Abstract
Atrio-ventricular dissociation (AVD), including complete heart block (CHB), are far more common in the elderly. We report a rare case of CHB in a 40-year-old man, who tested positive for anti-Ro autoantibodies without systemic features. He had been suffering for giddiness over the previous two months. On arrival, his electrocardiogram revealed high-degree AVD. Upon further history, he mentioned that his 68-year-old mother with systemic lupus erythematosus (SLE) had suffered from similar episodes, requiring a permanent pacemaker implantation. On further investigation, he tested positive for antinuclear antibodies (ANA), anti-SSA/Ro and anti-RNP antibodies. However, from history and clinical examination, he had not manifested any articular, extra-articular or extra-glandular features suspicious of rheumatological conditions. Following a failed trial of intravenous hydrocortisone, he subsequently had a permanent pacemaker implanted himself. Although difficult to ascertain whether our patient suffered from a congenital form of anti-SSA/Ro-related CHB, there is evidence to suggest delayed presentation of CHB in those with anti-SSA/Ro and neonatal lupus syndrome. Anti-SSA/Ro antibodies without systemic features can be present in 3% of the population, although this occurs more commonly in the presence of a confirm diagnosis of SLE, Sjögren’s syndrome or poly- and dermatomyositis. Despite the scarcity of evidence, a trial of steroid-based treatment was attempted prior to subjecting the young patient to a permanent pacemaker and its associated complications. To our knowledge, this is only the second case of isolated anti-SSA/Ro syndrome presenting with CHB reported in the literature.
Introduction
Atrio-ventricular dissociation (AVD), including complete heart block (CHB), are far more common in the elderly. Causes include degenerative disease, myocardial infarctions, myocarditis and medication-induced CHB, among others. 1 We report a rare case of CHB in a middle-aged man, who tested positive for anti-Ro autoantibodies without any other clinical manifestation of autoimmune diseases or vasculitis.
Case report
A 40-year-old man presented to the emergency department following episodes of giddiness and having suffered a fall. He had been suffering for giddiness over the previous two months, but did not seek medical attention prior to presentation. He had no known medical illnesses and was a smoker of 20 pack years. He denied any use of prescription medication or substance misuse. On arrival, his vital signs included a blood pressure of 133/69 mmHg and heart rate of 38 bpm. His cardiorespiratory examination was unremarkable, including for any murmurs or carotid bruits. His electrocardiogram on arrival revealed evidence of high-degree AVD, likely due to CHB (Figure 1).
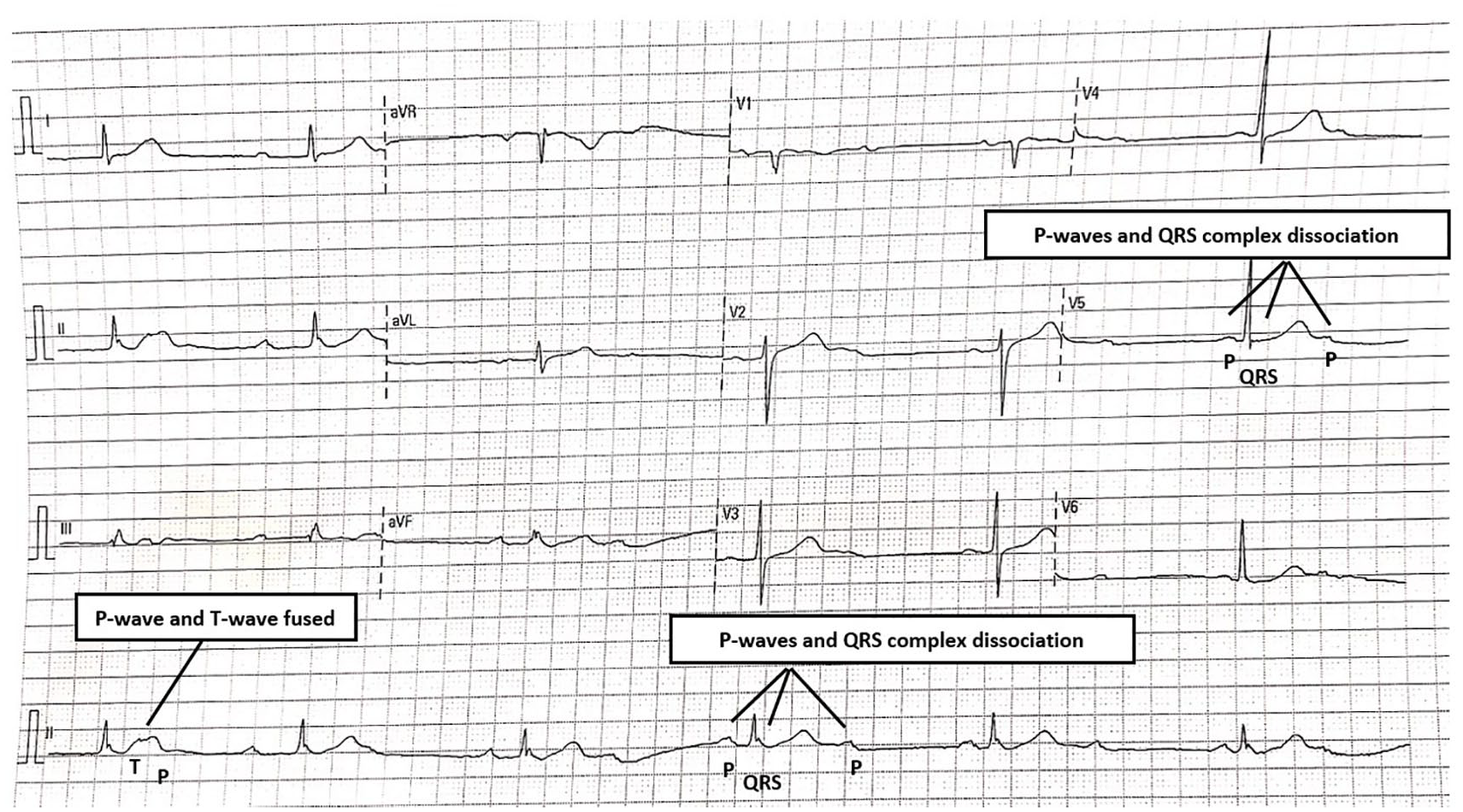
Electrocardiogram demonstrating dissociation between atrial contractions (represented by P waves) and ventricular contractions (represented by QRS complexes), suggestive of high-degree atrioventricular nodal block, likely complete heart block.
