Abstract
With the advent of augmented reality (AR), our team developed a prototype teaching module using the abdominal hysterectomy as a case study for the teaching of in-depth pelvic anatomy and the steps for performing a hysterectomy. Through this interactive module, trainees will be able to identify and fill knowledge gaps in pelvic anatomy with the benefit of spatial visualisation, and familiarise themselves with the steps of performing a hysterectomy in a safe controlled setting.
The prototype teaching module has eight sections, each with its specific aims, objectives and multiple choice questions to assess the participant’s knowledge and understanding. The scores will be tabulated and a final report will be generated upon completion of the entire module. This includes the breakdown of the scores, mistakes identified and recommended suggestions to facilitate learning.
Following completion of the prototype teaching module, we aim to carry out a trial on our residents and assess its effects on self-perceived preparedness, knowledge and impact on training. We believe that this can translate to better awareness with reduced errors in surgery and ultimately better patient outcomes and safety.
Our new prototype teaching module promises to be well-received, relevant and will take our training to a new level. There is enormous potential in using AR technology to provide realistic, interactive and safe training and this can be harnessed for the future development of other modules in the O&G curriculum.
Recent advancements in technology have greatly influenced training in medicine. Both medical and surgical specialties have started to adapt to learning by using clinical applications employing both virtual reality (VR) and augmented reality (AR) technologies. This has not only led to enhancement of training but also to improvements in clinical outcomes. 1 While VR seeks to create a digital environment for the user, AR creates an additional digital overlay to provide virtual content onto the real environment to create an interactive field.2,3 As learning in the medical field can be complex and potentially occur in a risky and stressful real-life context, there are numerous potential benefits of training using AR technology by creating a virtual training environment closely simulating real-life conditions.2,4
Traditional teaching methods such as lectures and tutorials have proven to be effective, but in certain circumstances lack realism and reproducibility, particularly in imparting the practical aspects of surgical skills. The utilisation of technology to create a realistic surgical simulation module prior to operating theatre exposure may make the learning easier, safer and more realistic for our doctors in training. A systemic review of the published literature involving AR on surgical education conducted by Kovoor et al reported positively on the validity and effectiveness of AR to supplement surgical training irrespective of surgical specialty. 5
With the aims of enhancing our teaching processes as well as utilising the benefits of AR, our team developed a prototype teaching module by using the abdominal hysterectomy as a case study for the teaching of both in-depth pelvic anatomy as well as step-by-step training for performing an abdominal hysterectomy. An abdominal hysterectomy is one of the most common gynaecologic surgeries, and understanding of pelvic anatomy is crucial, hence making it an ideal choice for our prototype.
Through a collaboration with A*STAR Advanced Remanufacturing and Technology Centre (ARTC), a core workgroup was formed comprising of clinicians, AR developers and administrators. Through monthly meetings over a year, the clinicians provided the framework, relevant images and videos while the AR developers developed the virtual module. This process is summarised in Table 2. Reference regarding the steps of the hysterectomy was taken from the Mayo Clinic Manual of Pelvic Surgery. The user will first be assessed on his theoretical knowledge of pelvic anatomy and the steps of a hysterectomy before going on to visualise a simulated patient in the virtual operating theatre to perform the hysterectomy. This module was carried out using an iPad tablet and an apple pencil (Figure 1) due to its easy availability. Participant carrying out assignment with iPad and Apple pencil.
Sections covered under the module.


Interface of module.

Example of a question the participant has to answer during module.

Example of graphics used in module.
