Abstract
de Winter syndrome is a rare but important electrocardiographic pattern to recognize in patients presenting with chest pain. Under-recognition and delayed revascularization in patients with de Winter syndrome may lead to poor clinical outcomes. Despite increasing evidence of its association with total occlusion of the left anterior descending artery, the role of thrombolysis in the absence of percutaneous coronary intervention is not specifically addressed in recent international guidelines. Herein, we report a case of a 50-year-old gentleman with no known medical illness who presented with excruciating chest pain associated with diaphoresis, nausea, and reduced effort tolerance. Clinical examination revealed a distressed patient with bibasal crepitations with no other significant findings. The first ECG was sinus bradycardia with poor R-wave progression. ECG repeated 6 h later revealed de Winter syndrome. Within minutes, the patient developed sustained pulse ventricular tachycardia requiring synchronized cardioversion. The patient was intubated for impending cardiorespiratory failure. We took the pharmacoinvasive approach. The patient received thrombolytic therapy as percutaneous coronary intervention (PCI) was not available and transferring to the nearest cardiac center was not possible within the therapeutic window. He was then subsequently transferred to the nearest cardiac center post thrombolysis for PCI. We report this case study to highlight the importance of recognizing this STEMI-equivalent ECG pattern in patients presenting with chest pain, and call for randomized control trials to evaluate the effectiveness of thrombolytic therapy as an alternative emergent reperfusion strategy in de Winter syndrome in non-cardiac centers.
Introduction
Acute myocardial infarction continues to be the most common cause of death worldwide despite enormous efforts implemented for early detection and treatment. Prompt recognition of acute coronary occlusion and early reperfusion strategy reduce the mortality and morbidity in patients with ST-segment elevation myocardial infarction (STEMI). With more emerging evidence, in practice, the full spectrum of ECG indicating acute coronary occlusion requiring immediate reperfusion therapy goes beyond the current definition of STEMI. A recent retrospective case-control study showed patients with acute coronary occlusions without meeting ST-elevation criteria suffer double mortality due to delayed revascularization. 1 de Winter et al. (2008) described the STEMI—equivalent electrographic signs known as de Winter syndrome—as an unusual but important pattern to recognize in patients presenting with chest pain as it signifies total occlusion of the proximal left anterior descending coronary artery (LAD). 2 de Winter syndrome is characterized by loss of R waves in precordial leads associated with upsloping ST-segment depression at J point > 1 mm and tall positive symmetrical T waves. Despite emerging evidence showing association of de Winter ECG pattern with significant occlusion of LAD, at present, the optimal management of patients with de Winter’s variant ECG is not specifically addressed in the latest international guidelines. The European Society of Cardiology (ESC) suggested percutaneous coronary intervention (PCI) strategy in patients with a clinical concern of ongoing myocardial ischemia with atypical ECG patterns; however, with almost 80% of cardiovascular disease burden falling in low-to-middle-income countries, accessibility to PCI lab still poses a great challenge. 3 In this case report, we have recounted this rare STEMI-equivalent syndrome leading to sustained pulse ventricular tachycardia from a center with no interventional cardiology. This case report aims (1) to emphasize the importance of promptly recognizing de Winter pattern as a STEMI equivalent to advance the patient to a rapid reperfusion strategy and (2) call for more randomized controlled trials to further evaluate thrombolytic therapy as an alternative reperfusion strategy for de Winter syndrome to assist in formulating evidence-based guidelines for non-cardiac centers.
Case report
A 50-year-old gentleman, active smoker of 13 pack-years, with no known medical illness presented with left-sided chest pain with a pain score of 9/10 for one hour, associated with diaphoresis, shortness of breath, and nausea. He also complained of having reduced effort tolerance for the past 6 months. The patient denied any other significant symptoms. Initial clinical examination revealed the gentleman was in severe distress. Vital signs were as follows: blood pressure, 98/65 mmHg; pulse, 84 beats/min; and respiration, 22 breaths/min. Pulmonary examination revealed bibasal crepitations, and cardiac examination was unremarkable with normal heart sounds and regular rate and rhythm. JVP was not raised, and there was no peripheral edema. His initial ECG upon admission (Figure 1) showed sinus bradycardia and poor R-wave progression. The patient was given sublingual glyceryl trinitrate, T aspirin 300 mg, T Plavix 300 mg, and subcutaneous fondaparinux 2.5 mg. shows ECG upon admission when patient presented with chest pain (Pic 1) and 6 h later (Pic 2). Pic 2 shows de Winter syndrome.
