Abstract
Colonic lipomas are rare benign tumours, although they constitute the most common non-epithelial neoplasm of the gastrointestinal tract. They mostly remain asymptomatic and rarely present with intussusception. A 62-year-old male presented with acute intestinal obstruction. On laparotomy, intussusception of the descending colon was detected, with a single sessile polyp measuring 3 cm×3 cm as the lead point. A left hemicolectomy was performed, and histopathological examination revealed a lipoma of the colon.
Introduction
Lipomas are the second most common benign tumours of the gastrointestinal tract. However, colonic lipomas rarely present as intussuception. 1 Most of these tumours remain asymptomatic, and resection of symptomatic lipomas has not been associated with recurrence. 2 In cases where malignancy is suspected or endoscopic resection is not possible, operative resection is normally performed with radical rather than segmental resection. 3 Frozen section at the time of surgical resection may be helpful in making a tissue diagnosis before radical resection. 4 We report here a case of a colonic lipoma presenting as intussusception.
Case report
A 62-year-old male presented to the emergency room with complaints of abdominal pain, a distended abdomen and non-passage of flatus and stools for 2 days. The episode of illness had only lasted 2 days, but a history of recurrent colicky abdominal pain had been present for more than 5 years. Recurrent episodic pain mostly subsided within a few hours, but it sometimes lasted for a few days. He had no history of the passage of blood or mucus in the stools. On examination, his abdomen was slightly distended with tenderness in the left iliac fossa. On percussion, the abdomen was tympanic and had exaggerated bowel sounds. An x-ray of the abdomen showed a dilated proximal large bowel suggestive of a large bowel obstruction. A computed tomography (CT) scan suggested a large bowel obstruction with dilated colon up to the right descending colon. A smooth, sharply defined, hemispheric mass measuring 3.52 cm×3.12 cm was identified in the descending colon, with a CT Hounsfield Unit value of –48, and the target sign was favouring a diagnosis of colonic lipoma (Figure 1). On exploratory laparotomy performed through a midline incision, intussusception of the descending colon was detected which was reduced, and on palpation, a mass lesion was detected. Segmental resection of the descending colon was performed, which showed a sessile growth measuring 3 cm×3 cm in the descending colon (Figure 2). In view of a large sessile polyp measuring 3 cm×3 cm (Figure 3), a left hemicolectomy with end-to-end colo-colic anastomosis was performed. The patient had an uneventful postoperative recovery. Histopathological examination of the specimen showed a lipoma of the descending colon (Figure 4).

Preoperative computed tomography scan of the abdomen with showing the target sign.
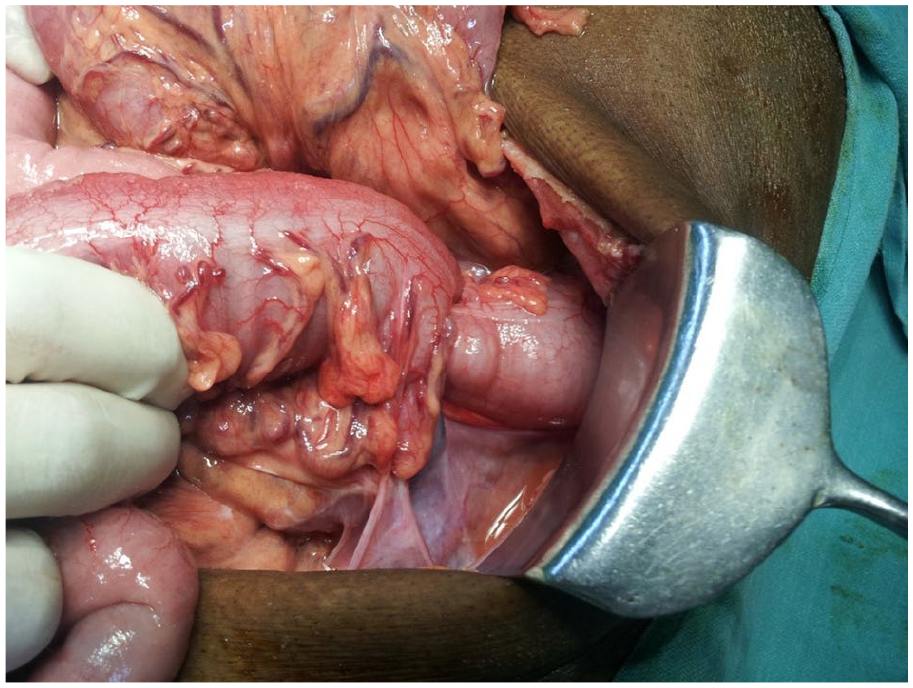
Operative photograph showing lipoma of the descending colon.

