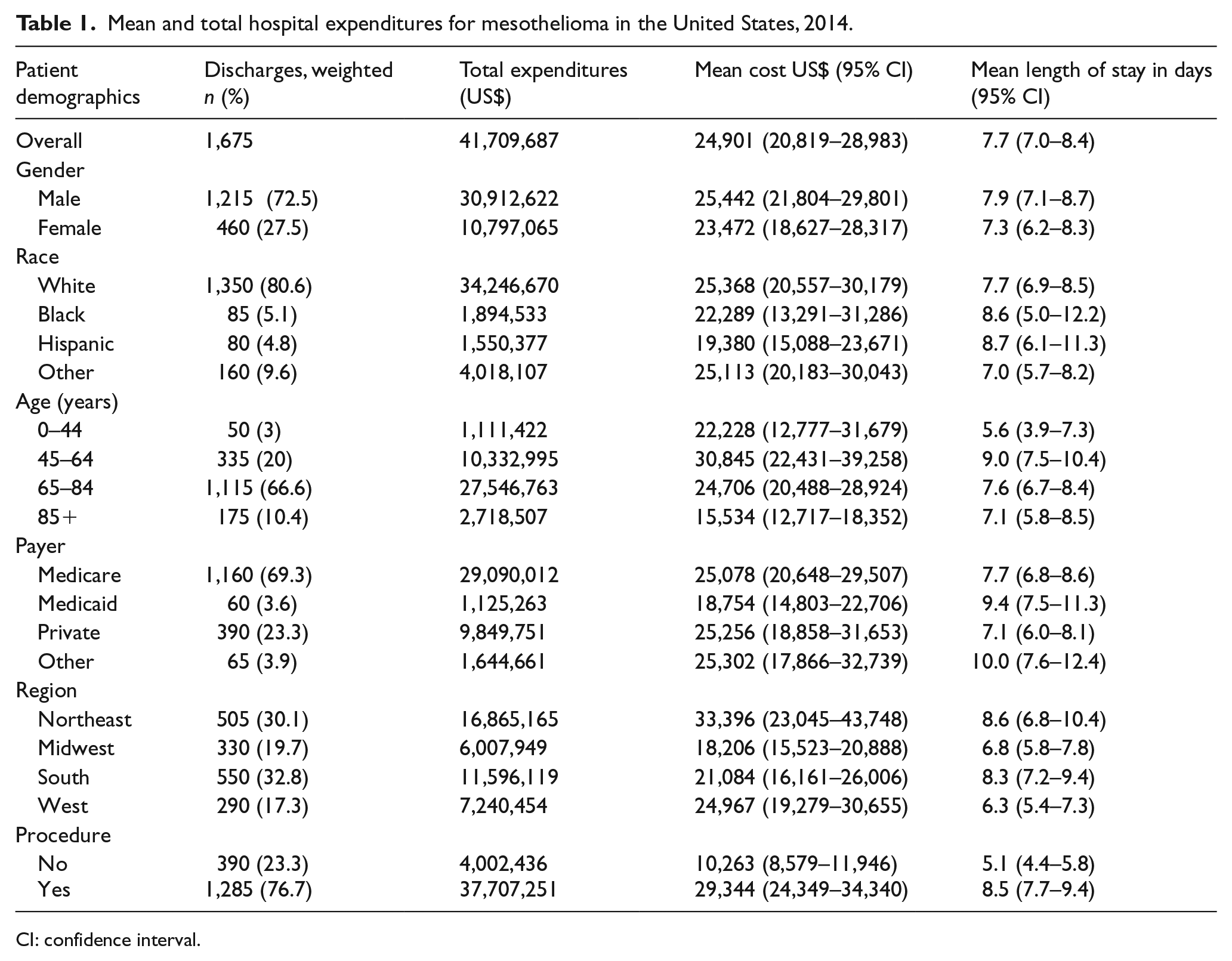
CI: confidence interval.
Mean hospital cost and LOS for mesothelioma-specific medical procedures in the United States, 2014.

LOS: length of stay; ICD-9: International Classification of Diseases, 9th Revision; CI: confidence interval.
The cost of chemotherapy was estimated considering a first-line regimen with pemetrexed plus cisplatin for six cycles with standard dosing per NCCN guidelines, 11 assuming a male patient weighing 72 kg and having a BSA of 1.91 m2 (Table 3). Drug costs were derived from published WAC for 2017. Given these assumptions, the total cost of chemotherapy was estimated as US$38,779. If the patient also received bevacizumab (as recommended for unresectable disease), 11 the chemotherapy regimen cost would increase to US$87,741. These figures do not include facility costs or management of toxicity.
Cost of typical chemotherapy regimen for mesothelioma.

WAC: wholesale acquisition cost; BSA: body surface area.
Assumes patient weight of 72 kg and a BSA of 1.91 m2.
Our review of LexisNexis Academic returned 20 relevant legal cases describing monetary awards associated with mesothelioma (Table 4). Of these cases, 18 patients had careers that exposed them to asbestos while 2 had secondary exposure. In reviewing these reports, we were often unable to distinguish cost of care provided from patient out-of-pocket expenditures. Six of the cases included monetary awards to the patient for future medical expenses while 19 of the 20 cases detailed monetary awards for past medical expenses. The monetary awards for total medical expenses ranged from US$113,594 to US$900,000.
Example monetary awards for mesothelioma cases.