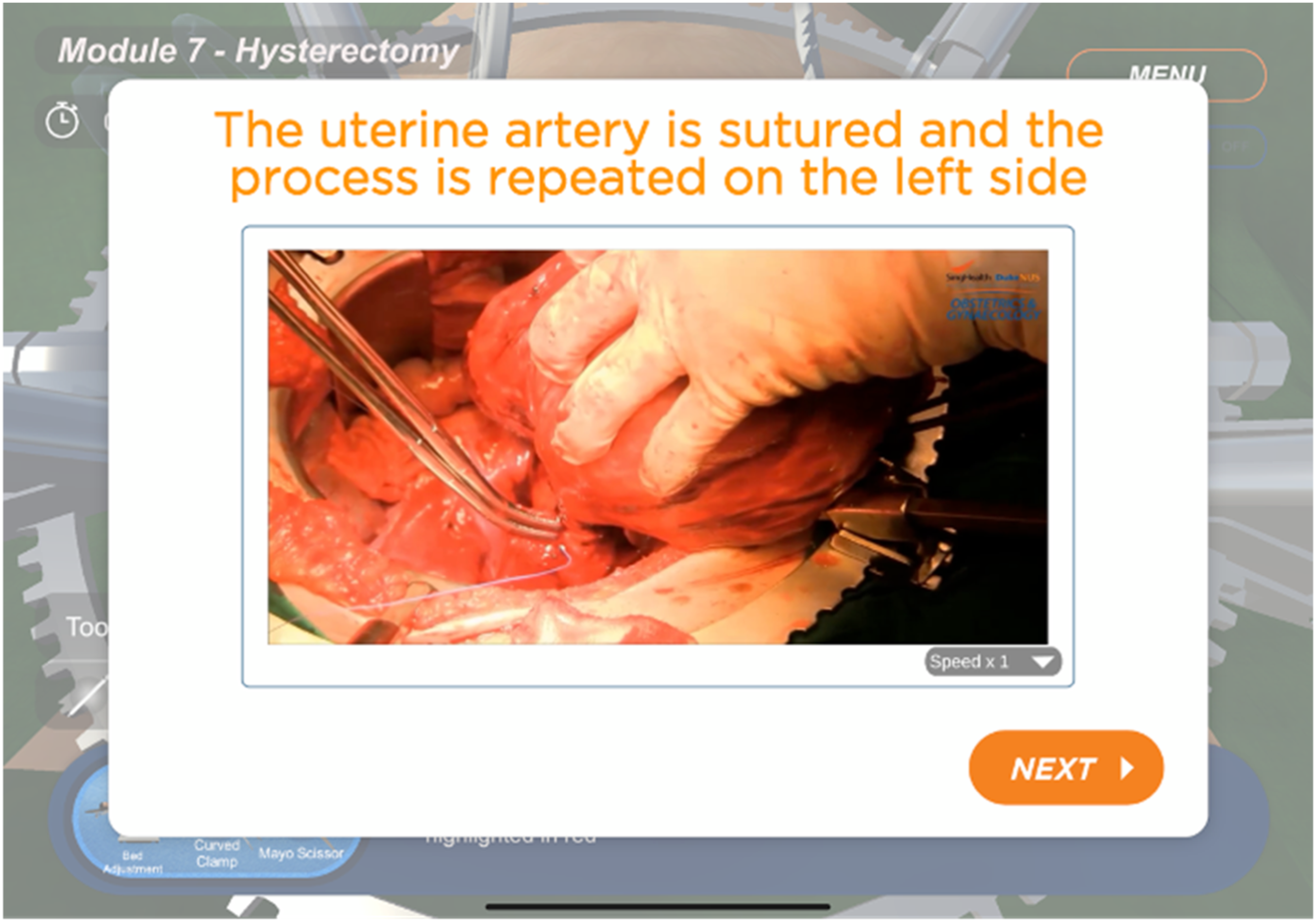
Example of instructional video filmed by our clinician faculty.
The scores from all eight modules will be tabulated and a final report will be generated upon completion. This report includes the breakdown of the scores obtained, mistakes identified with a clear explanation and recommended suggestions to facilitate learning. Any critical errors made would be heavily penalised and highlighted clearly to the participants, and explanations would be provided to strongly enforce the message in the hope of reducing the chances of these errors occurring in real-life. This feedback can be shared with the faculty mentors for further discussion and to fill the gaps in the learning.
