Abstract
Introduction:
The emergency department receives a whole breadth of patient types. Those who are imminently dying may attend the emergency department in the hours or days leading up to their demise, necessitating the initiation of end-of-life care in the emergency department.
Aim:
The aim of our study was to describe the characteristics and management of imminently dying patients who had presented to our emergency department to identify opportunities for improvement in the provision of end-of-life care in the emergency department.
Methods:
A retrospective study involving patients who died in the emergency department within 48 hours of registration presenting between 1 January 2018 and 31 December 2018 was carried out.
Results:
Out of 59 included patients, 91.5% had pre-existing medical conditions; 25.4% had end-stage organ failure of which renal and cardiac were most common. Only 15.3% had preferred care plans documented and among these, only a minority (33.3%) had undergone formal advance care planning. The most common presenting symptom among patients who died within 48 hours was dyspnoea (44.1%). The most common investigation done was capillary blood glucose (84.7%) and the most common procedure was an intravenous peripheral cannula insertion (84.7%). Antibiotics were given in 30.5% of the patients and fentanyl was administered in 20.3% for symptom control.
Conclusion:
The majority of patients presenting to the emergency department within hours or days of their demise had pre-existing chronic or terminal conditions but only a few had specified their preferences for end-of-life care. Investigations and procedures that do not affect patient comfort or outcomes should be minimised.
Introduction
The emergency department (ED) receives a whole breadth of patient types, ranging from acute trauma to those with chronic or terminal illness. Among the large number of cases every day, handling patients who are nearing the end of life (EOL) is not an uncommon experience. 1 Patients who are actively or imminently dying may present to the ED in the hours or days leading up to their demise. 1 This necessitates the initiation and provision of EOL care within the ED.
With chaos and overcrowding, it is often difficult to provide a peaceful and uninterrupted environment in the ED for families to spend their last moments with their loved ones.2,3 ED physicians and nurses may also lack confidence and knowledge in providing EOL care, especially as it seems to contradict their conventional training in instituting life-saving measures for critically ill patients. 4
The unmet needs of EOL patients and their families at the ED are increasingly being recognised. Guidelines have been introduced as part of the efforts to optimise ED EOL care.5–8 However, successful implementation of and adherence to such guidelines remains challenging in an ED environment, given the unpredictable and potentially chaotic setting, high patient load, frequent changes in staff and fast-paced nature of the work. 2
As imminently dying patients may share certain characteristics that could help predict their impending demise, awareness and recognition of these characteristics would enable healthcare providers in the ED to optimise EOL care for these patients.
Aims
The aim of this study was to describe the characteristics and management of imminently dying patients who had presented to our ED, in terms of demographics, comorbidities, presenting symptoms as well as the types of investigations and interventions performed.
Methods
This was a retrospective observational study. Our population of interest was defined as imminently dying patients from non-traumatic conditions who attended the ED from 1 January 2018 to 31 December 2018. ‘Imminently dying’ patients were identified as those who had been alive on arrival with subsequent demise within 48 hours9,10 of registration.
As this was a descriptive analysis, no sample size or power calculation was performed. All cases which had met the inclusion criteria in the study period were included. The ED electronic patient records system was used to identify all patients who died within 48 hours of ED registration. Patients were then selected using a set of predetermined criteria.
Inclusion criteria
Patients who had died in the ED within 48 hours of ED registration.
Exclusion criteria
Patients who were not alive on arrival at the ED
Patients with a trauma diagnosis
Patients aged 16 years old and below.
The initial list of eligible patients based on the inclusion criteria was generated electronically, together with extraction of the following variables: ED visit case identification number, date/time of ED registration, date/time of death and demographics (gender, age and ethnic group). A chart review of both ED and inpatient medical records was conducted to apply the exclusion criteria and further to collect the following variables for the final list of eligible patients:
Comorbidities and presenting symptoms
Diagnosis
Investigations performed for the patients
Interventions given to the patients
Documentation of communication about EOL care
Time spent in the ED before demise.
Ethical approval was obtained from our hospital’s centralised institutional review board (CIRB 2020/2024). Waiver of informed consent was obtained as this was a retrospective audit involving deceased patients. The data collected were input anonymously into the research database platform (REDCap).
Results
Out of 1014 patients who died within 48 hours of ED registration, 417 were admitted to the inpatient wards. Of the 597 who died in the ED, seven were under the age of 16 years, 14 were excluded due to trauma and 517 were not alive on arrival.