The subsequent ECG (Figure 2) done 6 h later due to persistent chest pain showed de Winter Syndrome-upslopingST-segment depression over V1-V6 at J point >1 mm; T inversion over lead II, III, and AFV; positive symmetrical T waves in precordial leads; and poor R-wave progression. Within minutes, the cardiac monitored showed sustained pulse ventricular tachycardia (Figure 3). After giving premedication, the patient was given synchronized cardioversion x 1 using 100 J which successfully reverted to sinus rhythm. Given worsening respiratory distress, the patient was intubated for impending cardiorespiratory failure. Post intubation, the patient was hemodynamically supported with single inotropic support. We took the pharmacoinvasive approach. The patient received thrombolytic therapy (methylase) as primary PCI was not available and the transport to the nearest cardiac center outlasted the recommended delay. Post thrombolysis, the ECG (Pic 4) did not show complete resolution, and the patient was urgently transported to the cardiac center for percutaneous coronary intervention. (Table 1)

shows ventricular tachycardia captured on cardiac monitoring (Pic 3) and ECG (Pic 4) post thrombolysis.
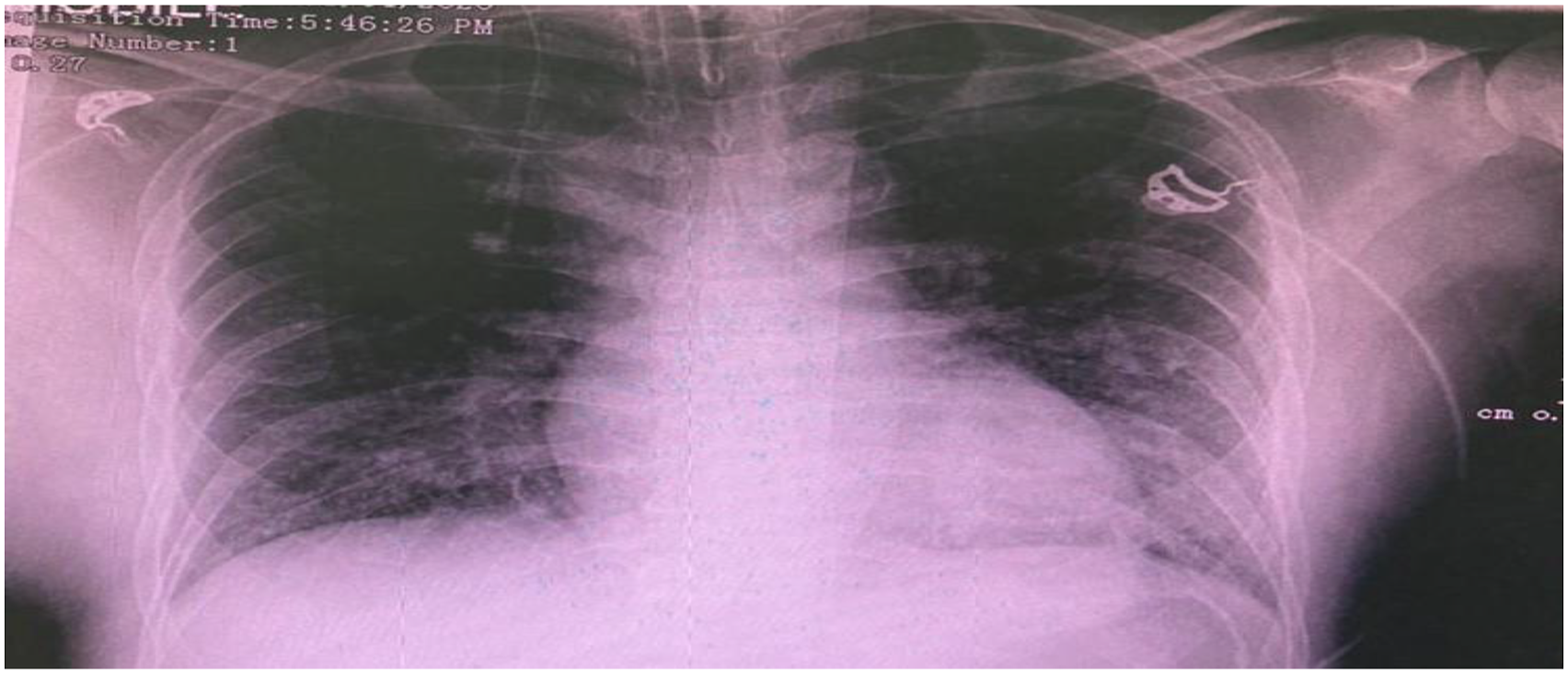
shows the chest X-ray of the patient.
