Abstract
Irritant contact dermatitis (ICD) is one of the most common occupational skin diseases, which is hard to differentiate from allergic contact dermatitis (ACD) clinically. Failure to identify the different forms of contact dermatitis can lead to suboptimal management of the patient, with long-term impacts on occupation and quality of life. We describe a case of ICD in a military healthcare personnel during the COVID-19 pandemic. He was exposed to butyl gloves from his protective equipment as well as frequent hand-washing during the COVID-19 period. The diagnostic approach to contact dermatitis as well as holistic management plan is further discussed in this case study.
Introduction
Irritant contact dermatitis (ICD) is one of the most commonly reported occupational skin diseases, which is hard to differentiate from allergic contact dermatitis (ACD) clinically. Failure to identify the different forms of contact dermatitis can lead to suboptimal treatment of the patient, with long-term impacts on occupation and quality of life.
In this case study, we describe an individual with overlapping clinical features of ACD and ICD to highlight the importance of detailed occupational history taking and patch testing in obtaining accurate diagnosis to guide treatment.
Case report
An 18-year-old male presented with an acute pruritic vesicular eruption over his bilateral hands during the first week of training as a combat medic. He has no significant history of eczema, atopy, or past medical history. The rash started over his distal forearms’ dorsal and volar aspect and extended bilaterally to his hands and fingers. The rash was intensely pruritic but not painful. His arms, face, trunk, and lower limbs were spared. The location of the rash did not follow a photo-distributed pattern. He was otherwise well with no fever or systemic symptoms.
Physical examination revealed vesicles with surrounding erythema and scaling areas localised and confined to the glove distribution (Figures 1 and 2). The rest of the photo-exposed areas including the scalp, face, and neck, were spared. His feet and ankles were unaffected. He had no stigmata of autoimmune disease. Vesicular eruption over the palmar aspect of right hand and wrist. Vesicular eruption over the palmar aspect of left hand and wrist.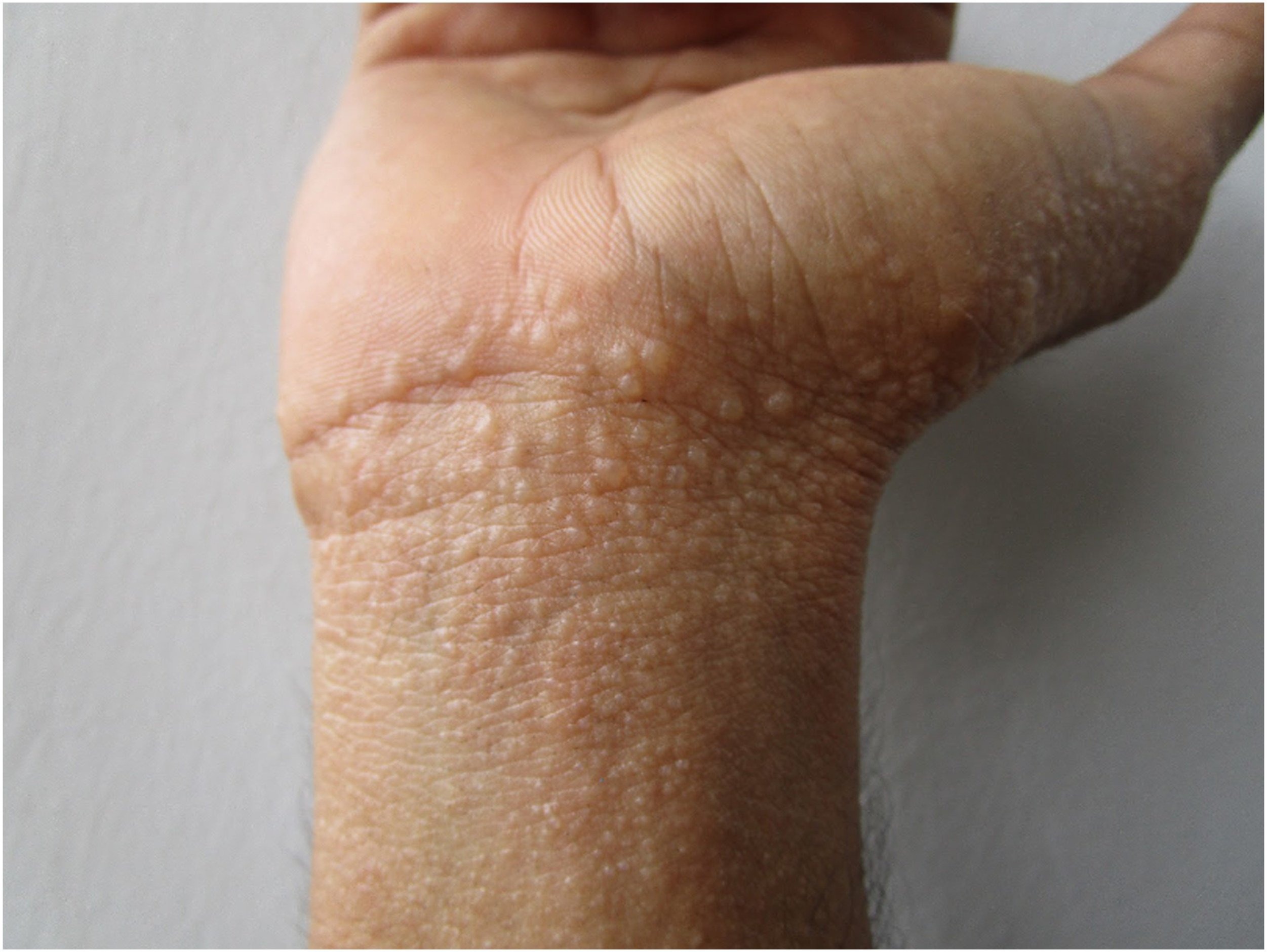

Exposures
The rash started within the first week of the medic’s training, coinciding with personal protective equipment (PPE), affecting his ability to continue training. His activities required repeated wear of rubber gloves, boots, mask, and protective uniform fatigues. He recalled wearing similar butyl gloves during his basic chemical defence training 5 months ago. He wore these gloves two to three times a day ranging from 30 minutes to 2 hours on each occasion. He developed an itch after day four of exposure, with rash onset on day five, before reporting to his superior on day six. He wore similar protective butyl coverings for his boots but without direct skin contact.