A total of 59 patients fulfilling our criteria were identified. The median age was 79 years (interquartile range (IQR) 69–84). Half of the patients were men, and the majority were Chinese (Figure 1). The mean time spent in the ED (between time of registration and time of death) was 157 minutes. More than a third of the participants presented in the afternoon within the period of 12:00 hours to 20:00 hours (Figure 2) and the hour between 18:00 hours and 19:00 hours saw the highest number of patients registered in the ED.

Ethnic distribution.

Time of presentation.
The majority (91.5%) of the patients in our study had pre-existing medical conditions (Table 1). For non-terminal illness, hypertension (74.58%), hyperlipidaemia (61.02%), diabetes mellitus (47.46%) and ischaemic heart disease (47.46%) were the most common. Less commonly seen were patients with previous strokes (25.42%), renal disease (23.73%), cancer (6.78%) and others (3.39%). For terminal illness, end-stage organ failure was present in 25.4%, chronic frailty was present in 6.78% and advanced cancer was present 6.78% of patients. Subtypes of organ failure were renal (10.17%), cardiac (5.08%), both renal and cardiac (5.08%), pulmonary (1.70%), hepatological (1.70%) and neurological (1.70%).
History of chronic disease.
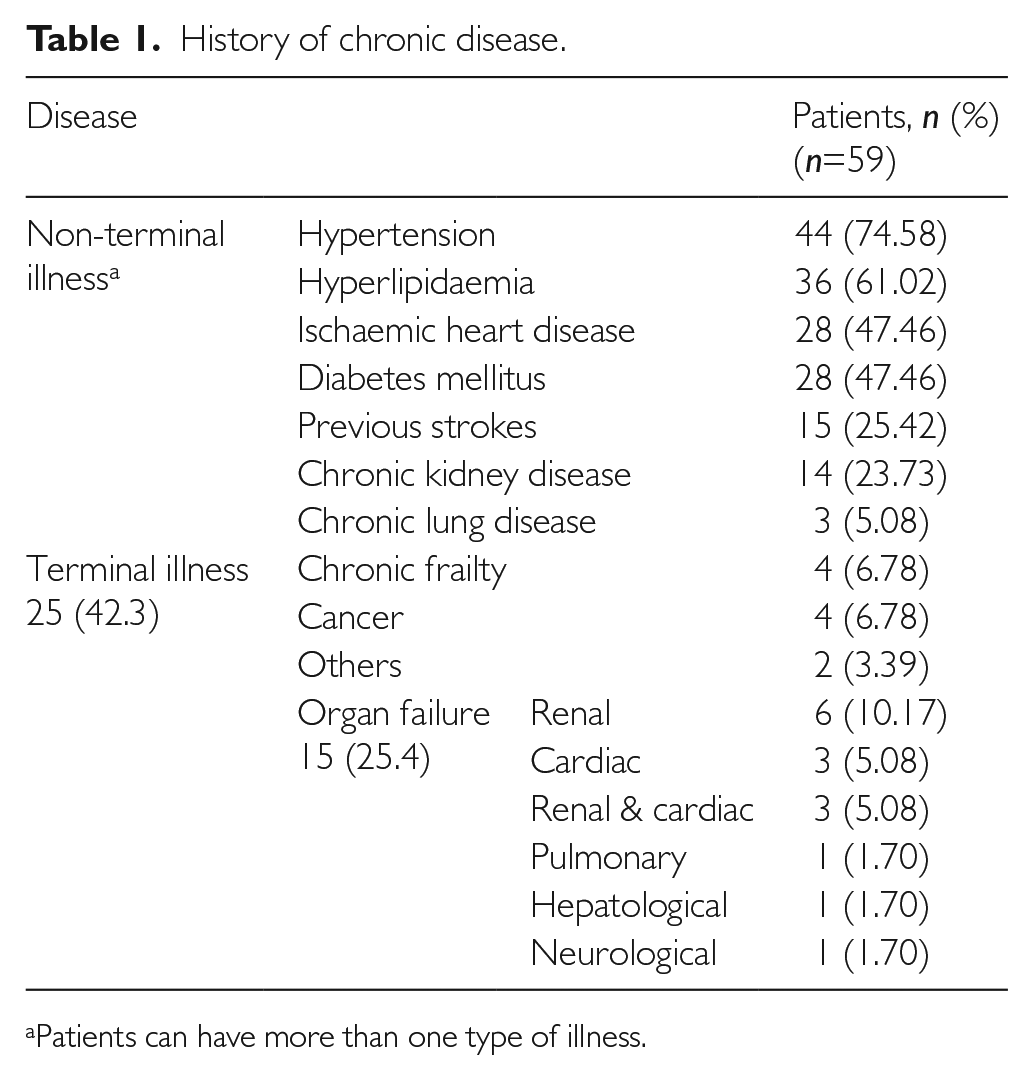
Patients can have more than one type of illness.
