Abstract
Suprasellar tuberculomas are uncommon causes of intracranial tumours worldwide, even in areas endemic for tuberculosis. Often, they present with combinations of pituitary hormone involvement, which can lead to various complications due to hypopituitarism. We present a rare case of suprasellar tuberculoma leading to diabetes inspidus.
Introduction
Intracranial tuberculomas account for only 0.15–0.18% of intracranial tumours.1,2 Suprasellar tuberculomas are much more uncommon, and often present with signs of raised intracranial pressure and optic nerve compression, as well as variable pituitary hormone deficiencies. 3 We report a unique case of suprasellar tuberculoma presenting as diabetes insipidus (DI).
Case presentation
A 43-year-old woman with a known history of poorly controlled type 2 diabetes mellitus, (haemoglobin A1C level of 13.0%) presented with a three-day history of lethargy and altered mental status. Her blood and urine tests (urine-specific gravity) on arrival (Tables 1 and 2) were indicative of a hyperglycaemic hyperosmolar state (HHS), for which she received treatment. She was hypovolaemic on arrival, with a blood pressure of 92/54 mmHg and pulse rate of 124 bpm. Her serum blood glucose on arrival was 37.0 mmol/L. Clinical examination was unremarkable apart from an excessive urine output of 1600 mL/h. Unfortunately, despite aggressive fluid resuscitation and intravenous insulin therapy, her conscious level remained poor, and biochemical investigations showed persistent hypernatraemia, prompting further investigations.
Blood Investigations on Presentation.

Blood and Urine Tests, Both Pre- and Post-Desmopressin Administration.

Urgent computed tomography (CT) imaging of the brain revealed multiple enhancing cerebral, cerebellar and brainstem lesions. These findings were further seen on magnetic resonance imaging (MRI) of the brain, with additional evidence of conglomarate enhancement and pachymeningeal enhancement (Figure 1(a) and (b)). Furthermore, MRI also showed a lobulated enhancing lesion affecting the hypothalamus, mamillary bodies and optic chiasm. There was also evidence of a well-defined central pontine lesion suggestive of osmotic demyelination (Figure 1(c) and (d)).
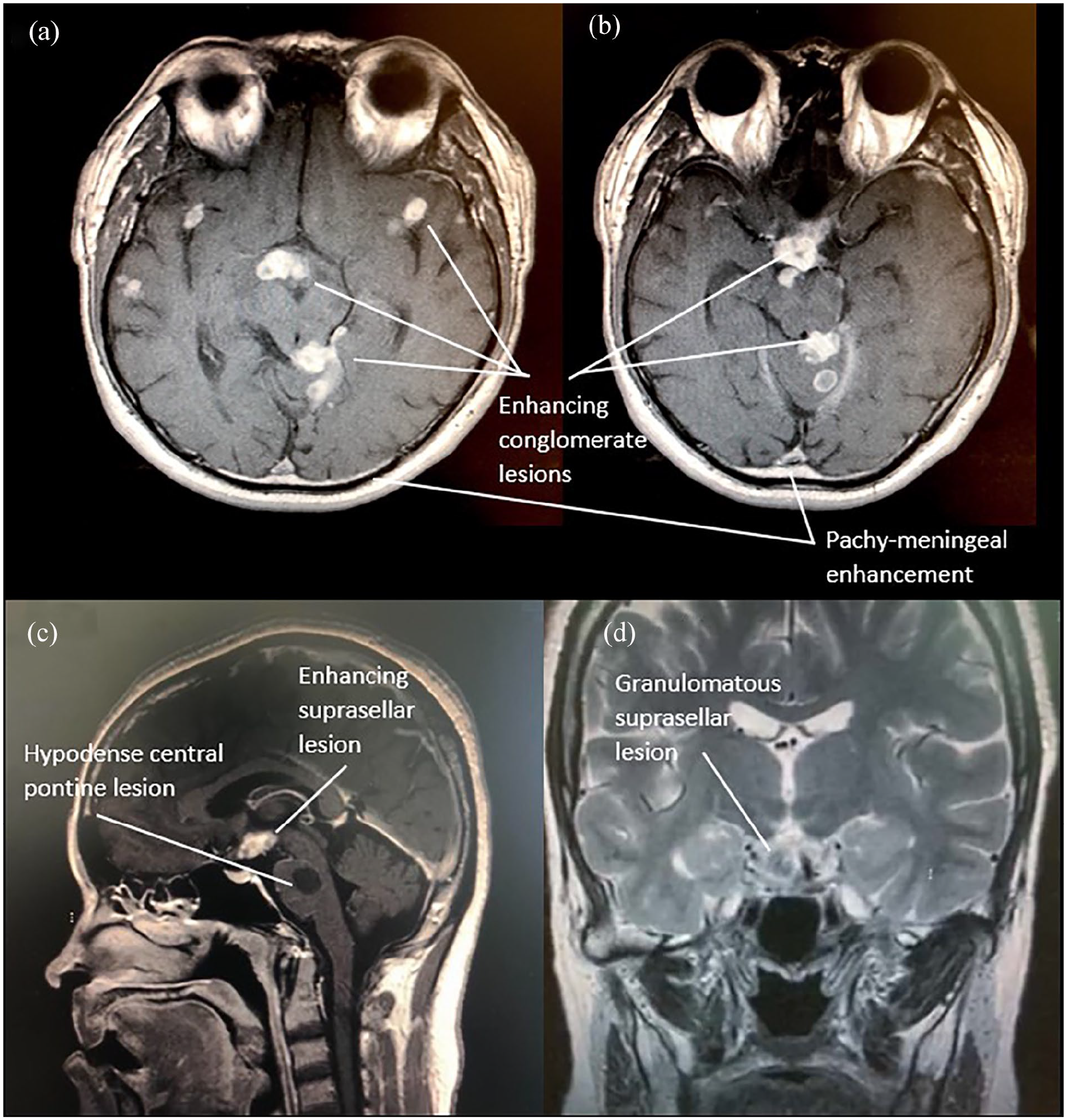