Represents award for future medical expense in addition to past medical expense.
Secondary exposure.
Discussion
Mesothelioma is a rare yet costly disease. However, data describing the direct costs of care in the United States for the treatment of mesothelioma are lacking, while recent reports from other countries are also scant. A study of the cost of mesothelioma in Italy during 2002–2015 estimated the per patient cost to be €67,000 euros (approximately US$73,700 in 2015 dollars). The average annual per patient cost burden of mesothelioma in France was estimated at €33,422 (approximately US US$40,899 in 2010 dollars). 20 These reports suggest that the cost of care for mesothelioma is comparable to costs of care for other respiratory cancers. For example, annual costs of initial care for lung cancer have been estimated at US$72,639 among non-senior adults (2010 dollars). 26 Patients with mesothelioma who undergo surgical procedures incur higher costs of care. For such patients, in our analysis we estimated an average annual cost of inpatient care of US$29,344 for 2014. Data from the US Medicare population indicate that approximately 30% of mesothelioma patients underwent a surgical procedure during 2005–2009. 27 Although surgical options are listed as a treatment option in current guidelines, the data related to the impact of surgery on health outcome is limited. 11 Taking this into account in combination with the high cost of care for surgical procedures, future studies might assess the cost effectiveness of these options. Radiation therapy may also be utilized in patients with mesothelioma. An analysis of data from the Medicare Surveillance, Epidemiology, and End Results (SEER) program reported a median cost of approximately US$9,000 (in 2009 dollars) per course for a typical patient with lung cancer. 28
Our analysis of the NIS yielded an estimated total annual hospital cost for mesothelioma of US$41,709,687, representing 1,675 care episodes during 2014. Medicare was responsible for approximately 70% of these inpatient costs, given the predominance of diagnosis at older age. Inpatient costs for those age 85 years and older were substantially lower than for other age groups, which may be potentially due to less aggressive care and surgery being provided to older patients. These figures represent a small fraction of the total annual inpatient expenditure for lung malignancies, which totaled US$2,161,540,025 for 2014 (n = 123,365 inpatient episodes). 14 Despite its small contribution to the total cost of care for all lung malignancies, the per patient annual costs for mesothelioma care are on par with other cancer types and pose substantial cost burden on health plans. It is important to note that hospital discharges should not be interpreted as a true incidence rate, as a patient may experience multiple inpatient episodes in a given year.
Medications also contribute substantially to the cost burden of mesothelioma. We estimated the average direct medication cost for recommended chemotherapy for a typical male patient receiving 6 cycles. For patients with unresectable disease, adding bevacizumab to the regimen more than doubled the total medication cost, yielding an average estimated expense of US$87,741 per patient (2017 dollars). Continuing maintenance therapy with bevacizumab increased treatment cost by an estimated US$8,160 per month. In one trial, the addition of bevacizumab to pemetrexed/cisplatin increased overall survival by nearly 3 months. 29 Cost-effectiveness studies evaluating the value of bevacizumab in combination with pemetrexed/cisplatin or as maintenance therapy from the US payer perspective are lacking. One analysis determined that the routine addition of bevacizumab was not a cost-effective alternative in China. 30
While treatment advances are critically needed given the limitations of existing chemotherapeutic options, new agents will likely significantly increase per-patient medical costs. Outpatient medication costs for palliation and side-effect management are typically less consequential given the availability of relatively inexpensive generic formulations of vitamins, corticosteroids, and pain medications.
We were unable to locate any published data detailing the end-of-life costs for mesothelioma specifically. Zuckerman et al. determined the end-of-life costs for lung cancer, which can be applied as a best available comparator. Depending on the extent of use of hospice services and nursing home care, the mean total spending for end-of-life costs in lung cancer were estimated to range from US$44,504 to US$57,811. 31
Additional inferences regarding the total lifetime medical cost burden of mesothelioma might be drawn from examining awards associated with legal settlements. In researching publicly available records of mesothelioma-related lawsuits, we identified monetary awards for medical expenses ranging from US$113,595 to US$900,000. These figures are within the range of the costs we estimated for inpatient care and chemotherapy combined. Although these legal awards identified the portion of the total award specifically attributed to medical expenses, details regarding how these amounts were calculated were generally not provided. Litigation for mesothelioma is expected to continue as cases arise during the next several decades. The overall cost of litigation claims are projected to range between US$200 and US$265 billion after all cases are settled in the United States. 32
Our study attempted to determine average treatment costs for a typical patient with mesothelioma in the United States. We considered a health system perspective, and did not include indirect or intangible costs, which are important to the patient and broader perspectives. In addition, we did not attempt to adjust for cost inflation or specifically contrast cost estimates across countries, given the complexity of accounting for differing health care systems and treatment standards. Moreover, we were unable to identify published information describing the cost of outpatient care for mesothelioma in the United States.
Conclusion
Mesothelioma is a rare form of cancer having a very poor prognosis. The cost burden of the disease to the US health care system is limited due to its relatively low prevalence, and data describing the average costs of care are lacking. We estimated the total cost of inpatient care in the United States to be US$41,709,687 for 2014. Additional research is warranted to determine the total costs of treatment overall, including outpatient care, the cost of emerging medication therapies, and indirect and intangible costs.
Footnotes
Authors’ note
Research was performed at the College of Pharmacy of the University of Rhode Island.
Conflict of interest
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Grant support for this research was provided by Verastem Oncology. (Needham, MA).