Of the patients recruited, only nine (15.3%) had any previously established extent of care. Among these patients, only three of them or about one-third had carried out advance care planning (ACP). The majority of the patients, 43 (72.9%), had their extent of care discussed in the ED, none of whom were referred to a medical social worker (MSW) or a palliative team. Only three (5.1%) of the patients were already known to palliative or hospice services.
The most common presenting symptom (Table 2) was dyspnoea (44.1%) followed by drowsiness (30.5%).
Presenting symptoms.

Some patients may have more than one symptom.
Initial investigations (Figure 3) for these patients were instituted in the ED. Most patients had blood investigations such as capillary blood glucose (84.7%), renal panel (79.7%), a full blood count (74.6%) and troponin T was sent off in 57.6% of patients. Non-blood investigations such as chest X-rays (76.3%) and electrocardiograms (78%) were also done in the majority of patients. A computed tomography (CT) brain scan was done in a smaller proportion of patients (23.7%). Only two patients (3.39%) had no investigations done.
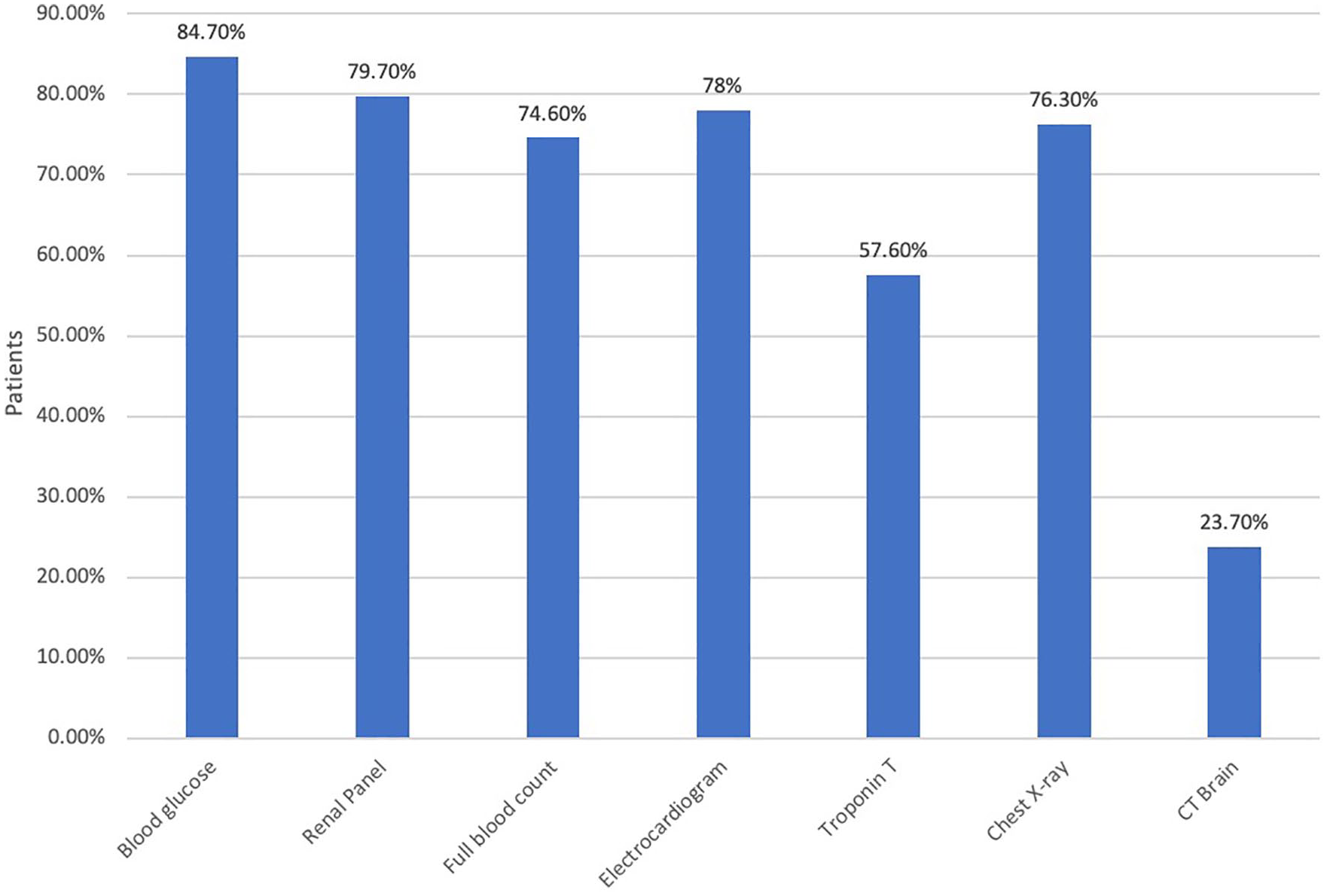
Investigations.