T1 gadolinium sequence magnetic resonance imaging (MRI) of the brain on ((a) and (b)) axial view, showing multiple cerebral, cerebellar and brainstem lesions, with evidence of conglomerate enhancement, and pachymeningeal enhancement, and on (c) mid-sagittal axis, enhancement of hypothalamic, both mammillary bodies and optic chiasm were demonstrated. There was also evidence of a well-defined central pontine lesion, suggestive of central pontine myelinolysis. T2 gadolinium sequence MRI on (d) coronal axis demonstrated the lobulated lesions. Findings were suspicious of multiple tuberculomas and tuberculous meningitis.
Her urine osmolality was raised on arrival (429 mOsm/L) but was attributed to presence of solute diuresis due to hyperglycaemia, which subsequently improved over the course of her treatment. However, despite rigorous fluid resuscitation and improvement in hyperglycaemia, she remained hypernatraemic and polyuric, and her urine specific gravity remained low at 1.005 (normal range 1.010–1.025), leading to suspicion of cranial DI. Her pituitary hormone profile, which revealed secondary hypothyroidism and hyperprolactinaemia, was also supportive of panhypopituitarism. Cranial DI was confirmed following a trial of subcutaneous desmopressin (1 µg/day), which showed an increased plasma sodium concentration, a rise in urine osmolality of >50% and a significant reduction in urine output (Table 2). Possible differentials included tuberculosis, sarcoidosis, lymphoma or metastases. Being from a tuberculosis-endemic area such as Malaysia, and having reported a history of significant unintentional weight loss, loss of appetite and dry cough, CT imaging of the thorax, abdomen and pelvis was performed which was unremarkable. Sputum sample staining using Ziehl–Niesen was negative for any acid-fast bacilli. Unfortunately, a lesion biopsy of the intracranial lesion was deemed risky due to a lack of access window to the area of interest by our neurosurgical team. The patient and her family had refused further investigations, including a bronchoscopy for broncho-alveolar lavage sampling.
A decision was thus made to start the patient on empirical anti-tuberculous therapy (ATT). This showed clinical improvement, with concurrent gradual reduction in serum sodium concentration through regular desmopressin use of 1 µg b.i.d. The patient was also commenced on levothyroxine and intravenous hydrocortisone (which was gradually tapered down to oral prednisolone) on discharge. Similarly, serial monitoring of intracranial lesion through CT imaging of the brain showed improvement over a three-month period. The patient was subsequently discharged well, with subcutaneous desmopressin, oral levothyroxine and ATT, and remains under regular follow-up.