He reported more frequent usage of chlorhexidine hand wash coinciding with the COVID-19 period. He was also exposed to water and soap for training on decontamination procedures, once or twice a day for 30 minutes to 1 hour.
He has no hobbies, pets, or contact history with any new agents over the area of the rash. He has no history of rash to latex gloves, or rubber products like watch straps. As his rash started within the first week of exposure to the gloves, he could not ascertain if the rash improved on rest days.
Management
Topical hydrocortisone 1% cream and barrier protection using a cotton glove interface to his butyl gloves were prescribed by the Unit MO, with improvement of his rash. However, the rash did not resolve completely despite compliance with topical medication and a Dermatologist subsequently reviewed him. A combination of betamethasone valerate cream/fusidic acid and antihistamines was prescribed for itch relief. Suspension of exposure through discontinuation of direct contact with butyl gloves was reinforced. His rash resolved with desquamation without scarring within 1 week (Figure 3). He was concurrently referred to a tertiary dermatological institution for confirmation via a patch test. However, these services were unavailable at tertiary institutions during the COVID-19 pandemic. Resolution of rash with desquamation without scarring.
Fitness for work evaluation
The Dermatologist issued a memo to consider discontinuing further exposure to the butyl gloves and redeployment. The MO then reviewed the safety data sheets available, including the butyl gloves product inserts to identify possible allergens. It was concluded that while butyl compounds are inert and current literature did not report ACD to butyl gloves, the possibility of allergy to rubber accelerators could not be conclusively excluded. The unit MO and direct superior also reviewed the working conditions in the unit compound. Given the control measures put in place, a decision was made not for unit reassignment, and he retained his vocation as a combat medic. He remained free from recurrence with strict adherence to the control measures at his workplace.
Diagnosis
Three months after the initial onset of rashes, he was reviewed at a tertiary dermatological centre when patch test services resumed. A patch test on his butyl glove, other gloves, standard series, and rubber series (including rubber accelerators) returned negative. In this case, the diagnosis of ICD can be made based on the morphology and distribution of the rash being sharply confined only to the areas covered by gloves, negative patch test results, and improvement of the rash after removal of the irritant having been given time off work.