Fentanyl (Figure 4) was used in 20.3% of patients and morphine in 1.7%. Intravenous (IV) antibiotics were administered in 30.5% of patients. Of these, piperacillin/tazobactam was the most commonly used antibiotic (44.4%). It was noted that all the antibiotic choices were ‘broad spectrum’ (co-amoxiclav, levofloxacin, metronidazole, ceftriaxone, meropenem). Other drugs used were paracetamol (6.8%), metoclopramide (5.1%), tramadol (3.4%), diazepam (1.7%), midazolam (1.7%) and omeprazole (1.7%).
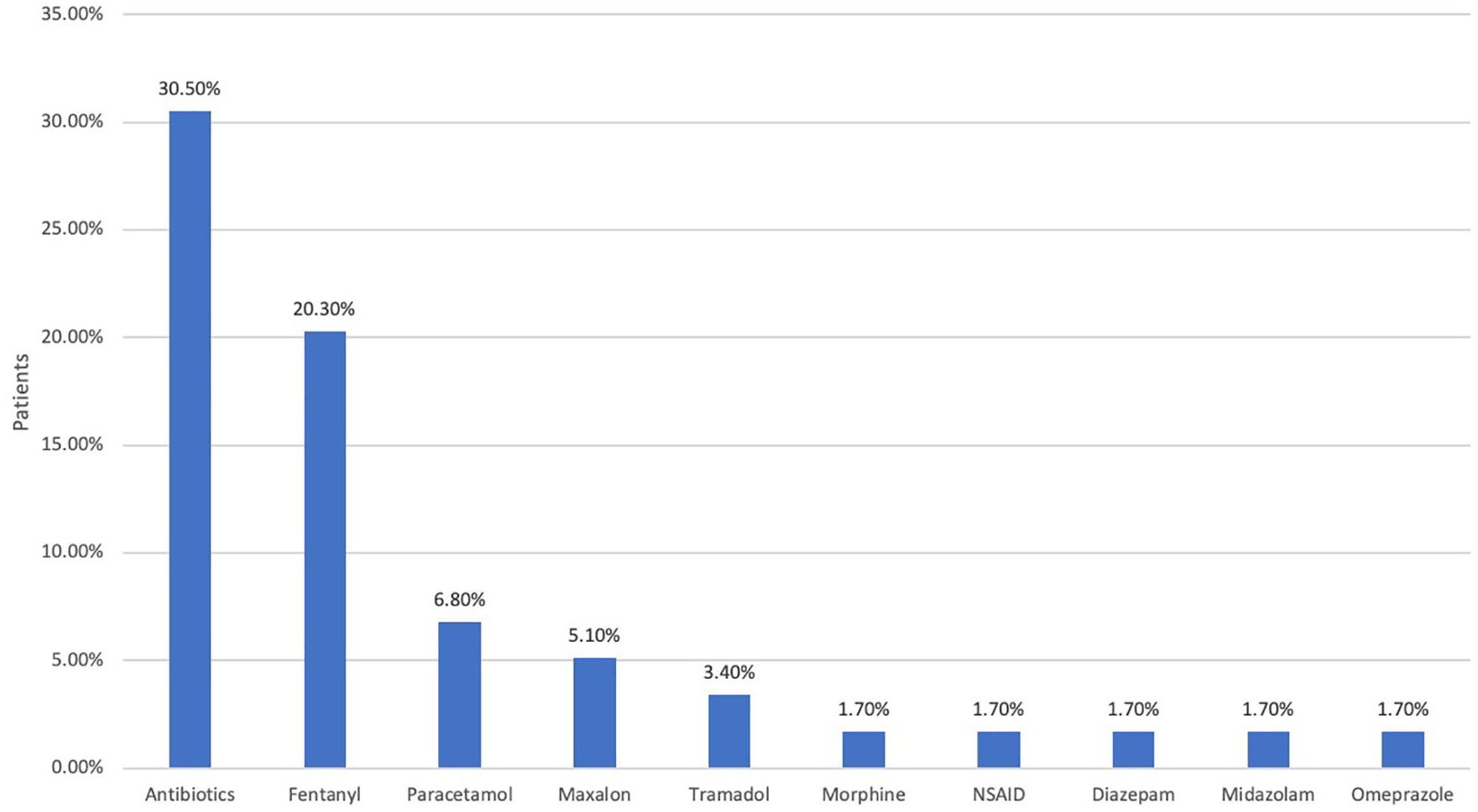
Medications.