Discussion
Intracranial tuberculomas commonly affect the cerebrum and cerebellum, with only 1% affecting the suprasellar region. 4 The majority of reported cases originate from the Indian subcontinent. 5 Suprasellar involvement often manifest as headaches, visual problems or symptoms suggesting anterior pituitary disruption, as seen in our patient. 6 Pituitary hormone dysfunction, including hyperprolactinaemia and secondary hypothyroidism, also occur in 20–25% of cases. 7 Rarely (11–28%) DI can occur as well, as illustrated in our case.6,8
Our patients displayed risk of immunosuppression due to poorly controlled diabetes, although it is not uncommon for suprasellar tuberculoma to occur in immunocompetent individuals. 8 Possible dissemination into the central nervous system from lung foci can occur, although pulmonary tuberculosis need not always be present. Sharma et al. reported only 5/18 patients with suprasellar tuberculosis having had a history of concomitant extracranial tuberculosis. 9 Other differentials that were considered in this patient include fungal infections, syphilis, Langerhan cell histiocytosis, granulomatous hypophysitis and neuro-sarcoidosis. 7
Our patient’s urine-specific gravity was low, despite elevated blood glucose levels on presentation. In a patient with poor glycaemic control, elevated blood glucose levels and hypovolaemia should lead to an increased urine-specific gravity. When there is a discordant picture in between the urine-specific gravity and blood glucose, DI must be thought of in a setting of poorly controlled diabetes. This happens due to inability of the kidneys to concentrate the urine. Furthermore, although hypernatraemia is very common in the setting of hypovolaemia, a rapid rise in sodium concentration leading to central pontine myelinosis is uncommon, even in HHS. We believe that it could have possibly been due to a rapid rise in serum sodium due to decompensated cranial DI that was further precipitated by the HHS.
A unique aspect of our case report was the management of the tuberculous lesion sans histological evidence. There was also no microbiological evidence (on acid-fast bacilli staining) or suggestive radiological evidence (no cavitating lesions or ‘tree in bud’ appearance on CT imaging of the thorax) to support a diagnosis of tuberculosis further. Although not ideal, there have been reports of successful empirical therapy, advocating a trial of 6–12 weeks of treatment, in the presence of peripheral evidence and suggestive clinical history.10,11 However, although ATT allows for improvement in structural lesions, there remains a sparsity of evidence in improvement of the pan-hypopituitarism state with initiation of anti-tuberculosis therapy. 12 Our patient was thus discharged on hormone replacement therapy and remains on close outpatient monitoring.
Conclusion
Although rare, intracranial tuberculomas should be considered in patients from endemic areas who present with intracranial mass. Definitive histological diagnosis is often preferred in such cases. However, there is evidence to support trial of empirical ATT, especially in areas limited by resources and appropriate skills to perform intracranial biopsies, which is a common plight in tuberculosis-stricken countries.
Footnotes
Acknowledgements
The authors would like to acknowledge Universiti Teknologi MARA and the Clinical Research Centre (Hospital Sungai Buloh) for supporting the submission of the following case report.
Authors’ contributions
R.E.F.R.S.: data collection and analysis, drafting of manuscript. S.F.W.M.H.: drafting of manuscript, revision of manuscript. S.S.: drafting of manuscript, revision of manuscript.
Availability of data and materials
The data that support the findings of this study are available from Hospital Sungai Buloh, but restrictions apply to the availability of these data, which were used under license for the current study and so are not publicly available. Data are, however, available from the authors upon reasonable request and with permission of Hospital Sungai Buloh.
Conflict of interest
The authors declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Ethical approval
Ethical approval to report this case was obtained from Universiti Teknologi MARA Ethics Committee and the Clinical Research Centre (Hospital Sungai Buloh) Medical Research and Ethics Committee. The manuscript DOES NOT report on any human (or animal) data or tissue.
Funding
The authors received no financial support for the research, authorship and/or publication of this article.
Informed consent
Written informed consent was obtained from the patient for her anonymised information to be published in this article.