Cut open specimen of large polyp measuring 3 cm×3 cm.
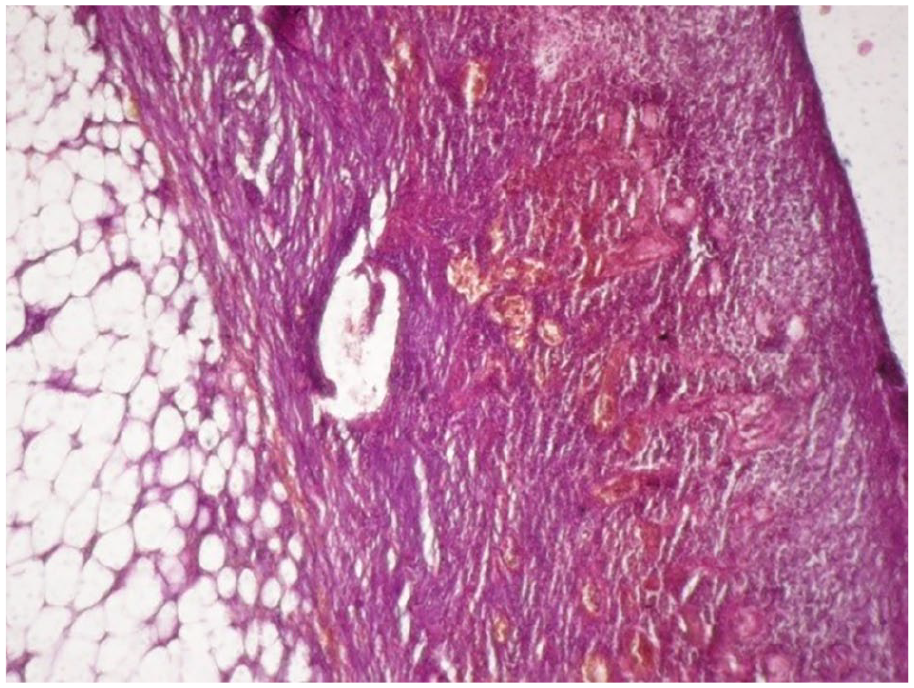
Histopathology of the polyp of the descending colon, showing fat cells suggestive of lipoma.
Discussion
Gastrointestinal lipomas are rare benign tumours. However, they are second most common tumour in the colon after adenomatous polyps 5 and the most common non-epithelial benign tumour of the gastrointestinal tract. 5 In autopsy series, the incidence of colonic lipoma ranges from 0.035% to 4.4%. 4 Lipomas described in the literature range in size from 2 mm to 30 cm. 5 Mostly, they remain asymptomatic and are diagnosed incidentally during colonoscopy or surgery. 4 They rarely become symptomatic, usually if they reach a large size (>2 cm) to manifest as abdominal pain, altered bowel habits, rectal bleeding and sometimes having more severe consequences such as intussusception, obstruction, perforation and prolapse. 4 They are common in the fifth and sixth decades of life and have a slightly female predilection. However, other series have reported equal sex distribution. They are usually solitary lesions of varying size, sessile or pedunculated, more common on the right hemicolon, with decreasing frequency from the caecum to sigmoid colon. Multiple lipomas are seen in 10–20% cases, particularly when present in the caecum. Colonic lipomas arise from the submucosal layer in 90% of cases, with just 10% arising from the subserosal or intermucosal layer. 4
Colonoscopy allows direct visualisation of a submucosal lipoma. It appears as a mass covered with normal mucosa. The other characteristic endoscopic findings are elevation of the mucosa over the lipoma with biopsy forceps (tenting sign), indentation and restoration of the shape of the lipoma with biopsy forceps (cushion sign) and extrusion of fat after biopsy of the colonic mucosa (naked fat sign). 6 On barium enema, a lipoma of the colon appears as ovoid, well-delineated and smooth radiolucent mass which changes its size and shape with bowel peristalsis (squeeze sign). 7 However, whilst a barium enema is not diagnostic for lipoma, it is a good investigation for intussusception. Careful ultrasonography (USG) evaluation in cases of pain in the abdomen focused over the region of interest and symptom in a symptomatic patient may identify an intraluminal space occupying the lesion if a lipoma is present. Lipomas are usually missed or overlooked if USG is performed too fast or may be mistaken for another pathology such as faecal material, or there is a missed differential diagnosis of lipoma in the mind of the USG operator. 8 Many factors may contribute to missing the lesions such as the small size, large body habitus, poorly prepared bowel and the presence of bowel gas. These all are limiting factors in the assessment and prevent precise identification by USG. Endoscopy and CT scan are usually required and are helpful in confirming the diagnosis.