Data on procedures (Figure 5) carried out were also collected. IV cannulas were inserted in 84.7% of the patients and IV drips started in 54%. Oxygen therapy was started for 66.1% of the patients. Nasogastric tubes were inserted in 18.6% of the patients, and indwelling catheters were used in 11.9% of the patients. Comfortable positioning was documented in only 6% of the patients. Other procedures such as subcutaneous needle insertion and oral care were either not carried out or not documented. As this was a retrospective study, any interventions which were not documented but carried out would be unknown to this study.
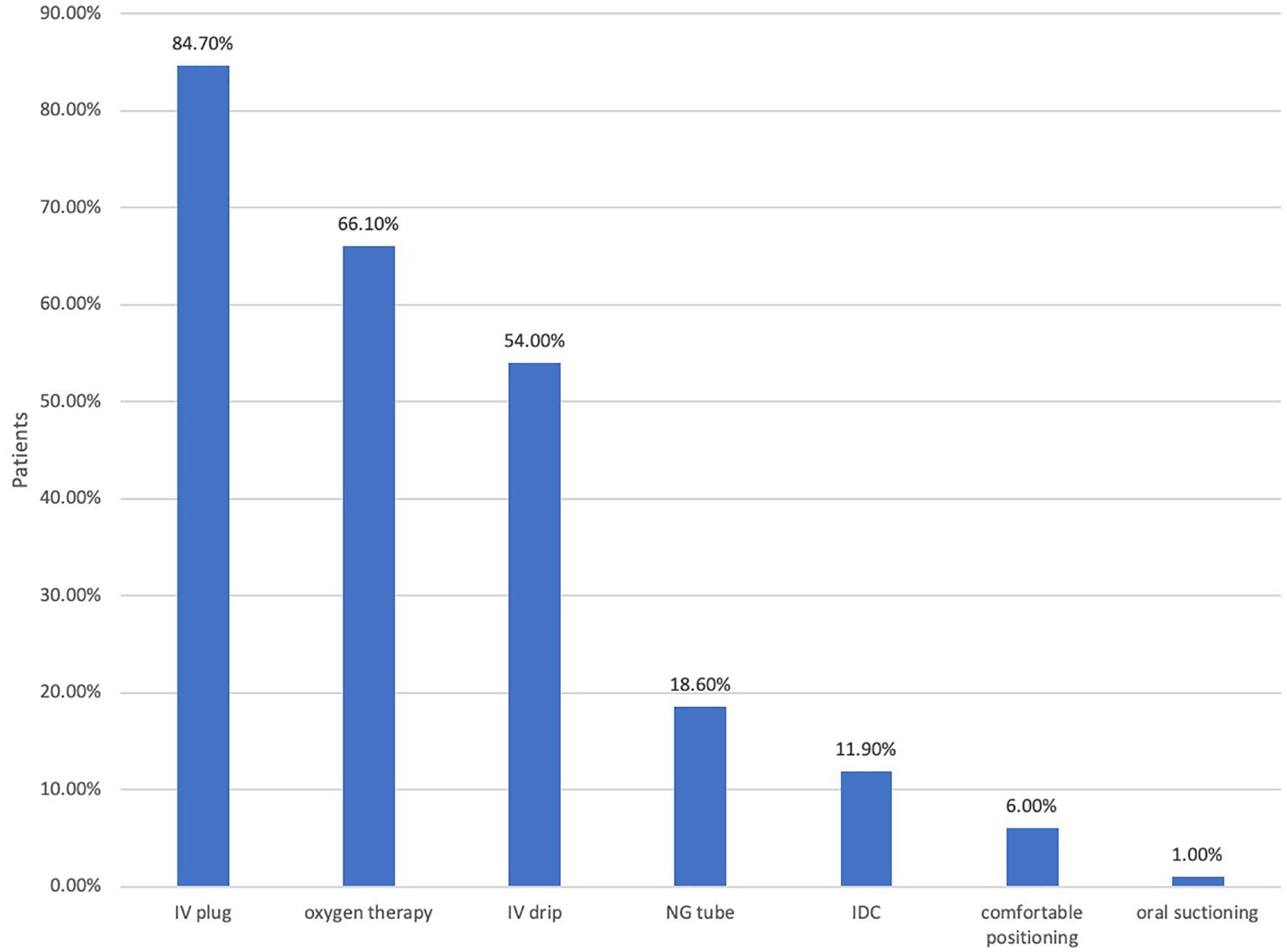
Procedures.