Upon further history, he mentioned that his 68-year-old mother, who was known to have systemic lupus erythematosus (SLE) for 30 years, suffered from similar ‘spells’, which required a permanent pacemaker implantation a year ago. Due to his relatively young age and significant family history, further investigations were performed (Table 1). He tested positive for antinuclear antibodies (ANA), anti-SSA/Ro and anti-RNP antibodies. However, from history and clinical examination, he had not manifested any articular, extra-articular or extra-glandular features to fulfil the diagnosis of SLE or Sjögren’s syndrome. The patient also underwent coronary angiography to exclude coronary artery disease, which was unremarkable.
Blood investigations

Positive results are shown in bold.
ANA: antinuclear antibodies
Following a rheumatology consult, a trial of intravenous hydrocortisone was commenced for several days to no avail. He subsequently had a permanent pacemaker implanted himself, which was uneventful, and he remains under regular follow-up.
Discussion
Anti-SSA/Ro antibodies are often associated with congenital CHB. Despite this known association, the exact mechanism leading to conduction delay remains unknown. 2 Placental passage of maternal autoantibodies damage foetal atrioventricular conduction tissue via various postulated mechanisms, including inflammation and direct channel action, with eventual fibrosis. 3 Although difficult to ascertain if our patient suffered from a congenital form of anti-SSA/Ro-related CHB, there is evidence to suggest delayed presentation of CHB in those with anti-SSA/Ro and neonatal lupus syndrome. 4
Anti-SSA/Ro antibodies without systemic features can be present in 3% of the population, although this occurs more commonly in the presence of a confirmed diagnosis of SLE, Sjögren’s syndrome or poly- and dermatomyositis.5,6 However, it remains pertinent to exclude more common causes of CHB in the young, including Lyme disease, sarcoidosis, thyroid disorders, myocarditis, electrolyte imbalances and auto-immune diseases, before concluding anti-SSA/Ro syndrome. 5
By excluding other causes (especially infection-based differentials), a trial of steroid-based therapy could be administered, as seen in our patient. However, the evidence for immunosuppression in reversing CHB is scarce, with only one other case of anti-Ro syndrome having trialled such therapy to success. 7 In our case, despite failing, we felt it was worthwhile prescribing steroid-based treatment to our young patient prior to subjecting him to a permanent pacemaker and its associated immediate and long-term complications.
Conclusion
Anti-SSA/Ro antibody-related CHB remains a unique entity and a challenge to treat, as evidence and guidelines to management remains limited. To our knowledge, this is only the second case of isolated anti-SSA/Ro syndrome presenting with CHB reported in the literature. A multidisciplinary approach to management remains key, as commitment to standard lifelong therapy such as a permanent pacemaker needs to be heavily evaluated in these often young patients.
Footnotes
Acknowledgements
The authors would like to acknowledge Universiti Teknologi MARA (UiTM) for supporting the submission of the following article.
Authors’ contributions
R.E.F.R.S.: data collection and analysis, drafting of manuscript. L.C.W.: data collection and analysis, drafting of manuscript. S.S.: drafting or manuscript, revision of manuscript.
Availability of data and materials
The data that support the findings of this study are available from UiTM Sungai Buloh, but restrictions apply to the availability of these data, which were used under license for the current study and so are not publicly available. Data are, however, available from the authors upon reasonable request and with permission of UiTM Sungai Buloh.
Conflict of interest
The authors declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Ethical approval
Approved by the Universiti Teknologi MARA (UiTM) Ethics Committee. The manuscript does not report on any animal data or tissue.
Funding
The authors received no financial support for the research, authorship and/or publication of this article.
Informed consent
Written informed consent was obtained from the patients for their anonymised information to be published in this article.