A CT scan is the preferred non-invasive radiological modality in patients with a lipoma presenting with intussusception. A colonic lipoma appears as a spherical or ovoid shape mass, with smooth, sharply demarcated margin having a thin fibrous septa within it. 9 The CT Hounsfield unit value is between –40 and –120. In the presence of prominent fibrous septa and nodularity, liposarcoma may be considered in a differential diagnosis.
The aetiology of intussusception in adults is usually identified in 90% cases, with tumours as the most common lead point. 4 Although lipomas are the most common benign tumours of the colon, they rarely cause colonic intussuception. 10
Therapeutic options for a colonic lipoma vary from colonoscopic resection, local excision, segmental resection and hemicolectomy. 5 Use of a barium enema as a diagnostic and therapeutic tool has been replaced by air or saline reduction as safer options in cases of intussusception, as the risk of perforation and barium peritonitis and poor pressure control are setbacks with barium which are not associated with air or saline reduction. We did not proceed with reduction by barium, air or saline, as the presentation was acute, and the size of the lesion was an indicator for operative intervention and resection. Even with imminent resection surgery planned for definitive treatment, reduction is preferable to minimise bowel oedema and to minimise microbial colonisation and migration. The choice of procedure depends on the size, location, preoperative diagnosis and presentation. The endoscopic removal of lipoma smaller than 2 cm is easily possible 11 . However, safe removal of larger lesions (>2 cm) by surgical procedure have also been reported2,11. A few studies have reported a greater risk of perforation associated with the removal of lipomas ⩾2 cm. 12 In patients presenting with intussusception and where intra-operative frozen section has not been not performed, extensive resection of the colon is recommended, as two thirds of colonic intussusceptions have resulted from primary adenocarcinoma. In recent years, laparoscopy and mini laparotomy have been reported as an alternative to conventional laparotomy in the removal of large colonic lipomas. The definitive diagnosis of a colonic lipoma is usually obtained from histological examination of the resected specimen. The malignant transformation is rarely observed or reported, although some may show atypical ‘pseudosarcoma’ features. The recurrence of colonic lipoma has not been reported.
In conclusion, colonic lipomas are uncommon tumours and very rarely present as intussusception. The preoperative diagnosis is sometime difficult. The therapeutic options include colonoscopic resection, local excision, segmental resection and hemicolectomy. The choice of procedure depends on the size, location, preoperative diagnosis and presentation.
Footnotes
Acknowledgements
None.
Authors’ contributions
P.K. and M.T. collected data and drafted the manuscript. A.K.K. and S.K.T. critically reviewed the manuscript and prepared the final draft.
Availability of data and materials
Data and materials are available from the corresponding author.
Conflict of interest
The authors declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Ethical approval
Banaras Hindu University does not require ethical approval for reporting individual cases or case series.
Funding
The authors received no financial support for the research, authorship and/or publication of this article.
Informed consent
Written informed consent was obtained from the patient for his anonymised data to be published in this article.