Discussion
A large proportion of our sample group of patients had known organ failure, with a smaller proportion who had chronic frailty or cancer. This is congruent with the concept of the ‘trajectories of death’11,12 as patients who have an expected trajectory towards death include those with chronic frailty, and/or organ failure.13,14 Frailty was described by Lunney et al. 12 as those with ‘steadily progressive disability before dying from complications such as those associated with advanced frailty of old age, stroke, or dementia’.
Yet, only a handful of patients had a previous extent of care plan documented or had ACP done before. This pattern is not unfamiliar. These are identifiable groups in whom EOL care goals would not be out of place for discussion. 15 However, across the board, rates of goals-of-care discussions are low.16,17 Many physicians treating patients with limited life expectancies 14 have identified the barriers they face for this discussion. Various articles describe patient factors such as lack of readiness, family factors such as denial as well as physician factors such as the fear of destroying hope and difficult prognostication.18–21 The ED, with its huge patient load and sometimes lack of space, is not the optimal setting to break bad news. 22
While an extent of care plan was quite readily documented in our sample of patients, they were mostly recorded as ‘not for CPR/ICU/intubation’ [cardiopulmonary resuscitation/intensive care unit]. It is not clear how the actual goals-of-care discussions were carried out. The quality of these discussions was not documented consistently, and therefore the understanding and reception of this information by the patient and/or next of kin remains unknown.
Beyond the scope of the ED, earlier ACP discussions among the elderly would be beneficial, especially among those with terminal illnesses, in order to provide more quality care. In the event that ACP was not previously carried out, discussions led by ED doctors to patients and their family should be optimal for informed decision-making in the patients’ best interest. 23 One way to improve communication would be to create a template for EOL discussions for ED doctors when patients who are actively dying are identified. 24 The hope is to provide a reminder in the steps of discussing goals of care and also for appropriate documentation purposes.
Even though studies25,26 have suggested that a multidisciplinary team that includes MSWs and a palliative team should be involved in patient care, there was no record of their involvement in this group of patients during their ED visit. Involving a multidisciplinary team would ensure more well-orchestrated communications, resulting in a positive therapeutic effect for patients and their families. Further studies have even illustrated that MSWs should be involved in outpatient EOL discussions as they would be able to harness the appropriate resources for social support, such as counselling, therapy, caregiver arrangements, exploring role changes within a family, spiritual guidance and even curating funeral arrangements. 26 This might alleviate patient and family factors of denial and unreadiness in discussing EOL decisions.
An increasing number of palliative and emergency medicine departments are collaborating to improve ED care for patients in their final hours in order to initiate palliative care consults earlier. 27 Social work models, such as palliative care service-initiated programmes, palliative care champions in the ED, and an ED–hospice partnership for hospice services, 28 were created specifically to recognise patients with palliative needs in order to increase their comfort level in their final hours. However, the study found a lack of involvement of the MSWs and palliative team, possibly due to the lack of time and the presence of logistical constraints. 29 Locally, Chor et al. 30 found that the implementation of an EOL pathway in their ED, through the use of a protocolised management care bundle, was feasible in providing ED physicians with a guide in managing such patients.