Blood investigations.

Discussion
de Winter syndrome is a rare phenomenon, and it occurs in approximately 2% of patients with myocardial infarction. 2 It has a high predictive value for LAD occlusion. 4 Recent studies suggested that de Winter syndrome may be a transient event before progressing into typical STEMI ECG. 5 The exact electrophysiologic mechanisms involved are not known. However, it has been postulated the ST-segment depression and the tall peaked waves are attributed to hypoxic-driven alteration in the ATP-dependent potassium channels, resulting in a delay in repolarization in the subendocardial region with change in the transmembrane action potential. 6 Life-threatening ventricular arrhythmias are more common in STEMI compared to NSTEMI. We believe the mechanism of arrhythmogenesis of these life-threatening arrhythmias in STEMI is similar to that of de Winter syndrome in which the damaged myocardium produces a medium for re-entrant circuits and has enhanced automaticity.
Although de Winter syndrome is not specifically mentioned in the recent European Heart Society and American Heart Society guidelines, it has been stated in the discussion of the Fourth Universal Definition of Myocardial Infarction as one of the atypical ECG manifestations of acute myocardial ischemia. Despite that, the misdiagnosis rate is still extremely high among clinicians because of the atypical pattern, and it is often classified as NSTEMI which may result in missing the appropriate therapeutic window for revascularization. 7 A systemic review by Joel et al. concluded early activation cardiac catheterization lab with PCI leads to better clinical outcomes. 8 However, with the majority cardiovascular burden in middle-income to poor-income countries, accessing the cardiac catheterization laboratory within the therapeutic window for revascularization can be a great challenge. Therefore, thrombolytic therapy may be the best alternative emergent reperfusion strategy in non-cardiac centers.
Besides the syndrome being underrecognized, having no multicentric blinded control trials to date evaluating the effectiveness of thrombolysis in patients with de Winter syndrome makes it more challenging for clinicians to choose thrombolytic therapy as an alternative emergent reperfusion strategy. A similar dilemma was raised by Pranata et al. who opted for conservative therapy with anticoagulant and double antiplatelet for de Winter syndrome and only gave thrombolytic therapy when it evolved to STEMI. 9 Our case is different as we opted for the pharmacoinvasive strategy. Thrombolytic therapy was given as soon as we recognized de Winter syndrome, and the patient was transferred in-patient to a cardiac center for PCI immediately post thrombolysis. The decision to initiate thrombolysis early was inspired by successful clinical outcomes reported by Rao et al. and Shergill et al.10,11
Conclusion
To our knowledge, this is the first case report of de Winter syndrome from Malaysia. It is of paramount importance for physicians to recognize this STEMI-equivalent cardiology emergency to ensure early revascularization. The case study also calls for further multicentric randomized blinded controlled trials to further evaluate thrombolytic therapy as an alternative emergent reperfusion strategy especially in hospitals with no interventional cardiology.
Practice points
1. It is imperative that clinicians identify the de Winter ECG pattern and consider it as STEMI equivalent. 2. The immediate recognition of de Winter syndrome is important for urgent reperfusion therapy for better clinical outcomes. 3. Further randomized blinded controlled trials are indicated to evaluate the effectiveness of thrombolytic therapy as an alternative emergent reperfusion strategy in de Winter syndrome.
Footnotes
Acknowledgments
The authors would like to acknowledge the medical department of Hospital Selayang and Faculty of Medicine UiTM for supporting the submission of the case report. Our utmost gratitude goes to our colleagues, supervisors, and family members for their active guidance and encouragement.
Authors’ contributions
NP and HS are responsible for the collection of data, drafting, and revising the manuscript.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Availability of data and materials
The data that support the findings of this study are available from Hospital Selayang and will be available from the authors upon reasonable request and permission from Hospital Selayang.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical approval
Not applicable
Informed consent
Written informed consent was obtained from the patient’s legal guardian for the anonymized information to be published in this article.