Discussion
Occupational skin diseases include a spectrum of conditions including ICD, ACD, skin cancers, infections, and injuries, amongst other skin diseases. ICD is one of the most commonly reported occupational skin diseases in Singapore and worldwide. 1
Given the non-specific pattern of hand dermatitis, it is often clinically difficult to differentiate between ICD and ACD. A detailed occupational and social history is required to identify the causative agent. In ICD, the rash is usually sharply confined to the areas of exposure as opposed to ACD, in which the rash often extends beyond the areas of exposure. In this case, the rash was confined to the areas of occlusive covering by gloves, pointing more towards ICD. Symptoms of ICD typically decrease in intensity after one or two days post removal of exposure to inciting irritant. Other differential diagnoses include photo-provocated dermatoses such as polymorphous light eruption, infections, or blistering dermatoses associated with autoimmune conditions. However, the history and physical examination excluded these differentials.
While a clinical diagnosis may suffice in most cases, a full evaluation with a patch test is warranted to confirm the diagnosis. It is important to identify if the patient is allergic to the butyl gloves or other allergens. 2 The rate of false negative results for patch testing is unknown but has been reported to occur in up to 30% of patients. 3 This can be due to a variety of factors. Patient factors include sweating, friction, and wet or loosened patches. Other factors include the failure to perform delayed readings, the use of immunosuppressants, systemic steroids, and the use of intermediate-strength topical corticosteroids. 4
The initial management of eliminating exposure to the suspected offending agent to prevent the recurrence of the rash is critical. Butyl gloves are made of inert compounds to act as protective barriers when handling hazardous material. However, there are rubber accelerators and compounds within the gloves during the manufacturing processes. Therefore, material data safety sheets are useful adjuncts for clinicians to make the correlation with the possible offending agent.
Long-term use of occlusive gloves has been reported to harm skin barrier function, especially when the occlusion is extensive and combined with exposure to skin irritants such as soap and detergents. 5 This leads to moisture trapped in the skin, resulting in softer skin that is more sensitive to irritants. 6 Hence, the cotton gloves served two functions. Firstly, they served as a barrier to prevent direct contact with the butyl gloves. Secondly, they soaked up water and sweat that may accumulate in the thick non-absorbent butyl gloves to prevent ICD. A double glove technique using a cotton liner can prevent the development of impaired skin barrier function caused by prolonged wearing of occlusive gloves. 7 Chemical additives in gloves, including rubber accelerators such as benzothiazoles and thiurams, may also contribute to skin irritation; and natural rubber latex gloves have been reported to cause occupational contact dermatitis and urticaria. 8
While butyl gloves are mainly used in specialised areas within the military, butyl can also be found in rubber boots and sporting equipment. The growing need for PPE usage in the COVID-19 pandemic necessitates increased awareness of contact dermatitis to PPE. There are increased numbers of healthcare workers and ancillary personnel working on the frontline who require donning of PPE. A similar phenomenon was also observed in the SARS epidemic according to a local study at the National Skin Centre Singapore. 9 Biosafety Level 3 precautions are also undertaken when handling samples associated with COVID-19 to reduce the risk of infection in healthcare workers. 10 This has led to the development of protective gloves used in biosafety cabinets for swabbing, made of heavy-duty rubber such as Neoprene. 11
It is important to recognise that latex or nitrile gloves used by healthcare workers may also result in contact dermatitis. There are numerous studies of healthcare workers affected by glove ACD due to prolonged exposure from regular use.12,13 Rubber accelerators such as carbamates, thiurams, 2-mercaptobenzothiazole, and 1,3-diphenyl guanidine are a few of the common contact allergens identified to be responsible allergens amongst healthcare workers as well. 14
Conclusion
Occupational history and a heightened awareness of the possibility of work-related illnesses were important factors in diagnosing contact dermatitis. Prompt suspension of exposure and institution of control measures helped to prevent recurrence.
Footnotes
Author contributions
CG wrote the first draft of the manuscript. All authors reviewed and edited the manuscript and approved the final version of the manuscript.
Availability of data and materials
Data sharing is not applicable to this article as no datasets were generated or analysed during the current study.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical approval
The Ministry of Health Holdings Pte Ltd, Singapore does not require ethical approval for reporting individual cases or case series for educational purposes.
Informed consent
Written informed consent was obtained from the patient for their anonymised information to be published in this article.
Trial registration
Not applicable.