Dyspnoea, being one of the more common symptoms at the EOL, has been extensively studied in palliative care, with opioids being a main pharmaceutical intervention as they alleviate anxiety and pain; commonly a key part of the dyspnoea cycle. 31 However, only a small proportion of our patients who had dyspnoea were treated with an opioid. Due to the retrospective nature of our study, there was insufficient information for us to postulate the exact reasons for this and it could be due to reasons that are worthy of further exploration. A Dutch study in 2015 studying the use of opioids in severe chronic obstructive pulmonary disease (COPD) with refractory dyspnoea have shown the reluctance of opioid administration in physicians; with fear of respiratory depression, unknown efficacy and insufficient experience being some of the barriers. 32
Of the myriad of investigations available in the ED, we found that the most commonly ordered investigations were capillary blood glucose, renal panel, electrocardiogram, chest X-ray and full blood count. Initial investigations are useful in diagnosis and prognosis, following which, EOL care, rather than aggressive futile resuscitation, should be initiated if the outlook is grim. However, the utility of these investigations may be questionable in the setting of a patient approaching death. Excessive redundant investigations that do not change the management of the patient may cause unnecessary discomfort to the patient, and incur unnecessary additional costs for the family. Given the variety of cases that were studied and the retrospective nature of our study, it is difficult to ascertain the absolute necessity of all the investigations done.
As such, ED physicians may consider the use of screening tools to aid in the identification of those who are imminently dying, 8 although we acknowledge that these may be time consuming for routine use. An example would be the criteria for screening and triaging to appropriate alternative care (CriSTAL), 33 which was developed as a ‘screening tool to identify elderly patients at the EOL and quantify the risk of death in hospital or soon after discharge to minimise prognostic uncertainty and avoid potentially harmful and futile treatments’.
Of the procedures done, intravenous cannulas were inserted in 84.7% of patients in our study. While they are quick to set up, and offer easy access for the administration of drugs, it is not always necessary in patients who are imminently dying. Drugs for symptom control can be given via other routes of administration, such as subcutaneously and transdermally. 34 IV cannulas are also painful to insert, and may cause anxiety and discomfort to the dying patient. 35 Although there may be a role for intravenous cannulas in certain situations such as acute resuscitation, ED physicians need to exercise discretion in weighing the benefits against the potential harm when making the decision.
As can be seen, there remains work to be done still for the development of EOL care in the ED, such as improving the rates of ACP and goals-of-care discussion in those with chronic or terminal conditions. Our study adds to a growing body of local literature30,36,37 in this area. An ongoing study by Pal et al. 37 may help to address some of the gaps, and also formulate improvements to their EOL care protocol.
Limitations
As this research involved retrospective data extraction from medical records, there were missing values due to incomplete documentation. In addition, interventions such as comfortable positioning and oral care were not consistently documented even if performed, unlike pharmacological interventions which have to be prescribed and are thus more likely to be recorded.
Patients who were transferred to the inpatient wards and then subsequently died within 48 hours were not included in this study. In our ED, patients who are still alive after an arbitrary cut-off duration of 4 hours are admitted to the inpatient wards for further management. Clinicians may exercise judgement and flexibility on the exact duration.
We recognise that this may be a major limitation considering the large number of patients admitted as compared to those who died in the ED, thereby potentially limiting the generalisability of our results. We believe that further studies exploring this group of patients would be helpful in elucidating any differences in their characteristics, as well as differences in EOL care by the ED versus the inpatient team.
Conclusion
The majority of patients presenting to the ED within hours or days of their demise had pre-existing chronic or terminal conditions, but only a few had specified their preferences for EOL care. Investigations and procedures that do not affect patient comfort or outcomes should be minimised.
Footnotes
Acknowledgements
The authors would like to thank Charlene Ong for her assistance as the research coordinator. They would also like to thank Tiah Ling for her guidance in this research.
Authors’ contributions
JLG conceived the study, was involved in literature review, data entry, editing and wrote the first draft of the manuscript. HX and JLYJ were involved in literature review, data entry, editing and analysis. VWML was involved in gaining ethical approval, data entry and review of the manuscript. All authors reviewed and edited the manuscript and approved the final version of the manuscript.
Availability of data and materials
The datasets generated during the current study are available from VWML (corresponding author).
Conflict of interest
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical approval
Ethical approval for this study was obtained from the Singhealth Centralised Institutional Review Board (CIRB ref: 2020/2024).
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Informed consent
Waiver of informed consent was obtained as this was a retrospective audit involving deceased patients.