After completion of the module, we aim to carry out a trial of this programme on our O&G residents, house officers and medical students and assess its effects on self-perceived preparedness, knowledge, impact on training and feasibility of future similar modules. Participants start by filling up a self-administered questionnaire to measure their confidence levels regarding their knowledge of female pelvic anatomy and performing the steps of an abdominal hysterectomy. They will then participate in the training module under an anonymous username, although they will be required to key in their current cohort level (for example O&G Resident Year 1, Medical Officer, Medical Student) so as to aid fairer analysis of score levels within their respective cohort. Following the completion of the module, they will complete the post participation questionnaire. Scores will then be tabulated and charted, and feedback regarding the module content and AR interface will be obtained.
With the incorporation of AR into our teaching module, trainees undergo an interactive and holistic learning experience with spatial assessment of anatomical structures, multi-modality assessment including theoretical and spatial assessment of surgical scenarios and instantaneous feedback with data-driven cloud analytics to identify and plug knowledge gaps. Such a module would ensure the streamlining of educational content and provide trainees with equal learning opportunities, especially with protected working hours for residents and heavy clinical responsibilities. Faculty members can also use these modules to assess and track residents’ progress, and reduce their teaching workload and resultant fatigue.
Despite an increase in existing clinical and education use of AR among different surgical specialties, there have been limited reported studies available in the field of Gynaecological surgery. Bourdel et al reported the first AR application for uterine surgery in 2015 where they developed an intra-operative myoma visualization system based on AR to enhance the surgical experience of a laparoscopic myomectomy. 6 A trial on 10 residents showed an improvement in the localization accuracy of myomas and they reported a potential for use of similar techniques in other gynaecologic surgeries. In 2018, Siff et al piloted an interactive holographic curriculum with the aid of AR to aid in the self-guided teaching of pelvic floor anatomy and surgical steps in the field of Urogynaecology. 7 They described high satisfaction levels amongst their trainees with majority keen to use the curriculum for surgical preparation but also reported considerations regarding cost effectiveness.
We believe the huge potential of AR technology can be effectively applied in the field of Obstetrics and Gynaecology training. Similar modules can be developed to cover increasingly challenging content such as pelvic lymph node dissection, or in obstetrics training to simulate performing a Caesarean section, assisted instrumental delivery and obstetrics emergency drills. Being the developer of these modules gives us the freedom to design programs that are customised to the needs of our residents and the environment they train in.
Process of developing the hysterectomy module.

Moving forward, assessment of outcomes from the module will need to be considered. In a review of 36 studies evaluating AR applications in healthcare education by Tang et al, attitudes towards AR being implemented in training programmes have been encouraging although evidence of its efficacy has yet to be established. 8 Similarly, Barsom et al reported huge potential for AR technology in training but noted a lack of follow-up studies to assess retention of skills, clinical improvement of trainees and effects on patient safety from AR applications. 3 We believe that with AR to facilitate training, this can translate to better awareness with reduced errors in surgery and ultimately better patient outcomes and safety. We aim to incorporate the use of mixed reality smartglasses such as the Microsoft HoloLens so as to provide better simulation and realistic 3D visualisation of gynaecological surgeries to further enhance the learning experience.
Our new prototype teaching module promises to be well-received, relevant and will take our training to a new level. There is enormous potential in using AR technology to provide realistic, interactive and safe training and this can be harnessed for the future development of other modules in the O&G curriculum.
Footnotes
Author contributions
JH reviewed the literature and co-wrote the manuscript with LX. MM reviewed the manuscript and supervised the entire project. WL and BH, together with JH, LX and MM, formed the team to develop the module.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
Name of Grant Agency: SingHealth Duke-NUS Obstetrics & Gynaecology Academic Clinical Program (ACP). Grant Name: Obstetrics & Gynaecology ACP Philanthropic Fund. Deadline of Grant Application: 1 Jan 2019 to 31 Dec 2019. *Amount: $50,000. Grant ref no.: 01/FY2018/EX/64-A105.

